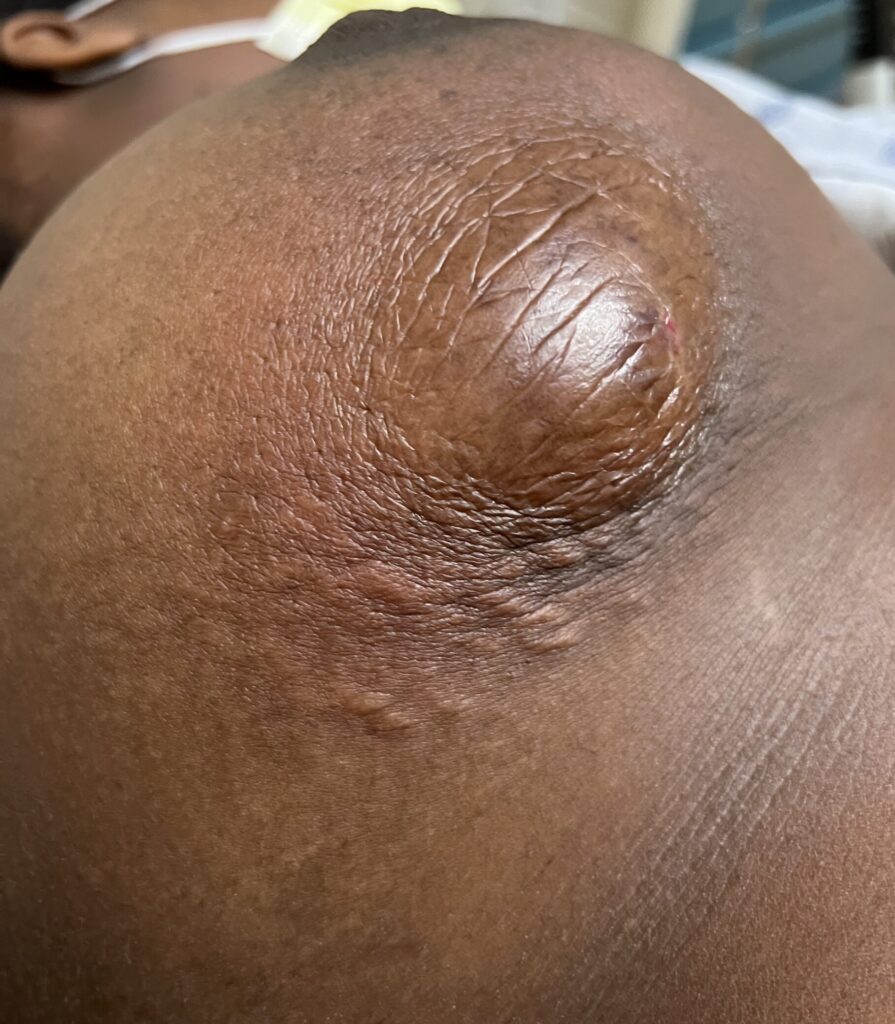
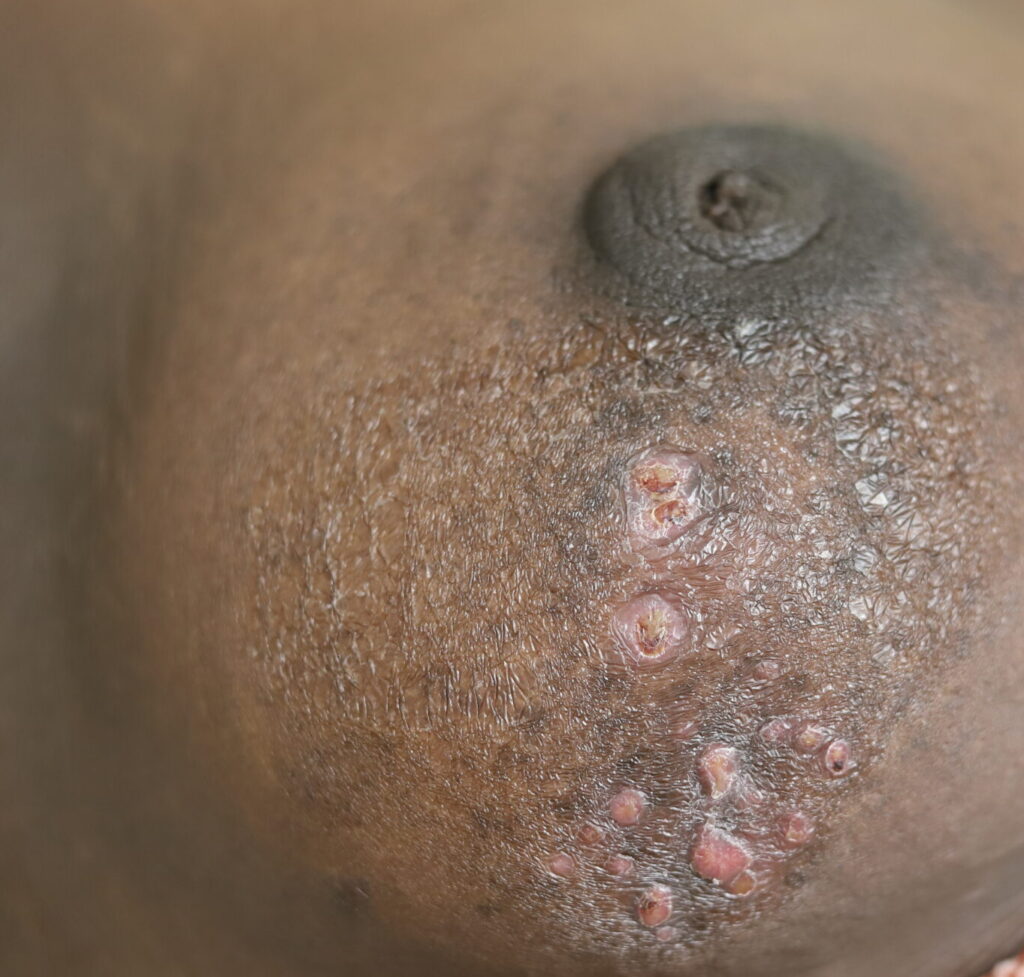
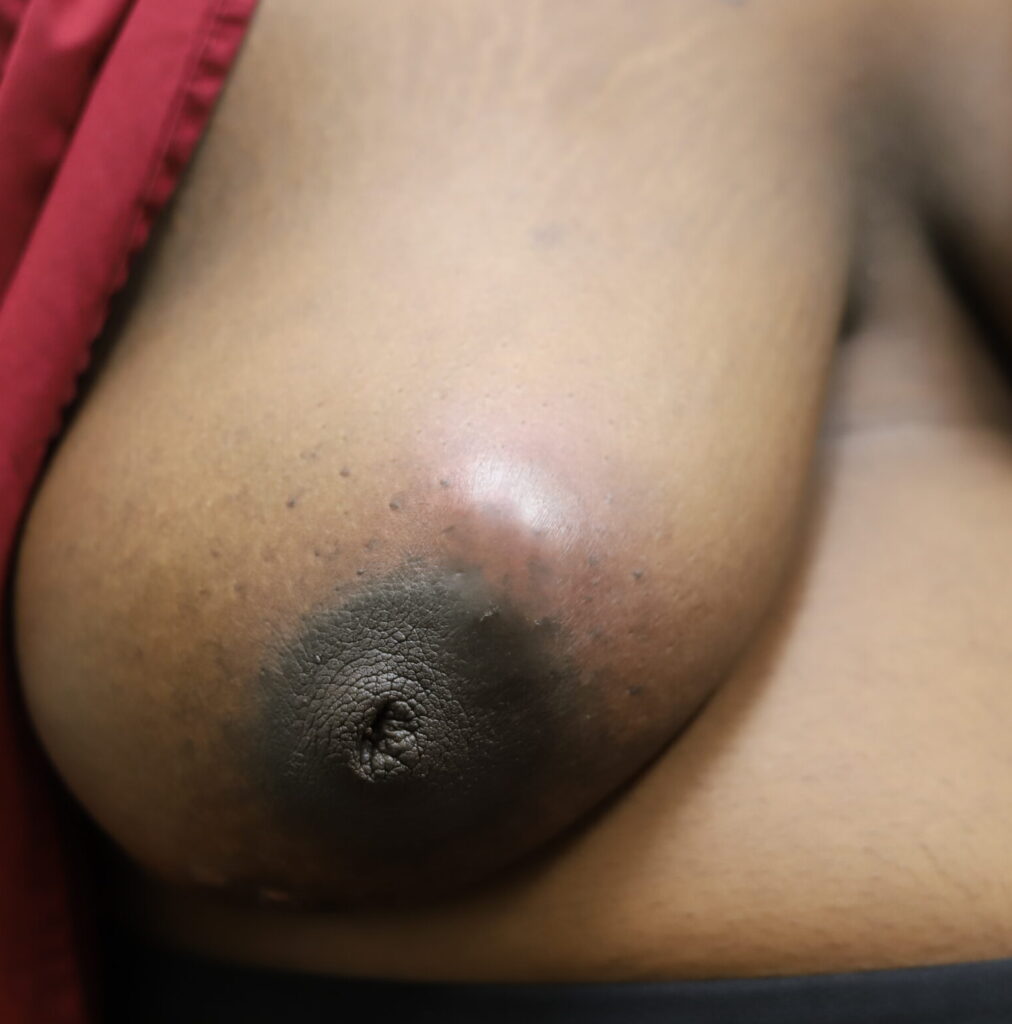
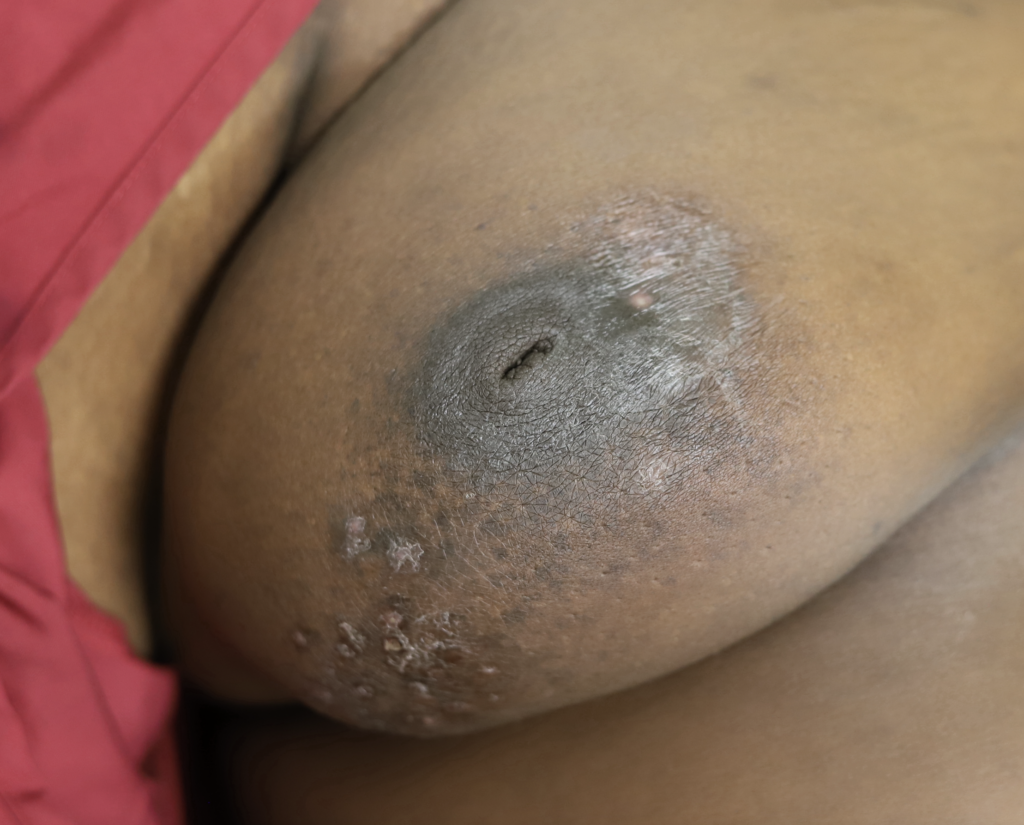
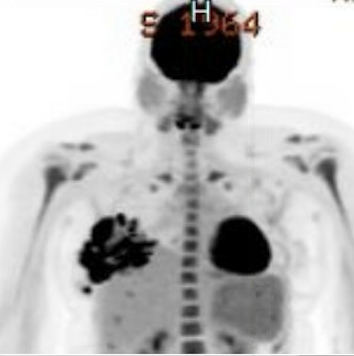
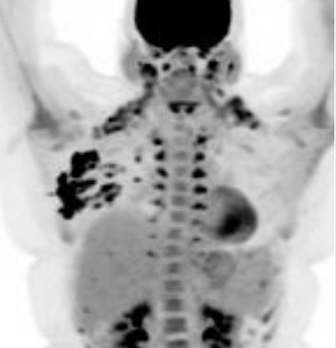
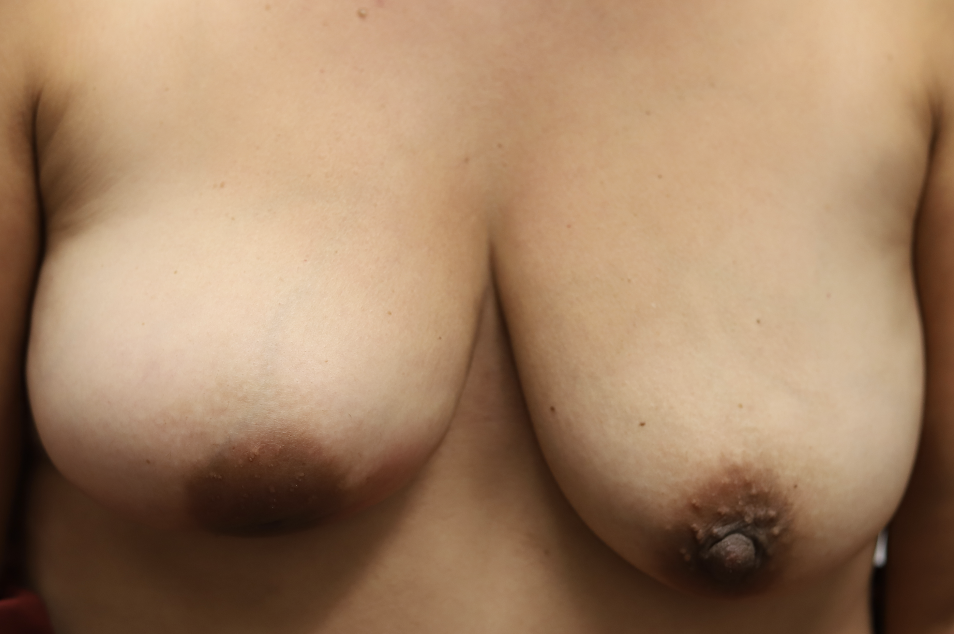
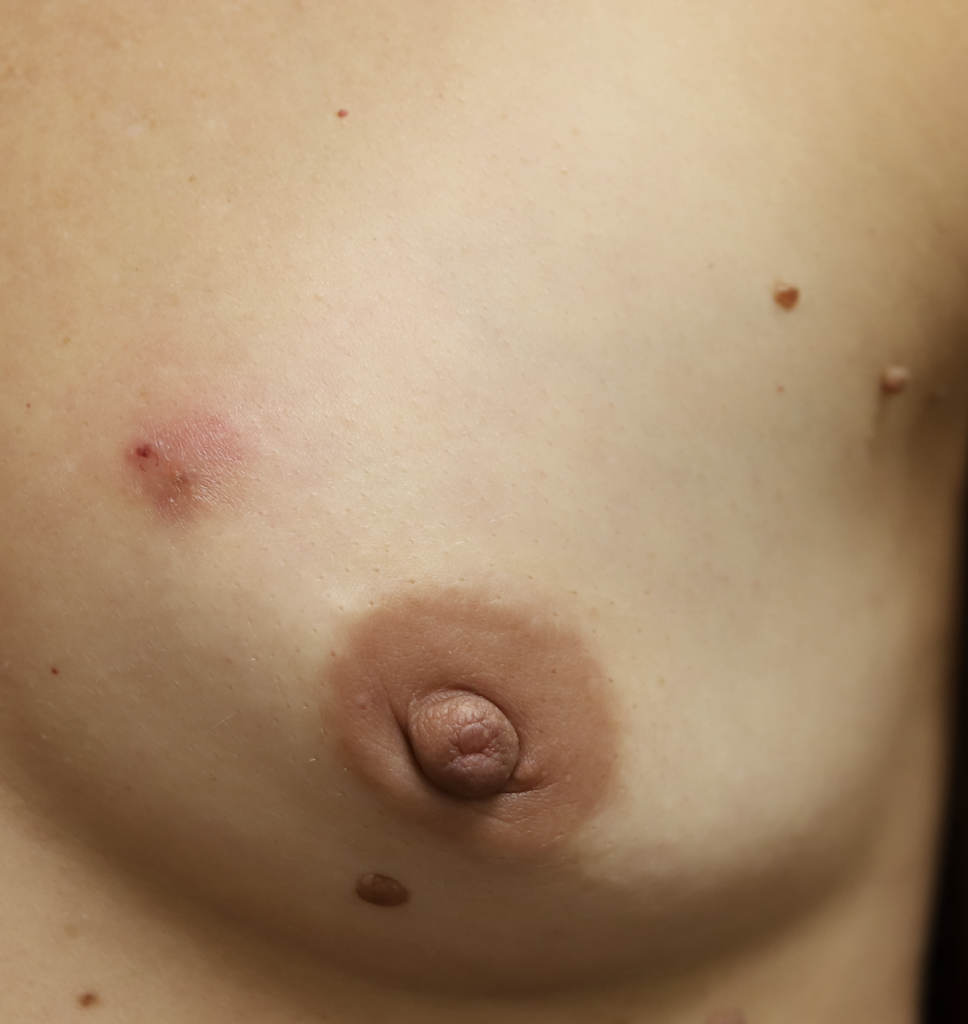
Idiopathic granulomatous mastitis (IGM) is an inflammatory disorder affecting the breast of young women in their childbearing years, and can overlap with lactation and pregnancy. It can result in development of painful inflammatory masses, fluid collections, and fistula formation. While breastfeeding from the affected breast in the setting of IGM is safe, mothers may report additional pain and difficulty with latch or milk production.
The definitive treatment for IGM is immunosuppression with the oral medications methotrexate (not safe with lactation or pregnancy) or azathioprine (safe with pregnancy and lactation). This case report describes continued breastfeeding and resolution of IGM with azathioprine therapy.
More mild cases can be treated with injection of steroid into the affected breast. This video that I presented at the American Society of Breast Surgeons in Boston spring 2023 illustrates this procedure:
PharmD Phil Anderson, who runs LactMed at the NIH, initially suggested that the infant would receive a large oral dose of steroid if they breastfed after injection. However, the dose of steroid is still lower than what would be used to treat infants for certain conditions. A more recent case report demonstrated no steroid in breastmilk, but it could potentially be impacted by time of collection and severity of disease.
So, this requires careful discussion with your healthcare provider. Without question, patients can feed from the unaffected breast during this time.
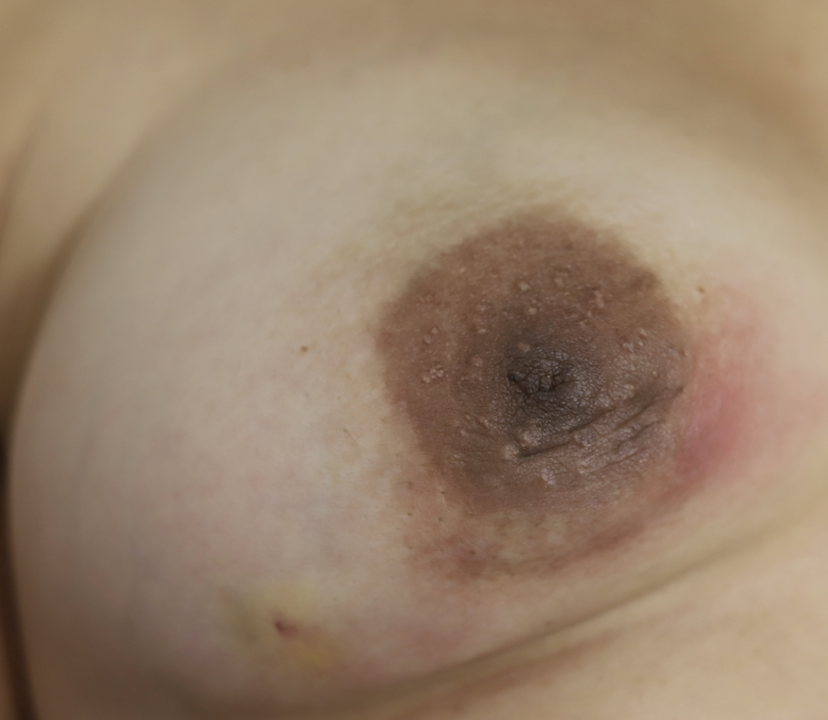
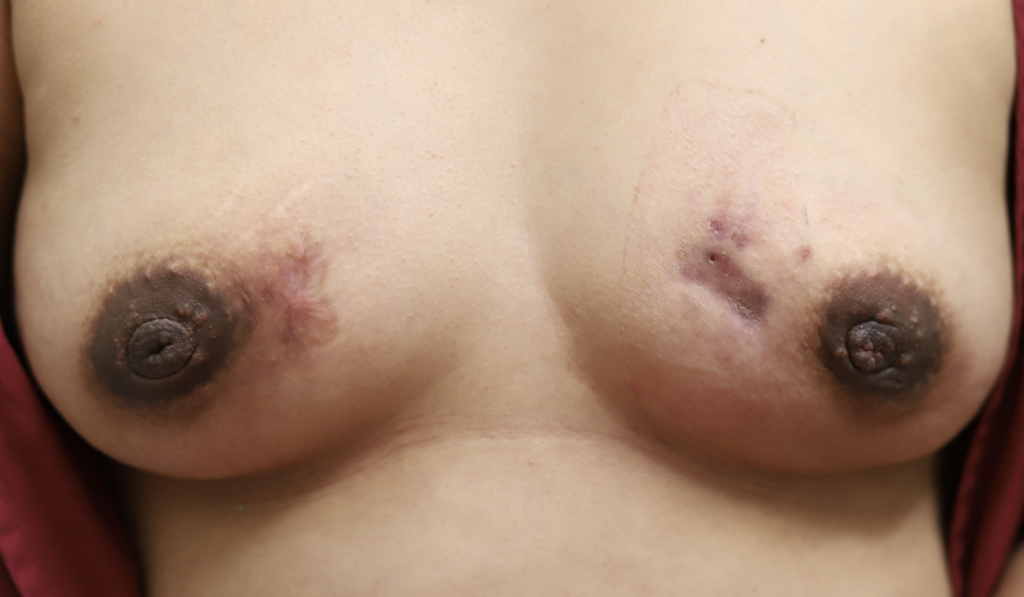
High-dose oral steroids may reduce milk supply, similar to the reported effect of high-dose triamcinolone injections at body sites other than the breast. However, if a mother has very high milk production in general, she may not notice a difference. Steroids also can cause significant insomnia and anxiety in patients taking them. Below is an image and video of a mom taking oral steroids and breastfeeding from her breast with IGM.
Mothers also may elect no treatment during lactation; fluid collections, fistula formation, and other symptomatology can be managed on an as-needed basis.
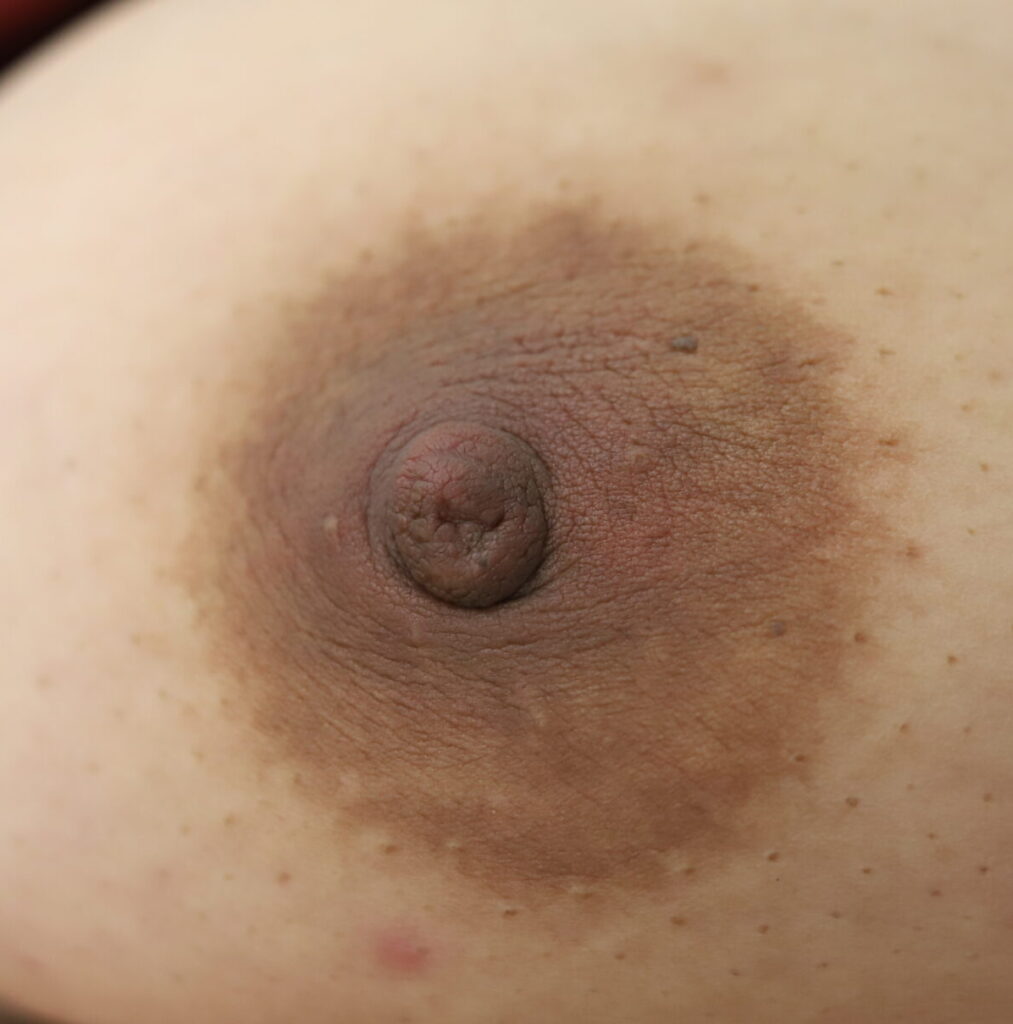
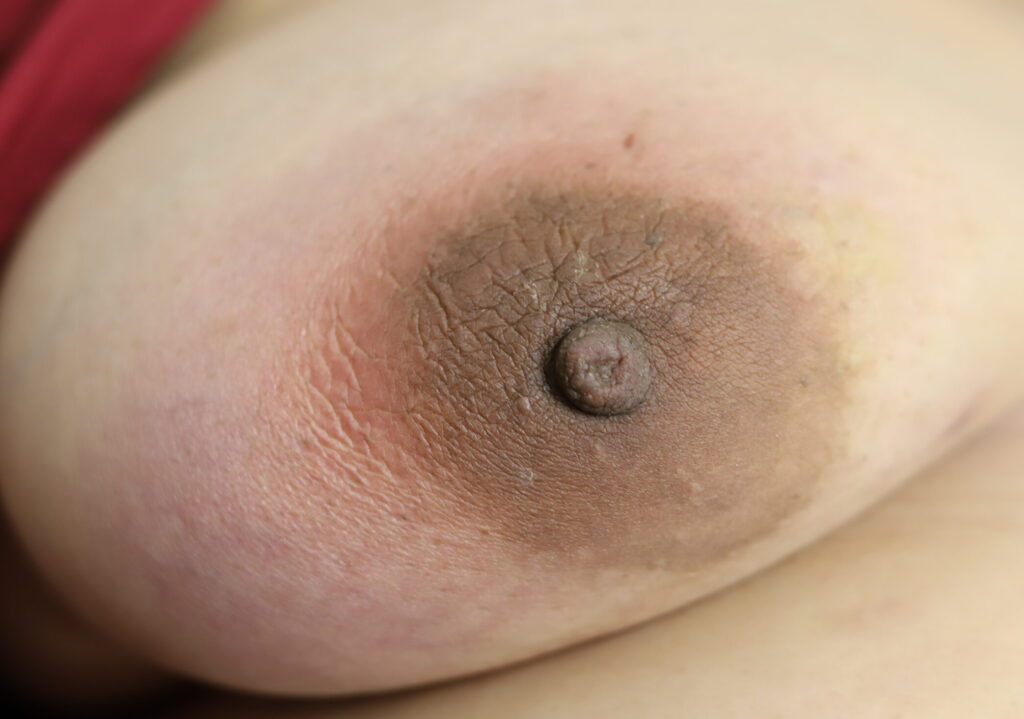

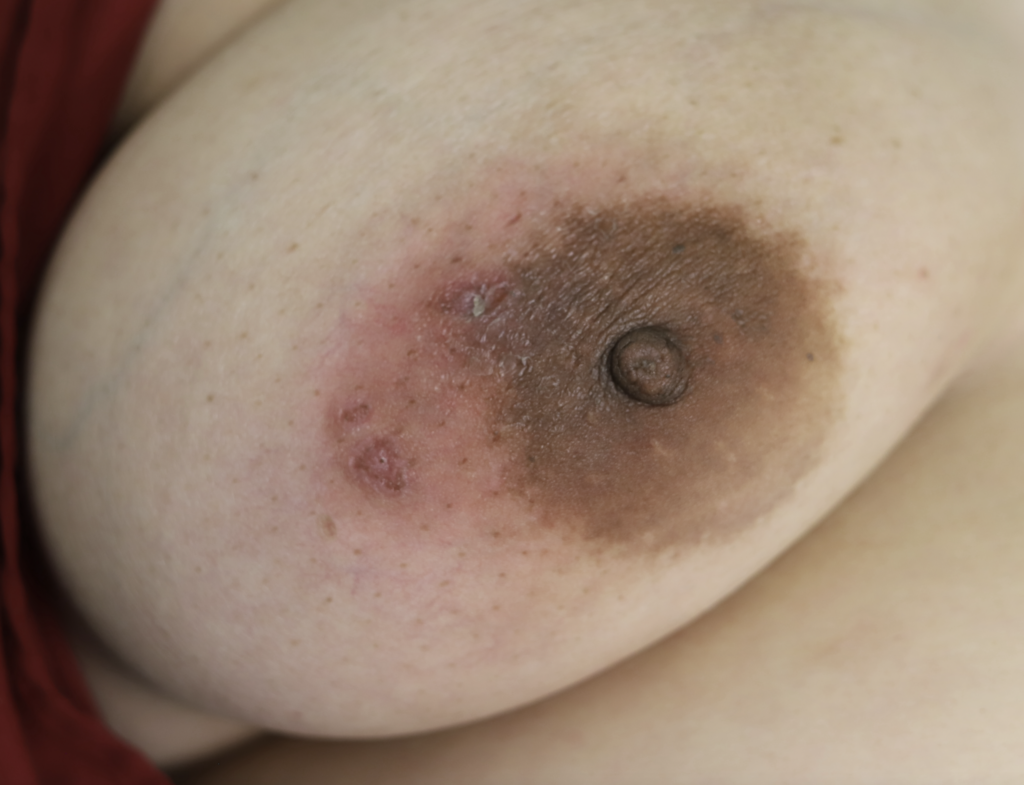
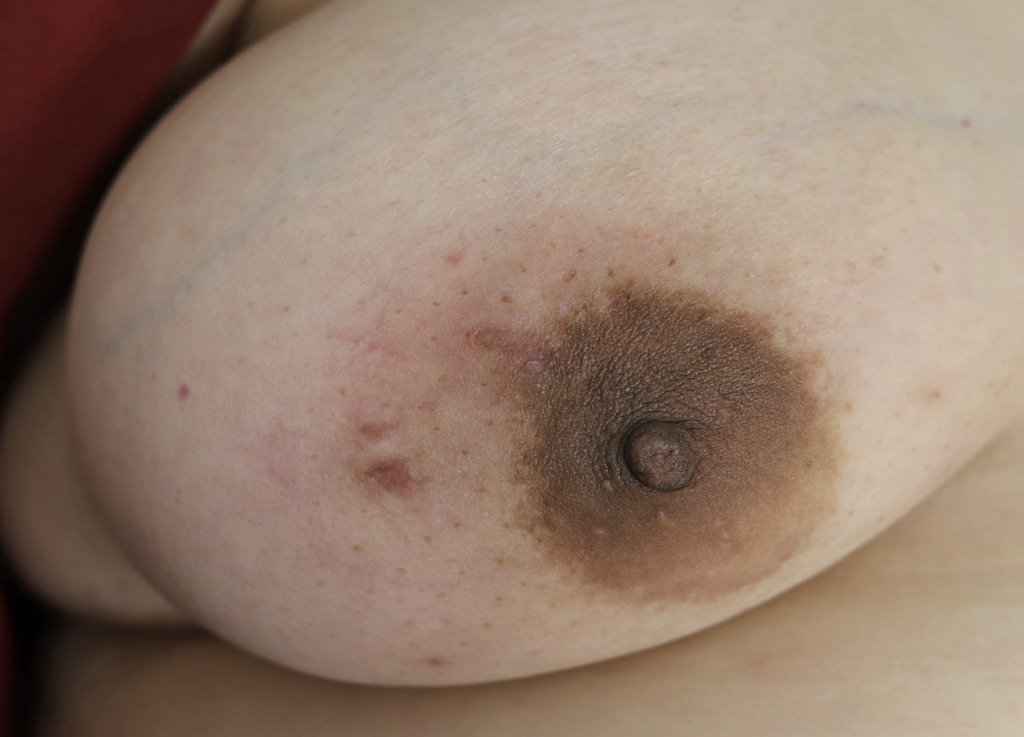
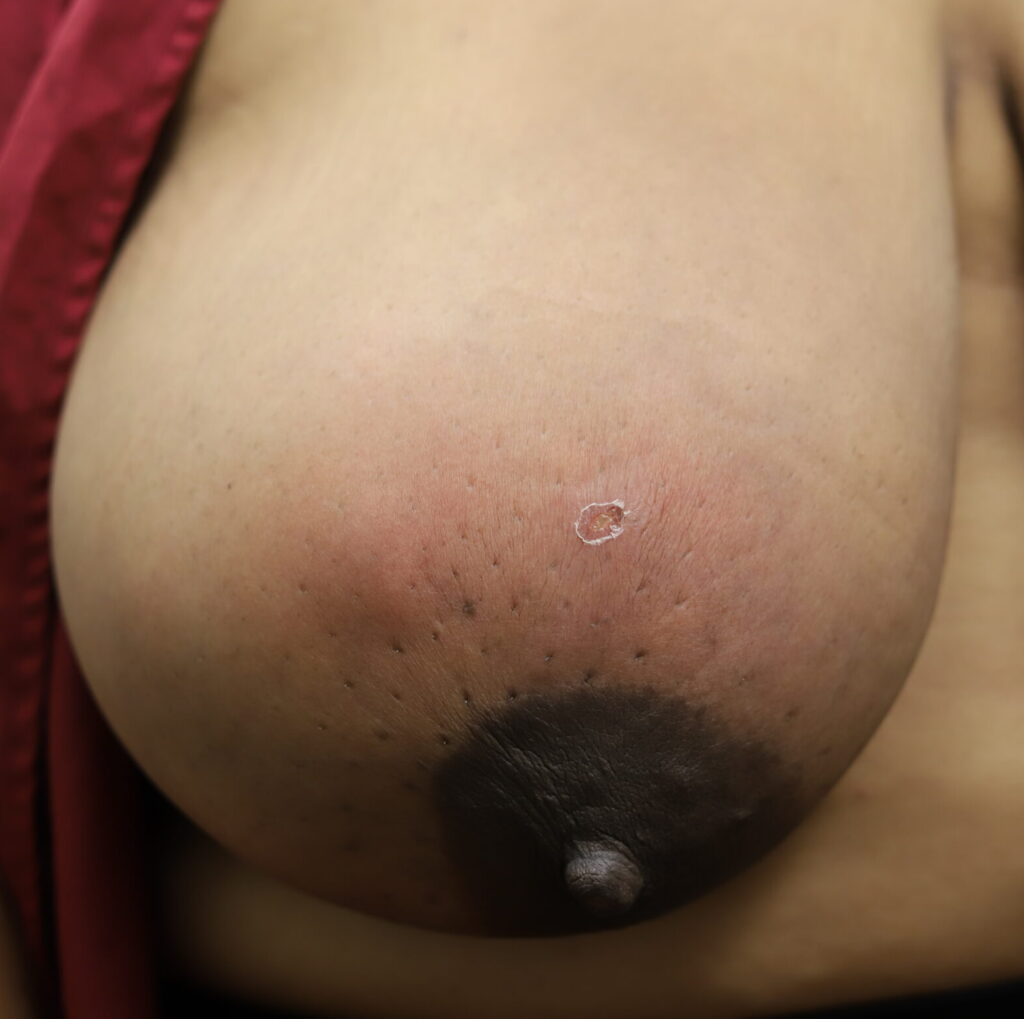
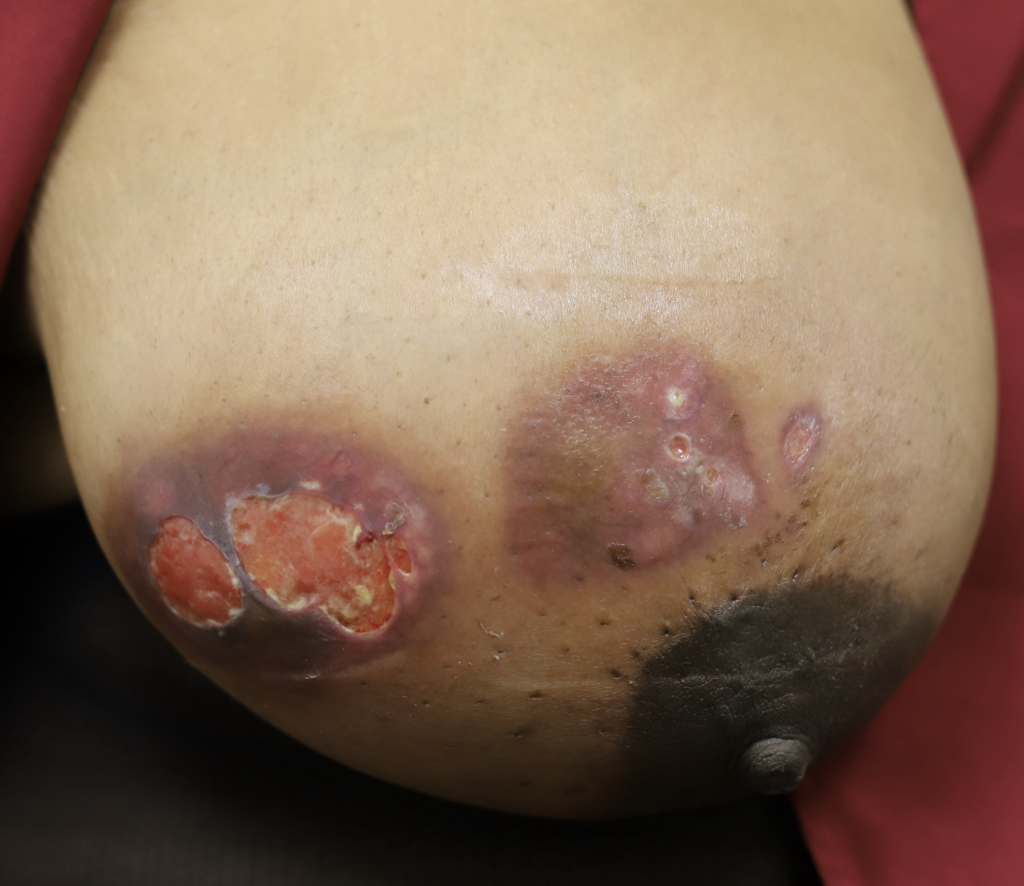
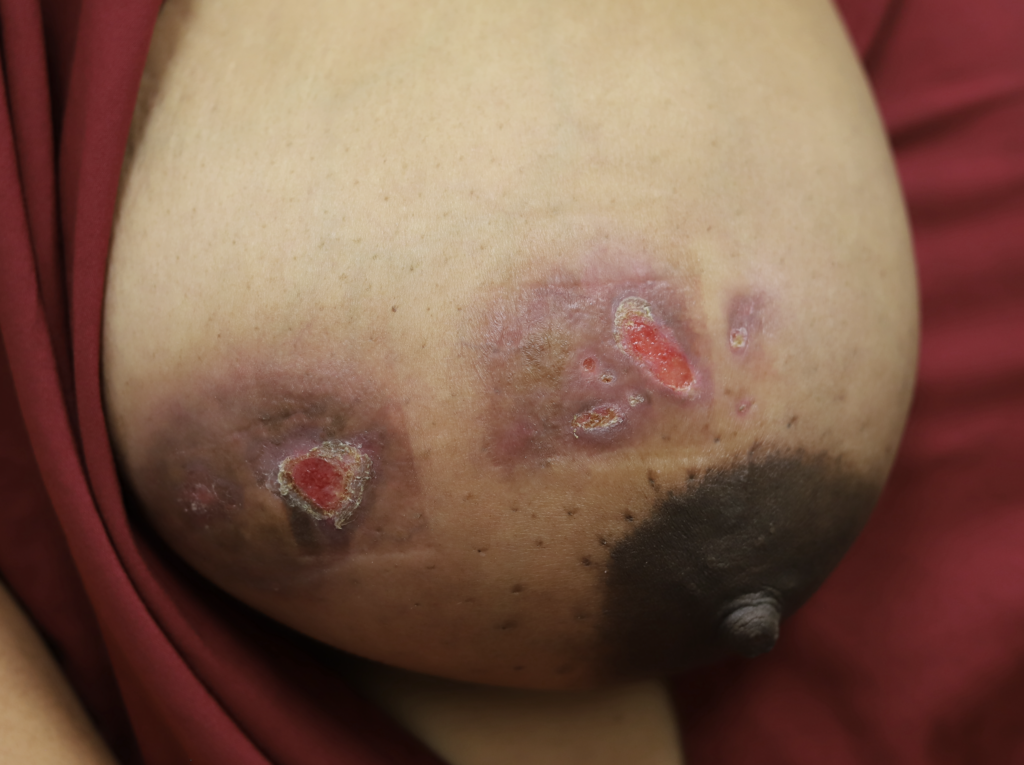
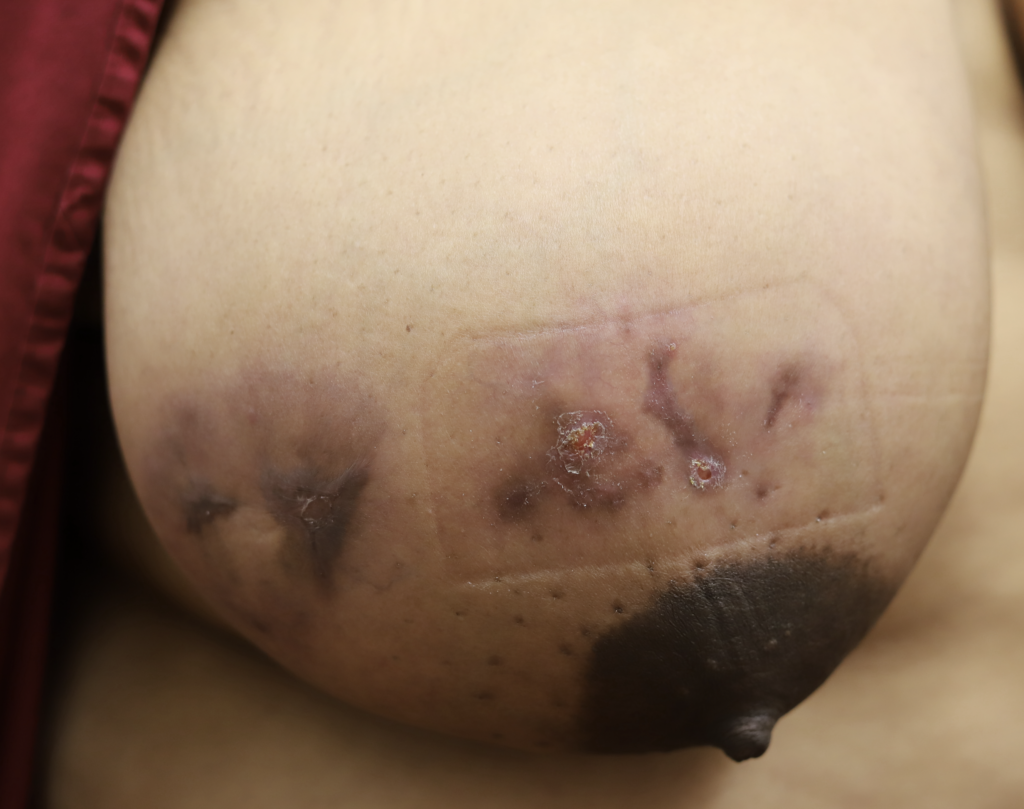
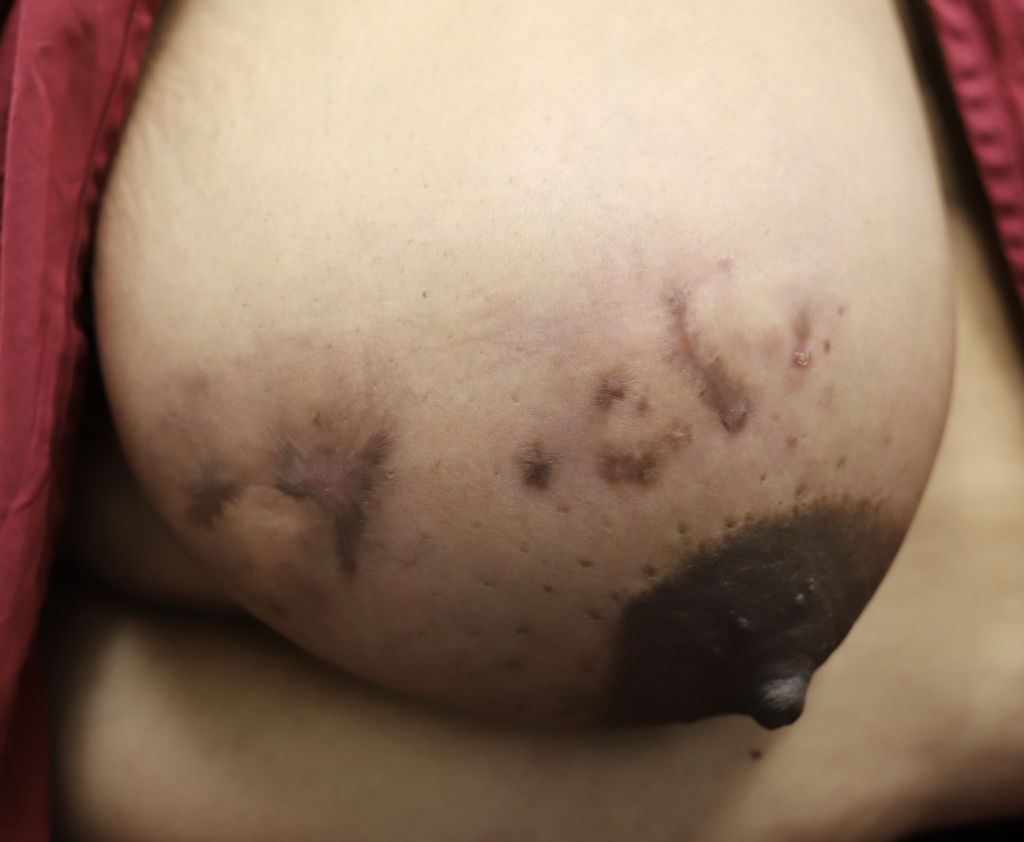
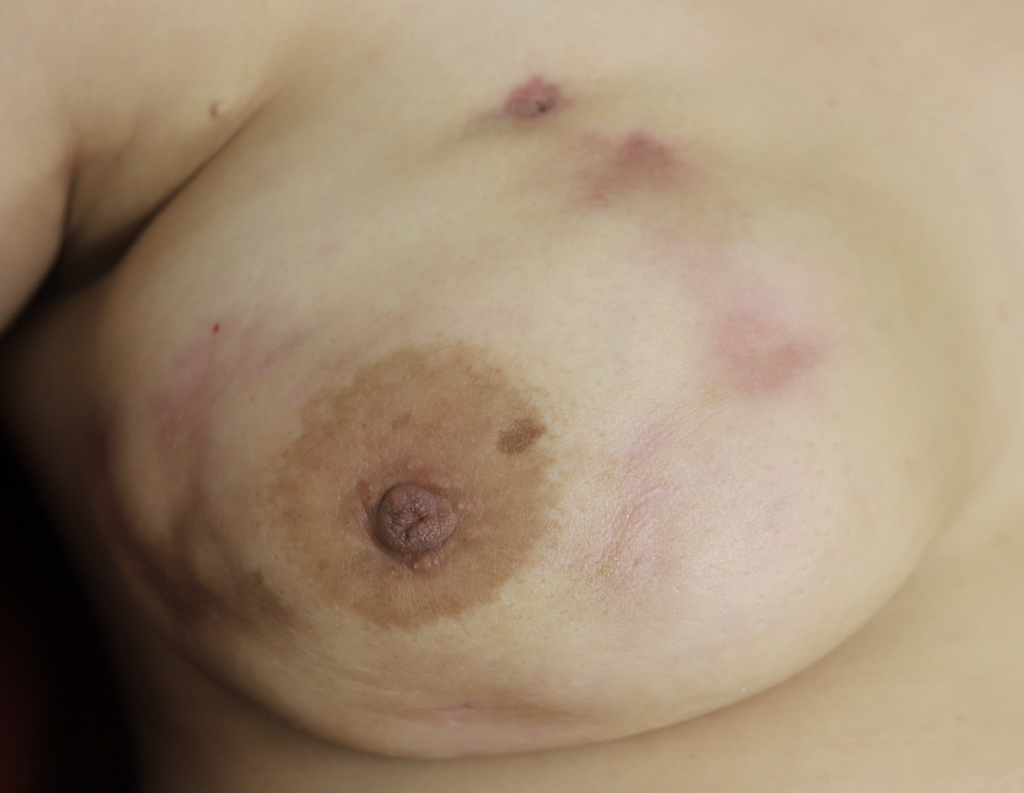
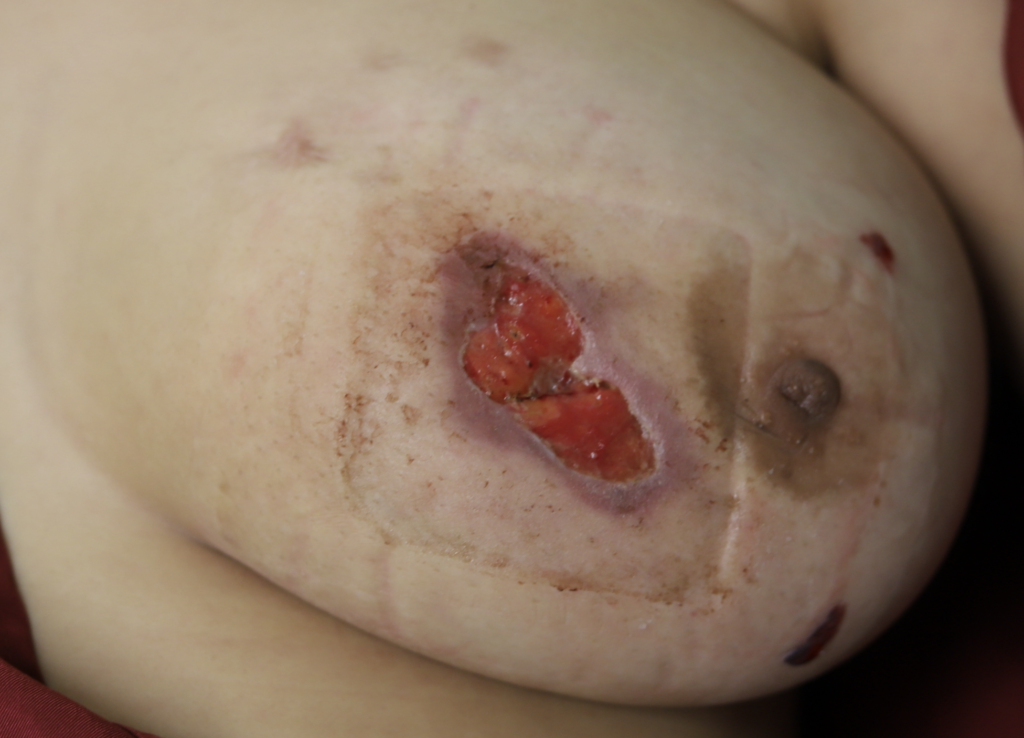
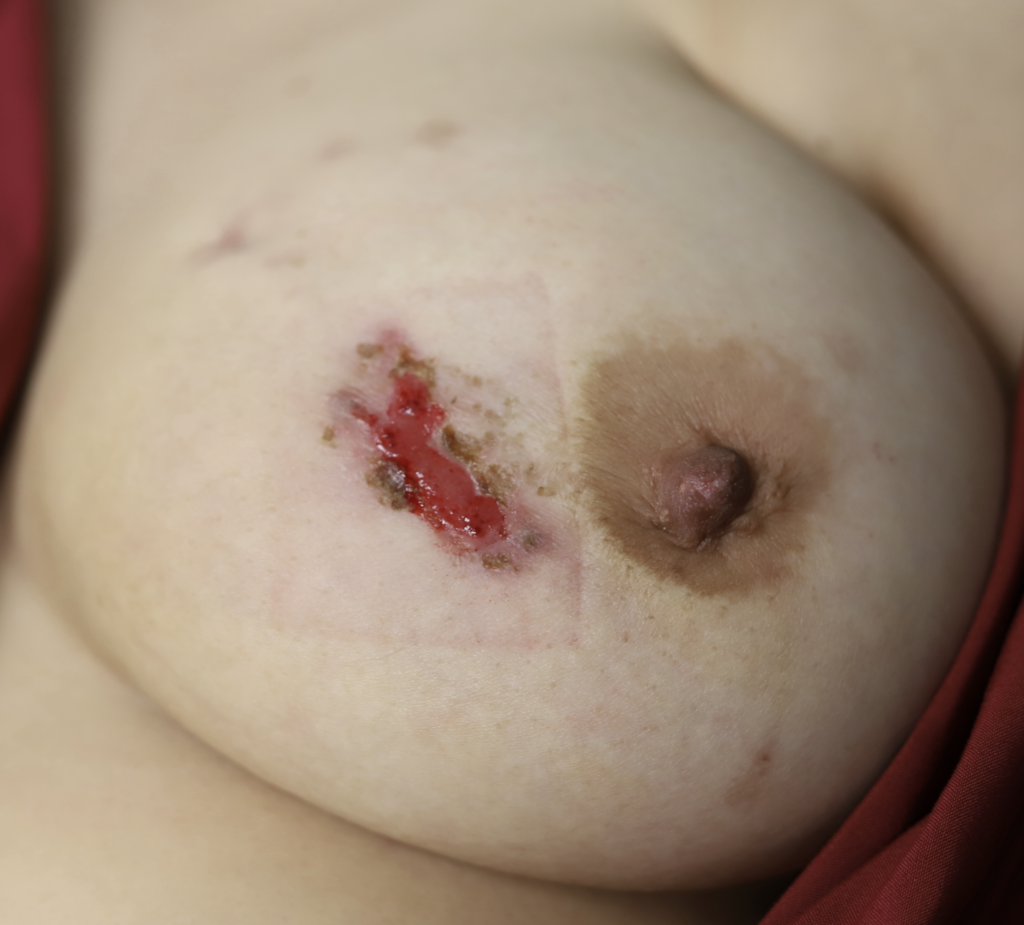
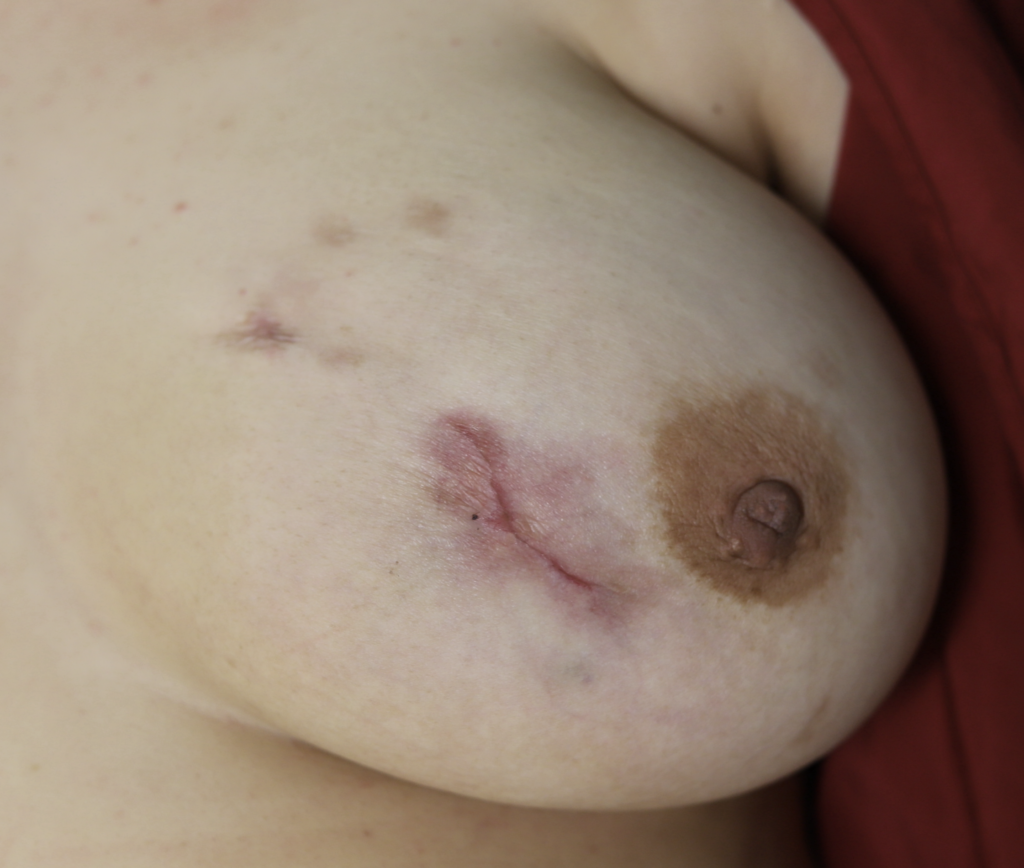
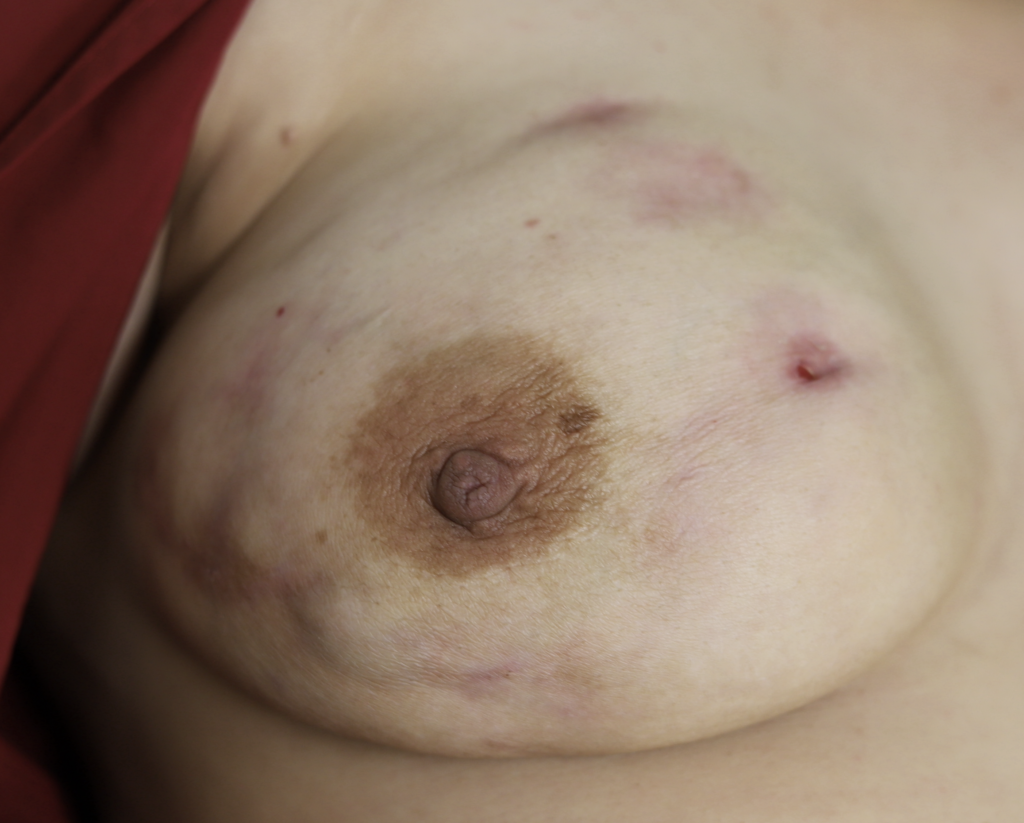
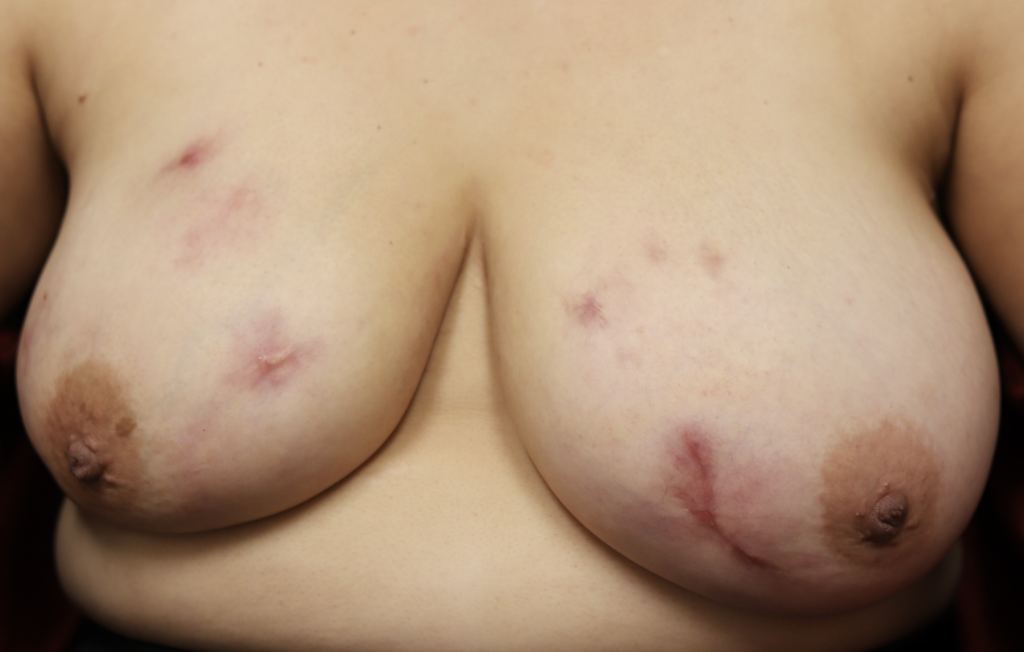
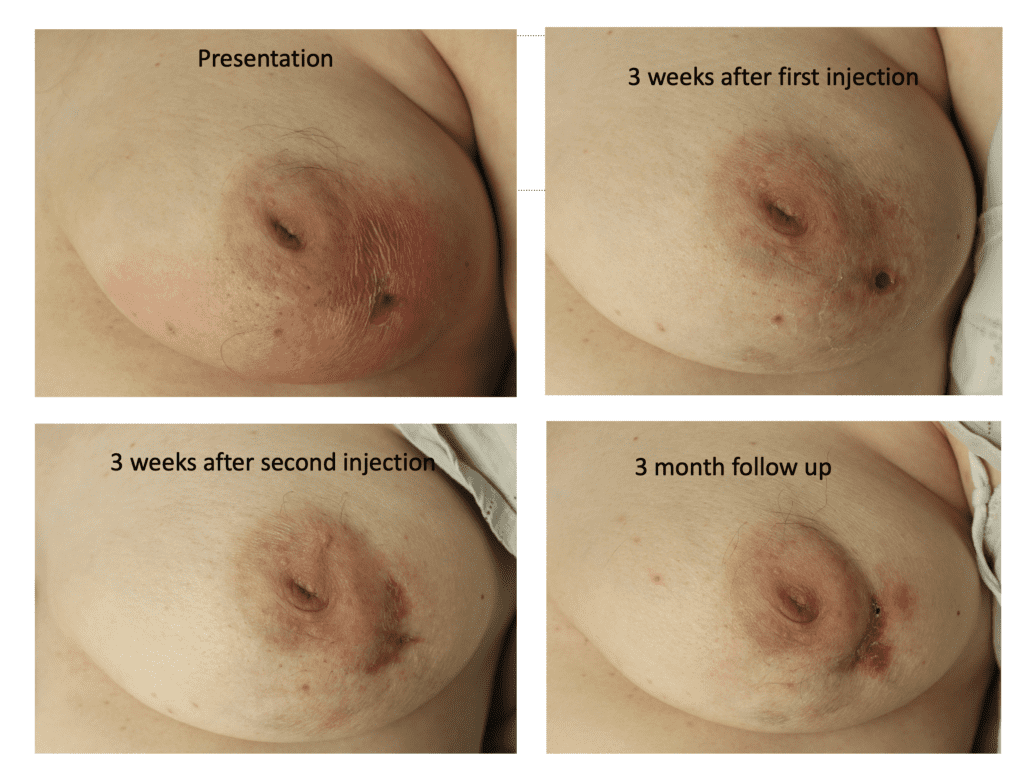

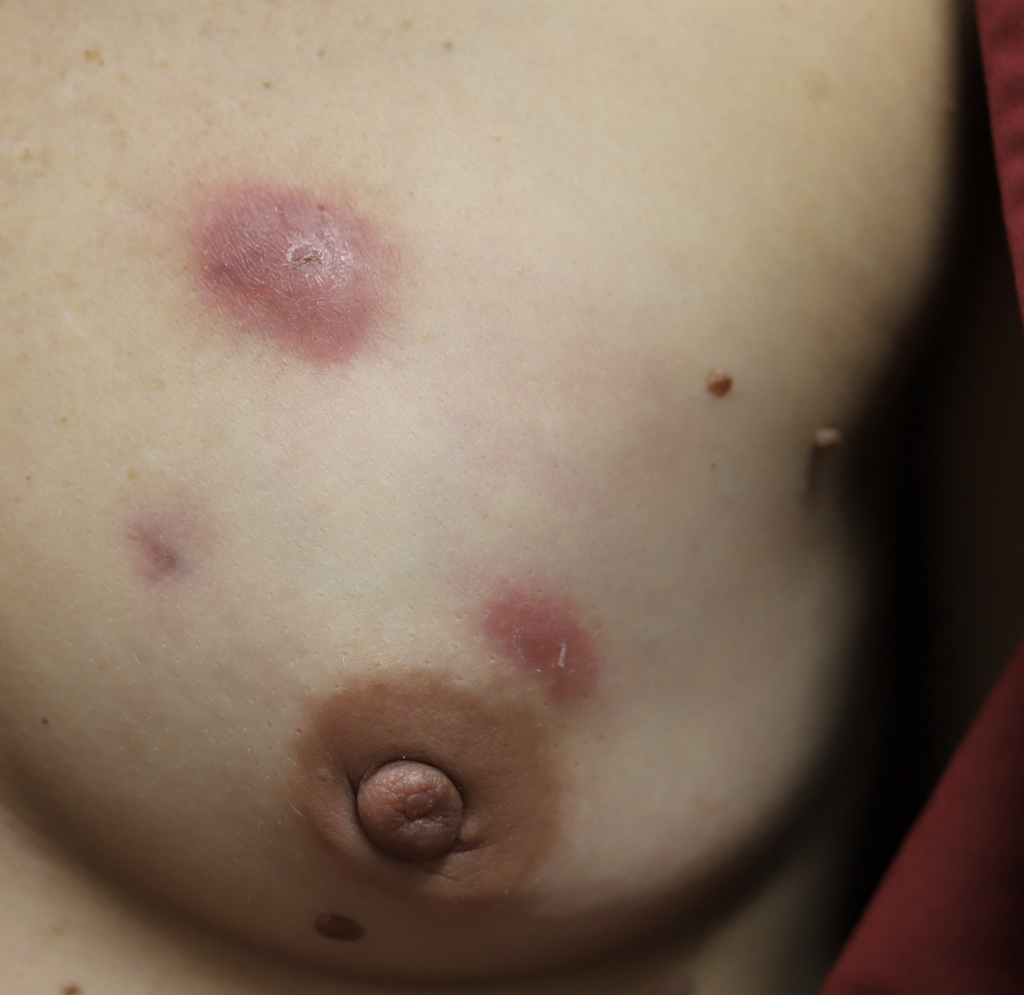
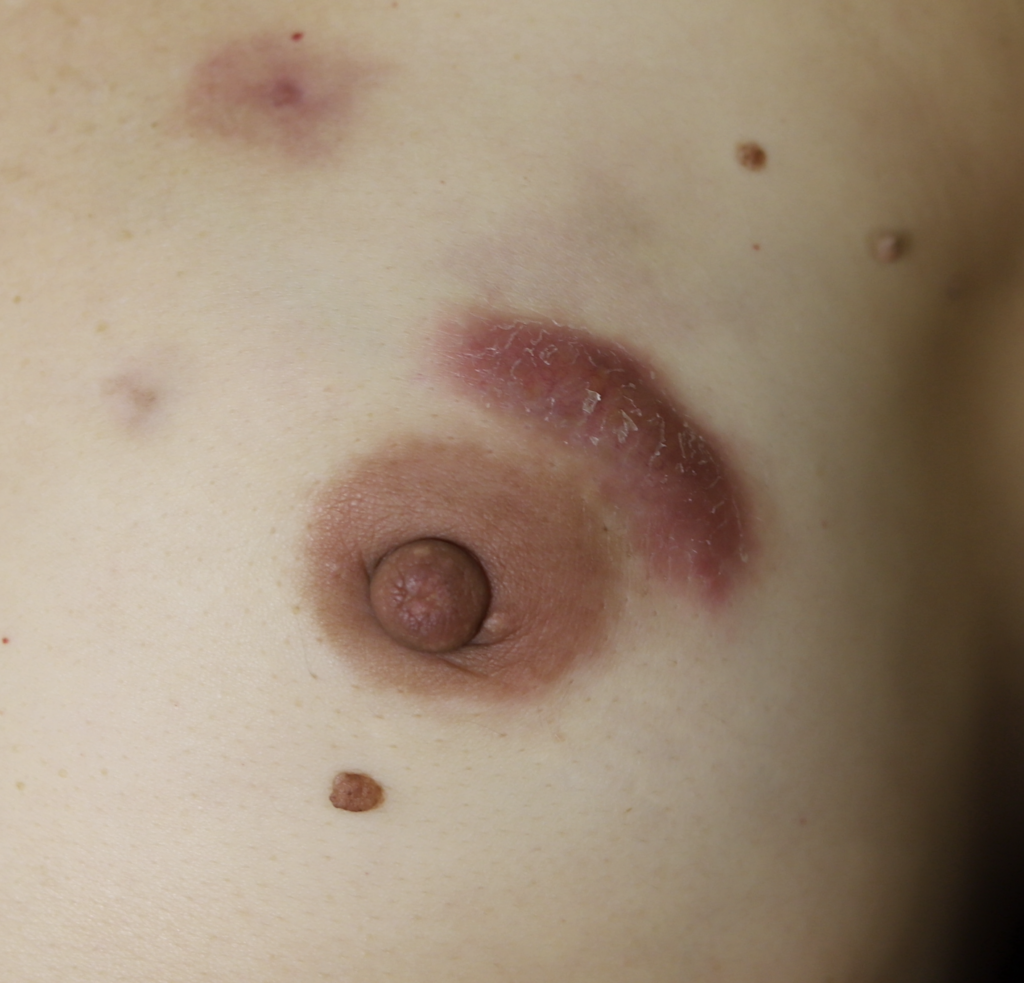
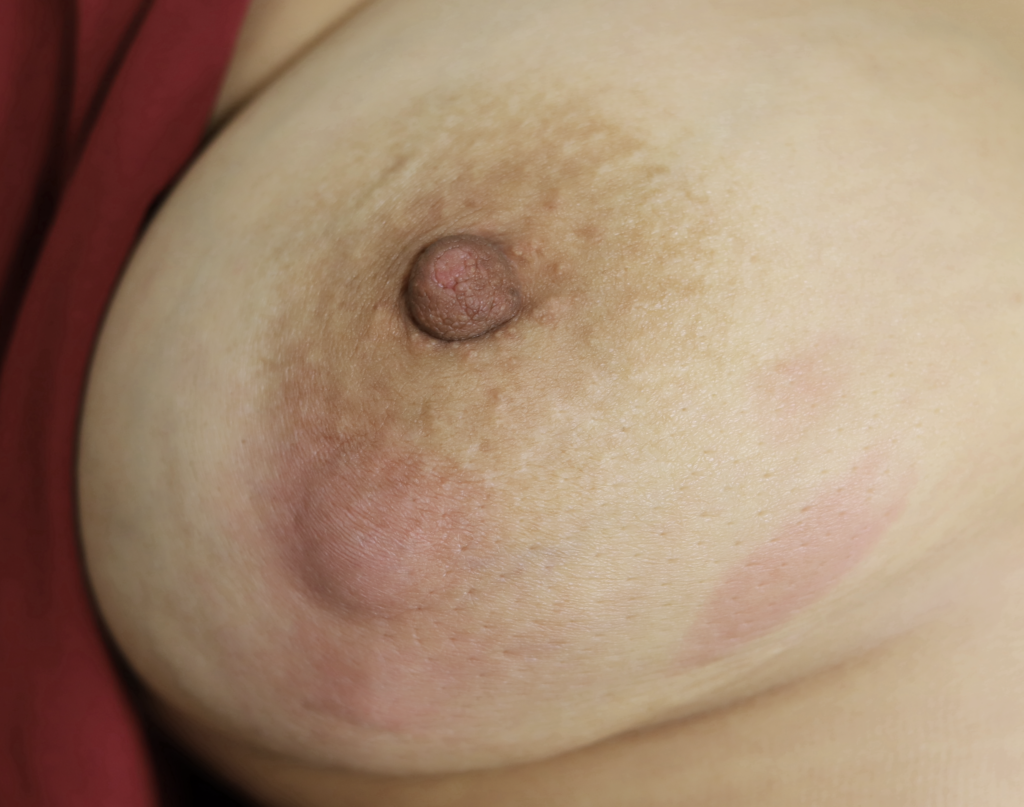
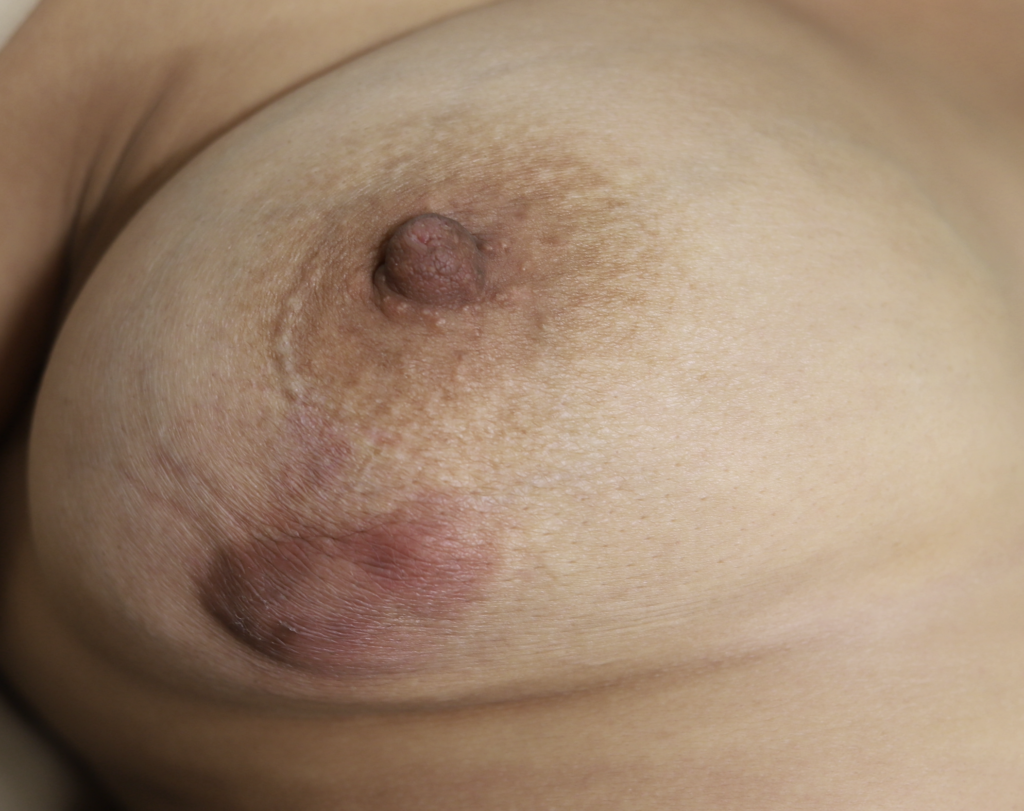
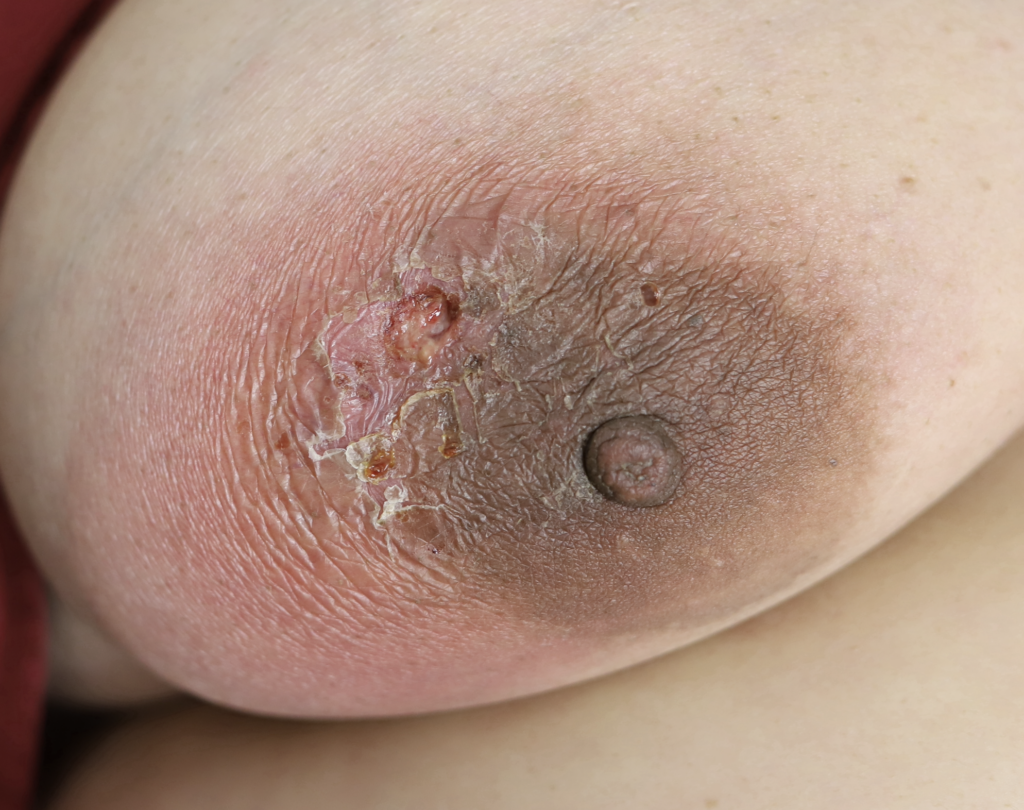
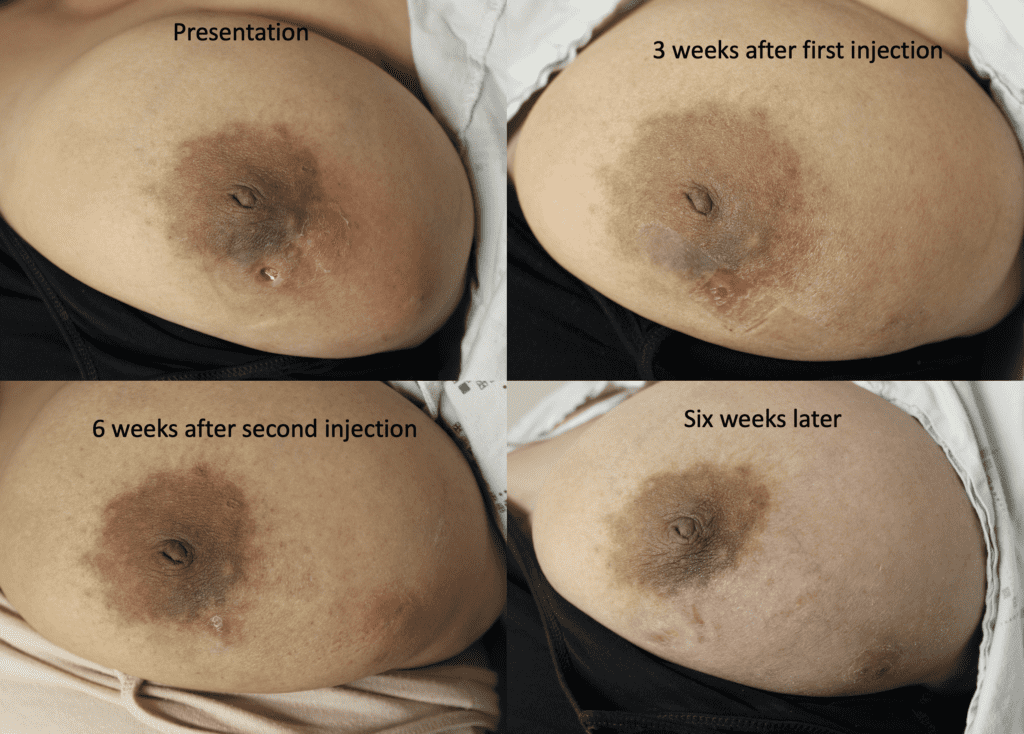
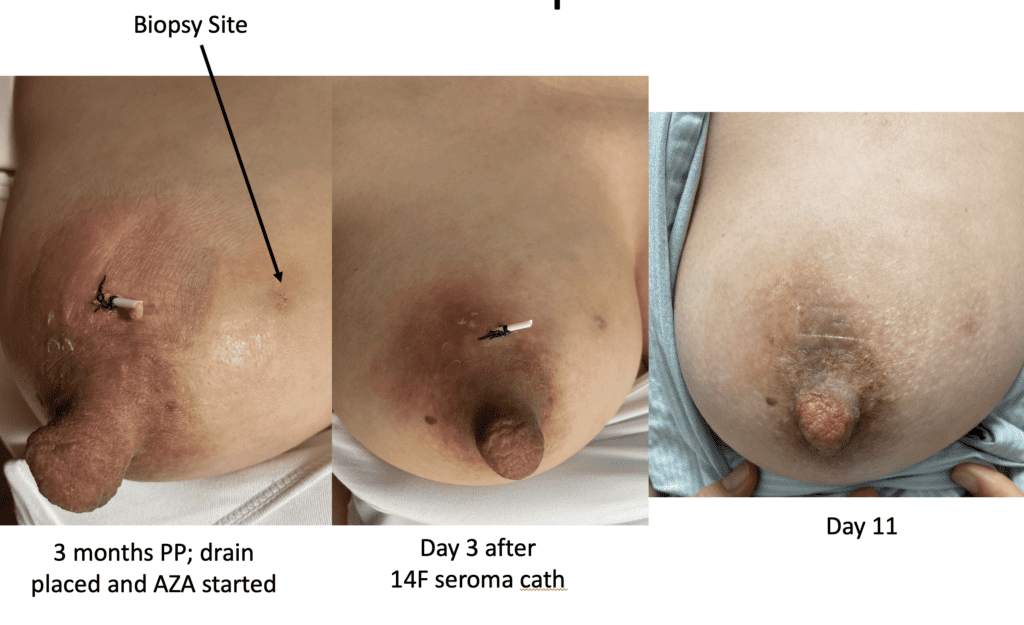
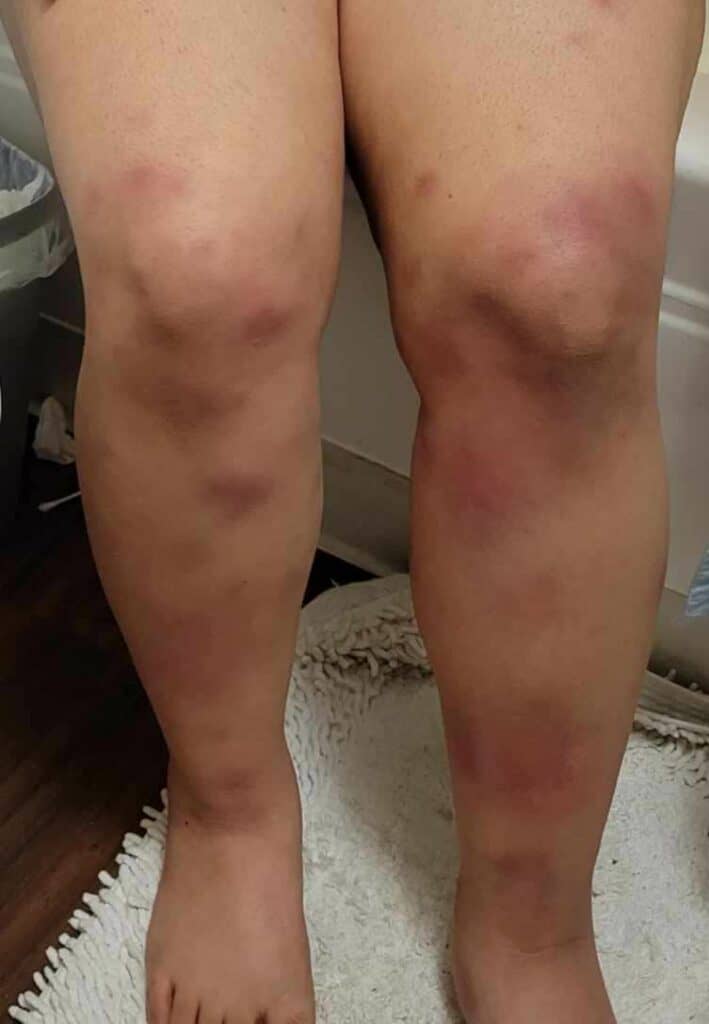
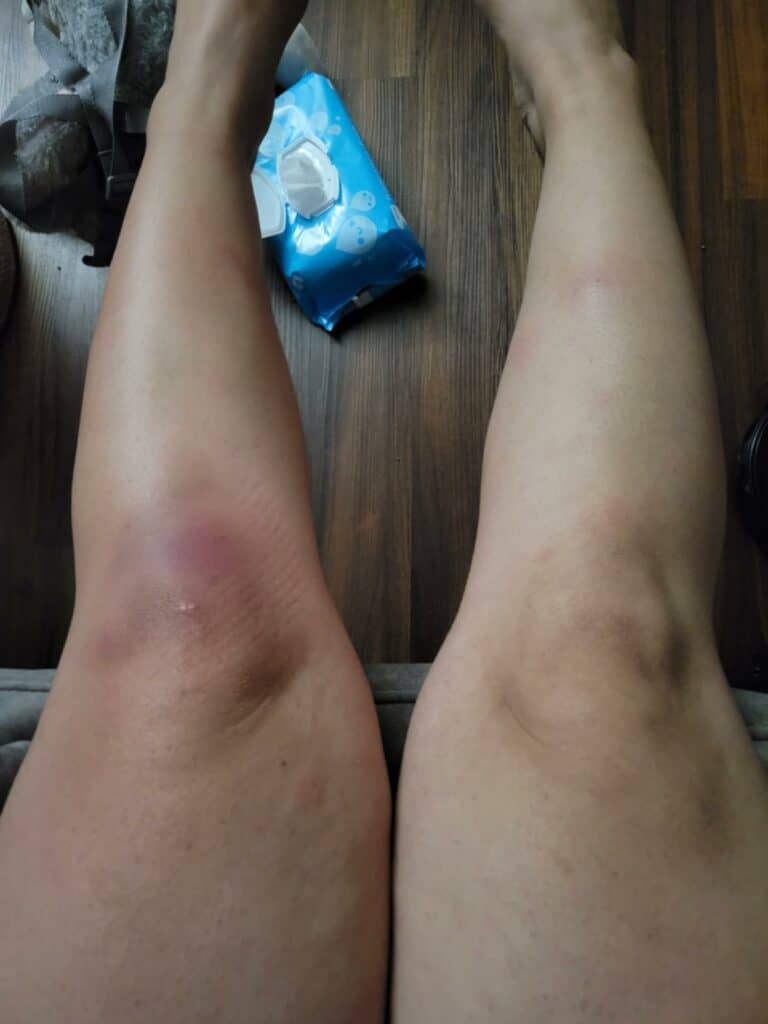
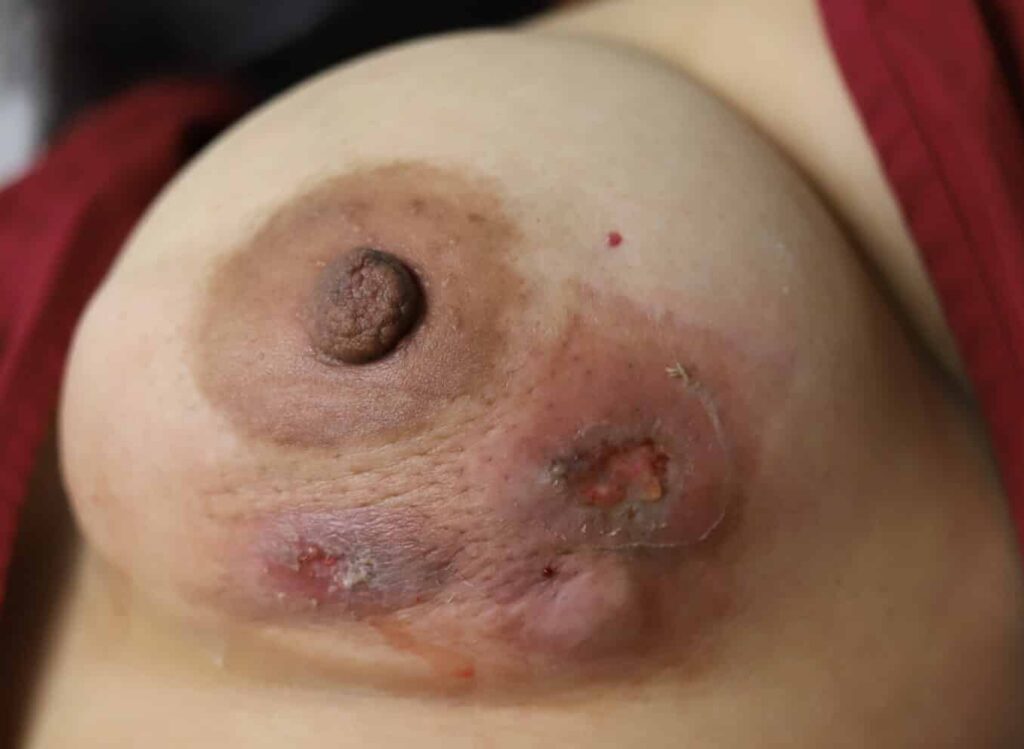
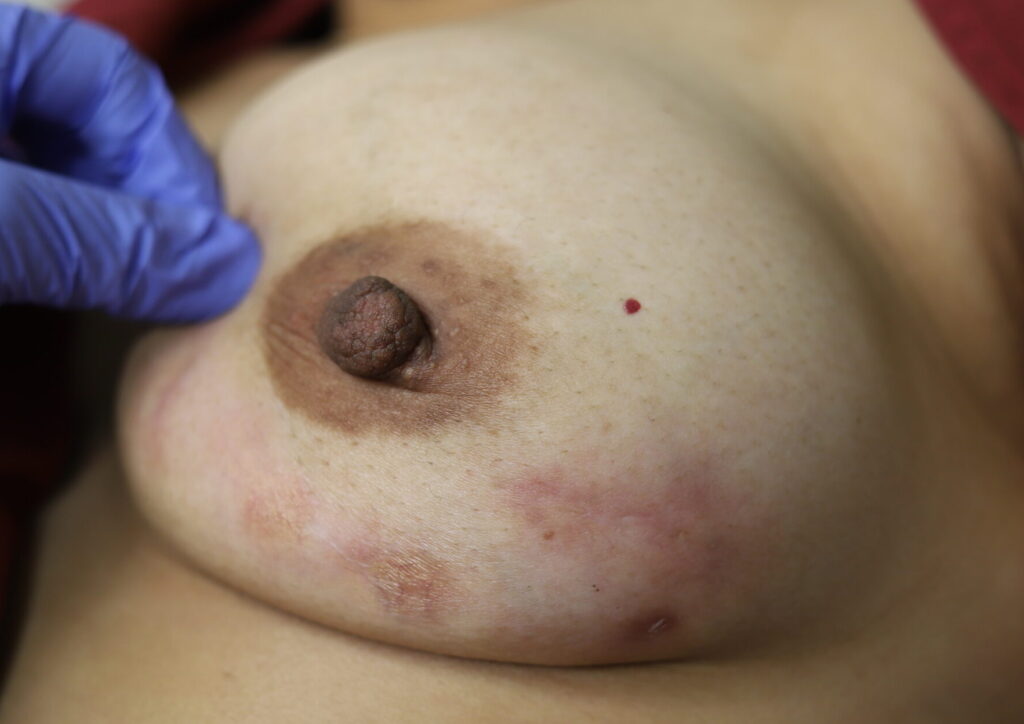
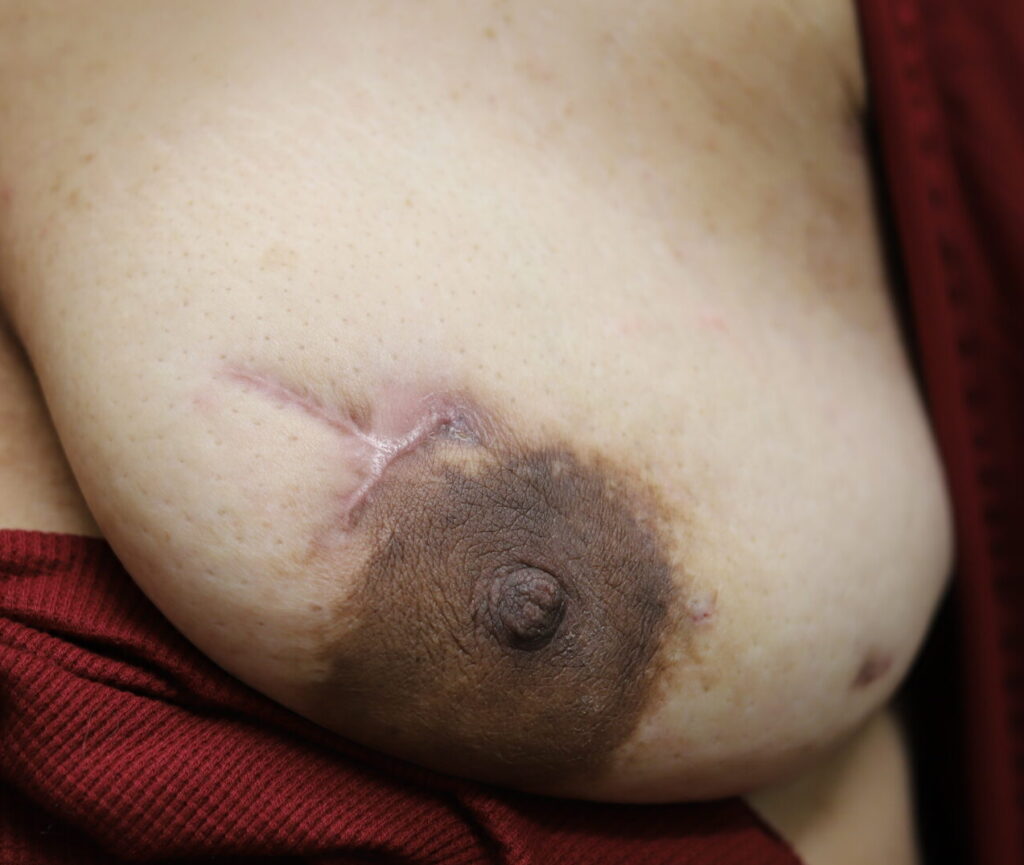
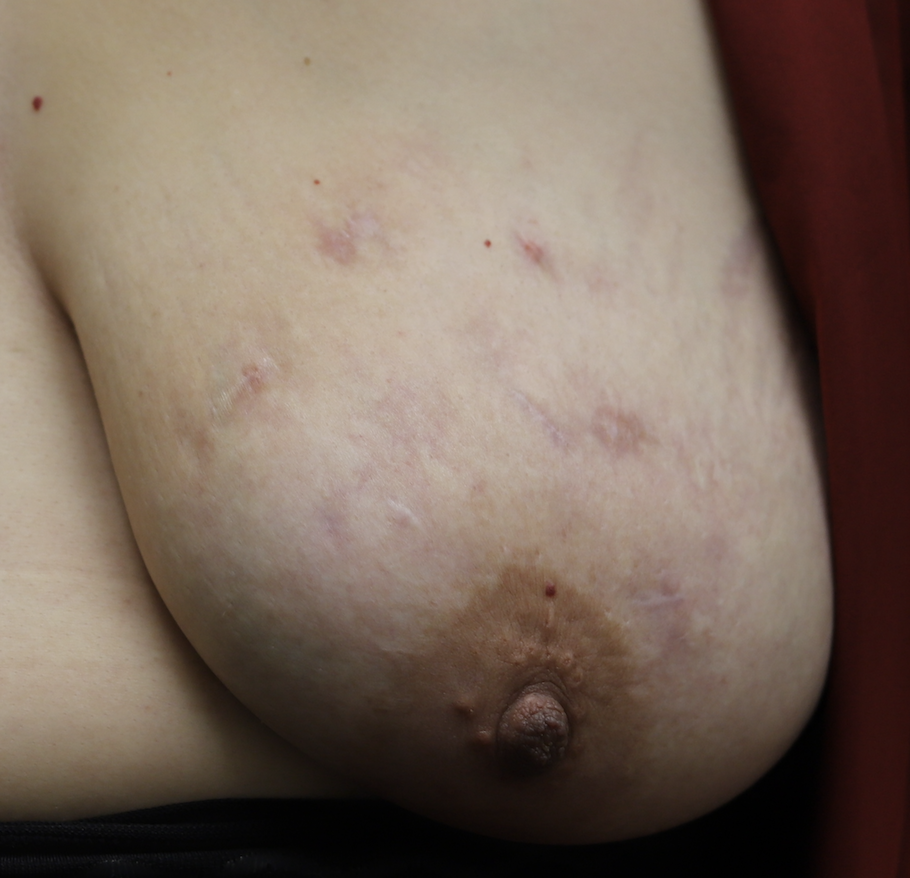

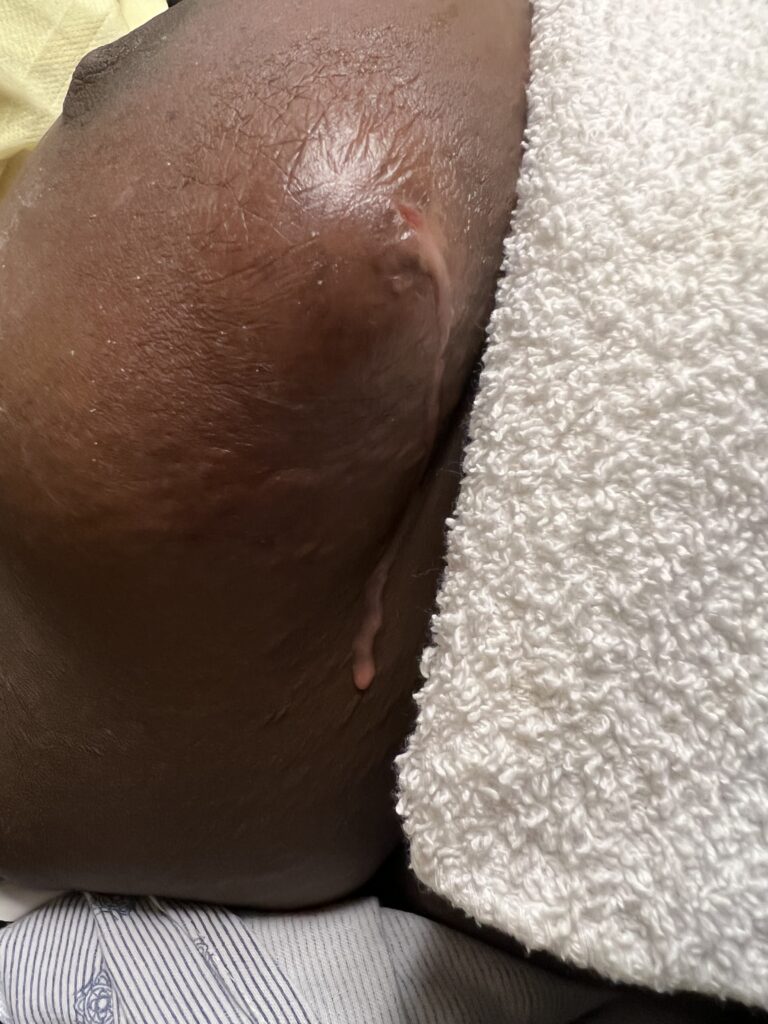
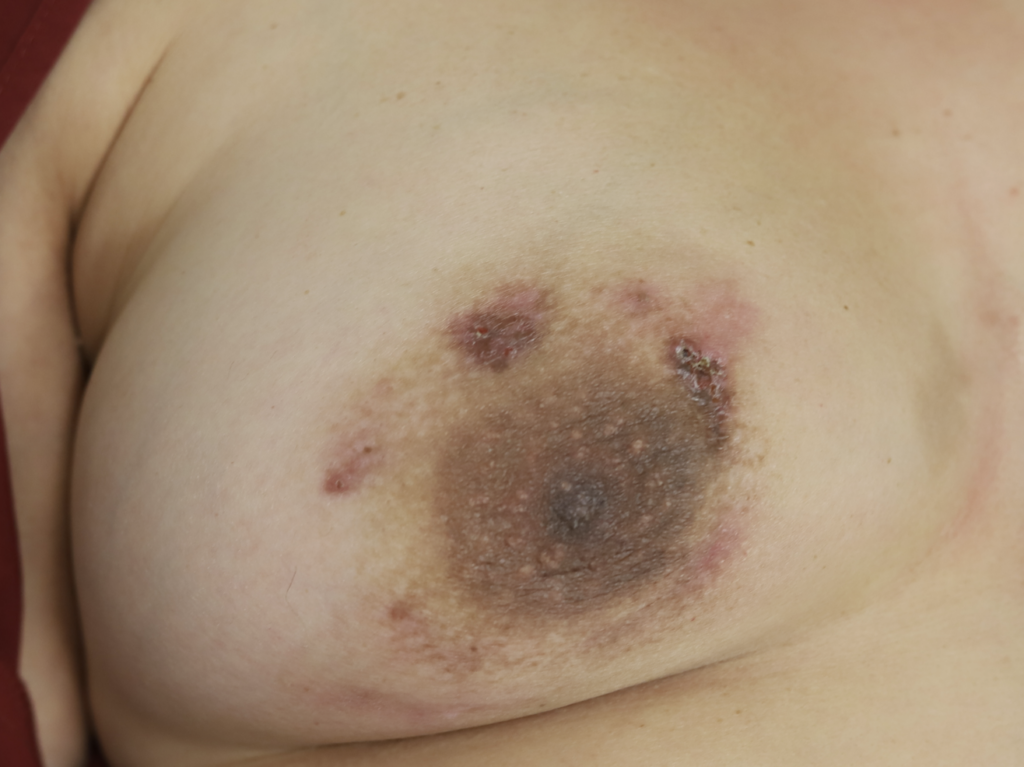
While some cases of IGM may resolve from a simple mass, many go on to form fluid collections (above and below) that may drain on their own. These are mistakingly called “abscesses.” They are in fact just fluid collections of dead inflammatory cells. Patients need either local treatment with needle drainage of the fluid (NOT large incisions with packing tape, which make inflammation worse) and steroid injection, or oral steroids/anti-inflammatories/immune suppressants.