For surgery involving breast cancer, see Breast Cancer section. For benign (non-cancerous) conditions, a patient may have undergone a needle biopsy by radiology and subsequent surgical removal of the lesion. Breastfeeding is safe and possible after a history of either of these procedures, and I also discuss this in a collaborative post with Babycenter.com.
Though theoretical risk of damage to nerves and/or underlying breast tissue is possible, this is uncommon in the setting of small incisions and minimal tissue removal. The most challenging situation for breastfeeding may occur in the setting of a large incision around the areola, or complete excision of the ducts behind the nipple. However, recanalization (regrowth of tissue) has been demonstrated in animal models. Patients should have a careful discussion with their surgeon prior to undergoing an elective operation.
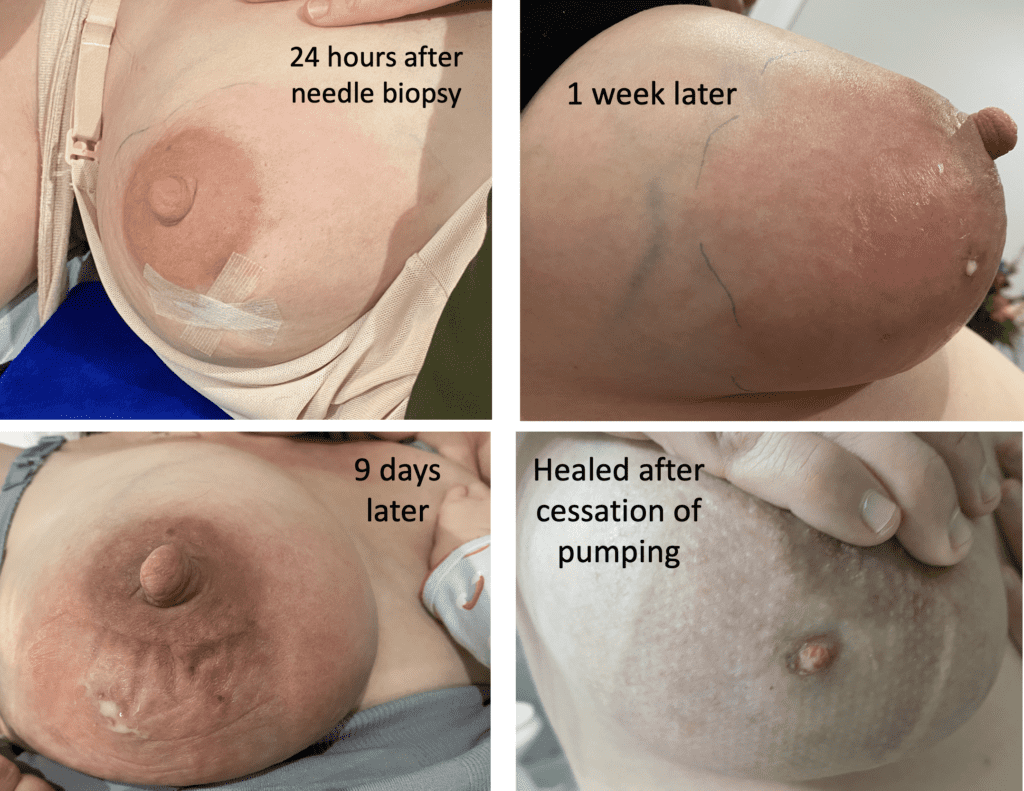
 Unfortunately, this patient did have her retroareolar ducts severed with a juvenile fibroadenoma procedure prior to lactation. There’s no way around needing to remove a juvenile FA, but anytime dissection can be performed extremely carefully in the retroareolar region, it’s most ideal. She was exclusively breastfeeding from her right breast after the left breast became engorged postpartum but zero drops of milk ever came out. This is also a great example of how redness doesn’t always = infection. Her right breast is engorged and upregulated, and the redness around her areola is simply a lot of congested blood flow prior to nursing.
Unfortunately, this patient did have her retroareolar ducts severed with a juvenile fibroadenoma procedure prior to lactation. There’s no way around needing to remove a juvenile FA, but anytime dissection can be performed extremely carefully in the retroareolar region, it’s most ideal. She was exclusively breastfeeding from her right breast after the left breast became engorged postpartum but zero drops of milk ever came out. This is also a great example of how redness doesn’t always = infection. Her right breast is engorged and upregulated, and the redness around her areola is simply a lot of congested blood flow prior to nursing.If a benign lesion (for example, fibroadenoma) is recommended to undergo removal during lactation, this is also safe and breastfeeding can continue uninterrupted with low risk of milk fistula.
However, it is very important to manage lactation physiology appropriately. This means feeding the baby normally at the breast, not pumping to “keep the breast empty” (which can stimulate hyperlactation, or oversupply, and predispose a mom to complications from that). Surgical incisions also should be placed away from the nipple and areola so the infant’s latch or pump does not traumatize the wound.
If a patient has to undergo removal of a very large lesion, it is likely favorable to reduce production on the affected breast and increase production on the unaffected breast. This will just reduce the risk of complications like fluid collections or wound opening post-operatively.
The video below demonstrates removal of a phyllodes lesion during lactation. There are several things to learn from this video:
- Breast imaging, breast biopsy, and breast surgery are safe during pregnancy and lactation. In fact, it would have been more ideal to remove this mass during pregnancy (before it grew and to rule out anything worrisome like a malignant phyllodes tumor). It also is far easier to operate without complication on a pregnant, rather than lactating, breast.
- In retrospect, this patient would have benefitted from a drain post-operatively rather than repeated aspirations.
- Breastmilk is under autocrine (local – i.e. the breasts function independently) control after two weeks postpartum (the first two weeks are endocrine, or central control). This means you can upregulate and downregulate the breasts independently.
- It is very important to treat hyperlactation (overproduction of breastmilk) in general, as well is when it is present when a patient requires surgery.

