What are the symptoms of mastitis?
Mastitis is a painful inflammation of the breast that affects breastfeeding women. Symptoms can include pain, swelling, and redness in the affected breast. Mothers may also experience fever, chills, and general discomfort.
What causes mastitis?
“Mastitis” (the vast majority of the time inflammatory rather than infectious) is often caused by hyperlactation (oversupply) and/or transient engorgement of a region of breast tissue. Full “milk sacs” (i.e. alveolar cells) can be painful and lumpy. In addition, a lot of blood flow in the area makes the area red and swollen.
It is a myth that infection can develop suddenly after a day of skipped pumping at work or after a baby sleeps through the night. When these situations occur, moms experience transient engorgement, breast swelling, breast pain, and redness for the reasons described above. This is NOT a rapid-onset, life-threatening infection.
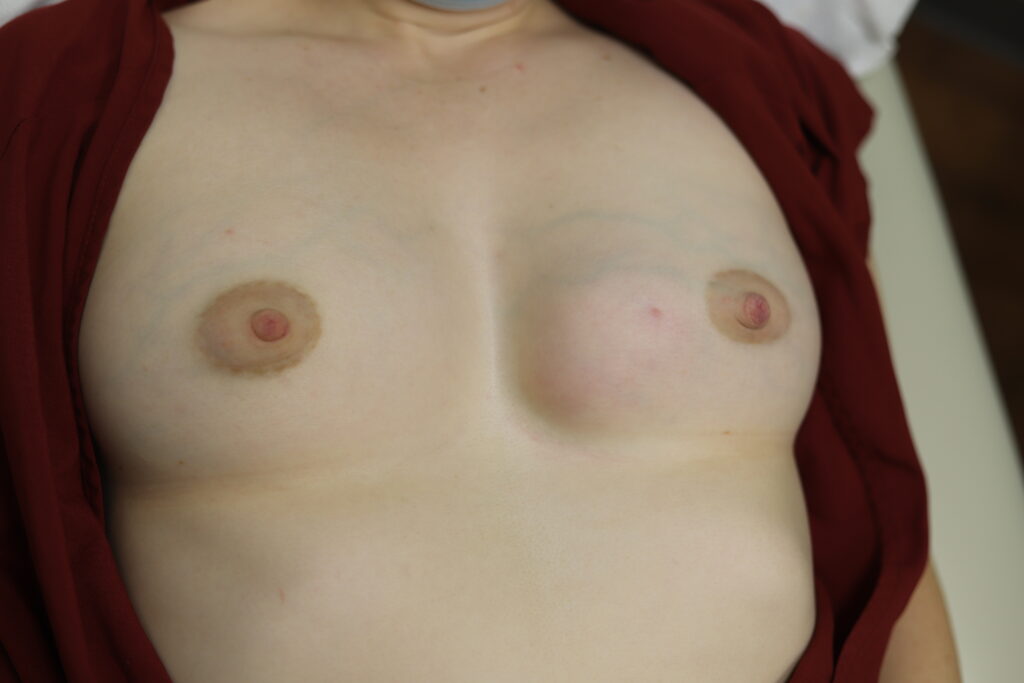
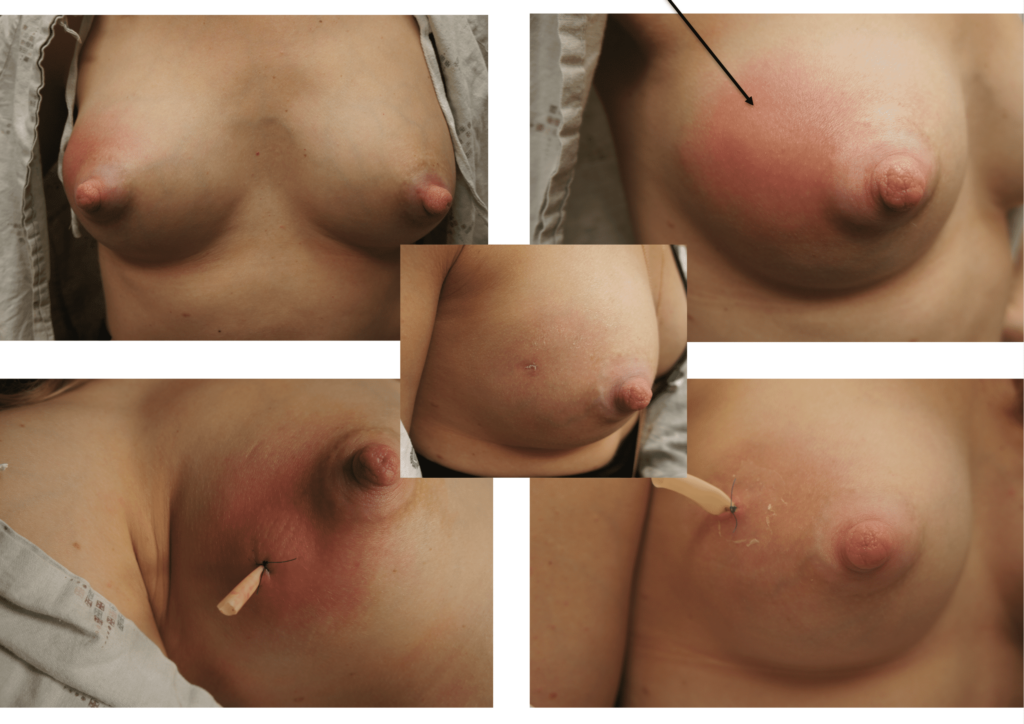
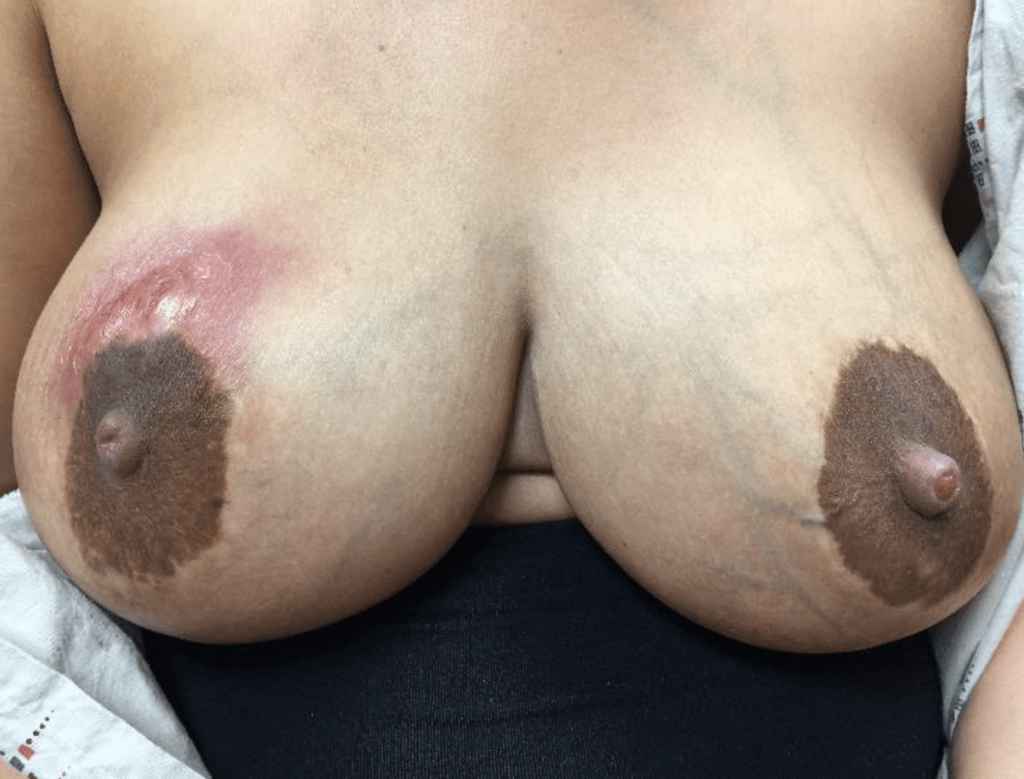
 This patient started to massage the area in the outer part of the breast and quickly developed more redness and systemic symptoms. Instead of prescribing antibiotics over the phone, I saw the patient in person. She resolved with ice and over-the-counter pain medication and anti-inflammatories (below):
This patient started to massage the area in the outer part of the breast and quickly developed more redness and systemic symptoms. Instead of prescribing antibiotics over the phone, I saw the patient in person. She resolved with ice and over-the-counter pain medication and anti-inflammatories (below):
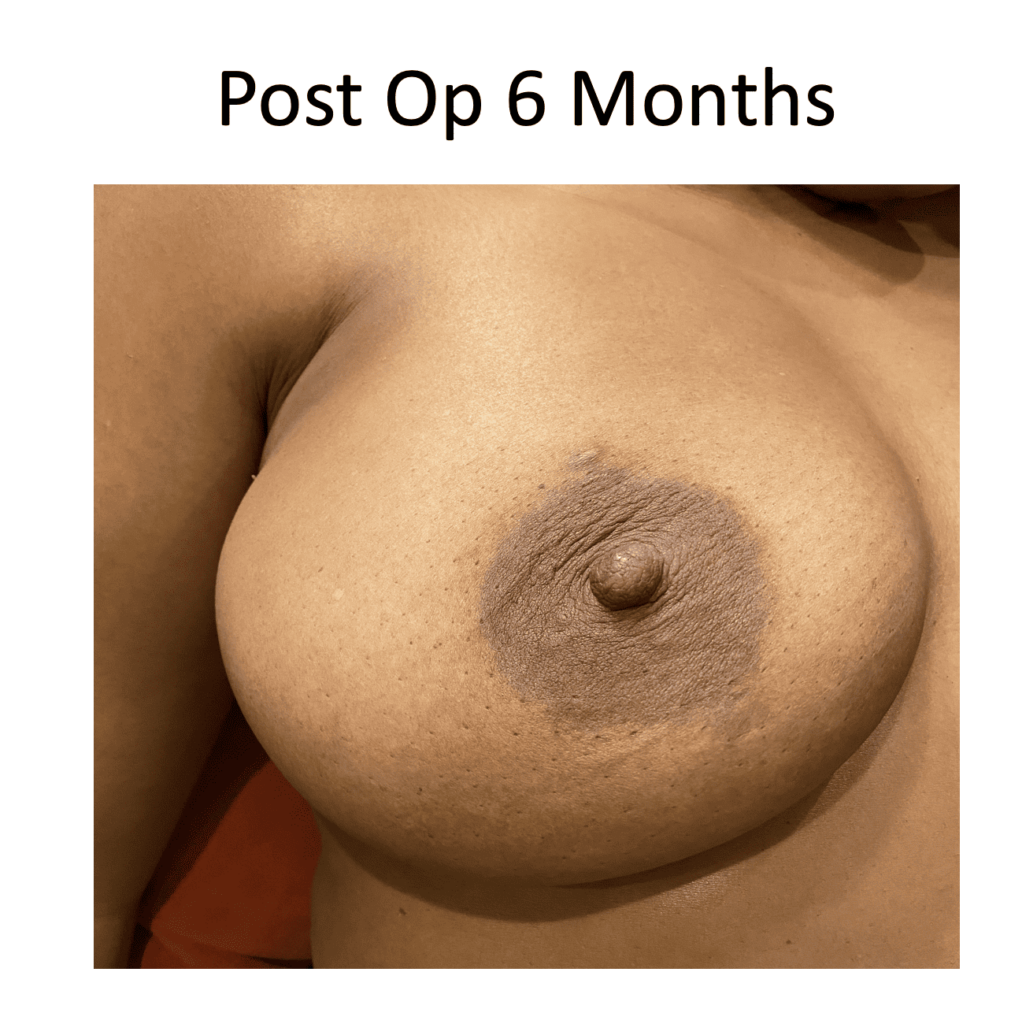
 She had faint residual redness (tissue/blood vessel damage) at the original site of massage but otherwise was asymptomatic.
She had faint residual redness (tissue/blood vessel damage) at the original site of massage but otherwise was asymptomatic.
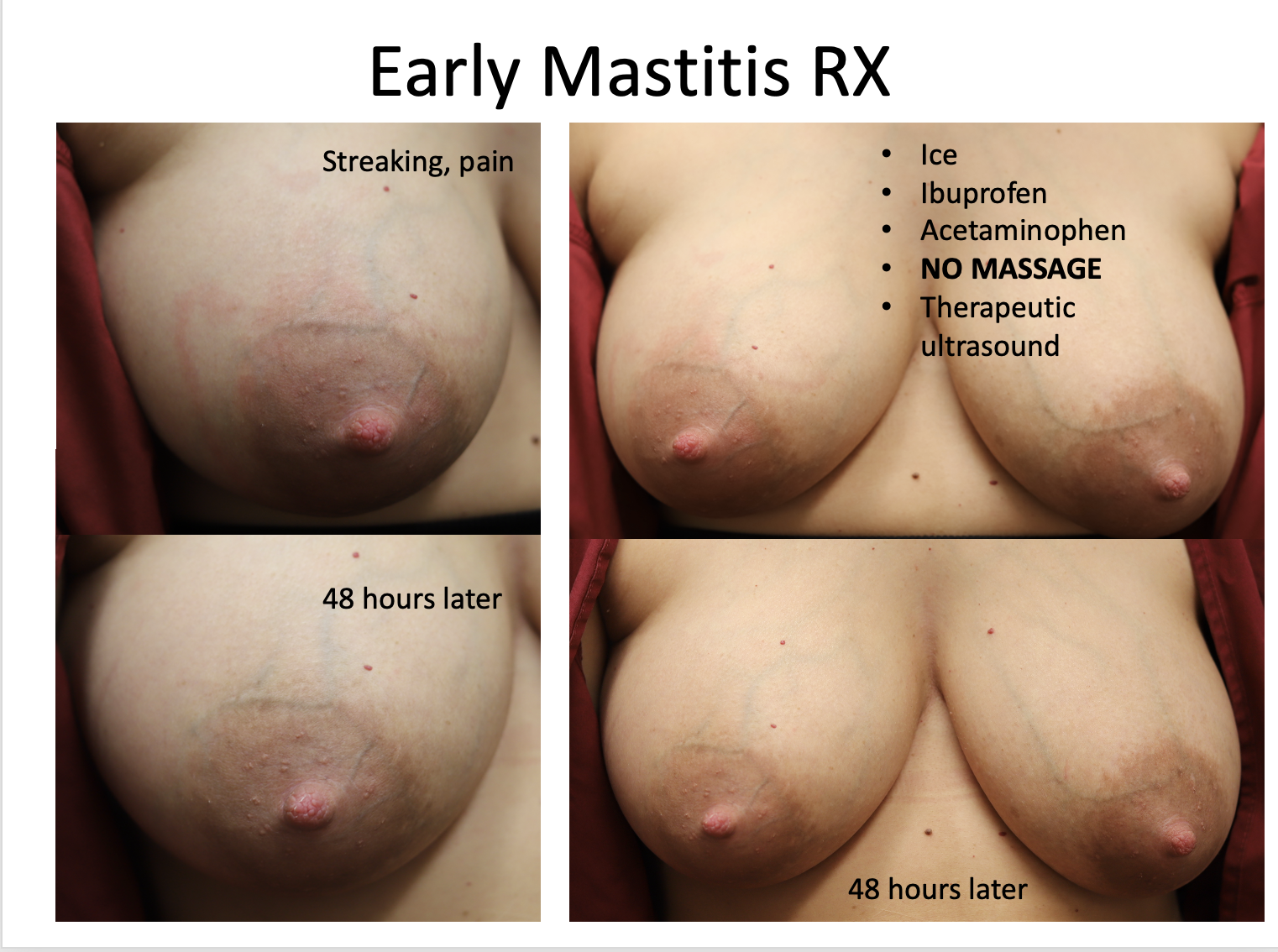
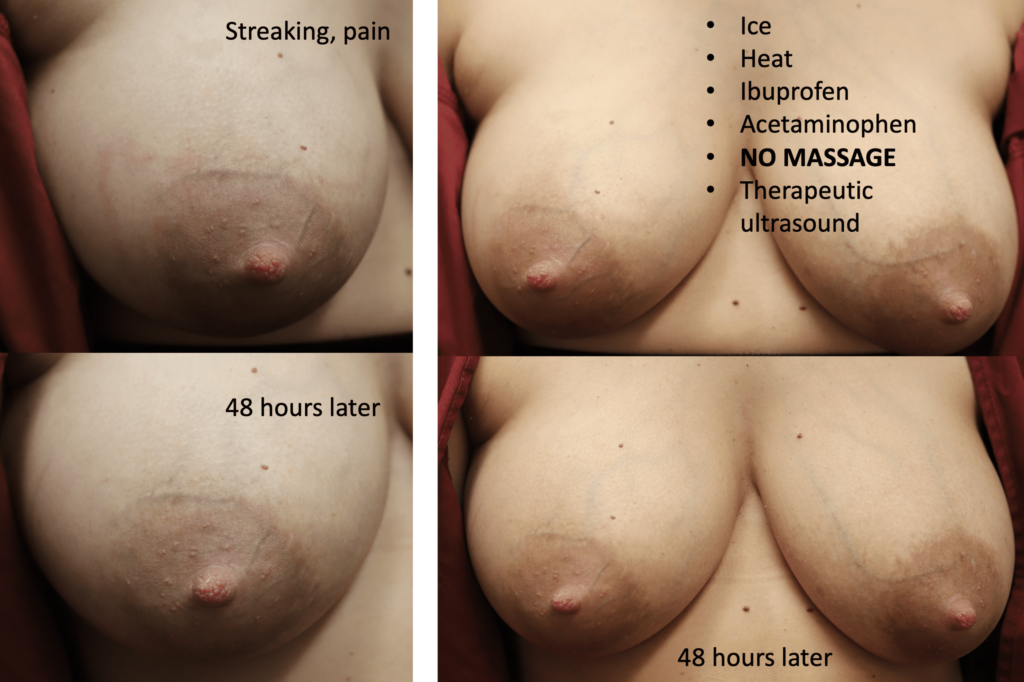
This is another patient who experienced the classic streaking (congested lymphatics) and resolved with ice. She also remarked that how painful it would have been to massage this if she were instructed to do that! It’s really the common sense of patients who are going to drive the change in care more than anything.


Complete resolution in 72 hours as shown below:
 Mastitis resolved.
Mastitis resolved.

 Blood flow, not infection.
Blood flow, not infection.
 Resolved with ice and time (72 hours). No massage, no heat. And NO antibiotics.
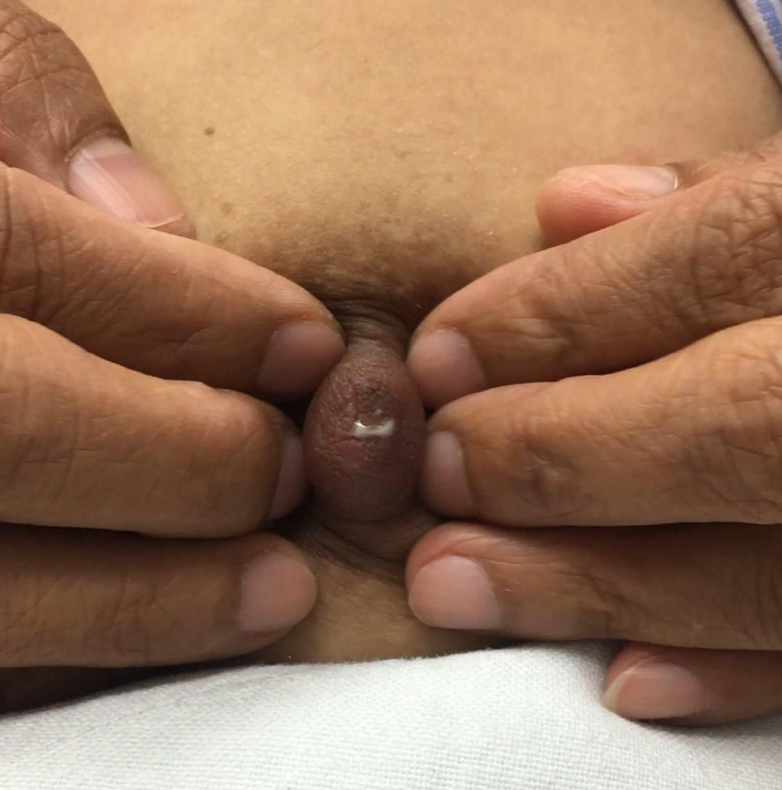
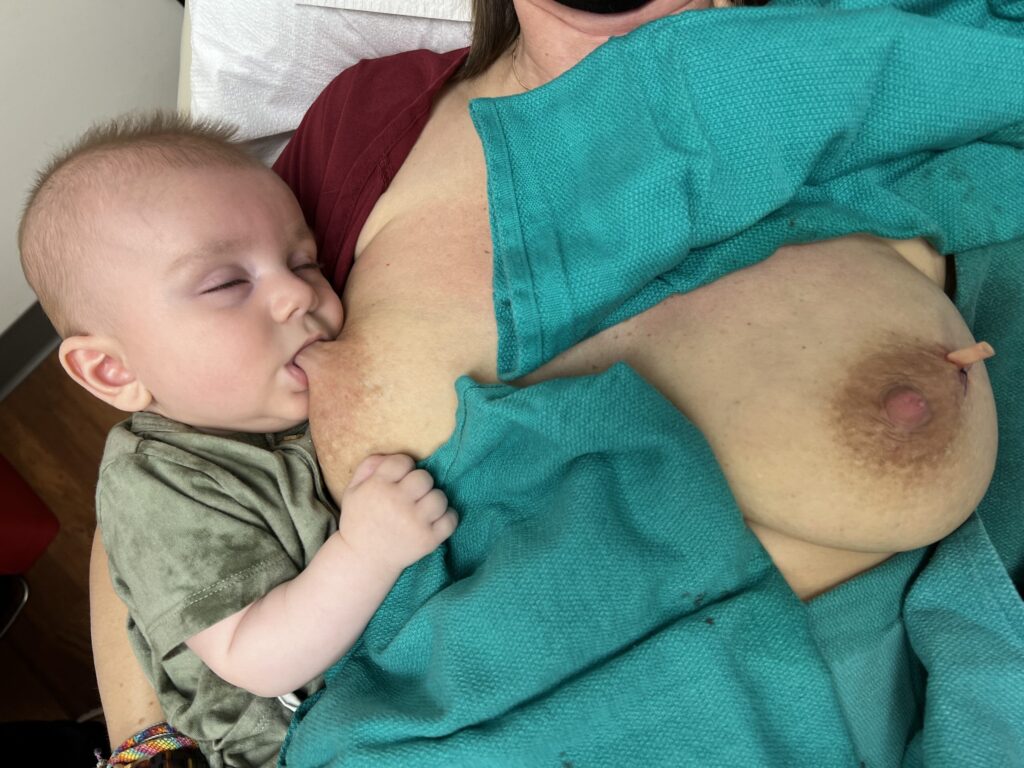
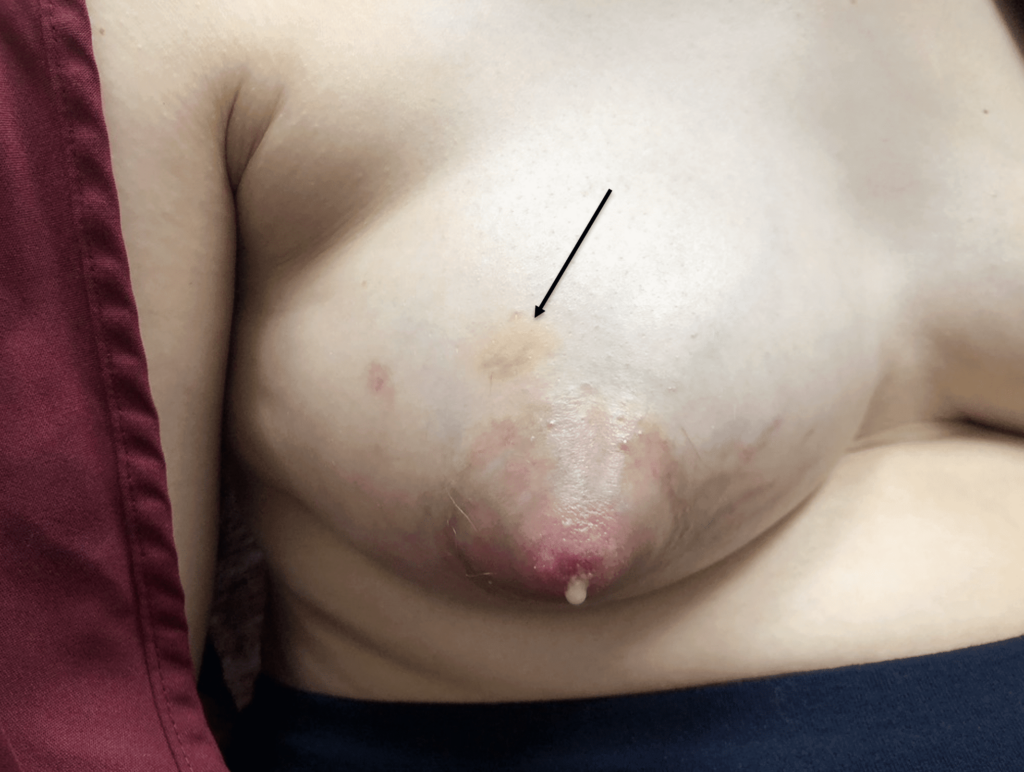
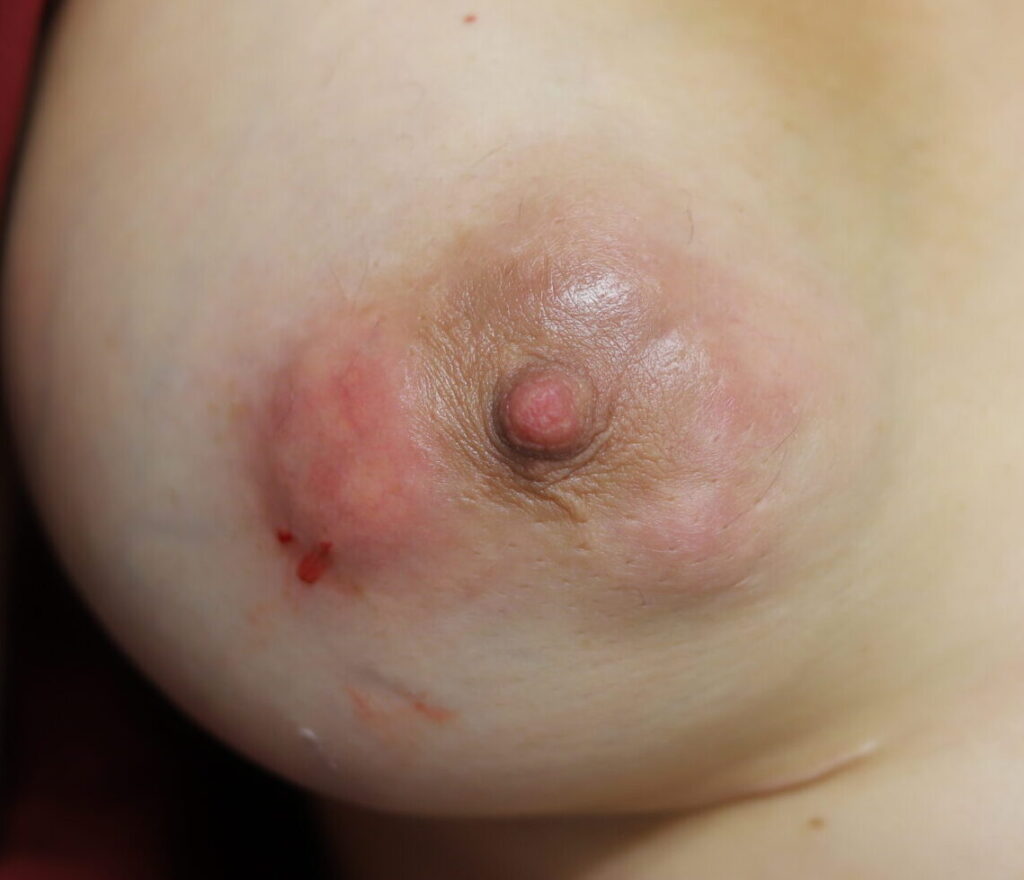
Resolved with ice and time (72 hours). No massage, no heat. And NO antibiotics.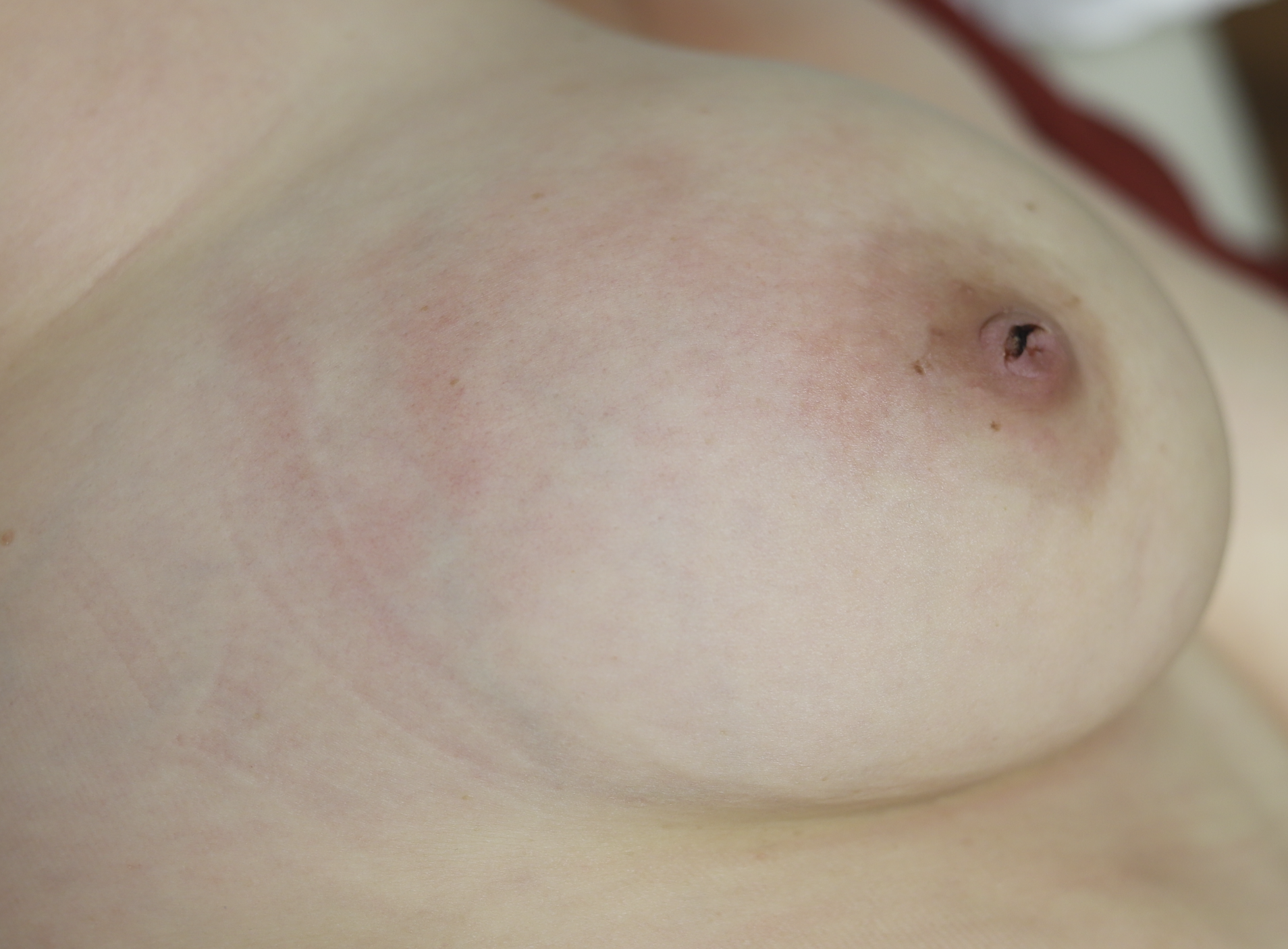 Early mastitis in the setting of a bleeding bleb.
Early mastitis in the setting of a bleeding bleb.  Mastitis resolved two days later with ice and therapeutic ultrasound. Bleb starting to improve with oral lecithin and steroid cream to bleb itself.
Mastitis resolved two days later with ice and therapeutic ultrasound. Bleb starting to improve with oral lecithin and steroid cream to bleb itself. Bleb fully resolved at two weeks and no recurrence of mastitis.
Bleb fully resolved at two weeks and no recurrence of mastitis.

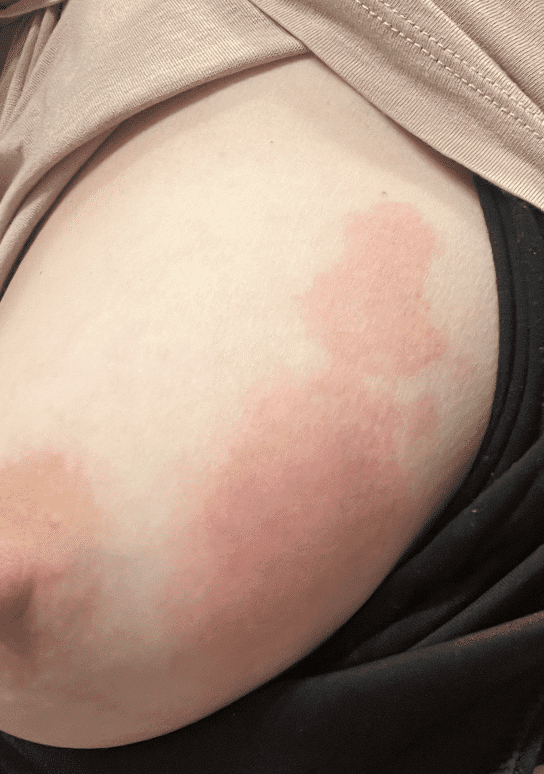
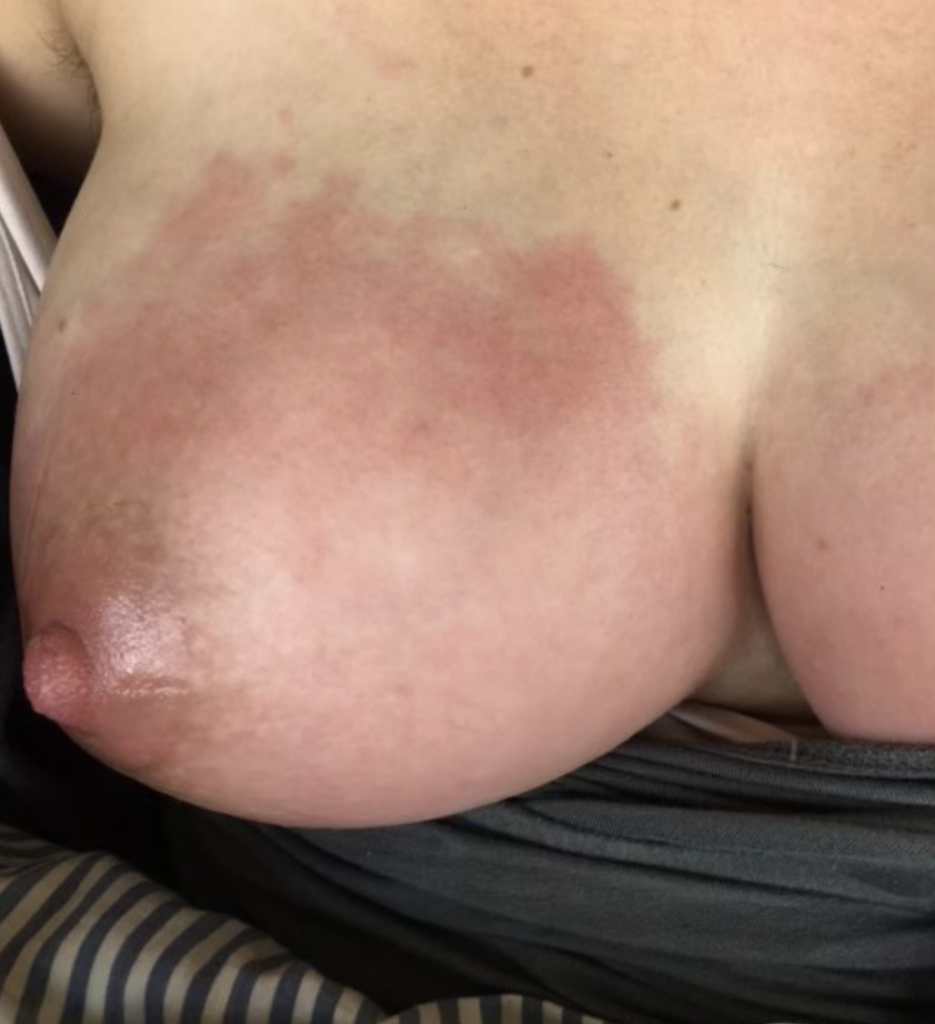
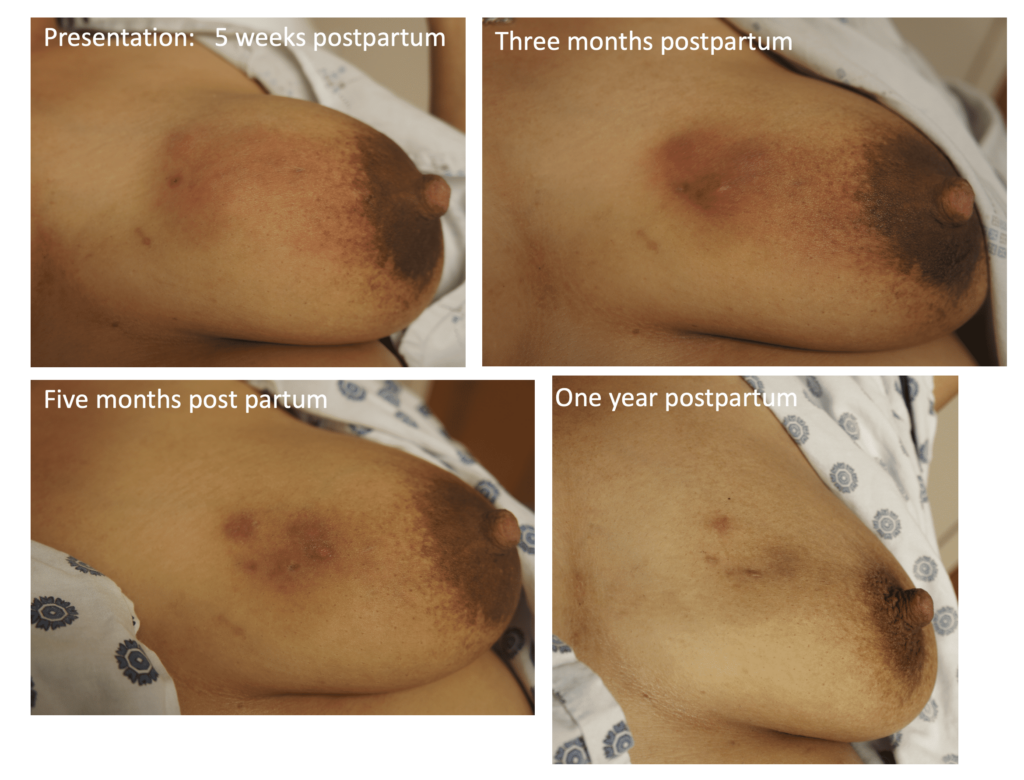
 Mastitis at presentation; patient was asymptomatic aside from the redness and pain.
Mastitis at presentation; patient was asymptomatic aside from the redness and pain.
 Mastitis at presentation.
Mastitis at presentation.
 One day after therapeutic ultrasound and ice: central area of breast starting to demonstrate less erythema.
One day after therapeutic ultrasound and ice: central area of breast starting to demonstrate less erythema. Resolved day four with ice and therapeutic ultrasound alone, no antibiotics.
Resolved day four with ice and therapeutic ultrasound alone, no antibiotics. The patient remained resolved at one week follow up. Note the slight erythema of skin upper quadrant is related to skin itching with her recovery and is not a cause for concern.
The patient remained resolved at one week follow up. Note the slight erythema of skin upper quadrant is related to skin itching with her recovery and is not a cause for concern.Risk factors for mastitis
As a breastfeeding mom, you may be more susceptible to developing mastitis if …
- You have hyperlactation (oversupply)
- You have been told to …
- “Pump to keep your breast empty” or otherwise told to feed more on a breast that feels full
- Massage
- Heat your breast
- Wrap your breast in castor oil and do other things such as shake your breast or do “breast gymnastics”
- Use a haaka device on your breast to “release a plug”
- Any other advice that hurts, feels counterintuitive, and isn’t working!
The above represents misconceptions breast anatomy and function over decades of lactation care. We in breastfeeding medicine leadership are attempting to change this, beginning with the ABM mastitis protocol 2022 and its accompanying mastitis treatment handout.
As an analogy, think of your breast like a delicate group of grapes or raspberries or fish eggs or anything else that would be harmed by mashing and heating (literally turning any of these substances into soup) …

Another example is illustrated here by graphic designer Mitch Rosefelt. The alveolar cells are like fluffy, delicate dandelions surrounded by innumerable microscopic ducts:

What’s encouraging is that it’s often patients themselves who recognize that traditional advice didn’t make things better. Incredibly lovely patient Tori Tso of Austin, TX details her story in Naiomi Catron RNC-OB, IBCLC’s wonderful Boob Business podcast (episode 21).
Another patient from a different state emailed me through my website, and shared her experience as well:
What to do if you have symptoms of mastitis
If you suspect you could have mastitis, it is incredibly important to not try to “empty” your breast (treat it like a sprained ankle, using ice and anti-inflammatories and not overusing it!).
This patient was unfortunately told to pump after every feed to “empty” her breast when she started to experience mastitis symptoms. Unfortunately, that just brought more blood flow to the area, reduced the ability to drain lymphatic fluid, and told the breast to make more milk, and resulted in a huge abscess.
 Abscess worsened by pumping after every breastfeed.
Abscess worsened by pumping after every breastfeed.
We would never tell someone to “keep eating” to treat an intestinal obstruction. We know that this would worsen bowel swelling. The exact same principle applies to your breasts. If your breast is swollen, red, and painful, it’s telling you to pull back and give it a rest.
Your breast is not a cesspool of stagnant milk full of dangerous bacteria. Milk is manufactured and stored neatly in alveolar cells, NOT ducts. You don’t need to pump or overfeed to “prevent milk stasis.” This is a made-up term in lactation that has no anatomic or physiologic correlate; trying to avoid “milk stasis” unfortunately results in many complications.
Why is ice so important?

If something doesn’t get better, patients should be evaluated by a physician for an exam and imaging. Temporary issues should resolve within a few hours or day or two. If they persist or get worse, it is important to ensure they haven’t turned into a galactocele (a true milk retention cyst that may require drainage) or another mass is not present in that location. Likewise, mastitis-like symptoms that continue to worsen with ineffective treatments such as massage and pumping may progress to an abscess.
Full discussion of topics in this section is available in the ABM mastitis protocol 2022.

Engorgement

Engorgement is common in the prenatal and early postpartum periods, and may occur at other times when nursing is interrupted. Engorgement of the breast in the early postpartum period involves swelling due to increased blood vessels and fluid in the breast. It is different than mastitis and hyperlactation, which are below. However, treatment is the same:
#1 Do not pump or continuously feed baby to reduce engorgement (this sets up a vicious cycle that makes everything WORSE). If necessary, use a hand pump to remove as little volume as possible to make yourself comfortable.
#3 Support your breasts with a good bra. If you don’t want to wear a bra, that’s fine. But know that if you have lots of engorgement and/or larger breasts, swelling in the connective tissue will collect in the bottom parts of your breast if you go without a bra. This is the same as what happens if you were to sit in a car for 12 hours and not move your legs: your ankles would swell.
If you wear a supportive bra, you will help your breast more naturally drain this fluid and it will improve pain and redness.
It a SERIOUS myth that bras cause mastitis, and it has resulted in so many women suffering from back pain, chest pain, and lymphedema (swelling in the lower portions of the breast). #Takebackthebras! Even small breasted women can develop lymphedema.
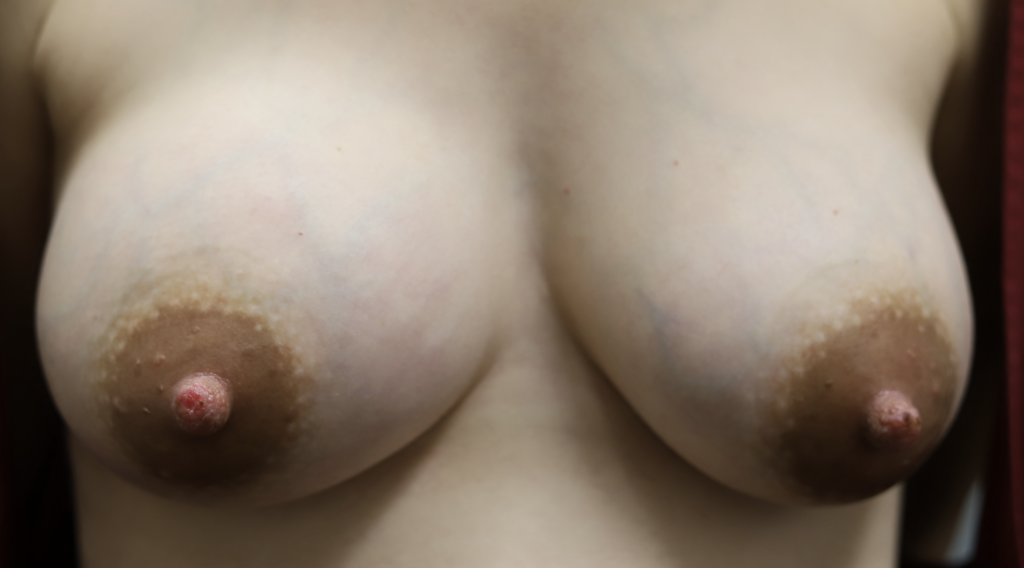
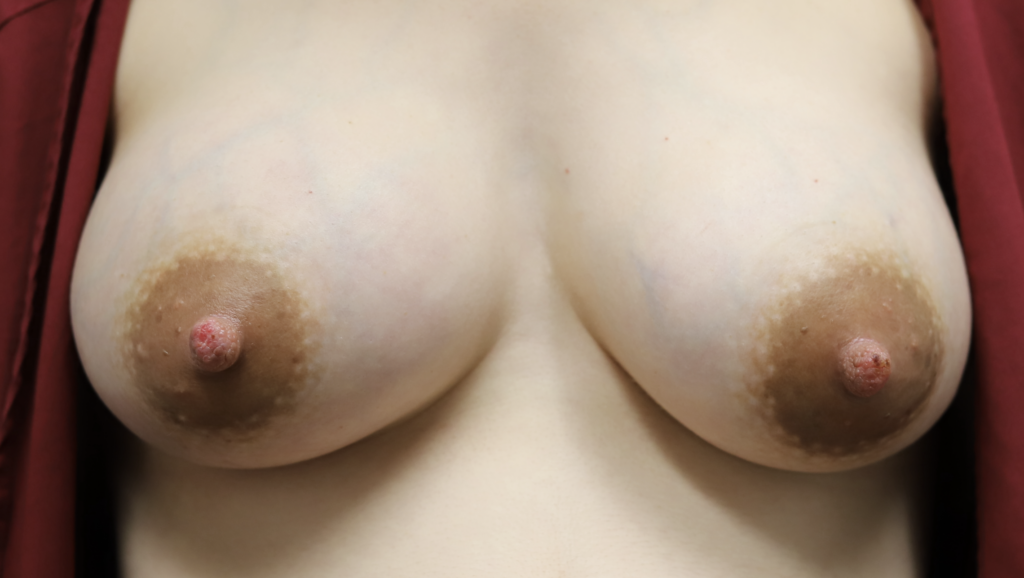
Right breast engorgement (day 5) with streaking right breast inner aspect (connective tissue fluid, NOT infection) and improvement day 7 (right).
Note that this patient also had nipple injury on both breasts from her engorgement. This is a great example of why people believe that “nipple wounds cause mastitis.” Nipple wounds are an ASSOCIATION, NOT CAUSE AND EFFECT.
I.e. women that have nipple wounds are more likely have engorgement and hyperlactation (oversupply), “streaking redness,” pain, and inflammatory symptoms such as fever and flu-like feeling (completely non-specific symptoms — not automatically infection!). So people incorrectly make the jump that the nipple wound “caused” mastitis.
As is clear with this patient, if you feed more off of the less full breast (in her case, the left), you let the engorged/hyperlactation breast calm down by leaving it more full (i.e. it gets the message that the milk isn’t needed). This patient also knew to not massage or pump her breast, and recognized the pain and “streaking” was just fluid in connective tissue space and not infection!
Below are more photos of early postpartum engorgement.
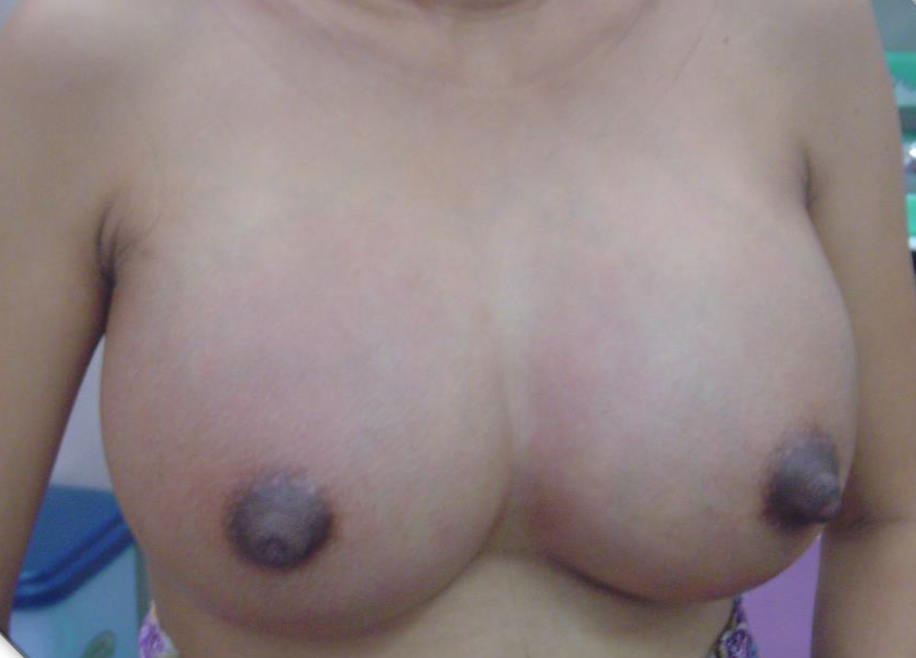
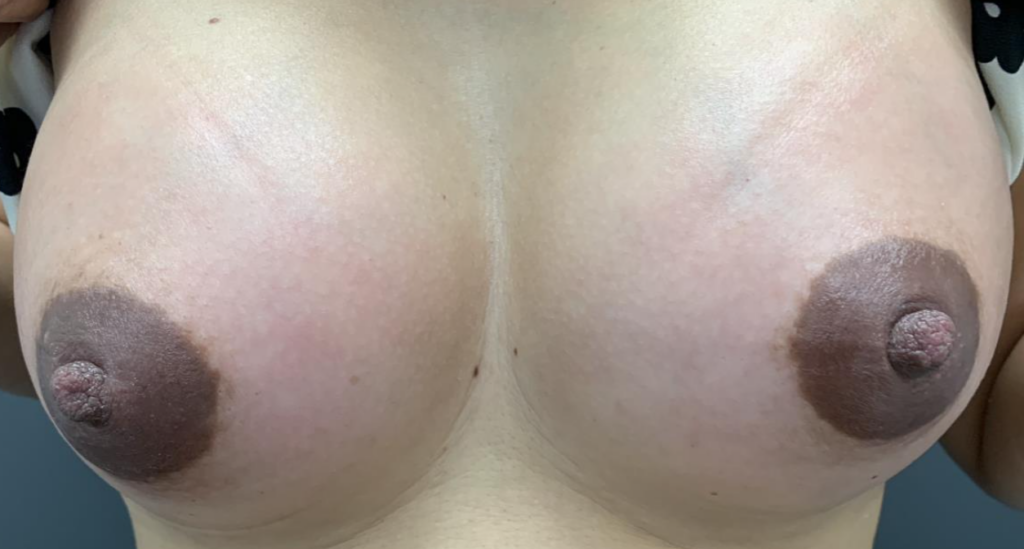
Engorgement generally peaks on postpartum day five, so know that it is a time-limited issue in terms of any extreme symptoms.
Other options for relief:
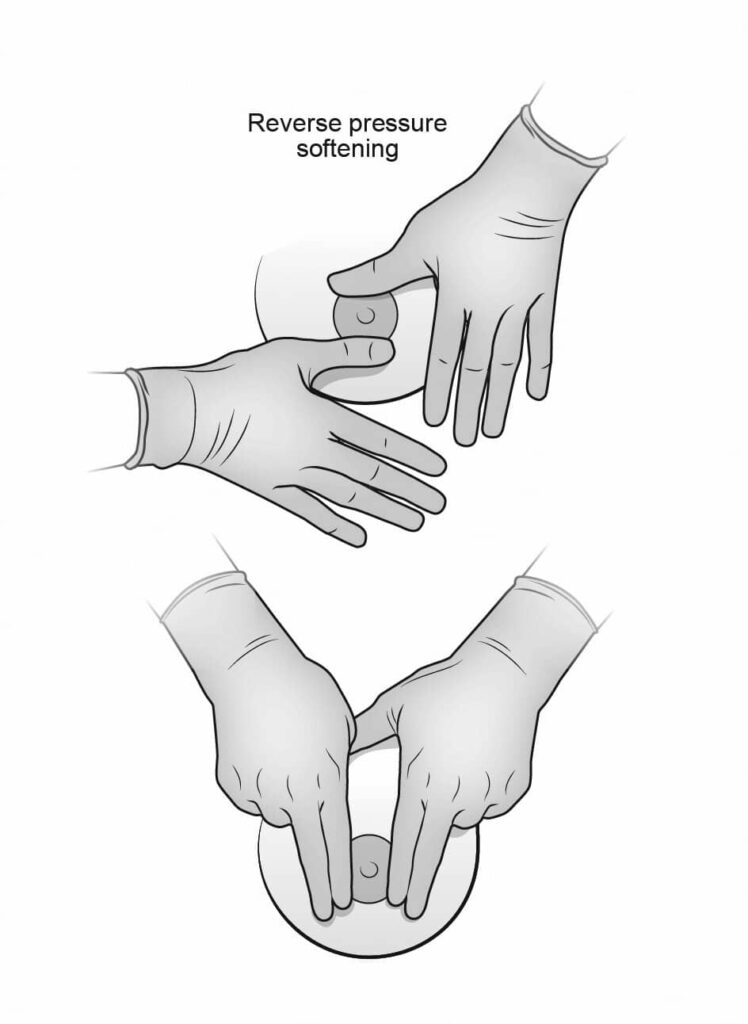
#1: Reverse Pressure Softening (RPS), which reduces swelling in the areola and nipple, can help an infant latch more easily to an engorged breast.
#2: Side lying nursing can help a LOT.
#3: Individual success with acupuncture has been reported
#4: Therapeutic ultrasound can relieve pain
#5: Pseudoephedrine (Sudafed) acts as a vasoconstricting agent (i.e. decreases blood flow) and can be useful for very severe engorgement. Cabergoline (a prescription medication that blocks prolactin, the milk-making hormone) can be used in situations where the mom is at risk of medical/surgical complications.
#6: Avoid breast shells (they cause swelling of the nipple) and utilize RPS and nipple balm/hydrogel pads instead.
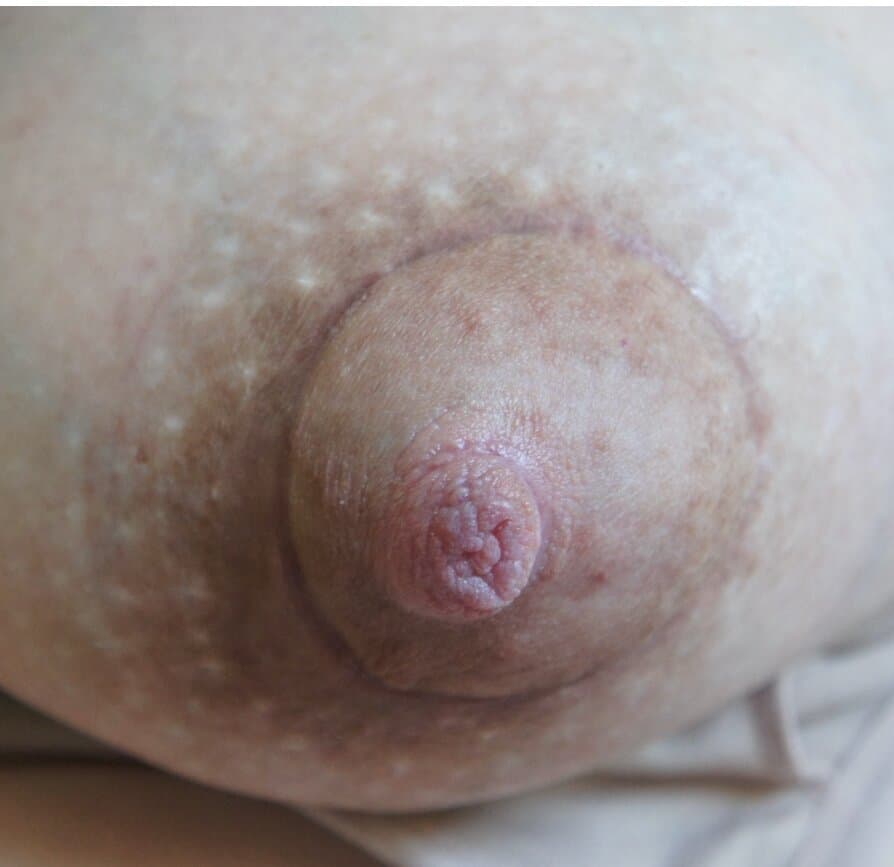
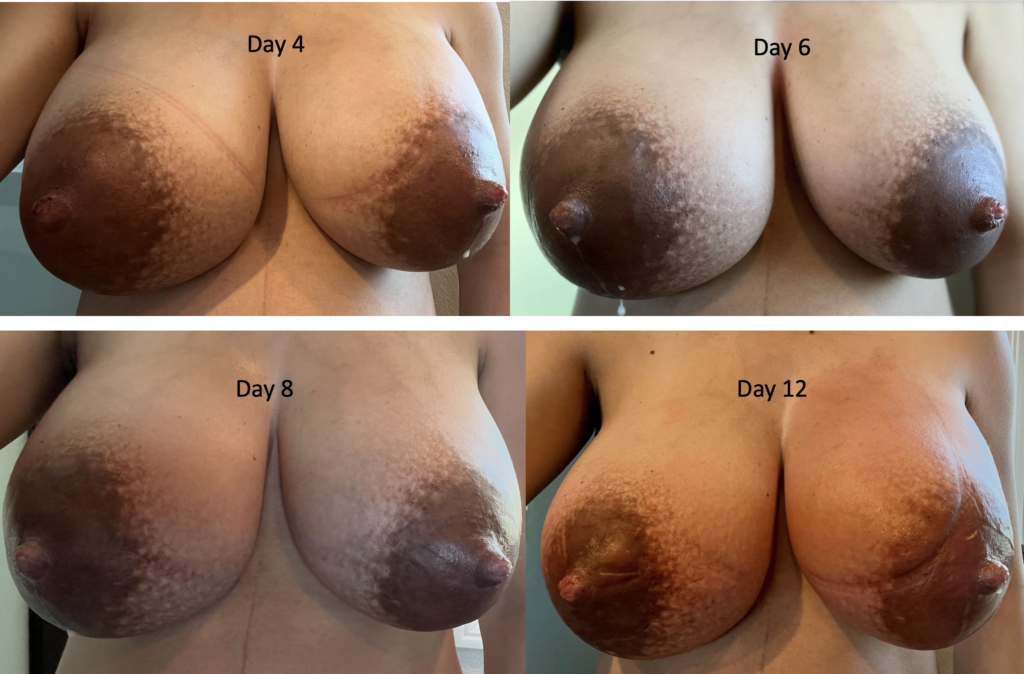
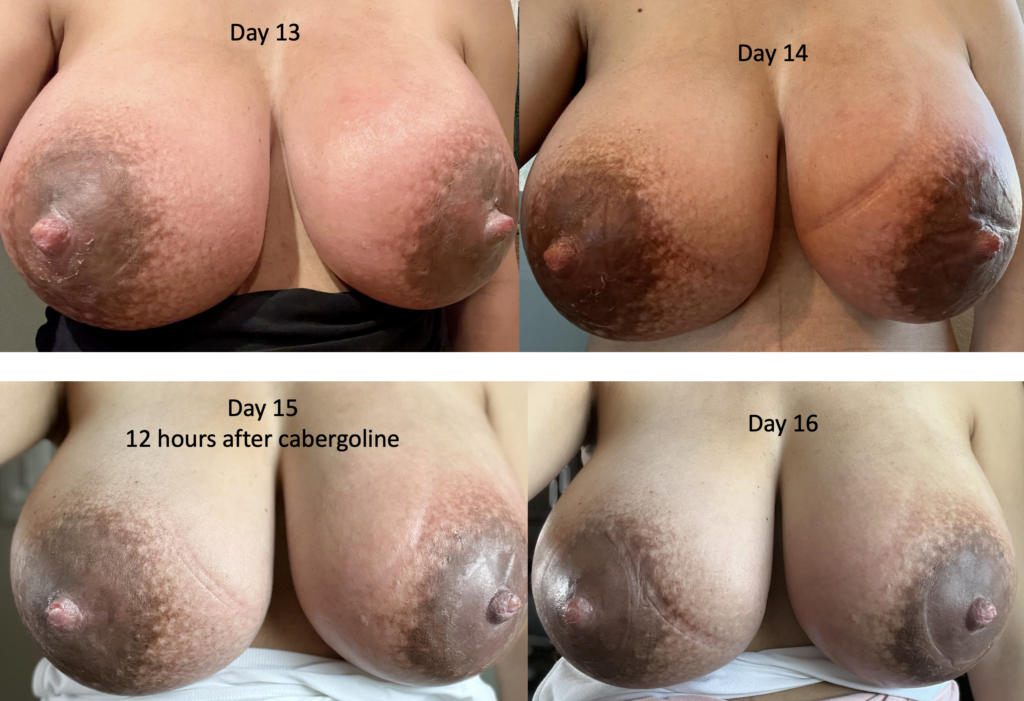
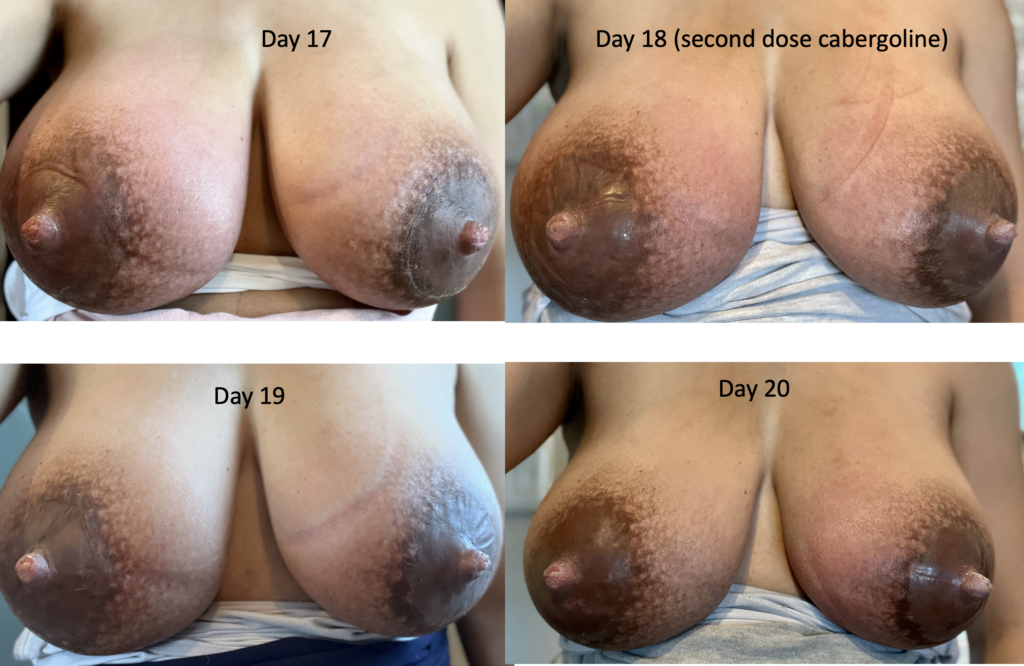
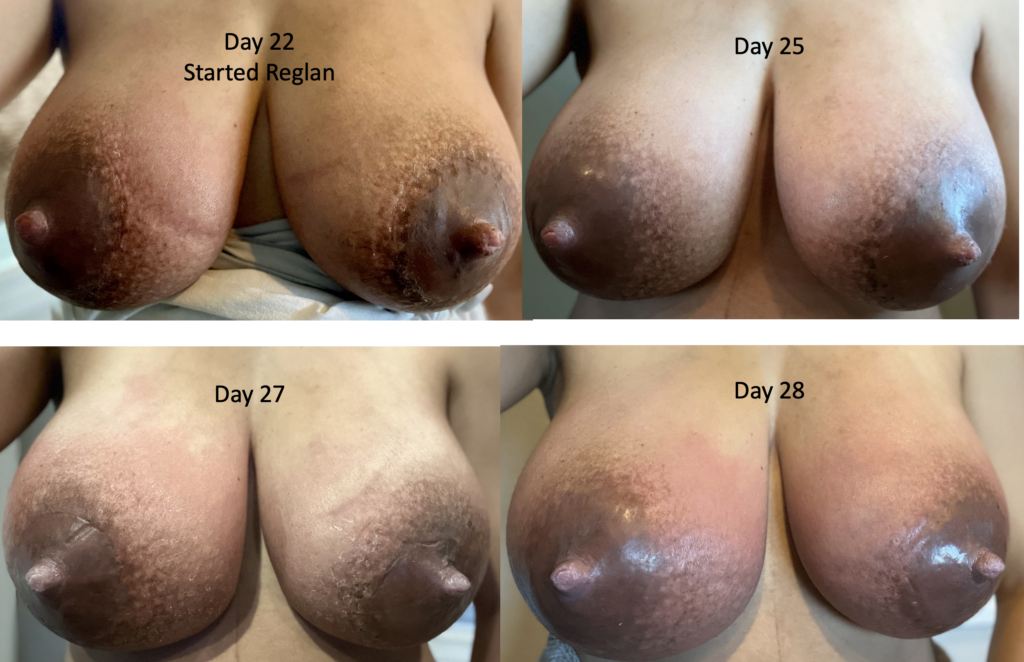
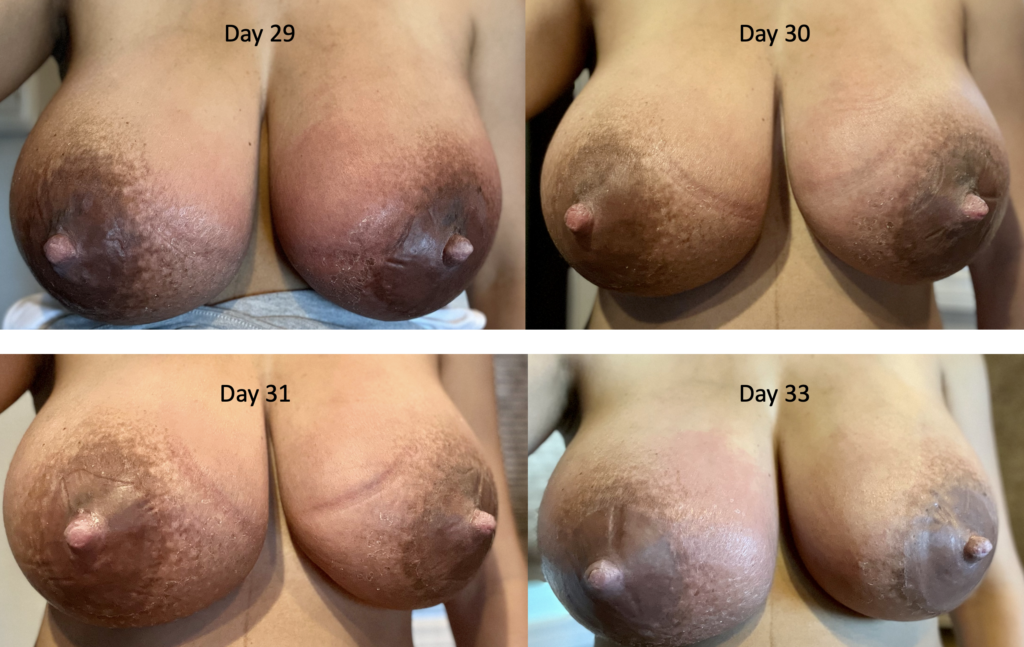
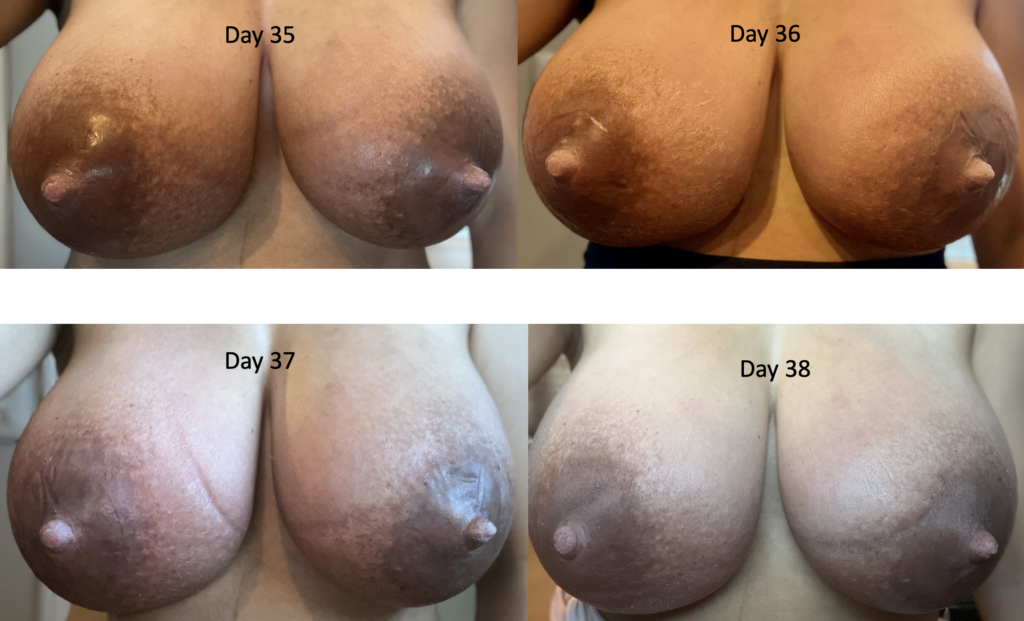
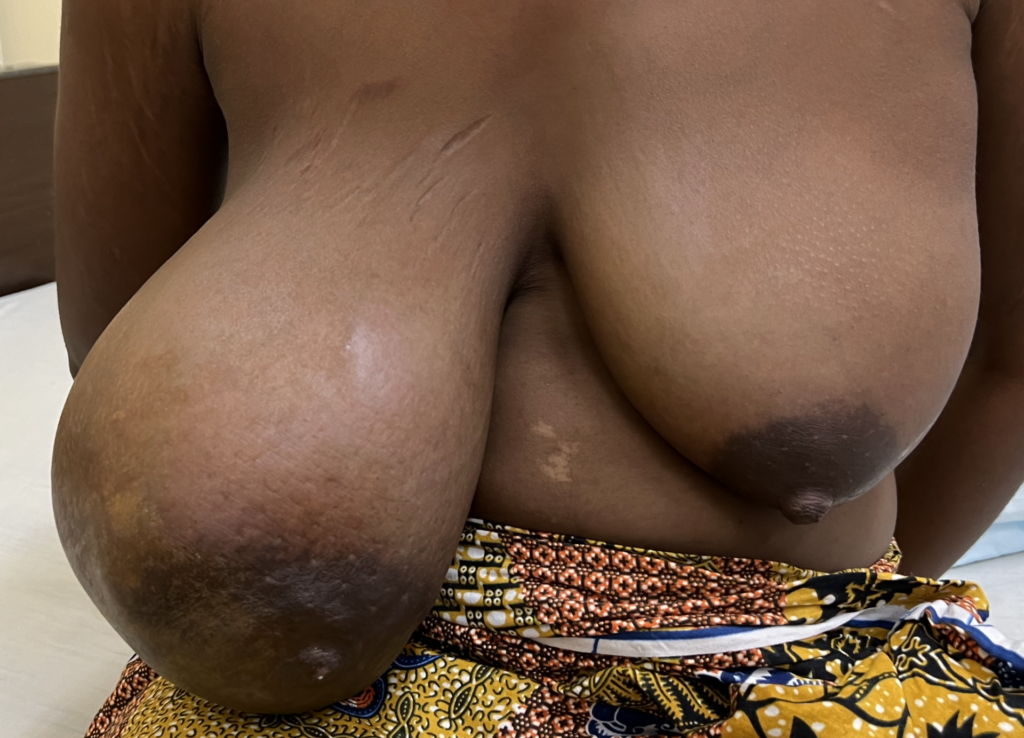
The images below demonstrate extreme postpartum engorgement that also involved hyperlactation (overproduction of milk). These are important images to understand that this is not infectious/bacterial mastitis requiring antibiotics. This is simply lots of blood flow in the breast, and lots of milk/fluid that needed to be downregulated (which took time and patience, given the severity of her symptoms).
We treated her with pain medication, a supportive bra, lymphatic drainage, and medication to reduce her production such as cabergoline and sudafed. At one point, we had to give her an agent (reglan) to increase her production again after she really decreased considerably with cabergoline.
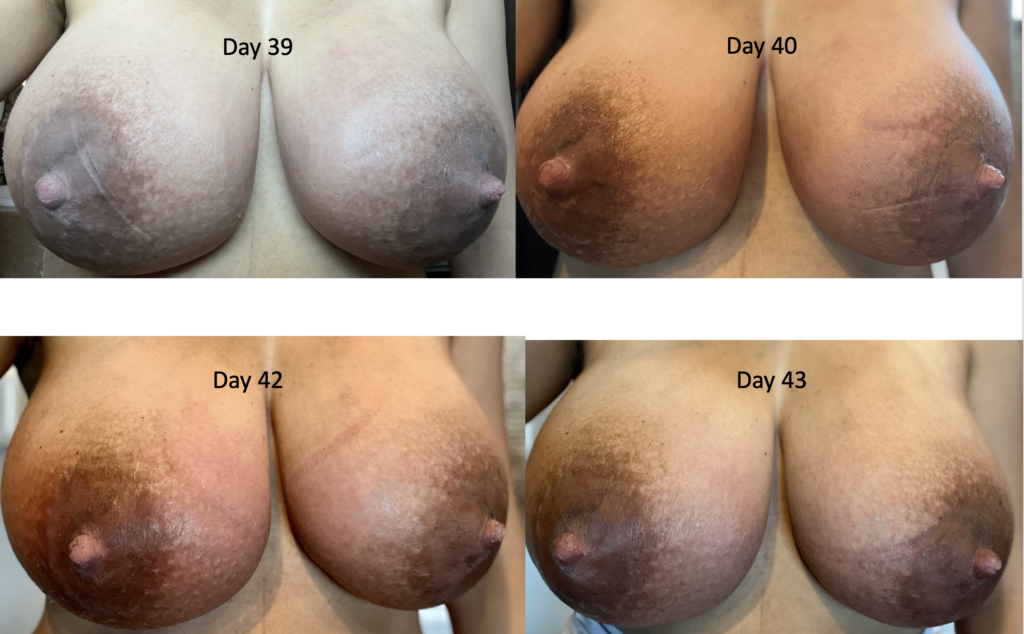
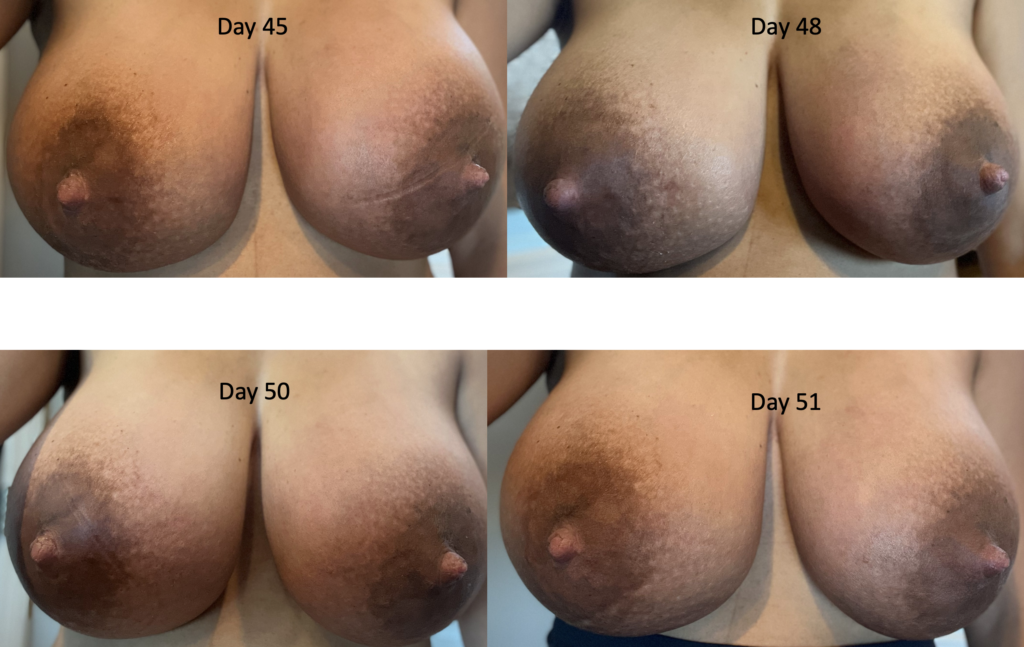
Hyperlactation or "Oversupply"
Hyperlactation may be iatrogenic (caused by interventions from medical providers or lactation consultants) or idiopathic (unknown cause).
Iatrogenic hyperlactation can be caused by early and/or excessive pumping, such as when a mom with adequate production of milk is told to pump every two hours to “empty” to prevent mastitis. She also may be told to feed the baby on both breasts for all feeds. This increases milk production and prevents Feedback Inhibitor of Lactation (FIL) from activating to reduce milk volume to a normal level.
Iatrogenic hyperlactation also may be caused by purposeful or inadvertent consumption of galactogogues (substances that increase breastmilk production).
If untreated, these things may happen:
- Moms’ breasts may be continuously painful, and they may experience frequent lumpy, red breasts, general feeling of being unwell, and nipple blebs.
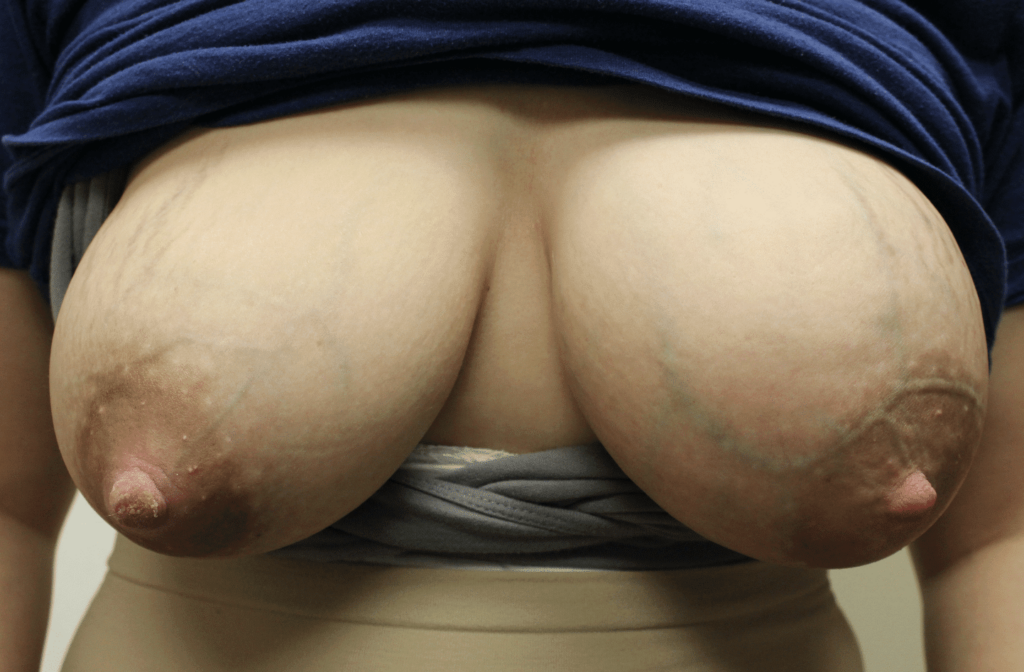
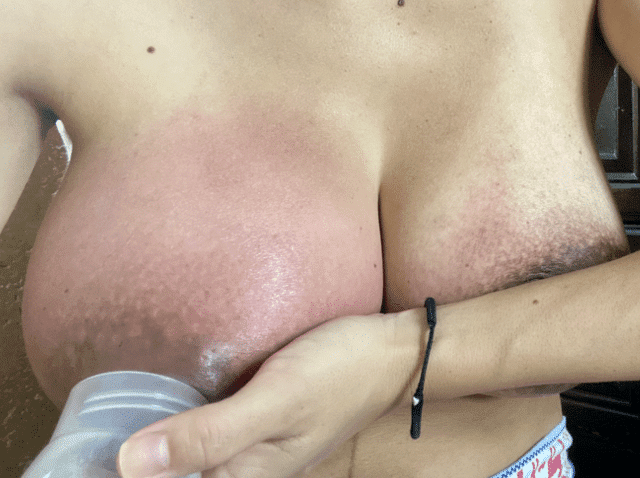
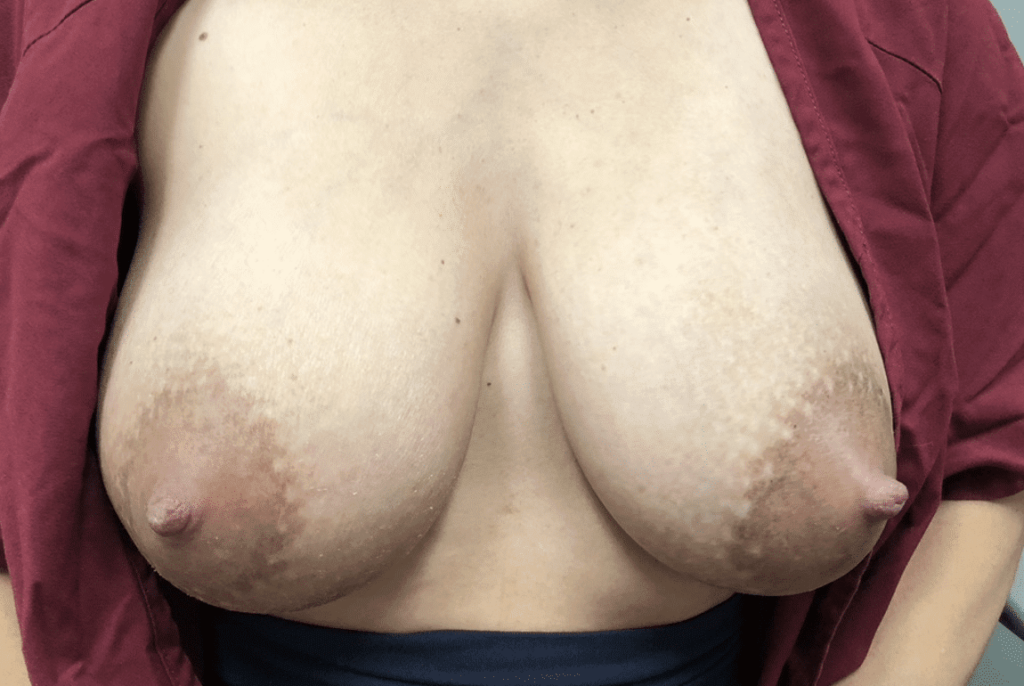
- Infants may cough, choke, and release the breast when feeding. Babies can be gassy and fussy, just like anyone who eats too much or drinks liquids too quickly. They may vomit frequently from the large volume of milk consumption; this often leads to misdiagnosis of reflux and unnecessary anti-reflux medications. Infants can develop extremely watery, “blow out diaper,” green, mucous, and even blood streaked stools and told they are allergic to something in mom’s diet. Mom is then put on a restrictive diet that is not the appropriate treatment for the problem.
This is a video of a baby feeding with pulling, grunting, and clamping against mom’s fast and heavy flow of breastmilk in hyperlactation.
You treat hyperlactation this way:
#1: Adjust your position to side lying. People are most often told to “lie back” to reduce the speed of flow of milk. Unless you are literally flat on your back with baby on top of you, this won’t work because there’s still enough gravity/vertical flow of milk getting to baby.
Lying back also is harder to do, especially if you’re positioned correctly on your back: it’s difficult to manage a floppy newborn or a heavier baby that is older. And if you’re doing laid back partially reclined, you often end up straining your shoulders and wrists to hold baby. And the bottom line is it doesn’t help enough.
#2: Stop any galactagogues, haaka use, and unnecessary pumping. I.e. the very first step is to eliminate any excessive removal of milk (more milk removed = more milk produced = vicious cycle). This will help mom’s pain, redness, and lumpiness as well as help baby.
If you are giving a baby a bottle to replace a breastfeed, pump ONLY the volume you need for that bottle (e.g. 2-3 ounces). If you leak lots of milk, collect it in a haaka WITHOUT suction (i.e. you’re not telling your body to remove more milk, you’re just catching what would be naturally landing on your nursing pad or shirt/bed).
You can SKIP pumping (get some sleep!) and use that leaked milk instead. Anytime you leave your breasts full, it will help reduce production.
#3: Recognize the situations when your chubby, gassy, spitting up, blowing-out-diapers baby is ACTUALLY hungry.
Babies that are getting flooded with milk in a short period of time, burped, and put back on a second breast can develop upset tummies very quickly. However, unlike an adult, they can’t explain to you that their tummy feels too full and they don’t want to be swaddled and put on their back (would you do this after a heavy/large meal?).
So they fuss and grunt and even get agitated/anxious with “pecking,” “rooting,” “chewing on their hands,” and crying to be picked up. And parents think this is hunger. But it’s really that the baby simply needs comfort/soothing/being held/bounced.
If your baby is gaining tons of weight and is behaving this way, you can assume the baby is NOT hungry 20-30 minutes or an hour after the last feed.
#4: Break the vicious cycle of overfeeding. This means letting a baby feed for 5-10 minutes max (this is not an exact number, but a general idea) when the baby is swallowing/gulping like crazy. The baby will take in a large amount of volume in a short period of time.
If the baby pulls off a few minutes into the feed after massive gulping, do NOT put the baby back on the breast or burp the baby. Let the baby stay relaxed (burping will just stimulate them and start the cycle over again). Give the baby a pacifier, bounce the baby on a yoga ball, wear the baby in a wrap continuously (doesn’t have to be mom – can be anyone). The holding/wearing part is essential for breaking the cycle feeding a baby when he just wants to be next to a warm human body.
If a baby pulls off and chokes/gasps with the heavy letdown, that may mean he just needs a break at the beginning of the feed. It’s different from the above situation. In either instance, however, do not repeatedly force a crying or fussing baby to relatch or stay latched.
It’s also not a good idea to start into overthinking/overmanaging a feed. E.g. people may be told to latch the baby AFTER the letdown. This usually ends up stressful in terms of trying to time that, making a hungry baby wait, etc. It’s far more natural for you/baby to let baby latch and pull off on own if he needs a break with letdown.
People also may be told to pump off some volume before latching baby. Not only does this add stress/overmanagement to feeding, but it removes more milk and tells your body to stay in overdrive.
If your breast is literally rock hard and you need to hand express or HAND pump (non-electric) to soften your nipple/areola, remove the smallest volume possible (electric pump can often remove too much too fast). If your baby can latch despite the firmness of an engorged breast, then let baby do the work instead.
#5: As part of not overfeeding, use one breast only per feed. If this is not enough to reduce your/baby discomfort, extend this to a prescribed period of time (e.g. 3-6 hours – if baby feeds once during that time or twice, you use the same breast). This is “block feeding.”
#6: Use herbs or Sudafed for VERY severe situations. The VAST majority of oversupply resolves with the interventions above. Sage and peppermint can help (however, really impressive hyperlactation doesn’t respond well). Pseudoephedrine (Sudafed) in 10-30 mg quantity can be tried once in the morning (some people can experience insomnia, and it shouldn’t be used with high blood pressure). After six weeks postpartum, estrogen-containing oral contraceptives can be considered. Extreme cases may require as needed individual doses of 0.25-0.5 milligrams cabergoline every three days
Plugging
A breast “plug” represents a focal area of swelling in the breast. It is NOT a true “plug” of milk stuck in a duct. Milk is made and stored in alveolar cells — not ducts (only a tablespoon or two of milk is in the ductal system at any one time).
What people describe as a “plug” is actually full alveoli (milk-making cells – the “grapes”) lymphatic fluid (connective tissue fluid like the kind that can give you swollen ankles), and lots of blood flow in an area.
With appropriate management (BAIT: Breast rest, Advil, Ice, Tylenol), symptoms generally resolve within 24 hours. Note that advil and tylenol are not mandatory — it’s not overfeeding/pumping and ice that is the biggest help. Therapeutic ultrasound is also NOT the mainstay of mastitis or “plugging” or any of these other conditions, though it can helpful at times.
Pseudoephedrine (Sudafed) acts as a vasoconstricting agent (i.e. decreases blood flow) and can also be useful in doses of 10-30 mg once daily in the morning. Diphenhydramine (Benadryl) 50 mg can be added to reduce histamine release.
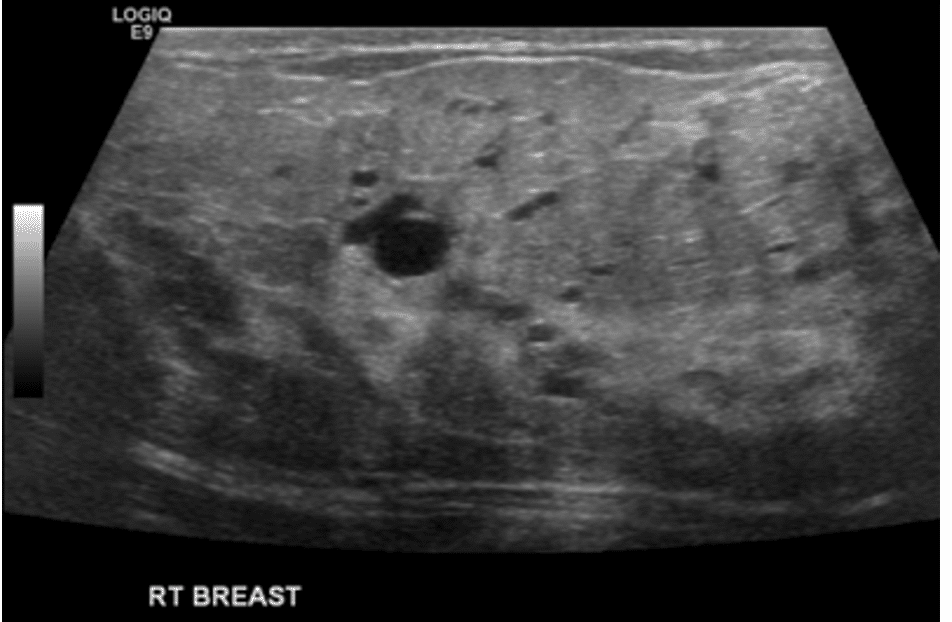
Patients with hyperlactation often experience “plugging,” though patients with average or even low milk supply also may experience “plugging.” Some women are particularly sensitive to any stretch in their breasts, something I call “Irritable Breast Syndrome” (analogous to Irritable Bowel Syndrome). So even if their overall production is lower than average, a particular area that perking up with fuller alveolar cells (compared to the others) can feel like a “plug.” Thin or small-breasted women who have less fat interspersed with gland in their breast can also feel prominent breast tissue that is perceived as a “plug,” but isn’t.
Other risk factors for experiencing “plugging” include pump usage, as pumps do not remove milk physiologically (i.e. “naturally”) like an infant does (i.e. they tell your body to make milk and the “grapes” get big, but the milk doesn’t come out. So you feel a “plug”). Nipple shields also prevent physiologic feeding and cause problems in the same way.
Mothers may report “plugging” after an infant sleeps longer than usual, or when they return to work or school and are separated from the infant for extended periods of time. It is important to recognize that this is not a “plug” in one of the hundreds of millions of ducts in the breast. It simply represents transient engorgement of milk-making cells and congestion of fluid and blood vessels.
If a mother experiences a “plug”, she should strictly avoid excessive massage as this traumatizes breast tissue, causes broken capillaries, worsens swelling and can lead to something called “phlegmon” or abscess.
If you are experiencing blebs, use 5-10 grams daily oral sunflower lecithin supplementation. The mechanism of this is unknown, though it appears lecithin may emulsify breastmilk and reduce inflammation.
It’s important to understand the difference between IN VITRO (in the laboratory, not real life) studies and mouse/rodent studies and IN VIVO (in alive humans). An isolated in vitro study showed that lecithin increases gut inflammation, and some social media sites are now recommending against lecithin. Not only is lecithin a component of most of our food products, but it is used is extremely high doses for neurological studies and treatment. This is a great example of how research cannot be taken out of context. We have cured cancer countless times in mice, but we can’t replicate this yet in humans. The context is important.
Any “plug” or mass persisting for several days and not resolving with conservative interventions requires referral to a medical provider, who may obtain breast imaging to rule out galactocele and/or other mass.
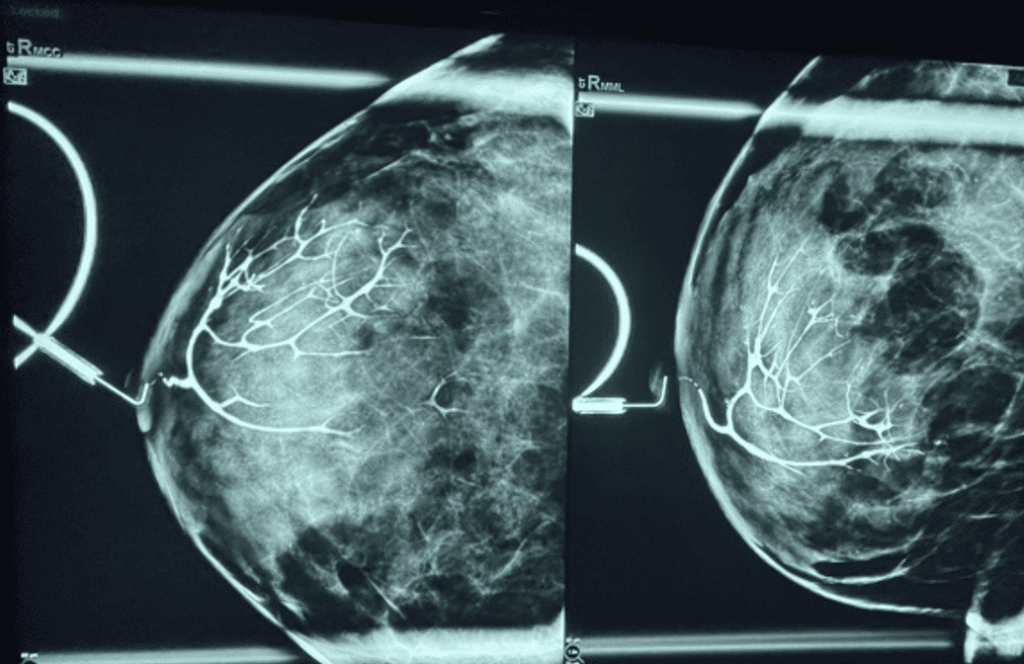
Mastitis
Traditional recommendations regarding mastitis unfortunately result in worsened symptomatology in most cases. For example, women are instructed to breastfeed very frequently or “pump to keep their breast empty” in the setting of mastitis. Unfortunately, this stimulates more blood flow and more congestion in the setting of an already inflamed gland, and it stimulates the breast to produce more milk.
I tell patients to treat their breast like a sprained ankle. You wouldn’t massage a sprained ankle.
You wouldn’t massage another gland like a thyroid in the setting of thyroiditis. You also wouldn’t keep eating to “flush out” a gallbladder or pancreas that is inflamed. You definitely wouldn’t eat to relieve an intestinal obstruction (the blockage comes from swelling of the walls of the intestine, not actual food, unless you have an unusual situation called a “bezoar.”) The breast is no different.
It is very important to distinguish inflammatory mastitis from infectious mastitis. Many types of inflammation in the body produce redness and systemic symptoms without being infectious, such as blood clots in the leg. Mastitis symptoms also mimic panic and anxiety symptoms, including sweating, flushing, alternating with shaking chills and racing heart rate.
Moms will sometimes describe sleeping through the night with their baby, and they awake to mastitis in the morning. It is not physiologically possible to have an infection develop that quickly unless it is an extremely rare flesh-eating bacteria that generally impacts chronically ill people — not healthy moms. What moms are describing is inflammation and tissue swelling in the setting of transient engorgement.
Moms also may report a history of nipple trauma. However, nipple trauma does not represent a cause and effect phenomenon. Instead, nipple trauma is simply a marker for a baby struggling with engorgement or oversupply, or moms resorting to pumping when they are struggling with latch.
Treatment for mastitis includes BAIT (Breast rest, Advil, Ice, Tylenol). Do not overfeed or overpump a breast to “keep it empty.” Pseudoephedrine (Sudafed) acts as a vasoconstricting agent (i.e. decreases blood flow) and can also be useful in doses of 10-30 mg.Diphenhydramine (Benadryl) 50 mg can be added to reduce histamine release.
It is very important to understand that Advil and Tylenol should be used for 24-72 hours and not longer, or not repeatedly. If you feel you need it longer, you need to be evaluated by a physician. If you have recurrent lumps and pain and redness, you may have Irritable Breast Syndrome (see above), which will not be helped by Advil and Tylenol, either.
Without question, patients should NOT MASSAGE their breasts as this worsens swelling and most often worsens pain as well. Therapeutic ultrasound can be helpful in decreasing inflammation. Antibiotic resistance is rampant at this point in time, so it is important to only utilize antibiotics for mastitis if conservative interventions do not resolve the symptoms. I rarely use antibiotics OR probiotics in my daily clinic; evidence for probiotics is VERY limited.
Infectious mastitis generally takes 24 hours or more to develop, and is most often associated with massage (i.e. tissue injury, cell death), overpumping or overfeeding from the breast. With lack of resolution, antibiotics should be initiated because a true infection has developed. Antibiotics work via an anti-inflammatory effect as well as anti-bacterial.
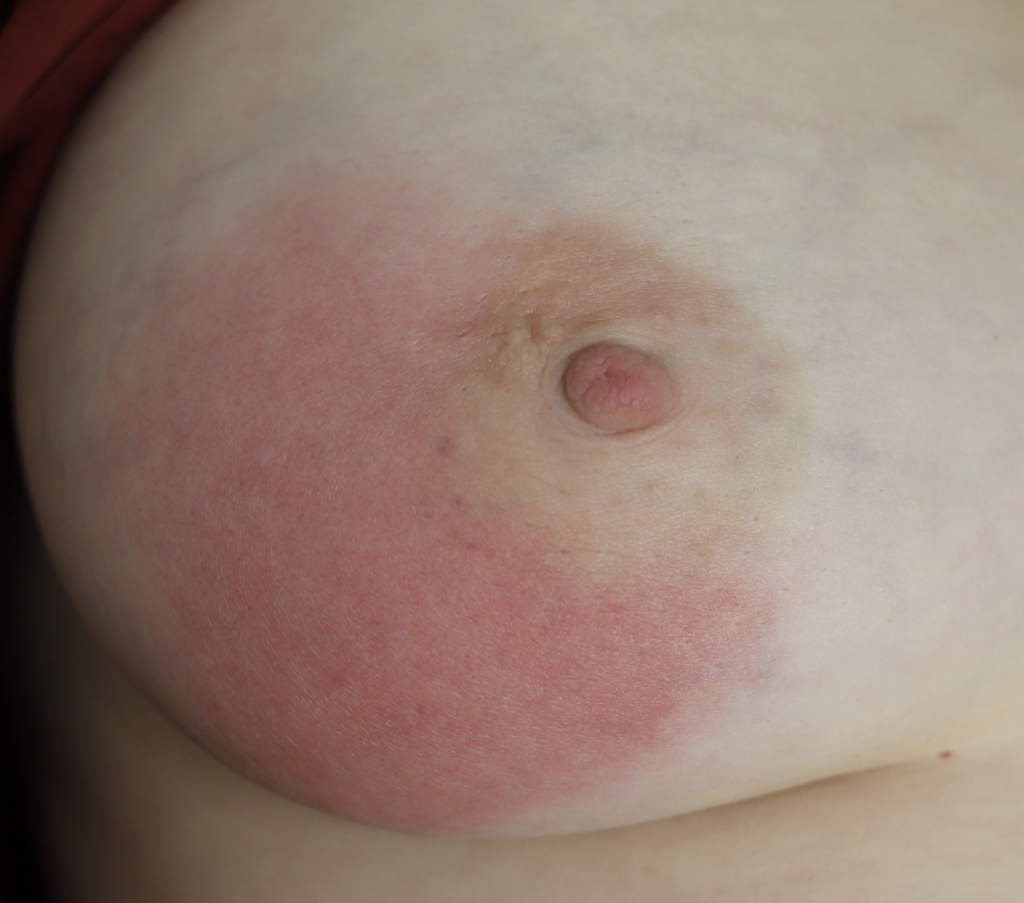
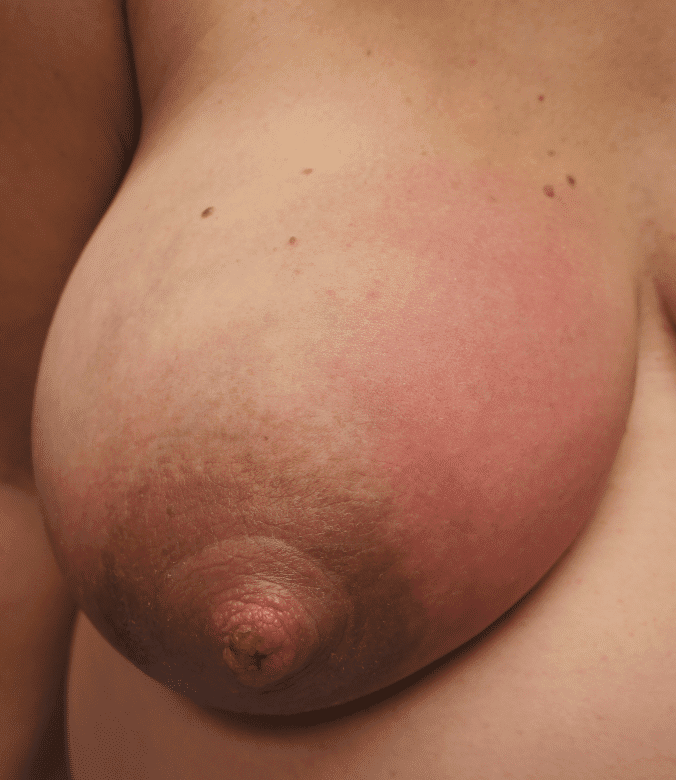
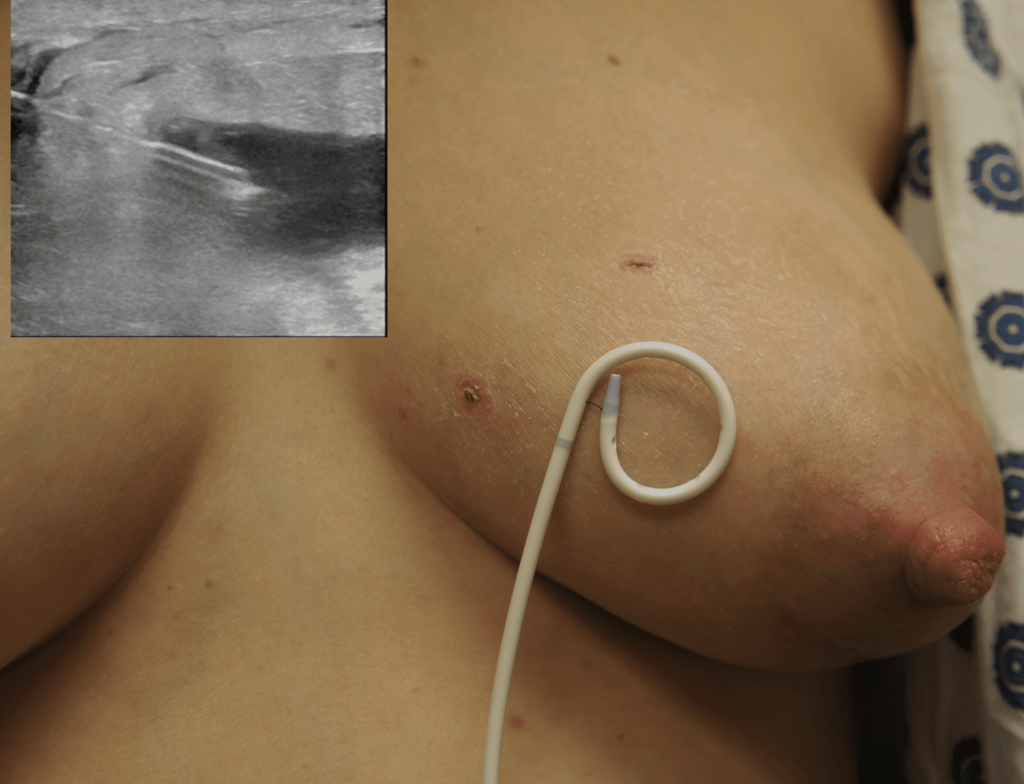
The above photo is a true case of mastitis requiring antibiotics in the setting of a patient not massaging or overfeeding. However, she had persistent hyperlactation and was needing to pump at work and developed a bleb. After 24 hours of no improvement despite ice, anti-inflammatory medication, and therapeutic ultrasound, we started antibiotics.
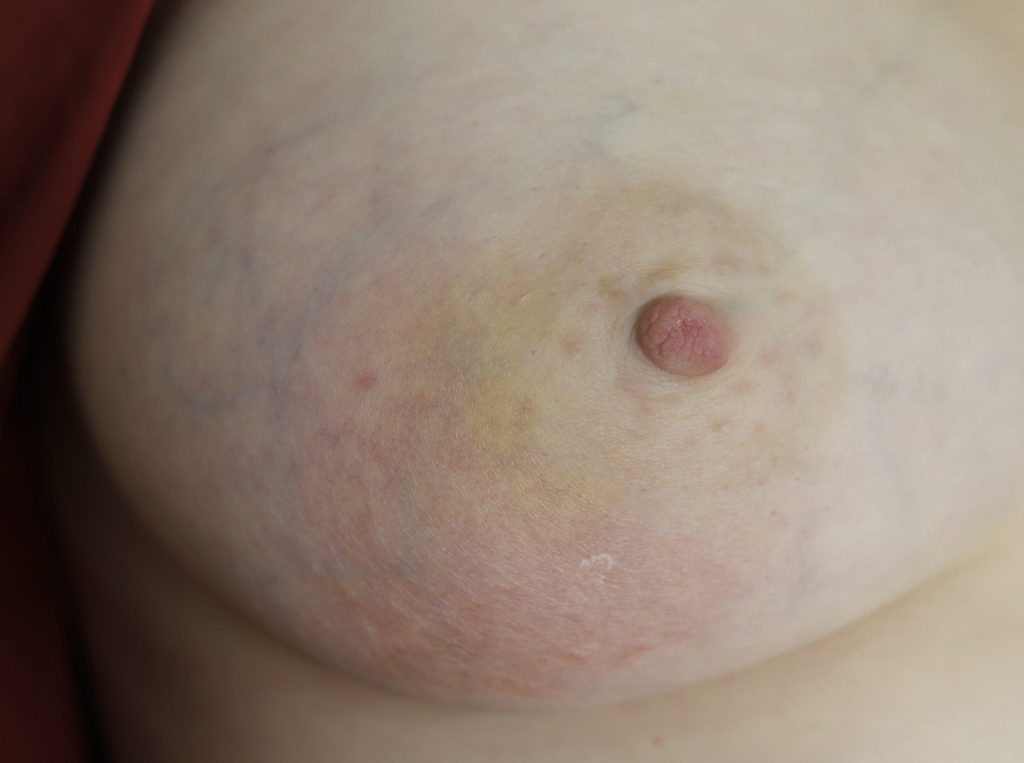
Three days later, the patient’s redness, pain, and swelling was markedly improved. However, she still had some residual edema (swelling) within her breast tissue on ultrasound and so we continued antibiotics until this resolved.
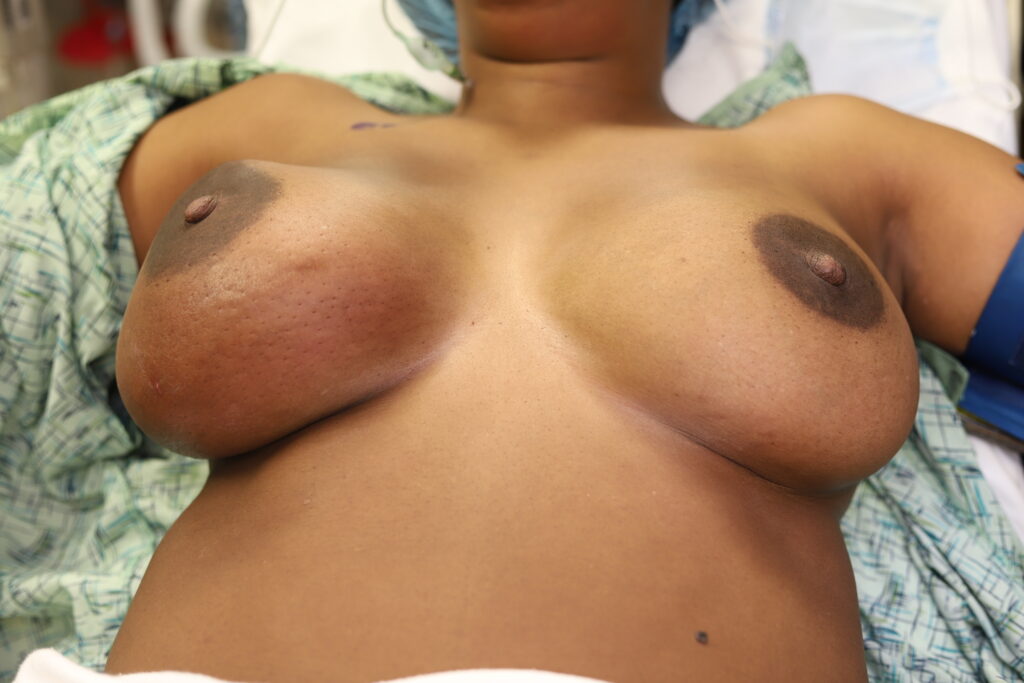
The anti-inflammatory effect is what causes some moms with early mastitis to believe that the antibiotic cured their mastitis. It very easily could have been resolved with BAIT (Breast rest, Advil, Ice, Tylenol).
The vast majority of antibiotics are safe in lactation and breastfeeding should not be interrupted. Any questions can be referred to the National Institute of Health Lactmed database or Texas Tech’s Infant Risk Center. For full references, see the Trash the Pump and Dump section). Dicloaxillin 500 mg by mouth four times daily is the “first line” antibiotic in mastitis. Cephalexin (keflex) 500 mg by mouth four times daily is another option with braoder coverage that may not be necessary. Clindamycin 300 mg by mouth four times daily used to be the “second line” antibiotic, but clindamycin resistance has become widespread. Trimethoprim/sulfamethoxazole (Bactrim) double strength is now the more common twice daily antibiotic, but it also has side effects such as headache and propensity to cause rash.
Be very cautious with breast milk cultures as they often are not performed correctly. A “clean catch” protocol rather than swabbing the surface of the nipple (any skin swab will always grow organisms, but may not be clinically significant) is important. Further, unless you address and resolve underlying risk factors for problems such as exclusive pumping, the culture may continue to show growth. This results in repeated courses of antibiotics without definitive resolution. Milk cultures also a very non-specific: i.e. we don’t know the clinical significance of whether growth is pathologic/problematic or not.
Recovery from infectious mastitis may result in decreased breastmilk production that generally increases within a few weeks. Infants may reject a breast that has considerable inflammation, and hand expression can be utilized to mimic physiologic milk removal rather than using a pump. Milk from a breast with mastitis may have increased sodium (salt) content and babies also may not like the change in taste of the milk.
Abscess
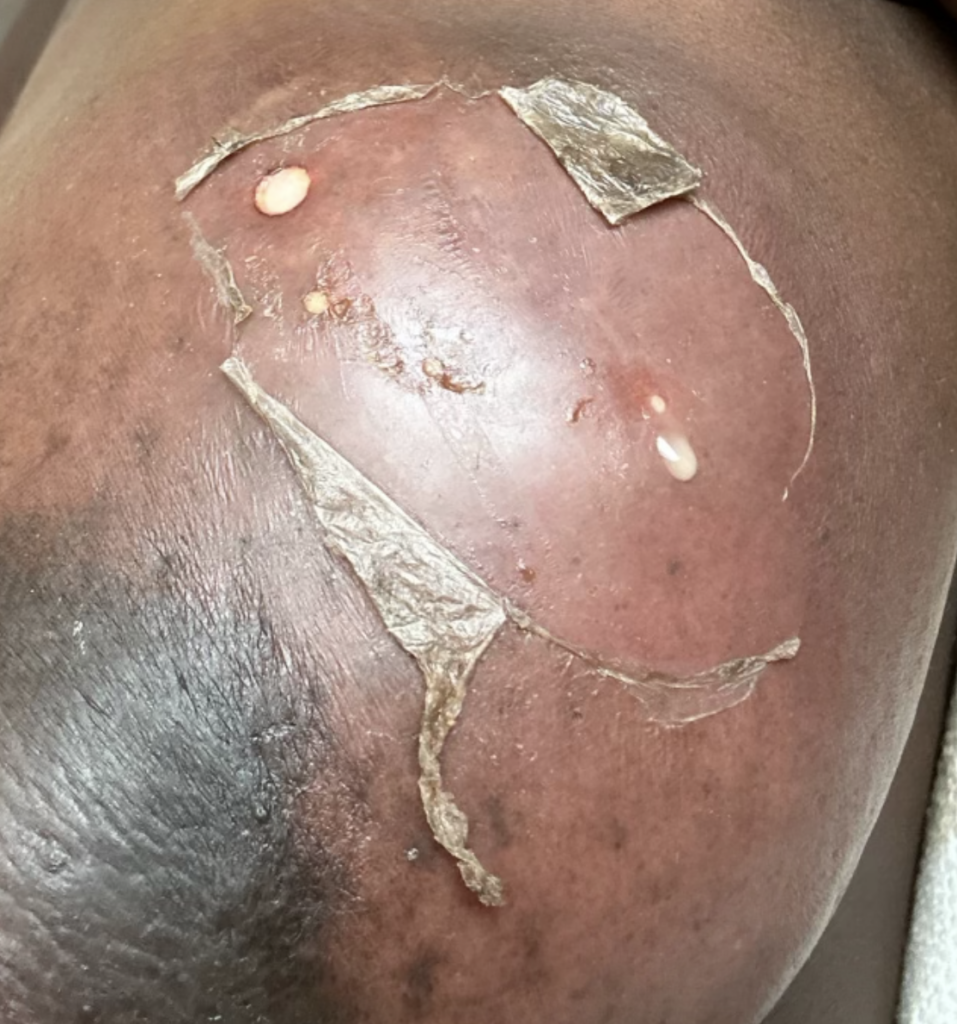
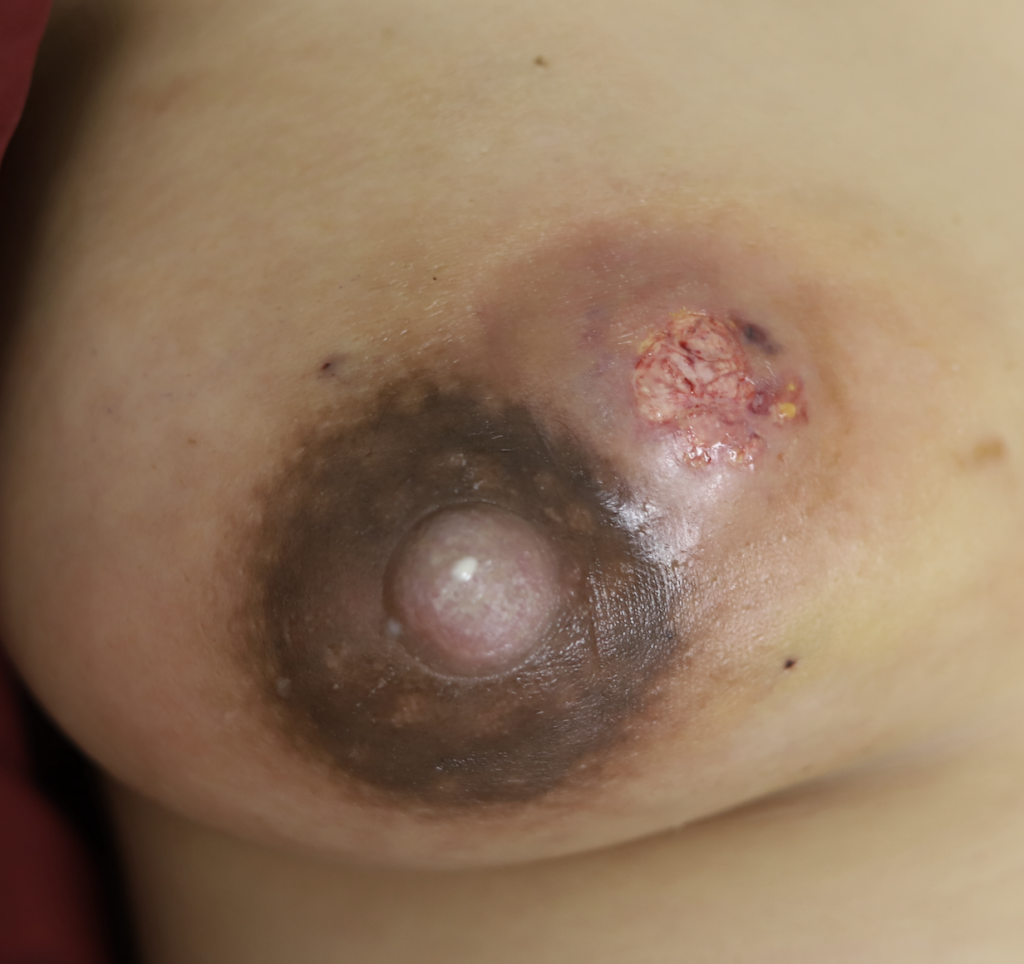

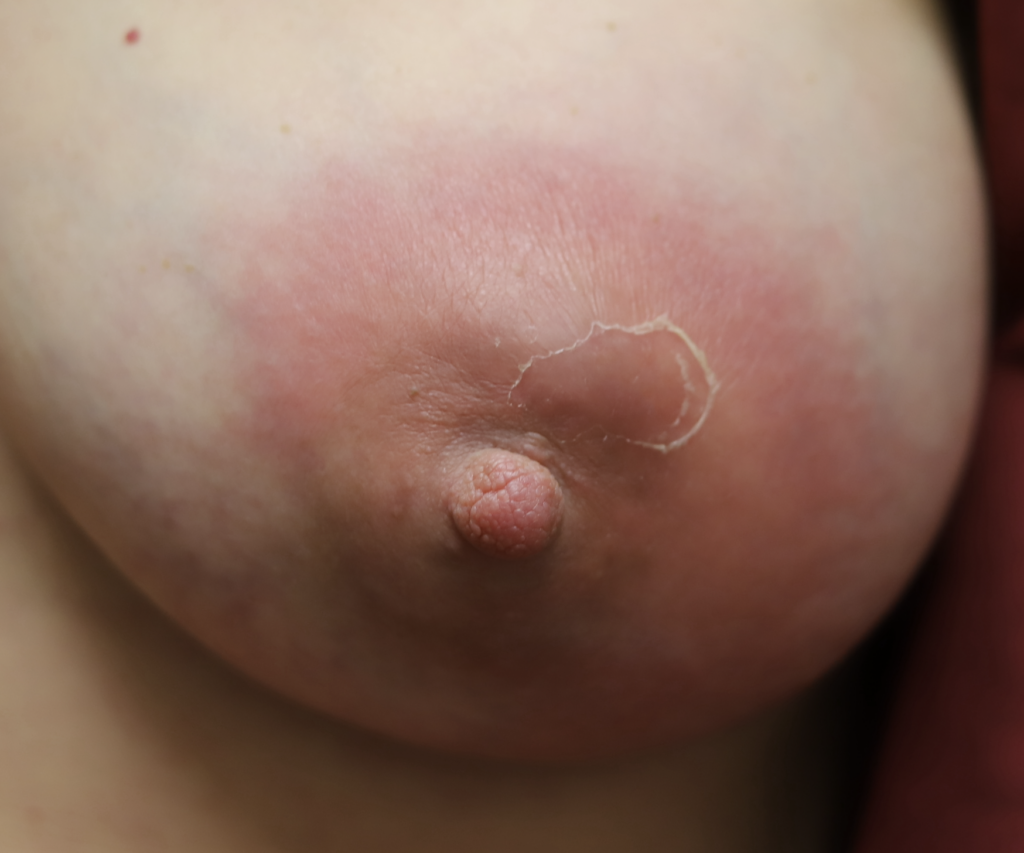
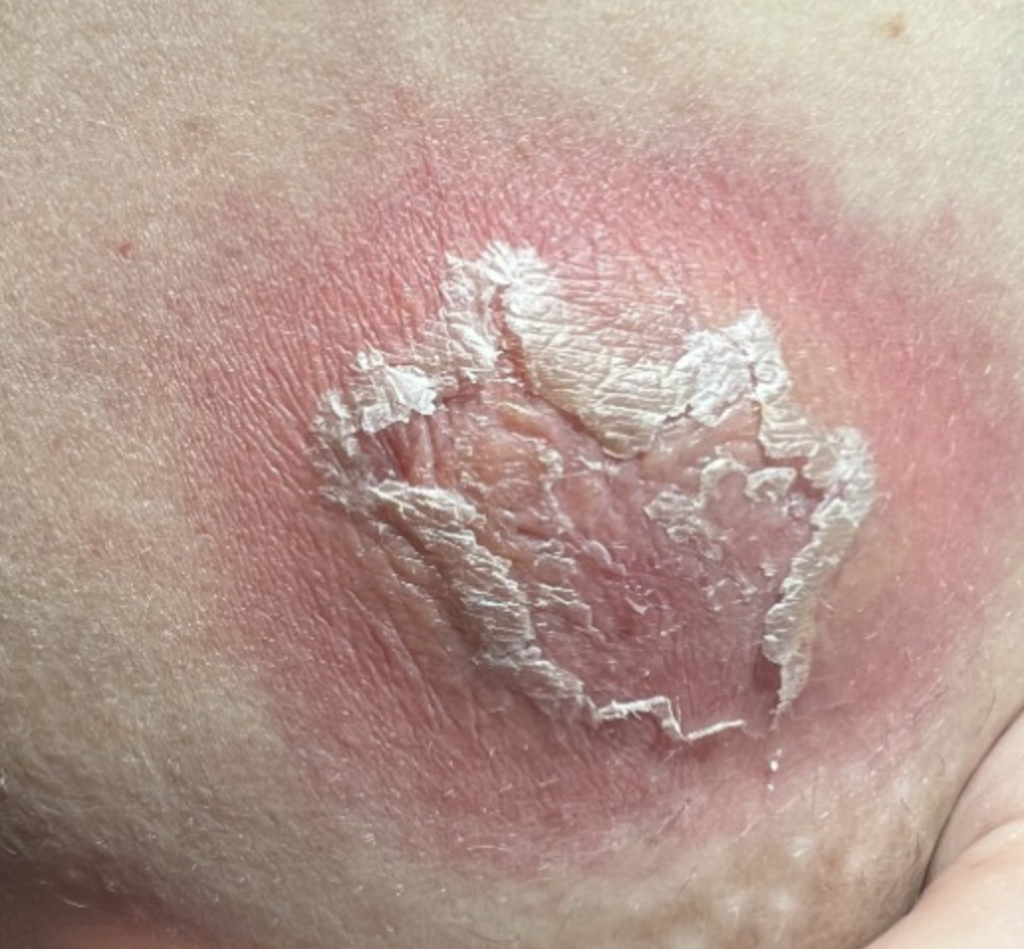
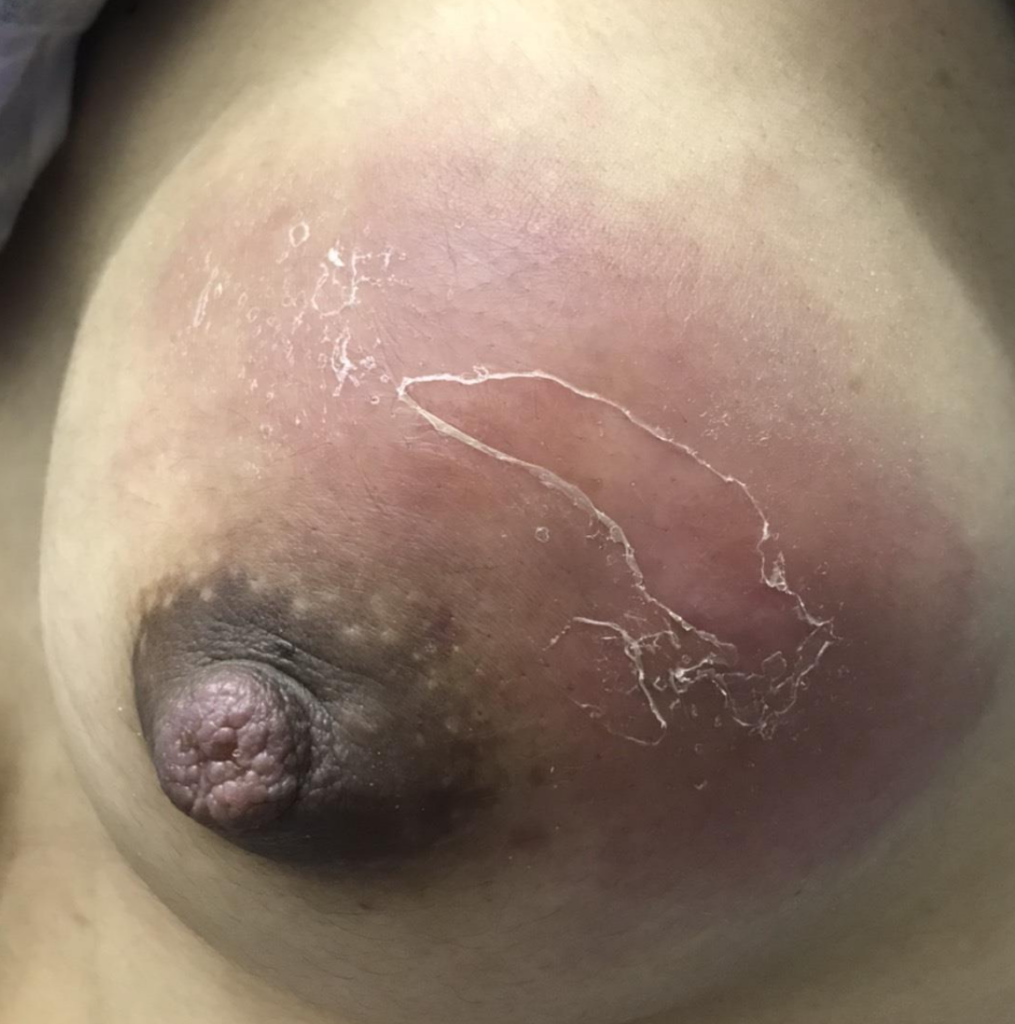
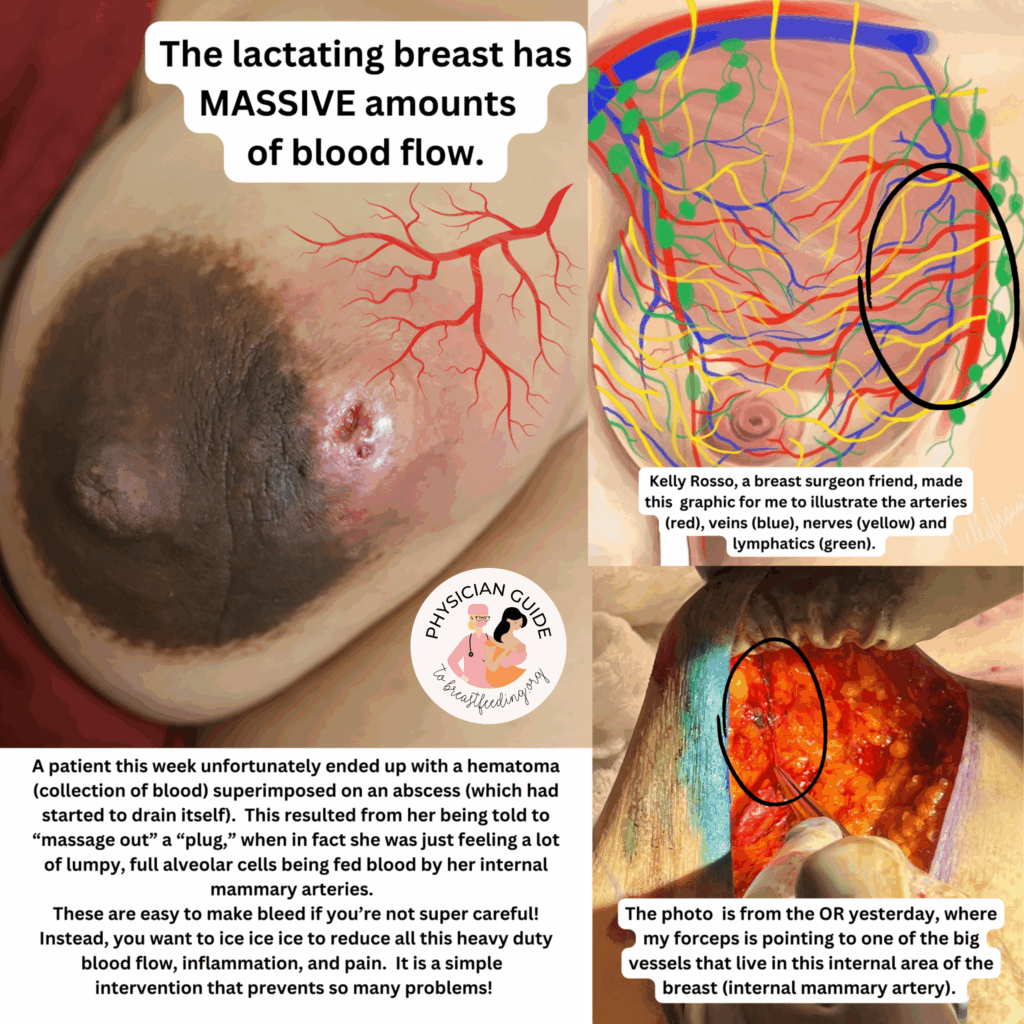
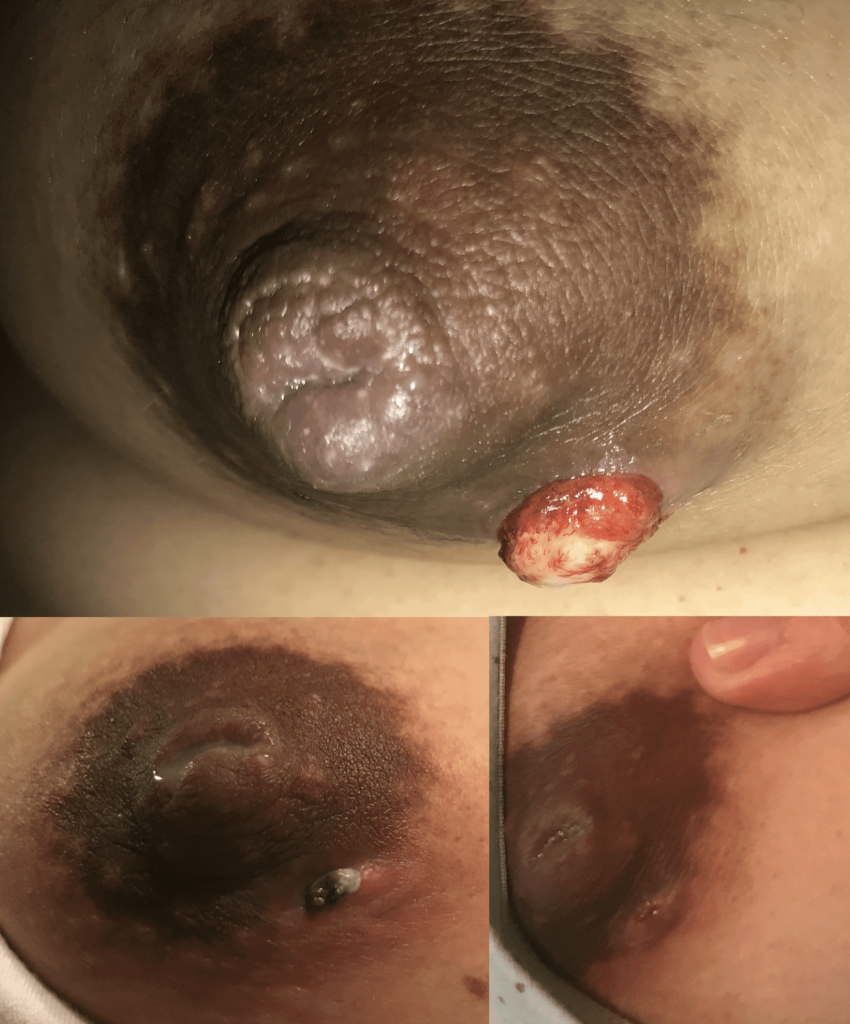
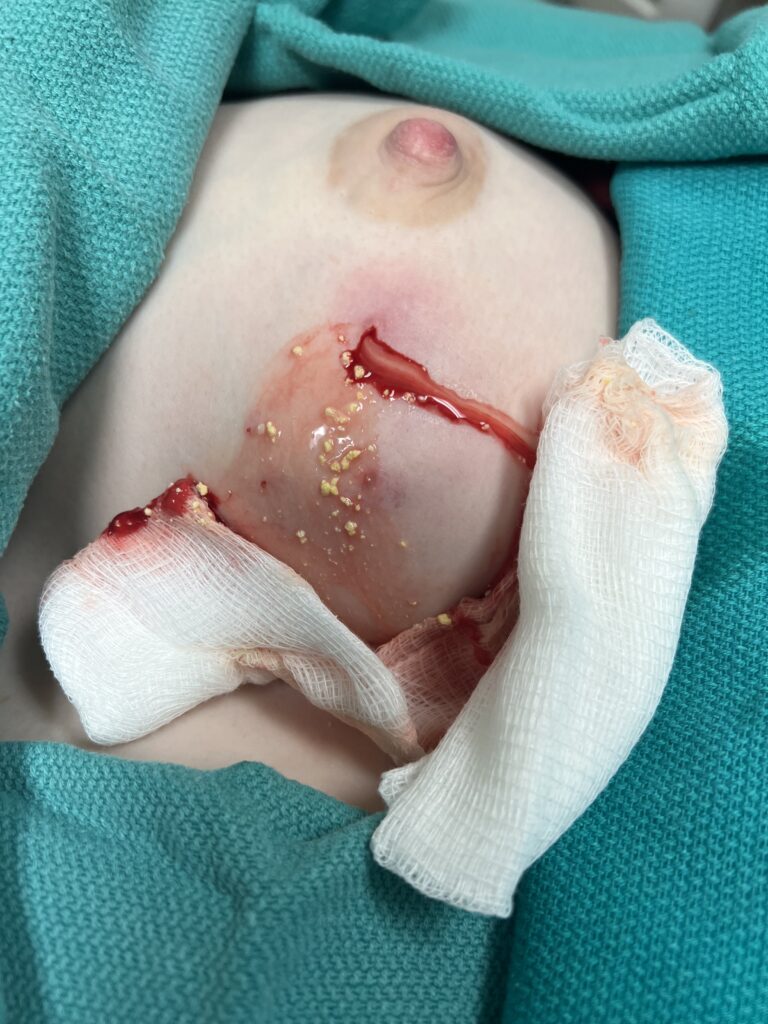
One of the first questions people have is “is this an abscess or just mastitis?” While an abscess can be a bit more subtle than these two images above, most of the time it is this obvious. The peeling skin means that the skin is about to breakdown and drain fluid itself. These patients all have a history of a “plug” they were told to “massage to get out” and then pump or feed (or both) to “empty the breast.” Then they end up with a bulging fluid collection. If this sounds like you, you need an ultrasound for diagnosis if you’re not going directly to a surgeon who can diagnose and drain it both.
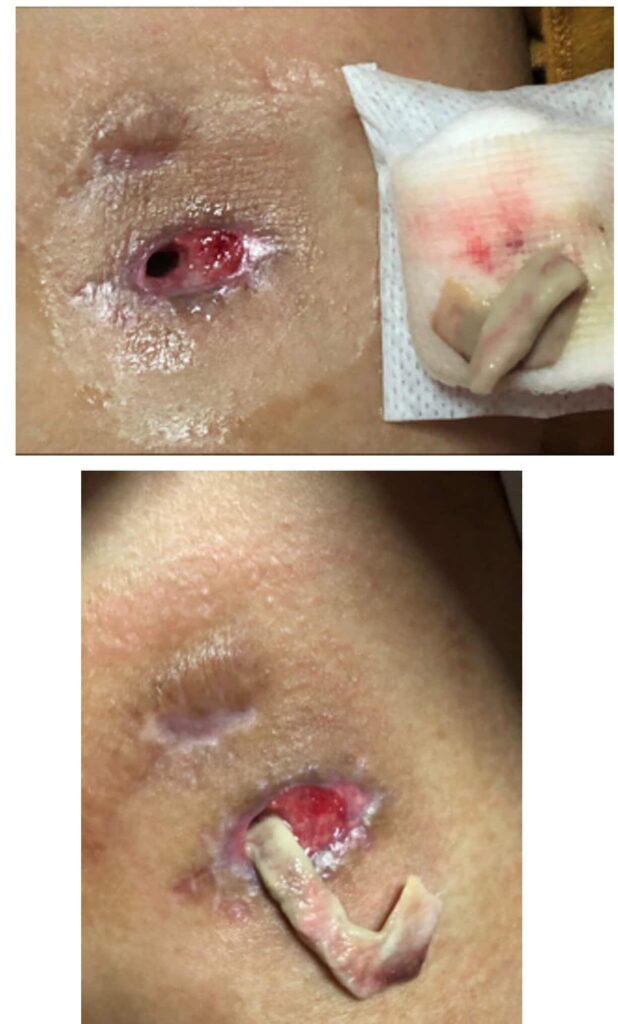
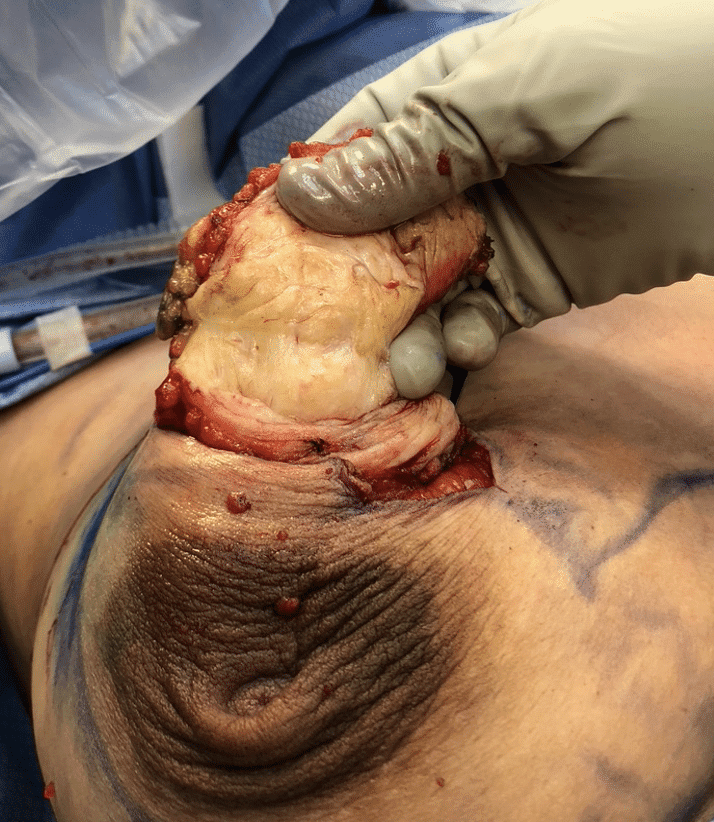
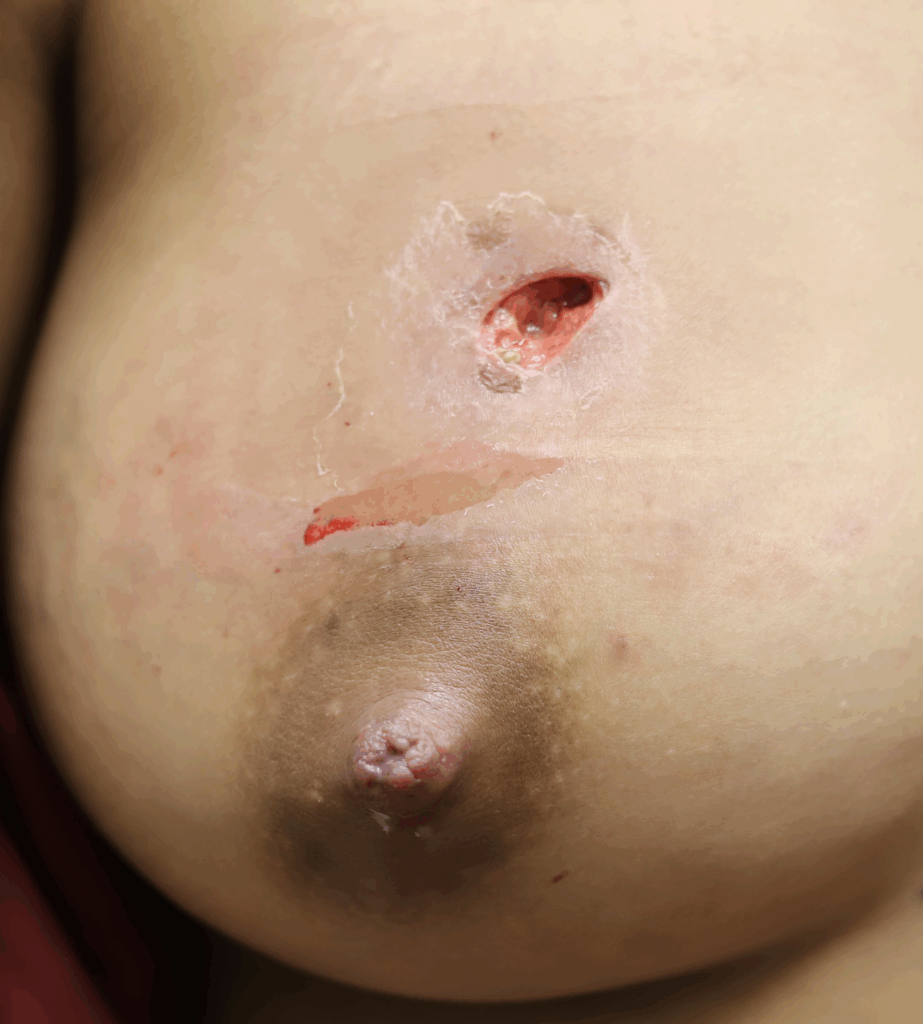
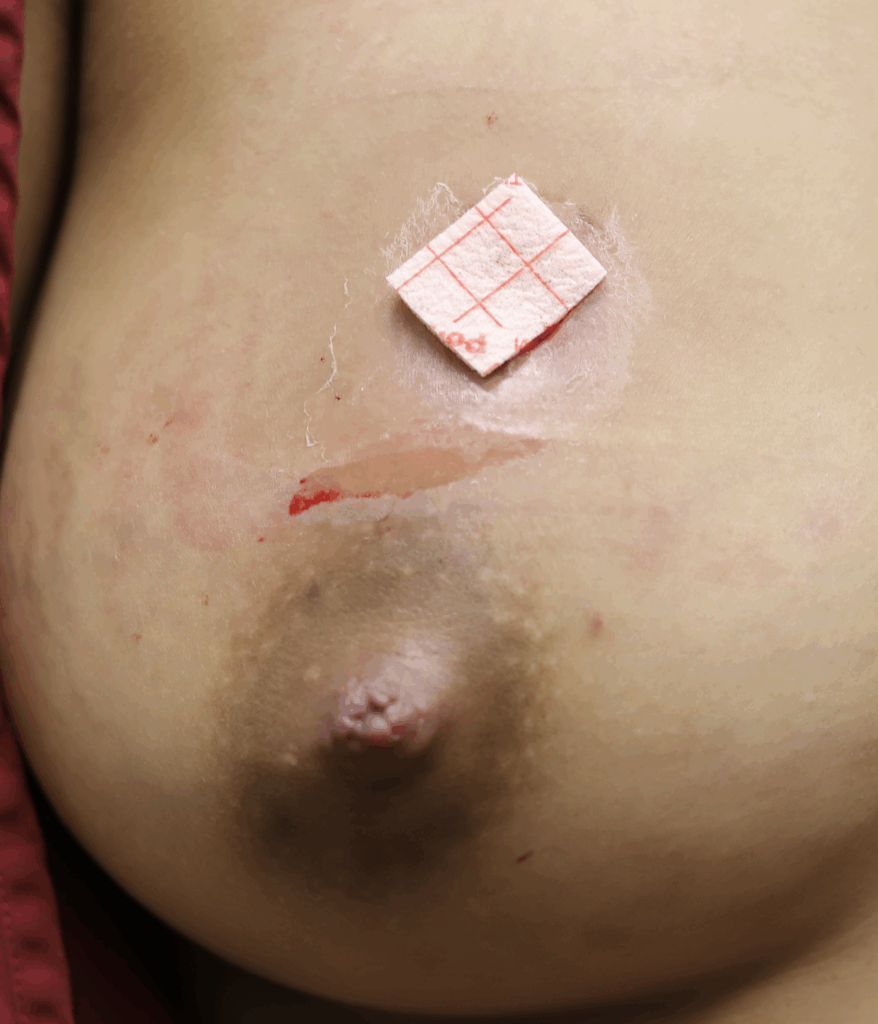
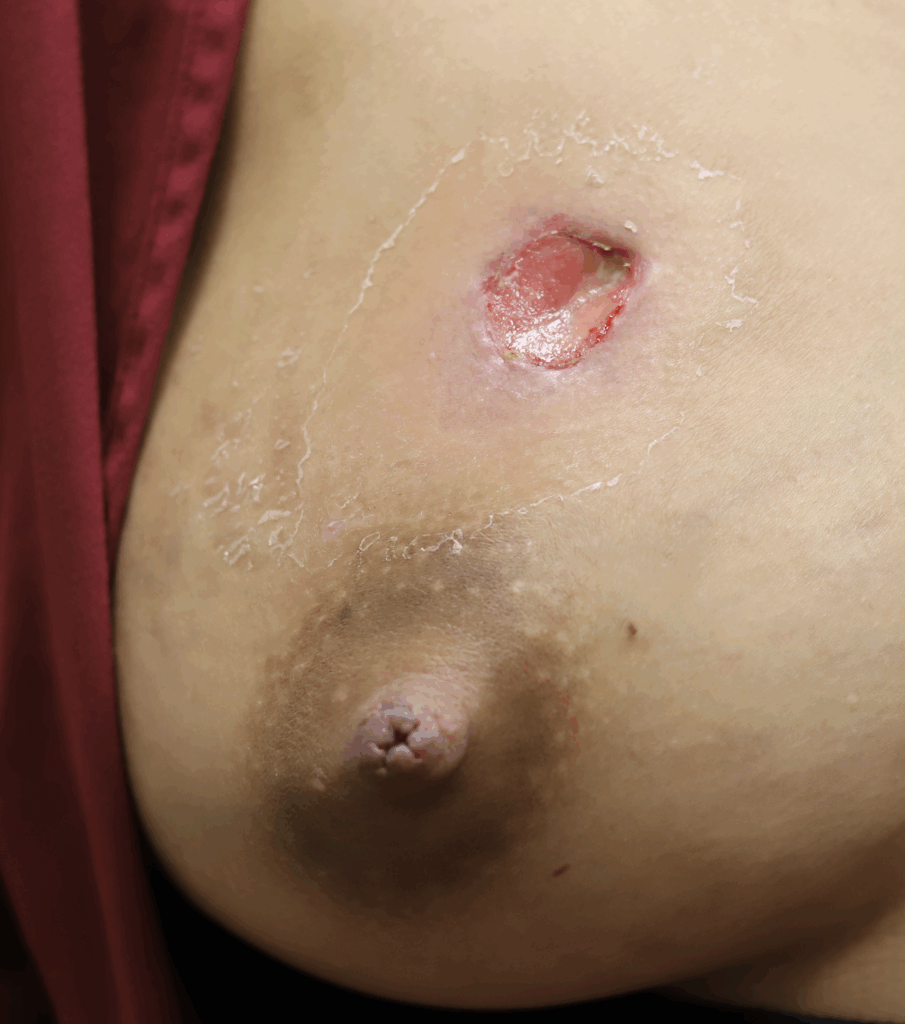
Below are a series of images captured by a patient in a different state who had one of the worst, if not the worst, situations of an abscess caused by heat and massage. Fortunately, the lactating breast is full of blood and wants to heal itself, so she did regenerate a lot of soft tissue coverage that she lost in this situation. Still, this is nothing you ever want to have happen to anyone, and it is a COMPLETELY preventable condition (e.g. had she just been told to use ice and not pump in the very first photo).
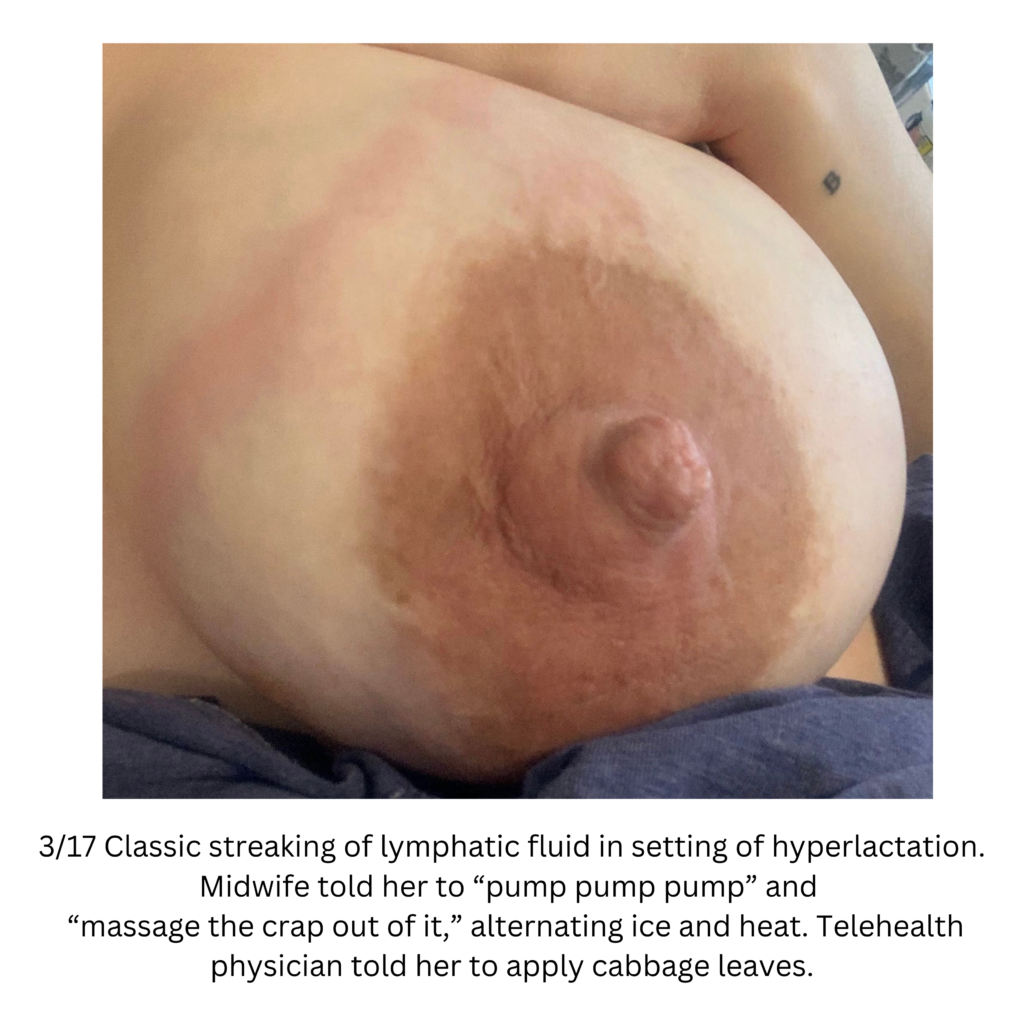
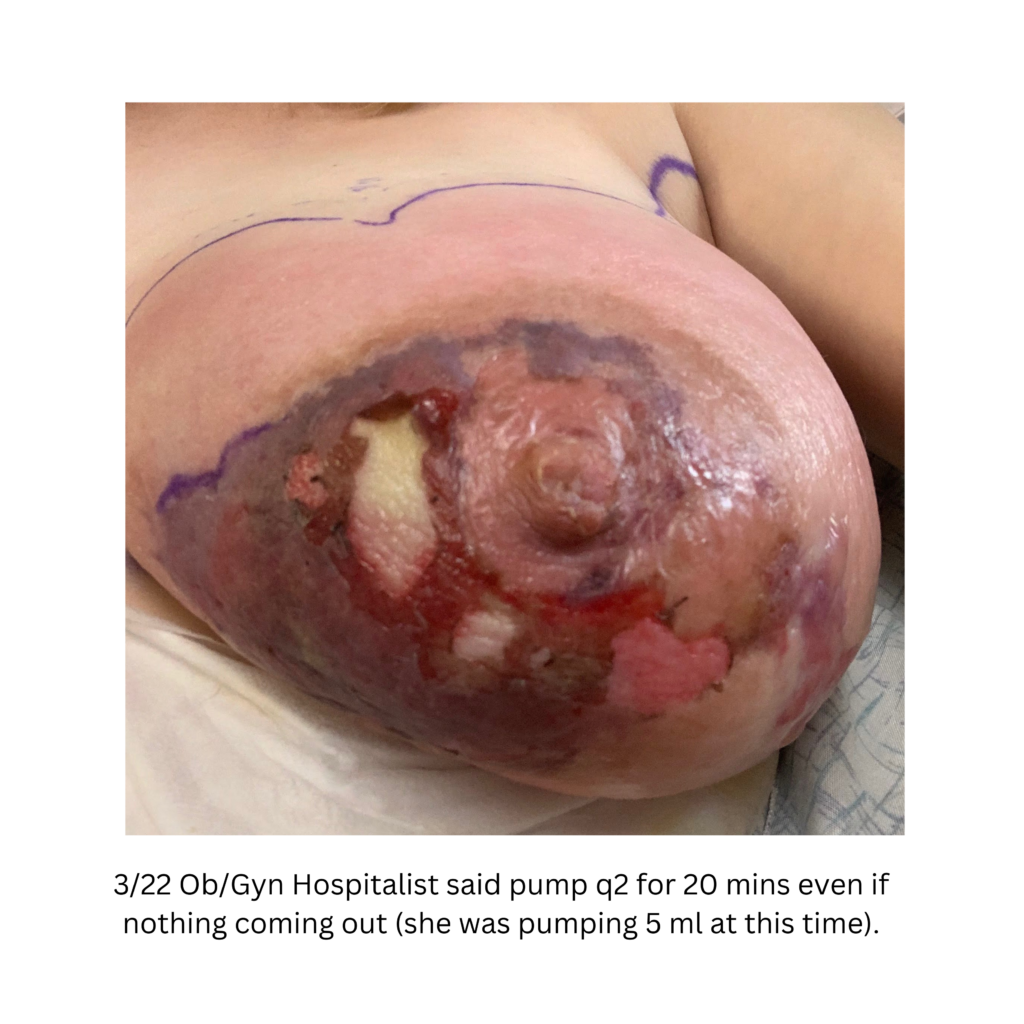
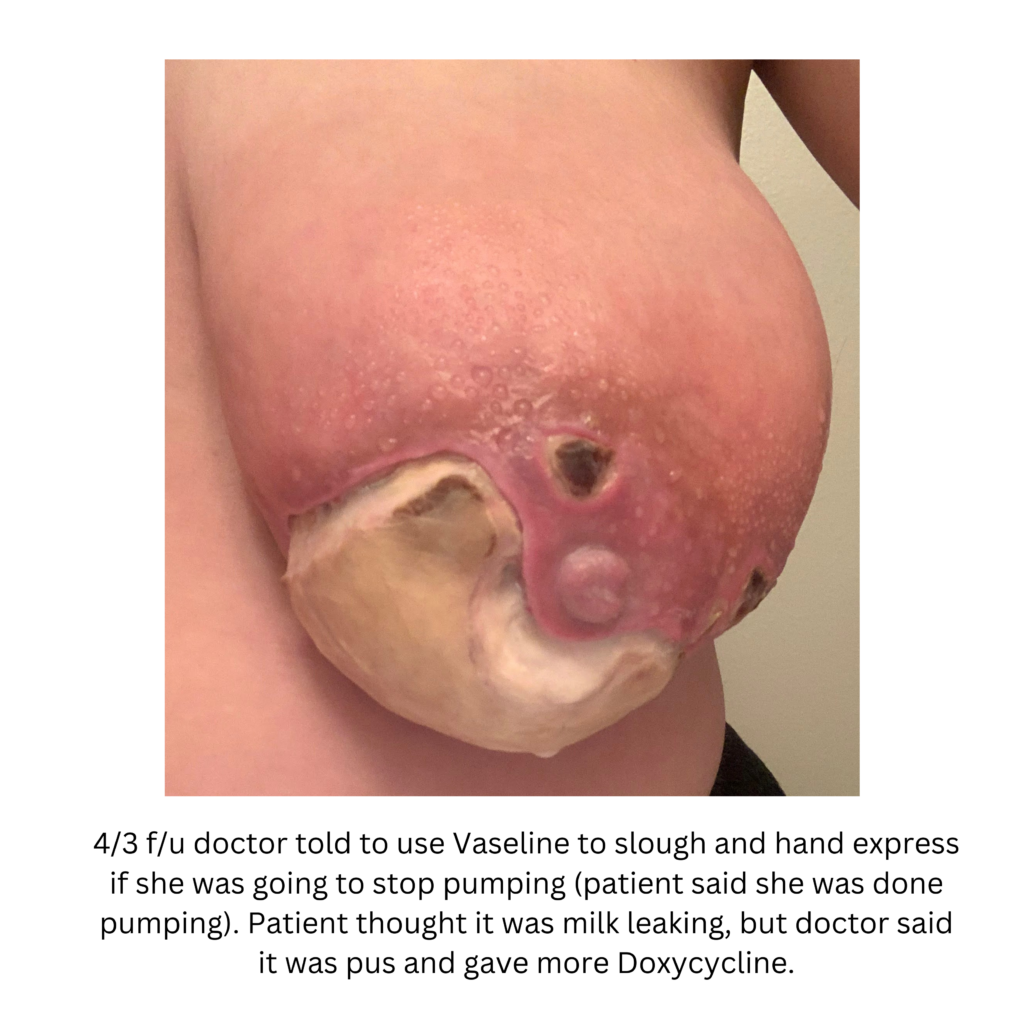
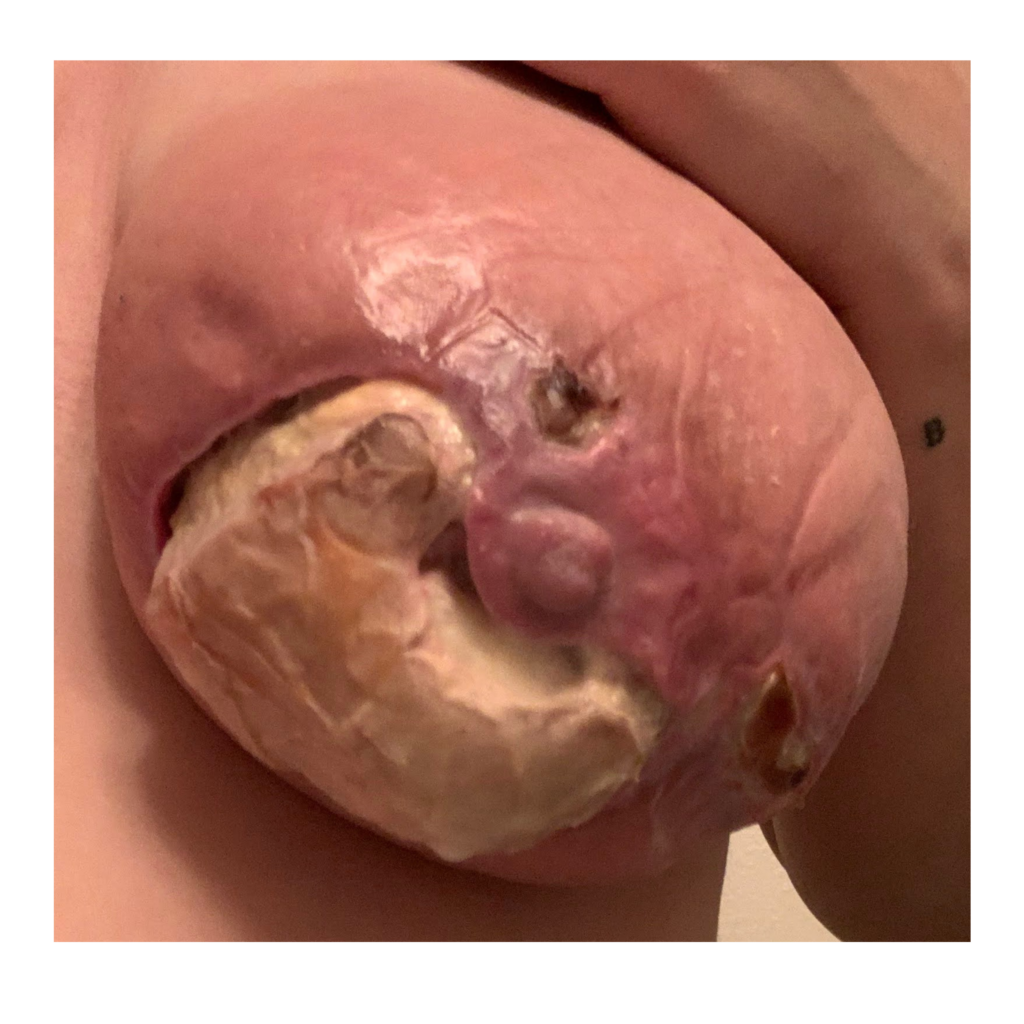
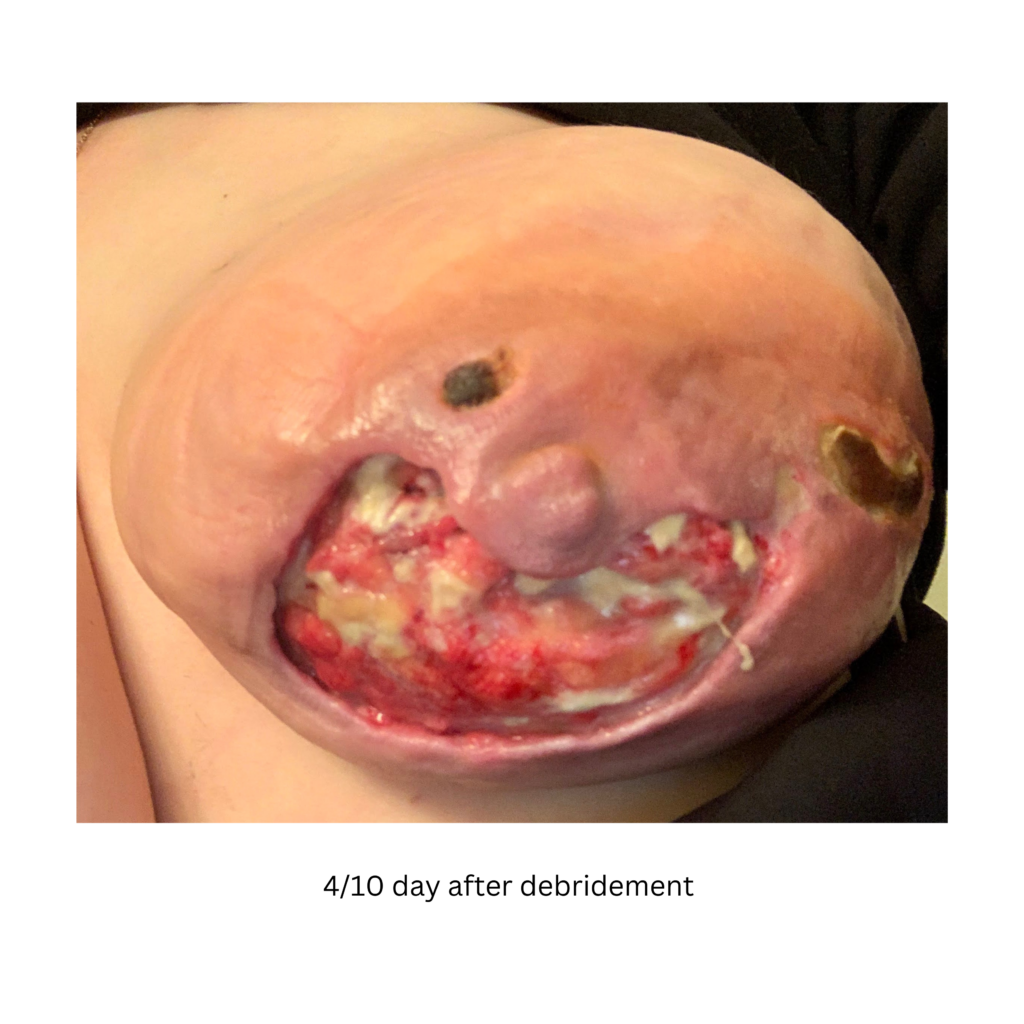
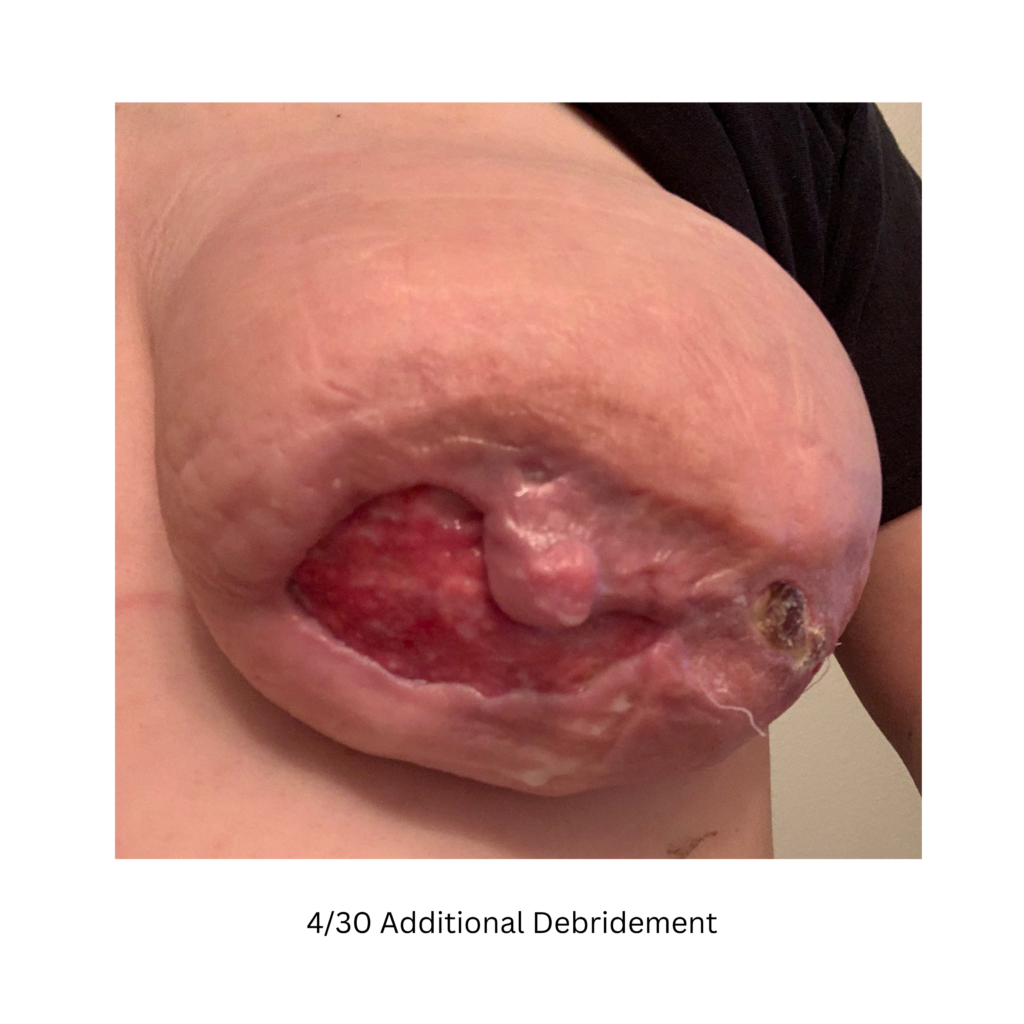
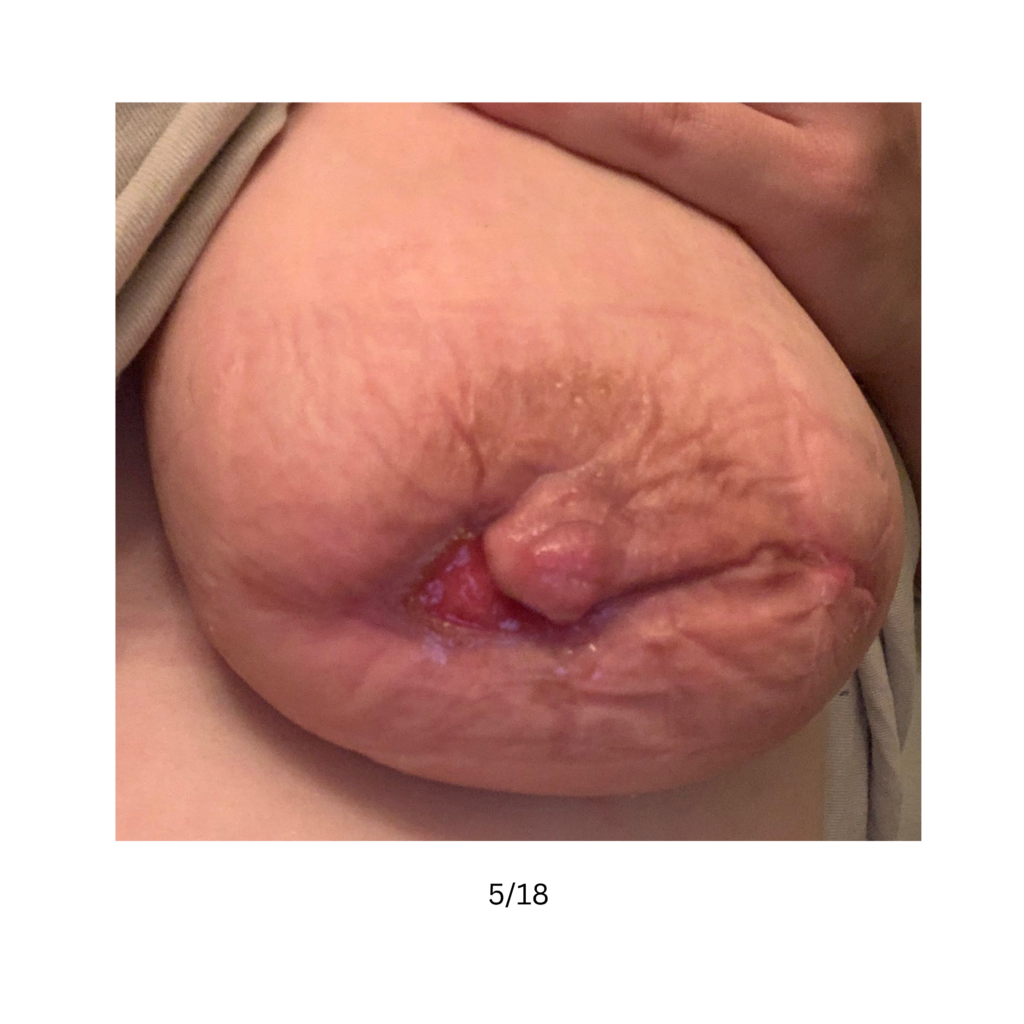
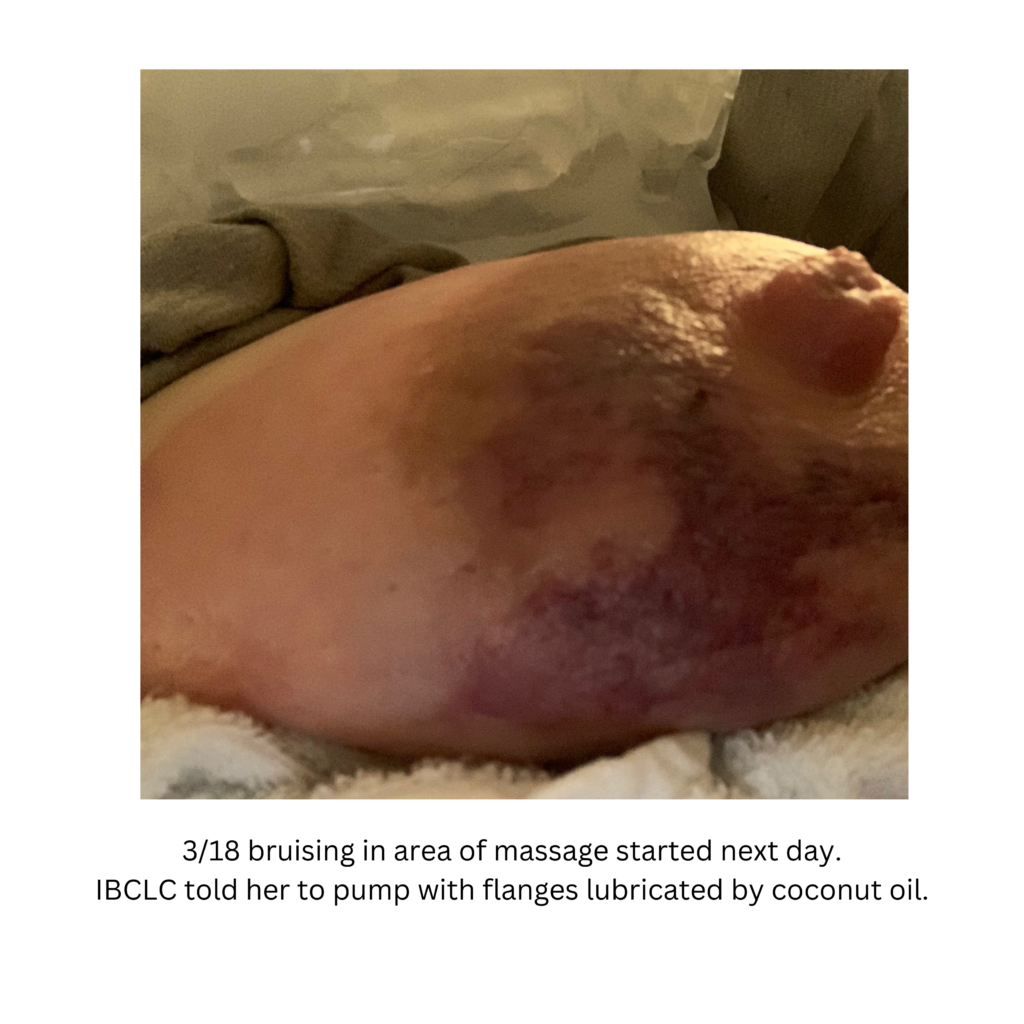
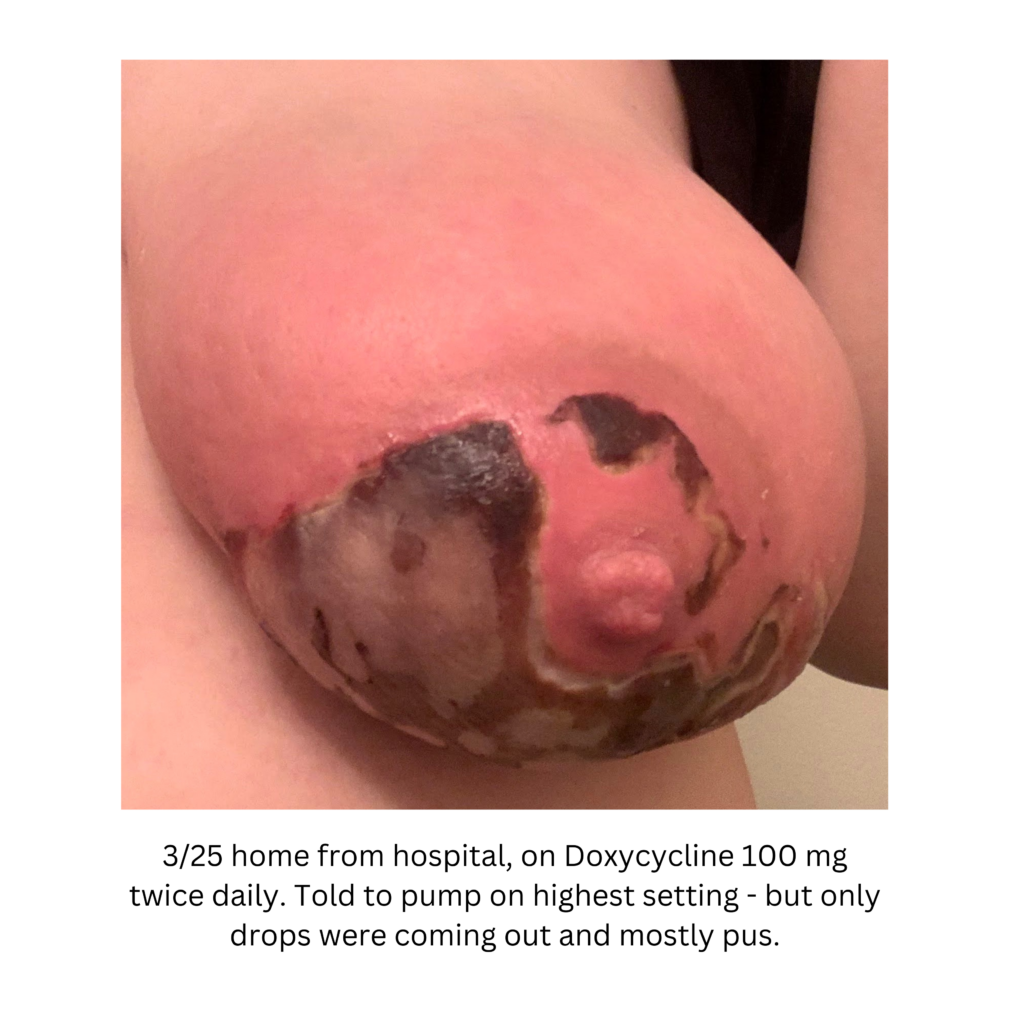
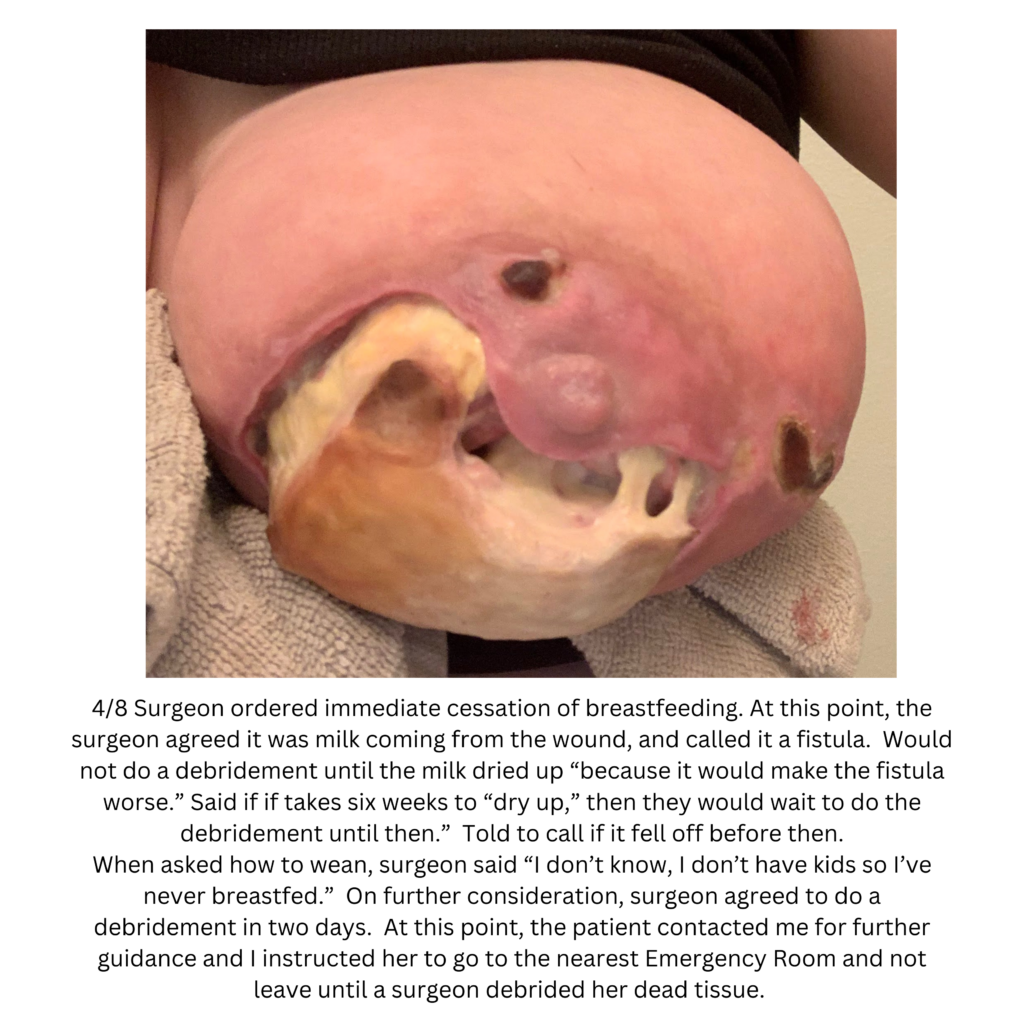
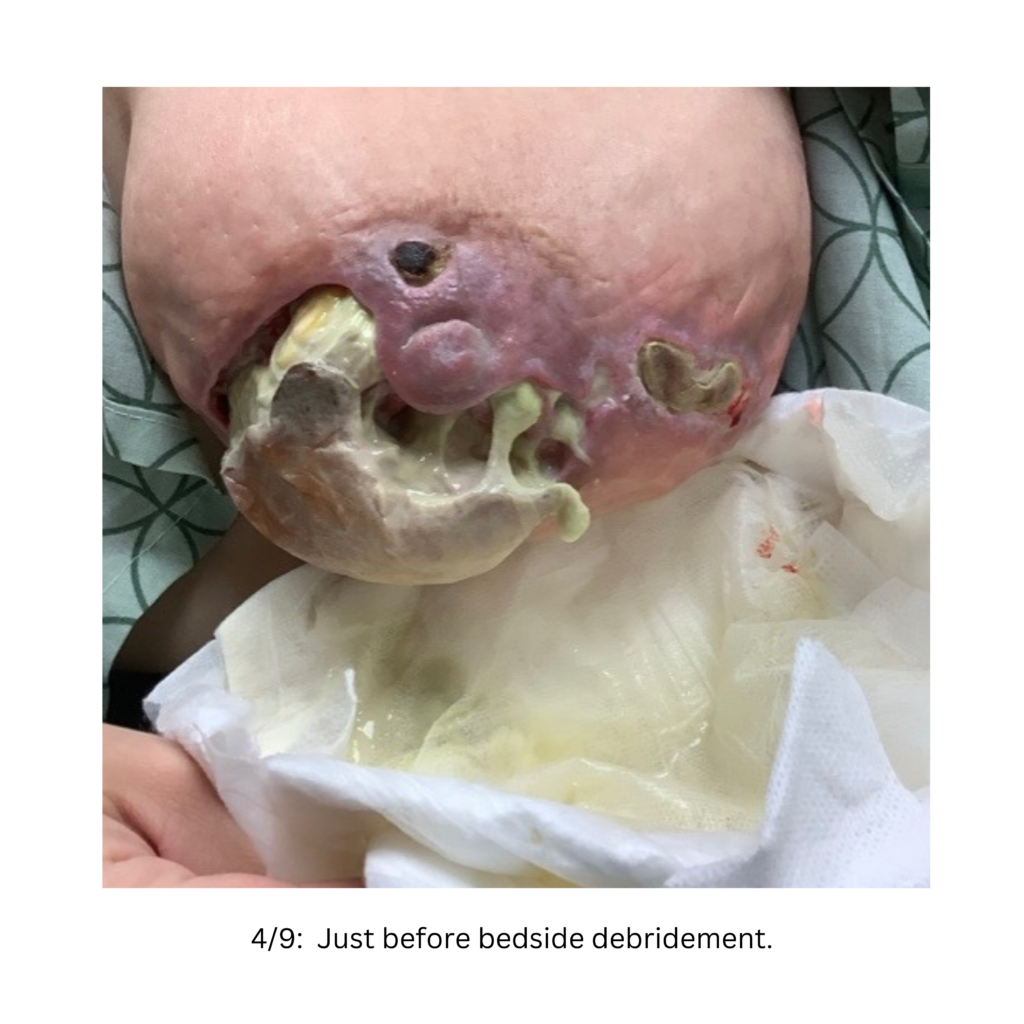
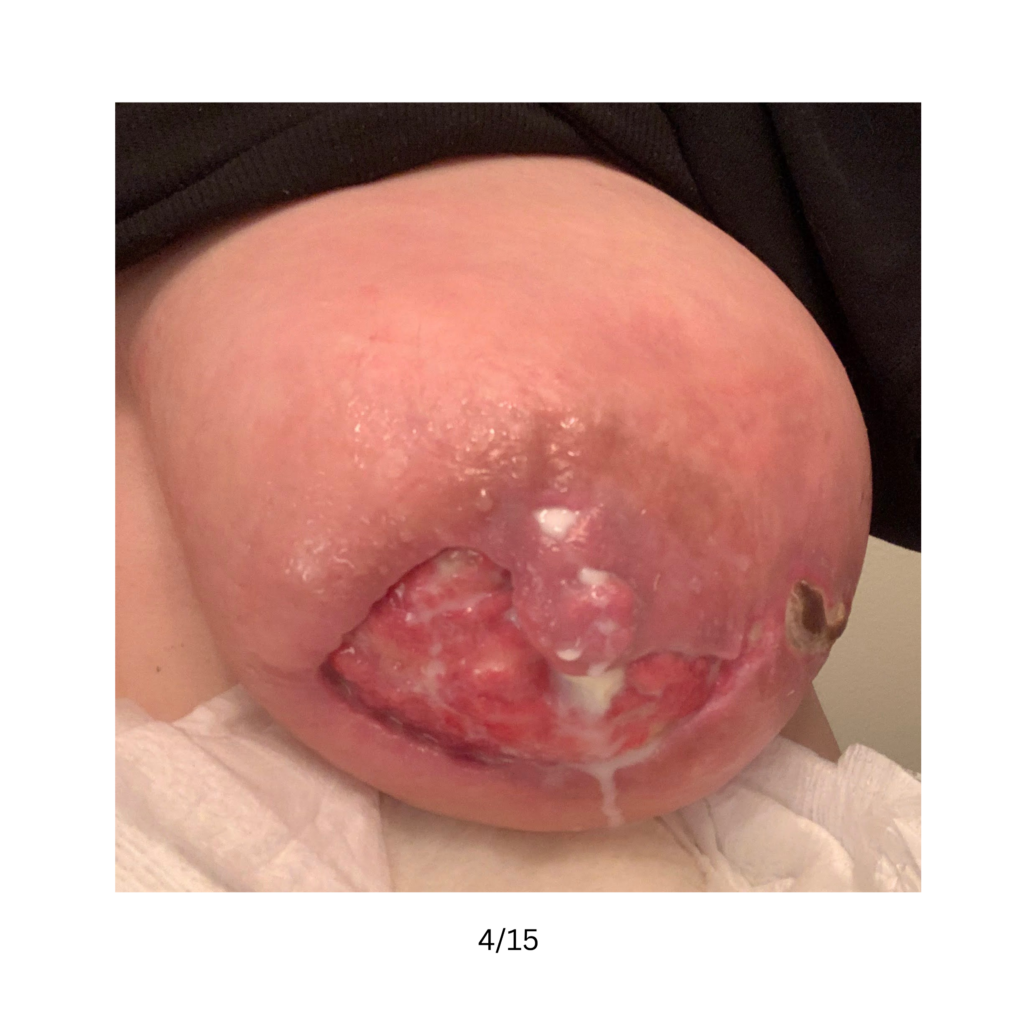
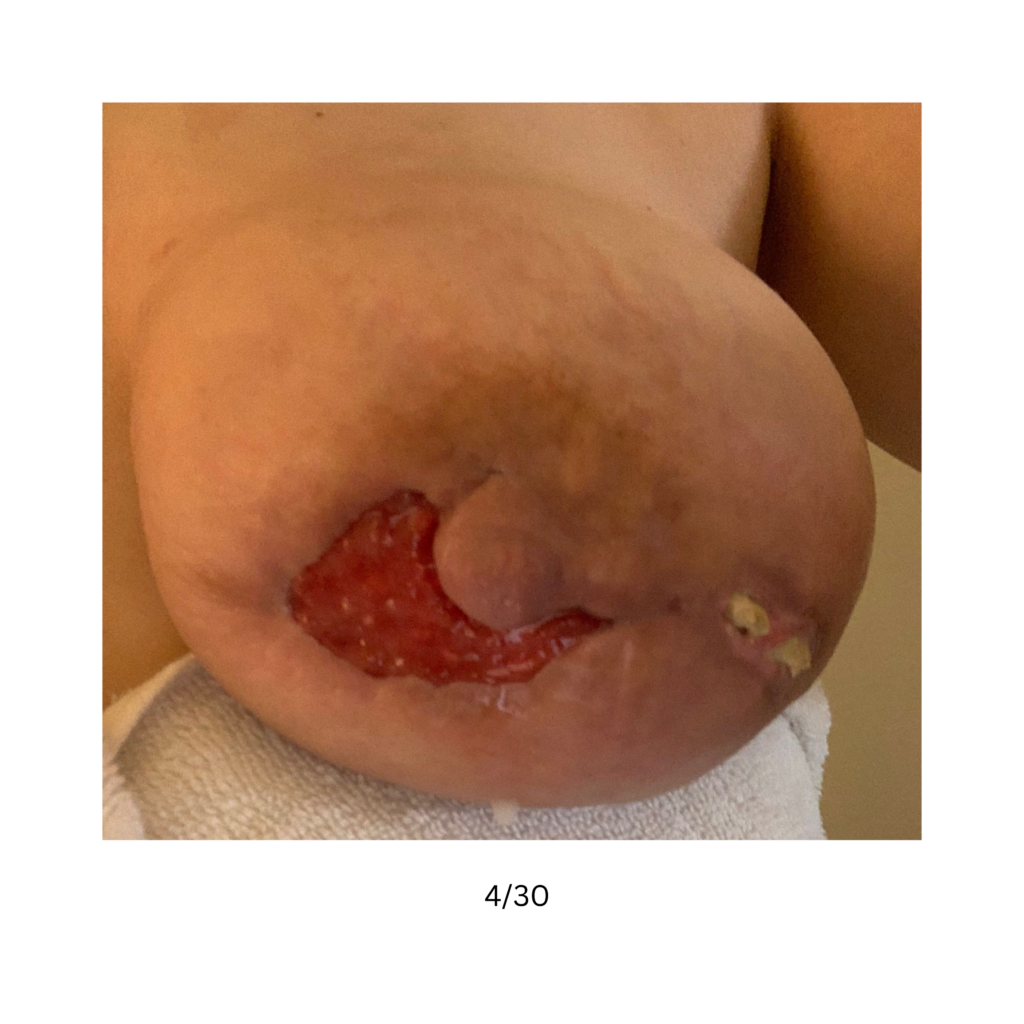
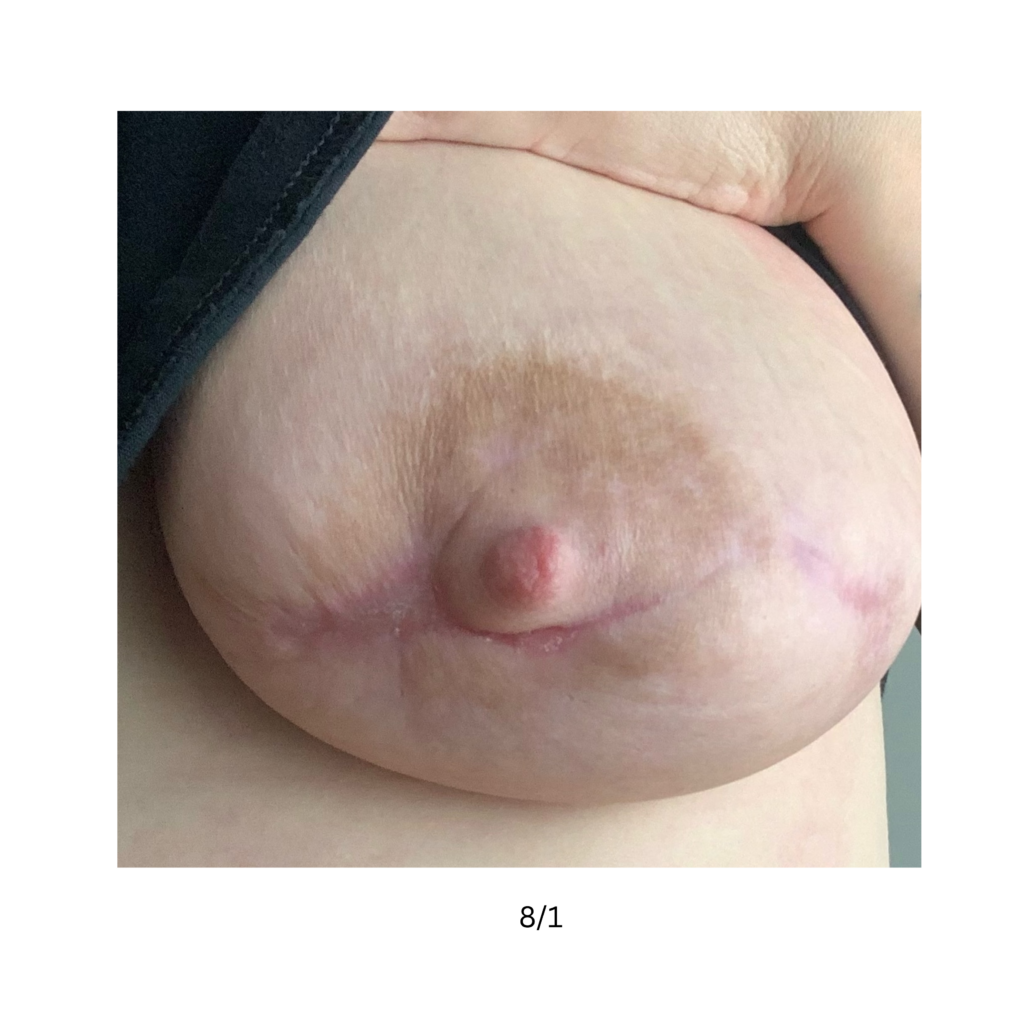
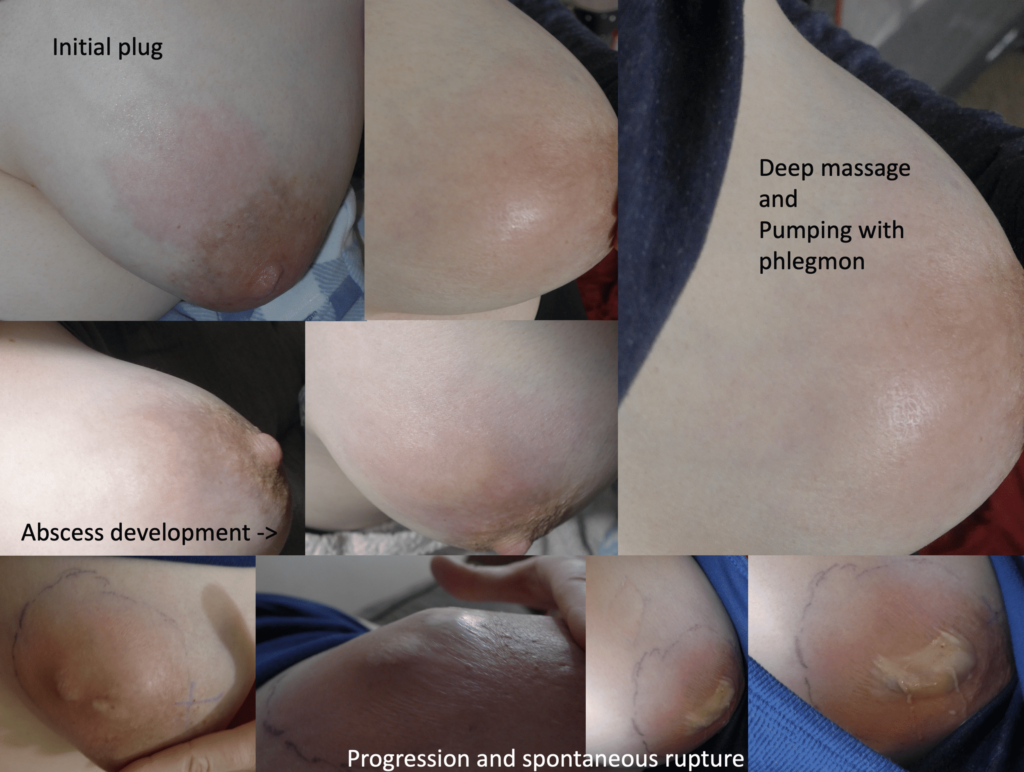
Excessive massage, overpumping, and not utilizing antibiotics with worsening symptoms can result in the progression of a “plug” to mastitis that then can develop into a phlegmon and finally abscess. “In Office Drainage of Lactational Abscess,” which I presented at the 2021 American Society of Breast Surgeons meeting, reviews this progression, as does the montage of photos below provided by a patient who was unable to access medical care during the height of the Covid-19 lockdown. It should be noted that while surgeons and radiologists have been instructed in recent years to aspirate (use a needle) lactational abscesses, this very often does not result in definitive resolution because breastmilk is too sticky to fully remove via a needle.
Instead, a very small incision with a skin wick or small drain should be used and removed after 3-5 days. Drains should not be placed to suction.
Below is a video a patient shared with me (she wanted her husband to film the procedure!), and was generous and emphatic that I should use this on my website as a teaching point of what happened to her after she was instructed to use a Theragun on her breast to “release a plug.”
This video is also a good illustration of setting the mood in the room. You can hear us chatting about their infertility journey, me pausing to give her more numbing medication, dad giving her encouragement, and her having comfort from her babies being in the room during the procedure. A breast abscess is extremely painful and extremely emotionally upsetting, but it is also very, very solvable and patients get instant relief. So it is important to take time to reassure patients, and work slowly and calmly.


This video shows an analogy of a simple breast cyst (represented by lemonade) versus a fluid collection with breastmilk (represented by yogurt). It’s easy to completely remove simple breast cyst fluid with a needle, but anything involving breastmilk gets stuck very quickly!
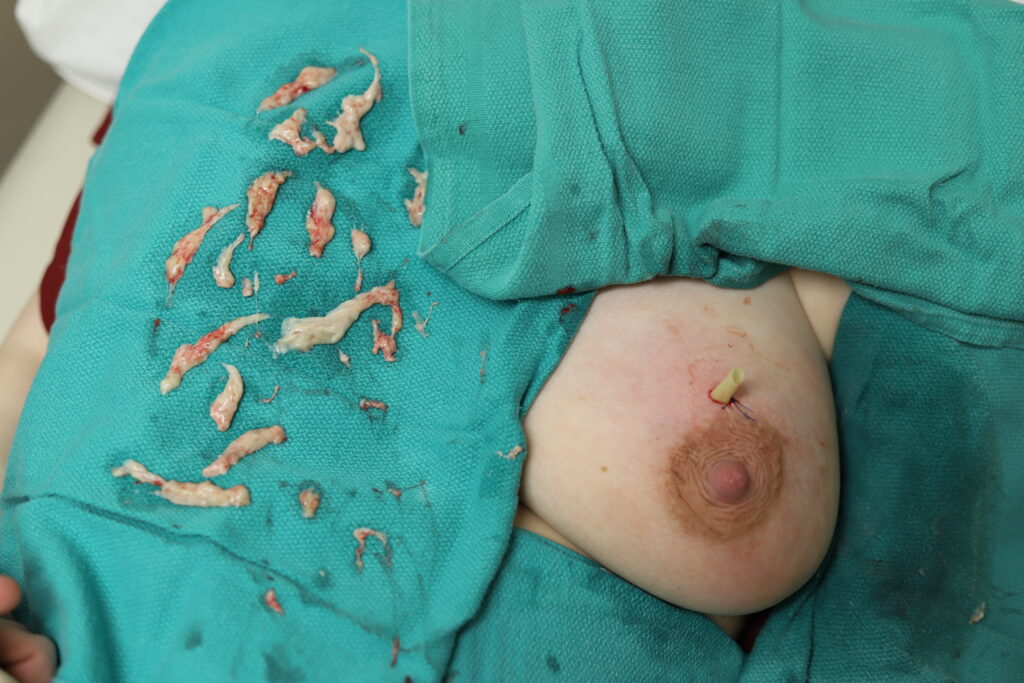



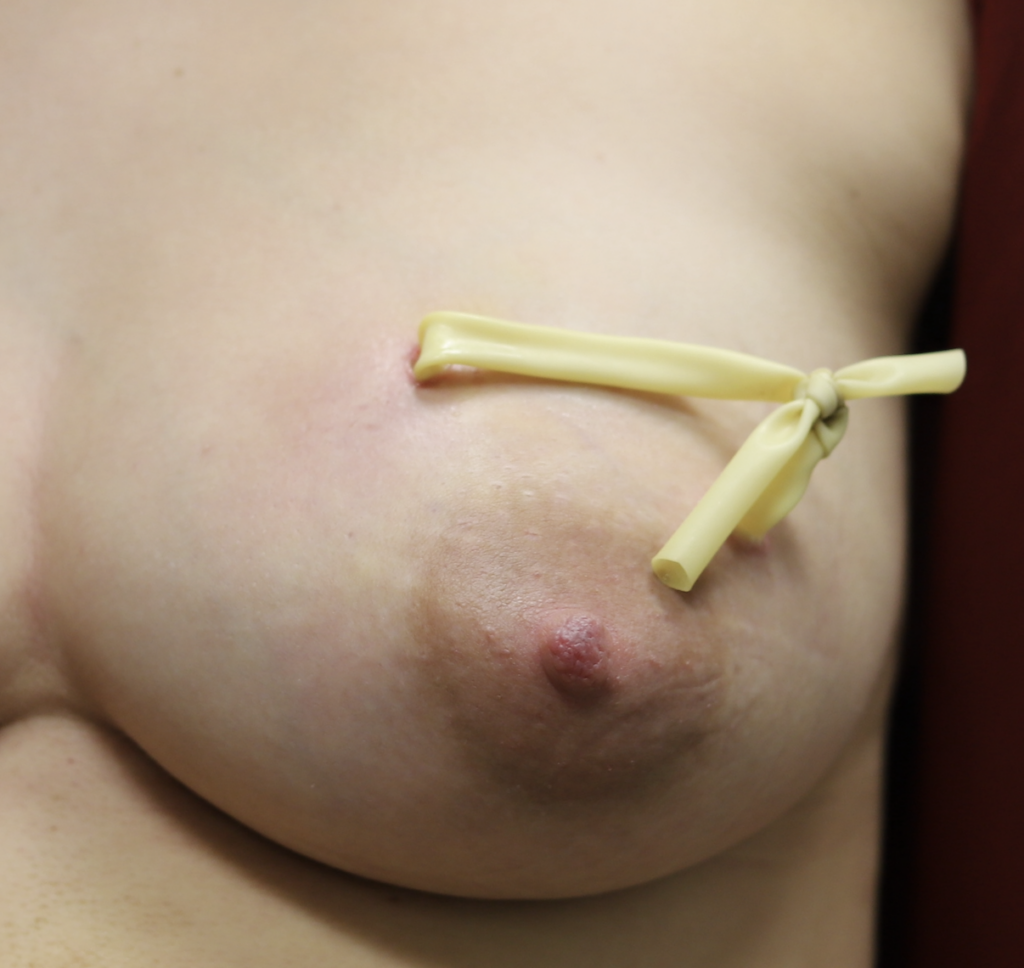
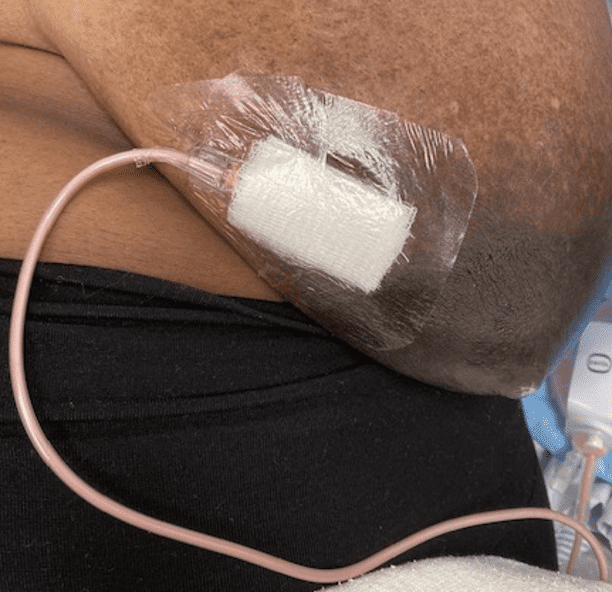
Unfortunately, this patient had such extensive interconnecting chronic abscesses that we had to make two incisions and connect them using this penrose drain. However, this was still a much more ideal approach than making a very large incision on her breast in an operating room and using packing that is painful, does not work with continued breastfeeding, and causes larges scars.
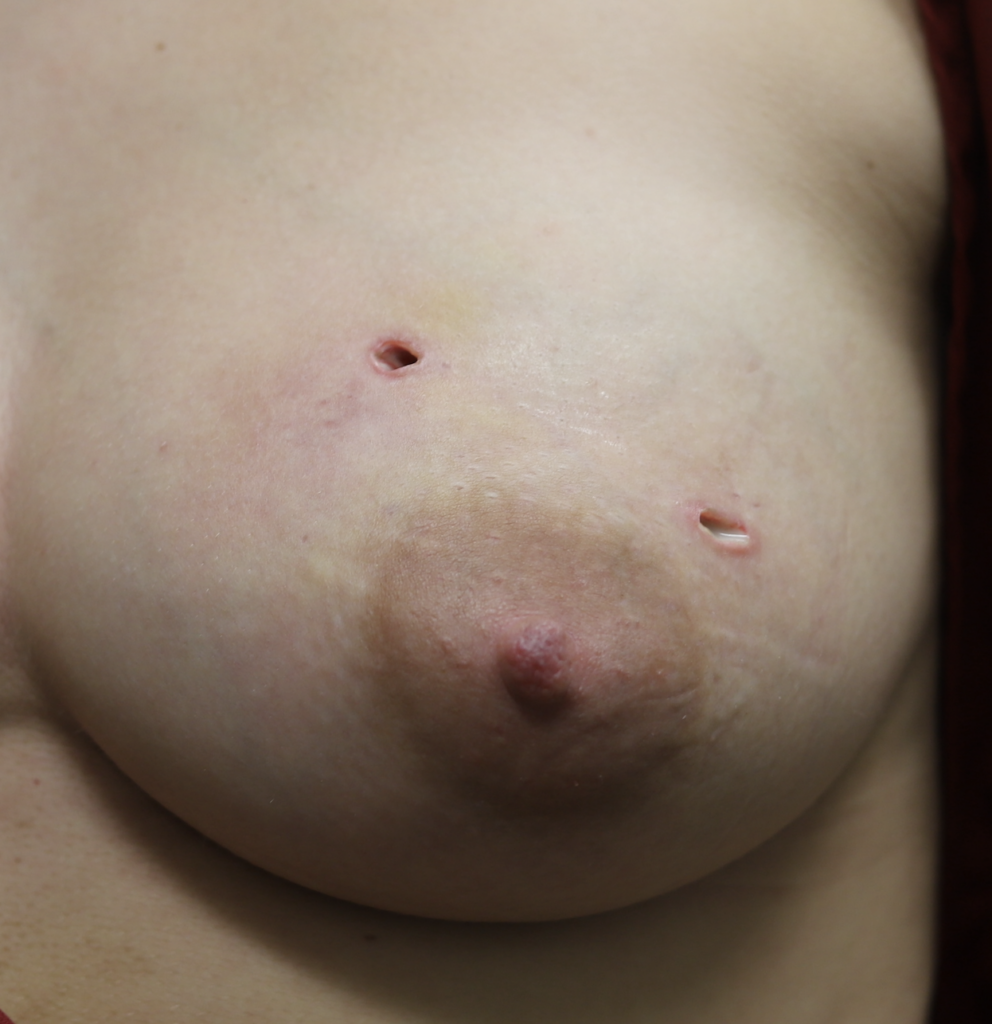
Drain removal – important to note that the pus-like material at the lower drainage site is called “fibrinous debris” and is just the body reacting to having had a drain in it. It isn’t infection.
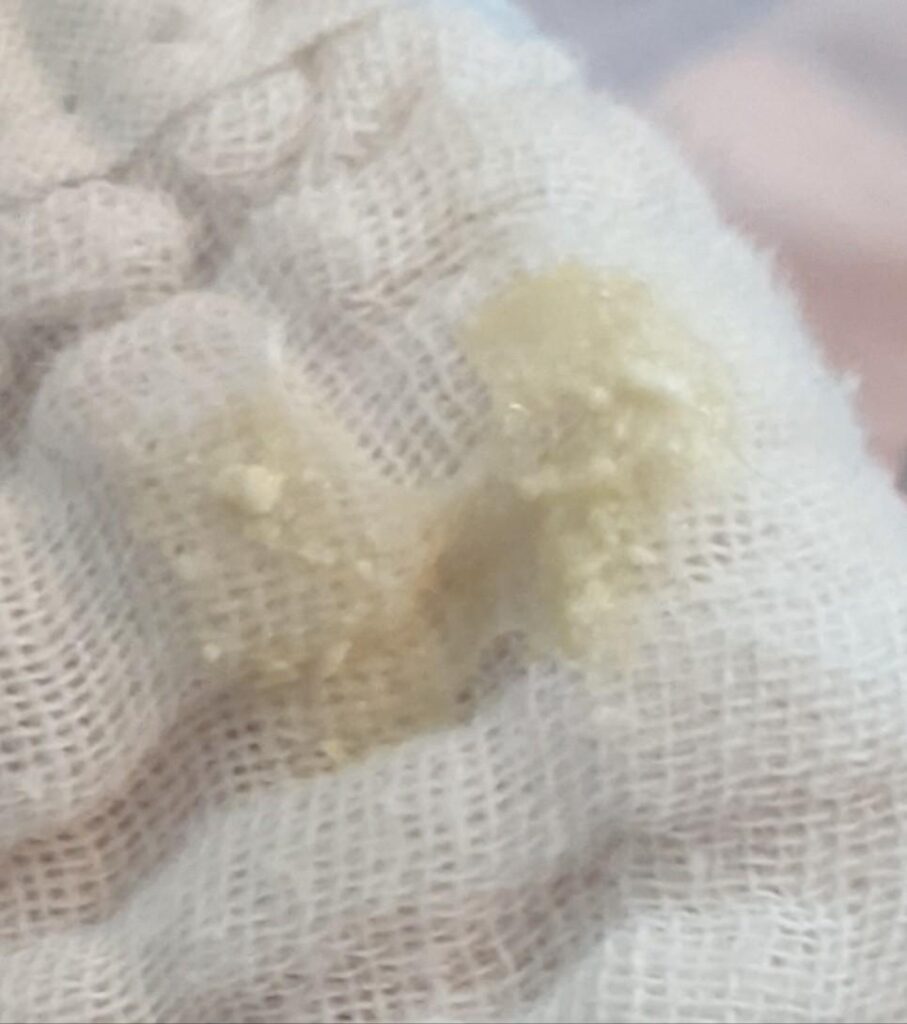
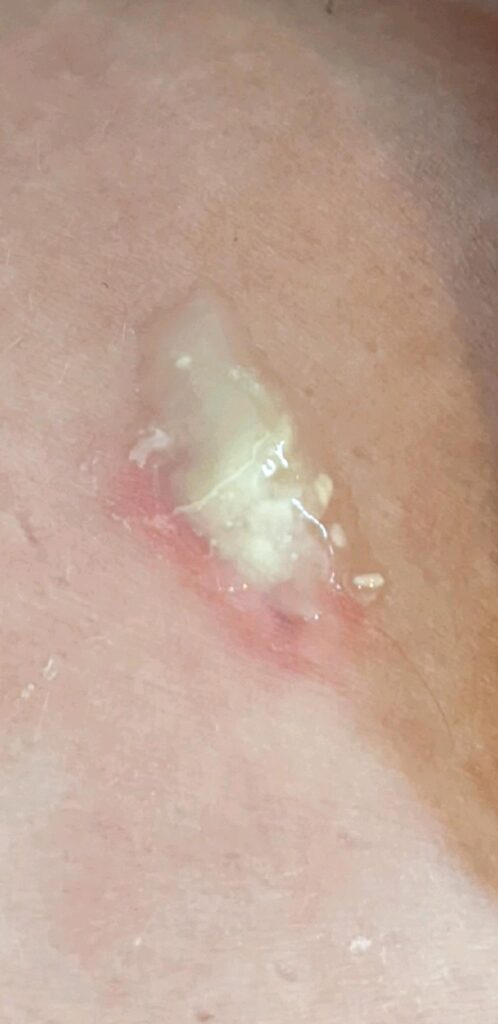

As her inflammation continued to resolve after drainage, her previously damaged breast tissue (dead tissue mixed with old milk) continued to drain — we wanted this for a period of time.
The images below show the presentation of a large area of swelling in the upper part of the patient’s right breast as well as two others in the lateral (side) of breast and below the nipple. This was another consequence of epsom salt soaks, massage, and hospital grade pumping around the clock. This patient needed four drains of separate fluid collections. One area at the 11:00 position of the areola had already started to drain itself before she came to see me:
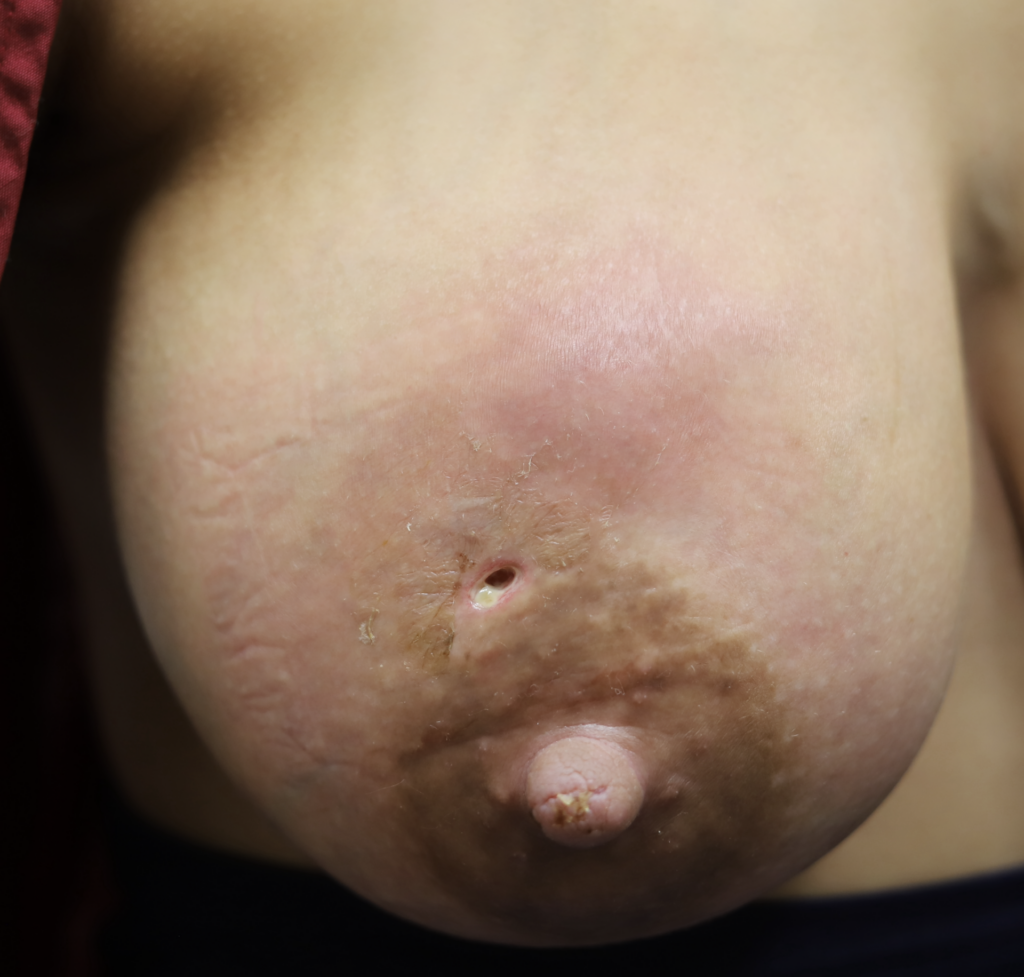
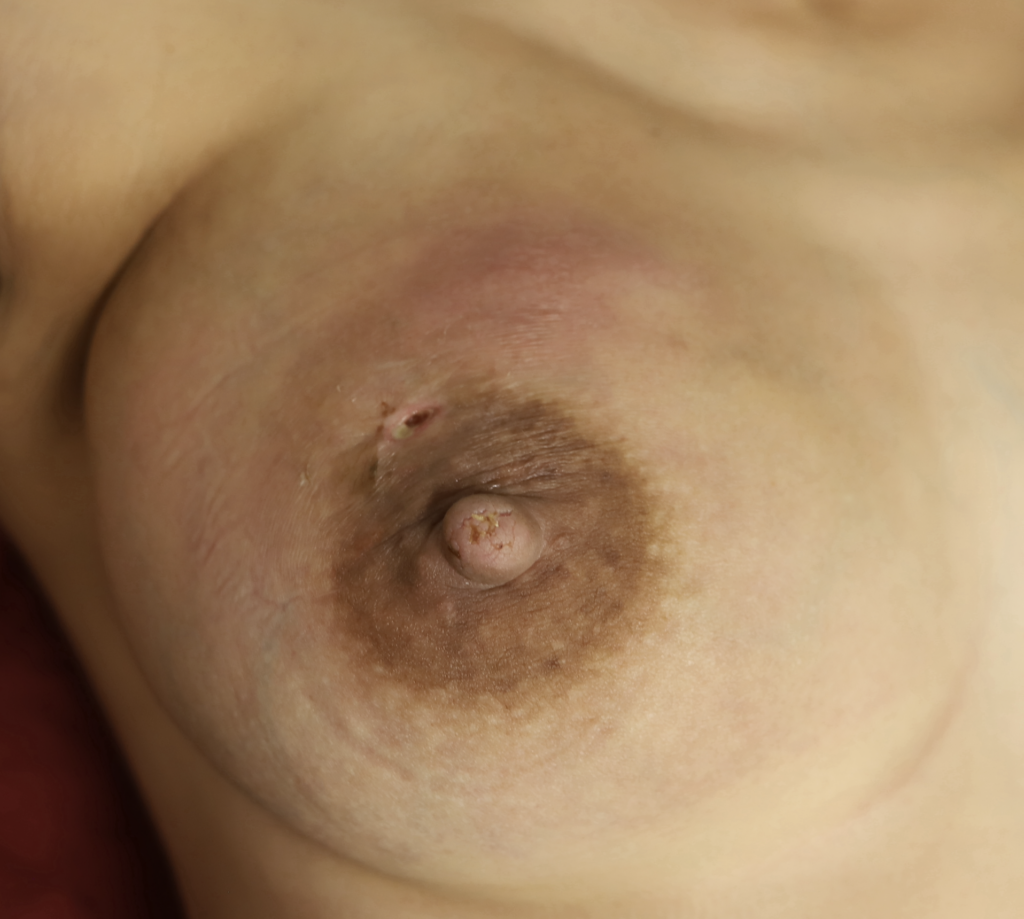
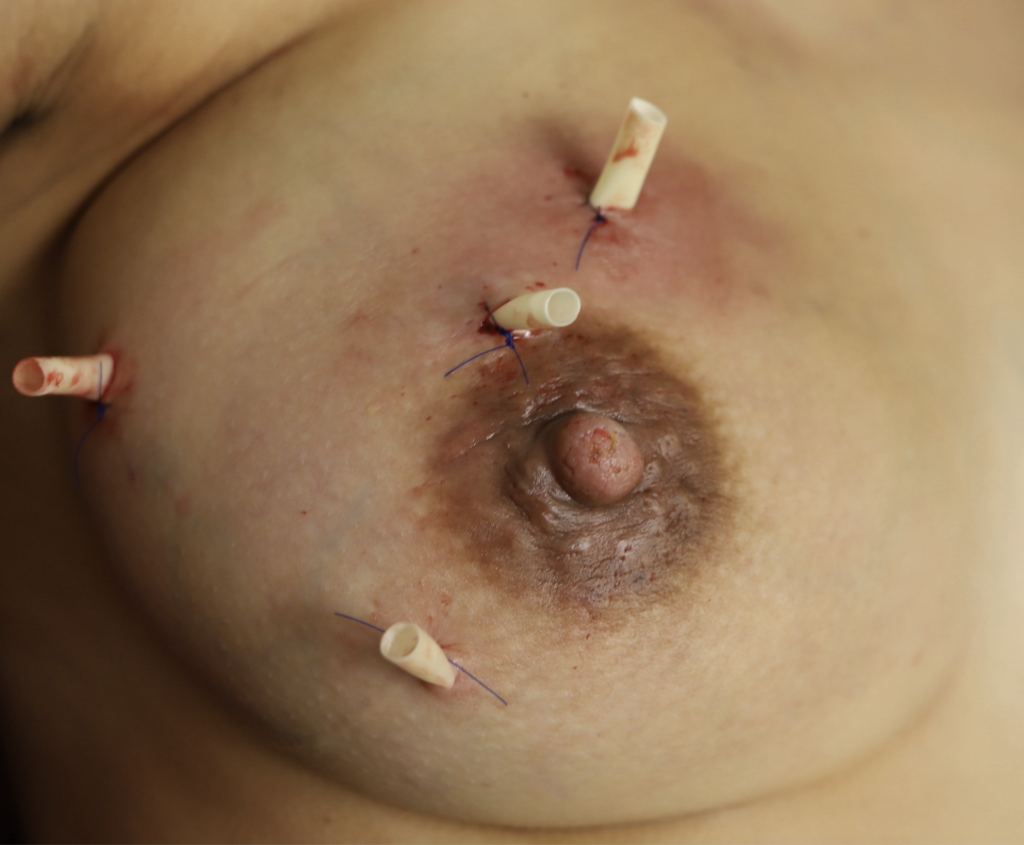
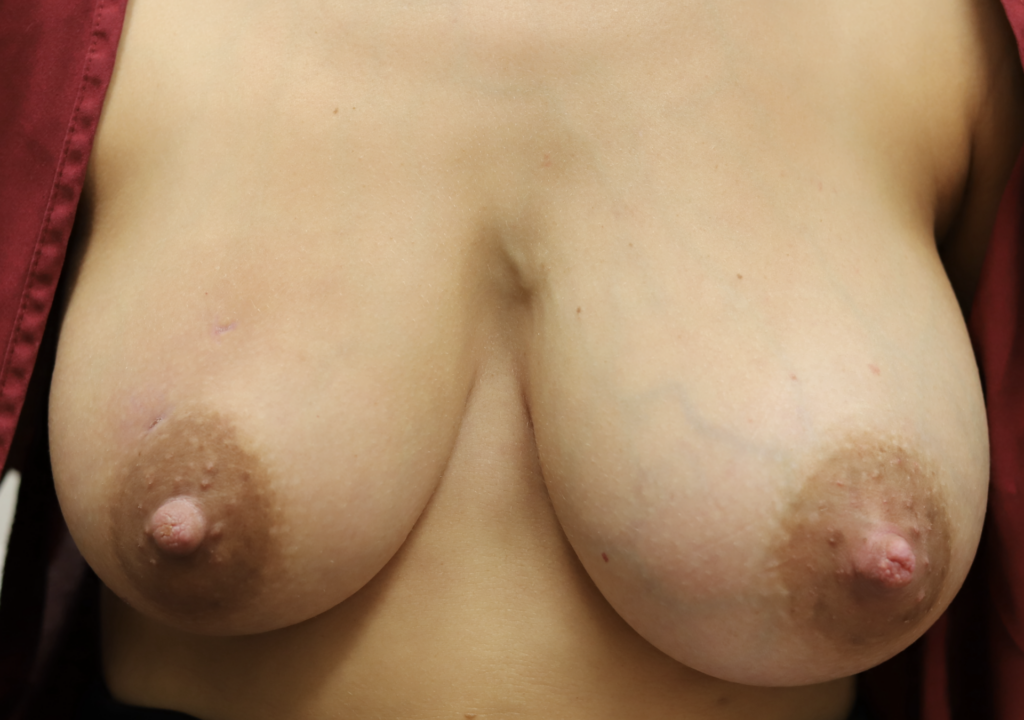


Abscess occurs when a phlegmon coalesces into a discrete fluid collection of pus and milk. This photo montage demonstrates in still frames the content of the Office Drainage of Lactational Abscess video. The drain was removed three days after placement and at one week followup, the incision site was closed.
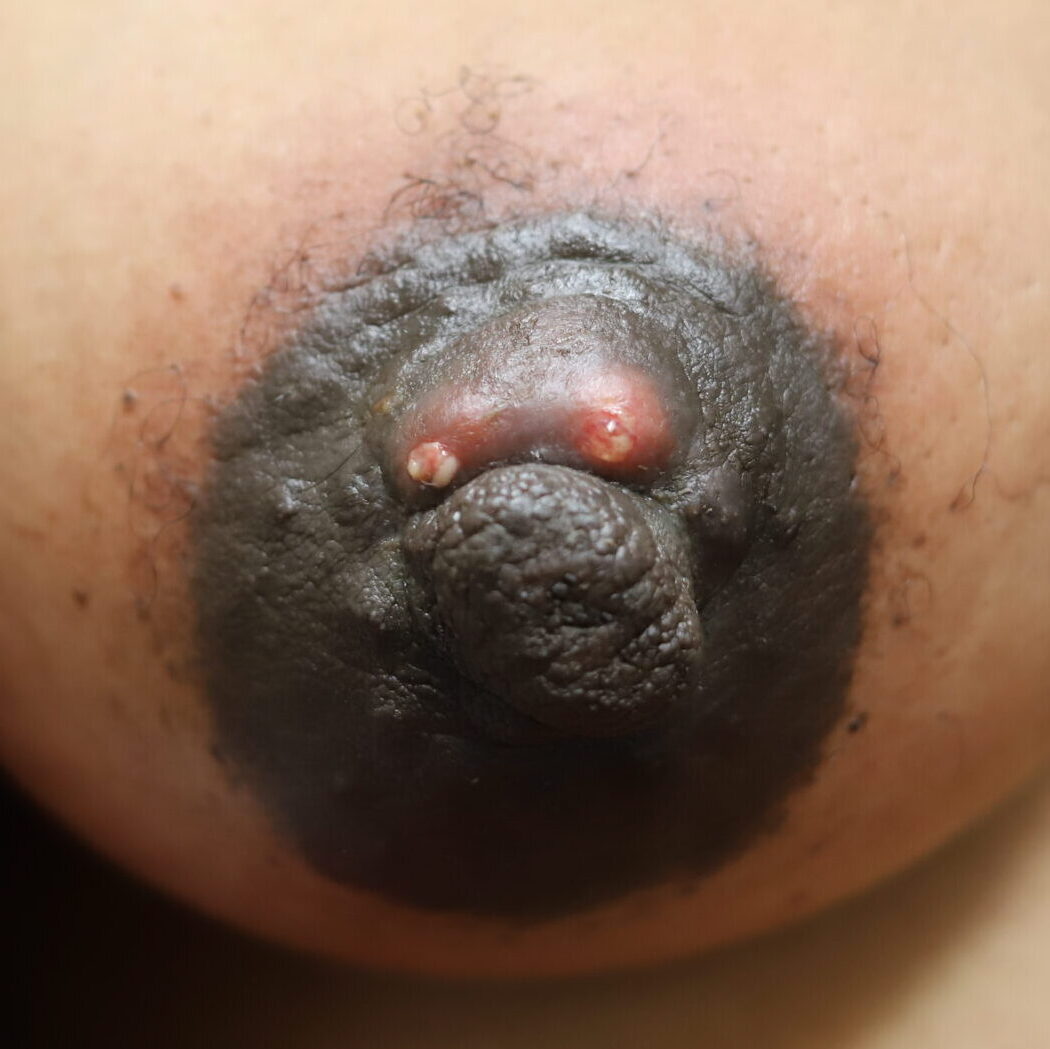
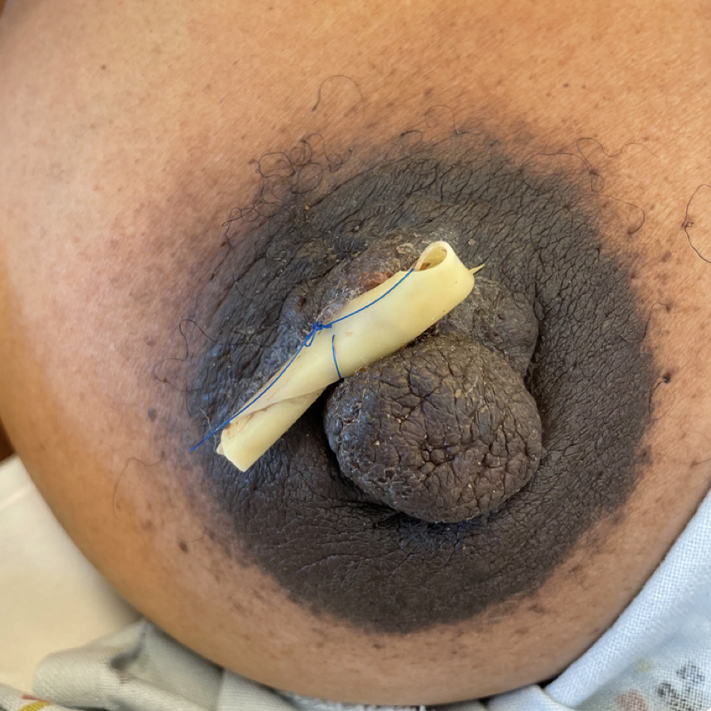
One of the rare situations where a true abscess occurs during pregnancy (this image to the left demonstrating an infected Montgomery Gland, with other pregnancy diagnoses including granulomatous mastitis and periductal mastitis).
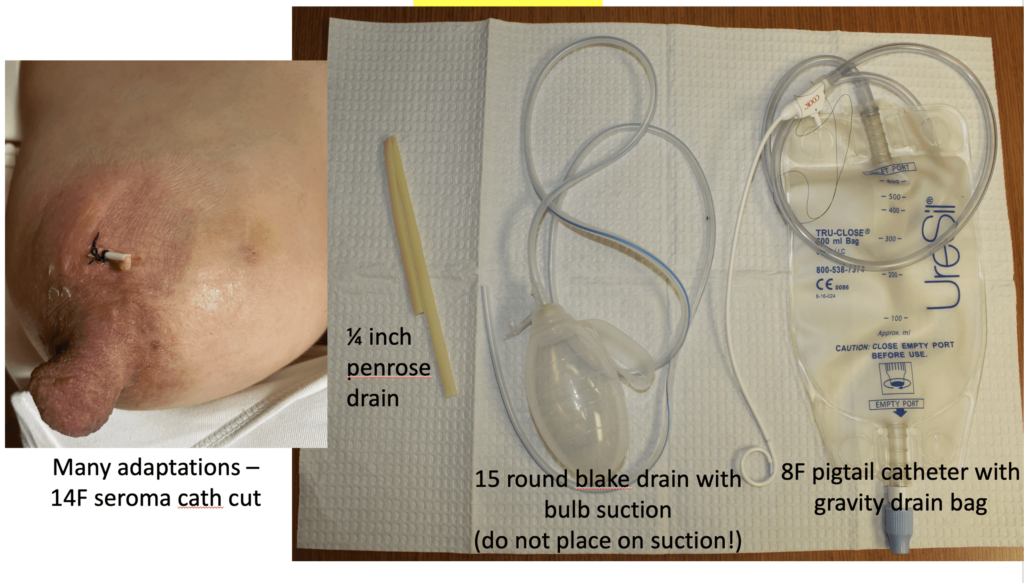
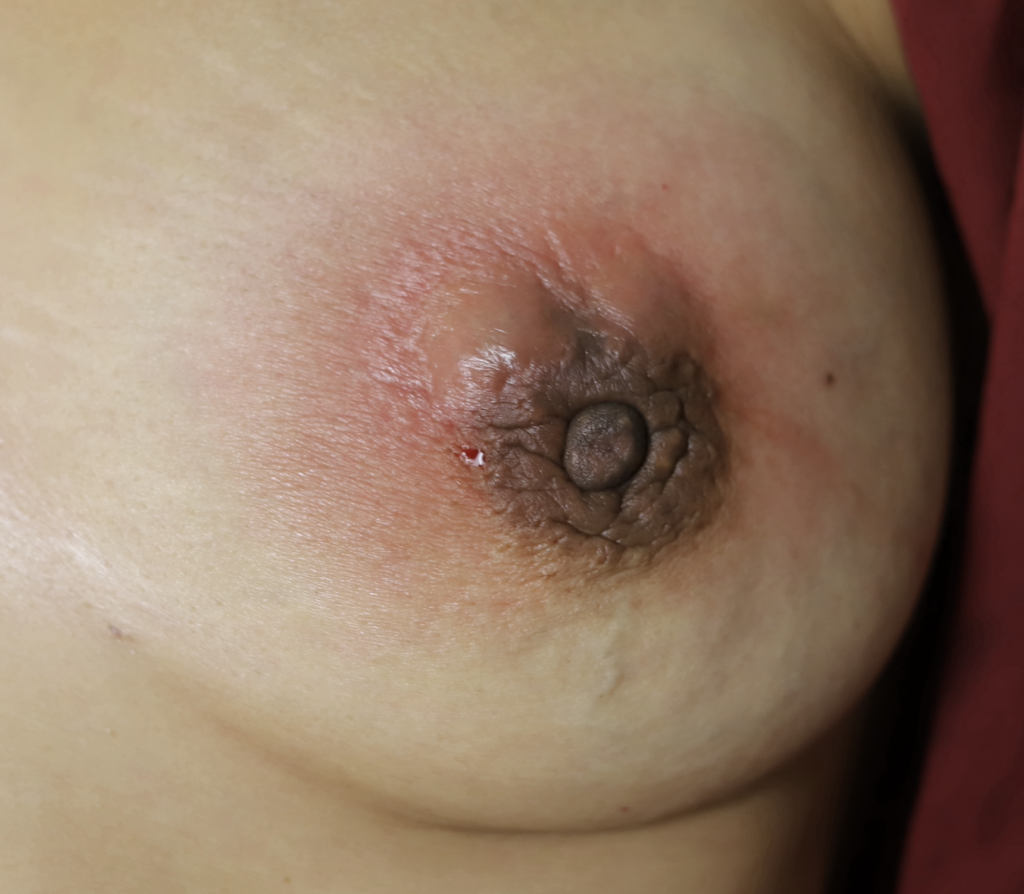
Reason to STOP PUMPING or trying to force a baby to nurse to “empty the milk”: The nipple and areola are extremely inflamed (and painful). No normal flow of milk will occur in this situation. Just like a traffic accident on the freeway, you need to let the inflammation calm down and get adequate drainage of the abscess before resuming feeding. Otherwise, you are just going to back up more cars in the traffic jam and worsen the problem (as what happened with this patient with misguided advice).
Phlegmon
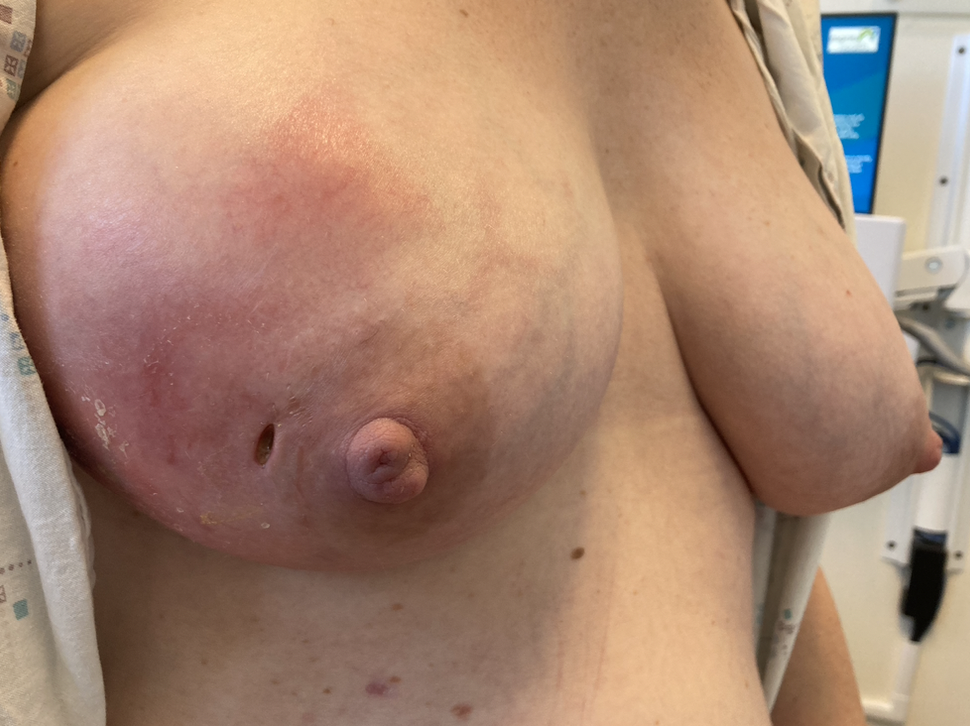
A phlegmon is an indistinct area of tissue inflammation, fluid collection, and inflamed capillaries (blood vessels). It can present with redness overlying the area of massage or it can present with a mass-like area in the breast. Ultrasound should confirm the difference between a phlegmon and an abscess (which is a fluid collection that requires drainage).
Phlegmon are managed with the same principles as plugging and mastitis. They may or may not coalesce into an abscess (drainable fluid). Abscesses will eventually drain spontaneously through the skin or obstruct the nipple region if they are not treated appropriately.
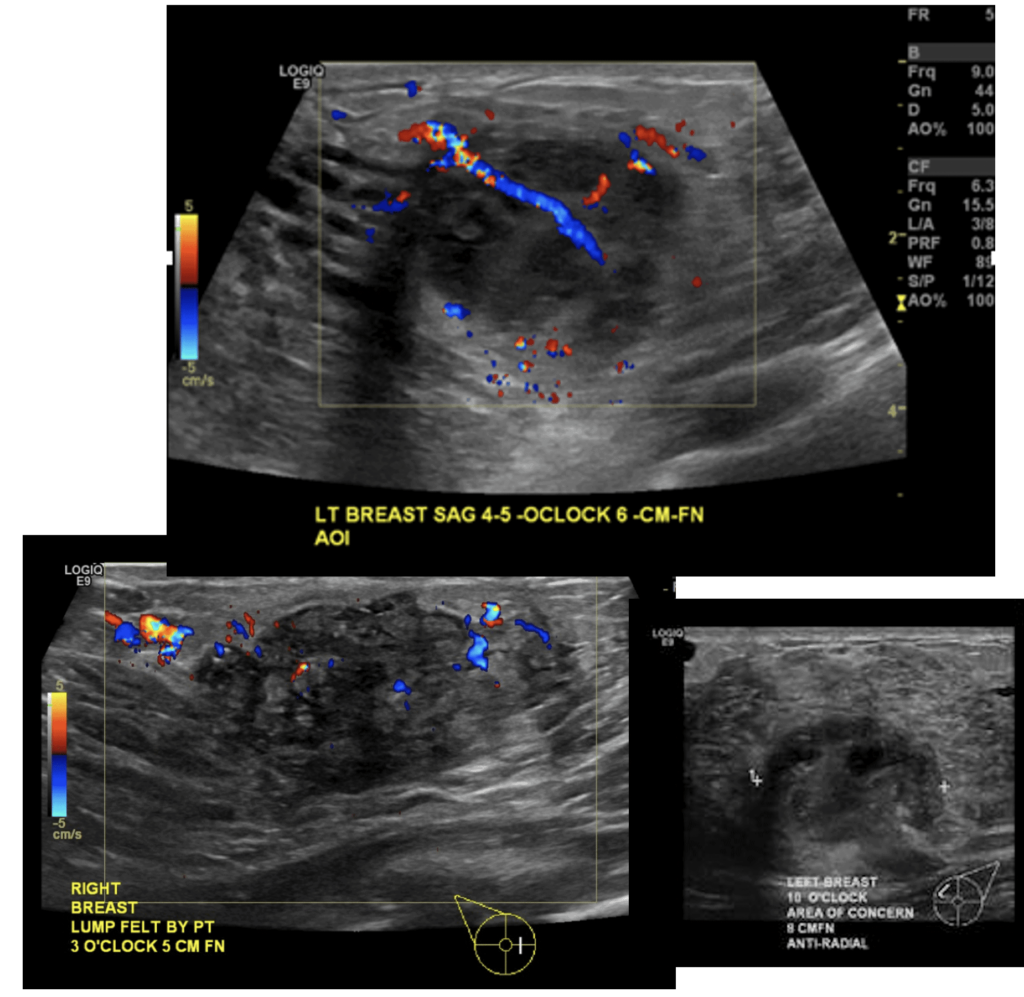
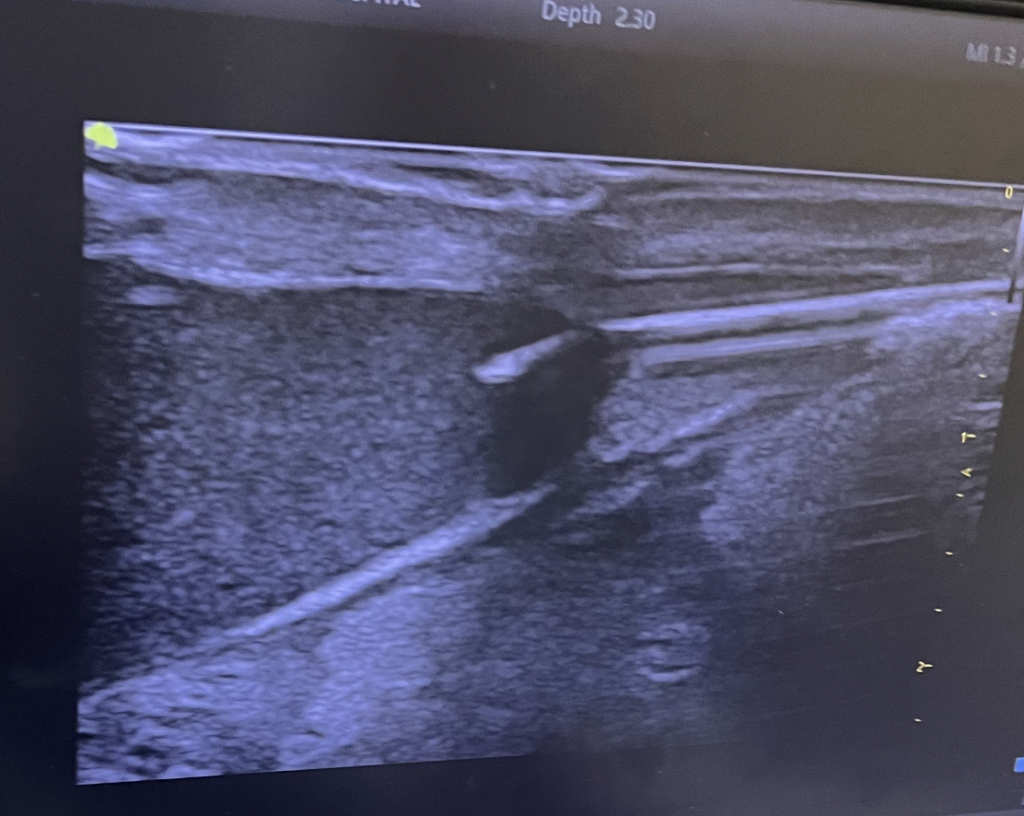
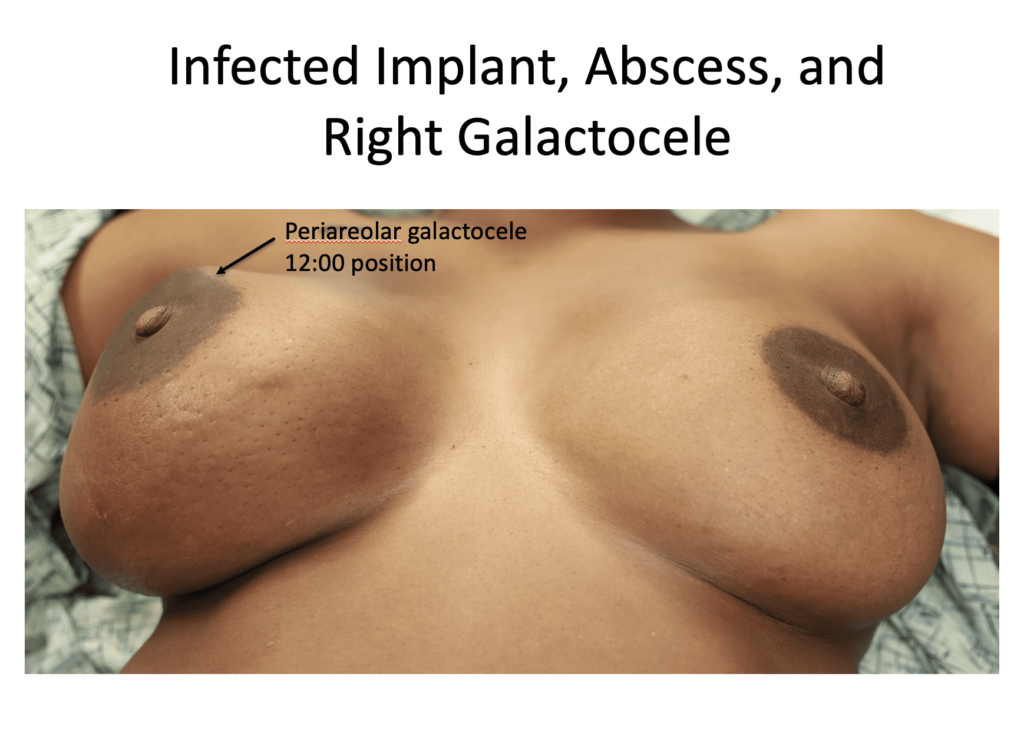
Galactocele
Galactoceles are true milk-retention cysts that develop most often in the setting of hyperlactation and pumping. Whereas early galactoceles may contain more simple milk, more chronic galactoceles ultimately can develop a collection of extremely thick, semi-solid material. They present with most often a painless swelling in a particular region of the breast and should be confirmed with ultrasound. Patients may be recommended to undergo aspiration, but this almost never resolves the collection and it refills quickly. They are drained as above.
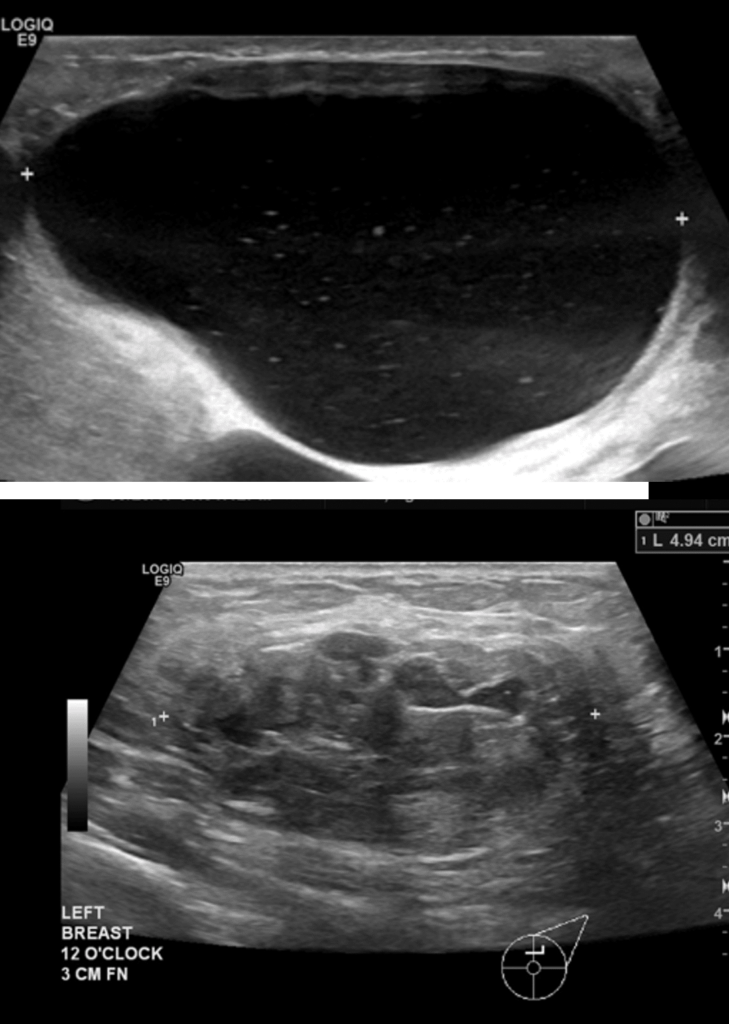
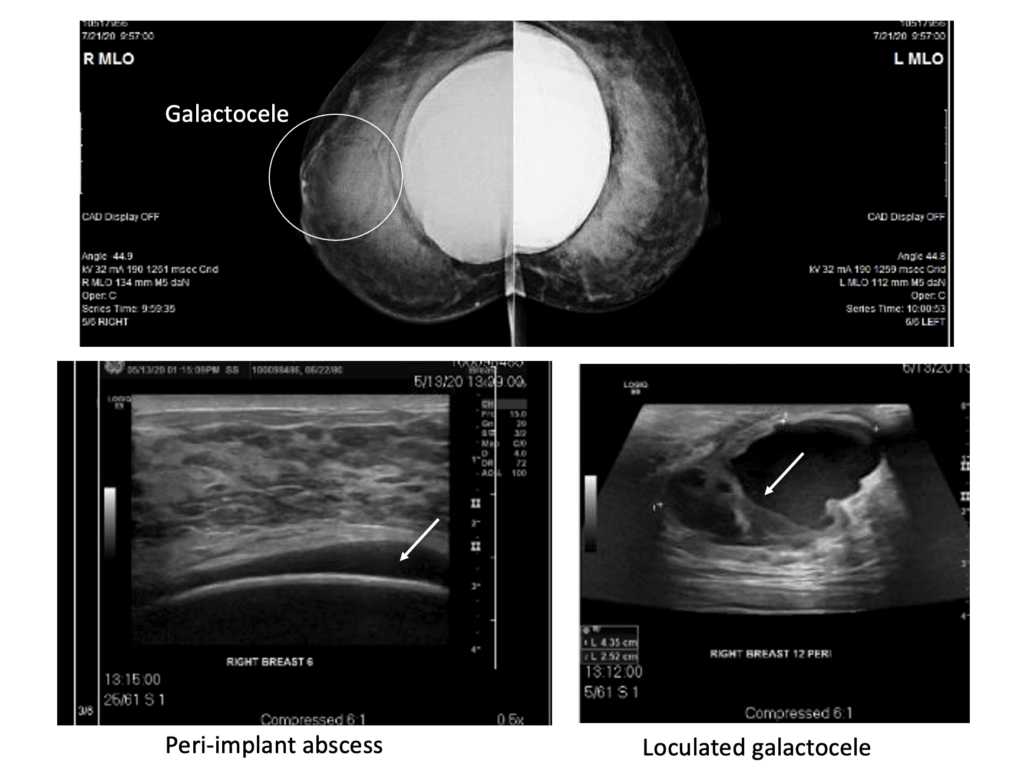
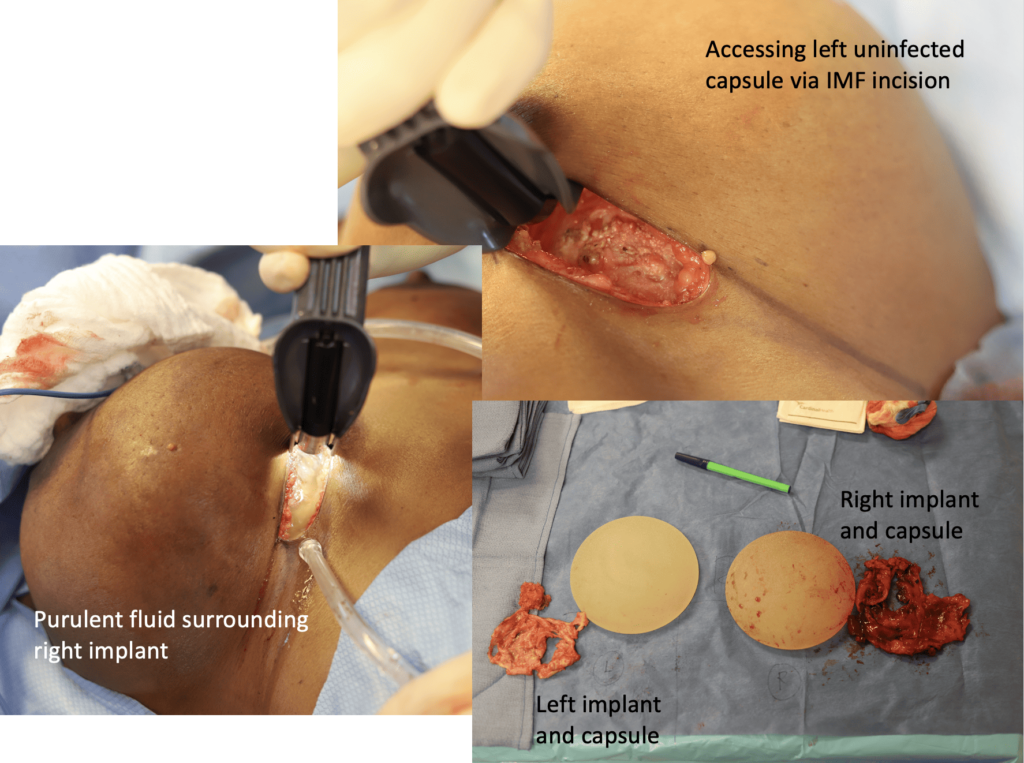
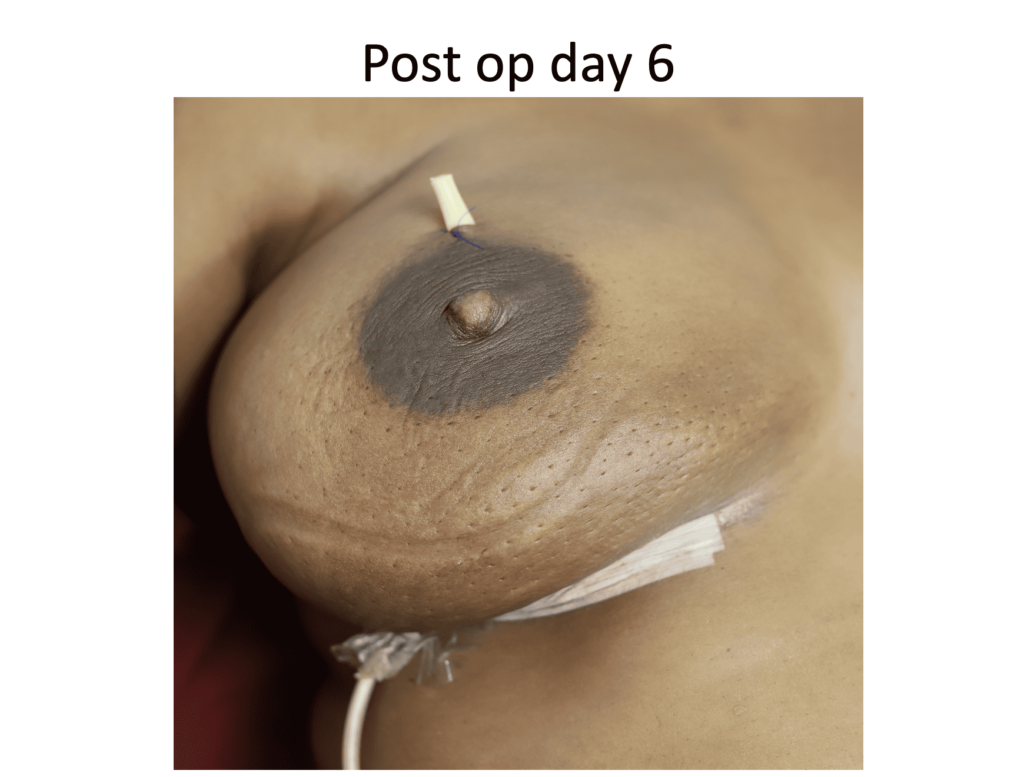
The below series of images demonstrate the unfortunate and unusual infection of a breast implant as a result of countless aspirations of a galactocele rather than definitive drainage. Fortunately, the patient did well and continued to breastfeed for years after this removal of the infected implant. But it was a 100% preventable issue. We detail more of her case in this report in a plastic surgery journal.
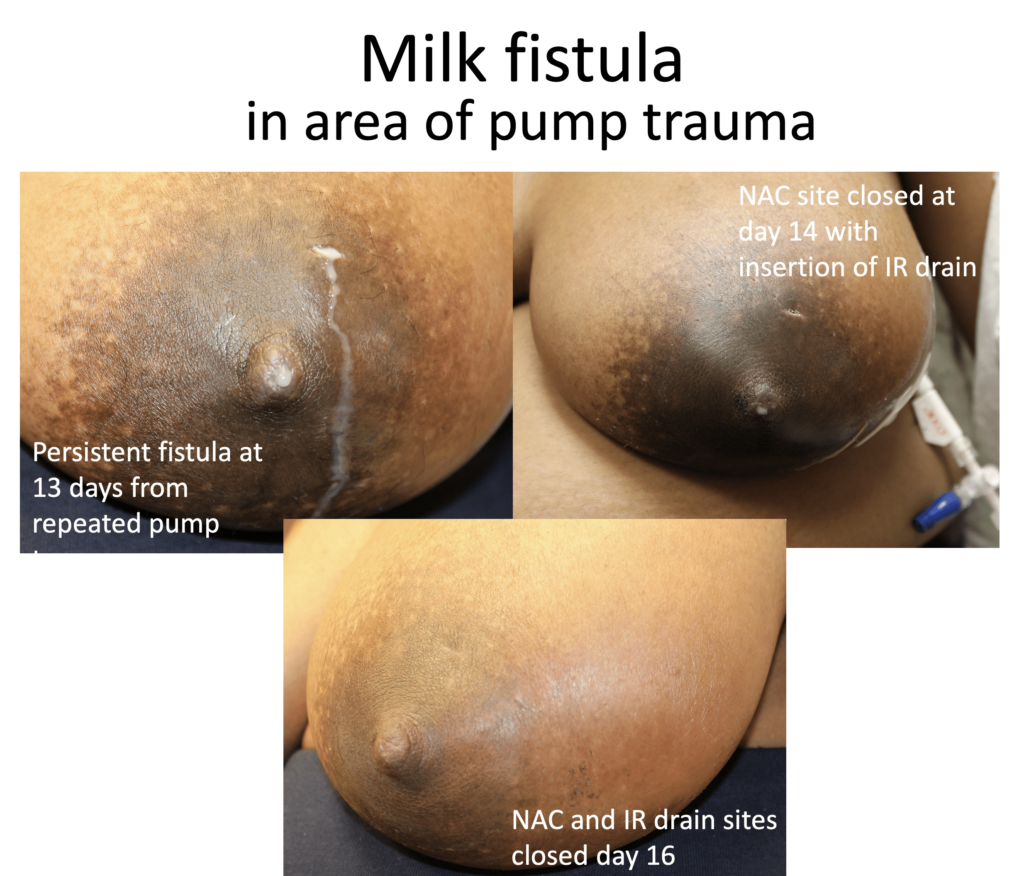
Milk Fistula
Milk fistula, a communication between a duct and the skin, is rarely persistent if managed appropriately. Cessation of breastfeeding is neither recommended nor required. However, to promote early and full resolution, conditions that led to the patient developing a fluid collection that required drainage should be addressed. This includes eliminating pumping or overfeeding, massaging, and hyperlactation. While a short term drain or skin wick is necessary to decompress inflamed tissue for a period of a few days at most, a lactating breast should never be packed with packing tape. Packing tape promotes increased inflammation and prolongs healing time. The packing tape also becomes soaked with breastmilk immediately. Packing can be extremely painful on any part of the body, particularly the lactating breast.