We recently published with the American Society of Breast Surgeons (ASBrS) an Executive Summary of oncolactation, the intersecton of breast cancer care and lactation. Our first and senior author reflection elaborates on future directions.
Depending on the type and size of cancer, and the trimester in which a patient is diagnosed, treatment plans can vary.
Surgery is safe in all trimesters of pregnancy, though operation during the first trimester is associated with increased risk of miscarriage and lower birthweight. It is unknown if this risk is related to the underlying medical condition necessitating surgery or the exposure to anesthesia itself. Chemotherapy for breast cancer is safe in the second and third trimesters, but not the first (due to effect on organ development).
You may want to ask your surgeon or radiologist about putting in a port (a semi-permanent IV that helps chemotherapy be delivered directly without requiring repeated “sticks” in your veins) in a location where the scar will be hidden. This is an example from two patients of mine:
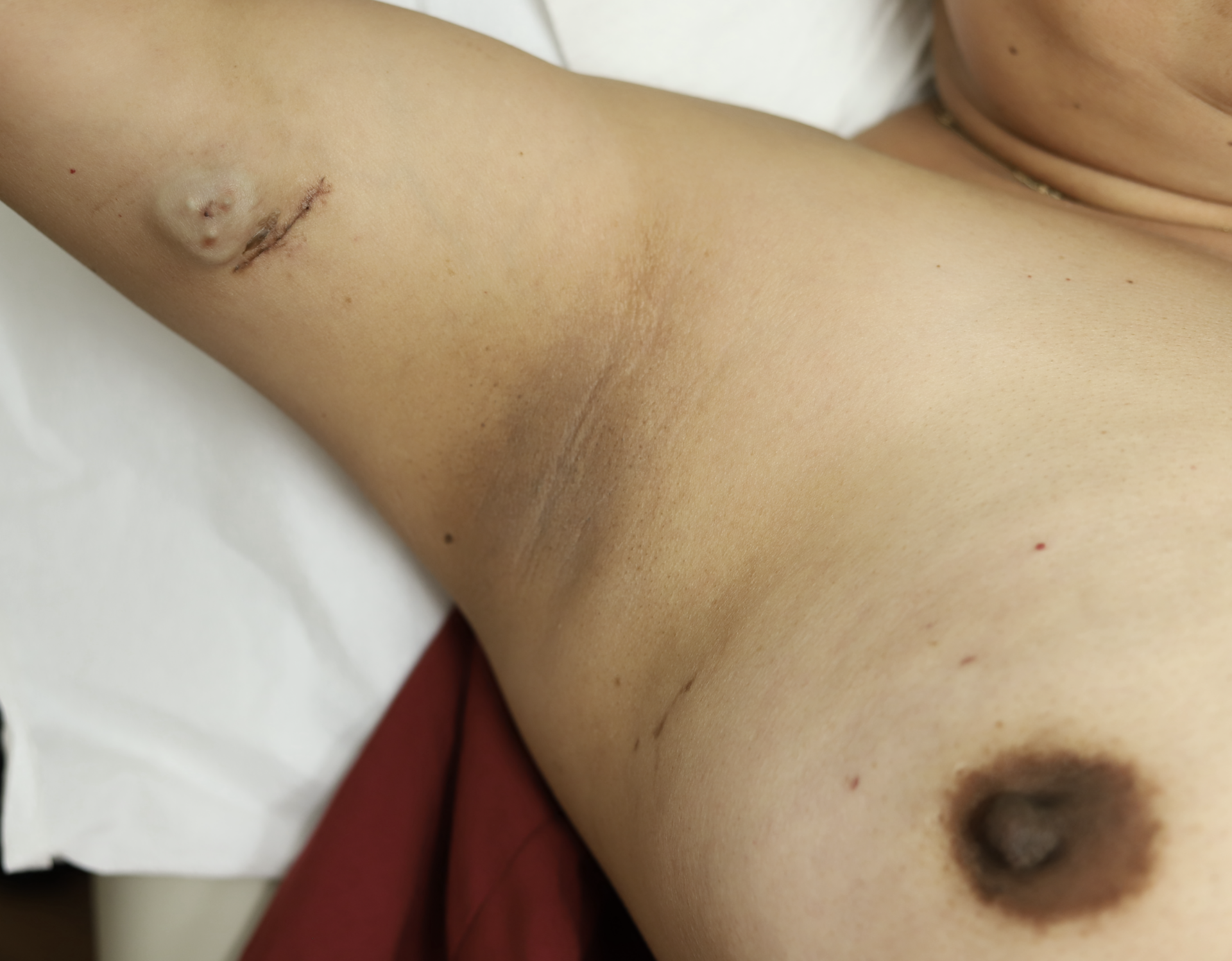
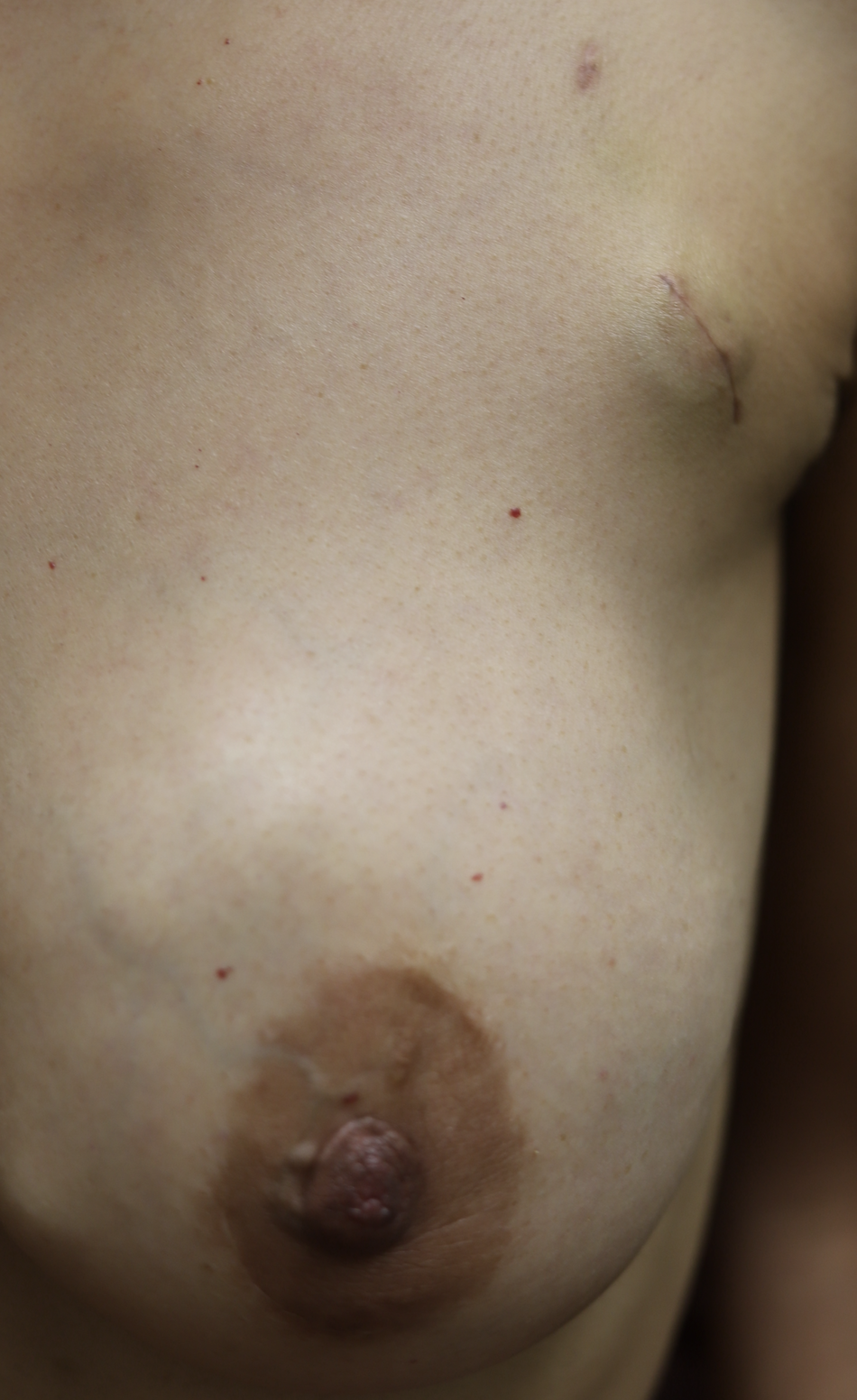
Radiation, endocrine therapy used in estrogen positive tumors, and anti-HER2 immunotherapy for HER2+ tumors are not safe in pregnancy. If a woman is a candidate for a lumpectomy based on the size of her tumor, then time to start of radiation should be considered when making treatment decisions. For example, if a woman undergoes a lumpectomy in the second trimester at 15 weeks pregnant, she would not start radiation for approximately 35 more weeks and she therefore should undergo a mastectomy. Mastectomy is generally recommended in the first or second trimesters for this reason. Lymph node biopsy is safe during pregnancy using technetium, but not blue dye (tracers used to “map” the lymph nodes for biopsy).
Patients who begin chemotherapy while pregnant typically have the systemic treatment interrupted at 35-37 weeks gestational age for delivery and likely will be restarted 3 weeks postpartum. Chemotherapy may impact gland development and milk production postpartum should be monitored. If a mother is breastfeeding another child at the time of her diagnosis during pregnancy, she must be counseled about the need to wean or discard breastmilk once chemotherapy starts. She also should be informed that staging studies as outlined above are safe with breastfeeding.
If weaning is needed, mom can explore formal donor milk options as well as informal milk sharing in her community.
Any other questions related to the idea of pumping during chemotherapy, radiation, and endocrine therapy is addressed in the Diagnosed During Breastfeeding section of this website.