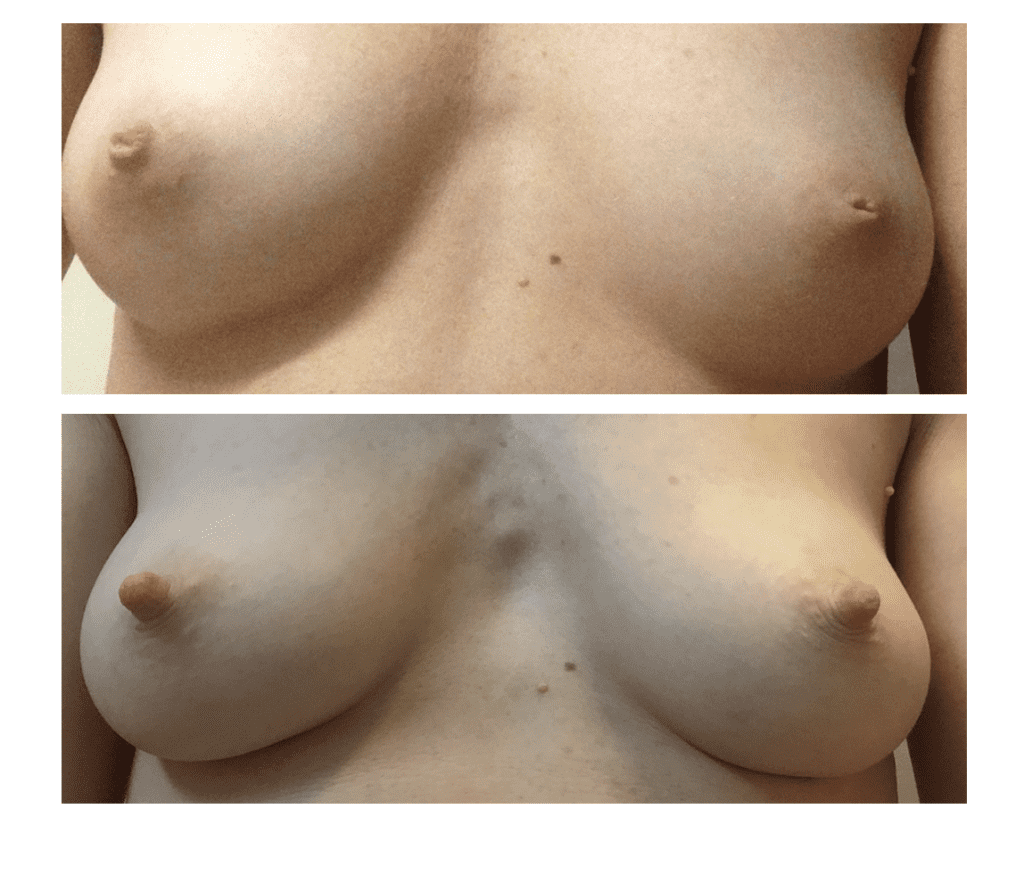
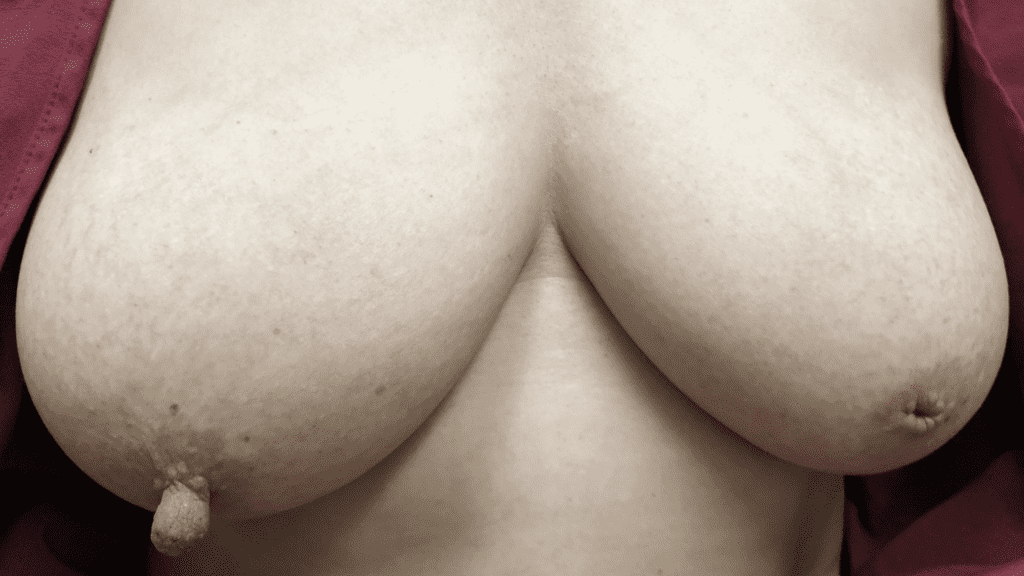
General Considerations for Plastic Surgery and Breastfeeding
It is possible to breastfeed after plastic surgery such as breast reduction, breast lift, nipple procedure, or augmentation. However, glandular tissue, blood supply, nerves, and/or the nipple and areola may have been disrupted during or affected by these procedures, and careful evaluation by a breastfeeding medicine specialist is recommended. It is very important to understand individual anatomy and why patients underwent a plastic surgery procedure.
Discussion with patients regarding prior history of plastic surgery should include background information about why patients elected to undergo a procedure. For example, patients may offer a history of markedly asymmetric breasts, which can be more common in a tubular breast deformity (also called insufficient glandular tissue (IGT), or hypoplastic breast tissue. These patients may undergo augmentation and/or mammaplasty and mastopexy. The ultimate cosmetic outcome may not reflect the presence of previous tubular breast appearance.

The impact of procedures on the mechanical aspects of breastfeeding also should be considered. For example, very large augmentations may produce difficulty with obtaining a physiologic latch and may potentiate nipple trauma and pain. Surgical techniques also can influence future lactation, including technique of parenchymal resection, location of incisions and closure, types of implants, and varied approaches to nipple areolar complex procedures.
Nipple Piercing and Tattooing
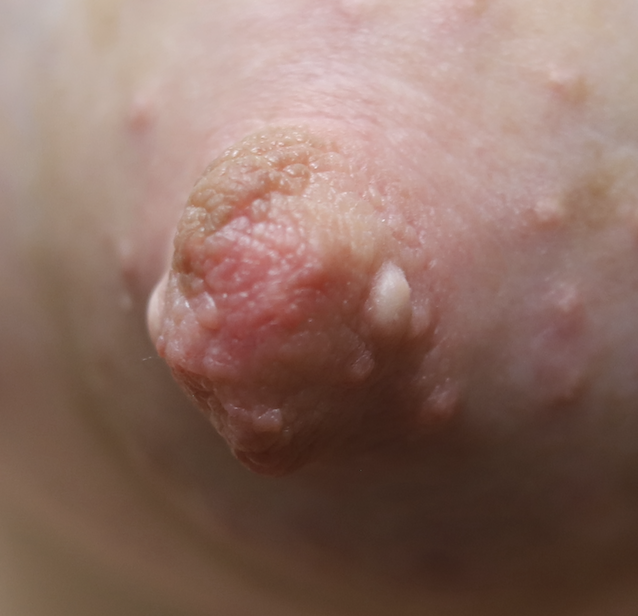
Patients with a history of nipple piercings should remove piercings during pregnancy since the nipple will hypertrophy (grow) and the piercing may be difficult to remove later. Depending on the type of piercing and how impacted the nipple ducts are by the procedure, breastfeeding experience can be variable. On occasion, with very small nipples and very large piercings placed prior to full nipple development, it is possible that the piercing damages a significant amount of ductal tissue in the nipple and may obstruct milk outflow. Tattoos on the breast and nipple are safe with breastfeeding.
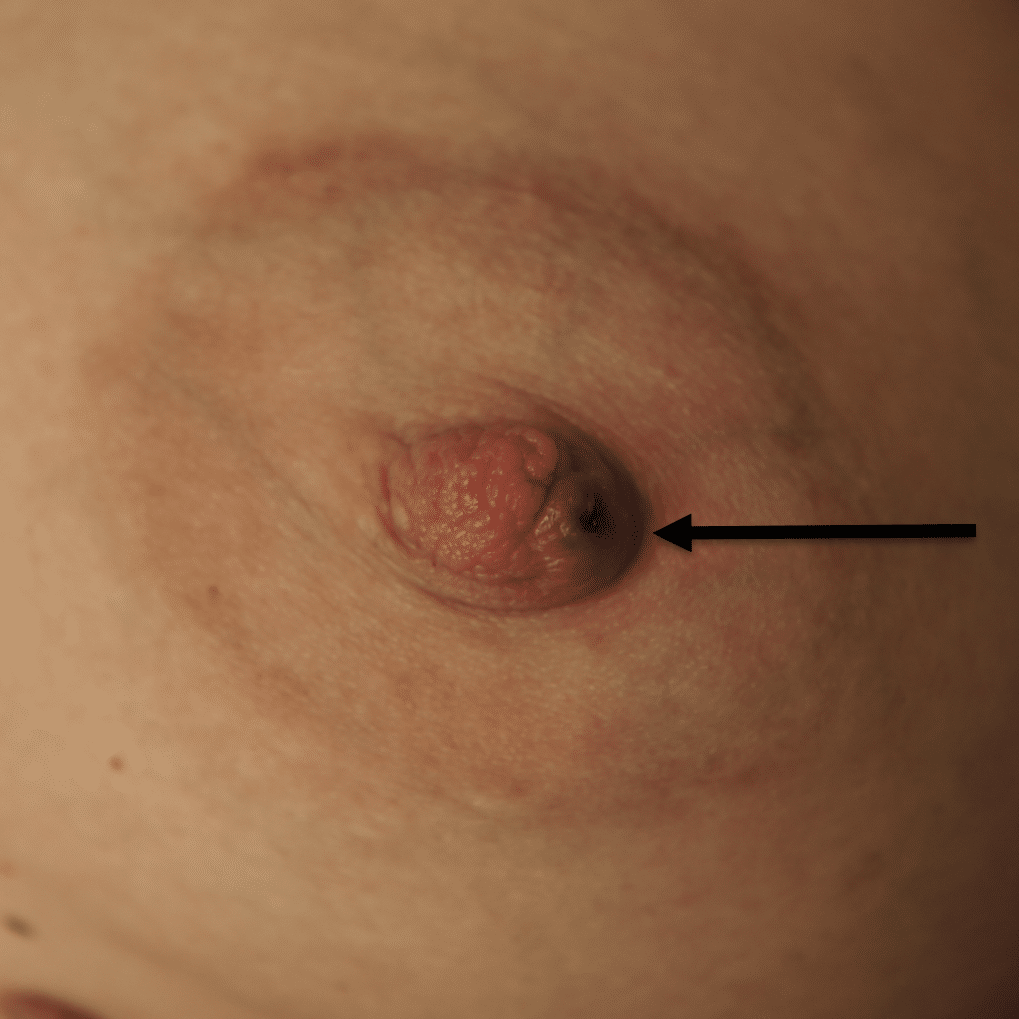
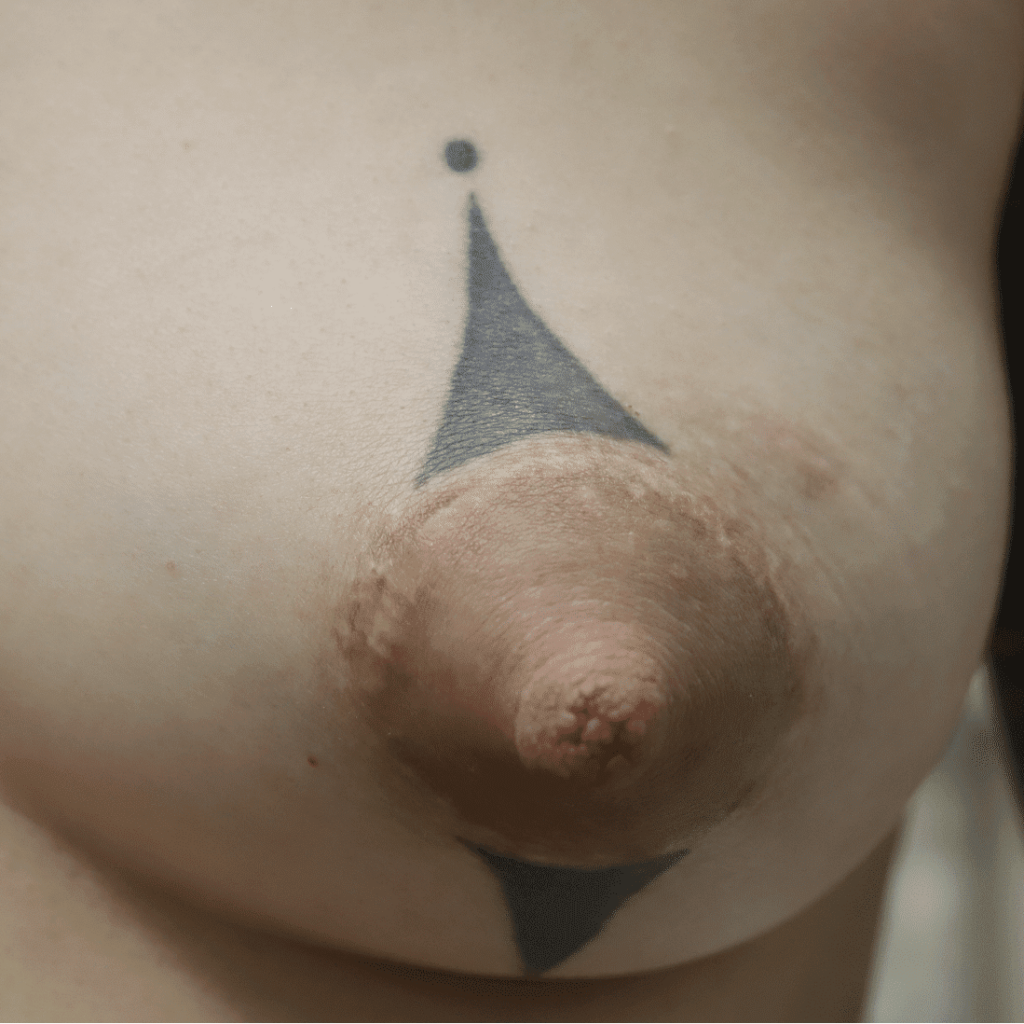
Breast Reductions
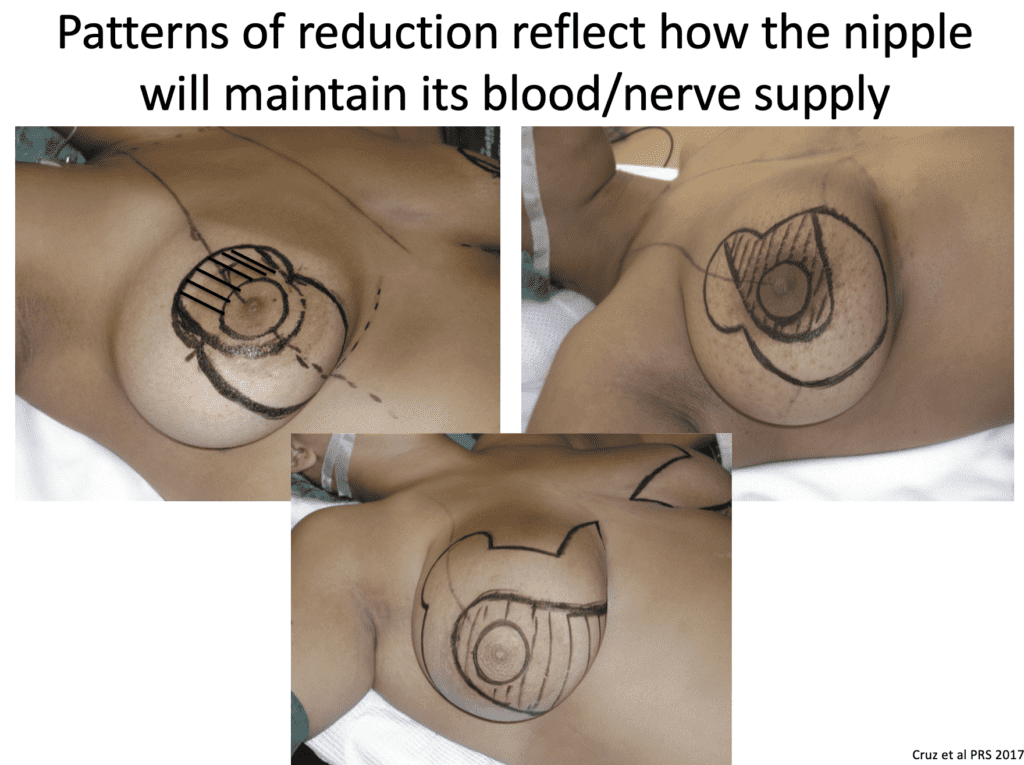
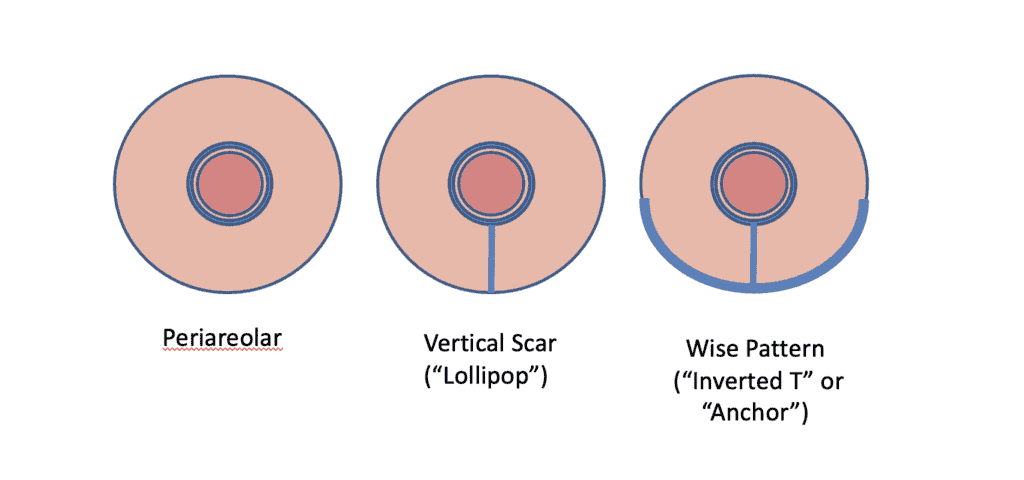
The major considerations with breast reductions (“reduction mammaplasty”, with or without concurrent breast lift or “mastopexy”) are the choice of surgical pedicle (part of the breast that remains intact with blood flow and nerves) and whether the nipple was removed and re-implanted (“free nipple graft”). Free nipple grafts are performed much less commonly today than in the past.
Multiple factors affect how breast reductions impact breastfeeding, and unfortunately the data is poor:
- Studies do not control for factors that otherwise impact breastfeeding, such as diabetes, obesity, and lack of prenatal and postpartum support.
- Studies also do not control for surgical technique, volume of breast removed, or age at which the reduction occurs.
- Further, the lactation world often significantly overestimates the impact of innervation disruption as a result of breast reductions. In fact, it is multifactorial and much more related to scarring and blood supply alterations. The nipple has multiple overlapping nerves contributing to sensation and function, and nerves can even regenerate over time.
To guide women appropriately, we need prospective trials on this topic that would capture this information:
- Follow patients from the time they are counseled regarding the procedure
- Record all pertinent operative details such which part of the gland is preserved and whether the nipple is removed and replaced
- Offer standardized prenatal counseling and postpartum lactation support
- Determine a clear definition of “successful breastfeeding,” including volume of milk produced, exclusive breastfeeding versus requiring supplementation, and duration.
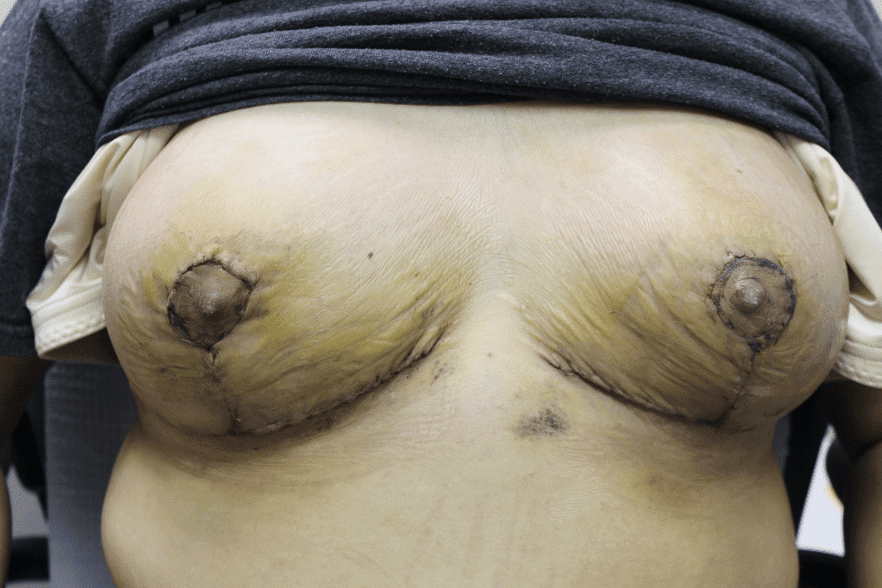
Breast reductions are a life changing procedure, including resolution of back and neck pain, bra grooving, chronic intertrigo (yeast infection on the underside of large breasts at the bra line), and pain and depression. Therefore, I do not discourage this procedure if it is strongly desired by patients and I explain the limitations of our current data and the need for careful support in the peripartum period.
Patients may express remorse regarding a past breast reduction. While these emotions are valid, studies document similar breastfeeding rates between unoperated macromastia and patients with a history of breast reduction. Untreated macromastia (large breasts) decrease breast and nipple areolar complex sensation, and can present difficulty to obtaining a deep latch and effective milk removal. Further, obesity represents an independent risk factor for poor breastfeeding outcomes, and no current studies on reductions and lactation control for groups with similar body mass index (BMI).

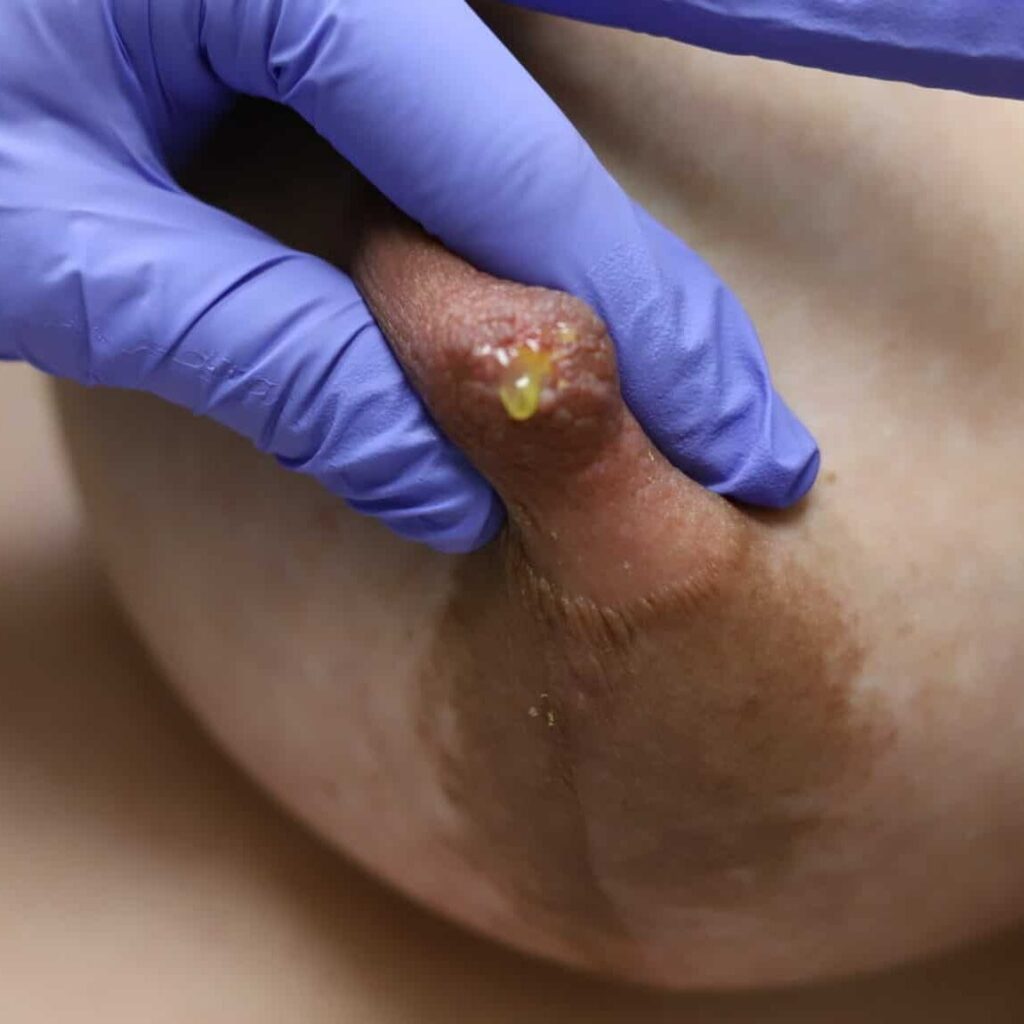
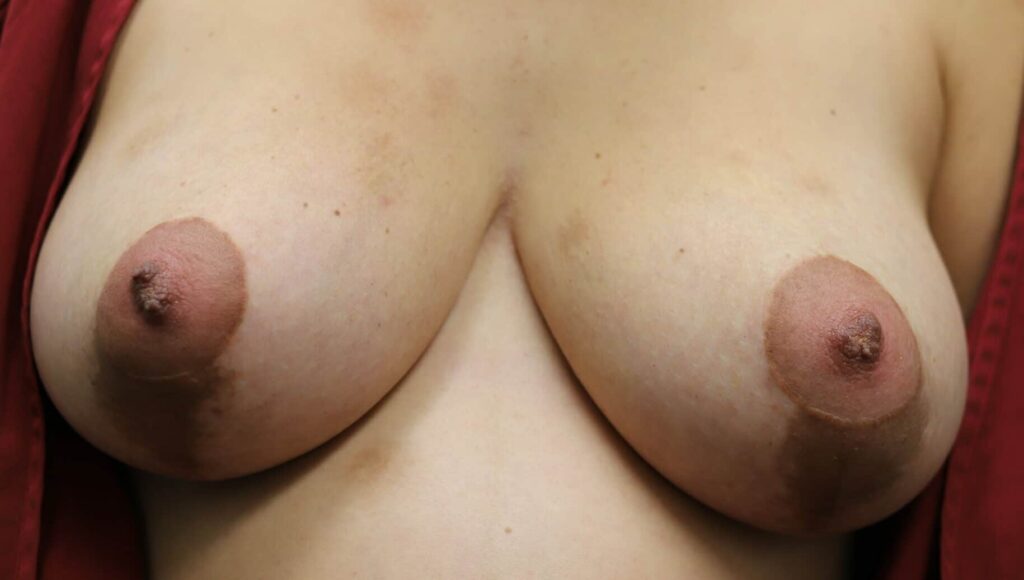
For example, in a hypothetical situation, this mother could undergo a long labor induction with significant amounts of intravenous fluid. This fluid would add to her natural postpartum engorgement and make her nipples appear even more “flat.” Babies that are born after long labors and epidural medication often are “sleepy” and can struggle to latch despite breast size or nipple shape. Moms are given a nipple shield for a “sleepy baby” and “flat nipples.” Babies then nurse from a nipple shield — which is like a pacifier at the breast — and often does not result in milk transfer nor stimulation of the breast tissue.
In this situation, babies can loose excessive weight and mom’s breasts are not stimulated in the critical early postpartum days. They are instructed to start supplementing and mom’s breast reduction is blamed.
These situations are 100% avoidable with prenatal counseling, assessing colostrum production, and teaching hand expression. It is much more beneficial for a mom to hand express postpartum and provide this to a sleepy infant than to introduce a nipple shield that results in multiple complications for both mom and baby.


Breast Augmentation (Implants)
Breast augmentation (breast implant) is the most common plastic surgery procedure worldwide. If it is for purely cosmetic purposes, I counsel patients to avoid until childbearing is complete. If it is for reconstructive purposes with a congenital deformity in the breast, then it may be more necessary at a younger age. Unfortunately, it is clear that augmentation impacts breastfeeding negatively.
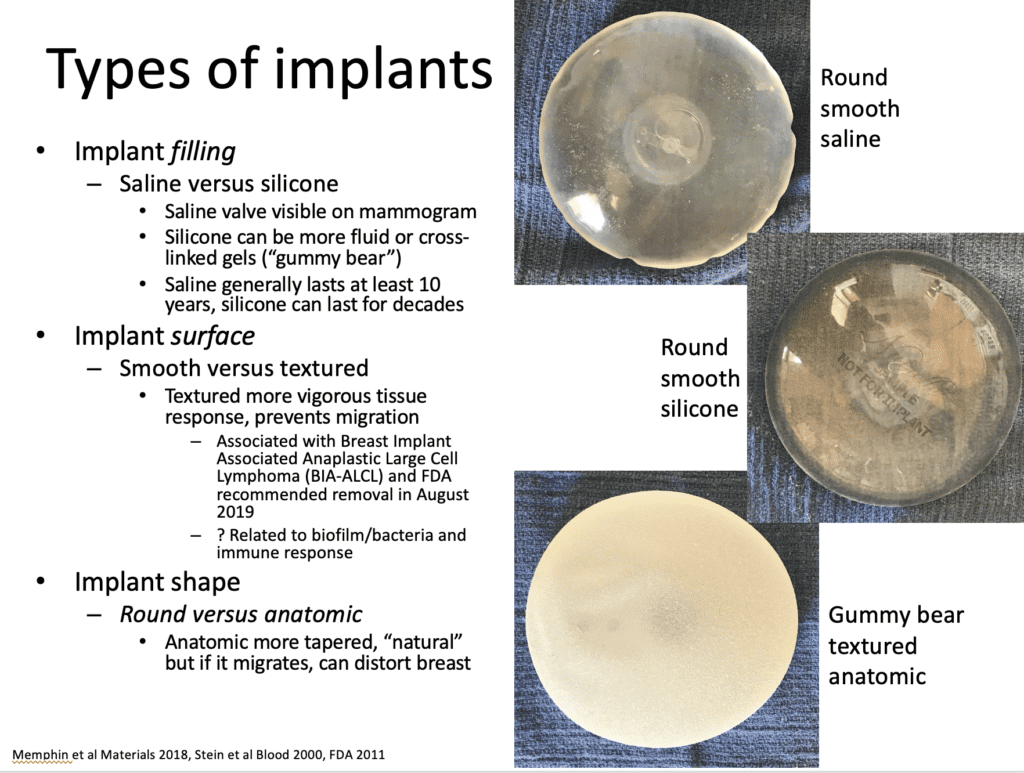
Information helpful to know about the procedure includes the following: size of implant, location of implant, location of incisions, and type of implant. These factors may individually and collectively affect lactation. Surgery can affect ducts and glandular tissue. All implants result in formation of a surrounding reactive capsule, which can undergo “capsular contracture” with resulting pain, breast distortion, and loss of elasticity.
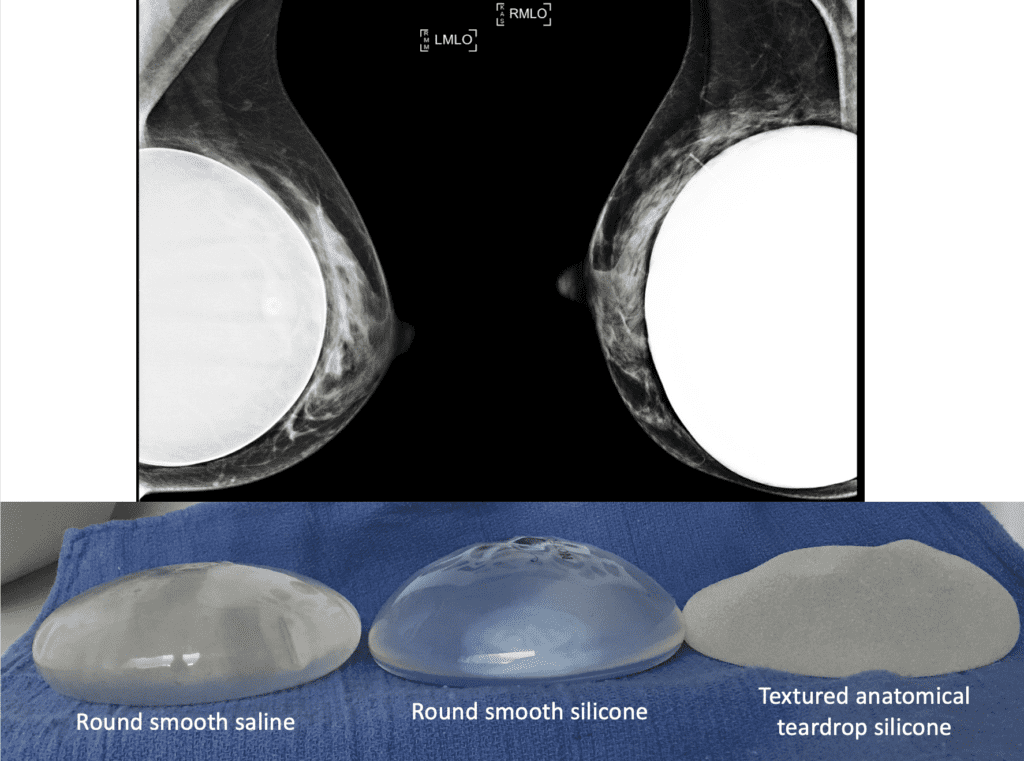
The smallest implants generally are 125 ml size, with the largest silicone 800 ml and largest saline 960 ml. “Extra large” implants result from overfilling of saline implants. Larger size implants likely correlate with increasing challenge with baby latch, positioning, and milk transfer. In addition, they may place pressure on native glandular tissue, leading to attenuation (decrease) over time. These larger implants also may contribute to nerve traction and reduced sensitivity of the nipple, similar to known phenomena with naturally large breasts.
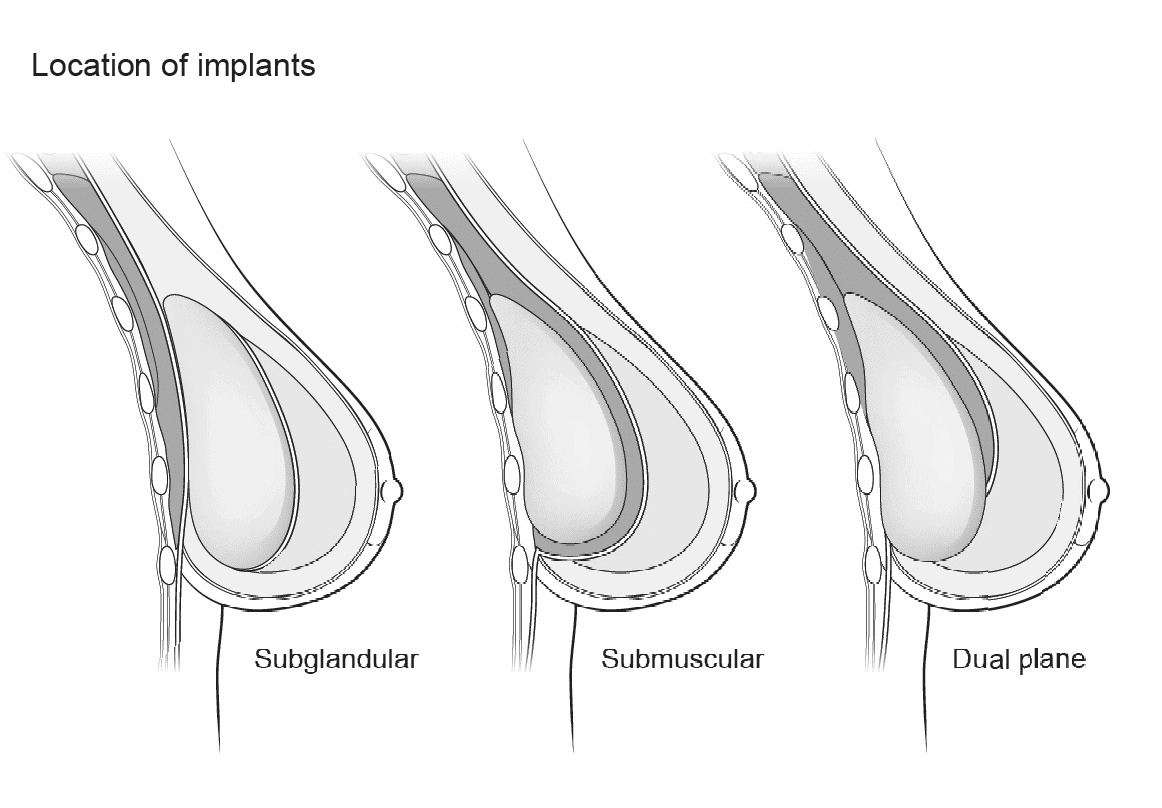
Implants may be placed subglandular (behind the breast and in front of the pectoralis muscle, also called “prepectoral”), submuscular (behind the pectoralis muscle), or “dual plane” where the implant is placed behind to the muscle, but a portion of the muscle is released to provide inferior pole fullness to the breast. Insertion of submuscular or dual plane implants may be more likely to disrupt nerves and blood vessels. Incisions for placement of implants include periareolar (around the areola), inframammary (underneath the breast where the bra line), axillary (under the arm) and transumbilical (through the belly button). Not surprisingly, due to the complex and overlapping innervation of the breast, no difference in nipple sensation has been demonstrated to correlate with incision type. Periareolar incisions do not appear to impact breastfeeding rates.
While infection of a breast implant is possible with untreated mastitis and/or repeated drainage procedures e.g for galactocele or abscess, in general this is very uncommon and is not a reason to avoid breastfeeding. Implant infections can be avoided by adhering to principles of mastitis management such as not massaging the breast and not overfeeding or overpumping.
Overall, patients with a history of breast augmentation, like other plastic surgery procedures, should be counseled in the prenatal period and followed closely postpartum. If infection does result in need for implant removal, the patient should continue breastfeeding uninterrupted during the perioperative time.



Silicone Breast Implant Rupture and Silicone Breast Injections
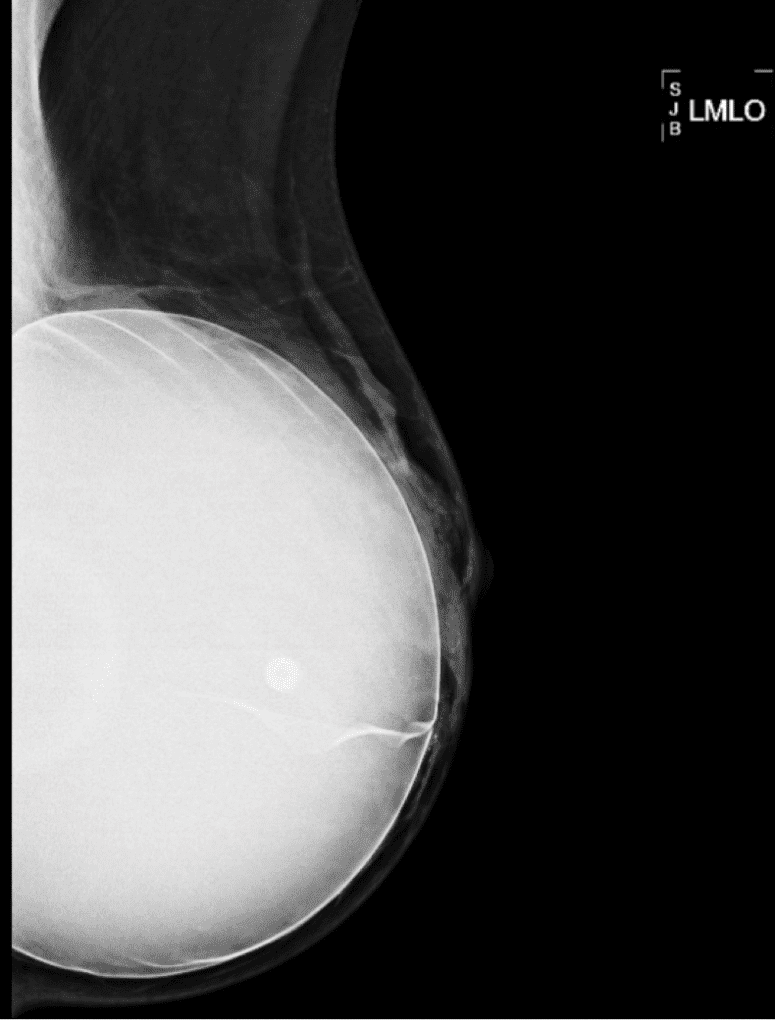
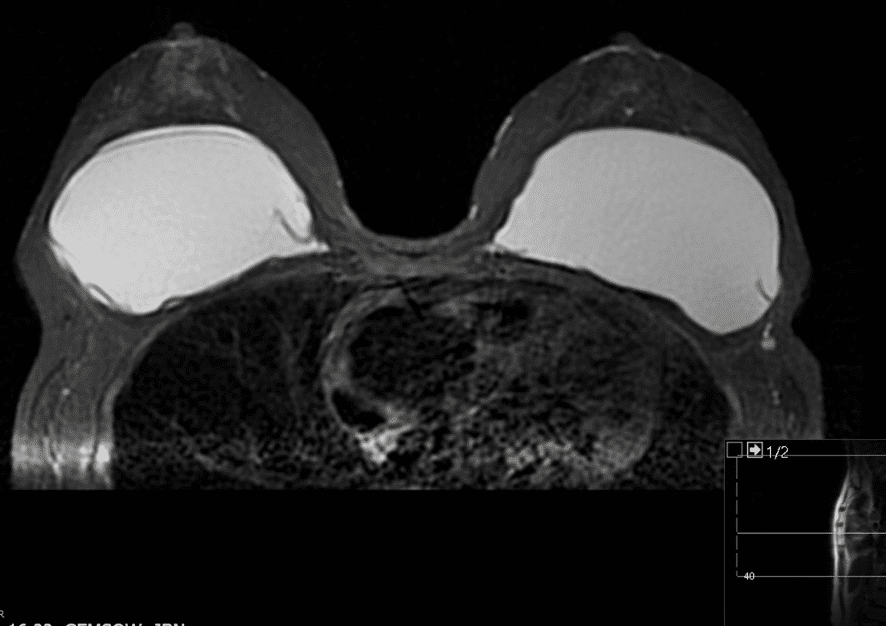
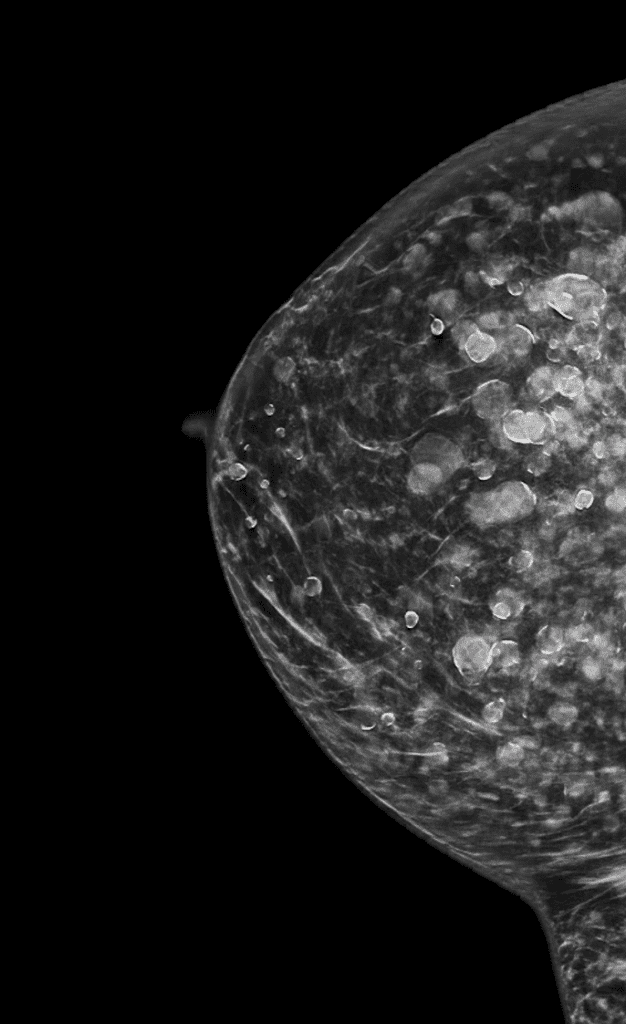
Silicone levels in the blood and breastmilk of women with implants are similar to those without implants, and breastfeeding is safe. Patients may report concern with a ruptured implant in the setting of breastfeeding, particularly with extracapsular rupture of silicone implants. Saline poses no risk and revision/replacement should be deferred until lactation is complete. Deferment of revision of a ruptured silicone implant may also be safe, given exponentially higher silicone levels in cow’s milk and formula. If rupture is suspected, breast MRI is the preferred imaging modality for evaluation. It is safe in lactation.
Infected Implant
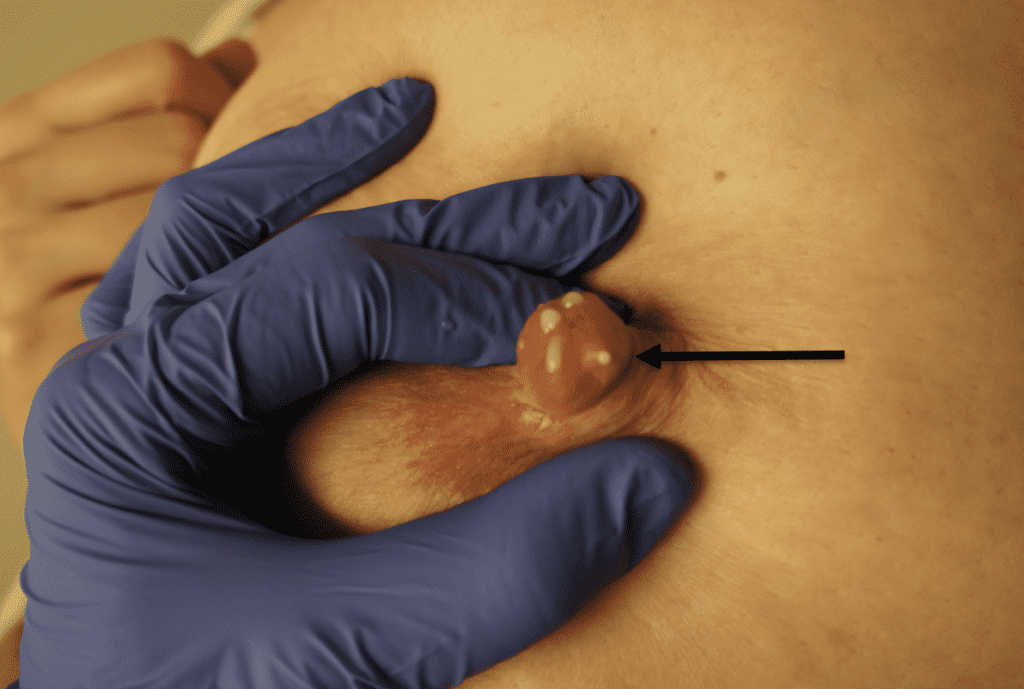
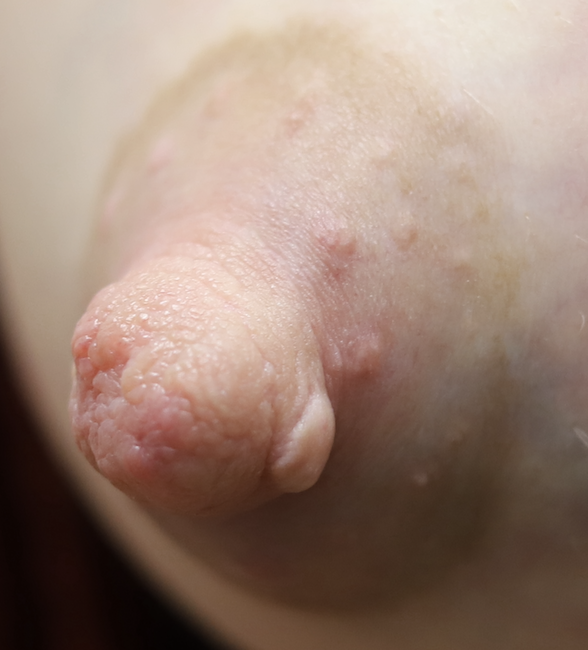
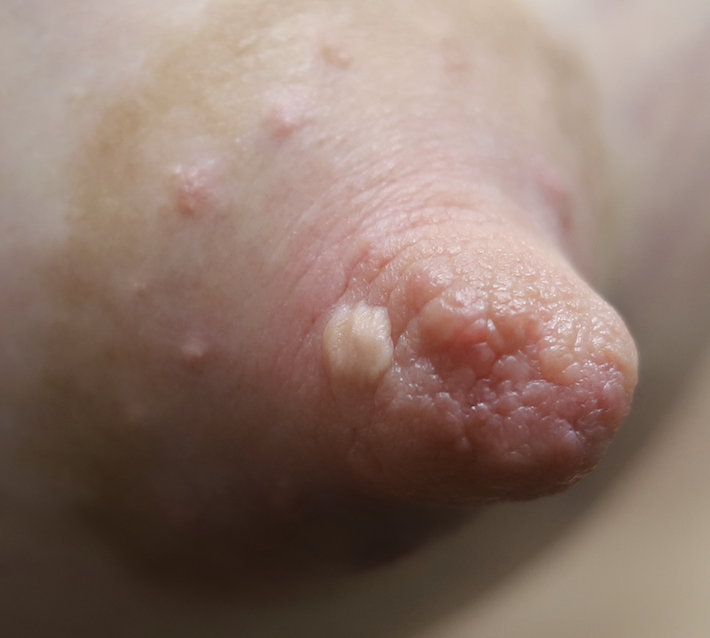
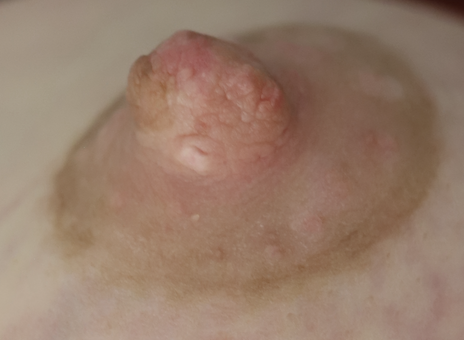
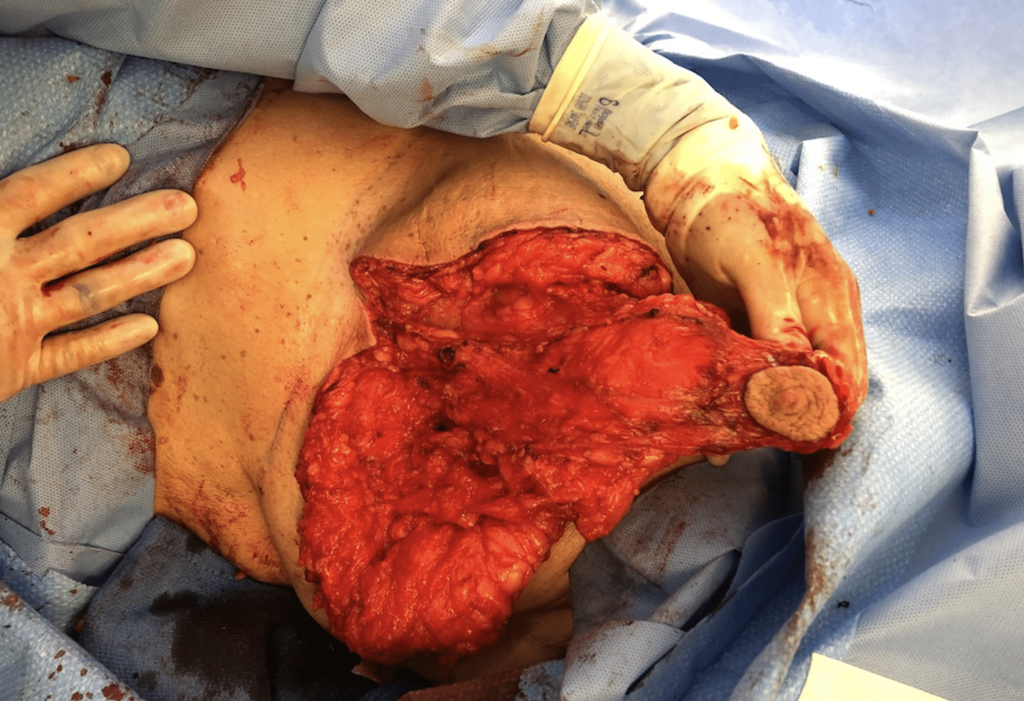
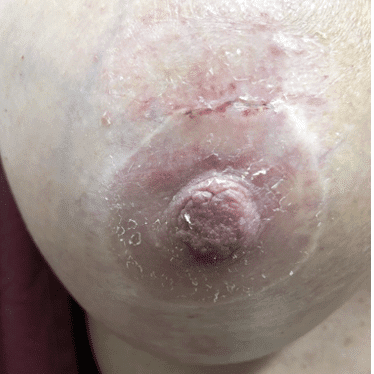
Infection of implants are uncommon during lactation, but possible. Infection is most likely if a patient has hyperlactation (oversupply of breastmilk), and develops mastitis and/or a fluid collection such as a galactocele or abscess in her breast tissue. Infected implants need to be removed. However, breastfeeding does not need to be interrupted for this surgical procedure. This report documents our experience with a patient requiring implant removal but who desired continued lactation.
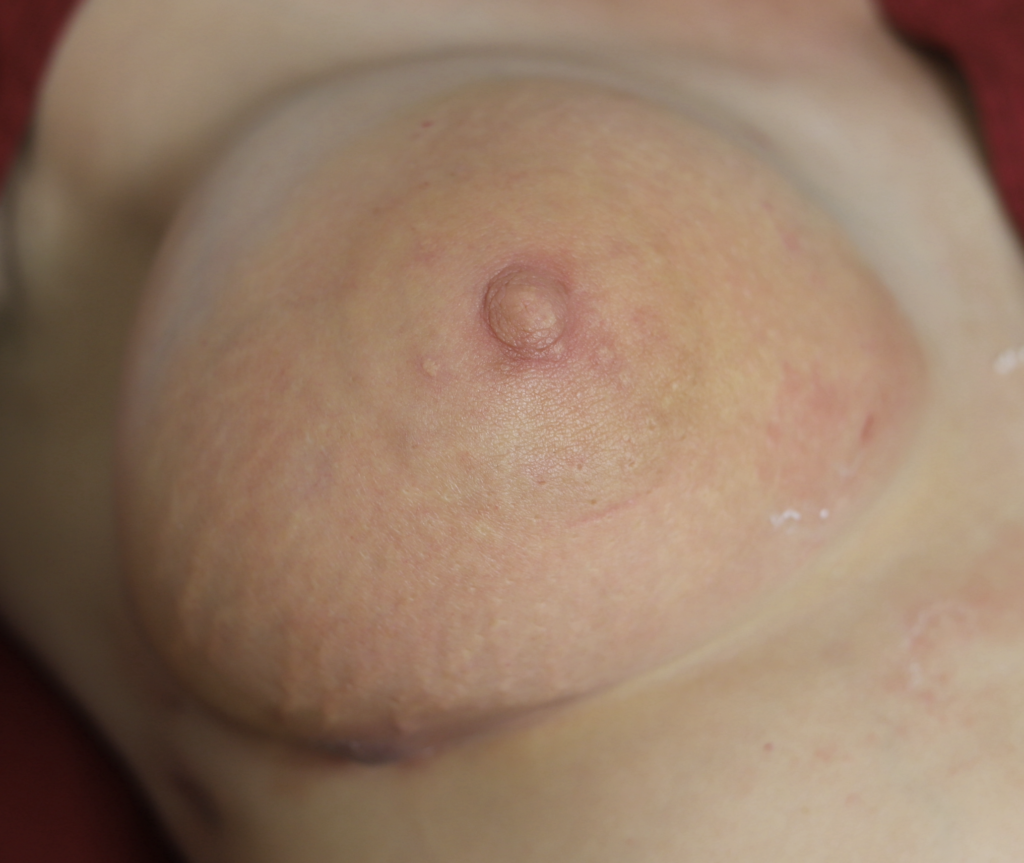
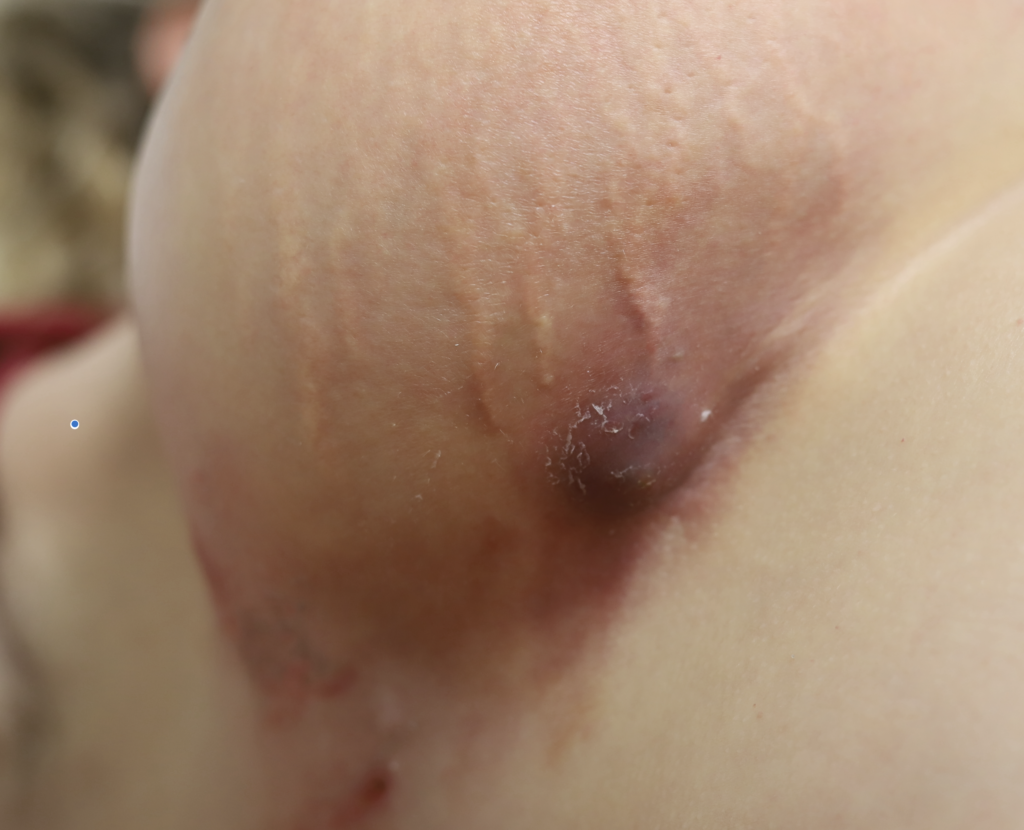
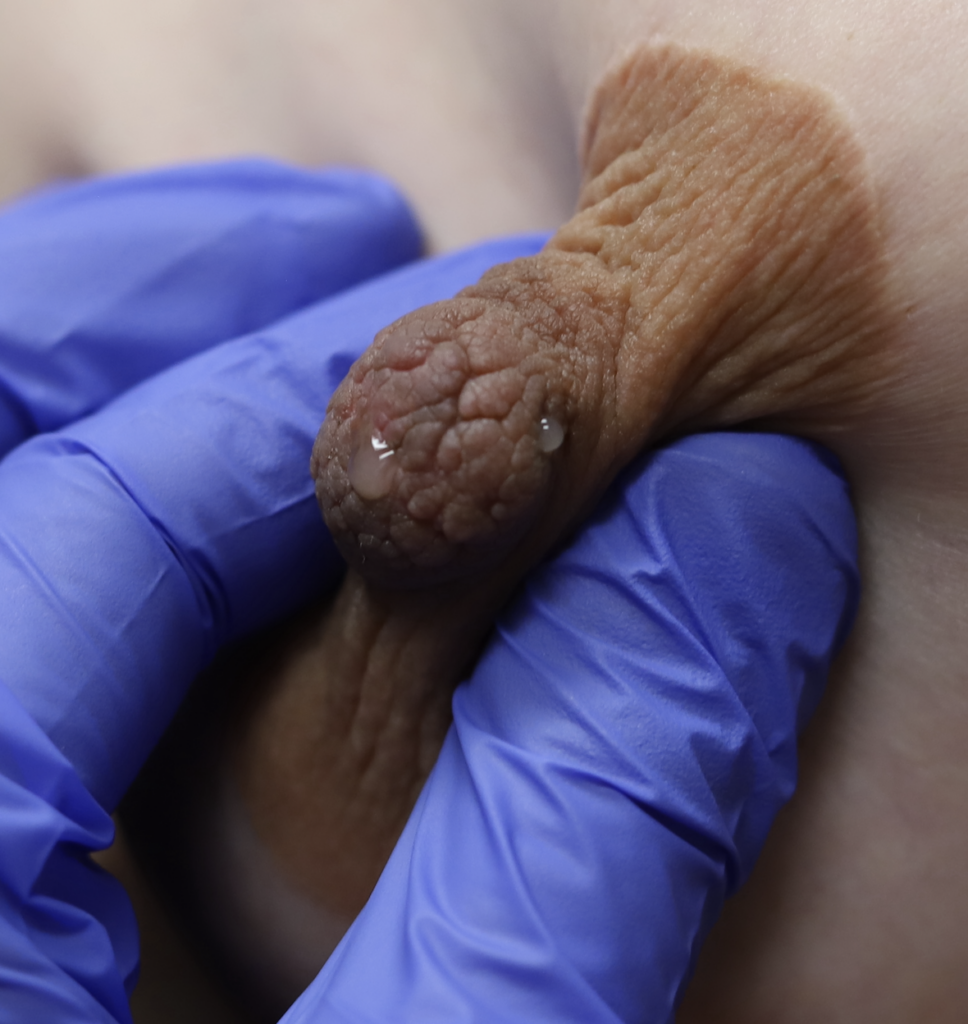
The photos are above are of a saline implant that ruptured but then became infected and needed drainage.
Nipple Areolar Complex (NAC) Procedures
Nipple Reduction
Countless surgical techniques have been developed to reduce large nipples. These include multiple approaches that attempt to reduce the outward projection of nipples. A “simplified reduction technique” involves excising part of the external projection of the nipple. There are limited data regarding lactational outcomes and this procedure should be deferred until breastfeeding is complete.
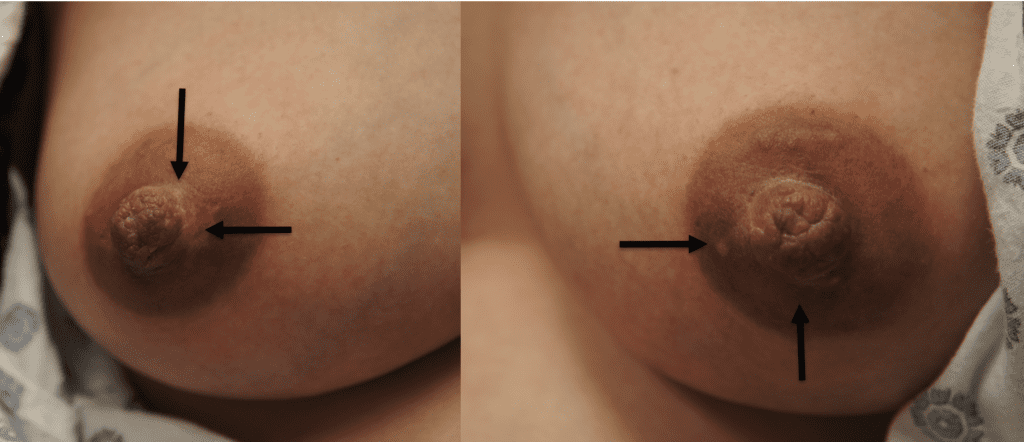
Nipple Eversion
Like procedures to reduce nipple size, numerous approaches to nipple eversion have been documented. Most involve disruption and scarring of ducts in the nipple and is not recommended prior to breastfeeding. Patients also should be counseled that breastfeeding is possible with inverted nipples, and nipples may naturally evert with breastfeeding and pumping.