So often, patients who are struggling with low milk supply, or those who see a sudden decrease in breastmilk production, are instructed to increase their milk supply with the advice: “Just keep nursing and it will get better” and “You make more breast milk the more the baby is on the breast.”
In some ways, this is correct. For example, if you were to restrict a baby to scheduled feeds (rather than letting baby feed on demand) as was often done in the past, this would not support you being in physiologic sync with your infant’s needs in order to increase your milk supply. If you don’t have any breast stimulation in the first few days postpartum, it can tell your body that it doesn’t need to make more milk.

However, in situations when mom’s milk production is persistently low (for a variety of physiologic and environmental reasons), putting a baby to the breast for extended feeds will not only exhaust your baby, but exhaust you. And, it won’t help you increase milk supply. Milk *removal* is what stimulates production to increase, not passive suckling.
This is particularly true when an infant is losing too much weight in the early weeks of life, is very behind in caloric intake, and continually falls asleep (from exhaustion) at the breast. The same applies moms who have lower than expected breast milk production as time progresses postpartum.
Reasons for sudden drops in milk supply
5 reasons for sudden drops in milk supply in months 3-6
There are many factors that could contribute to a decrease in supply before 6 months:
- Baby is becoming more interested in the world around them and may be distracted during the daytime feelings. They may feed for a quick minute here or there and be done. People may think this means that their milk is declining. In fact, this is absolutely normal behavior (we would be worried if baby WASN’T distracted in terms of appropriate developmental milestones). And it’s impossible to lose your milk production if you’re just feeding baby on demand in general. However, it can become a problem if baby isn’t otherwise feeding at night, before and after naps, in the morning at wake up etc (see below).
 This one month old is too young to be distracted in public. But in another month, he will not be interested in nursing in a grocery store when there is too much else to explore!
This one month old is too young to be distracted in public. But in another month, he will not be interested in nursing in a grocery store when there is too much else to explore!
- Many people have sleep trained, so their baby isn’t feeding at night like they normally would as a result of distracted daytime feeds (see above).
- As a result of sleep training, mom gets her period and her supply drops from that (i.e. two concurrent factors). Your milk production will ALWAYS be quite a bit lower right before you bleed, and then it picks up at the end of the week that you’re bleeding.
- Mom goes back to work and not pumping as much and not feeding baby at breast as much (e.g. she leaves before baby gets up so misses morning feed or gets home too late and baby is asleep and then baby is sleeping overnight).
- Mom gets hormonal contraception at 6 weeks postpartum.
Sudden drop in milk supply around 9 months
- Babies get more distracted and really are just feeding for nap times and bedtimes and wake ups.
- Because breasts will never be as engorged as they were in the early postpartum days, mom’s milk can “feel really low” or her breasts “empty.” However, this is normal. And as as above, you can’t go wrong just feeding baby on demand when you’re with them. and pumping when you’re away from them.
- Another EXTREMELY important point to understand is that breastmilk becomes HIGHER IN CALORIES as baby gets older. Babies are getting shots of nutrition (lower volume, higher calories).
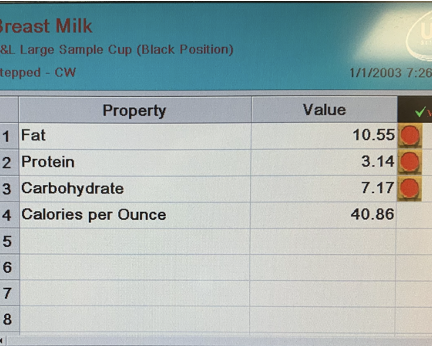 Average caloric content of breastmilk is 22 kcal/ounce. However, you can see in this breastmilk sample from someone nursing four years postpartum, the calories per ounce increased to 41!
Average caloric content of breastmilk is 22 kcal/ounce. However, you can see in this breastmilk sample from someone nursing four years postpartum, the calories per ounce increased to 41!
- Pediatricians who are not familiar with breastfeeding will tell moms that baby needs X volume per day (e.g. 30 ounces per day). This is an artificial number based on formula feeding averages and has zero applicability to breastfeeding at the breast.
- If your baby is growing well and nursing at the breast when you are not at work, take the stress out of how many ounces you are pumping and recognize there is a WIDE WIDE variability of “normal” volume consumption at this age.
- Daycare and other childcare providers also may not be familiar with breastfeeding behavior/volume and could be overfeeding breastmilk in a bottle (in this situation, reduce the ounces per bottle you send with baby). Also, if the daycare feeds so much extra breastmilk during the day (i.e. far more volume than an infant would take at this age breastfeeding during the day), the baby isn’t as interested in feeding when with mom after she returns from work.
Is it possible to “lose” or “tank” my supply if I’m feeding at the breast?
No! If you’re feeding on demand (not a schedule) at the breast, you can’t “tank” your supply. You literally can’t go wrong feeding your baby at the breast for sleeping and comfort when they are sick. If they are gaining weight well, they do NOT need any supplementation.
Often, I get this question from moms that have giant breastfed babies who are starting to move around a lot, and may be burning calories. Their pediatricians are just looking at number on chart rather than evaluating how the baby looks in general.

3 Tips to increase milk supply after a sudden drop … without exclusively pumping!
Patients may be instructed to exclusively pump for 24 hours to “see how much milk they are making.” Unfortunately, this approach is fraught with problems.
First, moms provided this directive are often making less milk than their baby needs, or there is some concern about the baby’s weight gain. Unless a baby is behind in calories or weak for another reason, a pump is never going to remove milk as well as a baby will. So, a mom could be pumping volumes that are lower than her true gland function, and feel falsely defeated. This inevitably worsens anxiety and stress. Read more about why you don’t need to measure your breast milk output.
 Chloe Trayhurn
Chloe Trayhurn
The other issue is that anytime you decouple mom and baby, you risk problems. This can include pump trauma for mom, or a baby not being interested in going back to the breast after a strict interruption.
Set a realistic expectation for pumping
Instead of overdoing your breast pumping with techniques like “power pumping,” it’s better for your breasts and your mental health to pump for 10-15 mins every 2-3 hours and give baby bottle of pumped milk or formula.
Make sure baby is nursing actively
Latch baby when you are awake/not frazzled and learn to watch for swallows. When baby sucks and swallows, it tells the breast that milk is being removed and cells should make more milk. But repeated nipple contact alone with baby falling asleep and dream feeding without swallowing tells the breast no up-regulation of production is needed, because no milk is being removed.

Why “triple feeding” is only a temporary solution
“Triple feeding” (feeding the baby at the breast for a prescribed period of time, then pumping, then giving the pumped milk back to the baby +/- other supplementation with donor milk or formula) becomes exhausting and demoralizing for parents, and exhausting for infants as well.
Infants should NOT be placed to the breast for a prescribed period of time (such as 15 minutes per side). Instead, they should only be at the breast if they are sucking and swallowing, or if they have been supplemented prior to the feed and are “finishing at the breast” for comfort only.
The “divide and conquer” approach to increasing milk supply
So, how can you increase milk supply without negatively impacting your mental health? I suggest a divide & conquer approach, with one parent focusing on milk production while the other feeds the baby:
Mom focuses on pumping and introducing galactagogues (herbs or medications that increase milk production) to stimulate her breasts and remind the breasts that even if the baby got sleepy and behind in calories, they do in fact need to produce milk. This is one of the few times where I actually feel a breast pump is useful and medically indicated (aside from NICU, or other separation of mom and infant). Dad, partner, or other relative focuses on getting calories in the baby.
It is OK to give a bottle at this point. “Nipple confusion” in the setting of low milk production is actually more of “flow preference.” Babies will either fuss at a breast without enough milk, or fall asleep.
I have mom put baby to breast at times when her milk flow should be higher (in the early morning hours; even moms with plenty of milk will have less in the afternoon and evening). This is simply to maintain baby’s familiarity with mom’s breast.
The baby can suck for comfort, but it is necessary to ensure the baby continues to take in adequate volume from the bottle. Over time, mom can gradually notice the baby swallowing more and the breast and being more satisfied. However, this does not happen immediately and some moms have to continue supplementing for the duration of breastfeeding.
Take a slow-and-steady approach instead of expecting to increase milk supply fast
Like all of parenting, breastfeeding is a MARATHON and NOT a sprint. It is much better for your mental health to give a baby a bottle to sustain early breastfeeding challenges than become utterly exhausted with syringe feeding or nonstop pumping and then give up.
Anything that is too good to be true IS. It’s impossible to “double” or “triple” milk production overnight (unless someone was very early postpartum and was measuring from before their milk came in).
Like everything else with parenting, there is an unfortunate large profit to be made from new moms lacking real support. Red gatorade and other expensive products are just that – EXPENSIVE, with no reason in the world that they would actually increase milk production like magic.
 Grandparents can be very helpful in giving mom a mental health break!
Grandparents can be very helpful in giving mom a mental health break!
Finally, my Irish colleague, Caoimhe Whelan, gave me permission to use these wonderful slides she created with UK artist, Lauren Rebbeck. They illustrate so well why we need to question and redirect triple feeding and other situations that emphasize breastmilk over mom’s well-being.