Baby Noise
Babies make noise! This can even sound like choking or gurgling at times. Breastmilk is a physiologic substance and if refluxed into the oral cavity, it can help prevent upper respiratory infections and ear infections. Further, neonates who have spent the past 9 months at human body temperature in cramped, tight spaces in the mother’s uterus will not always enjoy sleeping on their backs in a cold location. Some babies will do just fine, but others may grunt and protest and struggle to get comfortable. This is actually protective against Sudden Infant Death Syndrome (SIDS), as breastfed babies spend less time in deep neurologic sleep and therefore can awaken more easily to breathe.
If you are hyperaware of these sounds and unable to sleep, consider meditation, yoga, and essential oils for relaxation. Persistent hypervigilance may represent an emerging anxiety or mood disorder, and perinatal therapy and/or medication can help.
Baby making noises breastfeeding

Breastfed Stools
Infant diapers and breastfeeding stools are a hot topic! See this discussion under Hyperlactation (Oversupply) and Breastfeeding Stools in 3-6 Weeks section of Breastfeeding Basics.

Cleft palate, Down’s Syndrome, and other Congenital Conditions
Breastfeeding with congenital conditions such as cleft palate and Down’s syndrome can be challenging, but possible. It is important to work with local physicians and lactation consultants prenatally to develop a feeding plan
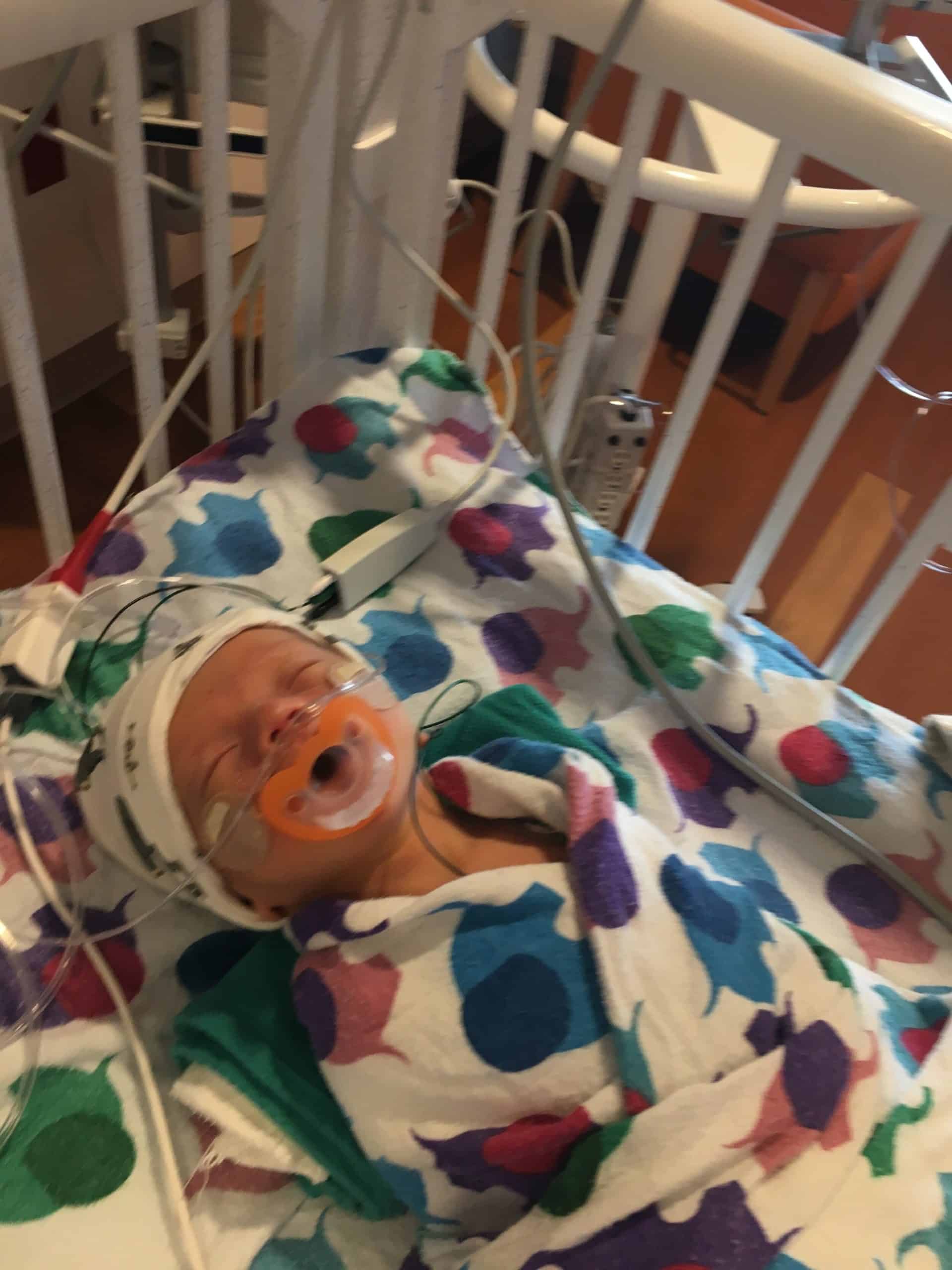



I was beyond impressed with this patient of mine who advocated for skin to skin time with her newborn baby girl in the NICU, as well nursing at the breast, in the setting of baby being born with a tracheoesophageal fistula (TEF) awaiting surgical repair.
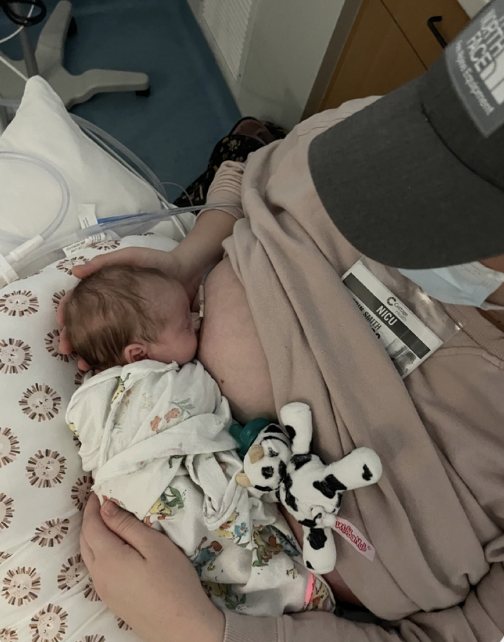
In a TEF, the esophagus may not connect to the stomach, meaning the baby needs nutrition via a feeding tube in the stomach (gastrostomy tube or g-tube). They have a “replogle” suction tube in their nose to remove secretions from their mouth and esophagus.
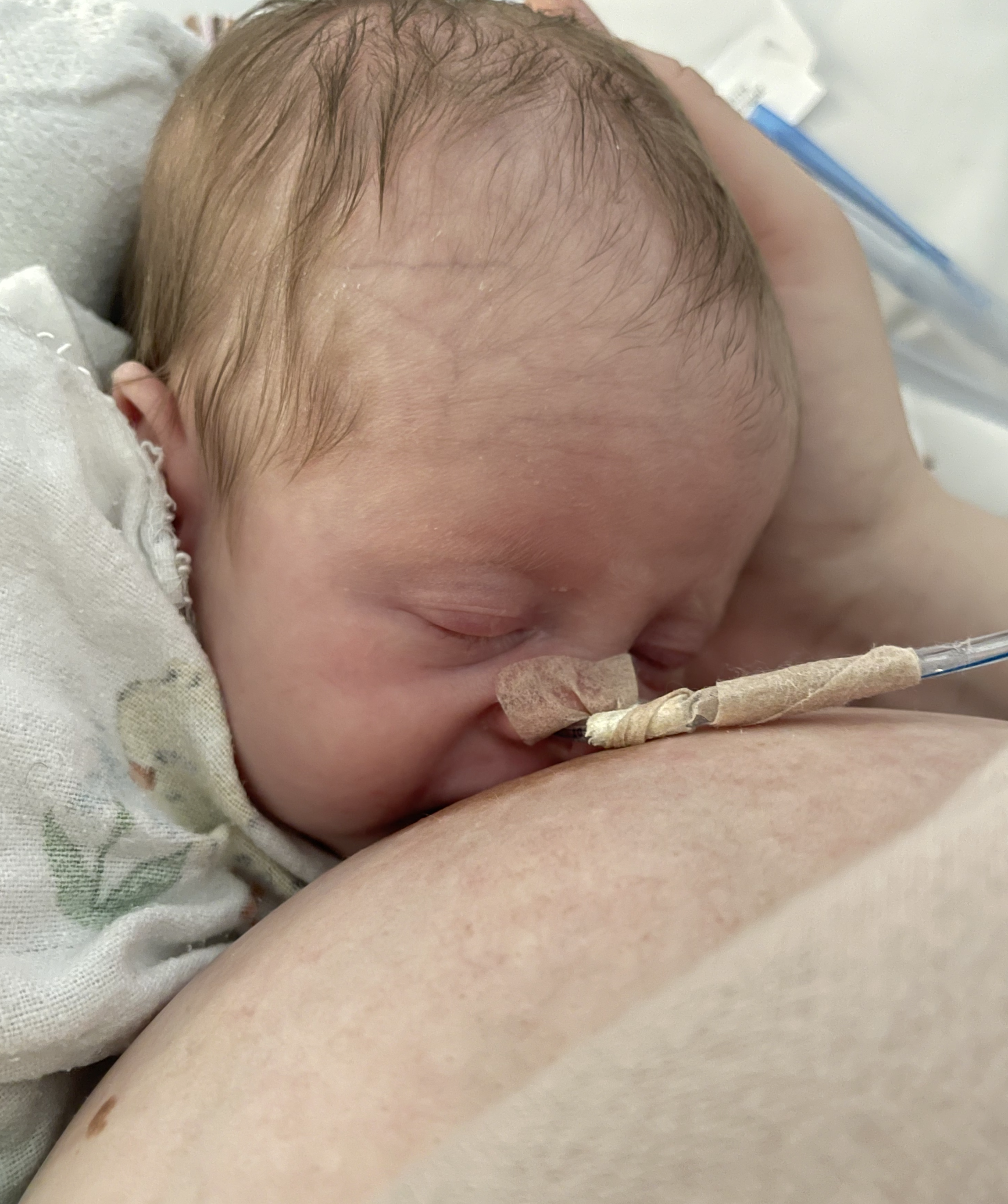
The vast majority of the time, these patients are instructed to pump breastmilk and feed via the g-tube only. However, studies have shown that “sham” feeding (i.e. practice sucking without the liquid going anywhere but out the tube) actually promotes earlier oral feeding after the surgical repair. Indeed, at two months old, this baby could suckle more than 40 ml from mom’s breast!
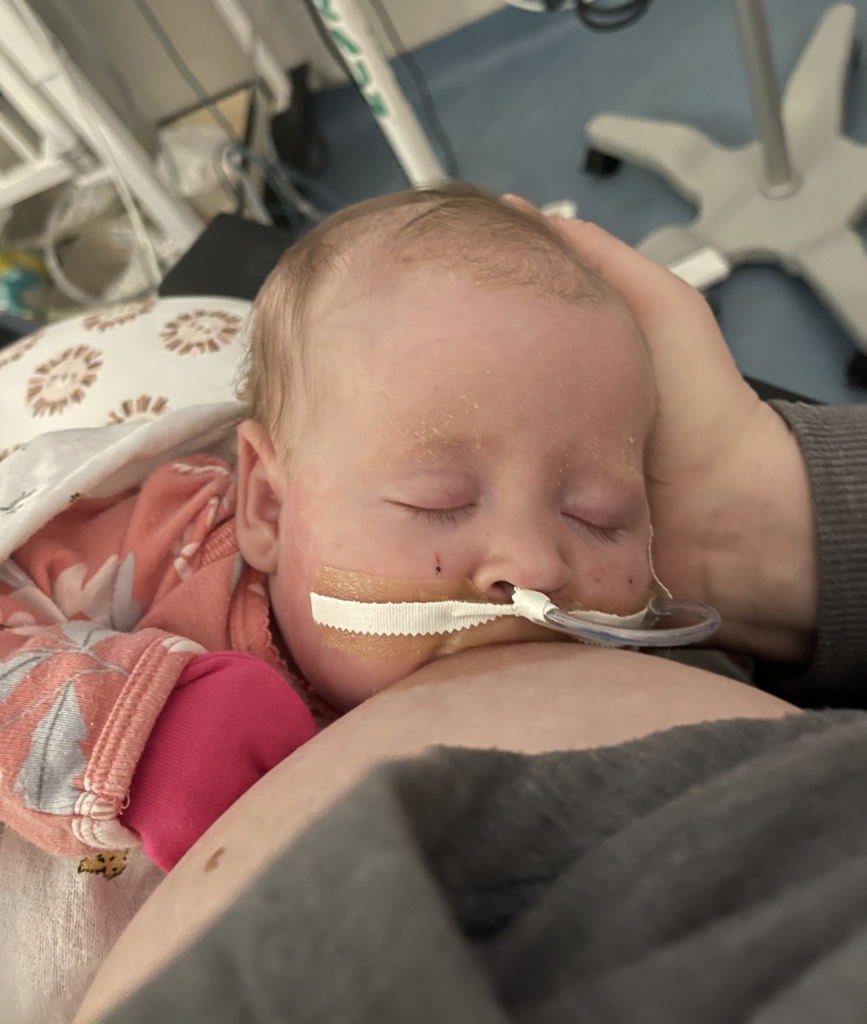




Aside from the feeding practice, nursing at the breast lowers stress hormones in both mom and baby. And the incredible molecular properties of breastmilk are limitless in terms of their healing ability.

Infants Admitted to the Hospital for Illness or Surgery
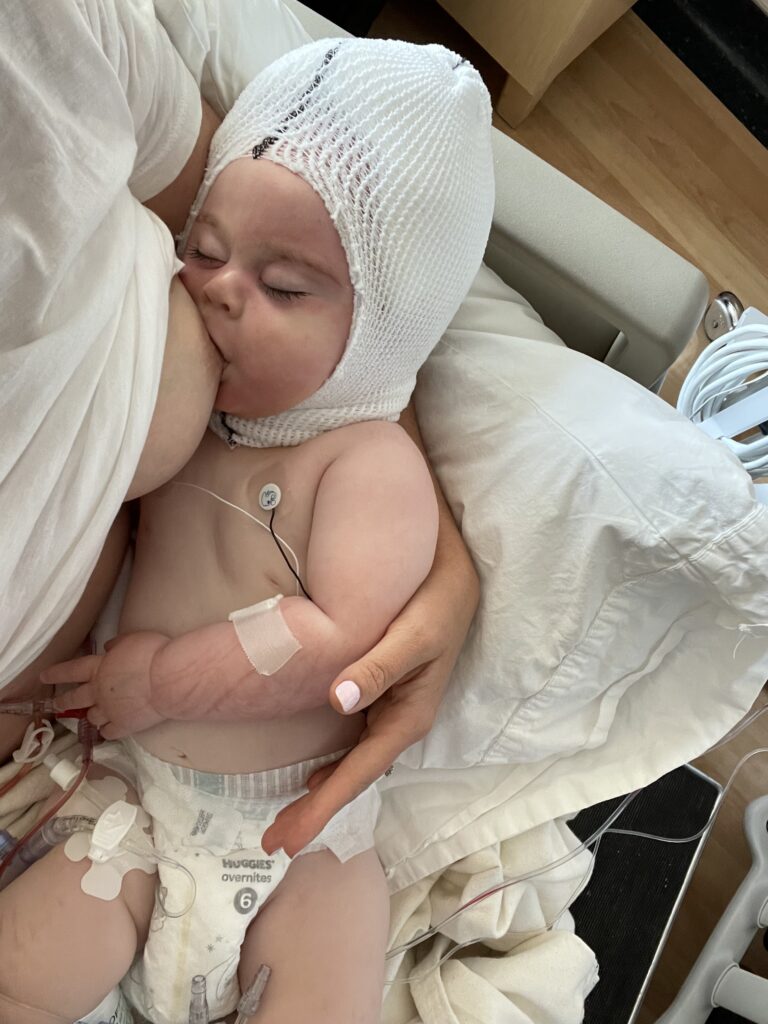
Infants admitted for surgical procedure or illness should not interrupt breastfeeding. Keep the baby at the breast and skin to skin. The Academy of Breastfeeding Medicine protocol on breastfeeding during maternal and/or child hospitalization provides detailed recommendations regarding this topic.

Infant Thrush
Infant thrush in full term, immunocompetent babies is not nearly as common as the lactation world makes it out to be. Further, thrush is not contagious. Vaginal yeast infections are not contagious, i.e. sexual contact with a partner does not transmit them in the way sexually transmitted infections occur. Yeast is a result of host microbiome disruption that occurs most commonly in areas like the vagina, inframammary fold of the breast (where the bra strap sits underneath the breast), and under the arm. Yeast also may occur in heavier individuals in areas of subcutaneous fat. It occurs in immunosuppressed patients (e.g. chemotherapy, HIV), diabetes, and obesity.
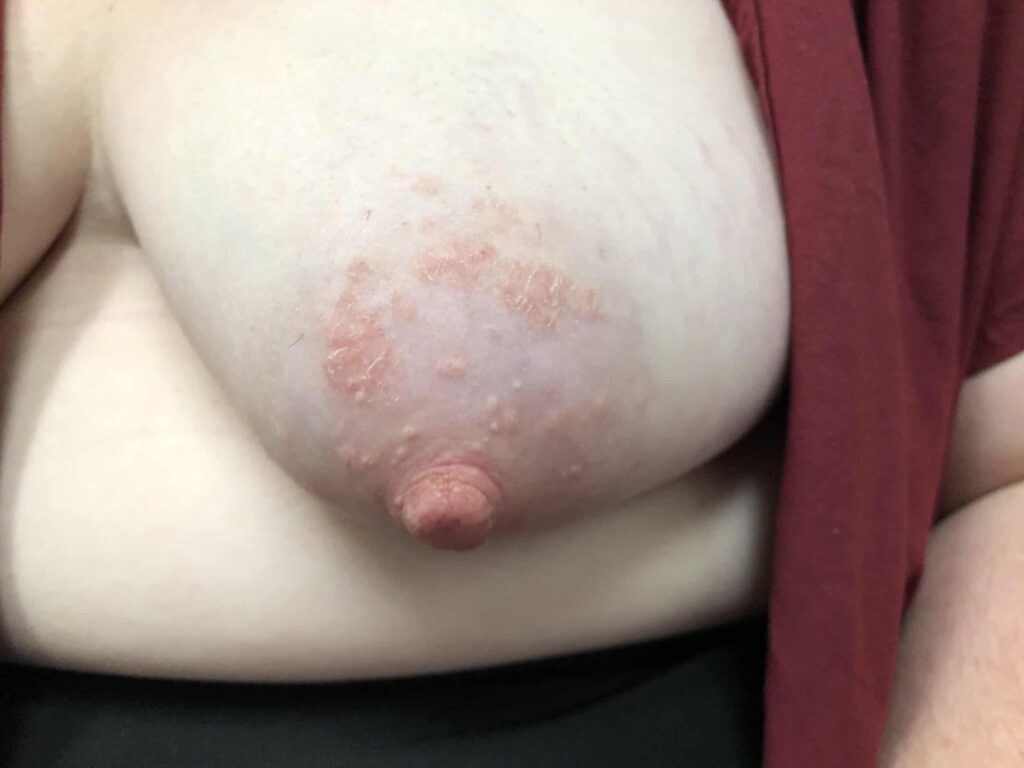
Therefore, infants with thrush cannot transmit yeast to their mothers. While they undergo thrush treatment, mothers do not need to undergo antifungal treatment themselves. In fact, anti-fungal treatments on the nipple can cause allergy and wound development.
Short Feeds
If mom has a lot of milk, the baby may feed for short periods of time. As long as the baby is sucking and swallowing, is satisfied after, and is gaining weight well, this is ok. If too fast of a flow becomes a problem, then the mom should feed in the side lying position to reduce rate of breastmilk flow and may consider evaluation for treatment of hyperlactation/oversupply.
If a baby feeds for a short period of time without sucks and swallows, and then falls asleep quickly, this is concerning for low milk production and mom/baby should be evaluated.

Feeding Cues
Parents often do not recognize the difference between a baby “rooting” because of poor head control and reflexes versus a baby that is truly hungry. Again, I have parents watch for sucks and swallows and baby satisfied with being held versus being put down, picked up and “rooting” at that point.
Beware the babies who want to be held! Mom may have plenty of milk, the baby is gaining weight and stooling well, but the baby is “constantly hungry.” I have parents differentiate between hunger and “wanting to be held” by waiting for baby to finish a feed, then holding the baby rather than putting the baby down on its own. Babies should suck and swallow vigorously for at least several minutes, then may slow down their sucking and eventually fall asleep (they should not require stimulation to stay at the breast and suck, or this is often a sign of low milk production) or be awake and not showing hunger cues.

Babies putting their hands in their mouths is an early neonatal feeding cue. As babies get older, chewing on fingers or hands is more just emerging awareness and exploration of their body and is not necessarily a feeding cue at this time.

Babies that Like to be Held
If you have a baby that wants to be held and you are struggling at night with the baby feeding, going to sleep, getting put into the bassinet, and waking up immediately, it is important to monitor for extreme exhaustion and frustration. This cycle can repeat itself night after night. In fact, humans, like other primates, have evolved as a “carry species” within the mammalian family to produce breastmilk that requires frequent feeding and infants who stay close to their mothers. And after nine months in a constantly moving womb at human body temperature, it’s natural that many babies will protest being placed on their backs in a cold, solitary bassinet.

If you are in this situation, the options are to take “shifts” with your partner (both parents are not awake at the same time holding the baby), involve relatives and/or hired help, or prepare to bedshare safely. Mostly, we do not want parents to become so exhausted that they fall asleep in an unsafe situation like a couch or rocking chair with the baby. It is FAR safer to share a safe bed surface with a baby than prop yourself up with pillows to try to avoid falling asleep.
James McKenna, PhD, new book, ‘Safe Infant Sleep’ is an excellent resource on this topic. He also gave me permission to summarize key points in this sleep resource for parents.
The American Academy of Pediatrics statement on safe sleep recommendation 4.e. states “parents frequently fall asleep while feeding the infant. Evidence suggests that it is less hazardous to fall asleep with the infant in the adult bed than on a sofa or armchair, should the parent fall asleep. It is important to note that a large percentage of infants who die of SIDS are found with their head covered by bedding. Therefore, no pillows, sheets, blankets, or any other items that could obstruct infant breathing or cause overheating should be in the bed.”
This AAP statement as well as the Academy of Breastfeeding Medicine Bedsharing Protocol, authored by the world’s expert on safe sleep, outlines safe ways to approach the reality of breastfed babies liking to be kept close to their mothers.
With babies who continue to have high levels of stimulation, occupational therapy can be helpful for reducing sensory overload. Speak with your medical provider about this.


Baby Cries or Fusses While Feeding

A baby crying or fussing at the breast is usually responding to high flow (oversupply) or low flow (lower supply). With high flow, babies may initially latch and be content, but when flow increases after a letdown, they may clamp, pull back and arch, cough, choke, and cry. Refluxing breastmilk is not dangerous (in fact it may prevent upper respiratory infections by bathing the mouth, nose, and ears in breastmilk loaded with antibodies and other immune cells). However, it is alarming and scary to mom. This is a situation where mom should feed in side lying position to slow down flow and seek treatment for hyperlactation if it persists.
If a baby latches initially but does not swallow and either falls asleep or cries, this is most often related to lower flow. Babies may respond to gentle compressions on the breast tissue to promote flow. They also may respond to SNS (though use with caution as above) or taking some supplement from a bottle prior to the breast.
Less commonly, a baby may be experiencing true gastrointestinal reflux disease (GERD or “reflux”). This is when a baby is desperately hungry, goes to the breast (or bottle of formula or breastmilk — it hurts with anything), starts to feed, and then stops about 30 seconds in. The baby is experiencing the pain of the reflux of stomach acids into their esophagus. They stop feeding and cry. Then they try again. This cycle continues.
It is incredibly stressful for mom, other caregivers, and baby. It also can impact mom’s milk production because the baby is never effectively feeding and removing milk. If mom has a lot of milk, she may have more wiggle room. But if she has less milk, it’s important to be really careful about maintaining it (and she may need to do some pumping).
The difference between true GERD and hyperlactation/oversupply “reflux” is that babies with GERD gain weight poorly. They are hungry, but they can’t feed and transfer milk effectively (despite trying). Babies of moms with hyperlactation will feed large volumes (as described above) and then fuss, spit up, and have gas. And they gain a lot of weight in general.
GERD does NOT cause gas. GERD is an upper GI condition (stomach/esophagus), not a lower GI condition (colon/rectum). Your baby may be in pain and/or want to be held, but it isn’t because of “gas.”
Babies with true GERD will generally improve with anti-reflux medications. If they are sensitive to something in mom’s diet that appears to be a trigger (e.g. milk) this can also be eliminated to see if symptoms improve.
Clicking
Mothers will often be concerned about an infant making clicking sounds at the breast. This is related to the baby breaking suction on the breast, which is often lower or higher flow (pulling back because there’s not much milk, or pulling back catch breath or not choke). Sometimes some infants are less coordinated with their entire oral cavity, and may benefit from an evaluation pediatric ear, nose, and throat specialist and/or occupational therapy exercises for strengthening.
Ankyloglossia (Tongue Tie) and Other Pediatric ENT Concerns
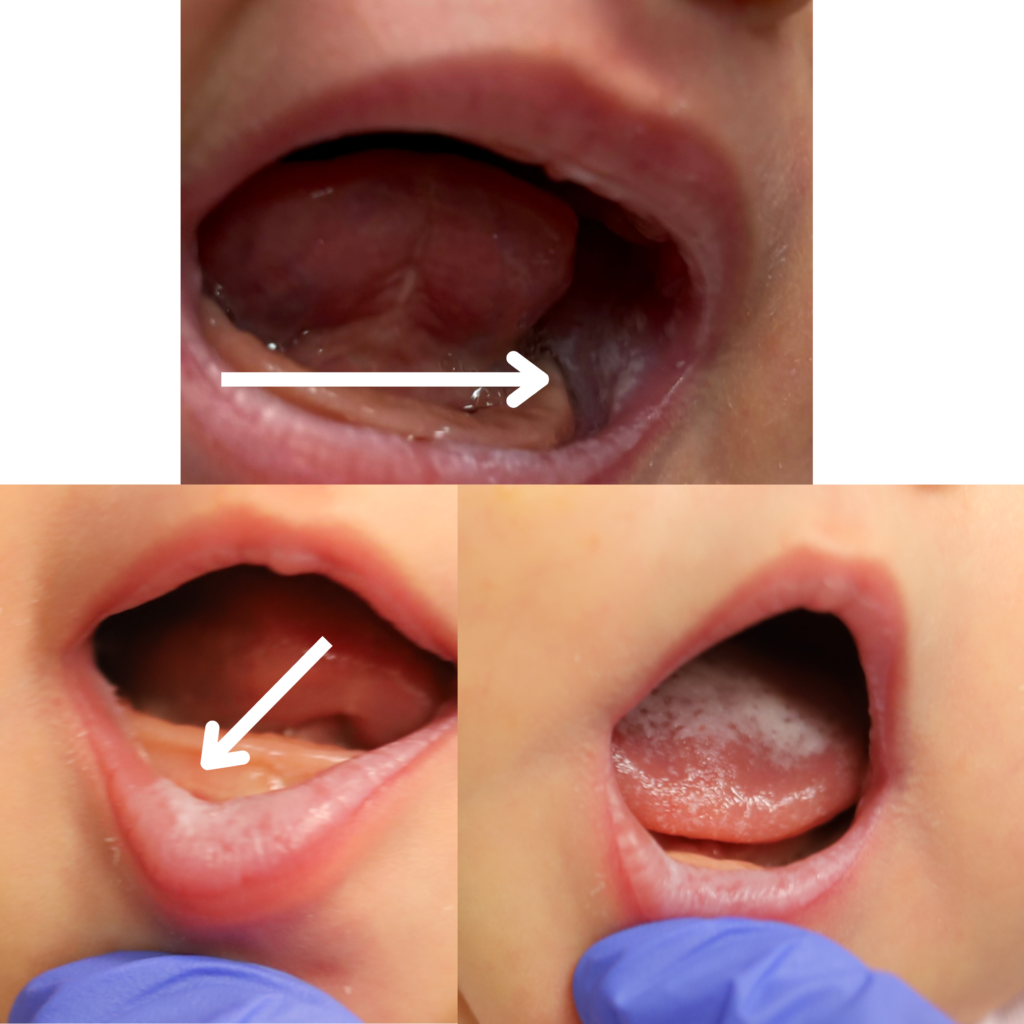
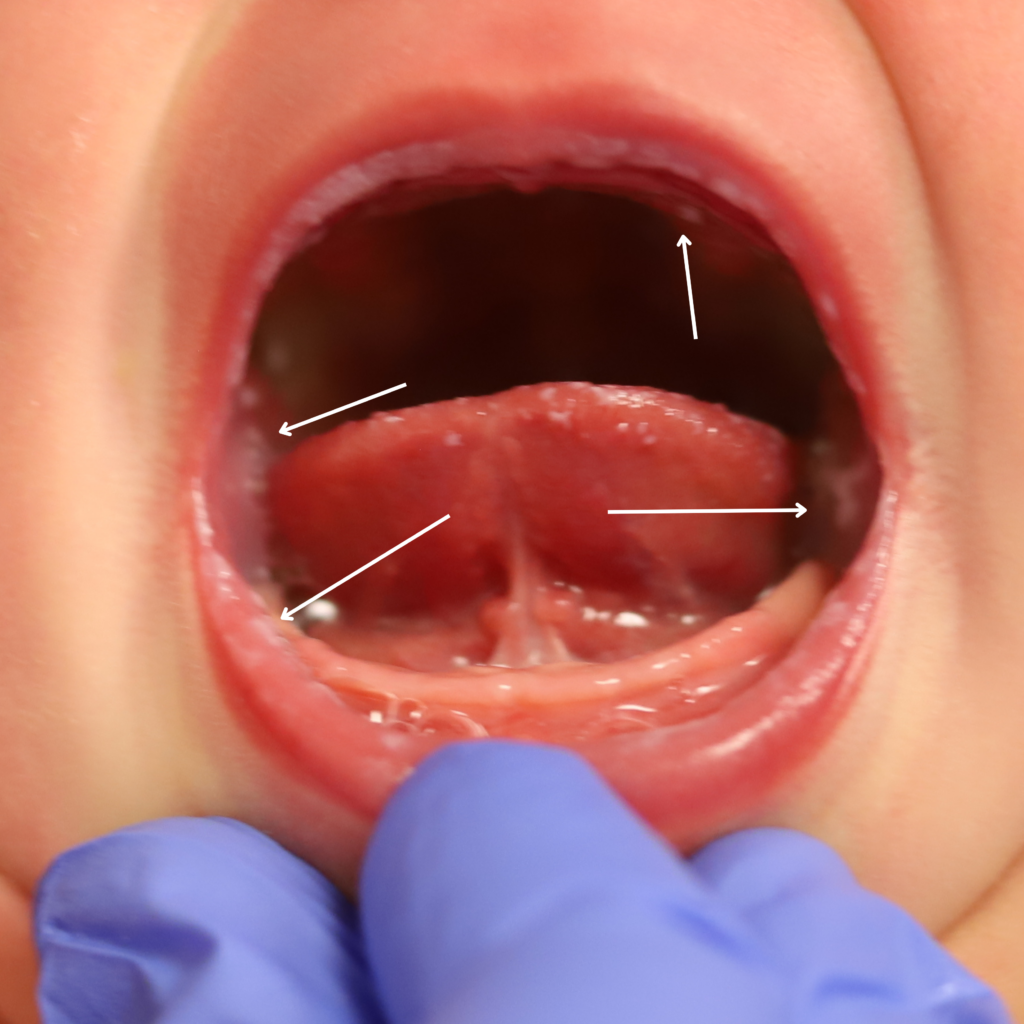
Ankyloglossia, or tongue tie, is the presence of a short, thick, or tight lingual frenulum (connective tissue underlying the tongue) that impairs sucking. This can occur as an “anterior” tongue tie (very tip of the tongue is attached to the lower gum), or a “posterior” tongue tie (further back on the floor of the mouth).
The interplay of baby’s mouth and mom’s breasts can impact lactation in different ways. Some babies with a restrictive frenulum can nurse without issue if mom’s nipples are elastic and she has ample milk production. Other infants with less restriction can struggle to feed if mom’s flow isn’t ideal for them. In some cases, infants also will have other oropharynx cavity variations, including high palates and generalized discoordinated sucking. These infants can benefit from occupational therapy exercises.
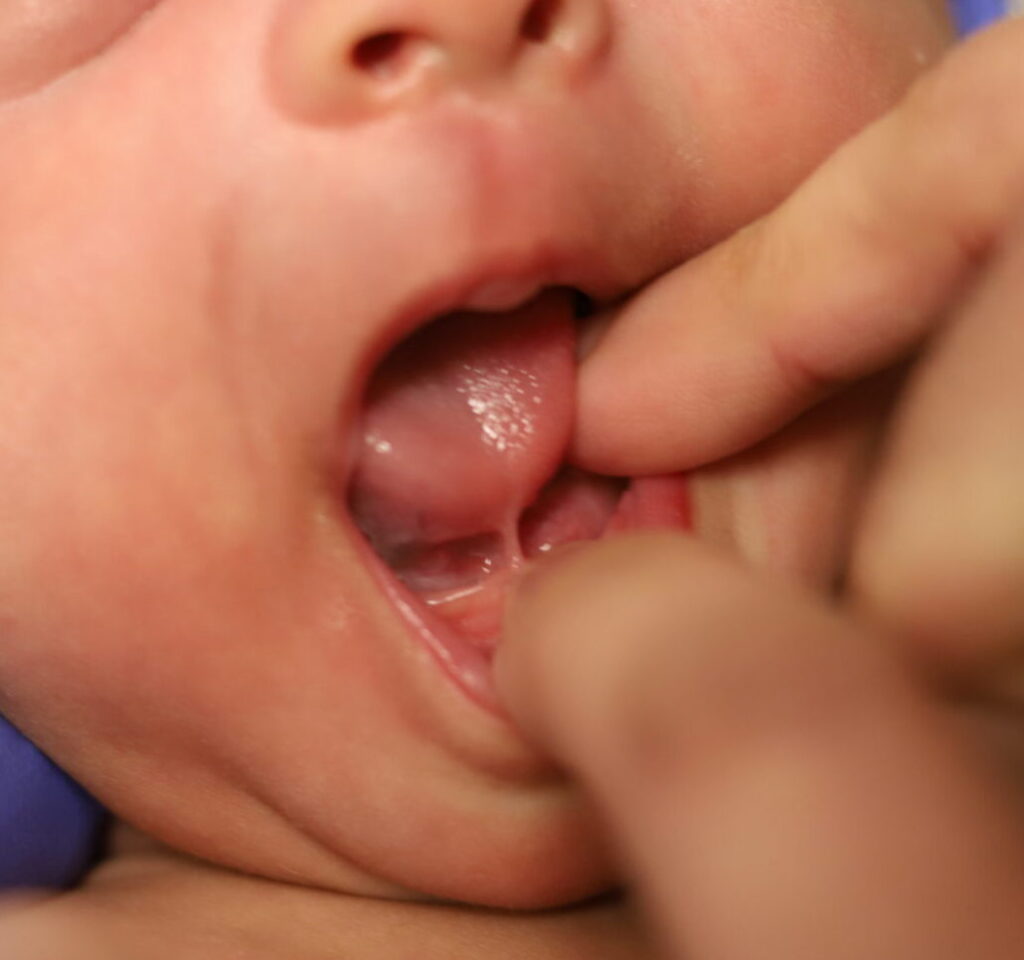
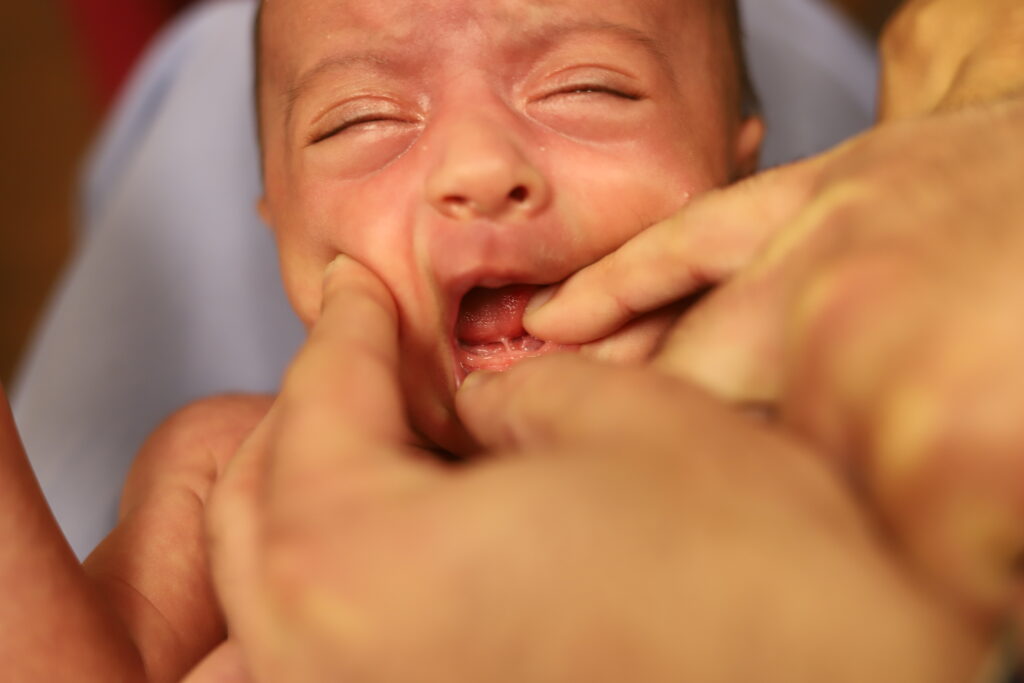
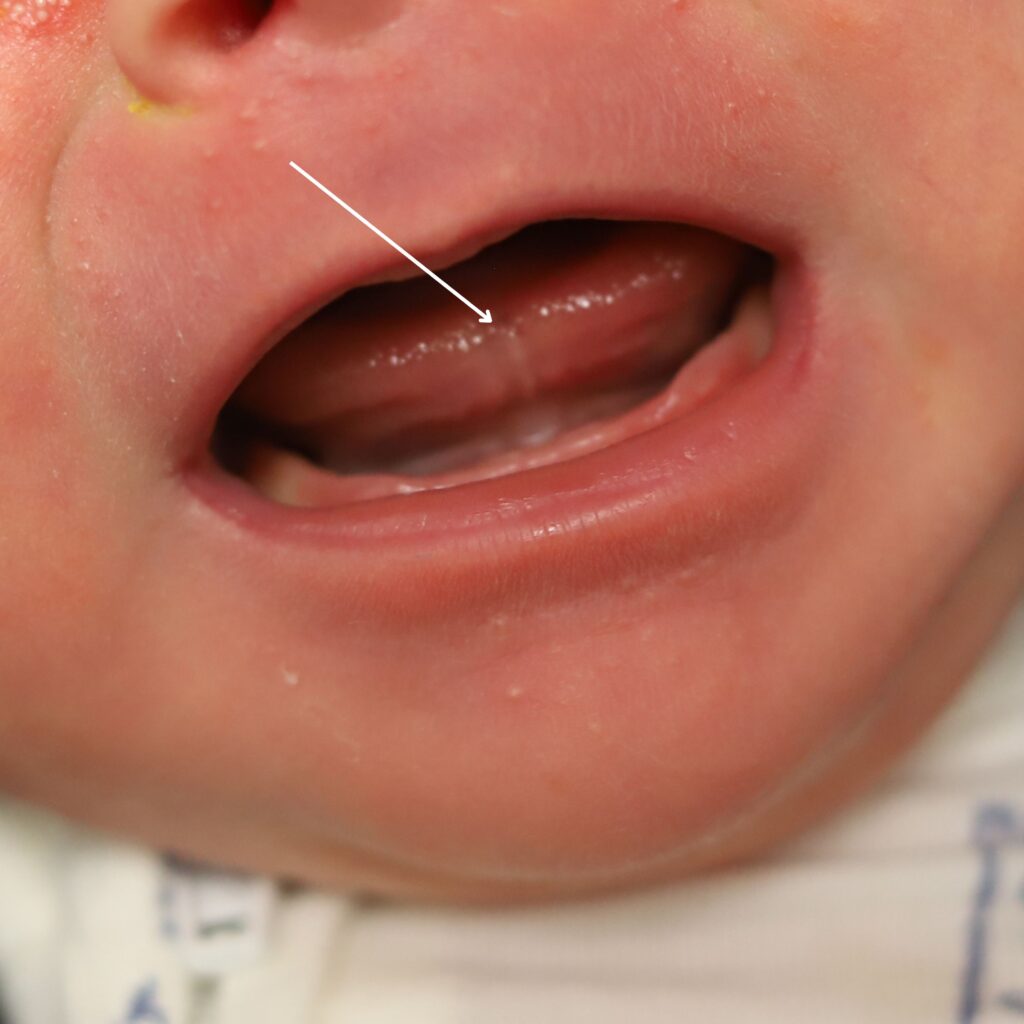
If you have any concerns about your infant’s oral cavity, seek evaluation from a knowledgeable pediatrician. Below are examples of an “anterior” frenulum that is attached from the end of the tongue to the gum line. These are generally addressed in the hospital or birth center before the baby goes home.
As the diagnosis of and interventions for tongue tie have skyrocketed in recent years, a reliable and evidence-based resource for reading further is the joint AAP and ENT society statement published in 2024. This is also a good video from Australia that illustrates the laser procedure itself and some of the controversies surrounding it.
“Bottle Refusal”
Breastfed babies may or may not take a bottle easily if they have only had feeding at the breast for several months. If you do anticipate returning to work and/or otherwise needing to express milk and feed using a bottle, you will want to introduce a bottle after breastfeeding is “well established” (usually a few weeks postpartum). You can pump or hand express once a day in lieu of feeding at the breast and have a partner, family member, or other caregiver offer the bottle. Infants may not take a bottle from mom as they would rather breastfeed.
Some infants will take very little from a bottle at all, and drink just enough to hydrate. Different nipples or bottle types may or may not entice an infant to take a bottle. Over time, they eventually may take more volume — but it isn’t abnormal if they don’t. It isn’t because their newborn “suck” reflex has disappeared. It’s simply because they don’t want the bottle.

Jaundice

Jaundice can be divided into “breastfeeding jaundice” (sometimes called “Not enough breastfeeding jaundice”) and “breastmilk jaundice.” A management schematic is detailed in the Academy of Breastfeeding Medicine Jaundice Protocol.
Some babies are more likely to develop jaundice, such as a different blood type than mom (ABO incompatibility), as well as those of Asian and Native American descent. If a baby is urinating and stooling and regaining birth weight appropriately, there is no indication to introduce formula (in fact, this may take a baby who is breastfeeding well and interrupt physiology of mom/baby connection).


However, if a baby is not urinating or stooling appropriately, has lost excessive amounts of weight, and is jaundiced, this is dangerous. This baby requires donor milk or formula supplementation. The baby also may require use of phototherapy (“bilirubin lights” or “bilirubin blanket”).
Other infants may remain jaundiced for a longer period of time (weeks) despite adequate weight gain, which is called “breastmilk jaundice.” It is harmless, and is related to a substance in breastmilk preventing the baby’s immature liver from processing bilirubin.

