What is mastitis?
Mastitis is a painful inflammation of breast tissue. Symptoms can include pain, swelling, warmth, and redness in the affected breast. The vast majority of the time, it is not infection and can be treated with ice and over-the-counter anti-inflammatory/pain medication as well as not overfeeding or overpumping.
When should antibiotics be used to treat mastitis?
Very few cases of mastitis need antibiotics when the issue is treated appropriately from the very beginning.
Remember that antibiotics are NOT harmless. There is widespread antibiotic resistance at this point (so very often, the effect people may get when they use antibiotics is anti-inflammatory and not antibacterial).
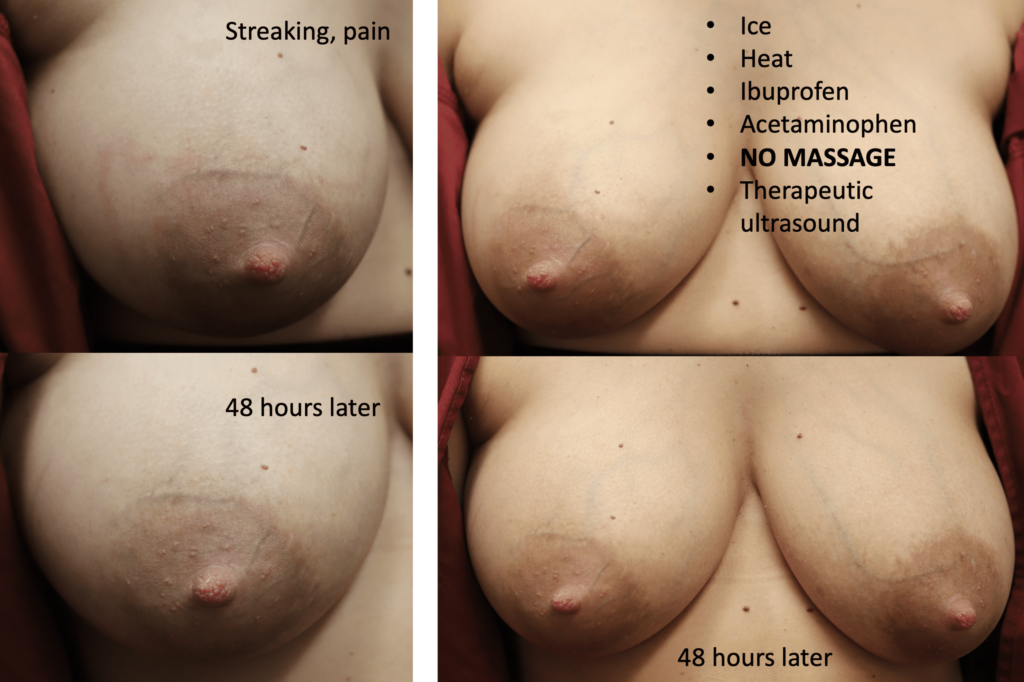
The photos below are a good example of a very bad drug reaction to dicloxacillin, the “first line” antibiotic for mastitis and not a particularly strong one. Others, such as Bactrim, can cause life-threatening rashes, blistering, and skin loss (equivalent to a total body burn) as well as life-threatening pneumonitis (inflammation of the lung). Clindamycin can cause life-threatening c difficile colitis (infection of the colon that can require emergency removal of the intestines and intensive care treatment).


Are antibiotics effective for treating mastitis?
If you have massaged your breast and caused tissue trauma/cell death, you may need antibiotics to treat a true infection. This should start to improve within 24-48 hours.
There are also rare situations when patients develop an infection without massaging. Usually, these involve cases of hyperlactation and pumping or pumping exclusively. Even still, all conservative measures (ice, not pumping, advil/tylenol +/- therapeutic ultrasound if you have that available) should be attempted in these scenarios for 24 hours before starting antibiotics.
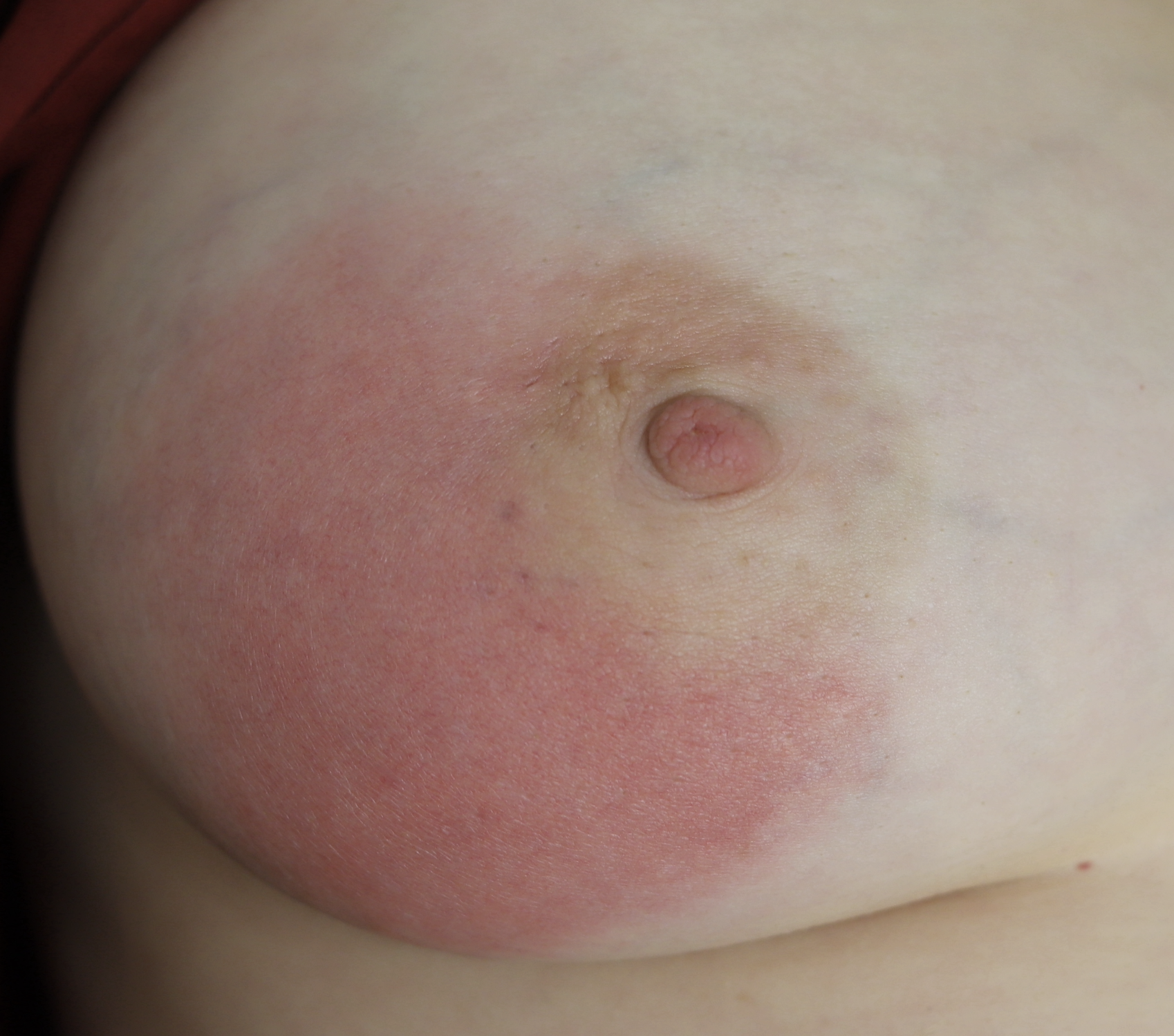 The above photo is a true case of mastitis requiring antibiotics in the setting of a patient not massaging or overfeeding. However, she had persistent hyperlactation and was needing to pump at work and developed a bleb. After 24 hours of no improvement despite ice, anti-inflammatory medication, and therapeutic ultrasound, we started antibiotics.
The above photo is a true case of mastitis requiring antibiotics in the setting of a patient not massaging or overfeeding. However, she had persistent hyperlactation and was needing to pump at work and developed a bleb. After 24 hours of no improvement despite ice, anti-inflammatory medication, and therapeutic ultrasound, we started antibiotics.
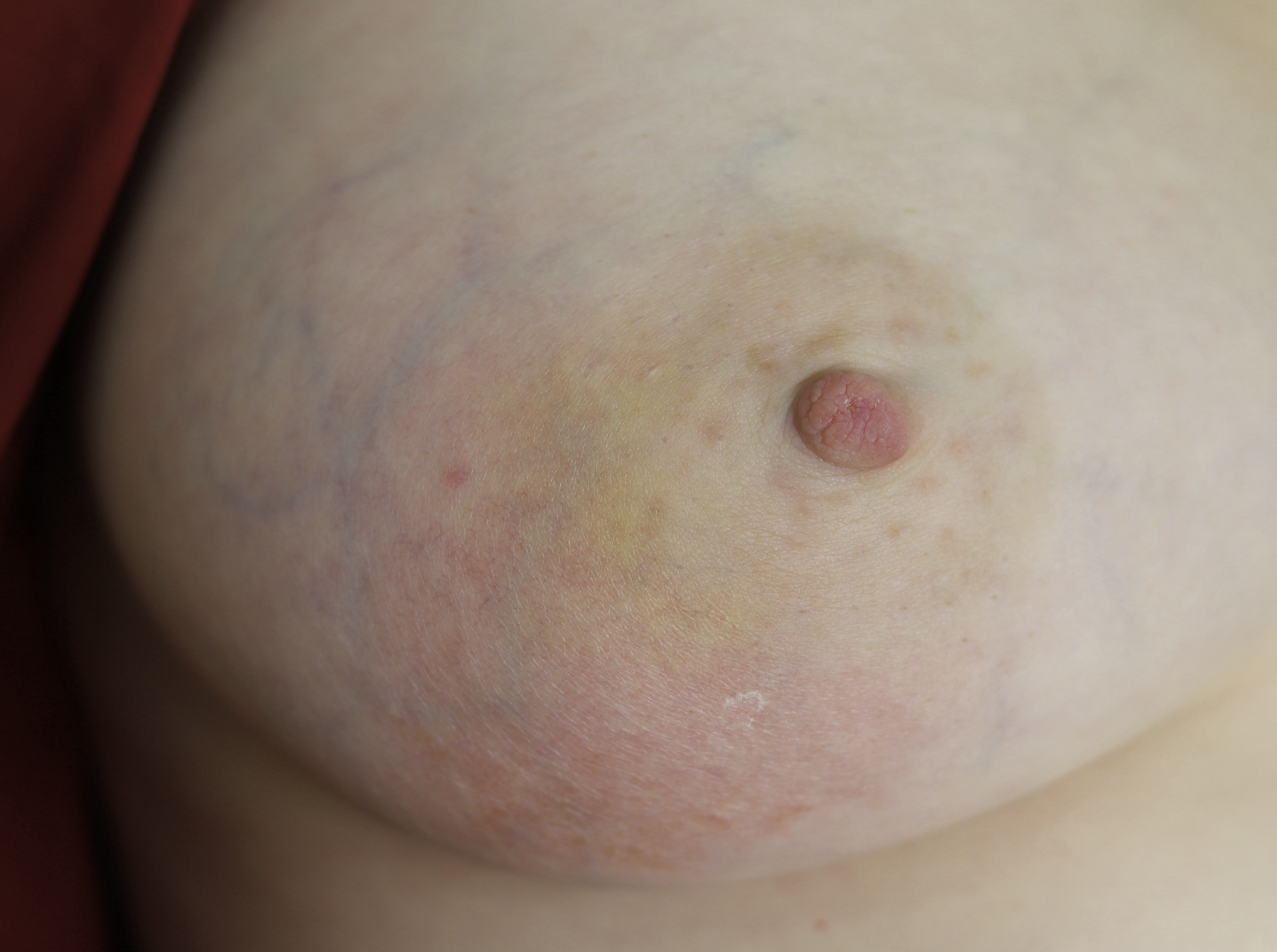 Mastitis improving after 3 days of antibiotics.
Mastitis improving after 3 days of antibiotics.
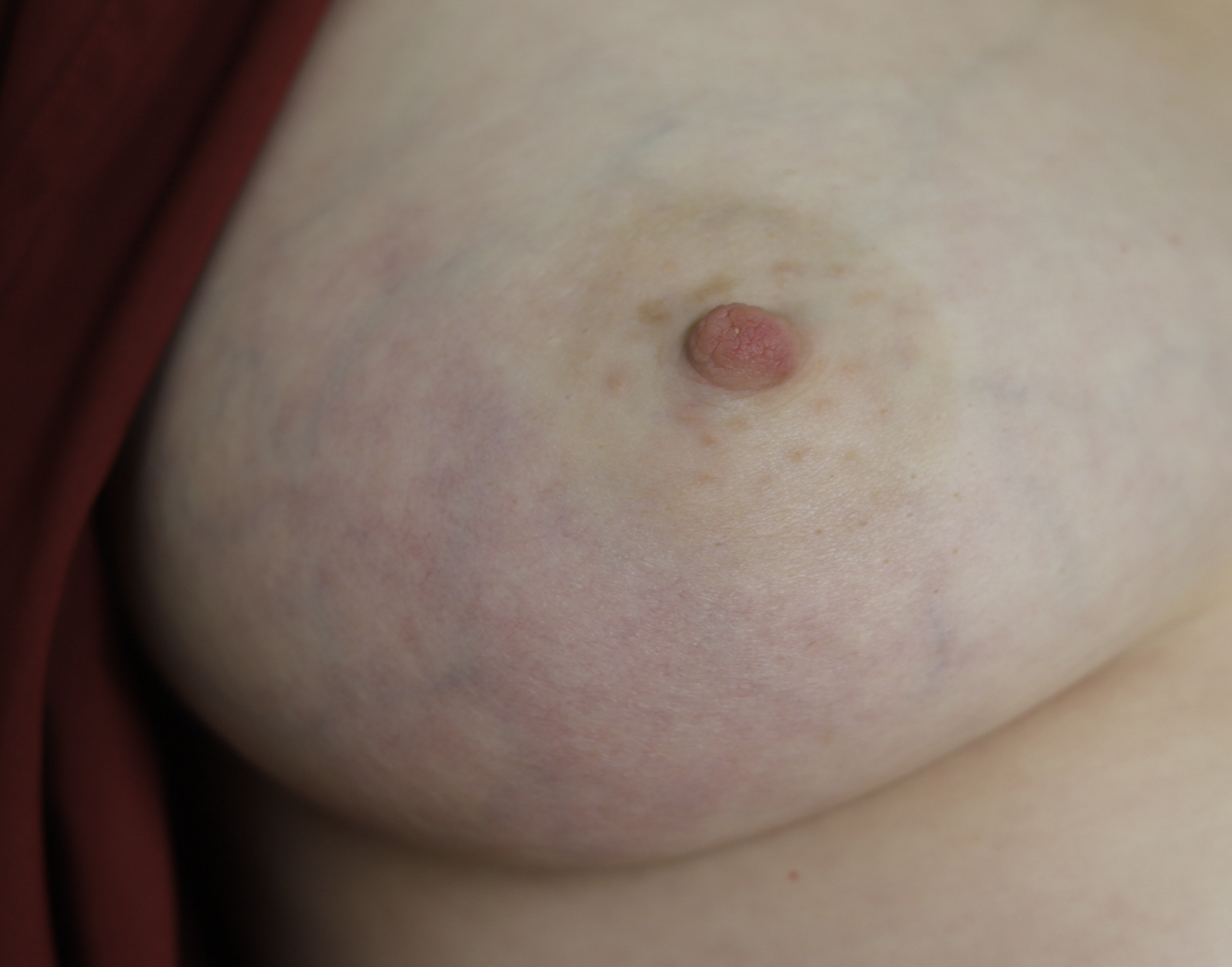 Mastitis completely resolved after one week. Note that regardless of skin tone (light or dark), it always takes some time for background inflammation (light redness) to return to normal.
Mastitis completely resolved after one week. Note that regardless of skin tone (light or dark), it always takes some time for background inflammation (light redness) to return to normal.
Is antibiotic treatment safe for my baby while breastfeeding?
Antibiotics are safe with breastfeeding and there is no need to “pump and dump.”
What to do if you have symptoms of mastitis
With early inflammatory mastitis, patients should use BAIT (Breast rest, Advil, Ice, Tylenol). Ice is generally the most helpful, but some people also prefer heat. Therapeutic ultrasound can use thermal energy to reduce inflammation and pain, as can lymphatic drainage.
I can’t repeat it enough — without question, do NOT MASSAGE the breast! Treat it like a sprained ankle. It will hurt more if you massage it.
If you suspect you could have mastitis, follow the above recommendations and seek evaluation if you do not improve within 24-48 hours.
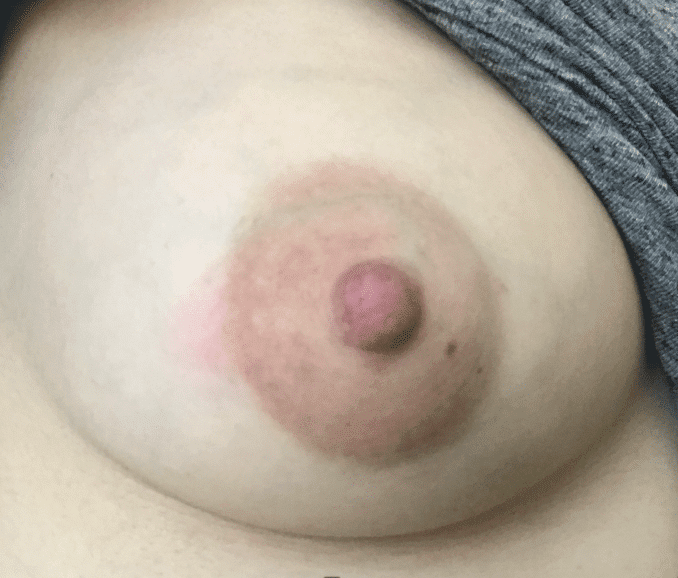
It is a myth that mastitis can develop suddenly after a day of skipped pumping at work or after a baby sleeps through the night. When these situations occur, moms experience transient engorgement, swelling, pain, and they may even have breast redness from congested capillaries and “interstitial fluid” (fluid that lives in connective tissue spaces throughout the body).
Because the breast has such incredible blood supply during lactation, this engorgement can result in inflammation and even fever or other systemic symptoms. However, unless a person has developed a very rare rapidly progressive soft tissue infection, it is impossible to develop infection this quickly.
When people ask how they can get hot, sweaty, and shaky with chills in the absence of infection, I explain the the sympathetic nervous system’s relationship with stress. In the setting of fearing mastitis, women may experience an early symptom and then become quickly more alarmed. It’s the same way we sweat and may even shake when nervous about something like public speaking.
All things red that cause fever are NOT infectious. Other examples in the body include blood clots (which can cause leg redness, swelling, pain, and fever), Systemic Inflammatory Response Syndrome (can occur after a bad traffic accident with multiple sites of body injury, not infection), bleeding in the brain, and pancreatitis.
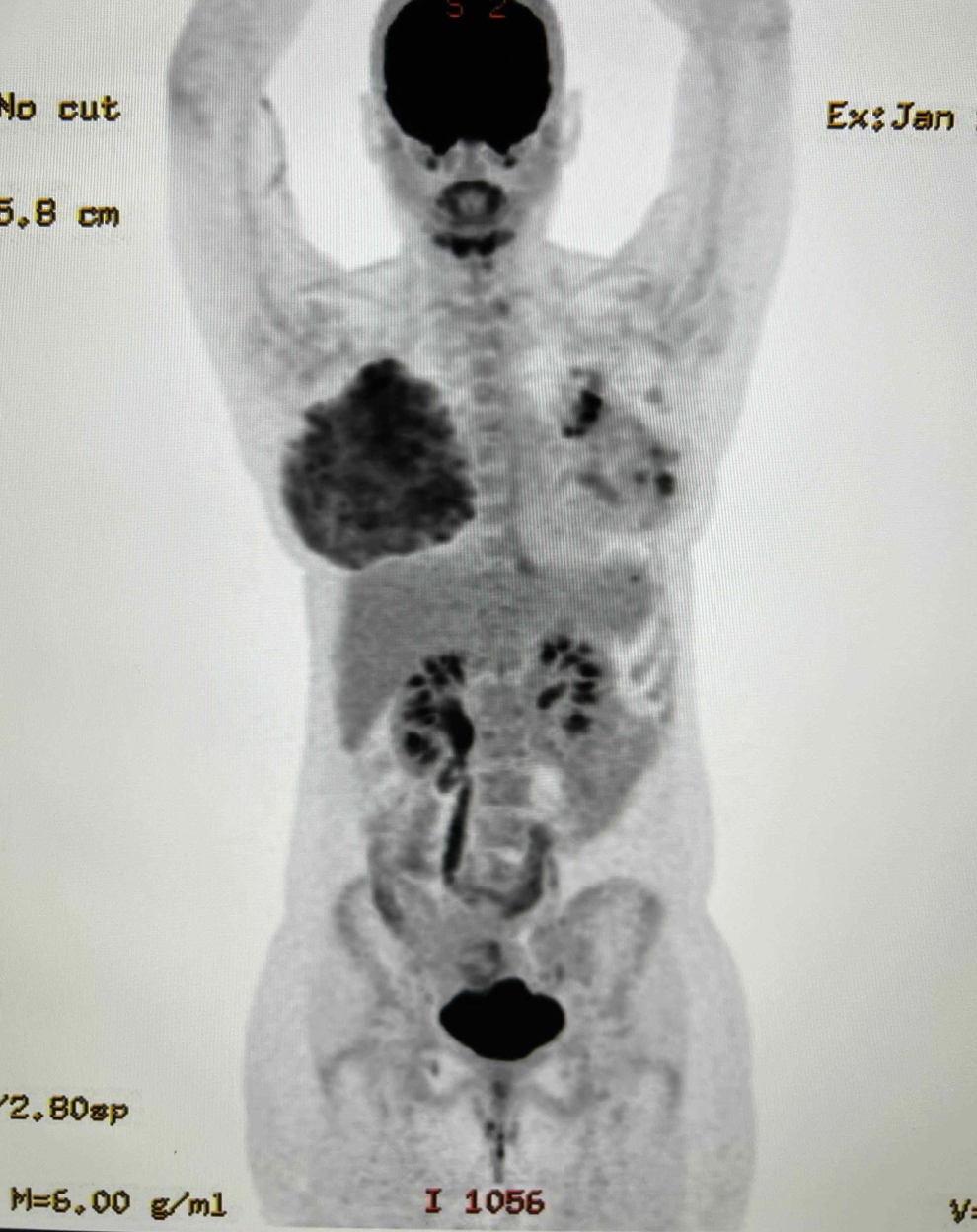
As an example of how extremely metabolically active the lactating breast is, a PET scan performed above for a left breast cancer (shown by the black areas in the left breast) demonstrates the remarkable lactating breast (right). This patient was mainly feeding on her right breast due to skin changes and inability to feed the infant on her left breast with cancer. You see that the lactating breast is actually MORE “FDG avid” (meaning it takes up more of the radio nucleotide, FDG, that the PET scan uses to determine metabolic activity) than the breast cancer itself!
The lactating breast is EXTREMELY active and powerful! THIS is why people can feel so bad with engorgement and inflammation. There is a LOT of blood flow and metabolic demand feeding the breasts during breastfeeding!
With early inflammatory mastitis, patients should use BAIT (Breast rest, Advil, Ice, Tylenol). Ice is generally the most helpful, but some people also prefer heat. Therapeutic ultrasound can use thermal energy to reduce inflammation and pain, as can lymphatic drainage. I can’t repeat it enough — without question, do NOT MASSAGE the breast! Treat it like a sprained ankle. It will hurt more if you massage it.
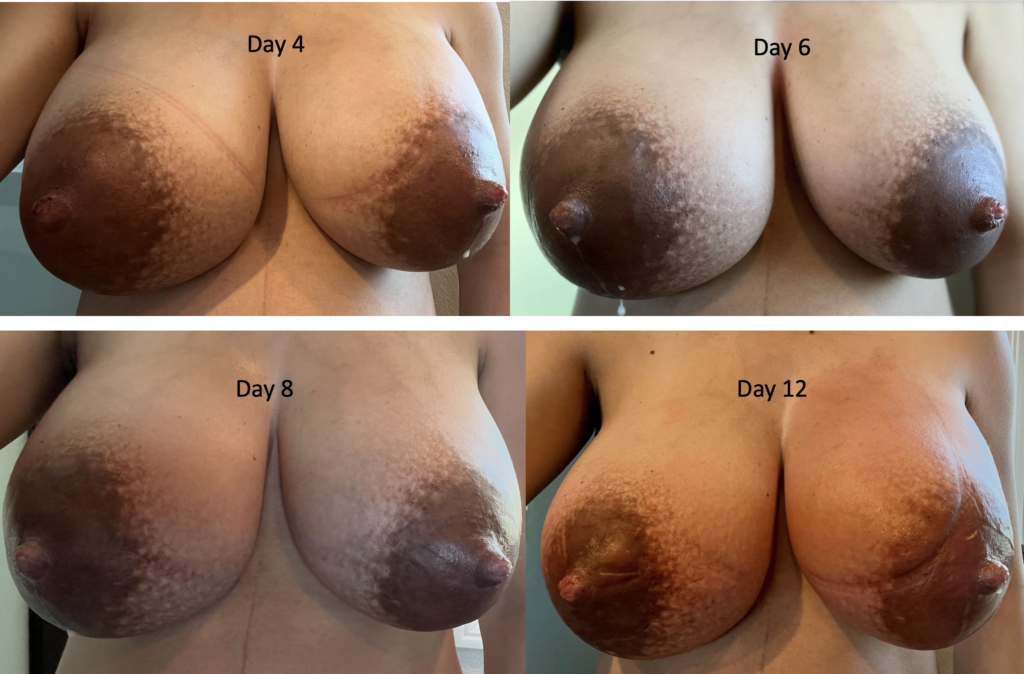
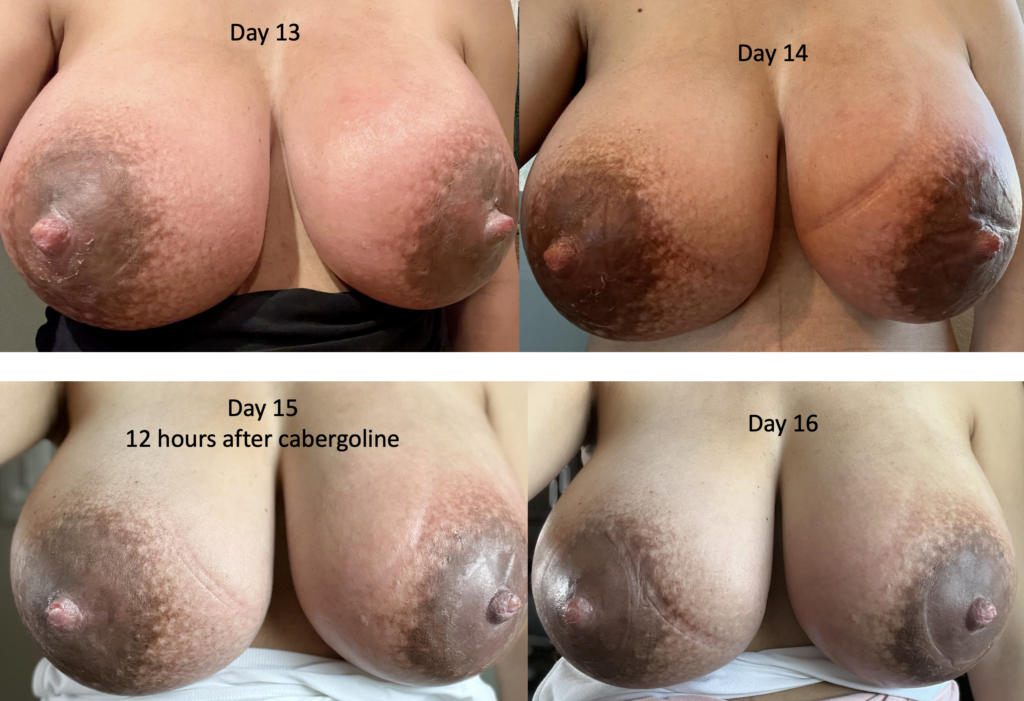
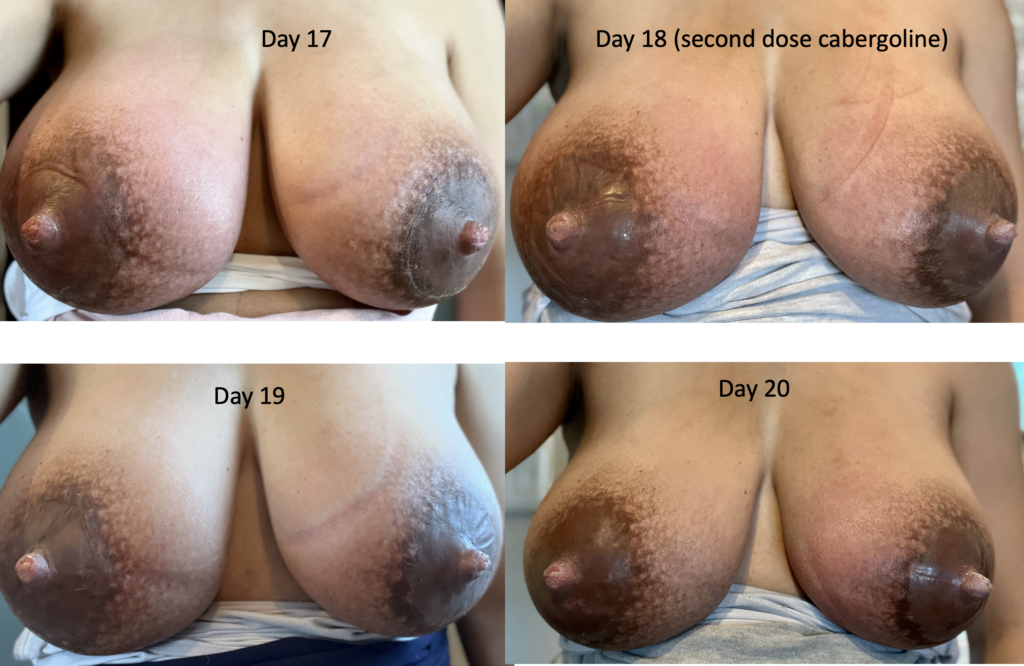
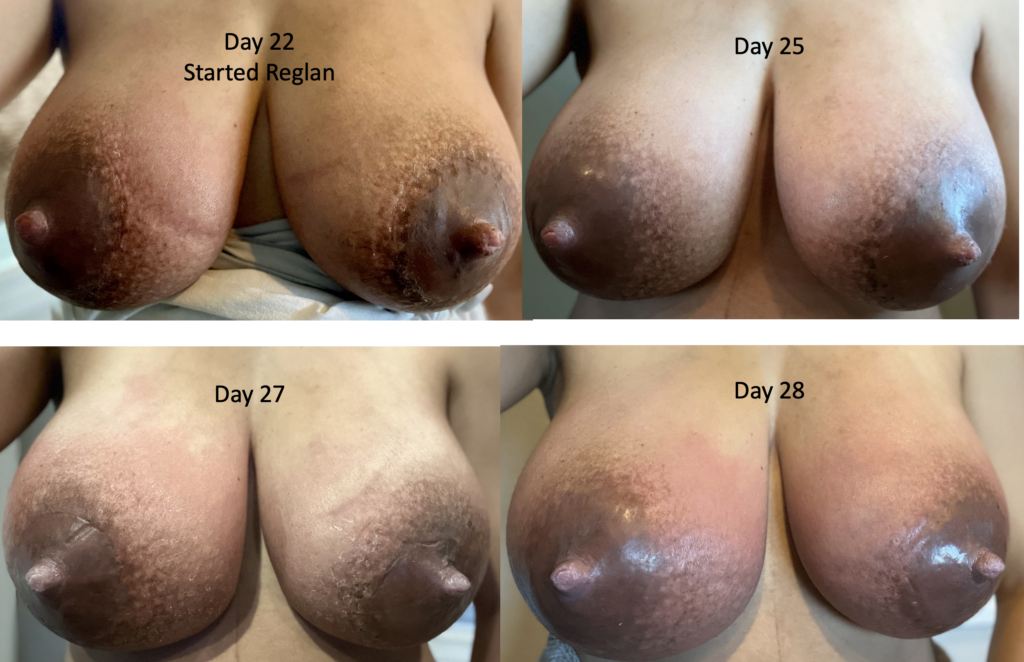
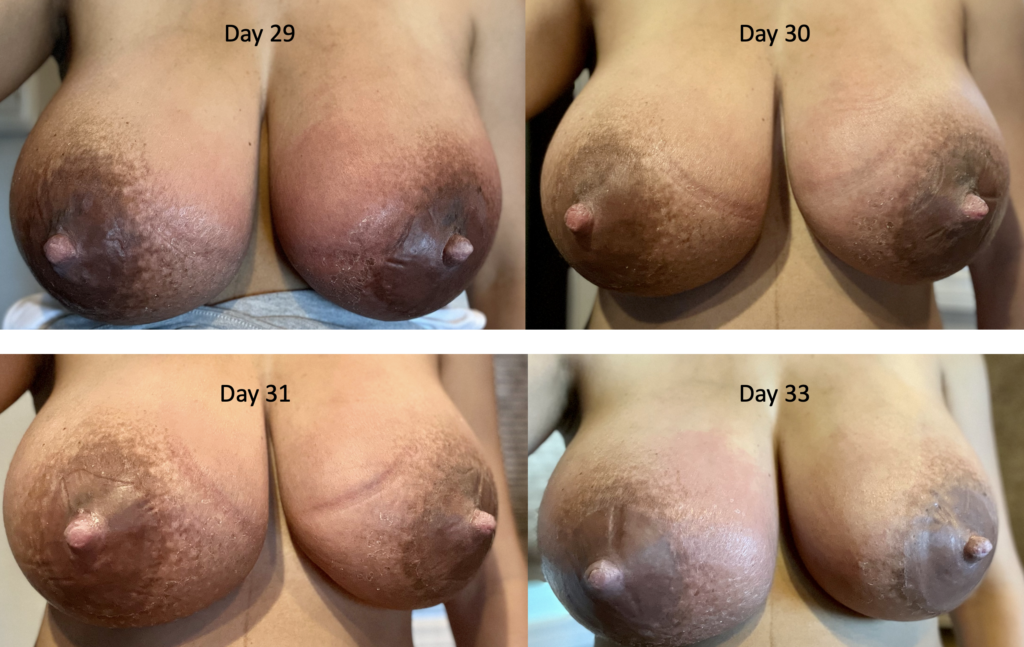
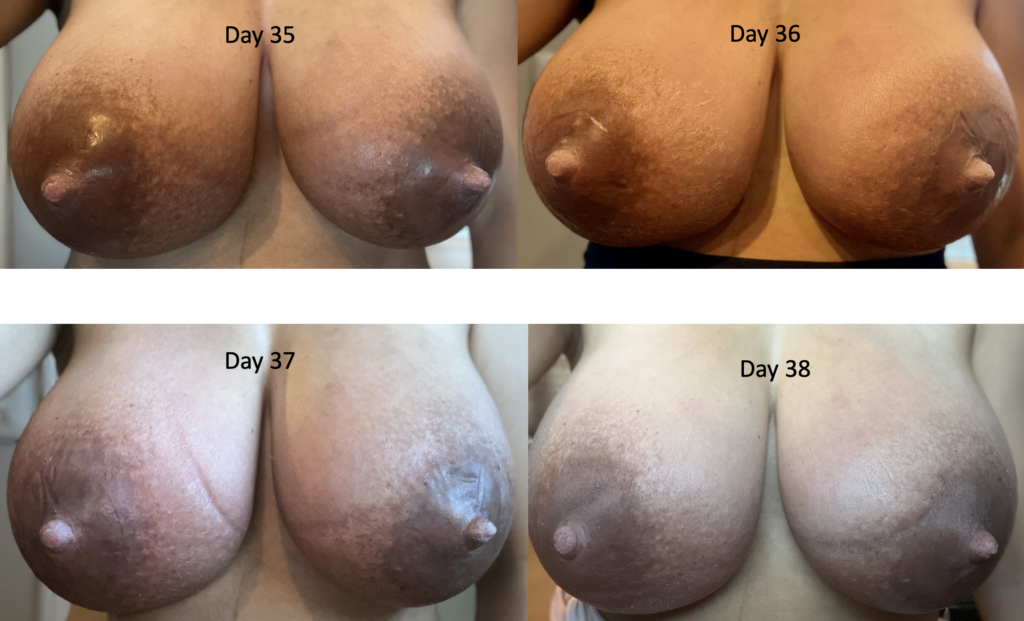
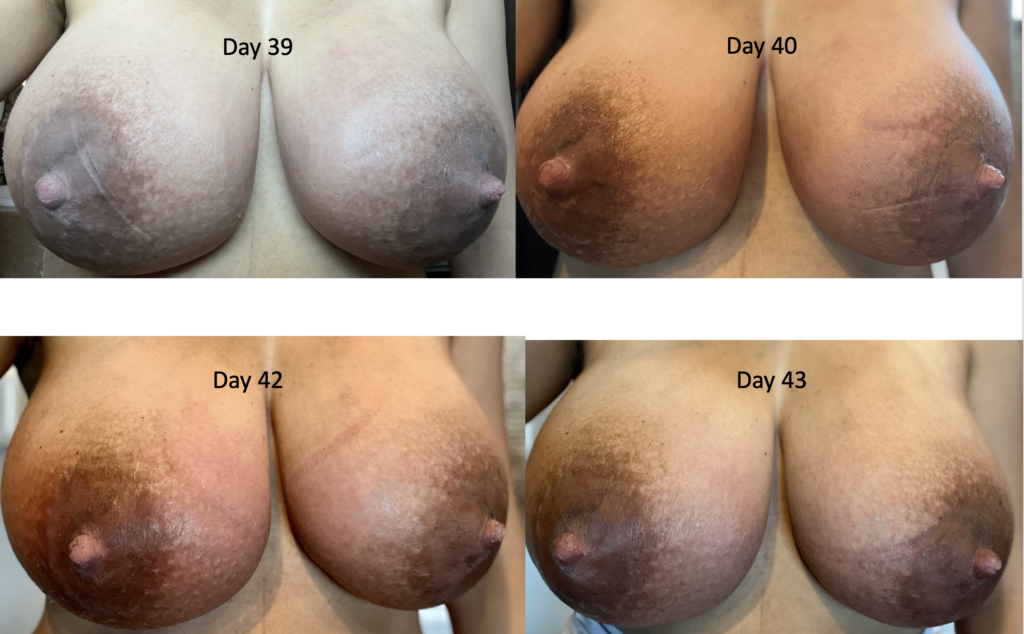
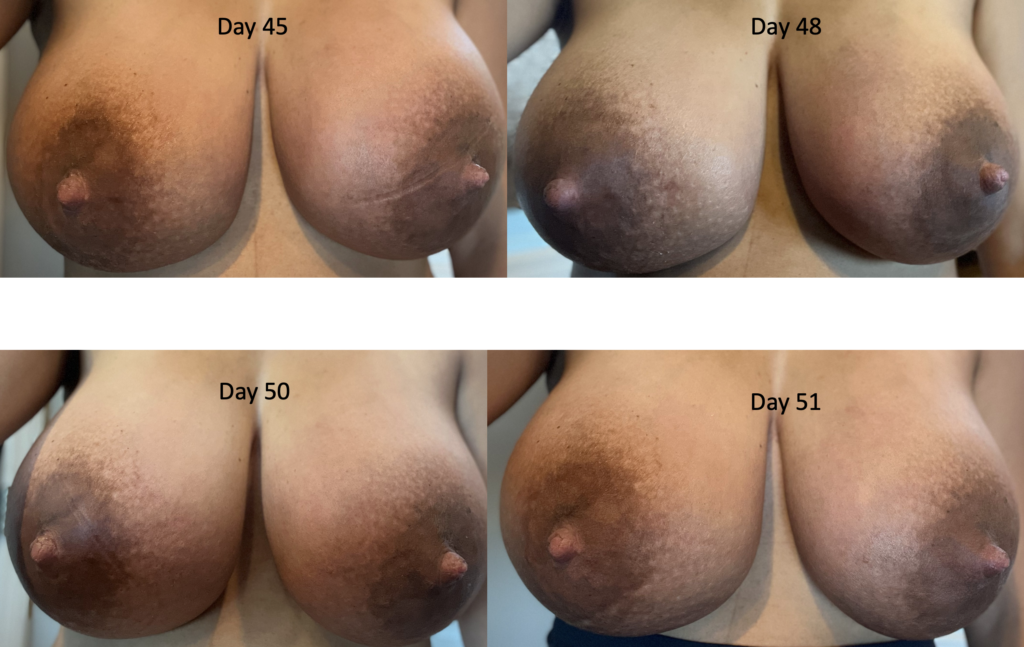
Below is a series of images from a patient with profound postpartum engorgement and hyperlactation (oversupply). She had experienced similar challenges with her first baby, but unfortunately had been admitted to the hospital multiple times for antibiotics (which, of course, were not effective). I met her at six months postpartum, stopped her antibiotics, downregulated her milk production, and she nursed for two years without any further issues.
With second baby, she graciously catalogued her breast changes over time to help other people understand that breasts can be quite red early postpartum, but it’s not infection (it’s dilated blood vessels, fluid collecting in the breast, overproduction of milk). They need down regulation of milk, lymphatic drainage, and good bras until they settle out.