
We recently published with the American Society of Breast Surgeons an Executive Summary of oncolactation, the intersecton of breast cancer care and lactation. Our first and senior author reflection elaborates on future directions.
Pregnancy is safe after breast cancer.
In fact, women who become pregnant after breast cancer treatment have improved survival compared to those patients who do not have a pregnancy.
Avoid Double Mastectomy Prior to Pregnancy
Sometimes a mastectomy is necessary for young women with breast cancer. However, young women should be counseled against removing a normal breast (“contralateral prophylactic mastectomy” or “double mastectomy”) on the non-cancerous side before they finish having children.
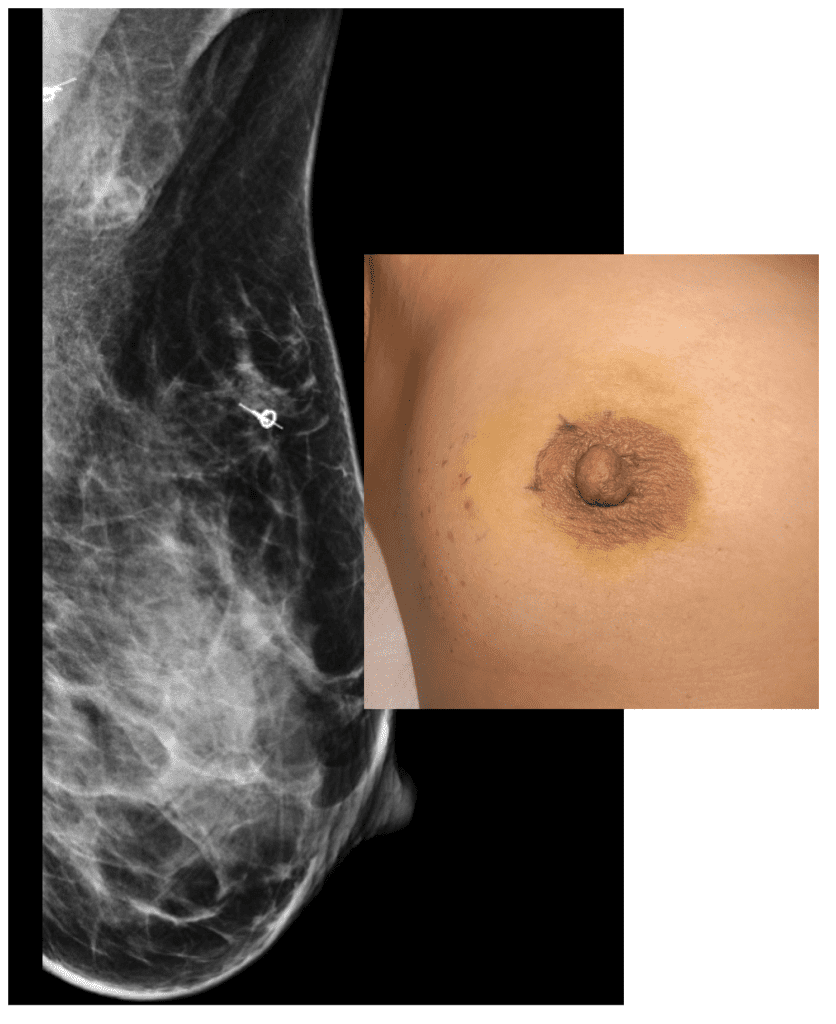
 Exclusively breastfeeding on unaffected left breast after chemotherapy, immunotherapy, lumpectomy, radiation, and endocrine therapy for her right breast cancer.
Exclusively breastfeeding on unaffected left breast after chemotherapy, immunotherapy, lumpectomy, radiation, and endocrine therapy for her right breast cancer.
Young patients unfortunately are at much higher risk of developing metastatic disease in other places in their body (liver, lungs, bones, brain) than a new breast cancer in the other breast during their childbearing years. All other organs in the body are treated with local excision (e.g no complete removal of a colon for a tumor in one location, no removal of both kidneys, eyes, testicles, lungs “just in case”). We don’t do preventative removal of all the skin in melanoma … we just remove the tumor.
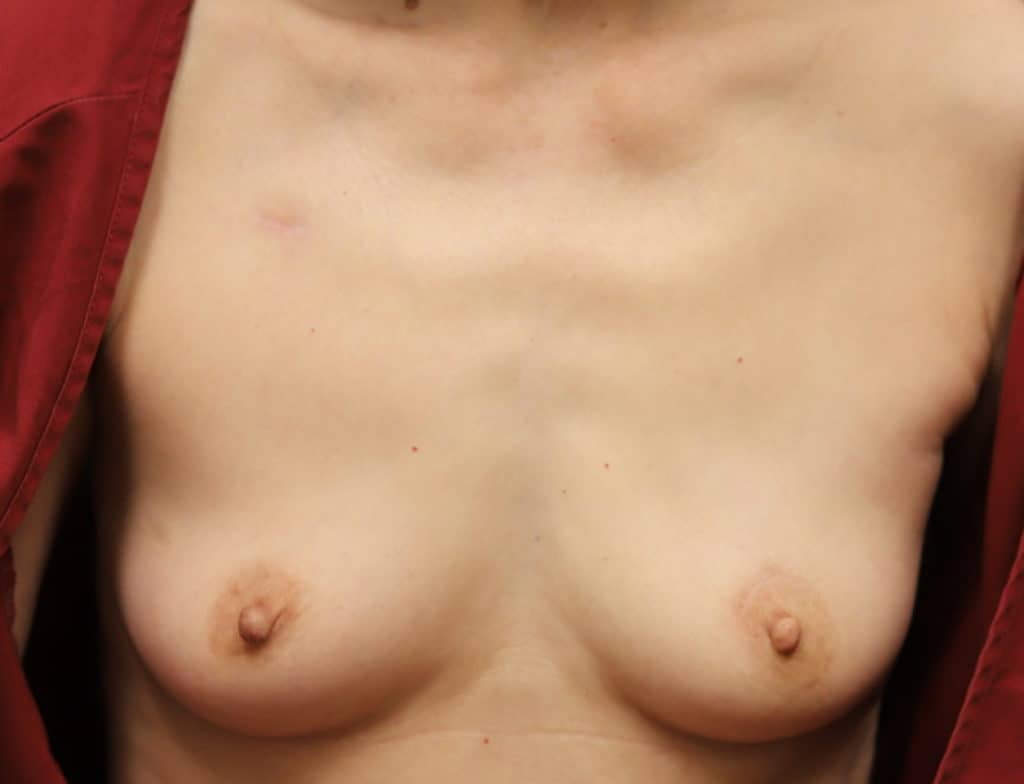
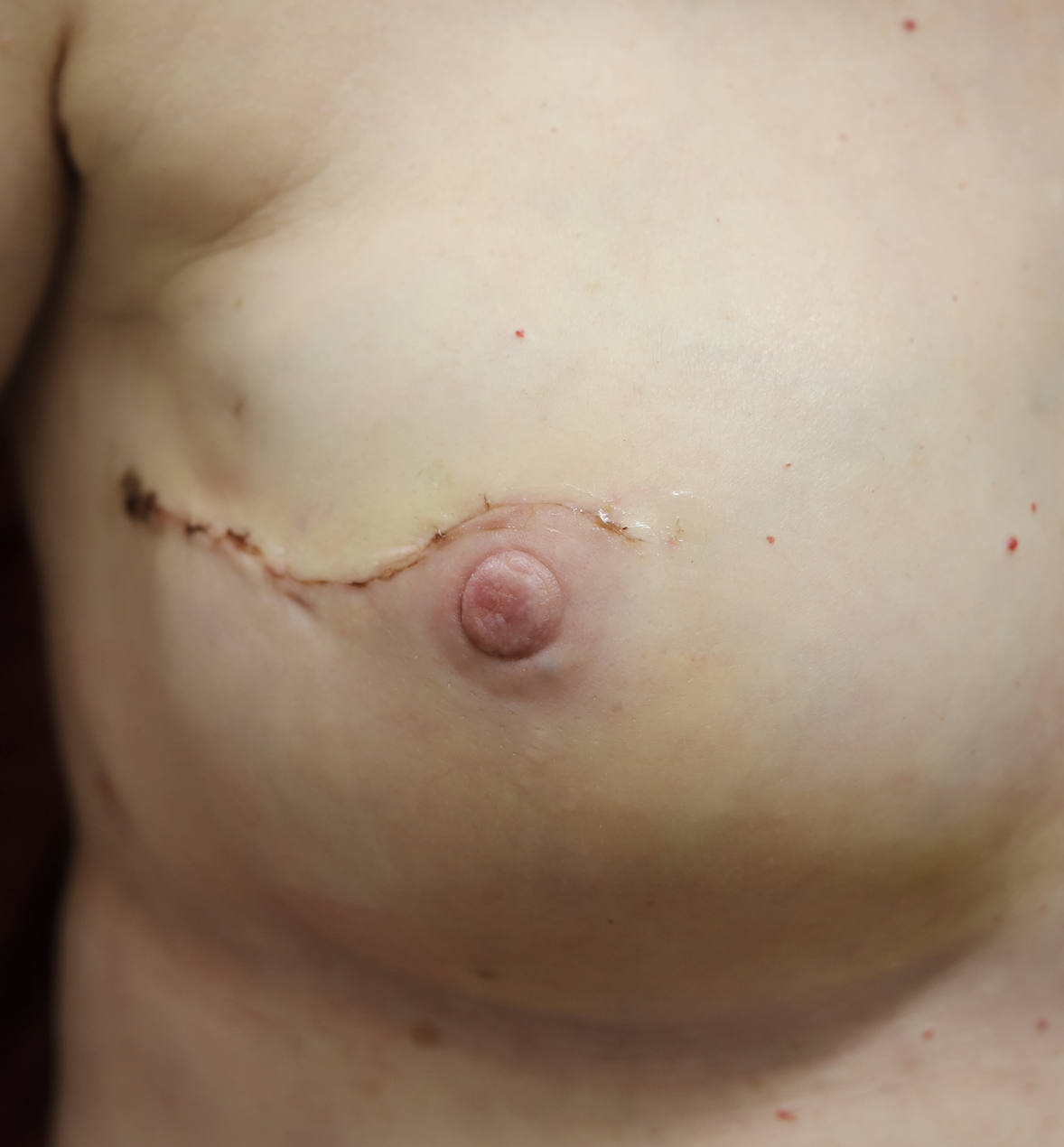 Right nipple sparing mastectomy with preservation of the left normal breast.
Right nipple sparing mastectomy with preservation of the left normal breast.
 Right nipple sparing mastectomy and tissue expander placement 10 days post op.
Right nipple sparing mastectomy and tissue expander placement 10 days post op.
Mastectomy is also unfortunately fraught with lifelong complications, and highly impacts sexuality and psychosocial aspects of a cancer survivor’s experience. And we now know that breast conservation, when possible, improves survival in young breast cancer patients. These articles from de la Cruz Ku, Orozco, and Pestana describe this in more detail.
In terms of lactation, preserving a normal breast allows a mom like this one above to breastfeed her baby (whether you have a mastectomy or lumpectomy with radiation, the cancerous breast will not lactate from either removal of all the tissue or radiation impact on remaining tissue in lumpectomy). In this Breastfeeding Medicine editorial, I discuss that we perform egg preservation before chemotherapy in young patients, and we should consider normal breast preservation to be equally as important. It’s also very important to note that breastfeeding significantly reduces the risk of ovarian cancer, particularly in patients with the BRCA mutation (additional articles under resources -> medical publications section of this website).
Treatment of Breast Cancer
- Previous chemotherapy does not preclude future breastfeeding. However, chemotherapy intended to concentrate in breast tissue to treat breast cancer may result in long-lasting effects on lactational ability. Patients should be referred for support and guidance during pregnancy and in the postpartum period.
- A history of a total mastectomy, skin sparing total mastectomy, or nipple sparing total mastectomy precludes breastfeeding on the affected side. Mastectomy removes 95% or greater of breast tissue. However, due to variation in mastectomy technique, some patients may have more residual functional breast tissue than others. This may grow during pregnancy and give the appearance of functionality. However, no normal lactation should be expected from this breast. If patients experience significant breast growth during pregnancy and/or milk production or engorgement postpartum, they should meet with their surgeon to discuss removal of residual tissue or future screening.
- Patients or lactation consultants may inquire about the idea of using a supplemental nursing system (“SNS” or feeding tube at breast) to give mom the experience of breastfeeding with the infant receiving nutrition via donor milk or formula in the tubing. I do not recommend using a SNS after a nipple sparing mastectomy or with a nipple reconstruction. A nipple preserved in a nipple sparing mastectomy still has ductal tissue through which the infant mouth or latch trauma could cause problems with underlying reconstruction (such as a breast implant). Reconstructed nipples are purely cosmetic, and extended suckling could cause tissue damage and infection.
- A history of partial mastectomy (“lumpectomy” or “segmental mastectomy”) does not preclude breastfeeding in itself. However, a patient with a history of partial mastectomy for cancer very likely would have undergo post-operative radiation therapy. Radiation therapy affects the functional ability of the breast, the elasticity of the skin, and its effects can continue for years after treatment. Limited lactational ability has been reported from a treated breast, but no normal lactation is expected. Instead, I encourage feeding on the unaffected breast and focusing on augmenting its production.
- Breast growth on the untreated breast is expected during pregnancy and lactation. Unusually significant growth should be investigated, as it is not possible to compare symmetry between breasts after one has been radiated. However, if imaging and biopsies do not show concerning findings, then a mom should be treated for breast lymphedema with lymphatic drainage and a supportive bra.
- Endocrine (anti-estrogen therapy) may be recommended following chemotherapy, surgery, and radiation. Due to suppression of lactation, transfer into breast milk, and suppression of estrogen in the infant, patients should not breastfeed while using endocrine therapy. The Pregnancy Outcome and Safety of Interrupting Therapy for women with endocrine responsIVE breast cancer (POSITIVE) trial demonstrated it was safe for breast cancer survivors to temporarily suspend endocrine therapy for pregnancy and breastfeeding.
- Detailed information about specific medications and lactation can be found at the National Institute of Health’s LactMed database or Texas Tech’s Infant Risk Center.
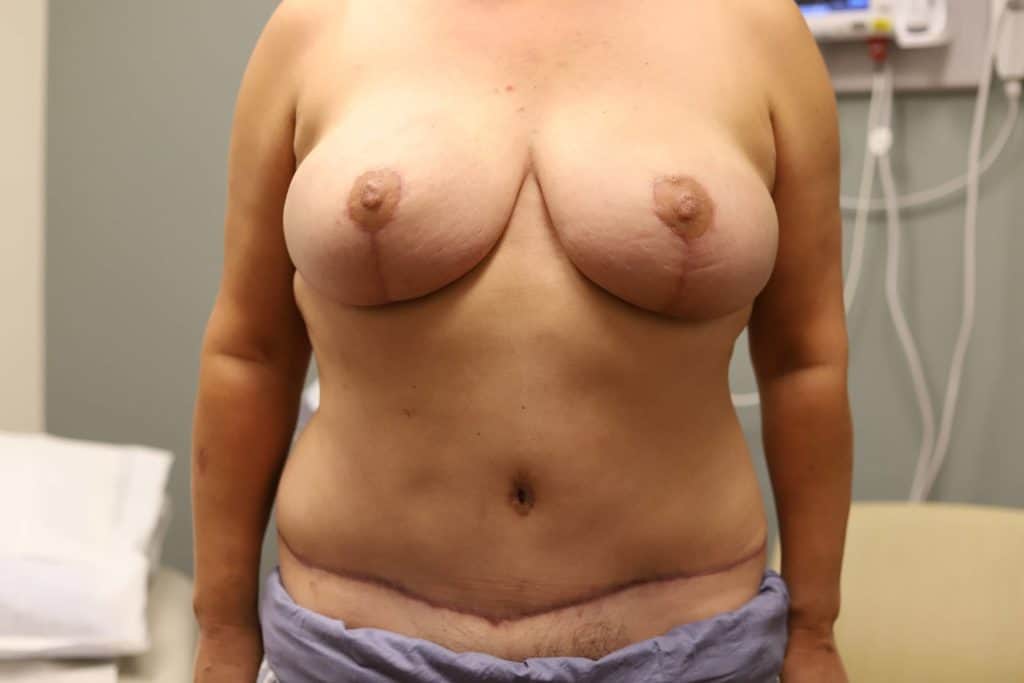
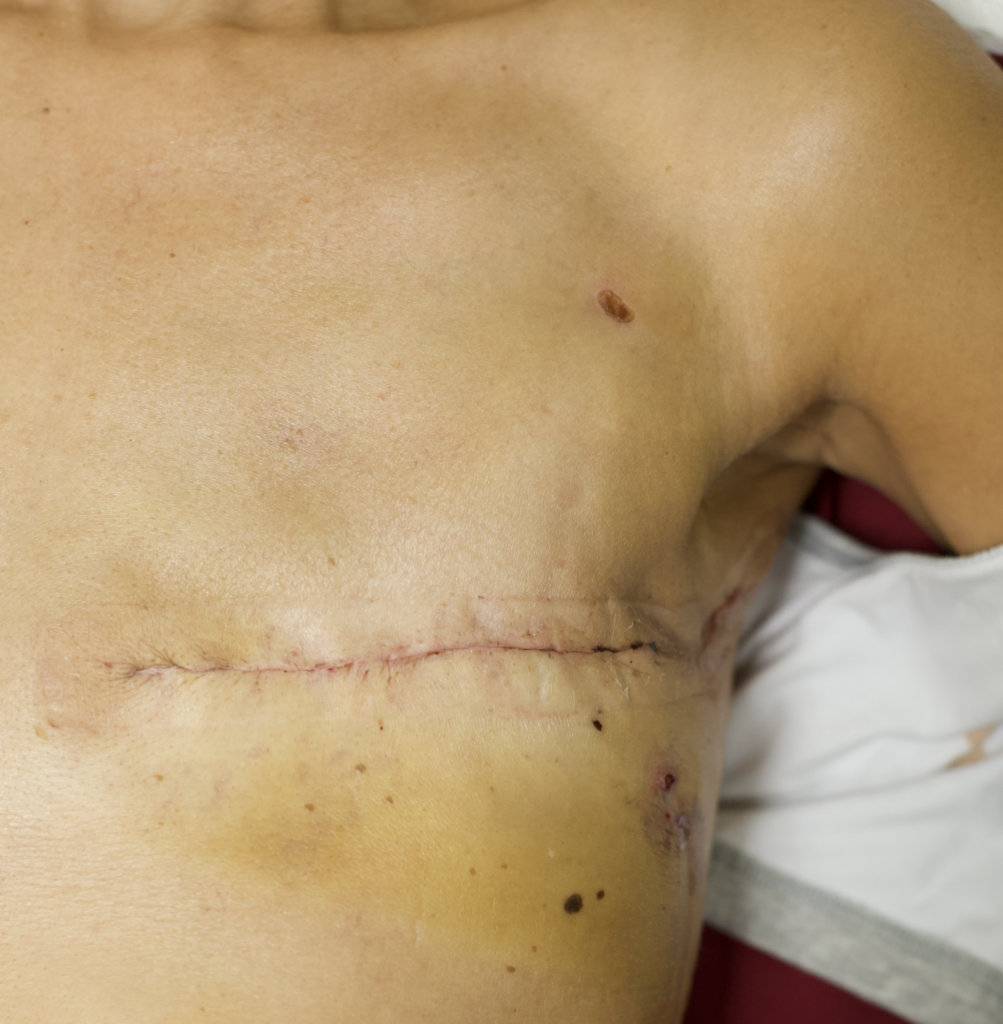
 Example of flat closure (older patient, not childbearing).
Example of flat closure (older patient, not childbearing).
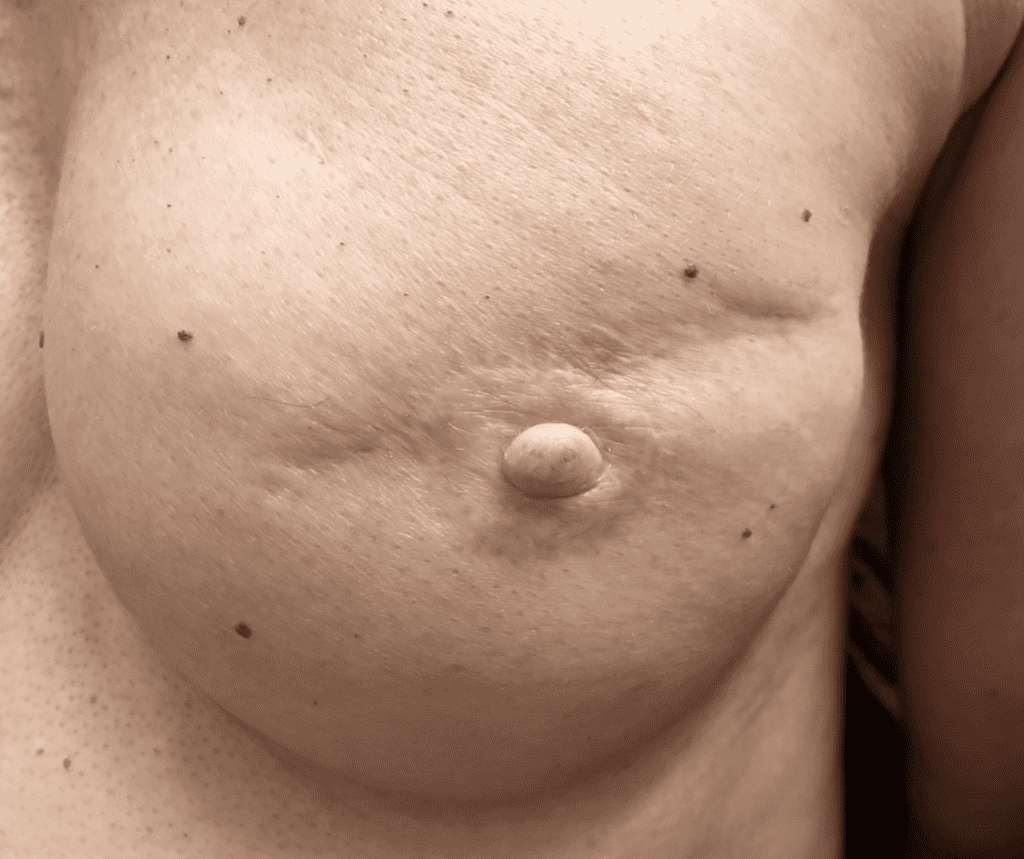





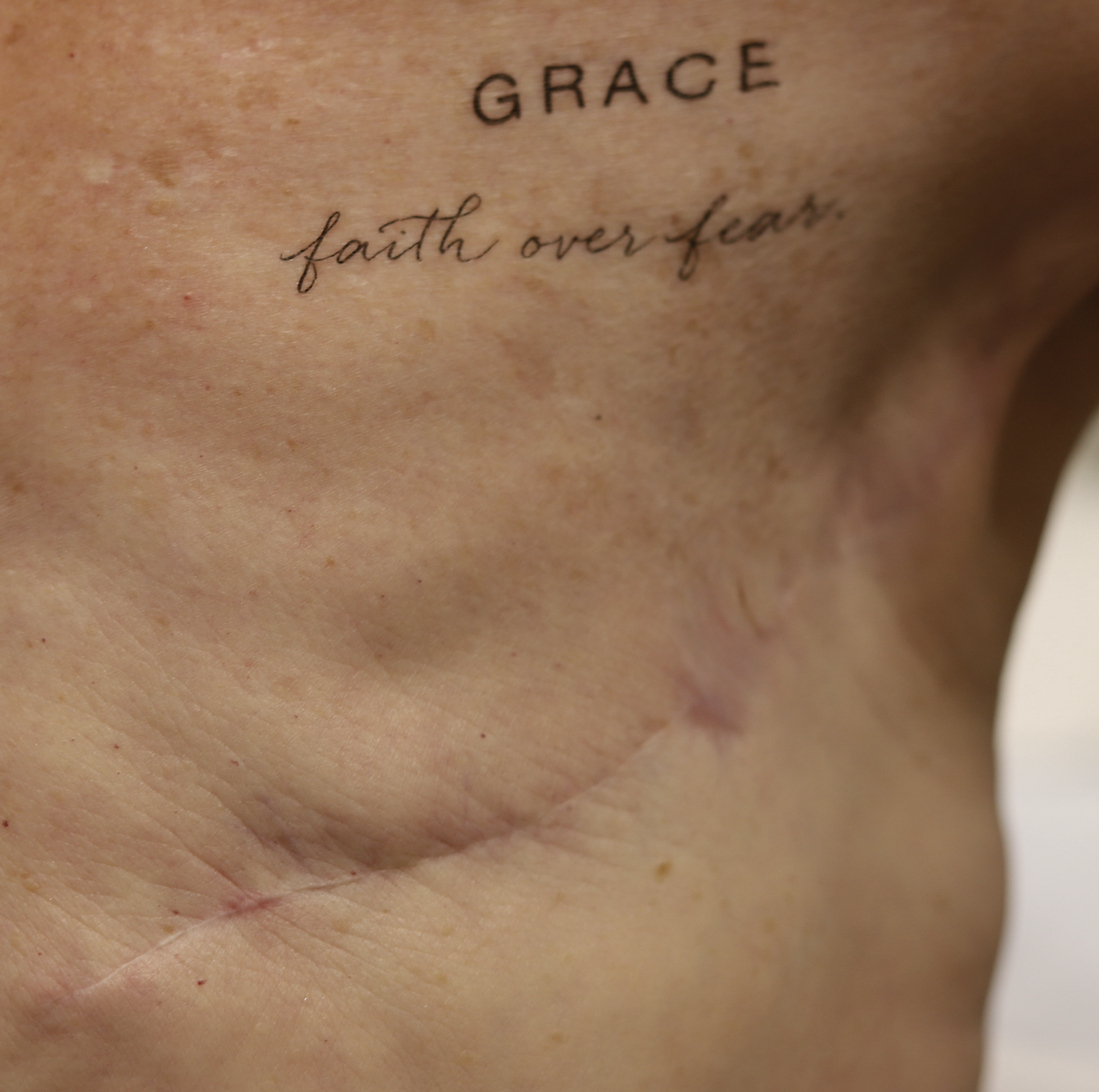
Recurrence of Breast Cancer
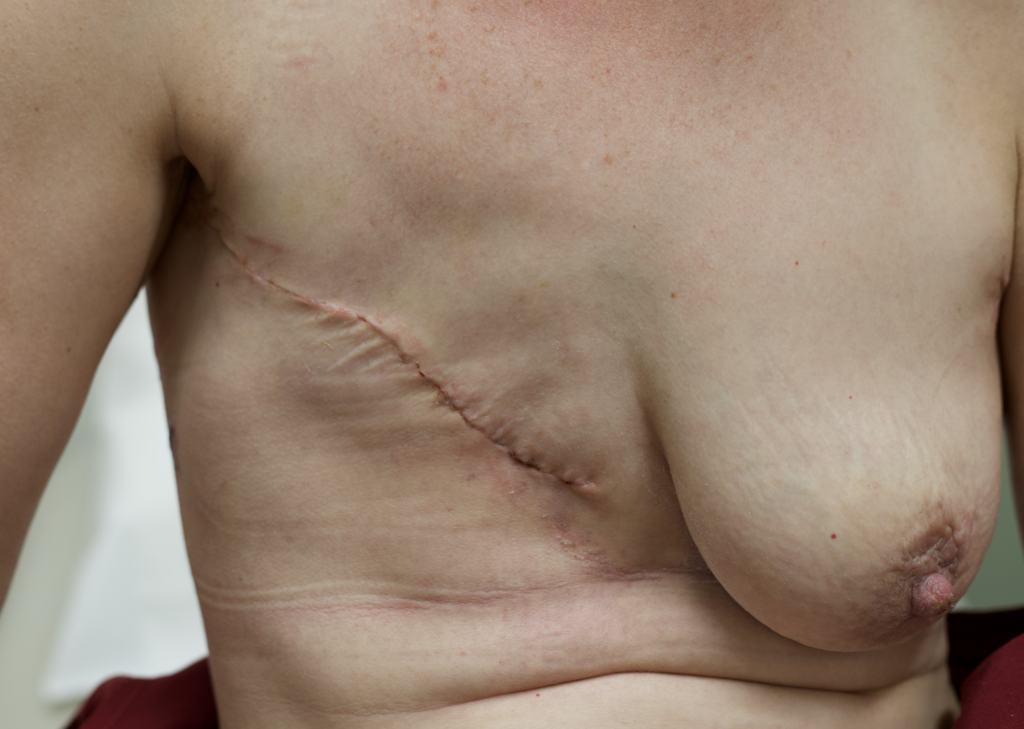
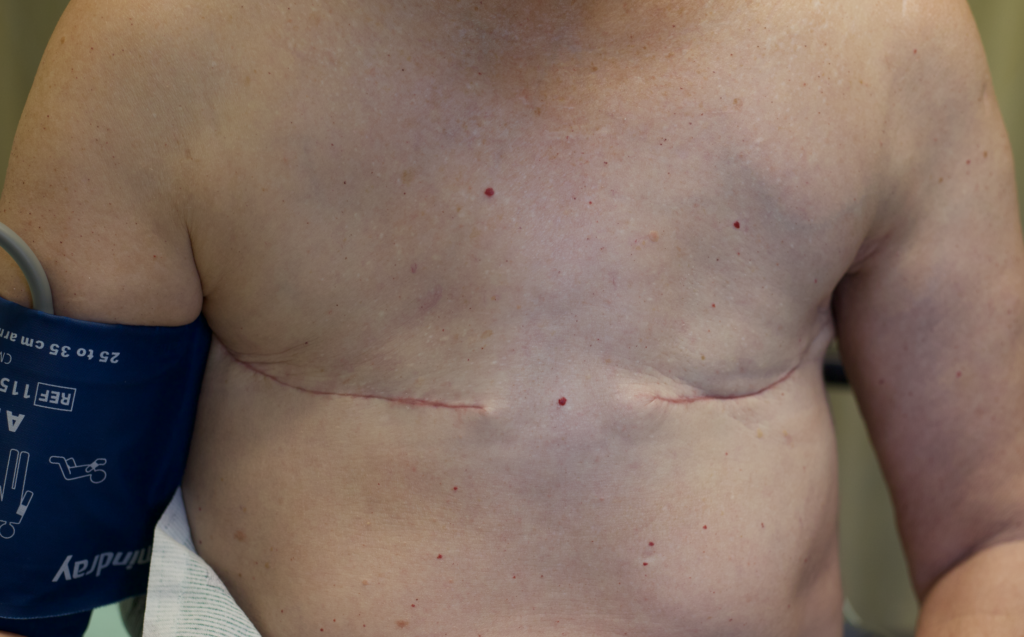
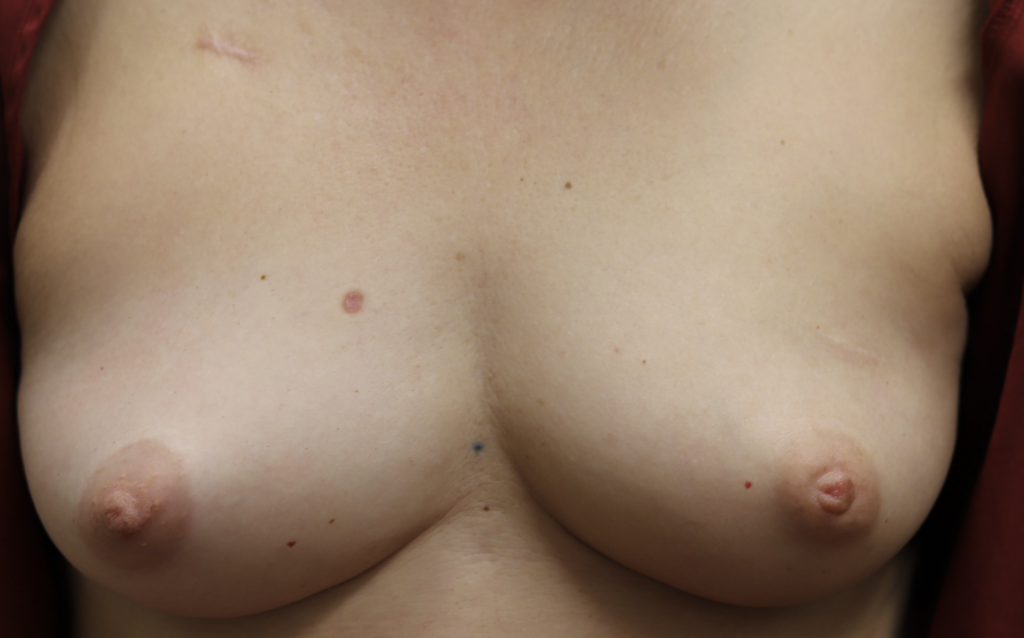
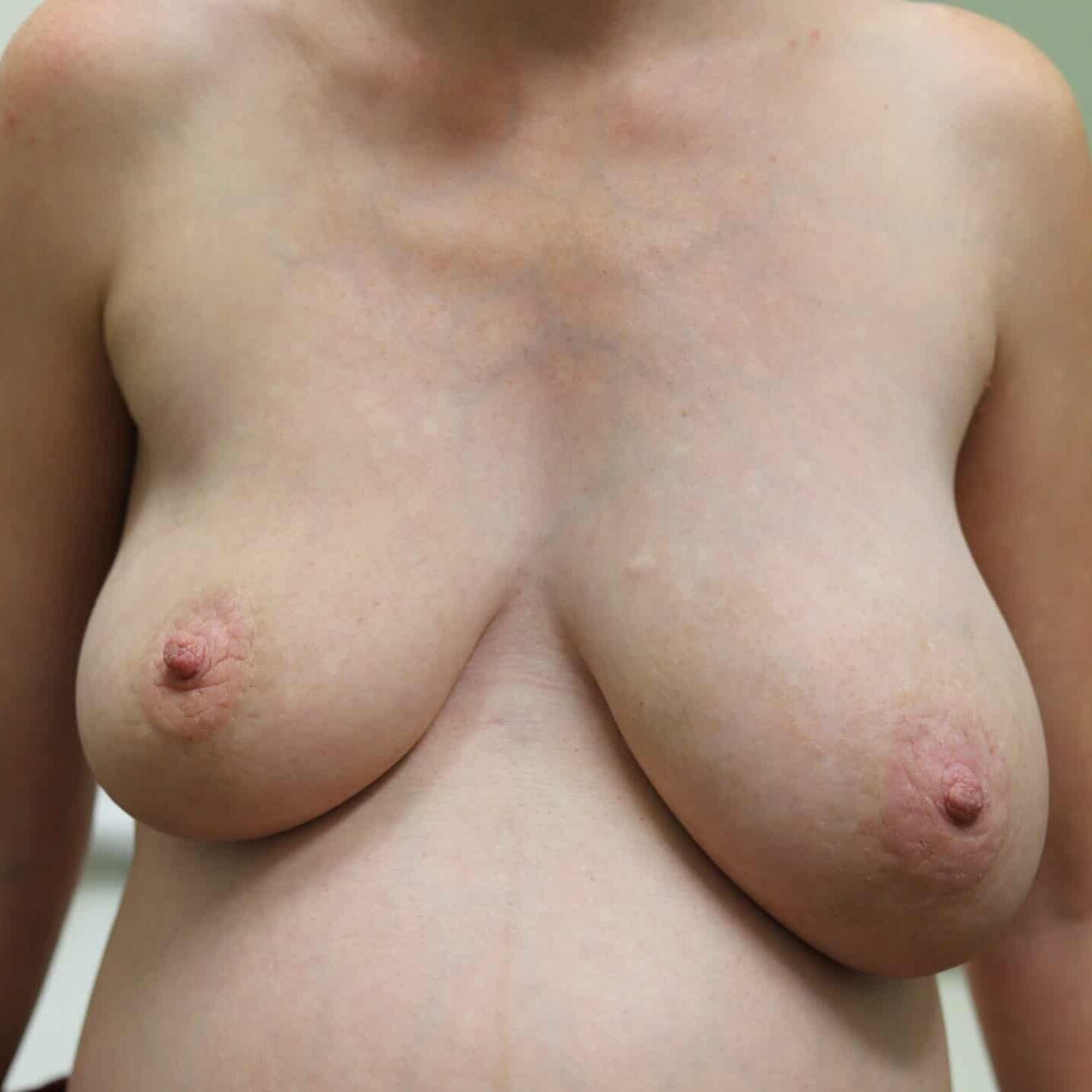
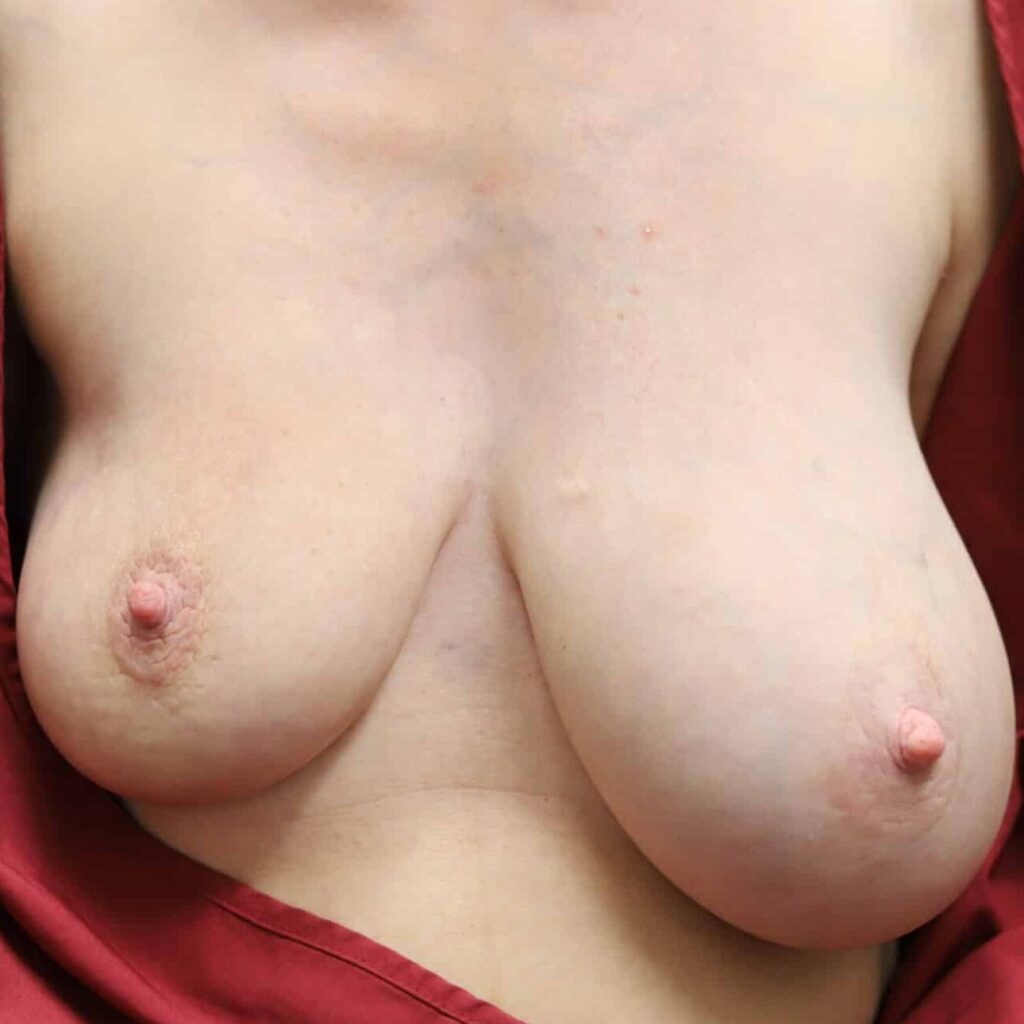
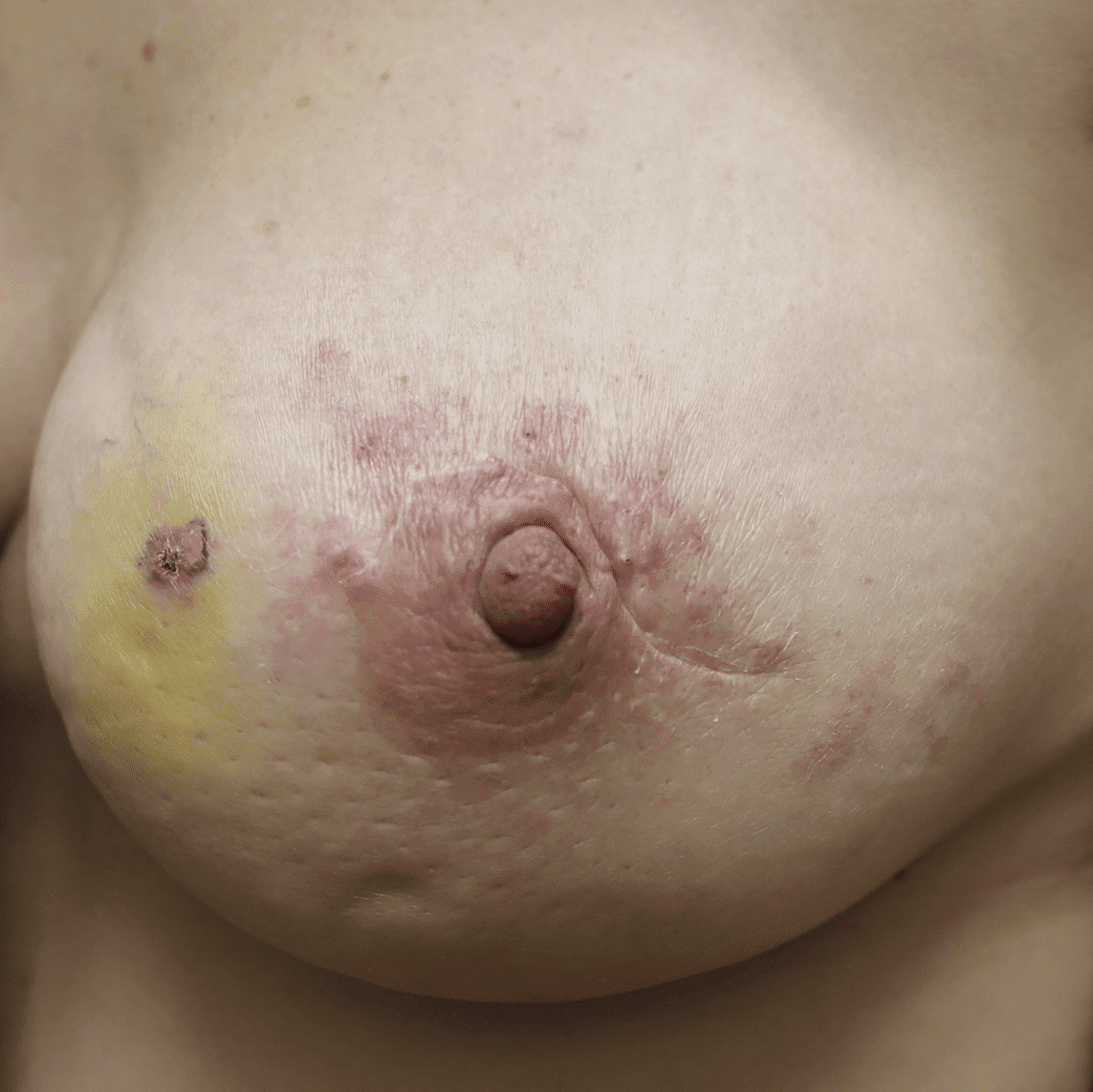
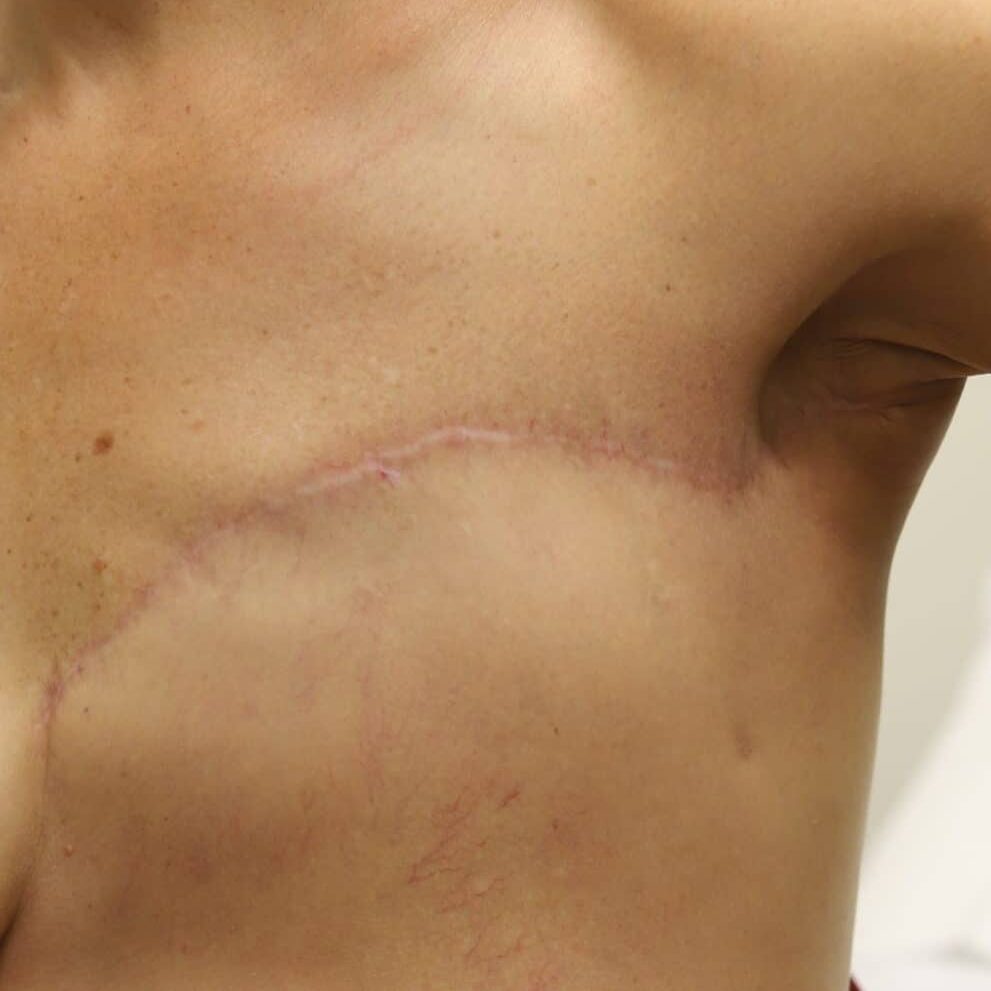
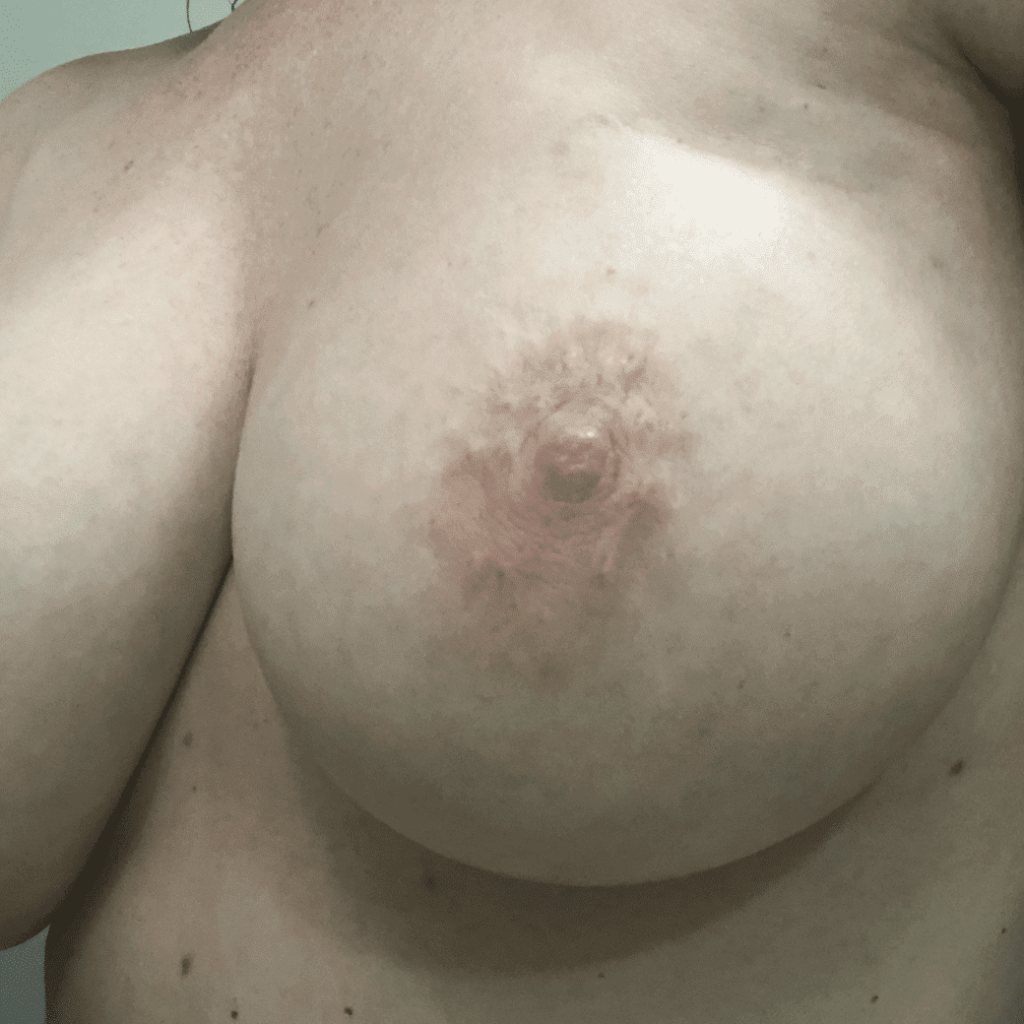
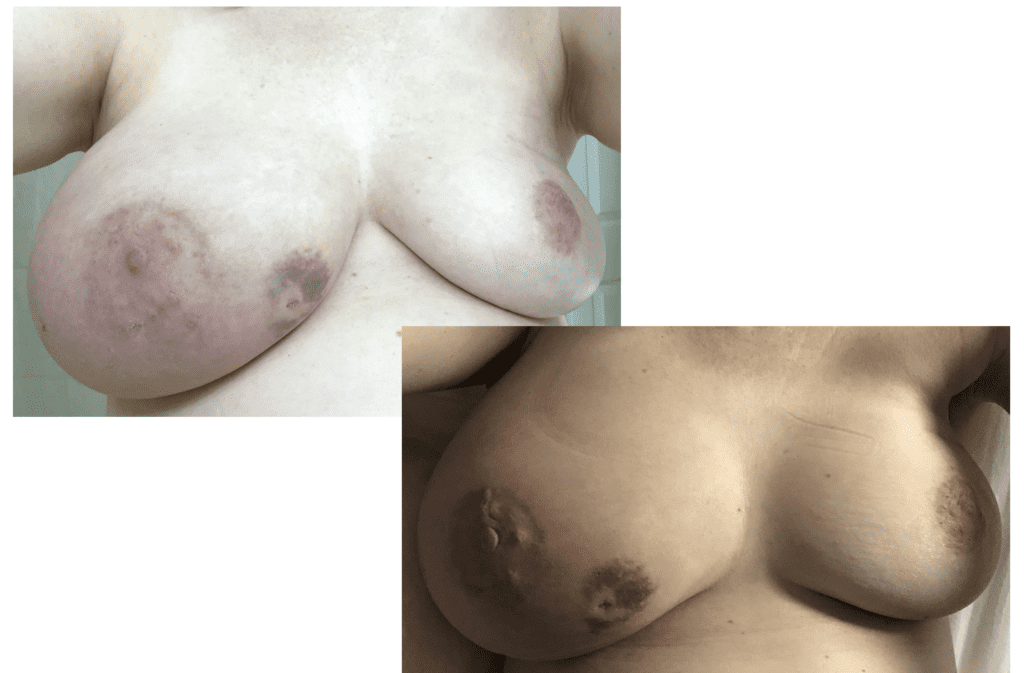
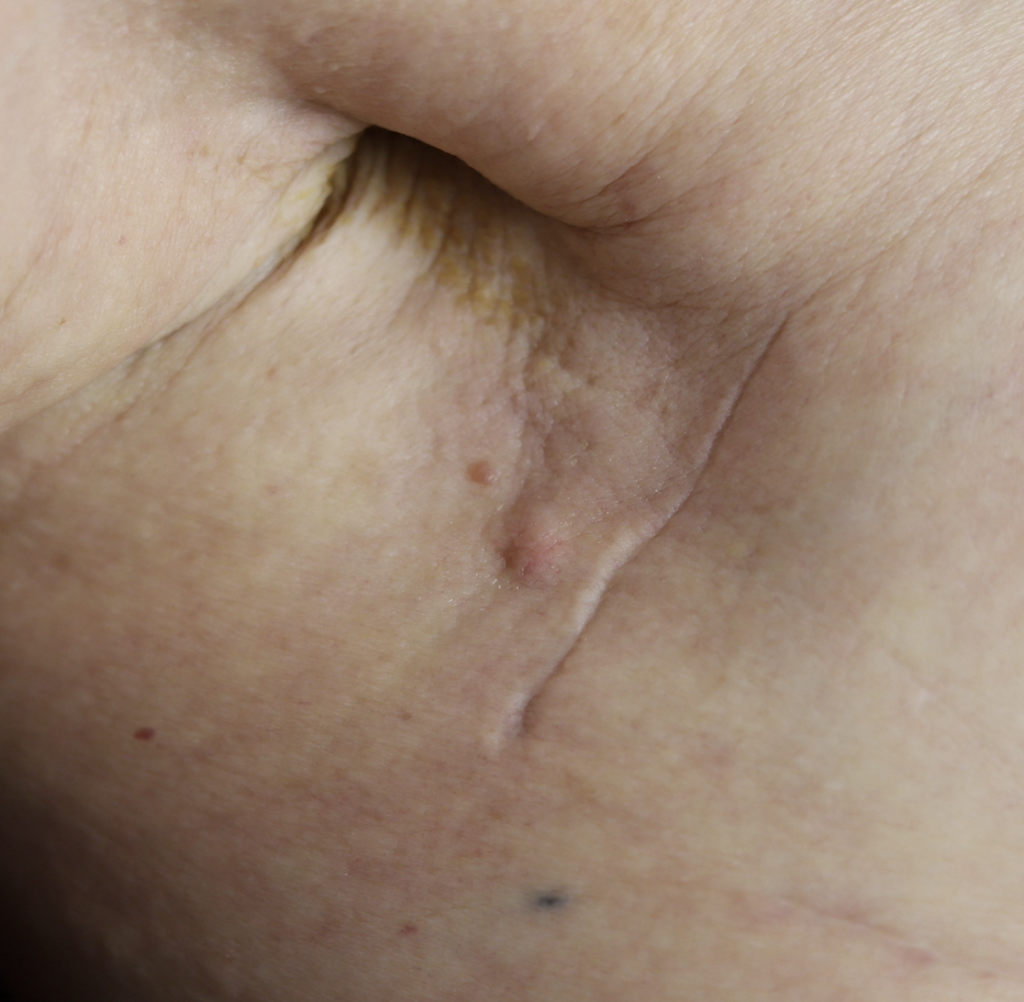
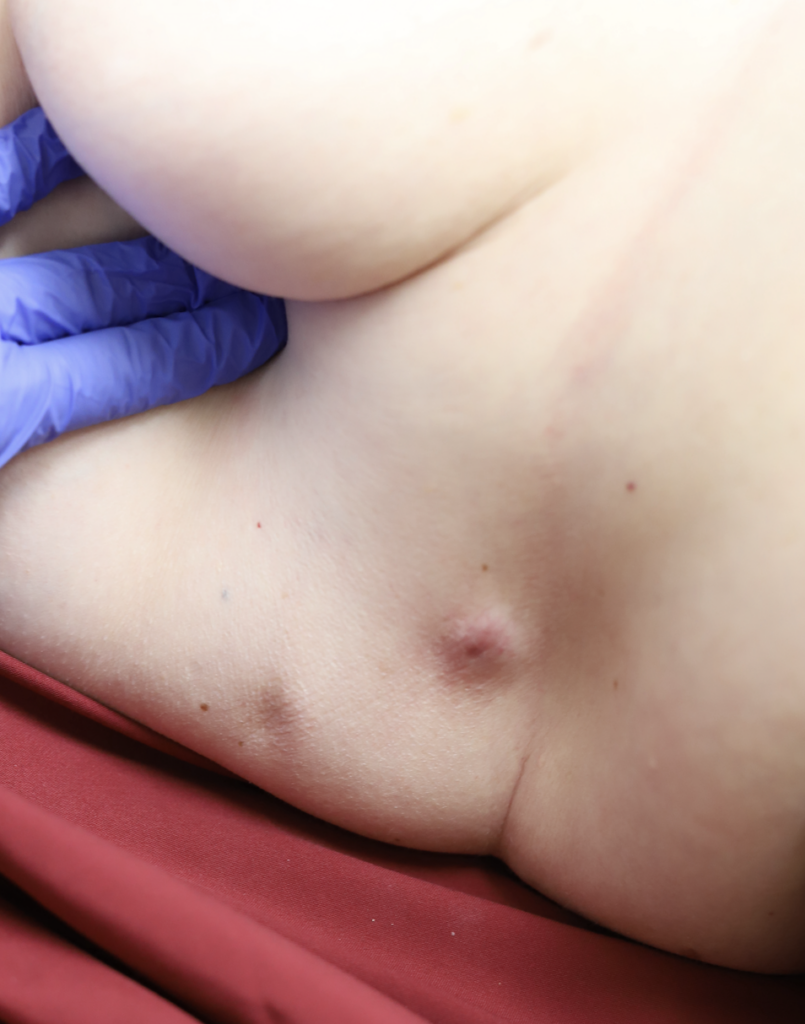
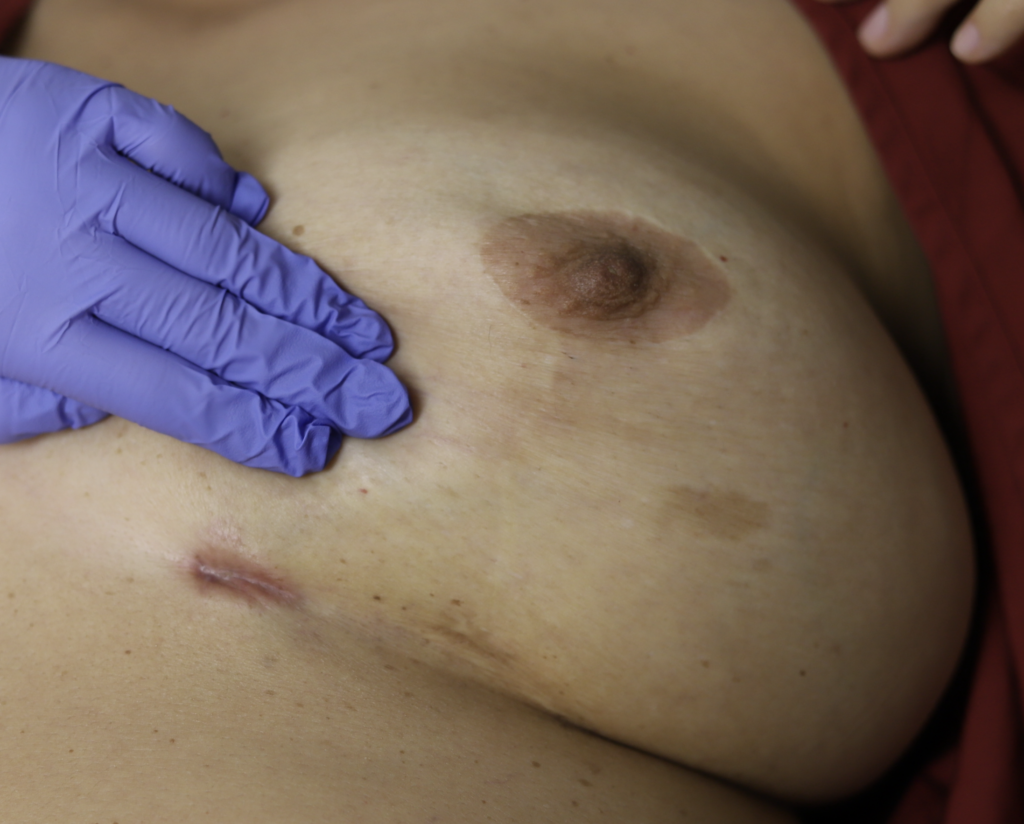
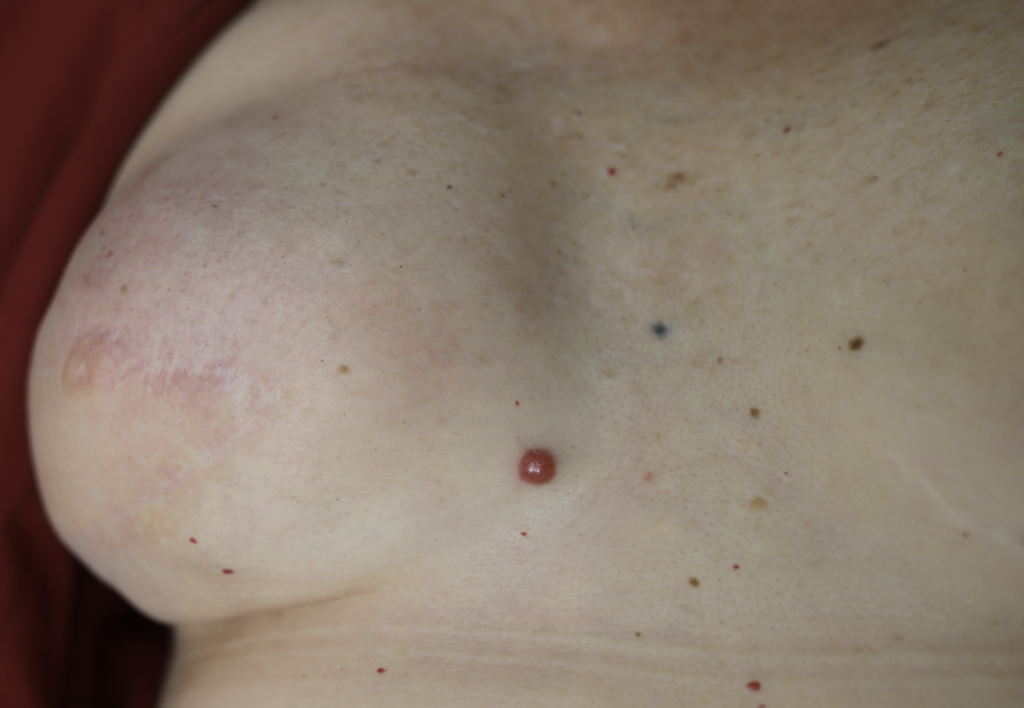
Any new “rash” or nodule or red spot on the skin or nipple after a mastectomy should be biopsied to rule out recurrent breast cancer. These are some examples below, the first one being a cancer presenting in the scar of a breast reduction patient and the second a chest wall nodule after a mastectomy in the right breast (middle blue spot is tattoo from previous radiation therapy).

Psychosocial Support During and After Breast Cancer
Women diagnosed with breast cancer at a young age — whether before, during, or after childbearing, or even in the setting of having no children — face unique challenges as cancer survivors. In addition to providing evidence-based information regarding lactation, these patients benefit from psychosocial care through patient support groups, social work, and reproductive psychology/psychiatry support.


Breast cancer survivor Miriam Dance embraces a life of “thriving, not just surviving.” She posted this stunning video the week prior to her surgery with me. It was recognized by producers, and she ultimately became the face of BCRF’s 2021 campaign. She also sang with members of the original Broadway cast of ‘Rent’ during the BCRF’s 2021 Virtual Hot Pink Evening!

