I see countless referrals for patients who have been on anti-fungal therapy for nipple and breast pain and itchy rashes on the areola. While the lactation world for decades has implicated yeast as a causative agent in this symptomatology, there is no scientific evidence to support this claim. A Spanish research lab does excellent research in this area and breastfeeding medicine physician Pamela Douglas of Australia published an excellent review on the overdiagnosis and overtreatment of nipple and breast candidiasis.
Innumerable websites and lactation lore report yeast as “burning, itching, and stinging” with “dry and flaky skin” or a “fine white rash.” This is a spot-on description of dermatitis or eczema.
The most common diagnoses I see in the setting of patients referred for persistent “yeast infection” are actually dermatitis, vasospasm, and classic neuropathic pain (burning, shooting, excruciating).

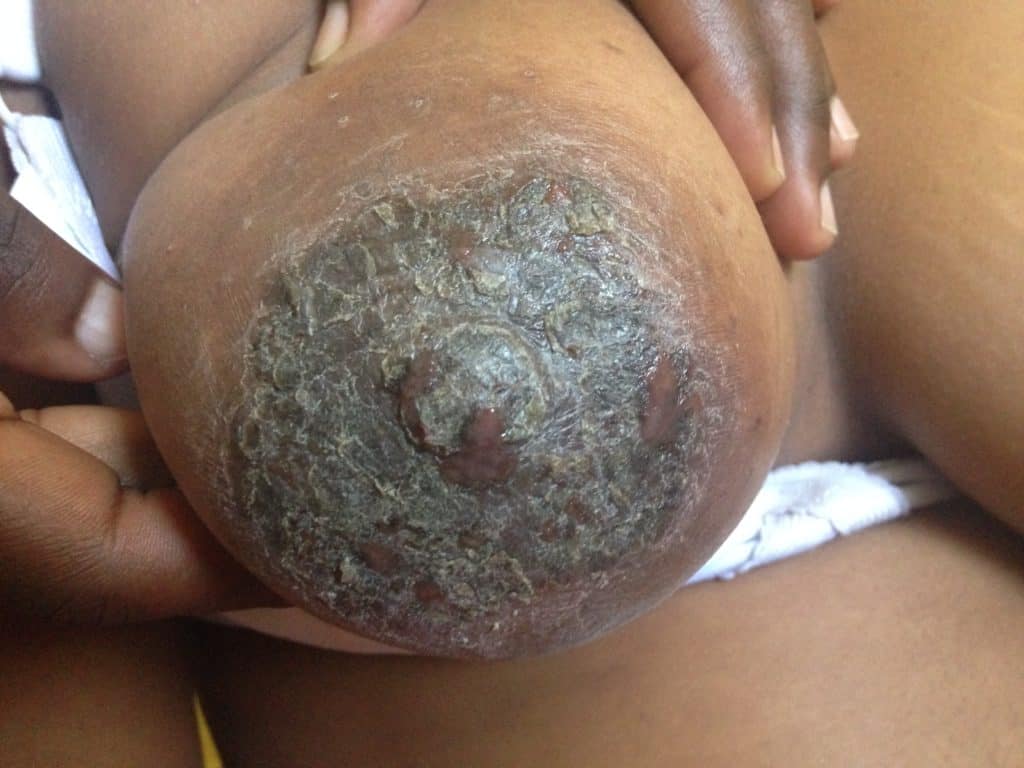
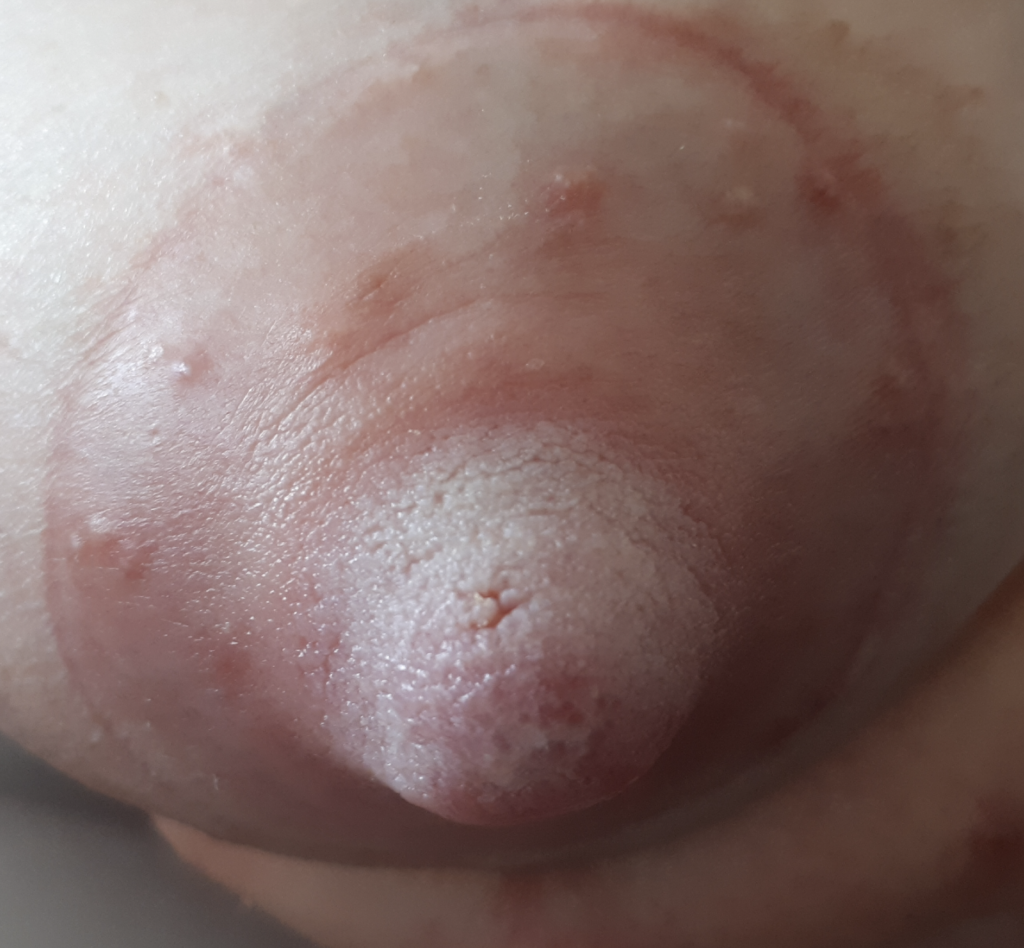
Nipple blebs (small white, yellow, or red blister-like lesions or “scabs” that occlude the surface of a nipple) are painful, but not yeast.
Nipples can be pink or red from pump or nursing trauma, blood flow changes, or simply an individual’s skin pigmentation (even in darker skin tones, the nipple tends to lose pigment during lactation) — this is also not yeast.
Anti-fungal medication by mouth is absolutely not indicated and anti-fungal crèmes and ointments applied to the nipple or the mouth of the baby can be very irritating to the nipple and areola, worsening vasospasm and causing surface wounds from contact dermatitis. Gentian violet can cause nipple ulceration and mouth ulceration in a baby (as well as in vaginas), and should not be used.


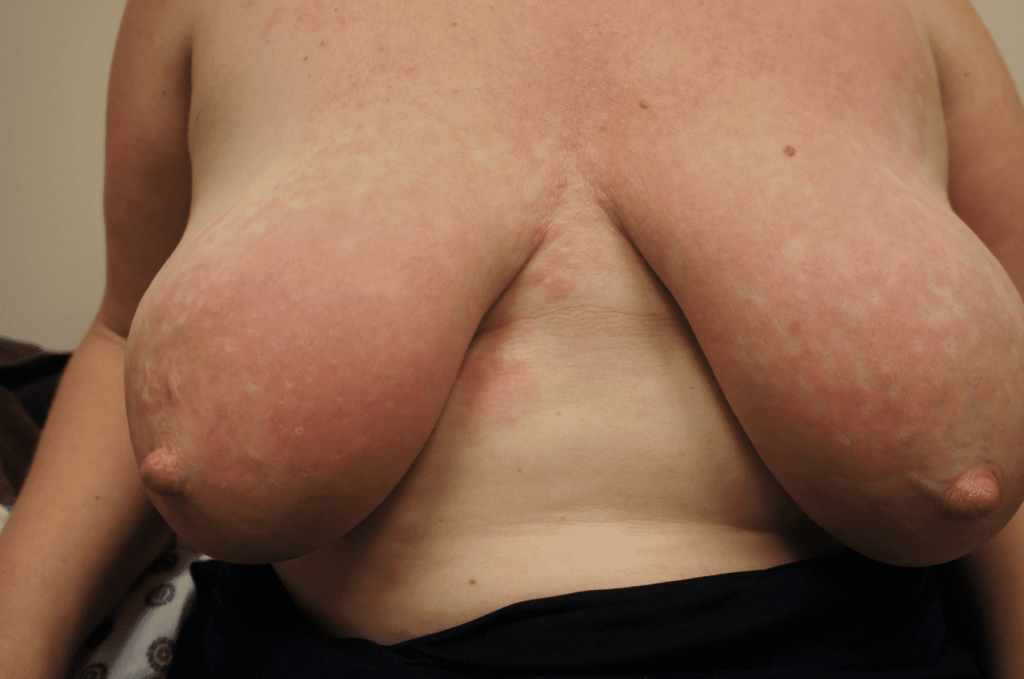
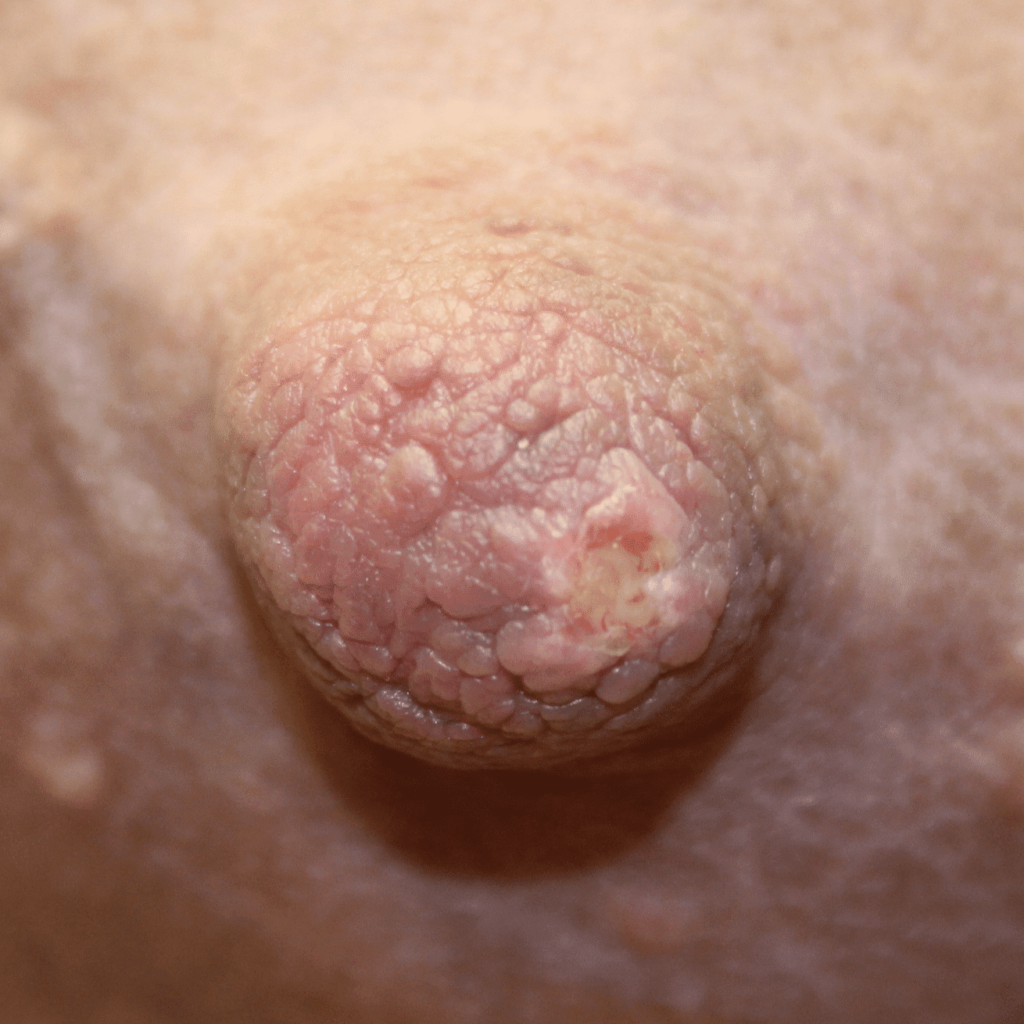
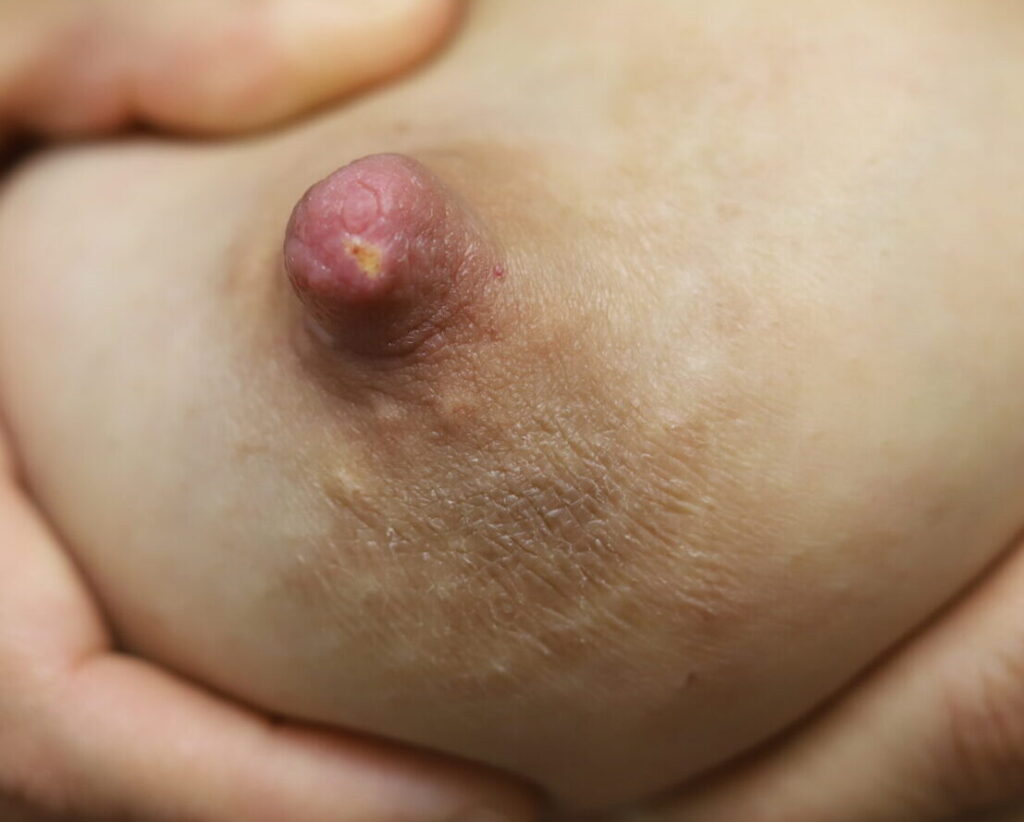
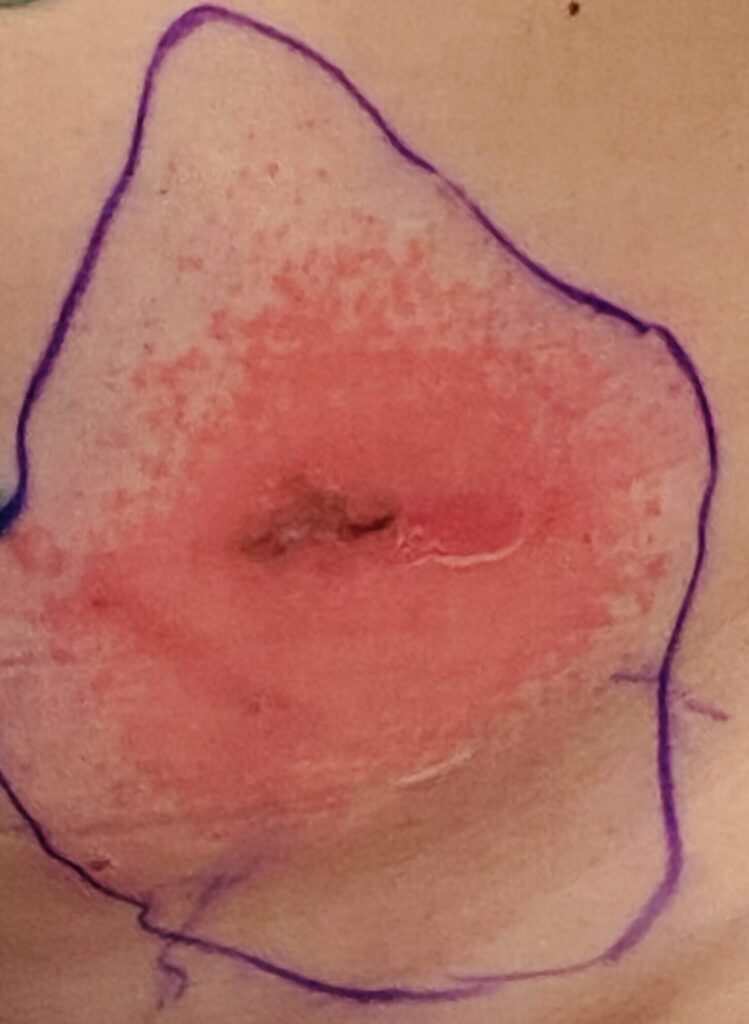
Thrush is not contagious. Vaginal yeast infections also are not contagious: sexual contact with a partner does not transmit them in the way sexually transmitted infections occur, and yeast from your vagina does not cause a yeast infection on or in your breast. Diaper rash isn’t transmissible to your breast. Yeast is a result of host-microbiome disruption that occurs most commonly in areas like the vagina, inframammary fold of the breast (where the bra strap sits underneath the breast), and under the arm. Yeast also may occur in heavier individuals in areas of subcutaneous fat. It occurs in immunosuppressed patients (e.g. chemotherapy, HIV), diabetes, and obesity.
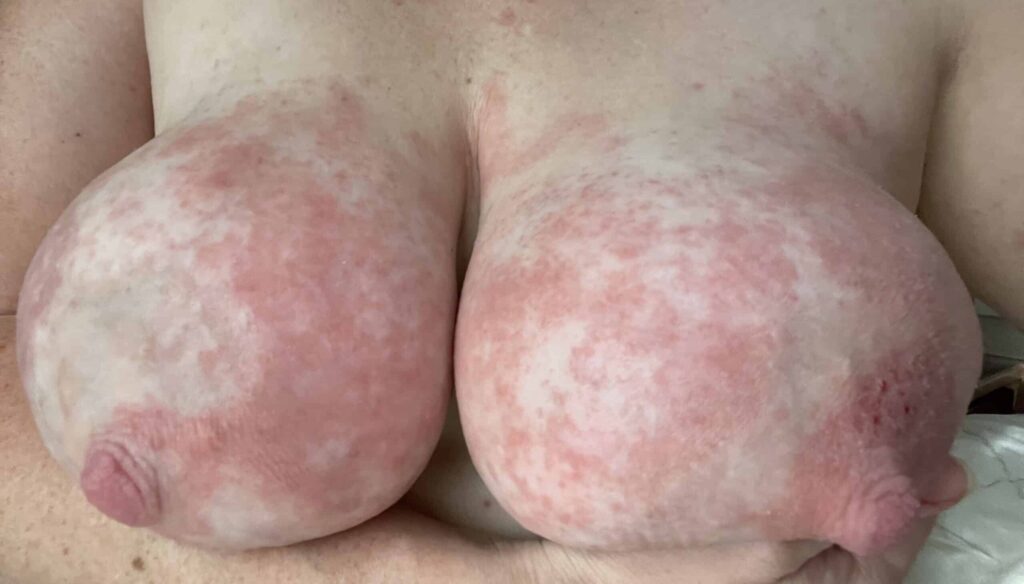

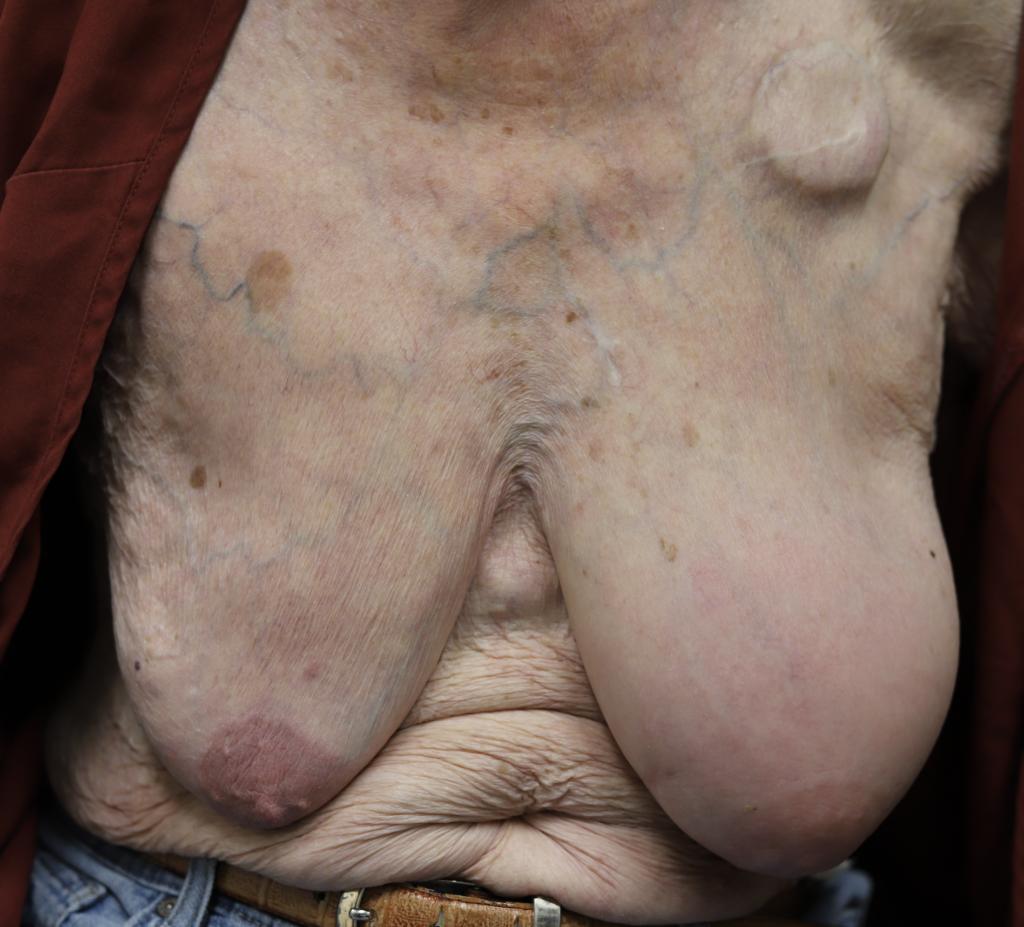
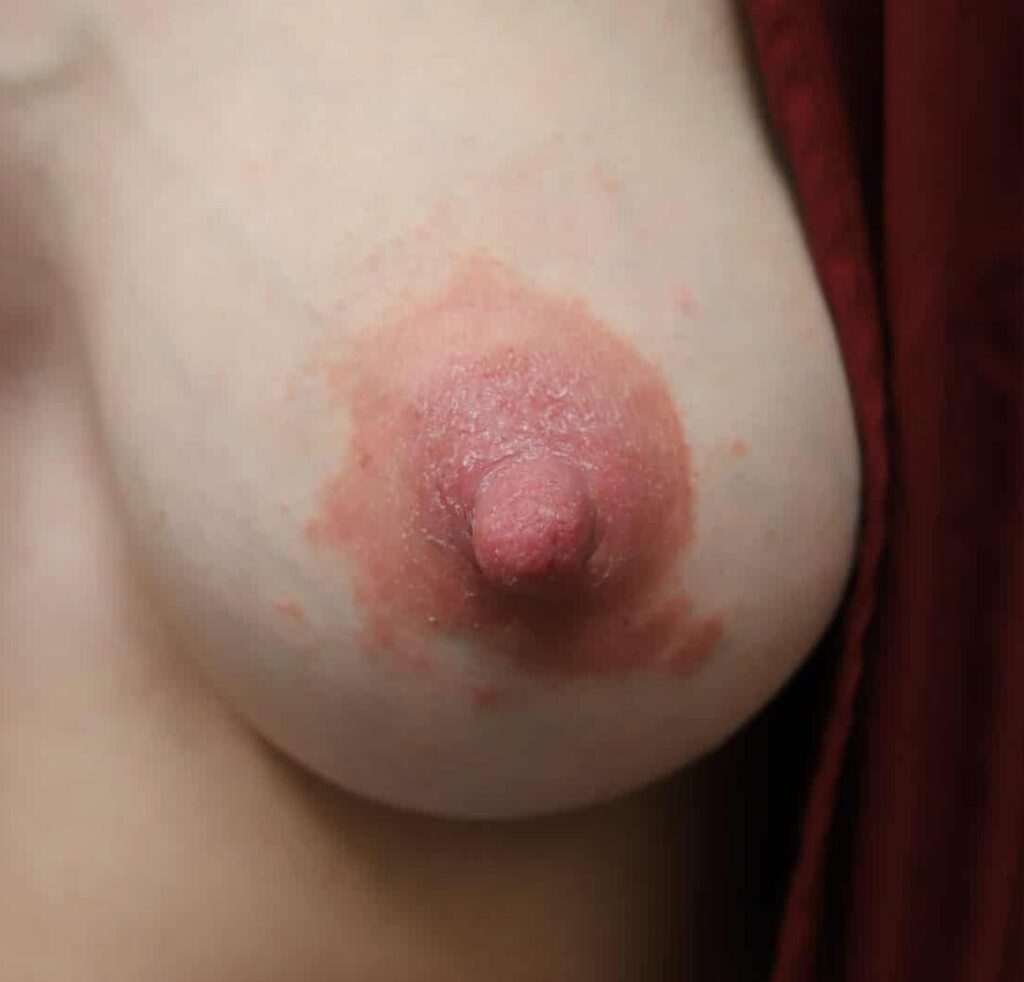
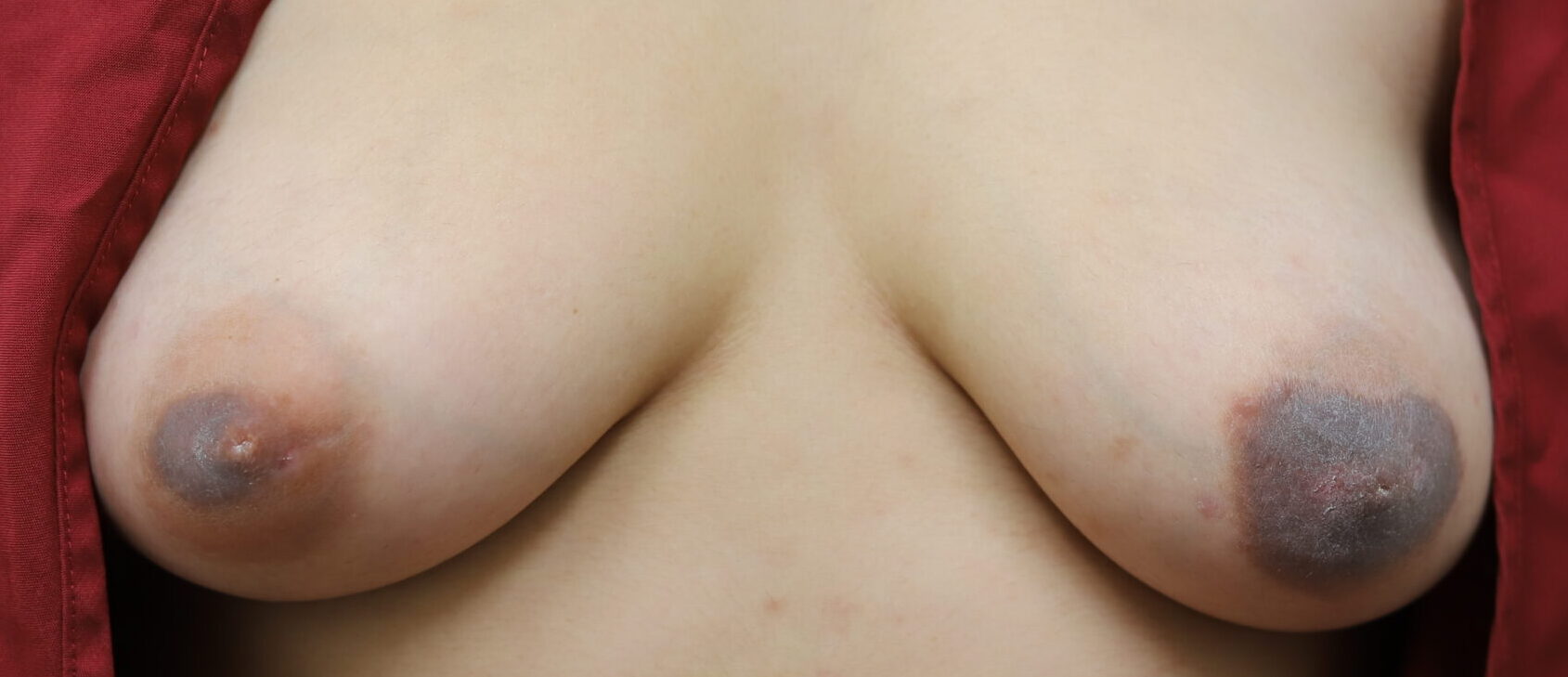
Below: two different patients, right and left nipples (the first patient is slightly worse) with classic lanolin allergy.




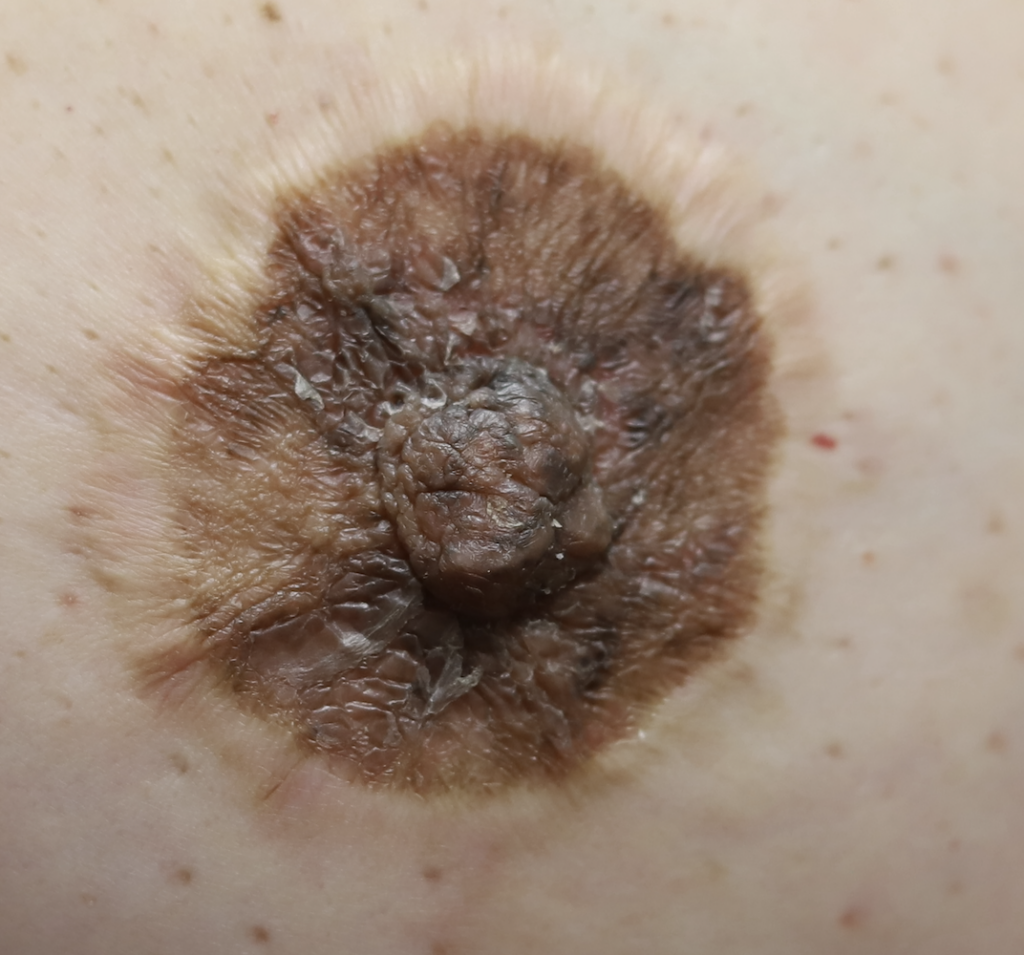
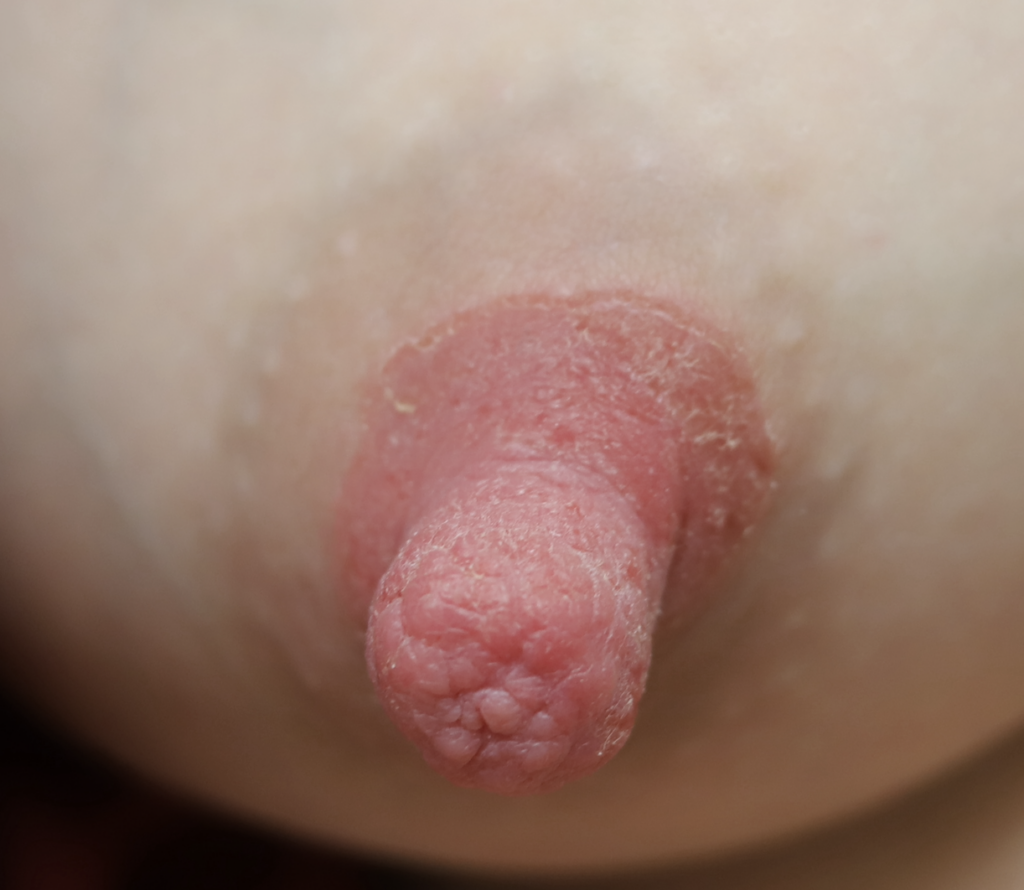
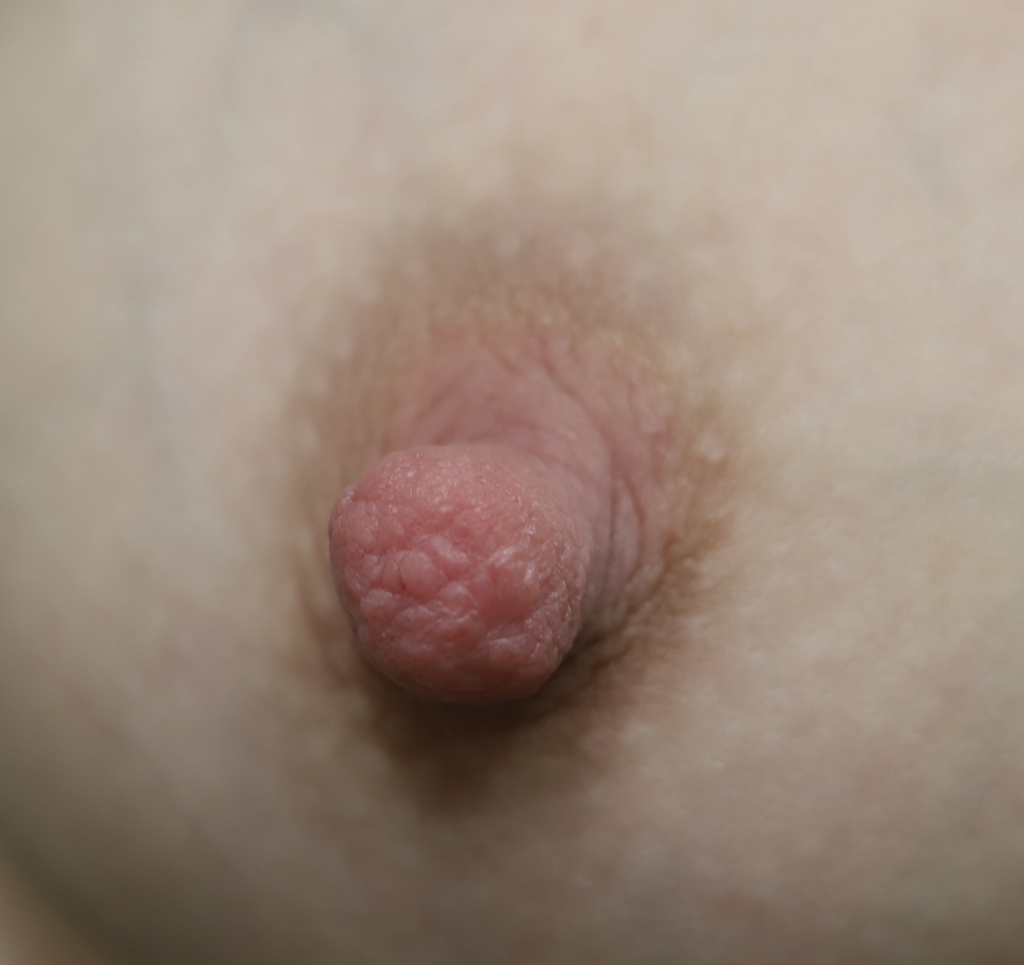


Infant thrush in full-term, immunocompetent babies is not nearly as common as the lactation world describes. So often, babies simply have a white coating on their tongue and/or cheeks from normal breastmilk. Mom may be suffering pain for a variety of different reasons, but due to many healthcare providers’ lack of familiarity with breast examination, they assume that the infant is the cause of the pain.

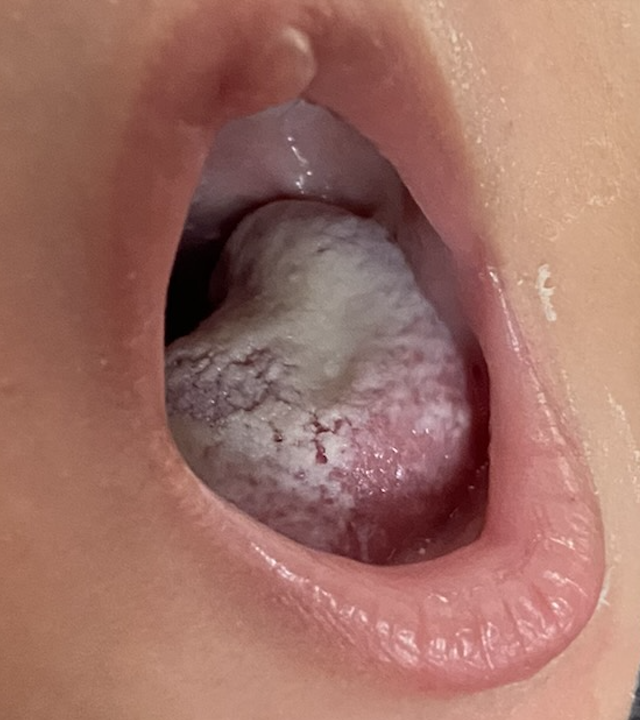
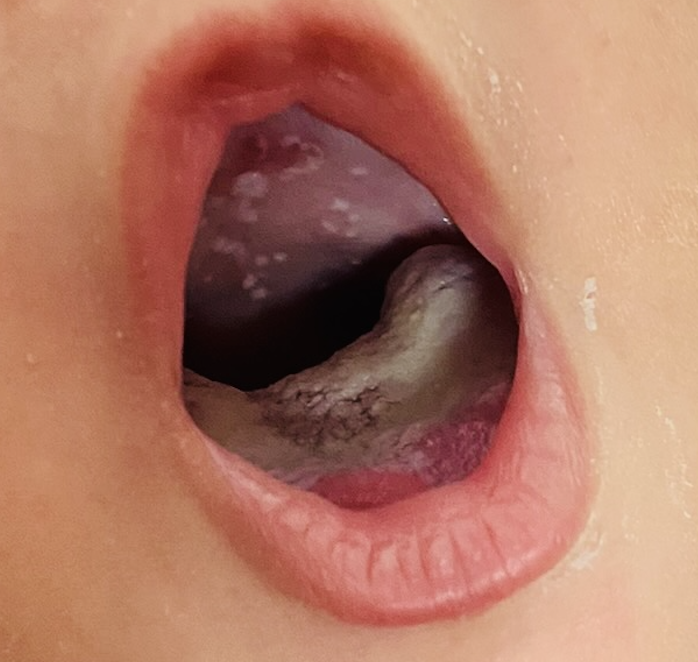
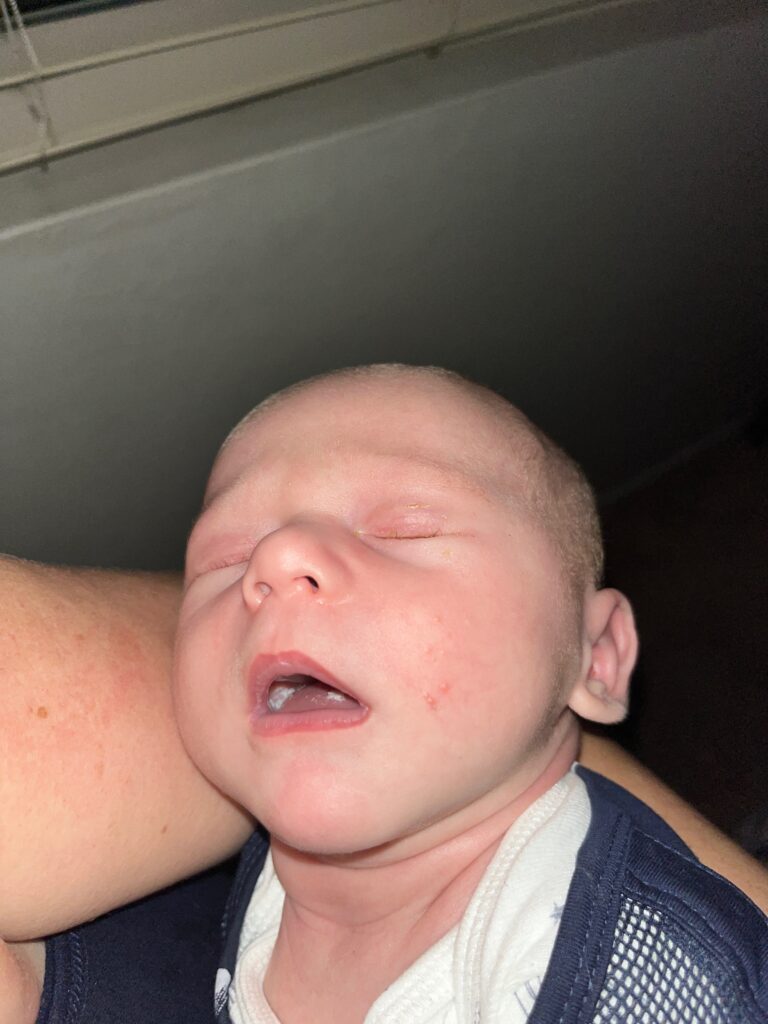
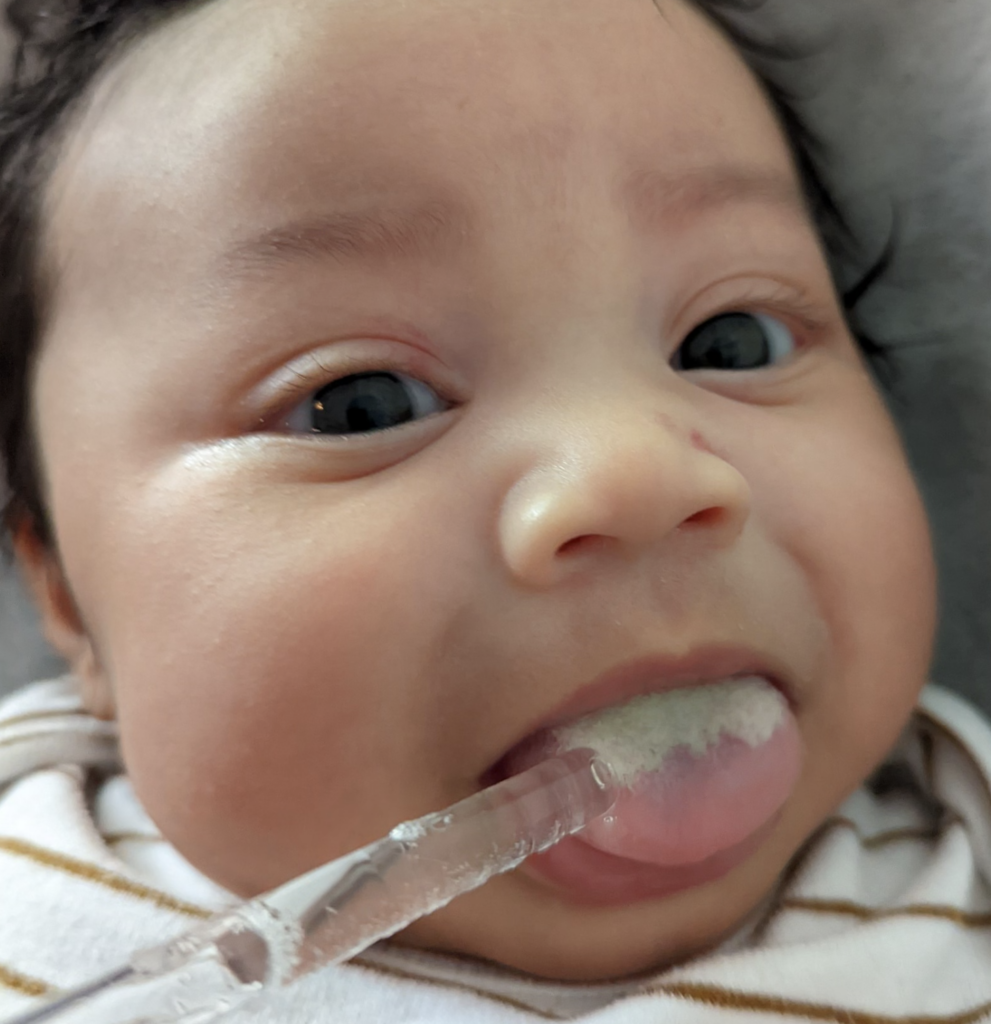
When infants undergo thrush treatment, mothers do not need to undergo antifungal treatment themselves. Pump parts, infant toys, and other household items do not need to be sterilized; in fact, harsh detergents may worsen allergy, which is often at the root of mom’s symptomatology. Many people ask why they temporarily improve after anti-fungal treatment. This is related to the anti-inflammatory effect some people obtain from anti-fungals. However, the improvement is almost always not definitive and moms will return for repeat treatment or seek alternative interventions.
All Purpose Nipple Ointment (APNO) is a compounded ointment that contains multiple unnecessary ingredients that are not indicated for use on a nipple, and can cause allergy and other complications. It also is expensive. Do not use this. Patients may be instructed to make their own with over-the-counter APNO with bacitracin, nystatin, and hydrocortisone. However, hydrocortisone is too weak a steroid to provide any benefit for blebs or dermatitis, and topical anti-fungals and anti-bacterials cause significant skin and nipple irritation. Fungal infection of the nipple is a myth not supported by any anatomic or physiologic principle.
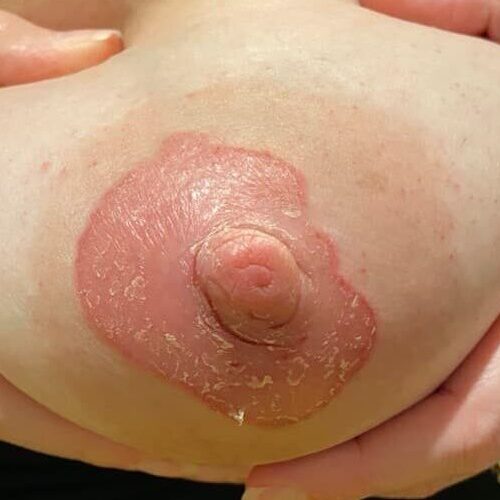
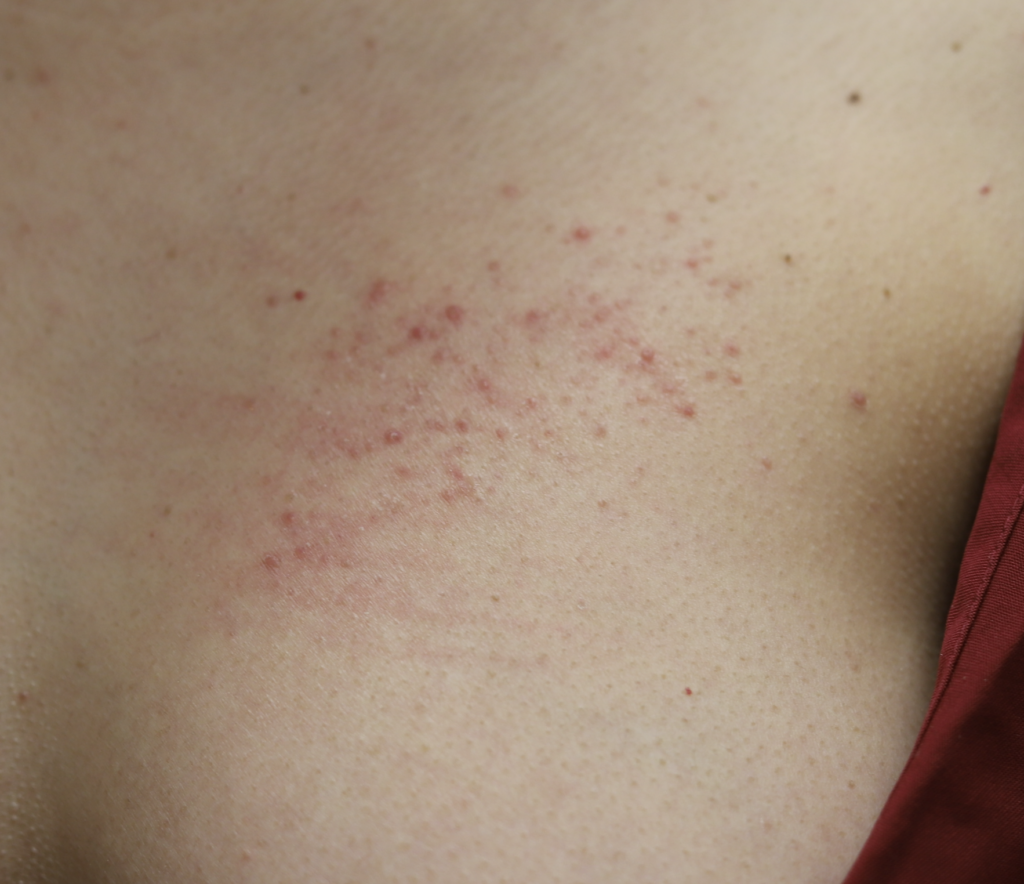
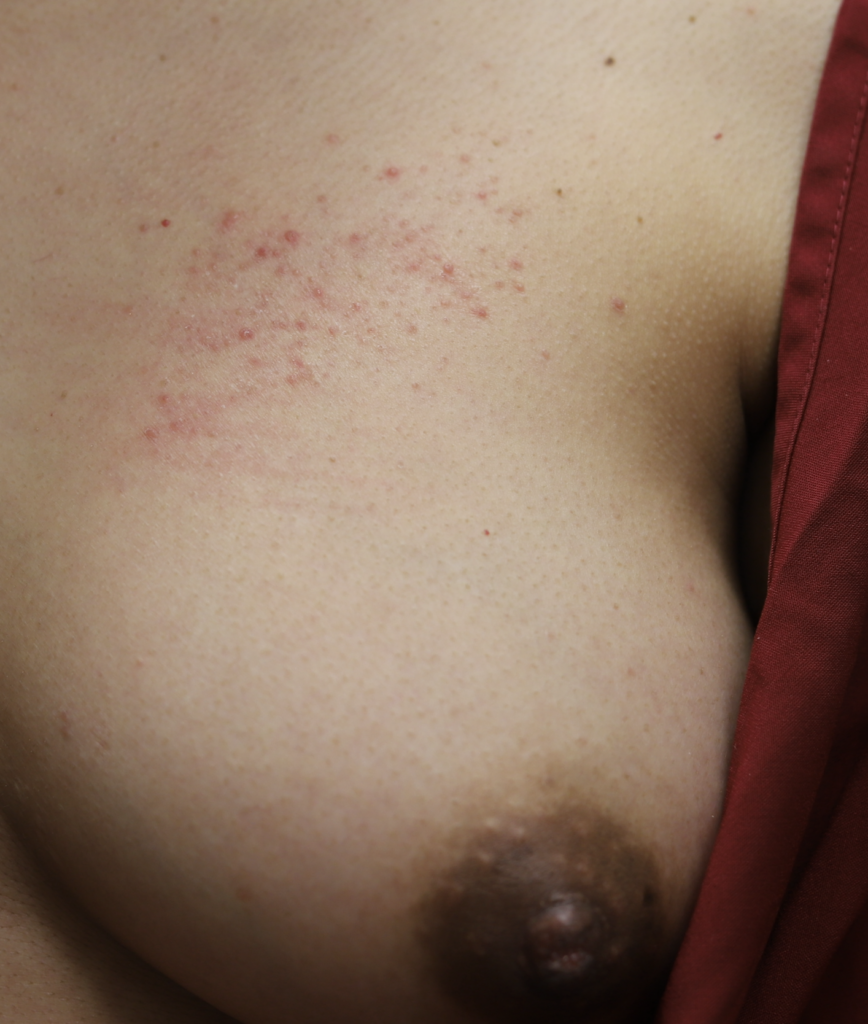
The following two photos show severe dermatitis worsened by application of topical antibacterial agent, and the third photo shows a week after treatment with steroid. Hyperpigmentation is common for several months to up to one year after resolution of a significant inflammatory process such as this, and is expected to fade after that time
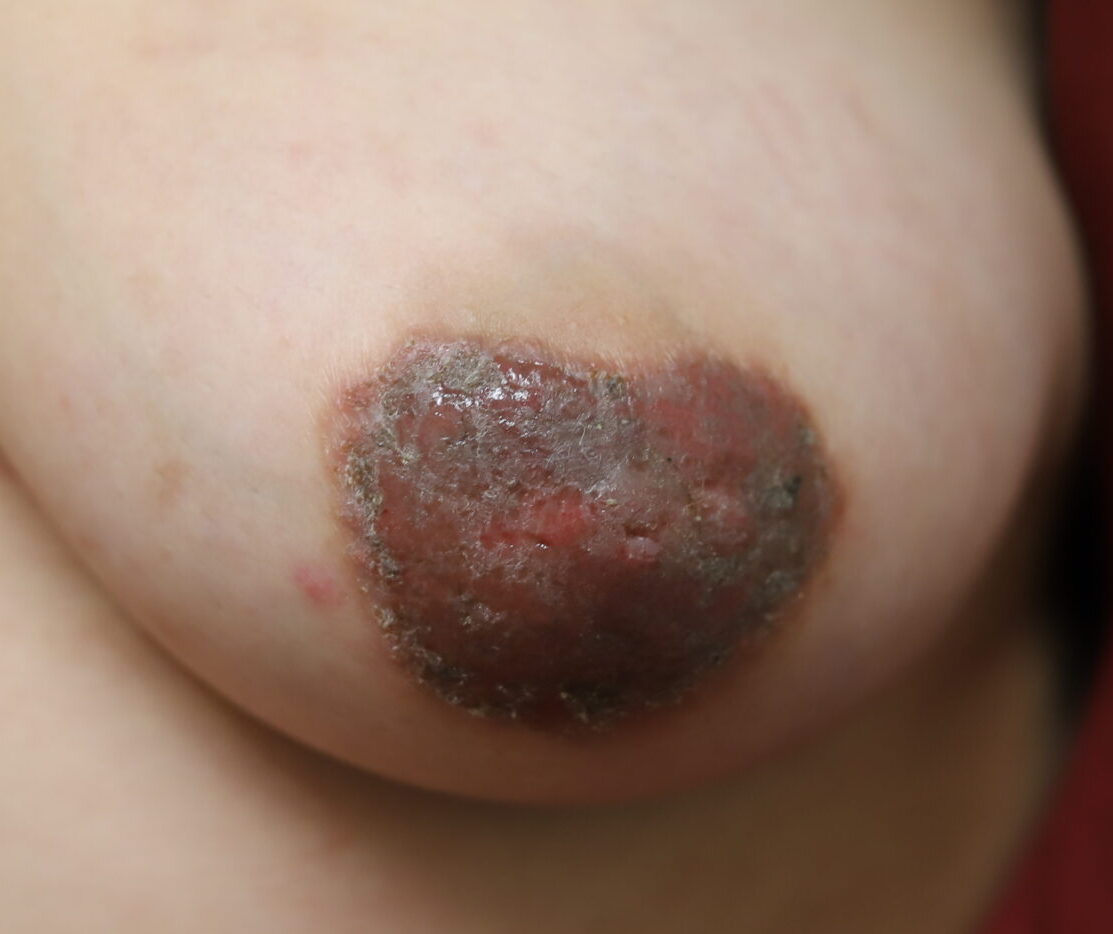
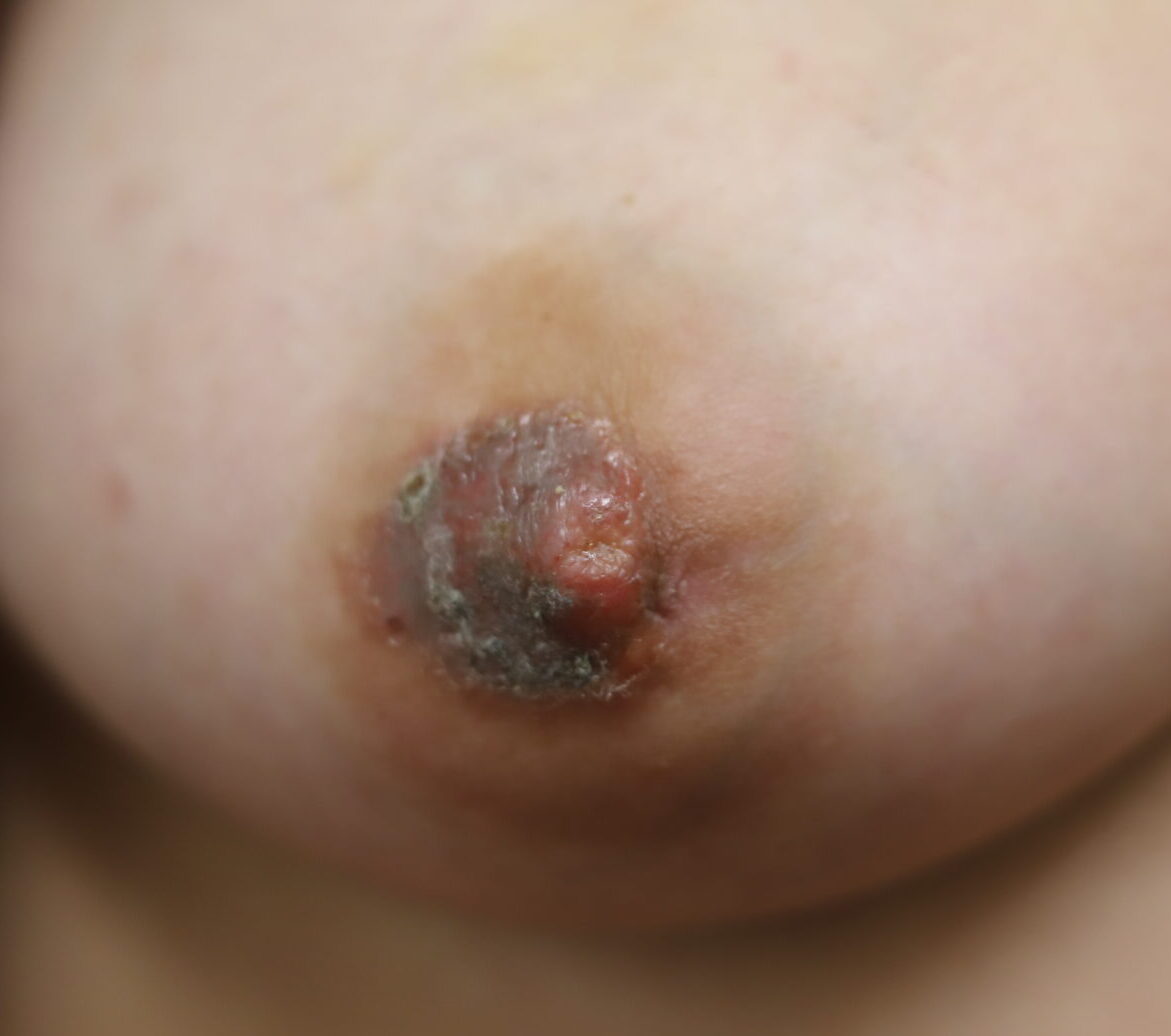
 Relief after steroid!
Relief after steroid!
The nipple has incredibly robust blood supply and therefore any surface bacterial infection is extremely uncommon. When patients describe pain relief from APNO, it is related to the fact it contains a prescription strength steroid crème (most often triamcinolone). Therefore, in patients with significant nipple trauma and/or pain and/or blebs, we utilize triamcinolone alone. 4th Trimester Physician Michelle Haggerty has a great blog post on the dangers of APNO as well.
Finally, moms will so often develop pain after a baby has had a recent ear infection and taken antibiotics. The infant’s potential “thrush” from antibiotics is not the cause of mom’s pain. It’s the fact that the infant could have been nursing much more frequently to soothe pain, or could be jerking/pulling at the breast. In addition, a mom can be allergic to the antibiotic the infant was prescribed. Therefore, her symptoms of itching and redness are allergy and dermatitis rather than “yeast.”

