Sleeping Through The Night
After surviving the initial weeks of sleep-deprived new parenthood learning how to take care of a baby, the next stage of approximately 3-6 weeks postpartum involves getting past colic and working through any new or continuing breastfeeding challenges.

If you’re lucky, you may have a baby who starts to stretch out its sleep overnight into 5, 6, or 7 hours by six weeks. This is not common, but possible if you have a lot of milk, baby is gaining well, and your baby is generally laid back. Often, this scenario results from mom having hyperlactation (oversupply) and the lack of stimulation overnight can help downregulate her production naturally, to a physiologic level that is more comfortable for baby.
Mothers may be told to wake up to pump to maintain their milk production, or to dream feed the baby. I do not recommend this, as it drives mom’s production higher. Needing to pump or dreamfeed at night to maintain production is different if you have sleep trained a baby very early (i.e. baby not instinctively sleeping longer stretches on its own).
Mothers may be concerned about developing mastitis or plugging if they sleep longer stretches overnight. Again, breasts must remain full to activate Feedback Inhibitor of Lactation (FIL), reduce overproduction, and decrease ductal inflammation. Unless you let your breasts rest and be in physiologic sync with baby, you will perpetuate a cycle of oversupply and complications such as mastitis.
Babies who sleep more overnight may feed very frequently during the day, as they need to make up for the calories they are not taking in at night. This is not abnormal.
Sleep Training
While breastfeeding medicine pediatricians do not recommend “sleep training” prior to six months, some moms are very sensitive to sleep deprivation and may require solid night sleep to maintain their mental health. Like trauma surgery involving a pregnant woman, the adage “save mom first” applies here. Nothing matters more than having a healthy, living mom to take care of a baby.
When counseling patients about the balance between breastfeeding and mental health, we discuss ways to maintain milk production while allowing a partner, other family member, or nanny to care for the baby overnight. This involves pumping before bed, feeding the baby on demand throughout the day, and pumping in the morning after the baby feeds at the breast. More pumping than this can often be detrimental to mental health.

Moms may also need to utilize galactagogues to maintain their milk production, as lack of feeding or pumping overnight will decrease prolactin secretion. Moms who have eliminated overnight stimulation very early also are at risk of early return of their menstrual cycle, which can decrease milk production significantly. However, moms with very ample baseline milk production often can maintain exclusive breastfeeding while also protecting sleep, so it is an individual discussion with all. The Academy of Breastfeeding Medicine Galactagogue Protocol offers more information on the topic of using herbs and prescription medication to maintain or increase milk production.
Colic and Evening Cluster Feeding
From 4-6 weeks, babies will develop “colic,” which is a period of neurological awakening. After this time period, babies move from the early neonatal period to infants who smile and engage in their environment. However, the 4-6 week period can be difficult in the afternoon and evenings, when babies seem inconsolable. They may want to “cluster feed” as they search for comfort, but are sometimes unable to find relief — even at the breast. This is a time, if breastfeeding is well established, to introduce a pacifier and take a baby outside for fresh air to calm them. Getting a break in the evenings from fussiness also can help moms maintain their mental health during this time period. If you’re able to get help, do it!

Oral Contraceptives/IUD
Unfortunately, misinformation abounds regarding lactation and contraception, and research on this topic is poorly controlled for confounders (factors that affect study results). The Academy of Breastfeeding Medicine Contraception Protocol reviews the existing data and provides recommendations regarding counseling based individual patient circumstances. IABLE also has an excellent podcast on the topic of contraception.
Moms with abundant production of breastmilk may not appreciate noticeable difference in breastmilk production after starting a progesterone-containing oral contraceptives (mini pill), hormonal IUDs, injectable or long-acting implantable birth control after their six-week postpartum visit. Estrogen containing oral contraceptives will, without question, decrease any mother’s production (we in fact use them to treat hyperlactation).

However, moms with a more marginal supply or lower supply can notice a decrease in production. This is worsened by the fact that many moms may return to work at six weeks and be pumping more rather than breastfeeding. They may be stimulating less frequently and less effectively than nursing on demand at home. Their babies may be sleeping more at night, so they are missing nighttime stimulation.
If you are in this situation and notice a drop, you should seek medical advice regarding galactagogues, effective pumping techniques, and tips for feeding the baby overnight and/or frequently at any other time you are away from work.
Lactational Amenorrhea Method (LAM)

While no single birth control aside from surgical sterilization or abstinence offers 100% protection against unintended pregnancy, the LAM method is 98% effective. However, it is not talked about frequently because strict criteria must be met for this to protect against pregnancy:
- A mom must be feeding the baby on demand, around the clock (including overnight)
- Baby receives only breastmilk
- Mom is less than six months postpartum and menstruation has not returned
Oversupply and Baby Poop






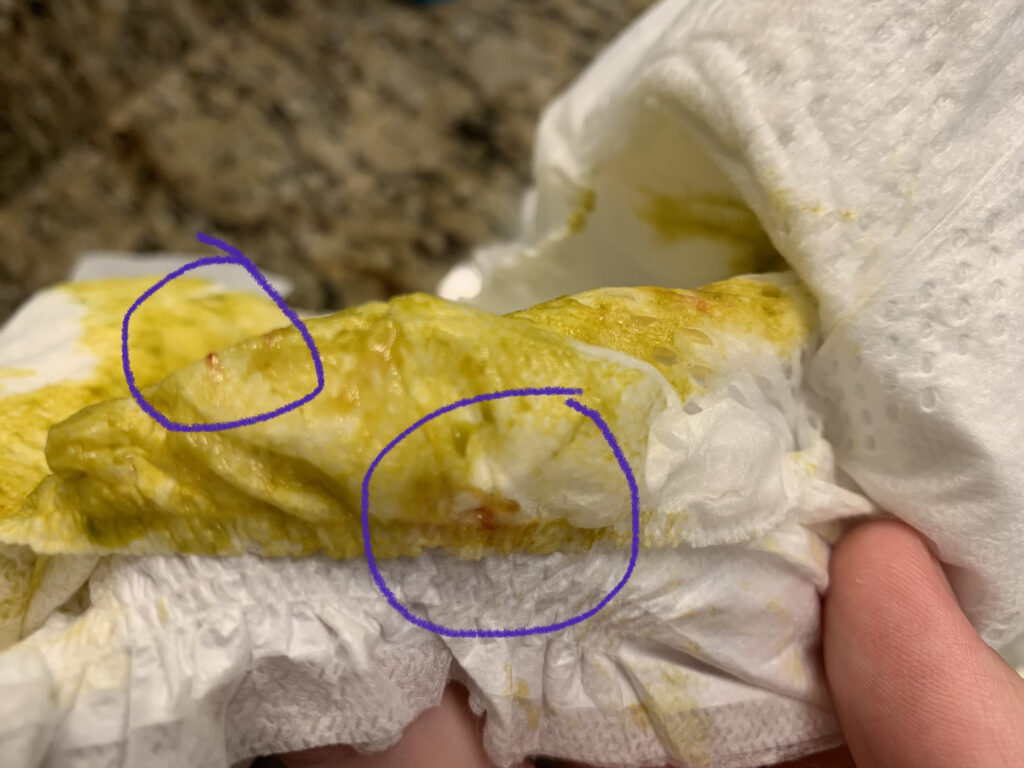
Breastfeeding stools are liquid, seedy, yellow, and may even be green or mucousy. They will never be solid. If you simply notice some transient variation in stool color or presence of mucous, this is not a problem. I talk to patients about the “big picture patterns” more than day-to-day changes, which are normal during breastfeeding (and parenting in general). As babies continue to get older, they may only stool once daily or even go several days to week without stooling. This is normal because the breastmilk is absorbed so well by the body. Laxatives are used commonly with formula feeding, as cow and soy milk protein are not well digested and cause constipation. However, laxatives are not indicated in breastfed babies and can cause harm with excessive diarrhea and diaper rash.
If a baby is gaining very well and has very frequent “blow out” stools as well as reflux and gas, the mom very likely has hyperlactation (oversupply). If your pediatrician recommends you start formula to make the stool more solid, seek consultation with a breastfeeding medicine physician for treatment of hyperlactation. The solution is to treat hyperlactation, not make the stool artificially firm by introduction of cow or soy milk formula. Babies also may be referred to pediatric gastroenterology and moms told to eat a restrictive diet and/or start elemental formula. This is devastating in a situation where otherwise mom produced very adequately to exclusively breastfeed the infant. Infant symptoms such as diarrhea, reflux, and excessive gas will resolve with treatment of hyperlactation. Mom’s breasts are half of the organ system and the baby cannot be evaluated without the mom being evaluated.



Donor Milk
If you need to continue to supplement your own milk production, you can source formal donor milk or follow safety precautions if informal milk sharing.
Exclusive Pumping

If it looks like you’re going to be exclusively pumping for a NICU baby, or because your nipples are quite large and baby is small, or you have a lower production/flow of milk, be wary of coconut oil to lubricate the flanges. Some traction against the flanges is normal to prevent too much tissue from being sucked into the flange.
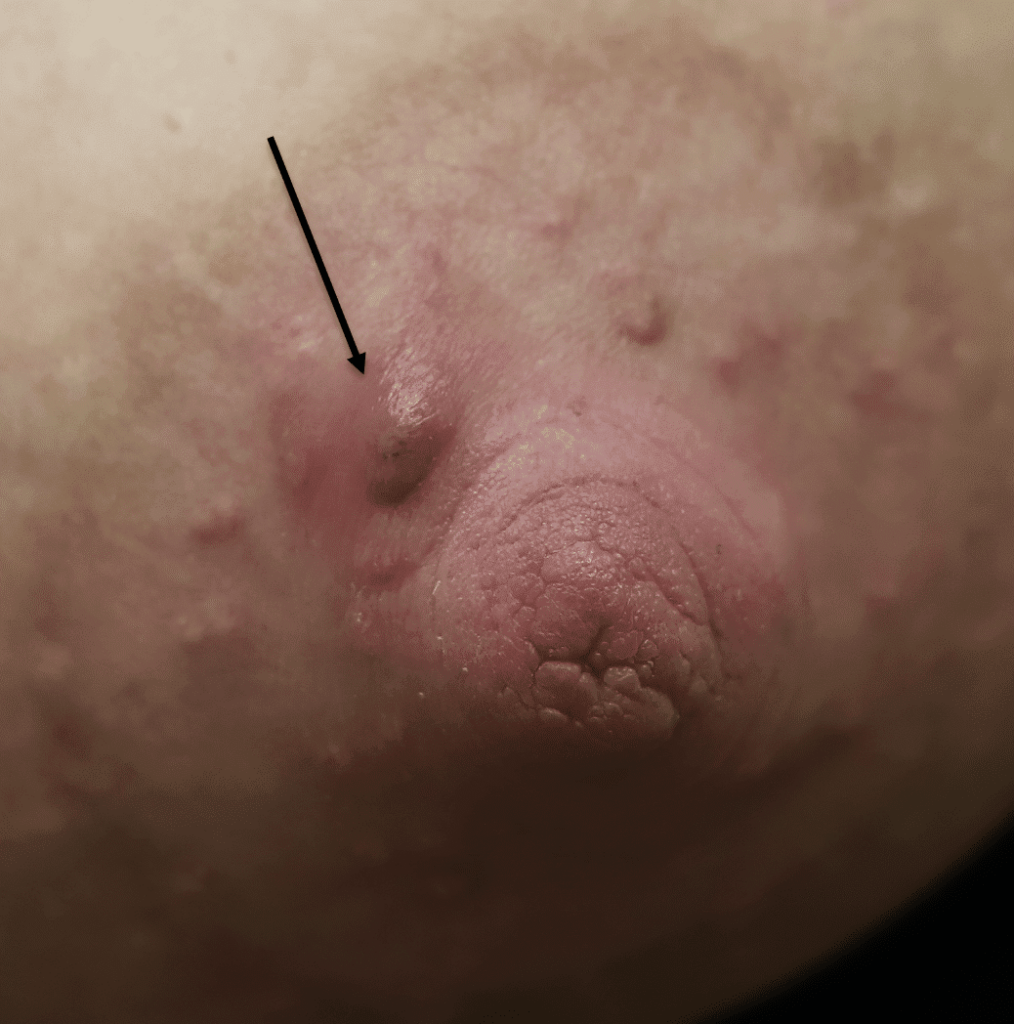
Coconut and other oils artificially lubricate and allow for more pull than is healthy. Coconut oil also can obstruct the Montgomery glands (oil glands on the areola) like a zit on your face. If you do experience this, seek medical evaluation. You also can treat a minor obstruction with salicylic acid or benzyl peroxide creme, and washing with gentle soap and water.
If you believe your baby may be able to latch directly to the breast, but you had a rocky start to breastfeeding, seek professional guidance for positioning and latch help. If you are pumping because of pain and/or DMER with breastfeeding, that also is very treatable by a professional. EP can seem like it’s easier, or a solution to breastfeeding woes, but it unfortunately is fraught with complications and you want to avoid if at all possible.
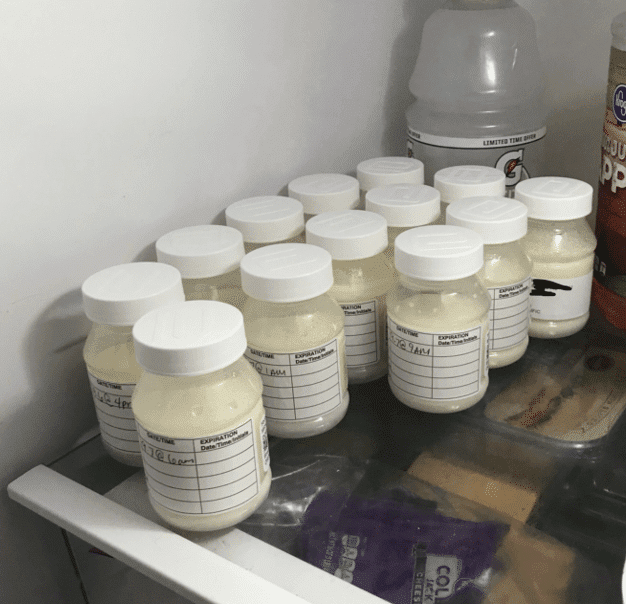
Pump only what baby needs. Do not store excessively as you want baby to have current antibodies and other breastmilk components present in unfrozen milk. Often, babies won’t take the frozen milk, either. I describe it to patients as analogous to old ice cream in the refrigerator: it tastes freezer burned, and you would rather get a fresh scoop from the ice cream shop instead.
Small flange sizes have become very popular in the lactation world. When nursing effectively, infants don’t just latch to the nipple — they also latch deeply into the areola. So if you don’t have pain and milk is flowing freely, it is ok if your areola is also pulled into the pump flange. I tell patients the right size is the size that is comfortable. Using an excessively small or excessively large flange that hurts can cause tissue trauma and other complications.

