We recently published with the American Society of Breast Surgeons (ASBrS) an Executive Summary of oncolactation, the intersecton of breast cancer care and lactation. Our first and senior author reflection elaborates on future directions.
Look for These Changes
If you notice any changes in your breast while pregnant or postpartum (regardless of whether you weaned from breastfeeding or not), contact your healthcare provider for evaluation:
- Breasts becoming different sizes (some asymmetry is common and normal, but the key is CHANGE).
- New lump or redness that doesn’t go away
- Nipple changes that don’t go away, such as inversion or being unable to move it freely like the other one
- Swelling in the armpit that doesn’t go away
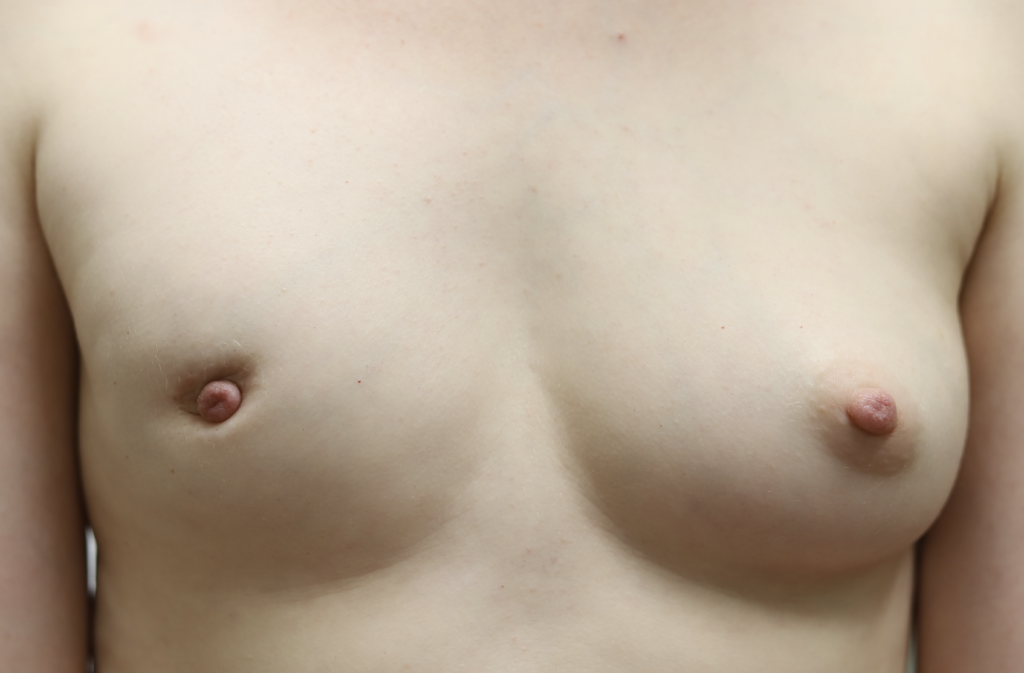
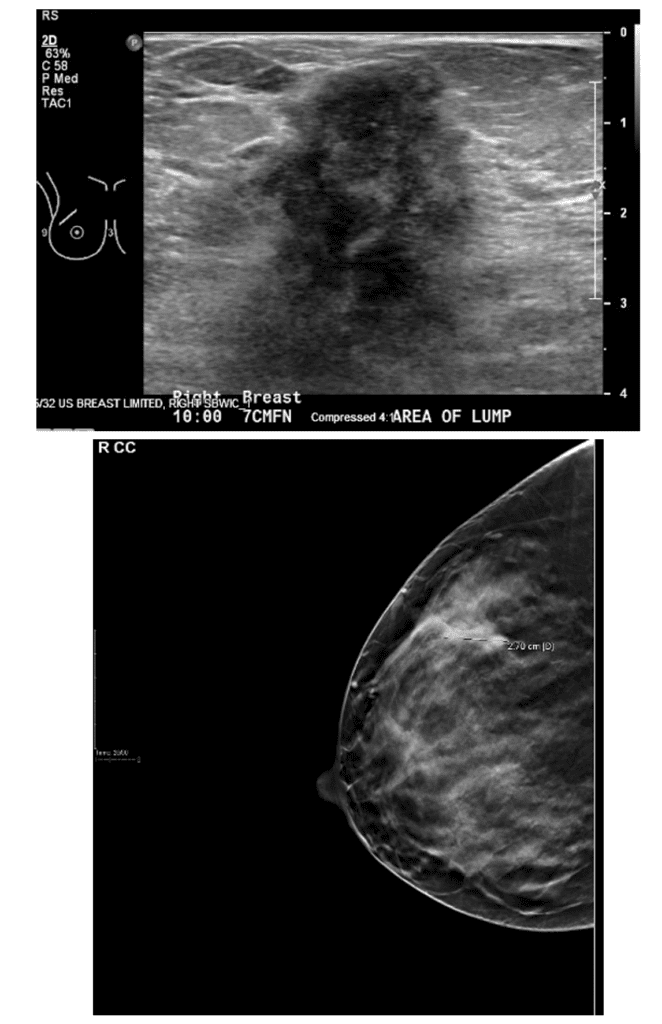
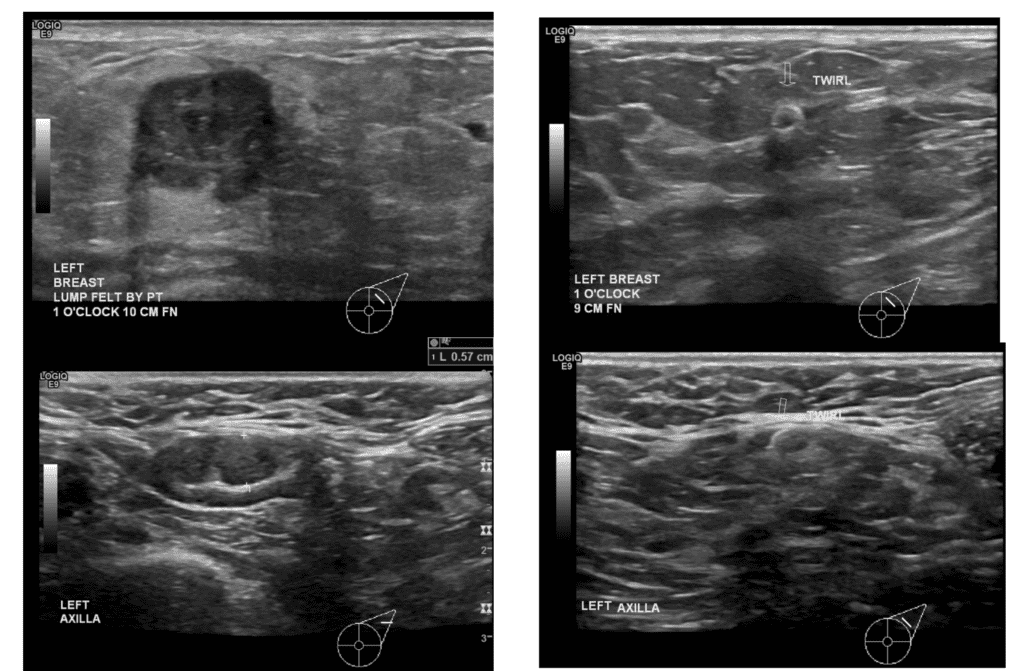
Below are two examples of women who noticed breast changes, the first during pregnancy and the second a few months after weaning her nearly year old baby. Both had symmetric breasts prior to the change.
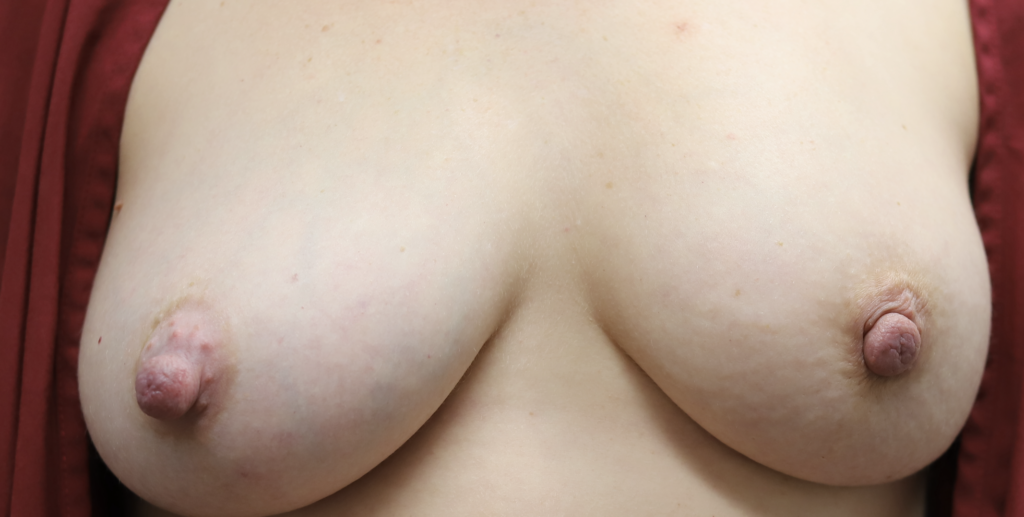
This patient noticed left breast shrinkage during pregnancy with additional areas of lumps she could feel that had grown (above). After chemotherapy, her left breast completely normalized and they became symmetric again (below).
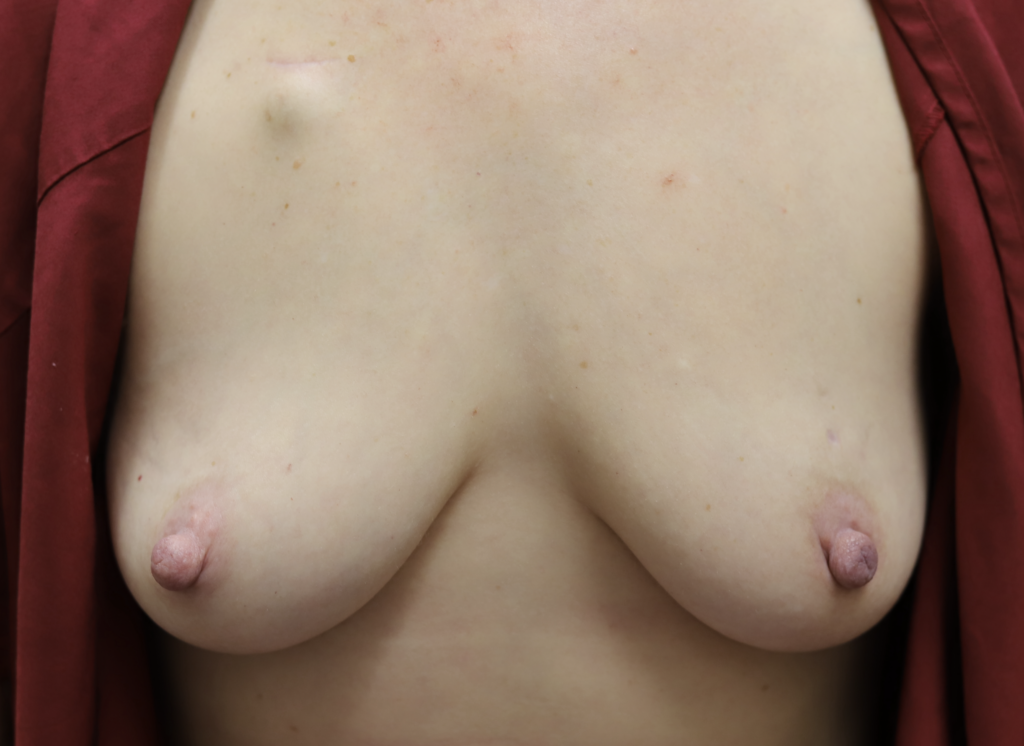
Second example:
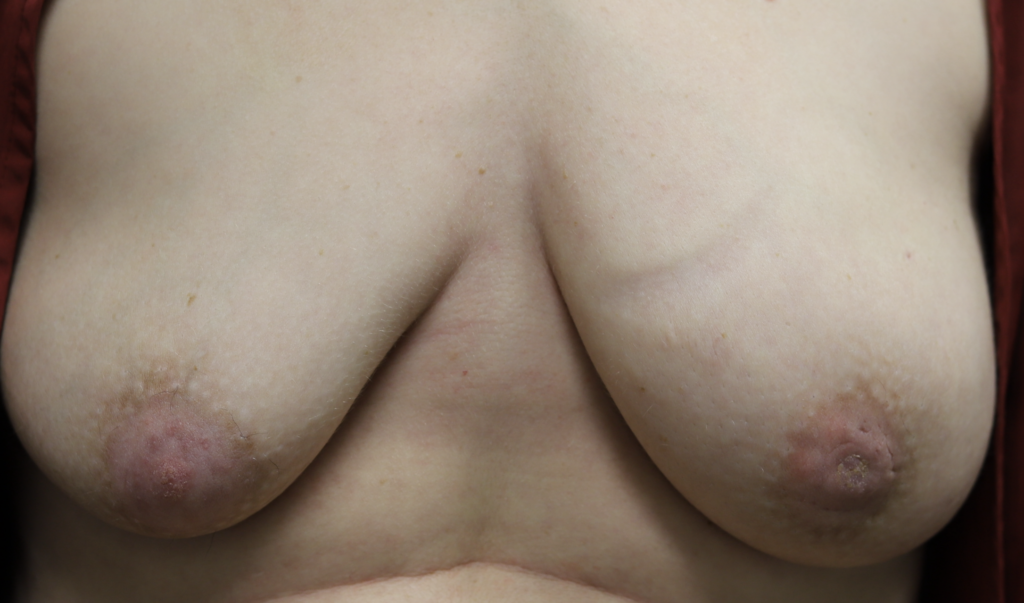
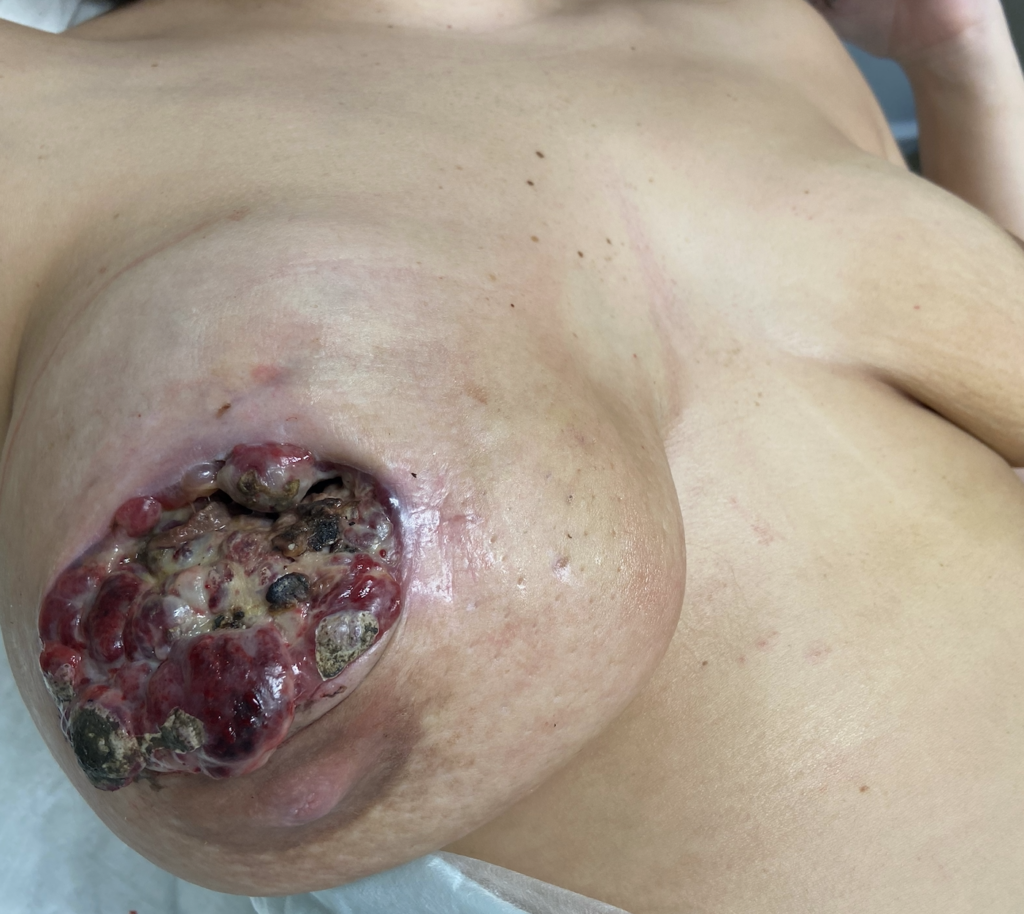
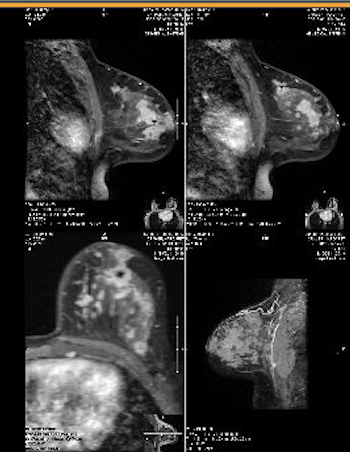
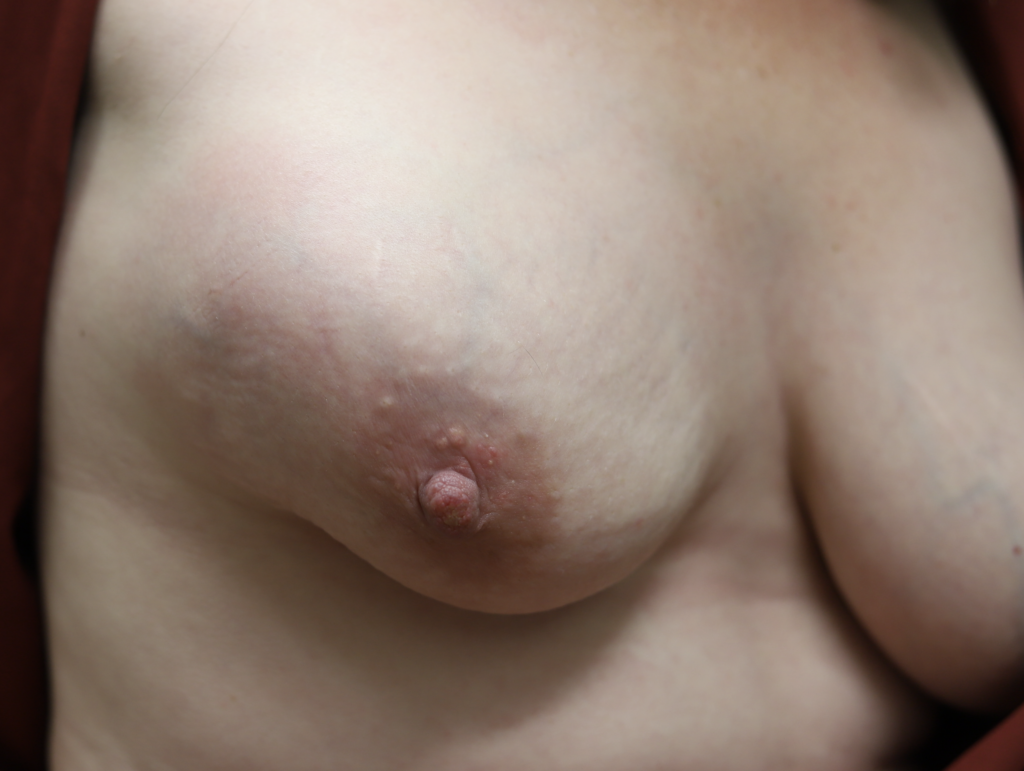
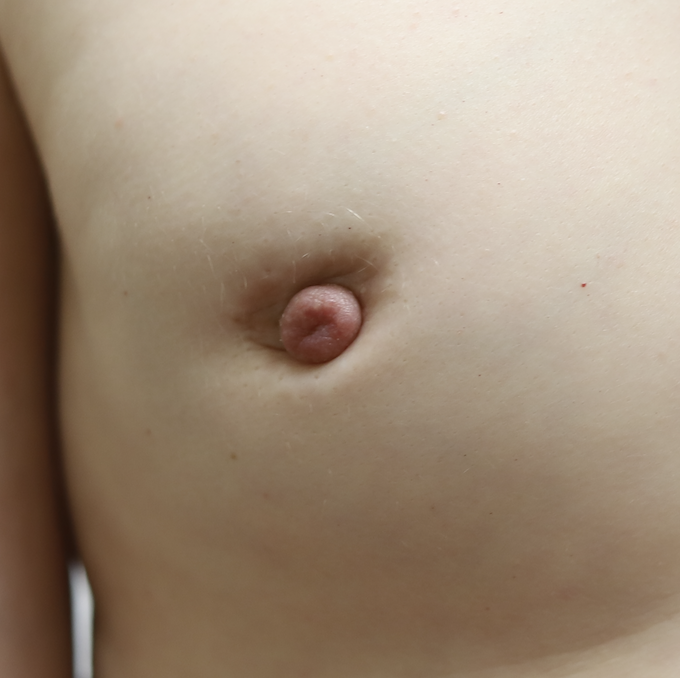
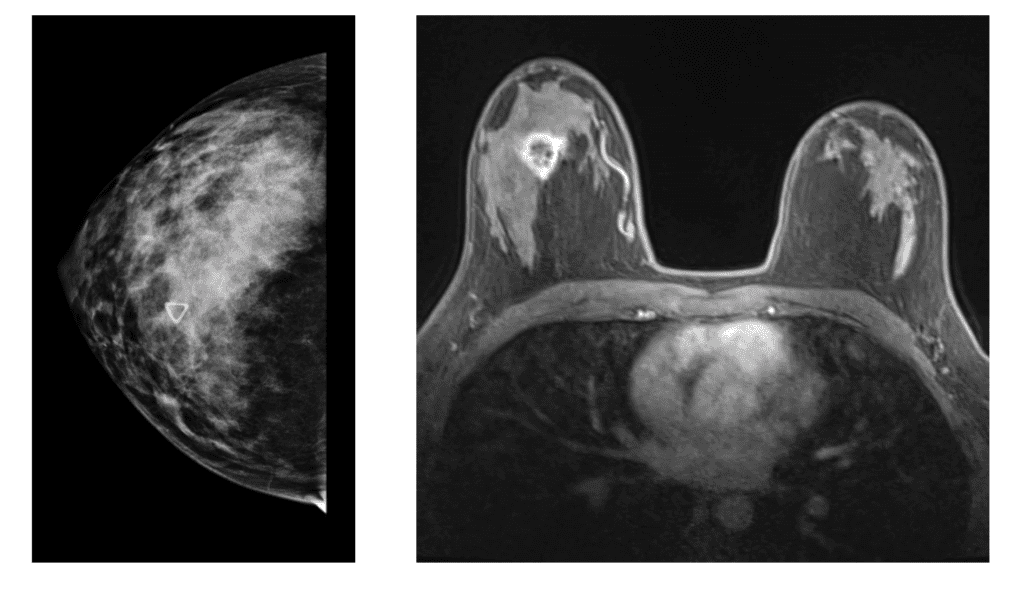
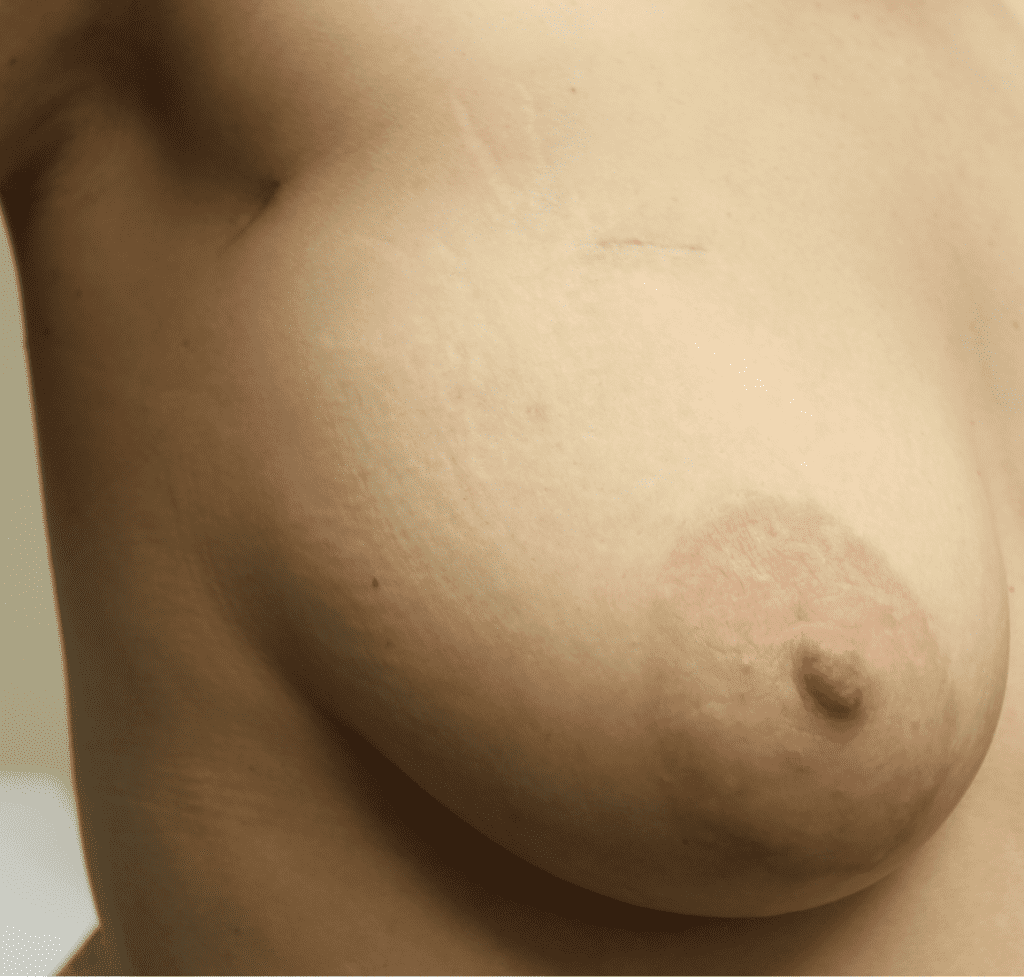
This patient above noticed left breast growth and swelling a few months after she weaned her infant. She fortunately sought medical evaluation quickly, as this was an early presentation of inflammatory breast cancer (skin involved with cancer). You can see the lymphedema (swelling, pitting in the left breast) in the upper inner quadrant where her bra has created a mark (asymmetric from the right side). Her MRI below shows the conglomerate masses and skin thickening.
Babies Can't Taste Cancer
It is important to understand that cancer doesn’t have a taste and your baby won’t detect your breast cancer. If your baby is refusing one of your breasts, this is likely for a variety of countless other circumstances (flow too low, flow to high, forcing it, ear infections etc).
The only time a baby will refuse a breast because of cancer is if there are too many skin and nipple changes (case example #1 above) that make milk flow and latching unideal and unappealing. However, this is not an early sign of breast cancer — these changes occur much, much later.
Unfortunately, a report from the 1960s (prior the introduction of modern breast imaging and essentially modern/current medicine) documented the “Goldsmith Sign” as being indicative of a mom’s occult cancer detected by baby. There is no actual history or physical exam reported in the case. It is simply the doctor’s recounting of the mother’s own interpretation of the situation. One of the main improvements we need with lactation is for a provider to take their own history and physical exam, and make their own differential diagnoses and conclusions — not just report personal observations that could be remembered incorrectly or confounded (confused) in different ways.
Diagnosis and Breast Imaging

Mammograms, ultrasounds, and MRIs are safe with breastfeeding. When a breastfeeding mother has a suspicious mass or other concerning finding, she will first be recommended to undergo biopsy. There is no need to interrupt or stop breastfeeding before or after an ultrasound- guided core needle breast biopsy, stereotactic core needle biopsy, or MRI-guided biopsy. Because the stereotactic and MRI-guided biopsies use a larger size needle, remove more breast tissue, and produce a larger size opening in the skin, the theoretical risk of milk fistula may be higher.
A large cohort of pregnancy-associated breast cancer (PABC) patients demonstrated no milk fistula after surgical procedures. A study of nearly 80 patients in my practice who underwent surgery, core needle biopsy, or other interventional procedure such as abscess drainage showed < 2% developed persistent fistula.
The key is to manage lactation appropriately. Patients should not pump to “keep their breasts” empty after a procedure, as this worsens hyperlactation (oversupply) and will in fact promote fistula development.
Biopsies, Clips, and Lidocaine
Incision should also be placed away from the nipple and areola to avoid trauma to the incision from a pump or infant latch. Patients should simply breastfeed as normal after a procedure to promote physiologic healing.
Temporary low-volume drainage lasting several days is normal and expected after a biopsy. Milk may be blood-tinged, but is safe. Titanium clips placed at the time of biopsy are safe and nearly microscopic in size. Anyone with a history of breast surgery very likely has surgical clips in their breasts that are similar. All are safe.
Lidocaine, a local anesthetic used during breast biopsy, is considered safe with breastfeeding after intravenous, epidural, and high doses as a local anesthetic. There is no data on small volume injection used locally in the breast. However, lidocaine has poor oral absorption and therefore breastfeeding does not need be interrupted with small volumes. Epinephrine, a local anesthetic that may be used in conjunction with lidocaine, has no available data in breastfeeding. However, it also has poor oral absorption and therefore is unlikely to necessitate interruption in breastfeeding.
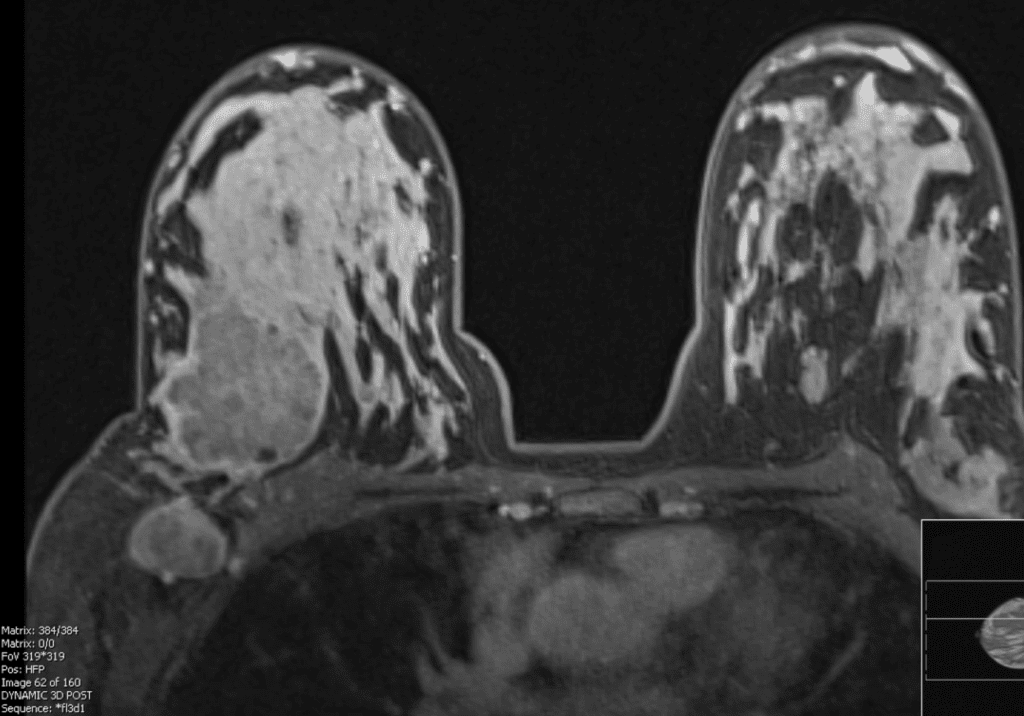
Staging
After initial diagnosis, patients will often be recommended to undergo systemic staging (looking for any cancer elsewhere in their body). This is performed with a single PET CT scan or a plain CT of the lungs and abdomen/pelvis combined with a bone scan.
A PET CT requires 12 hour separation of baby/mom due to external radioactivity, but the milk itself is safe to give as FDG (the IV agent given to localize cancer) is not excreted in breastmilk.
No interruption of breastfeeding is necessary after plain CT or bone scan.
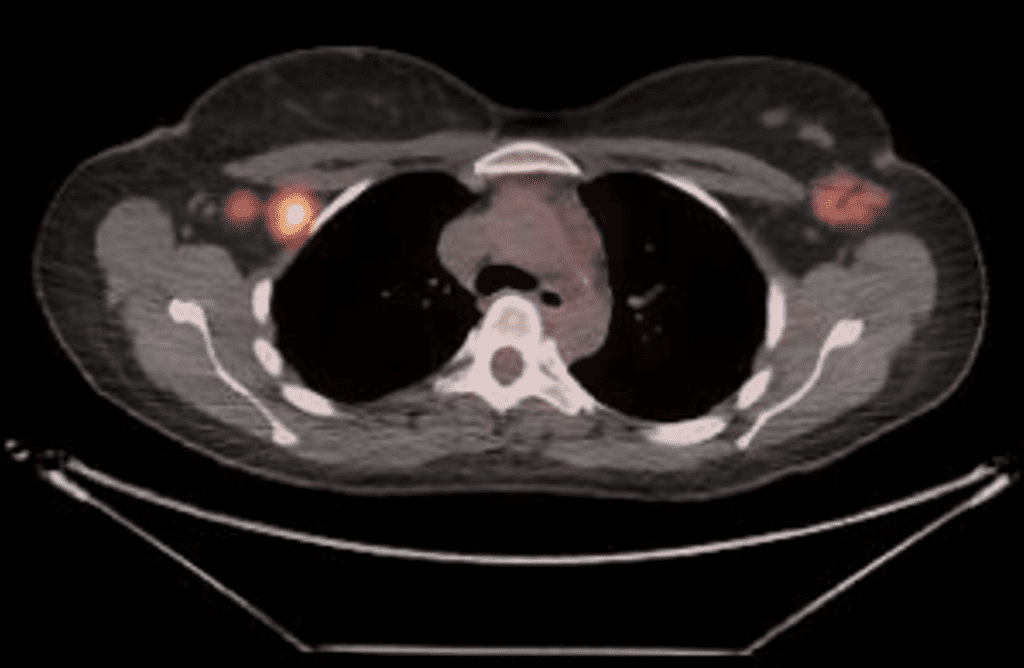
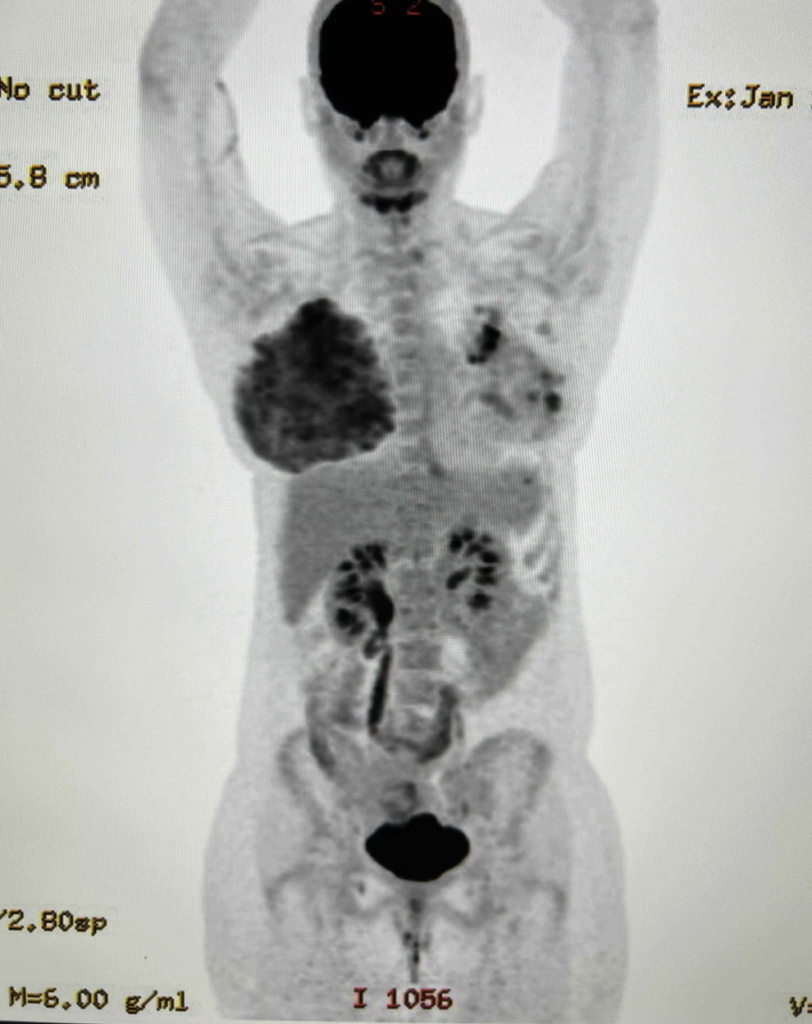
This PET scan performed above for a left breast cancer (shown by the black areas in the left breast) demonstrates the remarkable metabolic activity of the lactating breast (right). This patient was mainly feeding on her right breast due to skin changes and inability to feed the infant on her left breast with cancer. You see that the lactating breast is actually more “FDG avid” (meaning it takes up more of the radio nucleotide, FDG, that the PET scan uses to determine metabolic activity) than the breast cancer itself.

Chemotherapy
Once diagnosed, young breast cancer patients may be recommended to undergo chemotherapy prior to surgery. Due to the transfer of chemotherapy agents into breastmilk, breastfeeding is not possible with chemotherapy for breast cancer.
If you are in this situation and have high milk production (e.g. early postpartum), then your physician can prescribe cabergoline 0.5 mg by mouth (taken every 72 hours) the day chemotherapy starts. Usually, with very high production, you need 2-3 doses. If you’re further postpartum you can stop feeding and hand express or manual pump just to comfort and/or ice and advil and/or tylenol for pain (check with oncologist about other pain medication options if needed).
This is often the worst part of diagnosis for many of these young breastfeeding patients. It’s truly heartbreaking.
They may ask about pumping and discarding milk, and breastfeeding at short intervals during chemotherapy. While I always tell patients I will support them in what they desire, I do not recommend doing this for these reasons:
- Unlike other cancers that may require a shorter duration of chemotherapy, breast cancer regimens generally last 4-6 months. This is a LONG TIME to pump and dump.
- Tumors that are HER2+ will also require treatment with trastuzumab and pertuzumab in the postpartum period. There are no data on these agents during lactation (though, like other monoclonal antibodies, they likely are not excreted in milk — we just can’t prove it yet).
- While young, healthy women generally do very well with chemotherapy, it’s still HARD on the body. You add breastmilk pumping around the clock to this and it becomes even more exhausting.
- Breastmilk is going to decrease considerably in volume during chemotherapy (the chemotherapy is targets the breast tissue to shut down!)
- Breastmilk microbiome changes during chemotherapy.
- Pumping has its own set of risks — mastitis, blebs, galactoceles, etc. A bad infectious mastitis could land a neutropenic (when the immune system is at its lowest) mom in the hospital. Any infection during chemotherapy can be life-threatening.
- Unfortunately, bringing baby to the breast at short intervals in between chemotherapy regimens is not particularly realistic. A baby will be getting bottles for a week or two or three at a time. A mom may have a short (day or two at most) window where she could safely breastfeed (this is because we need to keep the levels of chemotherapy constant in the blood during treatment).
- When mom does bring an otherwise bottle-fed baby to the breast every few weeks for a short period of time, it can be very emotional if the baby refuses the breast (for both mom and baby).
- This occasional latching with lowered milk volume can cause pain or nipple wounds.
Overall, I try to support the breastfeeding grief in this scenario. A diagnosis of young breast cancer comes with innumerable losses, many of which are irreplaceable. I help moms find donor milk and formula options, as well as perinatal mental health therapists.

Surgery
If a patient is recommended to undergo surgery before chemotherapy, there is NO INDICATION TO DELAY SURGERY. I can’t emphasize this enough, as I have had countless patients seek second opinions with me who were told they needed to wean completely and/or wait to undergo surgery for cancer.
This video below is a patient who contacted me from the UK after her original surgeon said she couldn’t get a mammogram for at least four weeks after completely weaning both breasts, and said her surgery would have to be delayed even further. She sought a second opinion and found a surgeon who performed the mammogram immediately and supported her continued breastfeeding from her unaffected breast. She was reunited with her one year old and three year old tandem feeders two days after surgery.
Patients also should not be denied reconstruction after mastectomy if this is something they otherwise would have wanted. If anything, recent lactation means the breast is very vascular (i.e. very good blood supply), which is important for healing and prevention of wound infections. The antimicrobial components of breastmilk also theoretically provide benefit.
If you are in this situation, start to downregulate the breast that will be undergoing surgery. This means feeding on the unaffected breast first to empty it and then just “topping off” any additional milk your baby may want with the affected breast. You may get lumpy and engorged in the affected (downregulating) breast, but know that this is not dangerous, it’s not an infection, and it will get better after a few days of support with lots of ice and pain/anti-inflammatory medication. Even if you only have a week before your surgery, this downregulation will still help and will also start sending signals to the normal breast that it needs to step up its production.

As described in the History of Breast Cancer section, mastectomy or lumpectomy and radiation preclude breastfeeding from the affected breast. It is not unsafe to give the baby milk from the affected breast after a lumpectomy and before radiation, but the wiser approach is to continue to allow that breast to downregulate,
Cancer patients also may undergo a procedure called “sentinel lymph node biopsy.” To perform this procedure, patients undergo injection with “blue dye” or technetium, a nuclear medicine agent. The use of technetium for lymph node mapping is likely safe in lactation, but there are no data on blue dyes. If the patient’s tumor is hormone receptor positive, she ultimately will be recommended to start adjuvant endocrine therapy at the completion of other treatments. Patients should have a careful discussion regarding possible approaches with their physicians.

Radiation
Even if you were able to preserve your breast with a lumpectomy, you very likely will require radiation after surgery. Radiation causes cell death and prevents cancer recurrence. You should not attempt to continue breastfeeding during radiation, as this can cause infection and other complications that may delay or otherwise impact your cancer care.
Once you have radiation treatment to a breast, it will never function normally again. This is important for preventing breast cancer recurrence, but it also means you can’t resume breastfeeding after radiation treatment is complete.
It is also important to note that radiation therapy is extremely precise and only impacts the affected breast. It does not scatter to the normal breast. And even if it were to inadvertently happen (extraordinarily uncommon), it would simply cause some cell death in the tissue that was impacted. The breastmilk wouldn’t be “radioactive.”
Radiation is not “radioactive” the way “nuclear medicine” tests are radioactive (e.g. PET scans or gallbladder HIDA scans). Radiation is ON/OFF – just like a plain X-ray. You get radiation to that specific body part in the exact moment, but it doesn’t continue after that. Otherwise, we would all be radioactive after dental x-rays, mammograms, arm x-rays and every other test like that!
Endocrine Therapy
You may be recommended to wean from the unaffected breast to start endocrine (anti-estrogen therapy that reduces recurrence) if you are still lactating from one breast after the completion of surgery and radiation. Endocrine therapy will be recommended with tumors growing using estrogen and/or progesterone.
This becomes a very nuanced conversation and shared decision making with your oncologist, as we do not have any data in this arena. We don’t know whether continued breastfeeding may reduce recurrence risk and/or survival (i.e. whether it is equivalent or possibly superior to endocrine drugs).
Unusual Circumstances
There are a few unusual circumstances that I want to mention in the event it may help someone working through something similar.
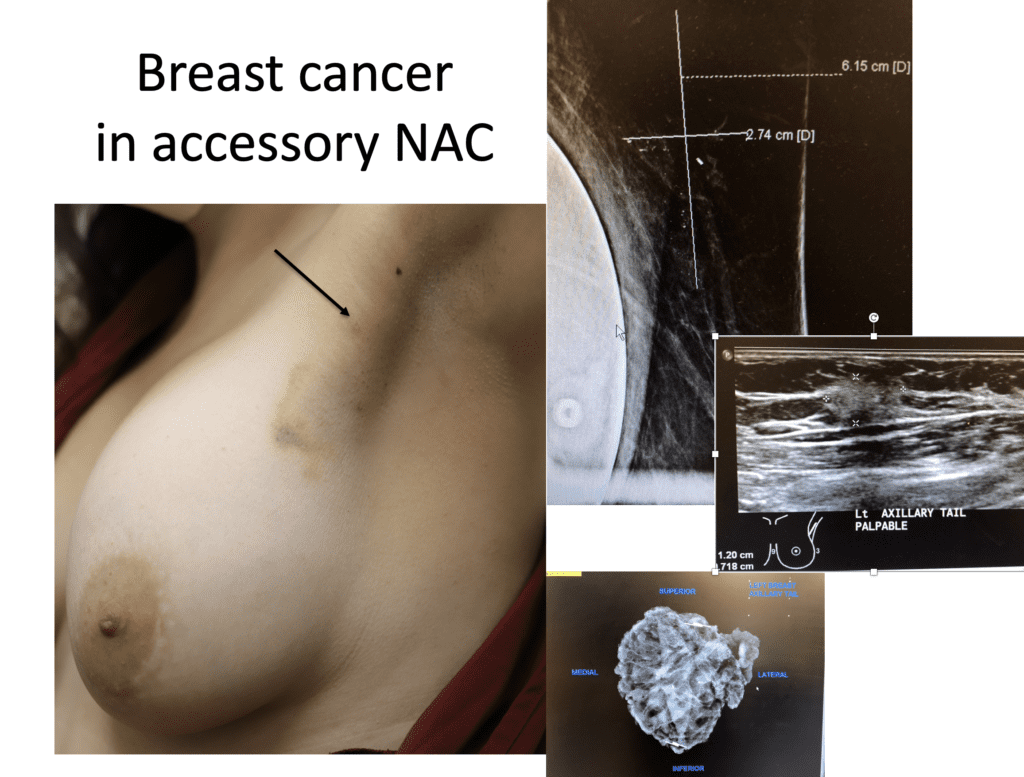
First, it is uncommon, but possible, to develop breast cancer in an accessory (extra) nipple areolar complex (NAC). This patient below presented with a mass under her arm that initially was thought to be scar tissue from a previous history of breast augmentation. However, ultrasound showed the presence of a concerning mass, and mammography confirmed additional calcifications suggesting additional areas of disease. The patient underwent a lumpectomy of this region with removal of the small accessory NAC from which the tumor arose.
Angiosarcoma is an extremely rare cancer, particularly in the breast. Because of this, despite all the correct interventions, it can be misdiagnosed. This patient underwent appropriate imaging and biopsy, but the biopsy unfortunately did not contain angiosarcoma tissue for diagnosis when it first was performed. The team thought this may be a particularly terrible abscess in lactation, but performed a second, diagnostic biopsy when it did not improve.