Breast Growth and Engorgement
Significant breast growth can be painful, and cause the lower parts of the breasts to swell and develop a pink or reddish color. This is called breast “lymphedema” (similar to swelling of ankles when sitting for too long). The first step is to obtain a very supportive bra, as tight fitting as you can handle with comfort (similar to compression stockings for your calves). It is a myth that tight fitting bras cause breast problems or mastitis after the baby is born. Mastitis results from factors such as hyperlactation (oversupply) and high blood flow into the breast, NOT from external compression. It is also very uncommon to develop mastitis during pregnancy. If you do experience symptoms, you should be evaluated by a breast specialist to ensure the changes are consistent with normal breast growth versus another process such as granulomatous mastitis (which is not caused by pregnancy or lactation, but can occur in women of childbearing age).
You also can perform light lymphatic drainage yourself. If this does not resolve your swelling, or if you only have one breast that is affected, you should seek evaluation with your healthcare provider. I developed a handout demonstrating the technique of lymphatic drainage. I also co-authored a manuscript that summarizes the application of physical therapy pain relief techniques in lactation.
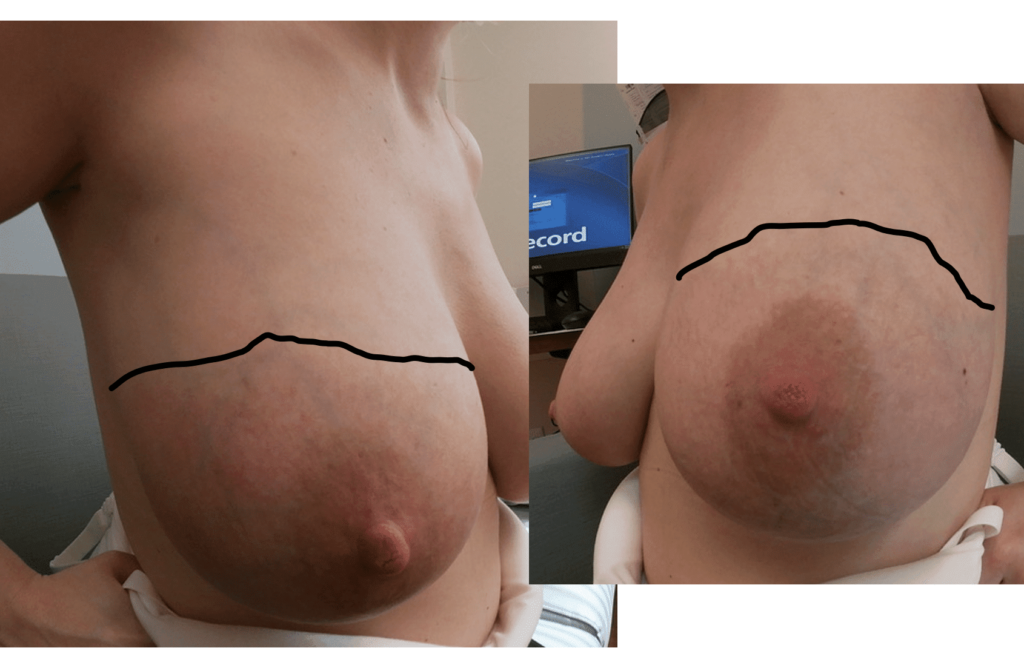

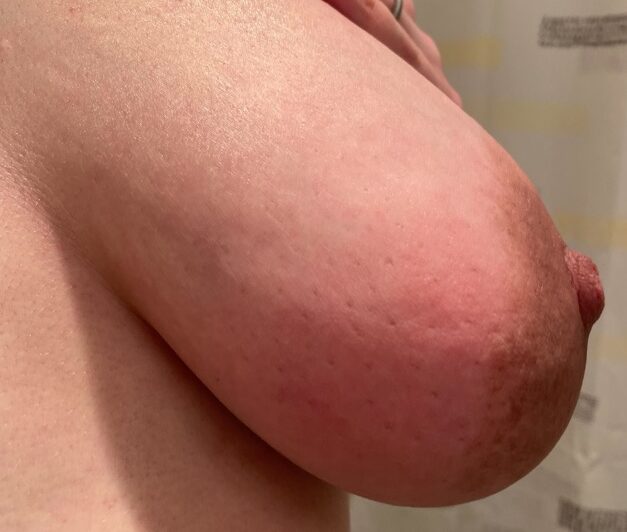
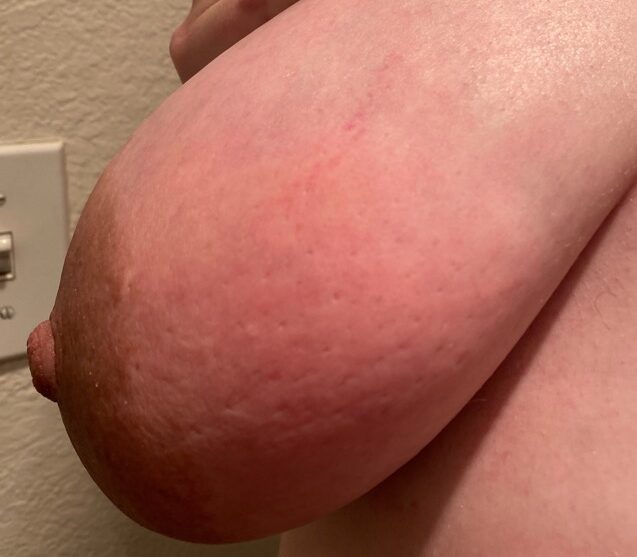
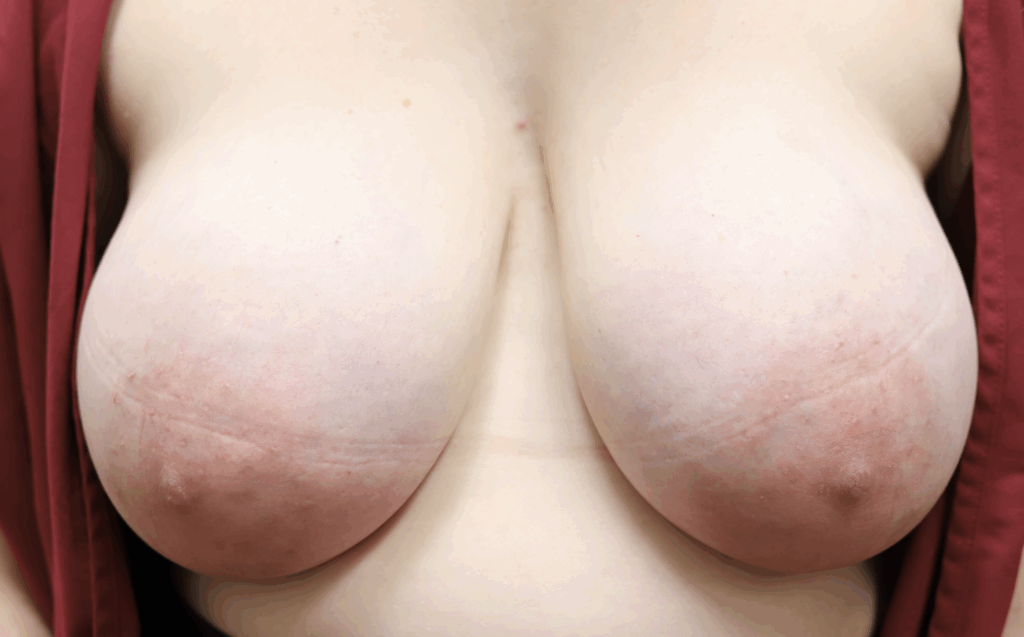
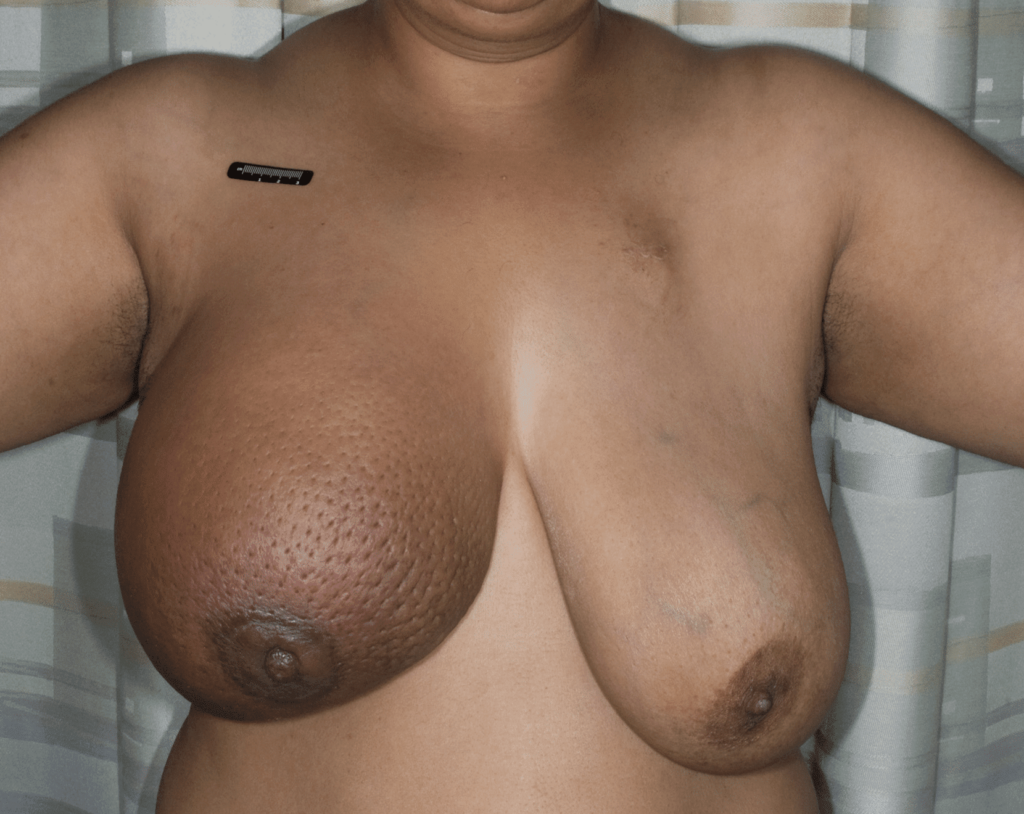
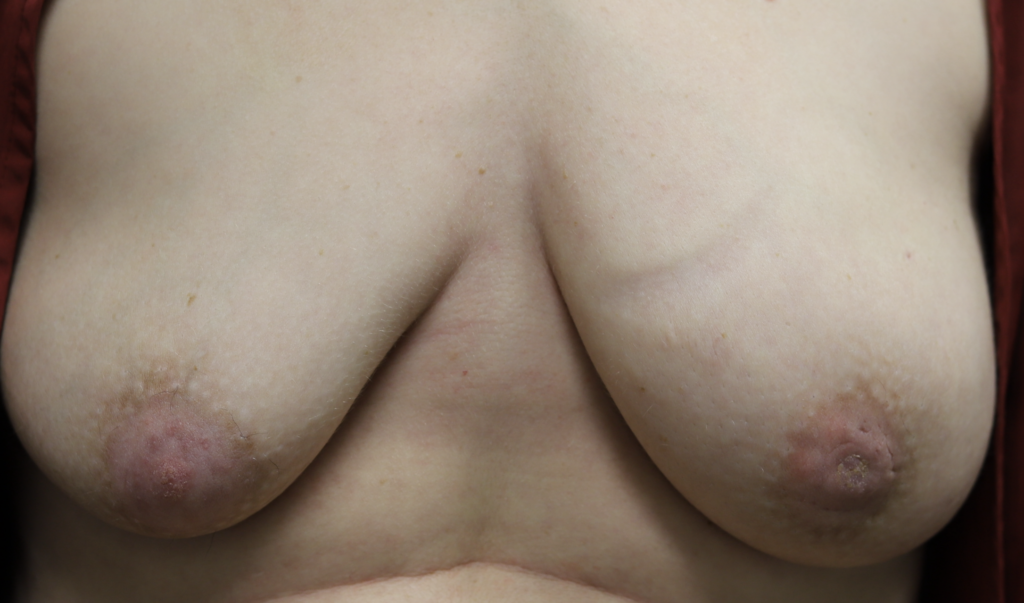
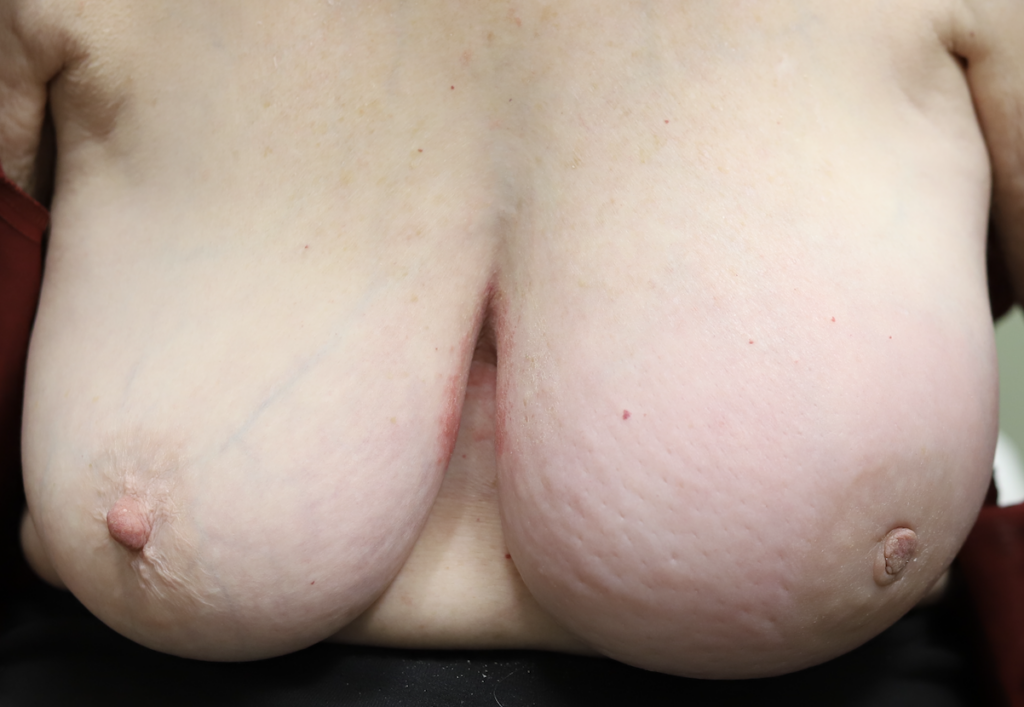
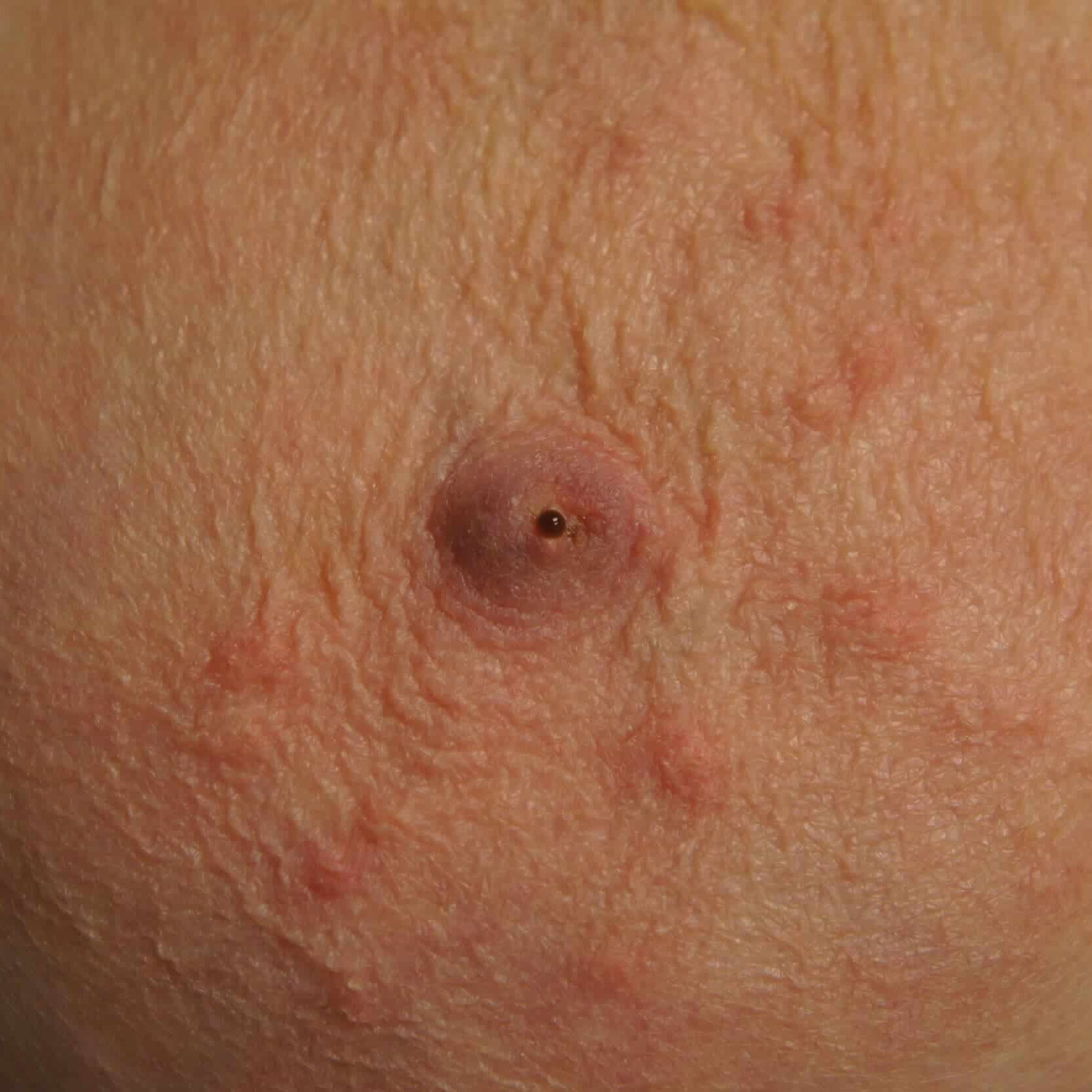
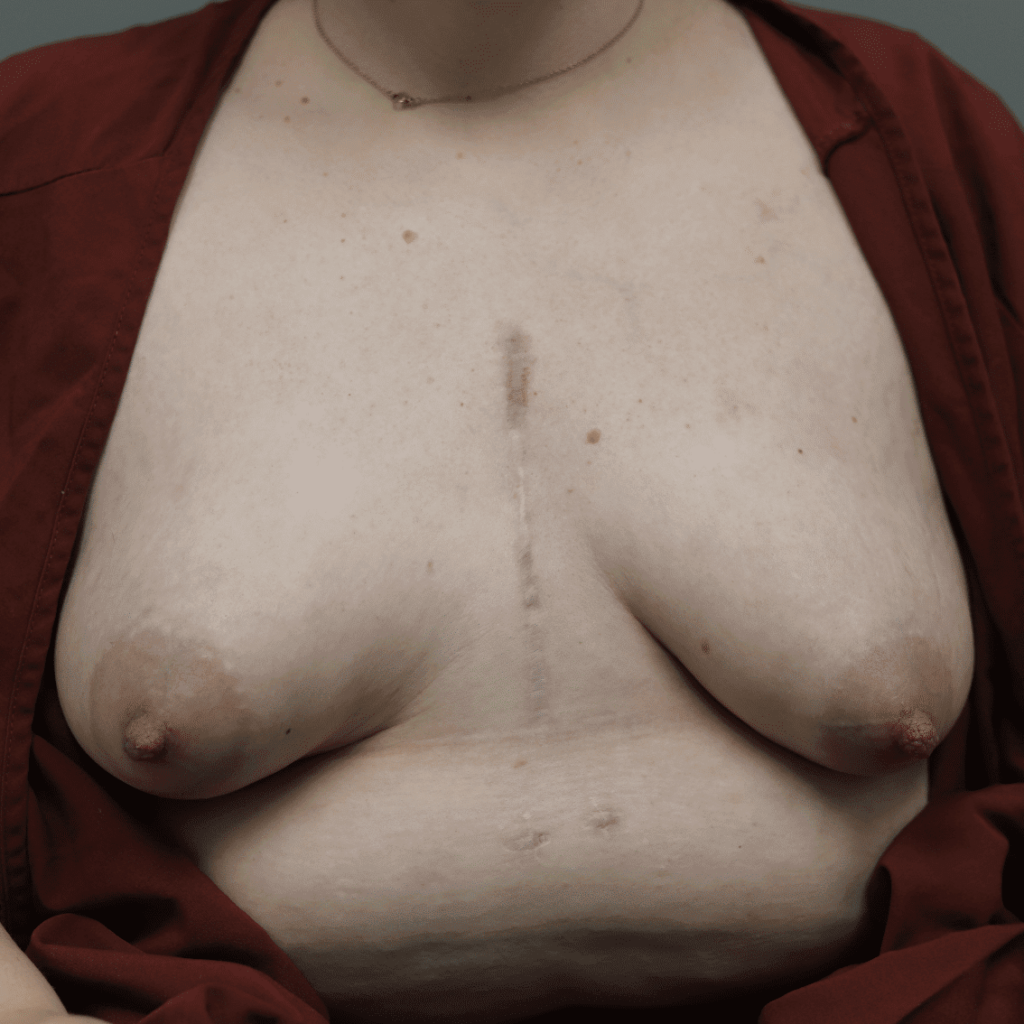
Redness, pitting, and swelling (edema) on in the lower part of both breasts during mid-pregnancy (above). Symptoms greatly improved after initiating lymphatic drainage and wearing a compressive, supportive bra (below).







Inflammatory Breast Cancer Versus Engorgement
It is not uncommon for women to experience significant breast growth and notice that the lower parts of their breast are faint pink or red in color, or even pucker a bit as shown in the breast growth photos above. However, it’s important to assess the swelling and puckering for symmetry (i.e. it is the same on both breasts, and focused the lower portion where fluid collects, much like swollen ankles on a long plane flight).
Inflammatory breast cancer develops the vast majority of the time on one breast and progresses very rapidly in an asymmetric way. The entire breast is affected and becomes thickened, very tight, and often shrinks/retracts with classic “peau d’orange” changes. It is frequent to have lymph nodes involved with cancer.
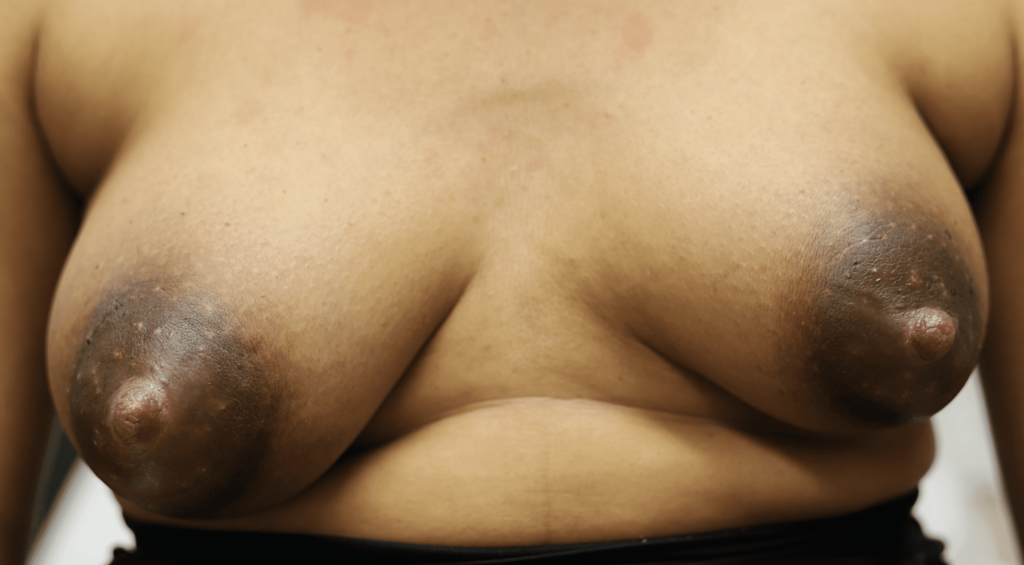
As you can see, this image of inflammatory breast cancer below are very different from the photos above that show both breasts being affected in the same way, mainly in the lower parts of the breast. Further, swelling caused by significant breast growth responds to a tight fitting bra and lymphatic drainage, whereas breast cancer does NOT.
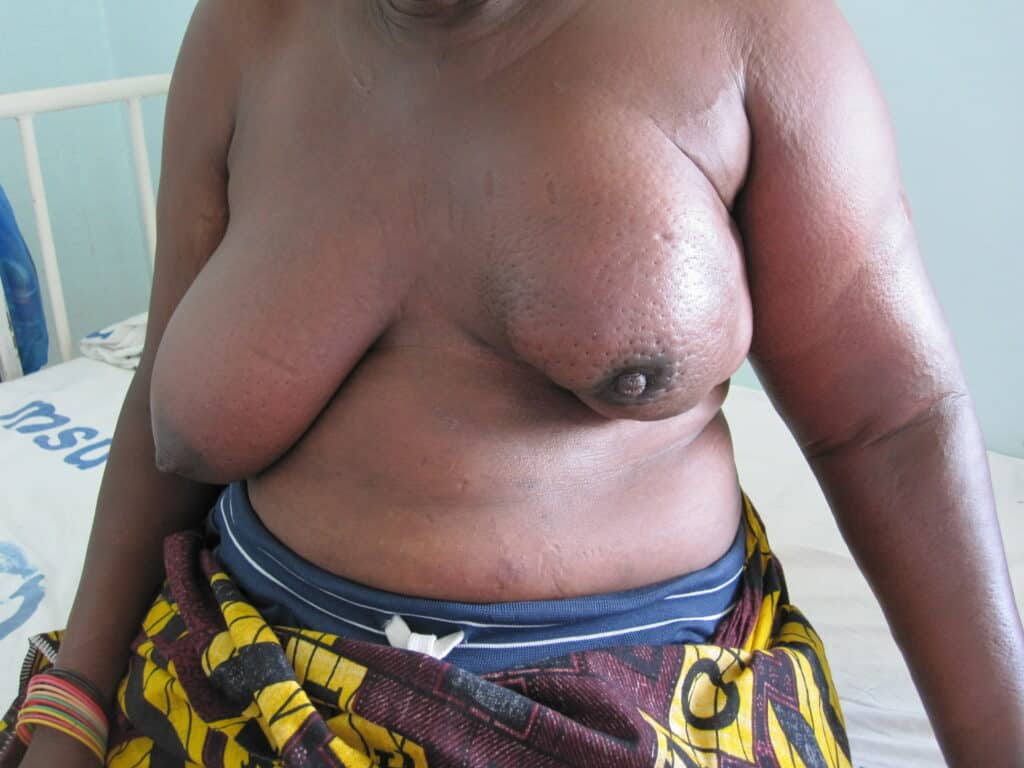
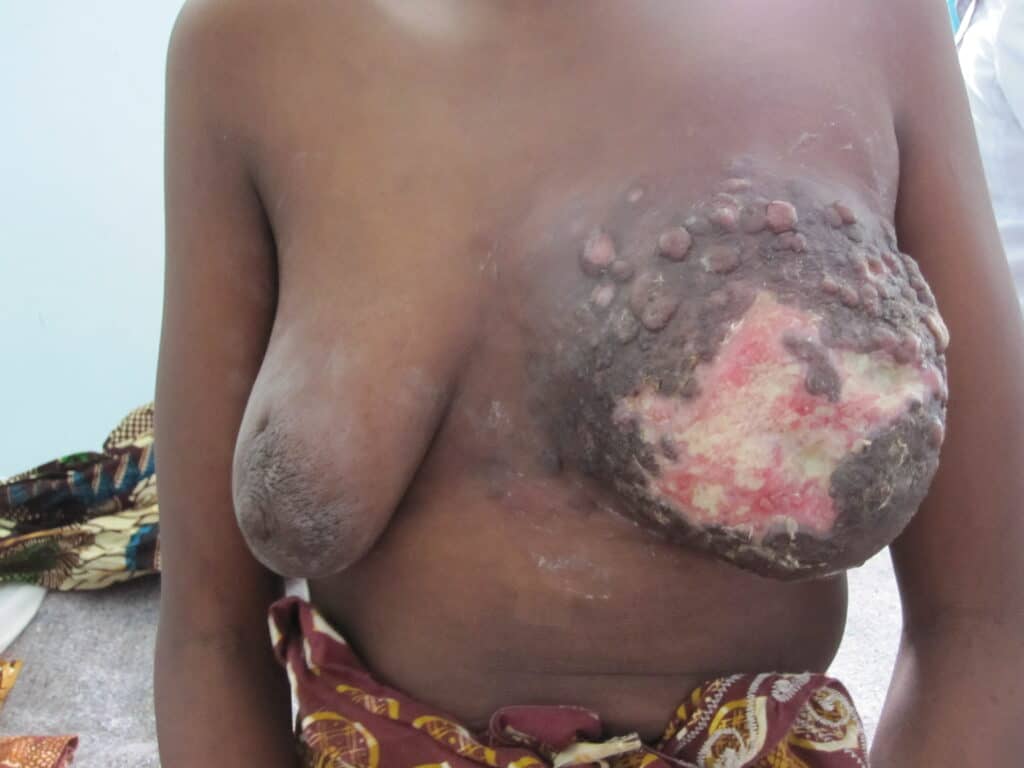
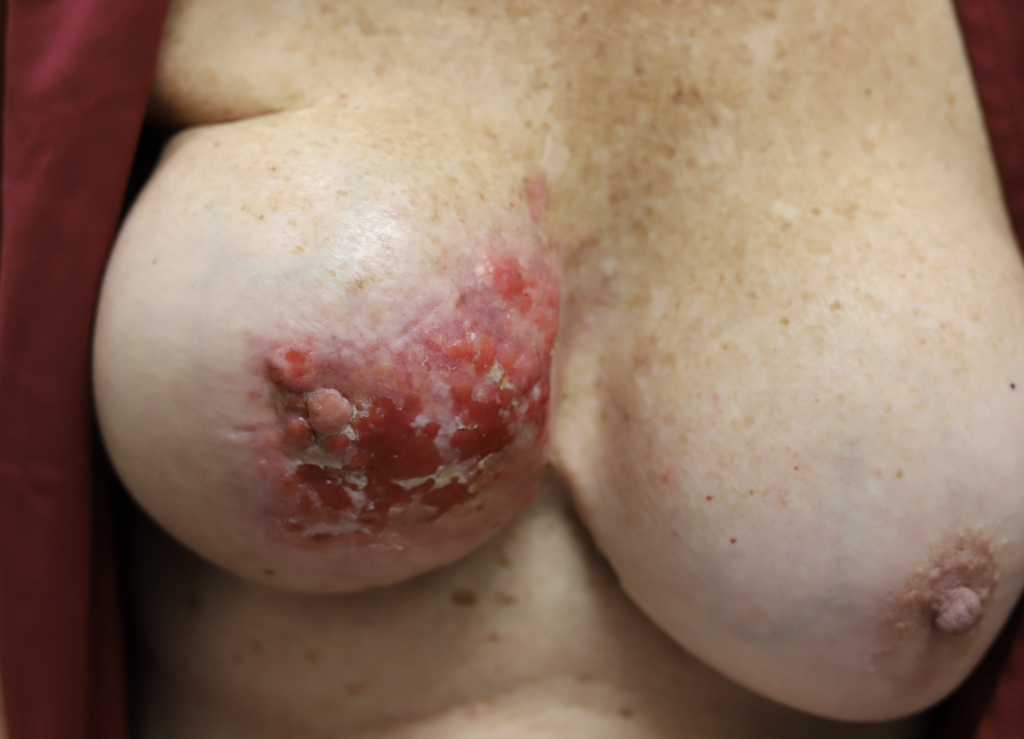
This is a very early presentation of inflammatory breast cancer without any delay to diagnosis (therefore the redness and peas d’orange had not started to take place). This patient noticed left breast growth/firmness (where her breasts had previously been symmetrical) a few months after weaning her baby. Imaging showed concerning tumor masses, lymph nodes, and biopsy of the skin showed dermal lymphatic involvement. You can see that her left nipple has started to become retracted, and you also see some new edema (upper inner quadrant) from her bra (lymphatic system of breast not working well when involved with tumor cells).

Colostrum in Pregnancy
From the beginning of pregnancy, the breasts prepare to make milk after delivery. Breast growth may be the first sign of pregnancy, even before a missed period. Breast growth tends to be the most significant during the first trimester and the last trimester. Lactogenesis I, or “secretory initiation,” occurs in the second half of pregnancy and is when the breast cells begin to prepare to make milk.
It is normal to notice colostrum (clear or yellow tinged “early milk”) in the second or third trimester of pregnancy. Mothers who may be at risk for lower milk production (e.g. diabetes, obesity, infertility, previous breast surgery and others as detailed in the Maternal Health and Illness section of Maternal Concerns. Moms also can learn hand expression to stimulate their breasts and store colostrum prior to delivery.
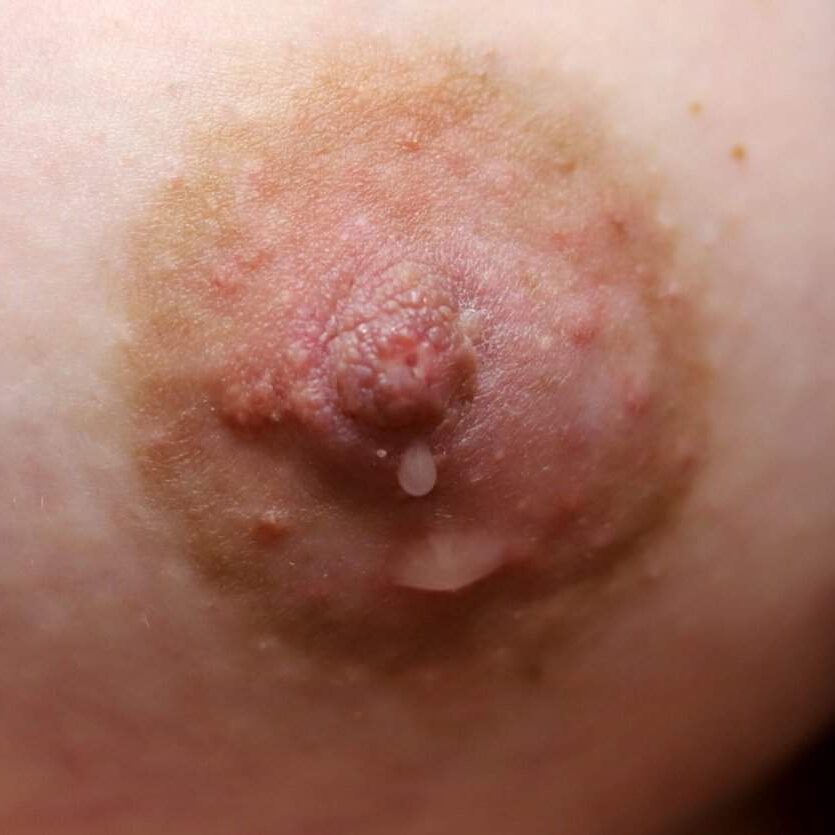
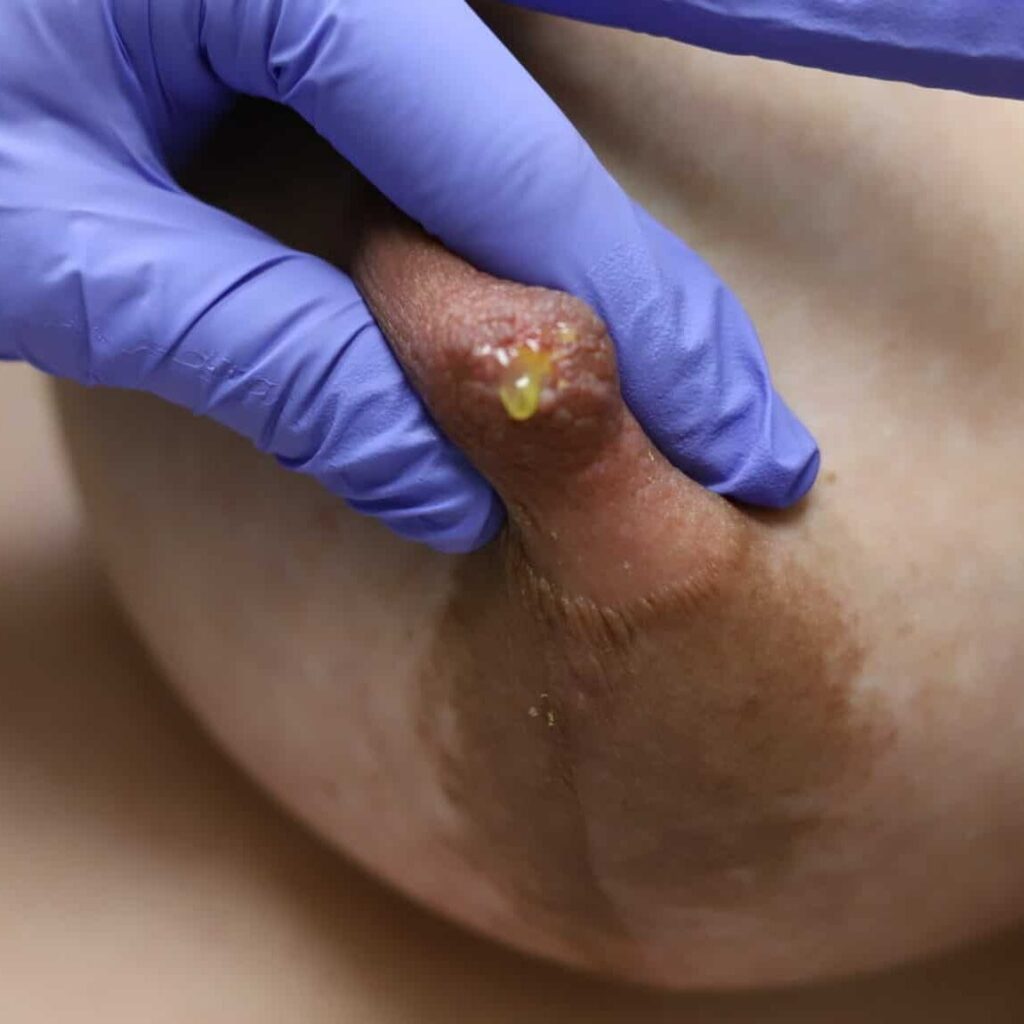
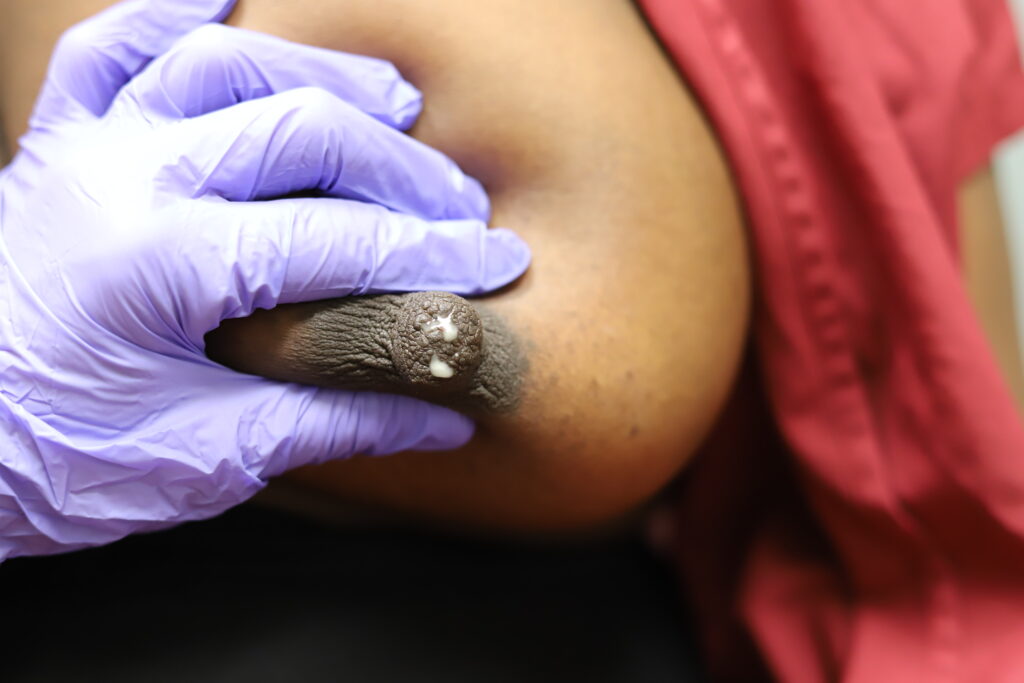
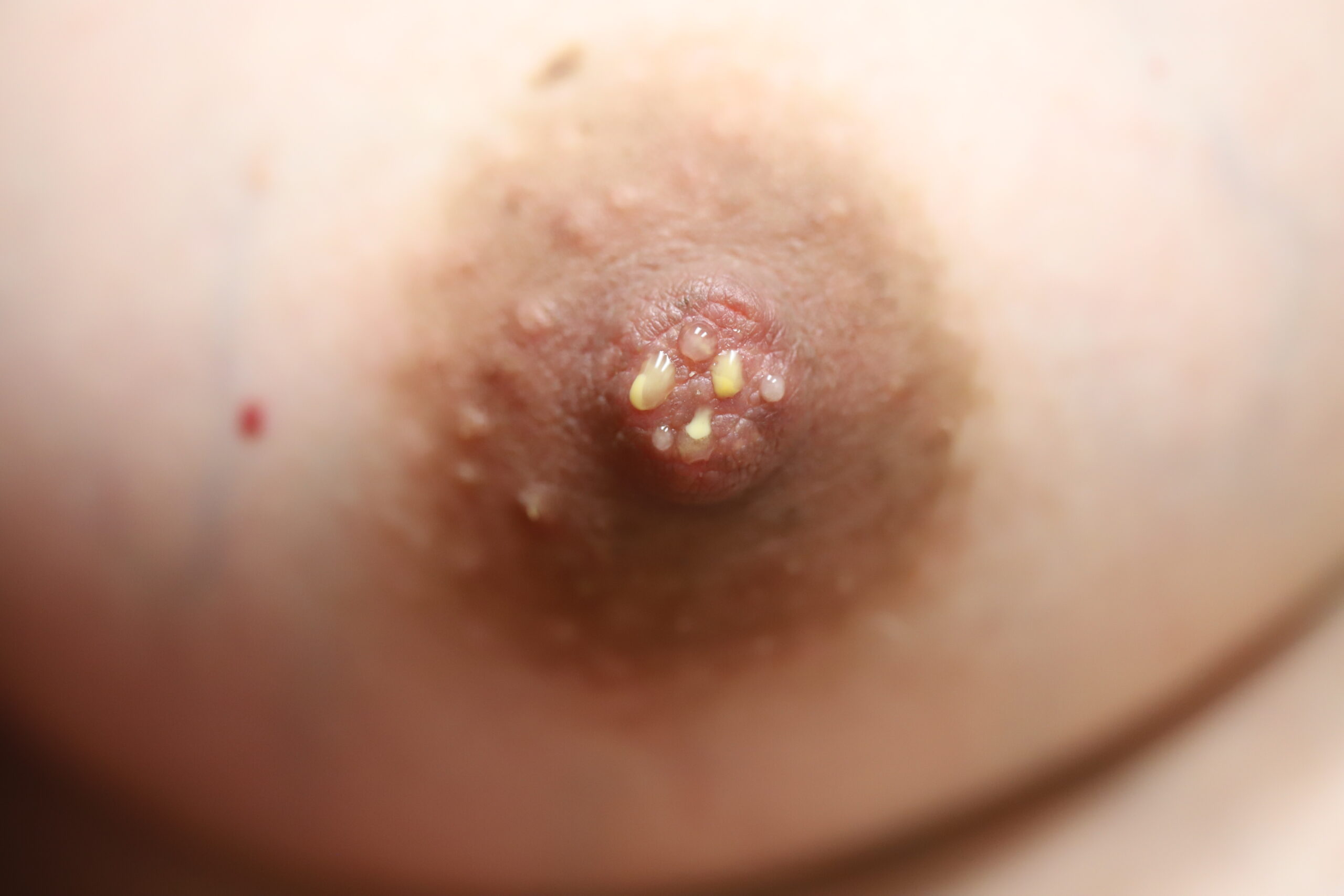
Bloody Nipple Discharge
Bloody nipple discharge may occur in up to 20 percent of women in the pregnant and early postpartum period. It is related to breast growth, increased blood flow, and preparation of the breast to make milk. It generally occurs in both breasts and from several nipple orifices and will worsen with nipple stimulation. If you have any concerns, you should seek evaluation by your healthcare provider. More concerning discharge is from one breast and one ductal orifice.
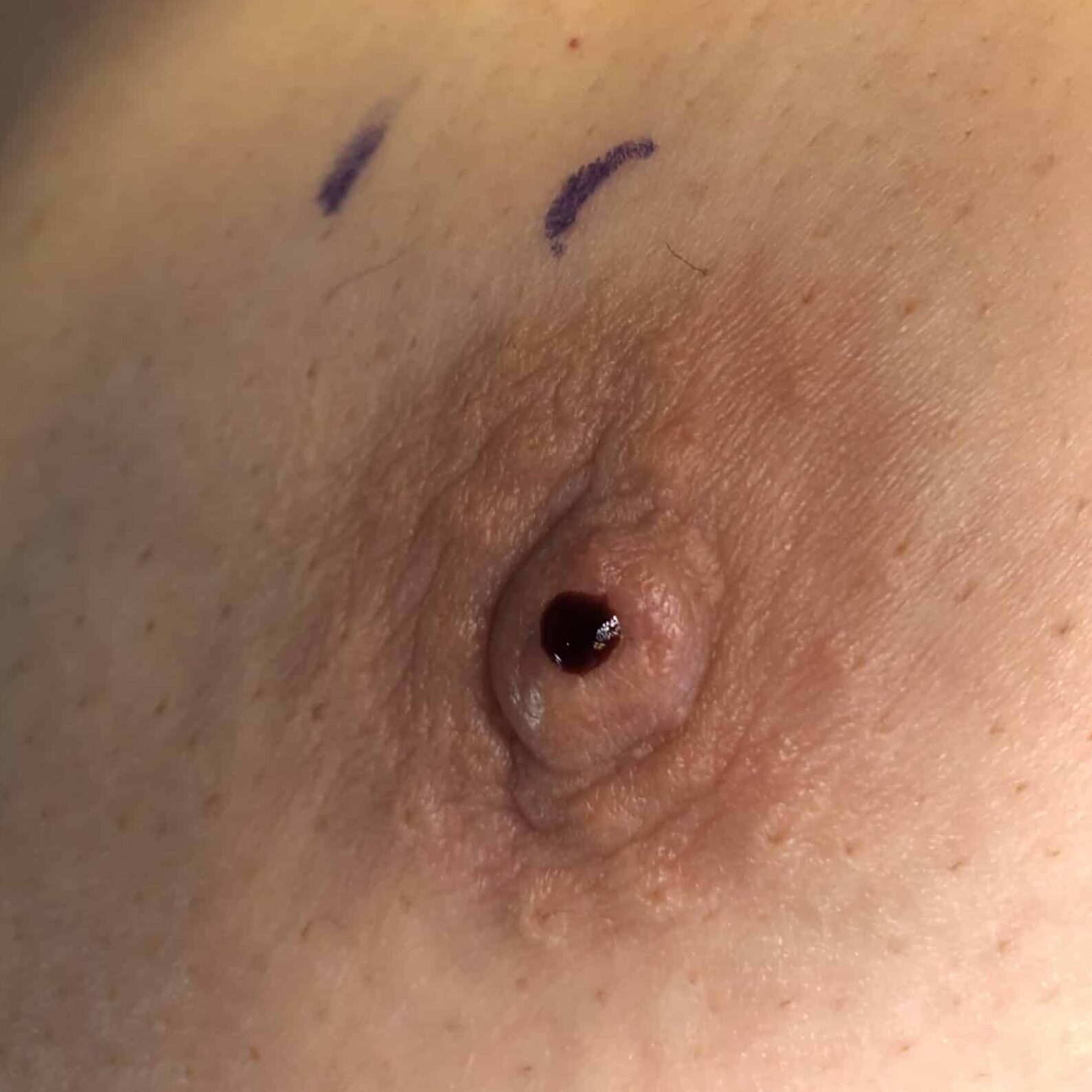
Prenatal Breastfeeding Support
See prenatal breastfeeding counseling if you have a history of any of the following conditions, as these may impact need for supplementation postpartum:
- Significant medical history that has required medications (e.g. high blood pressure, thyroid disease, diabetes)
- Cosmetic breast surgery history (implants, reductions, nipple procedures)
- Breast cancer or other cancer history
- Breast surgery history
- Surgery anywhere in the chest (e.g. heart surgery in infancy)
- Breasts that are significantly different sizes and/or have a more tubular appearance
- Infertility
- History of struggling with breastfeeding with a previous child
- Anything else that may concern you – it’s never wrong to ask for help
The “4th Trimester"

The healthcare system and the American College of Obstetrics and Gynecology (ACOG) recognizes the significance of supporting new moms, infants, and families in their “4th Trimester” after birth. While much attention is given to mothers during pregnancy, they actually need more support AFTER the baby arrives. Despite this, women generally have only one or two visits with their ob/gyn in the first six weeks and no scheduled exams thereafter. Pediatricians may not routinely screen for anxiety and depression, and visits are largely focused on infants. Mothers also may be hesitant to make their needs known to a pediatrician — for fear of seeming selfish or like a bad mother.
Many 4th Trimester programs and medical practices are being established throughout the United States. The University of North Carolina Jordan Institute for Families has a good set of resources for their 4th Trimester Project. This project has a very helpful Toolkit for pregnant moms to review. My favorite “tools” in this group are the Postpartum Planning Tool and the Postpartum Healthcare Visit Checklist. While some women have a “birth plan,” many are less prepared to anticipate exactly what they need as a “postpartum plan” for help and self care.
Breastfeeding Supply List
I do not have any commercial conflict of interest in my medical practice, and do not receive any financial compensation for recommending or supporting particular brands. That said, like anyone, I have some “favorites” that I tend to recommend. This printable list is an example, but any variation on it in terms of branding is absolutely fine!
Nipple and Breast Care
- Organic nipple balm (organic balm has many fewer ingredients than other balms, and does not contain lanolin)
- Lansinoh “Soothie” gel pads
- LanaCare Wool pads (“Uggs for the Breast”)
- Reusable breastmilk pads (causes less allergy than disposable pads)
- Silicone milk collector (e.g. Haaka)
- Hot and cold packs or heating pad
- Supportive maternity and breastfeeding bras
- Nursing pillow

Pumping and Bottles
- Hands free pump bra
- Pump bag
- Hand/Manual pump for middle of the night, small volume milk removal to enable easier baby latch in the setting of engorgement
- Breastmilk storage bags
- Extra pump parts and membranes (breastmilk is not sterile – you do not need to order sterilizing bags because the dishwasher is adequate)
Postpartum Care for Mom
- Advil (ibuprofen) and Tylenol (acetaminophen) or preferred herbal remedies for pain
- Postpartum disposable mesh or reusable underwear (postpartum bleeding should subside over a week or two like a menstrual period)
- Ice pads designed for vaginal/rectal region
- Miralax – Colace and Senna provided by the hospital are not enough!
- Mental health books and resources



Hospital Or Birthing Center
- The World Health Organization (WHO) Baby Friendly guidelines support breastfeeding against commercial interests of formula companies and protect maternal-infant health.
- The Academy of Breastfeeding Medicine has an excellent Model Maternity Policy Protocol regarding hospital guidelines for protecting breastfeeding.
- For delivery, take your pump (have the lactation consultant ensure your flanges fit well and the settings are correct), nursing bra, organic nipple balm, and hydrogel pads.
- Wear home comfortable outfit – you will still look pregnant after birth and won’t be wearing your regular clothes yet!
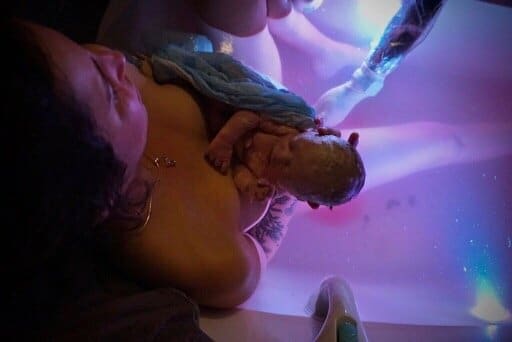
Labor


If possible, it is ideal to limit IV fluids as well as sedating pain medications. Infants of moms that receive epidurals and pain medication with long labors are more sleepy and less coordinated with nursing after birth. This does not mean breastfeeding is not possible. It just means you should be prepared to ask for help if the baby does not latch to the breast immediately.
Skin to skin with your baby after birth is an incredible way to use nature to stabilize yours and baby’s blood pressure, heart rate, temperature, blood glucose, minimize blood loss, and promote breastfeeding. This is particularly important with c-section births and preterm babies.
If birth does not occur in the way you were hoping, and in fact even became traumatic, it is important to seek counseling regarding birth PTSD.
Older Siblings
Depending on the age, older siblings can have variable difficulty in adjusting to a new baby. If your older child is near weaning age and may wean during pregnancy or at the birth of the new baby, you can help ease the transition by finding other ways to “hold” and comfort your older child.
My favorite book on mammalian behavior is If My Mom were a Platypus; this list offers other suggestions. If you have a child who is interested in nursing a doll, you may consider a “new baby” for your child to “nurse” alongside you. Manhattan Toy also has adorable nursing animals like dogs and kitties, and several Etsy artists make custom breastfeeding dolls as well.



Tandem Breastfeeding

It is safe to breastfeed an older child during pregnancy and to breastfeed children “tandem” when the new baby is born. This continued breastfeeding can help the older child adjust to the addition to the family.


Induced Lactation
Adoptive or surrogate moms as well as same sex female parents may wish to induce lactation. This is most successful when the mom has previously breastfed a child or multiple children for years.
Ideally, patients should begin taking an oral contraceptive without interruption (no “blank pills”) to simulate pregnancy. The oral contraceptive is stopped one month prior to delivery of the baby. She also takes prescription medications or herbs to development of glandular cells that make milk (e.g. domperidone or morgina as prolactin-stimulating agents). When mom stops contraceptive, she begins pumping every three hours with no more than a five hour break at night.
When patients present to me shortly before the birth of the baby, I discuss realistic expectations as well as the effect of sleep deprivation on maternal mental health. Each individual patient discussion is different regarding risks/benefits of inducing lactation.
Mood and Anxiety in Pregnancy

Aside from very few older generation mood stabilizing and seizure medications, the vast majority of medication for mood and anxiety disorders are safe to continue during pregnancy. In fact, reproductive psychiatrists and the Postpartum Support International recommend that women do not discontinue medication during pregnancy. Untreated perinatal mood and anxiety disorders (PMADs) are associated with pre-term birth, intrauterine growth restriction (IUGR) and low birth weight (LBW).
If you’re experiencing increasing insomnia or symptoms of anxiety and depression during pregnancy, you should speak with your healthcare provider to discuss therapy and/or pharmacologic intervention. When the baby arrives and sleep deprivation becomes significant, mood and anxiety disorders will only worsen. Patients with well-controlled mood and anxiety disorders have higher initiation and continuation of breastfeeding.
If you have a trauma or assault history, the entire experience of pregnancy and/or birth can be triggering for reactivation of memories. It is important to work with a therapist during this time, as well as inform your medical care team of your history and concerns.

