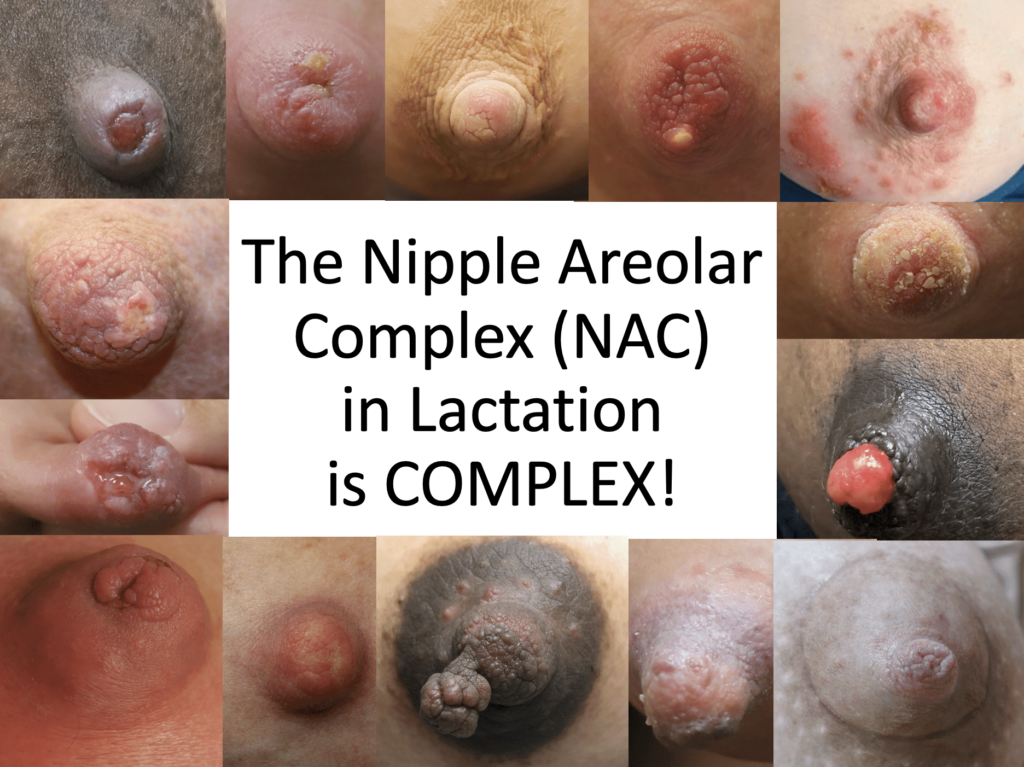
A full review of all maternal breast conditions in lactation is available with the new edition of Breastfeeding for Medical Professionals (Lawrence and Lawrence) textbook. We also review the management of common complications in Obstetrics and Gynecology Clinics.
Adenoma
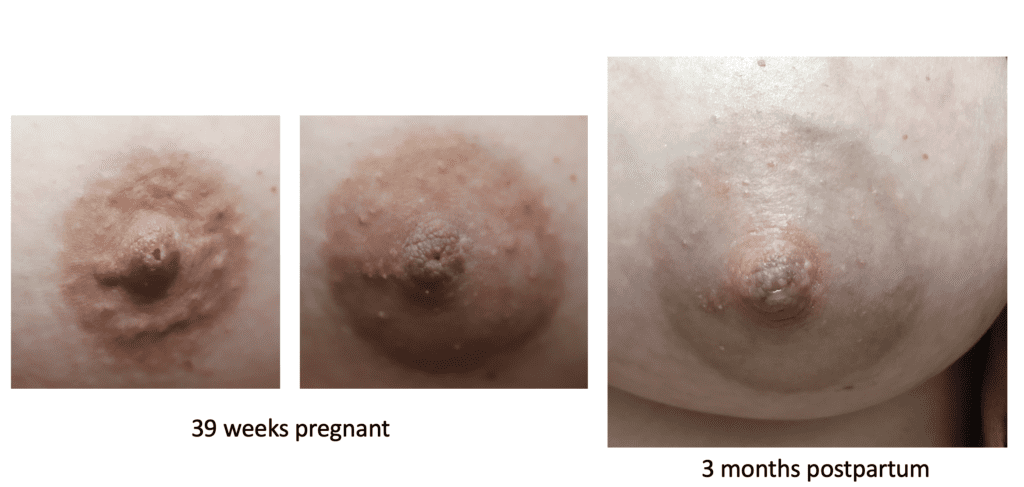
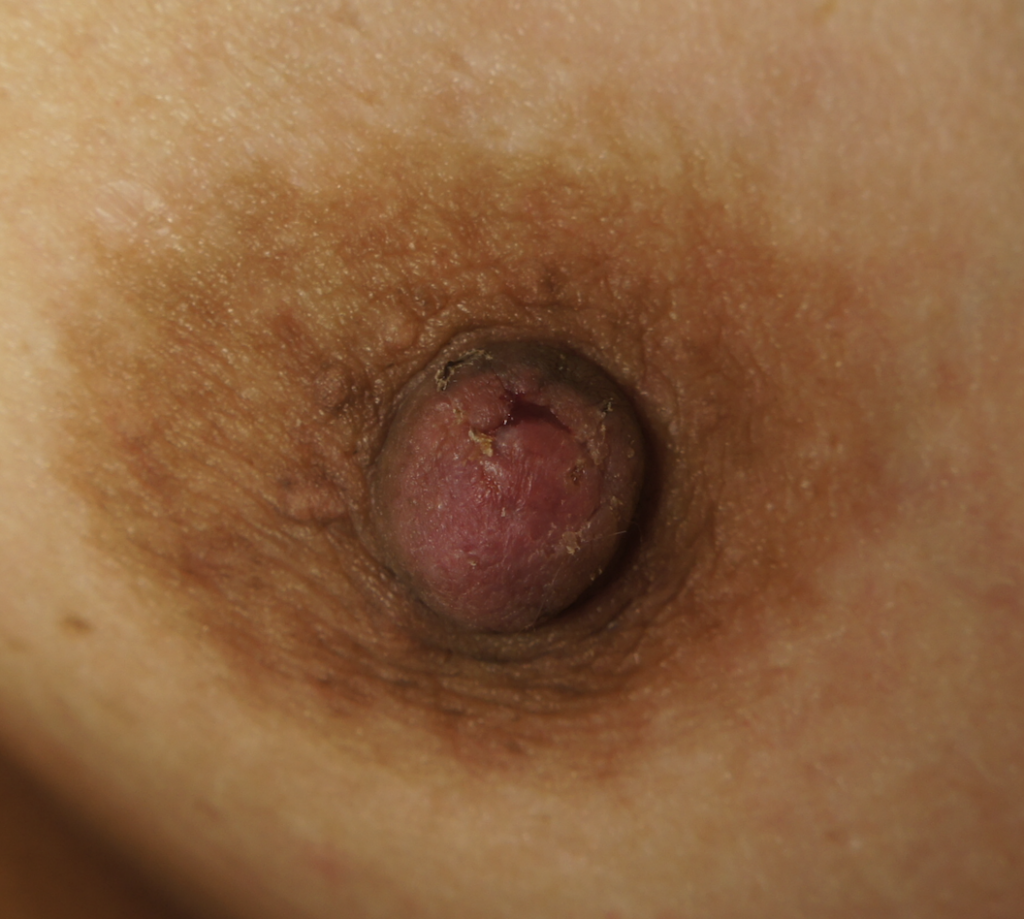
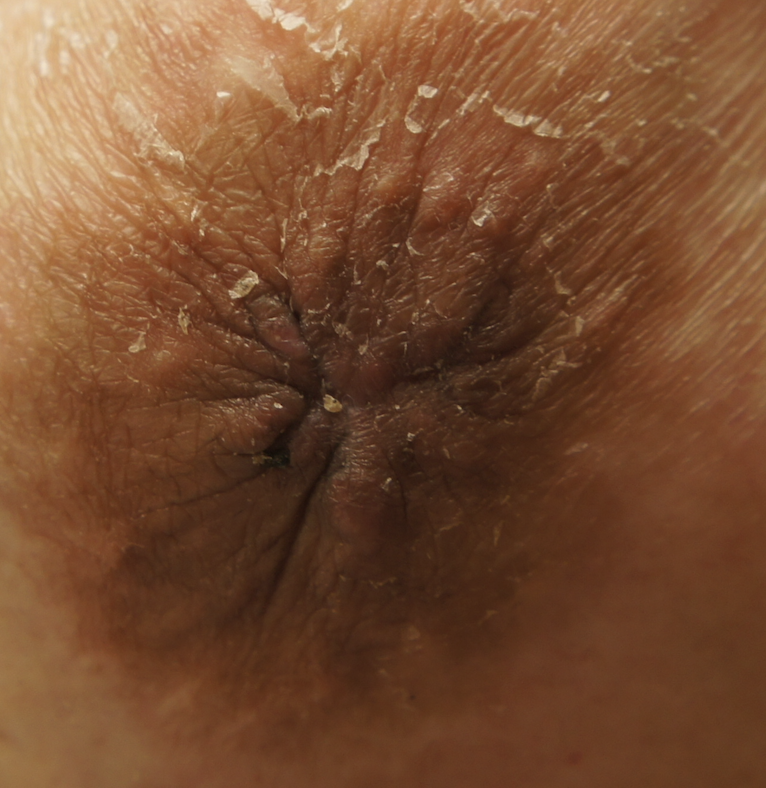
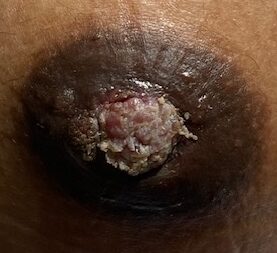
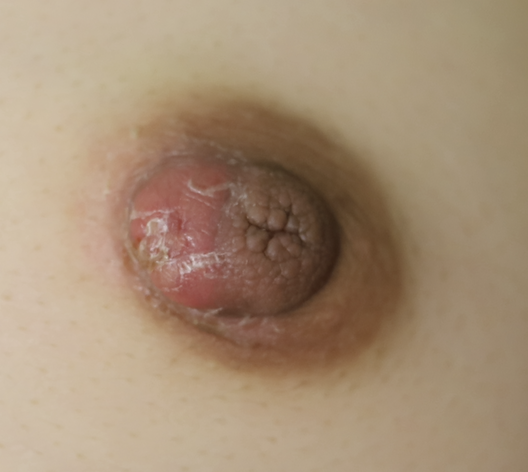
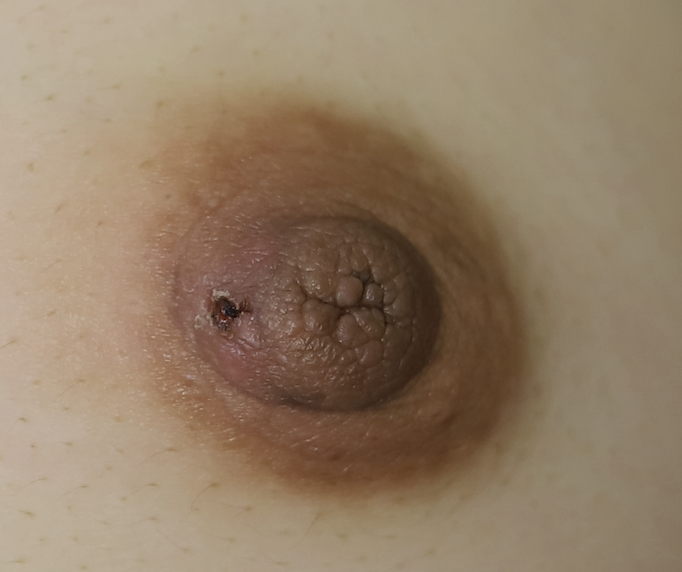
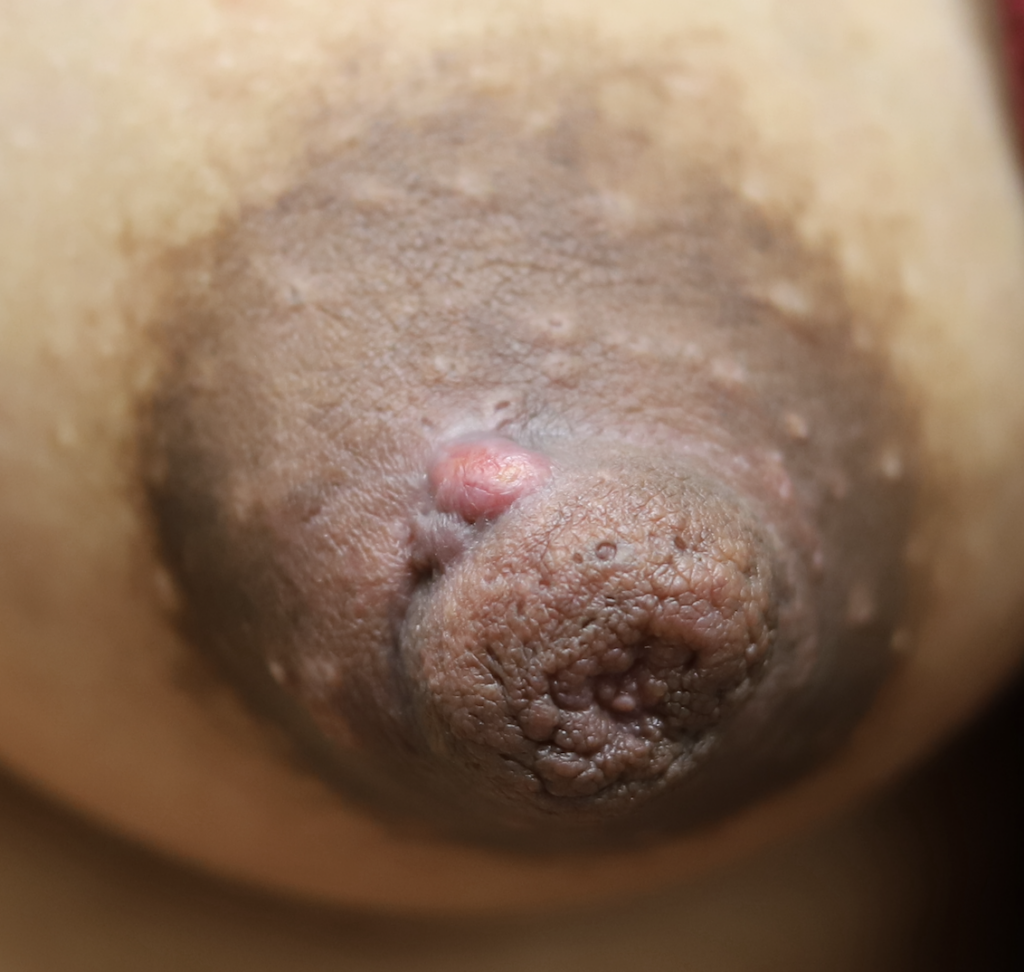
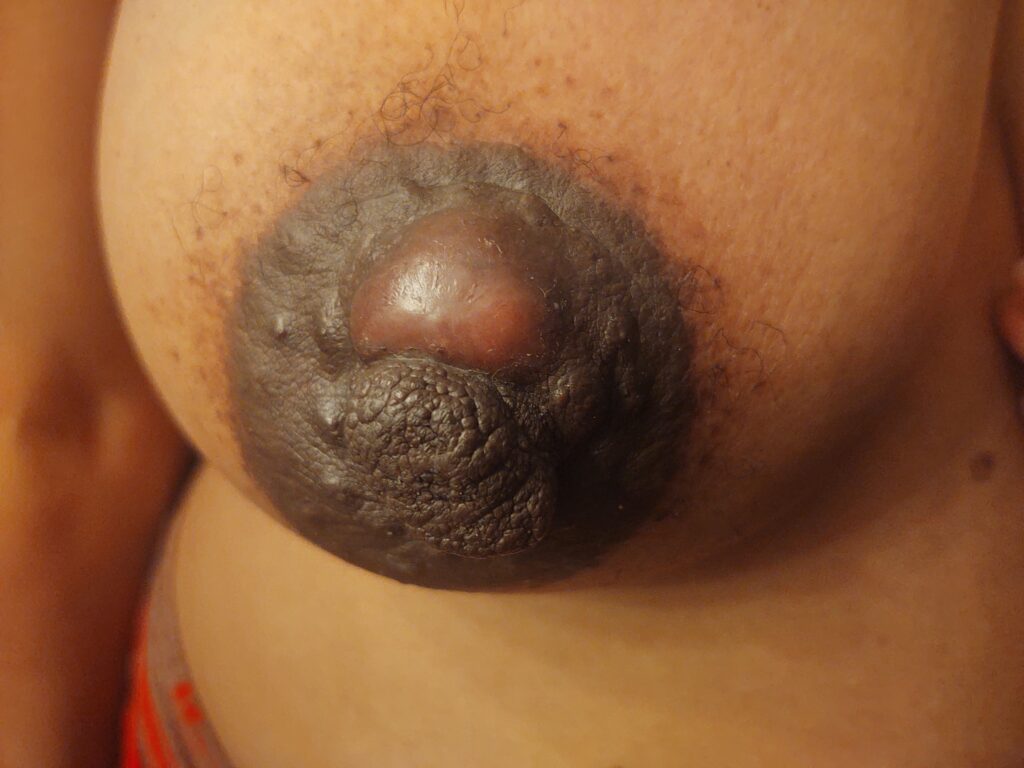
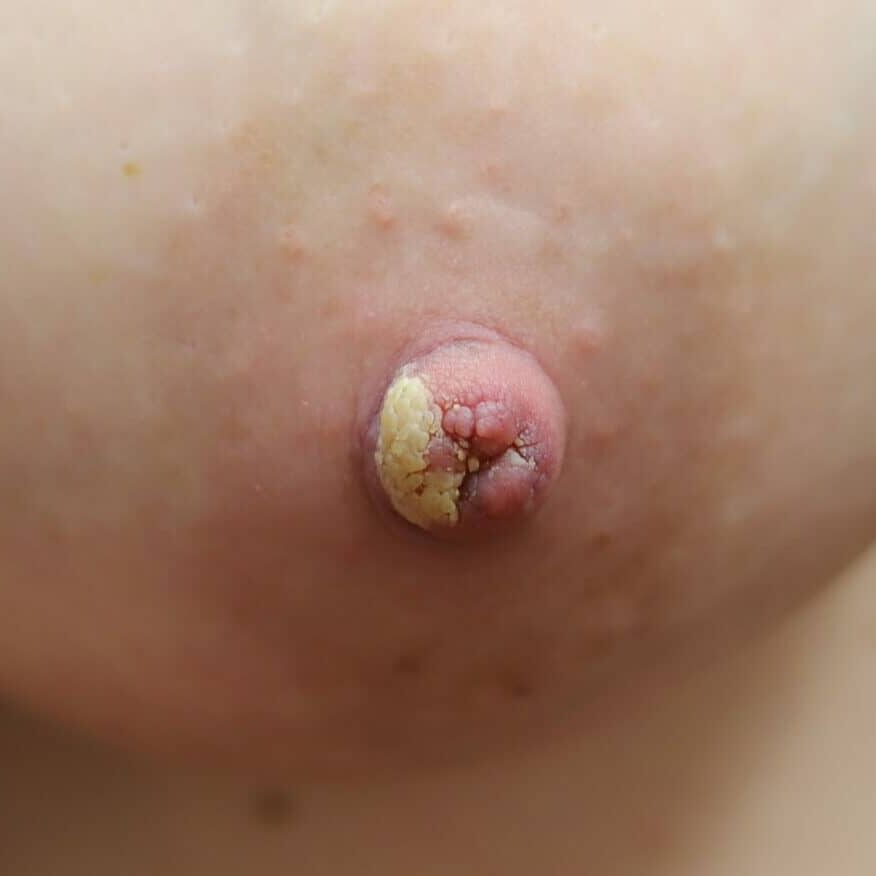
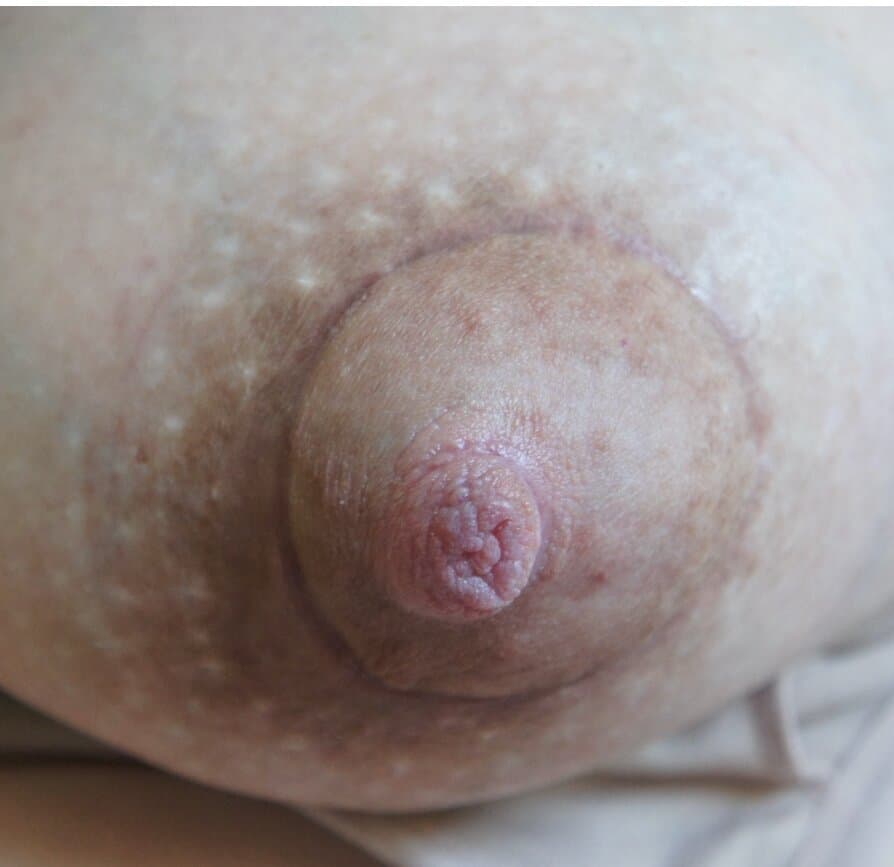
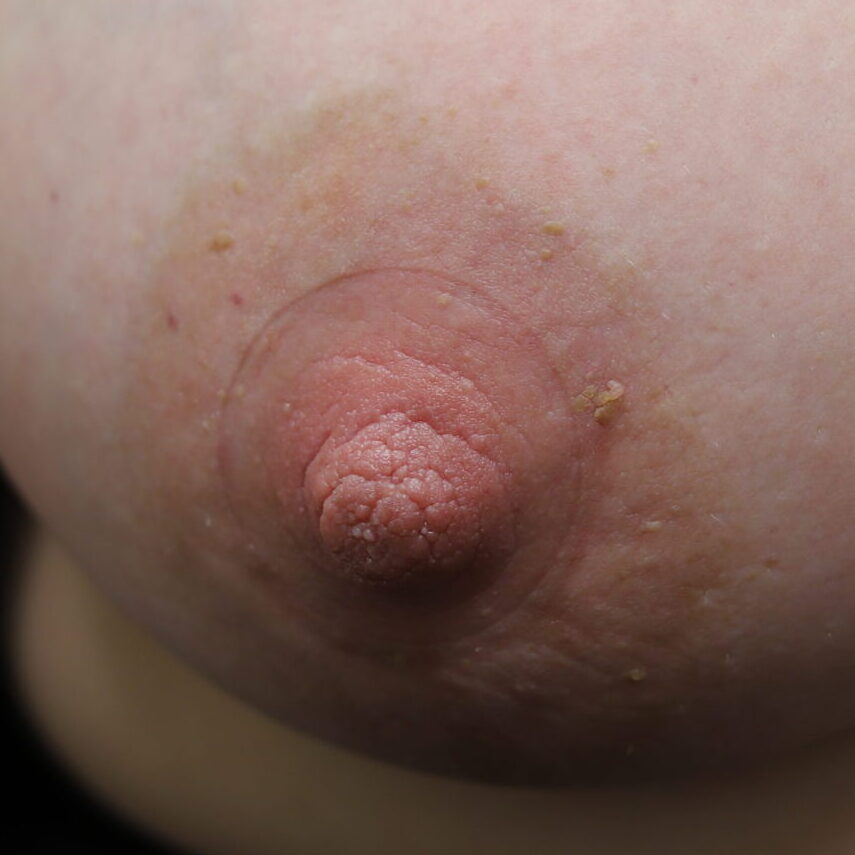
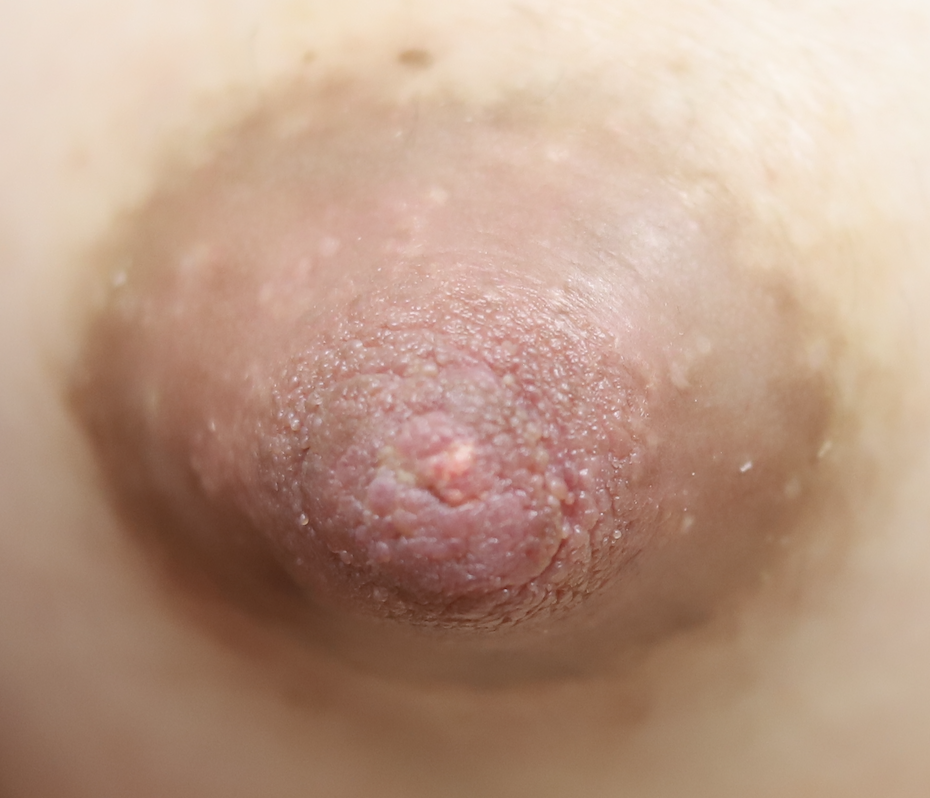
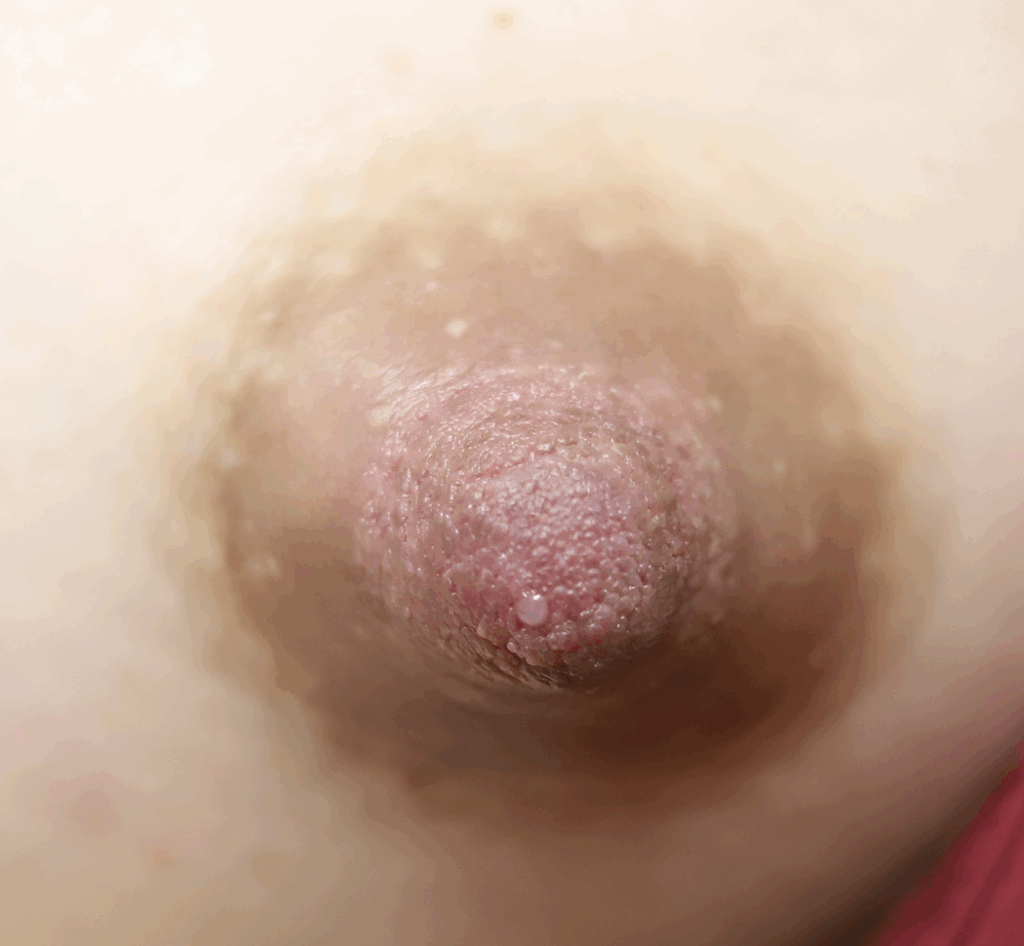
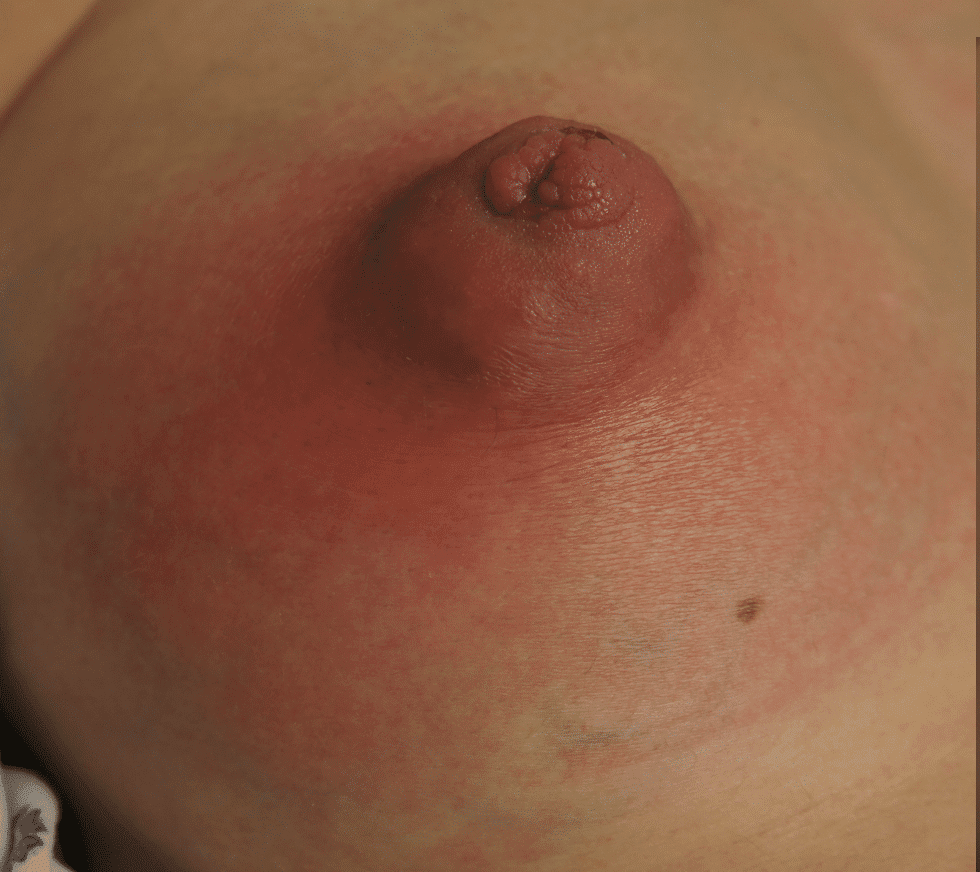
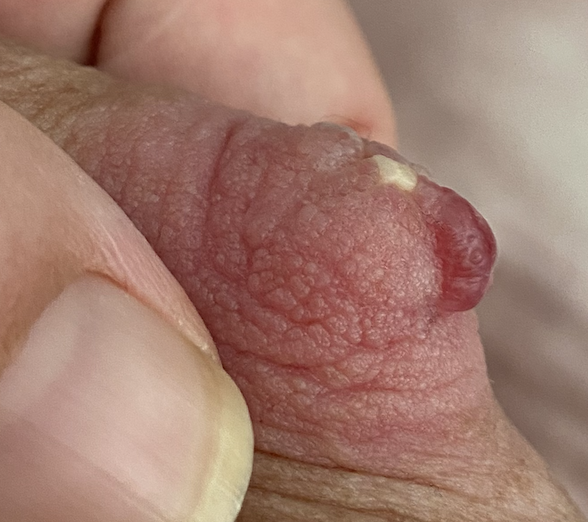
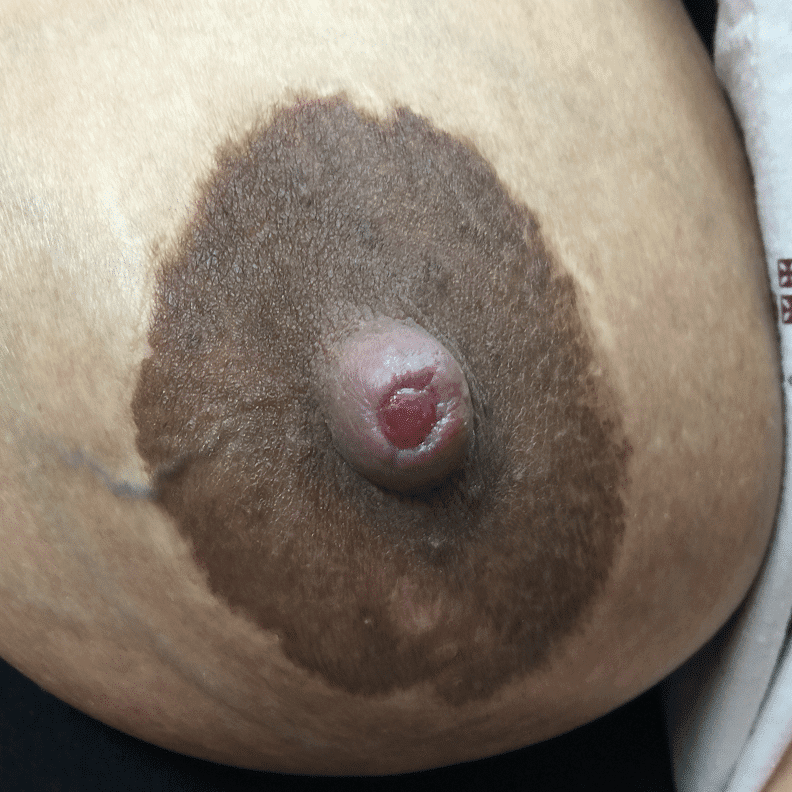
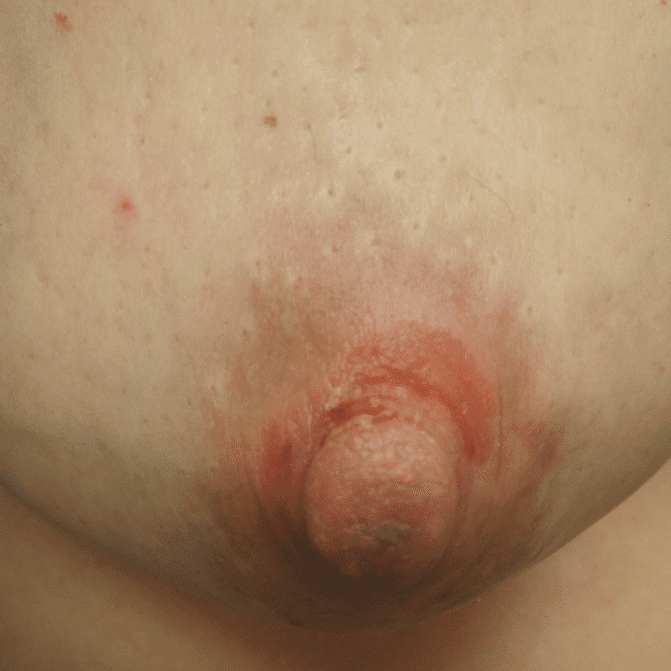
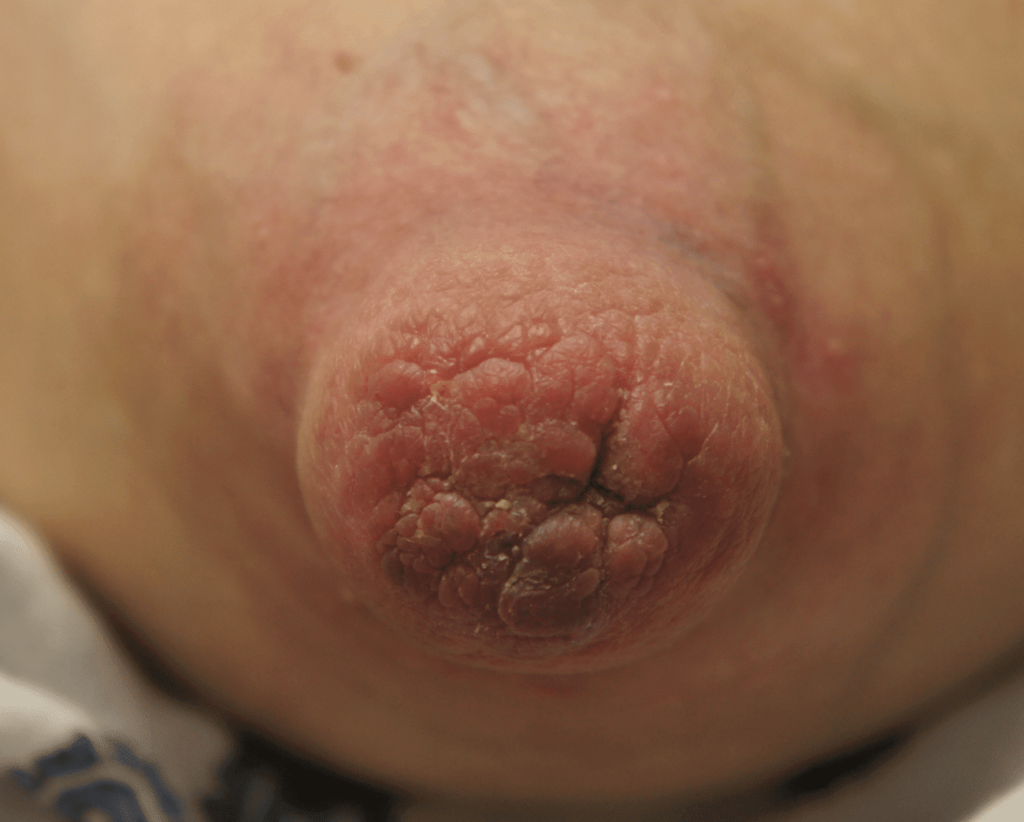
Nipple adenoma, also known as erosive adenomatosis of the nipple (EAN) or nipple papillomatosis, is characterized by nipple nodularity and can progress to erosion. It generally is a benign lesion not associated with atypical cells or cancer. Any nipple disorders not resolving with proper intervention should be referred for further evaluation with a breast surgeon. Biopsy is often performed to confirm diagnosis and treatment generally consists of excision, which may be able to be deferred if the lesion is not interfering with breastfeeding.

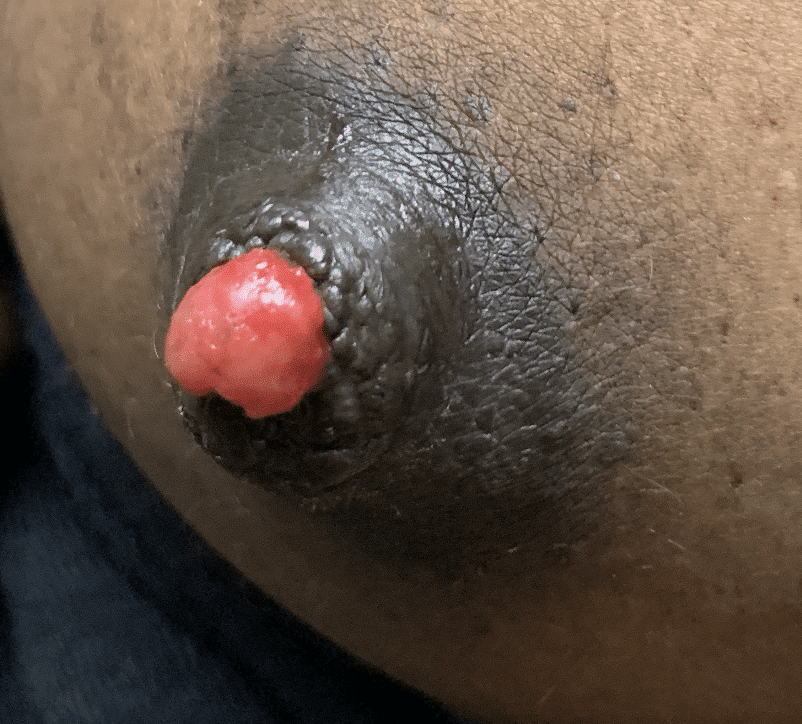
Blebs

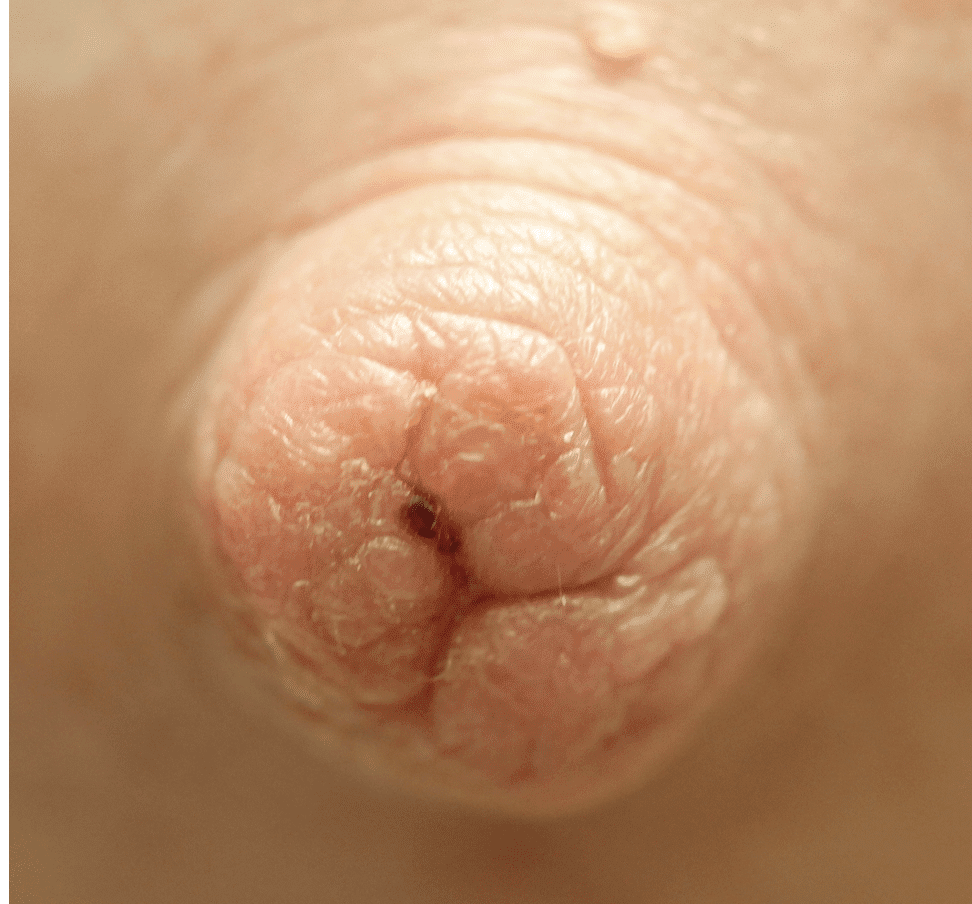
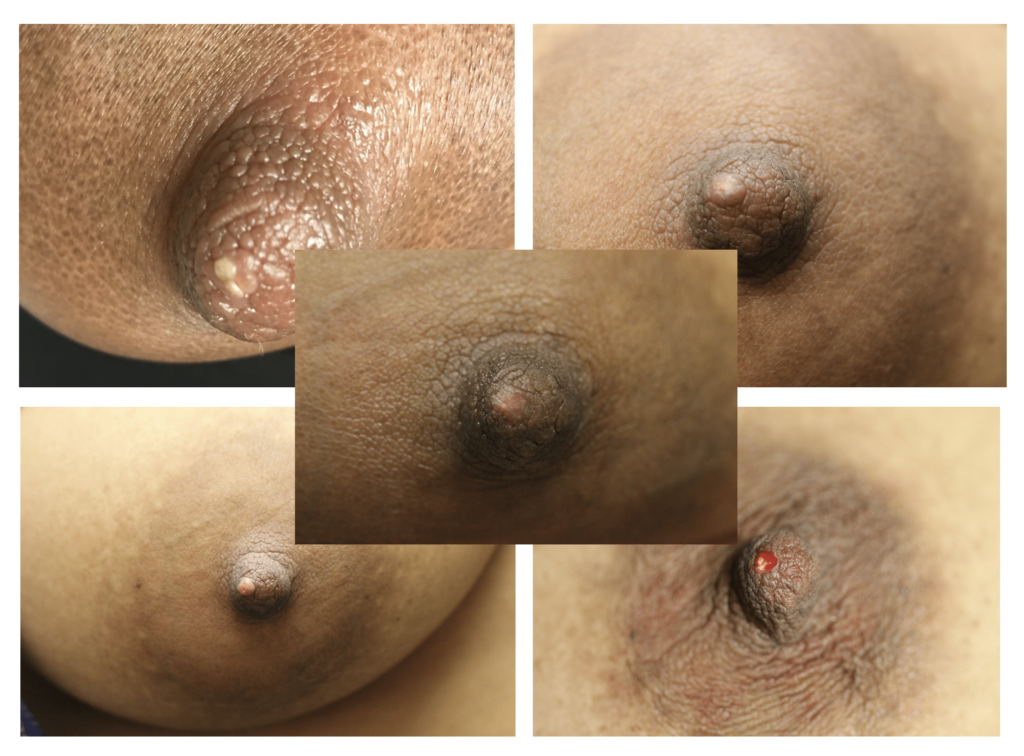
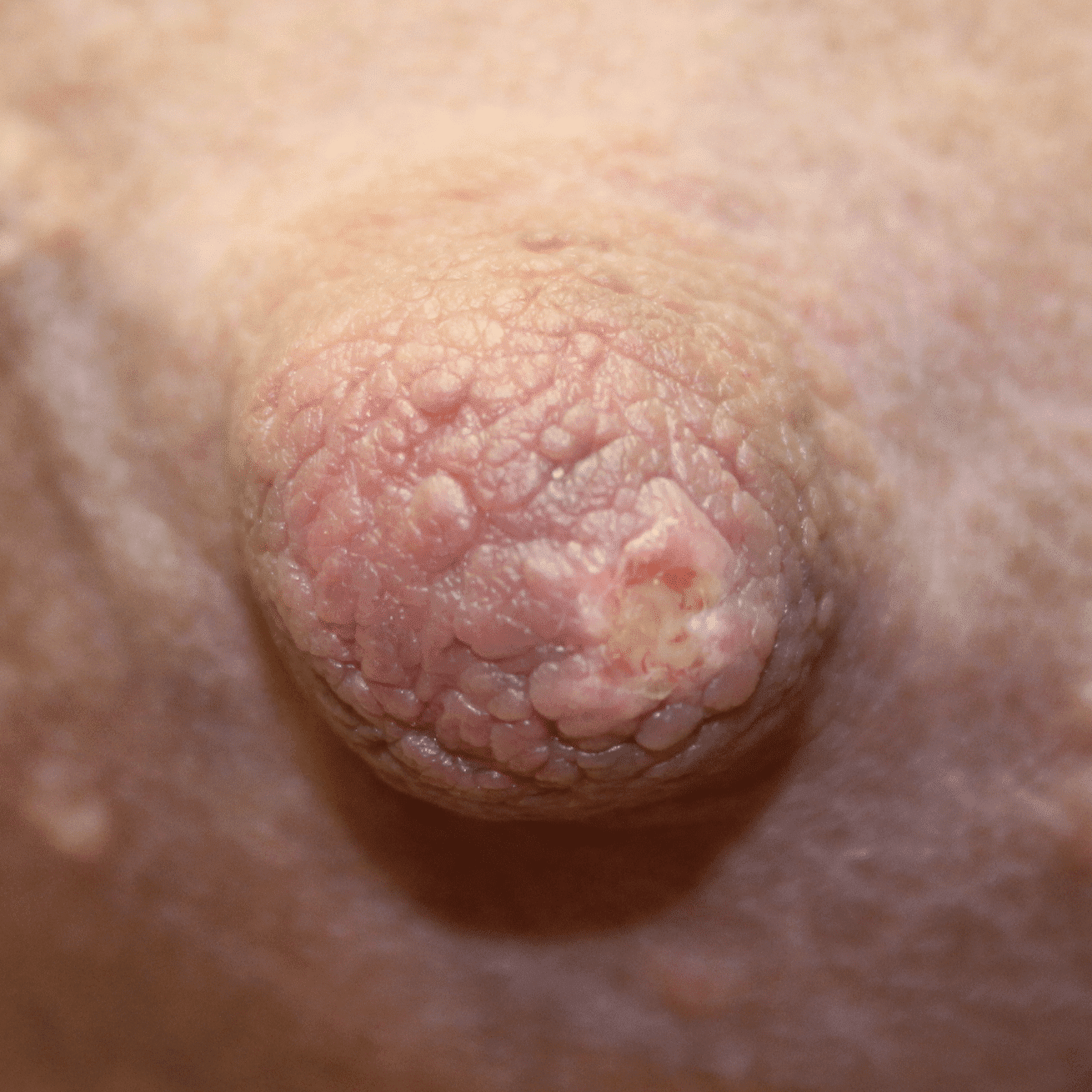
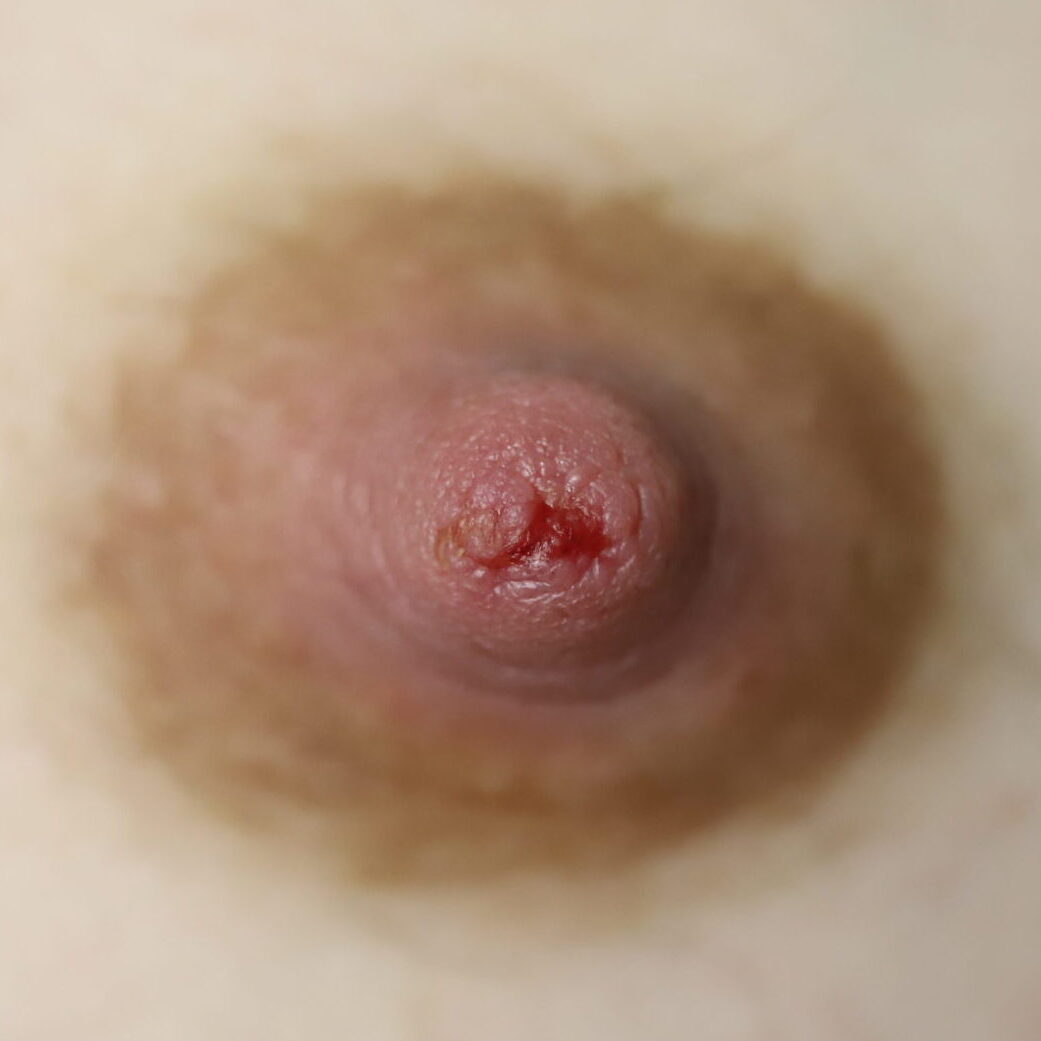
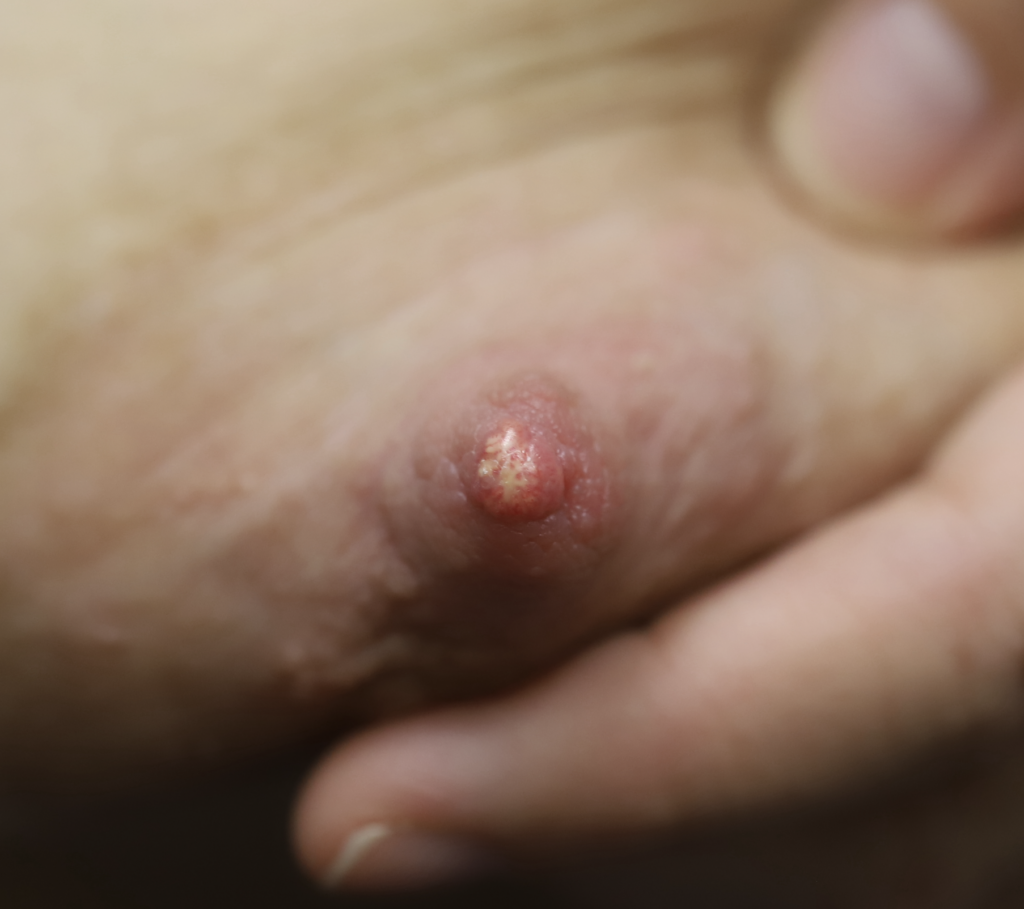

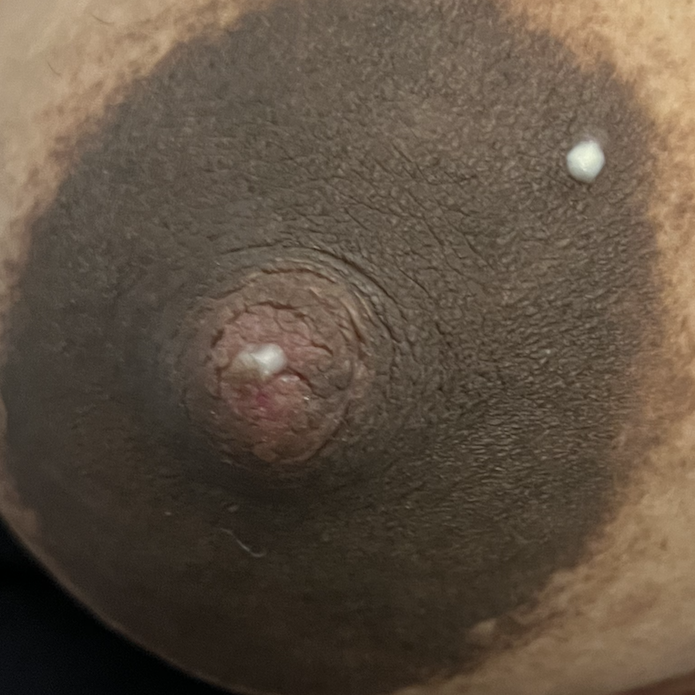
Often described as a “white dot” or a “scab,” nipple blebs are lesions on the surface of a single or multiple nipple orifices that reflect underlying ductal inflammation. They can cause exquisite pain when the baby breastfeeds. They also can cause obstruction of milk flow through the nipple orifice. Blebs have no association with candida (yeast), but are associated with hyperlactation, exclusive pumping, and localized breast tissue swelling. Some appear and regress and new ones reappear. Other patients experience one persistent bleb in one location.
Juan Rodriguez’s lab in Spain has produced excellent illustrations of how debris narrows ducts — this debris has many different components: sloughing inflammatory cells, cholesterol, other lipids (fats), biofilms, and likely countless others.
Do NOT unroof with a sterile needle or by “popping” the bleb. This may cause temporary relief, but it will worsen inflammation and eventually cause chronic scarring. Infants may release a superficial bleb while nursing, or more tenacious blebs may persist regardless of interventions.
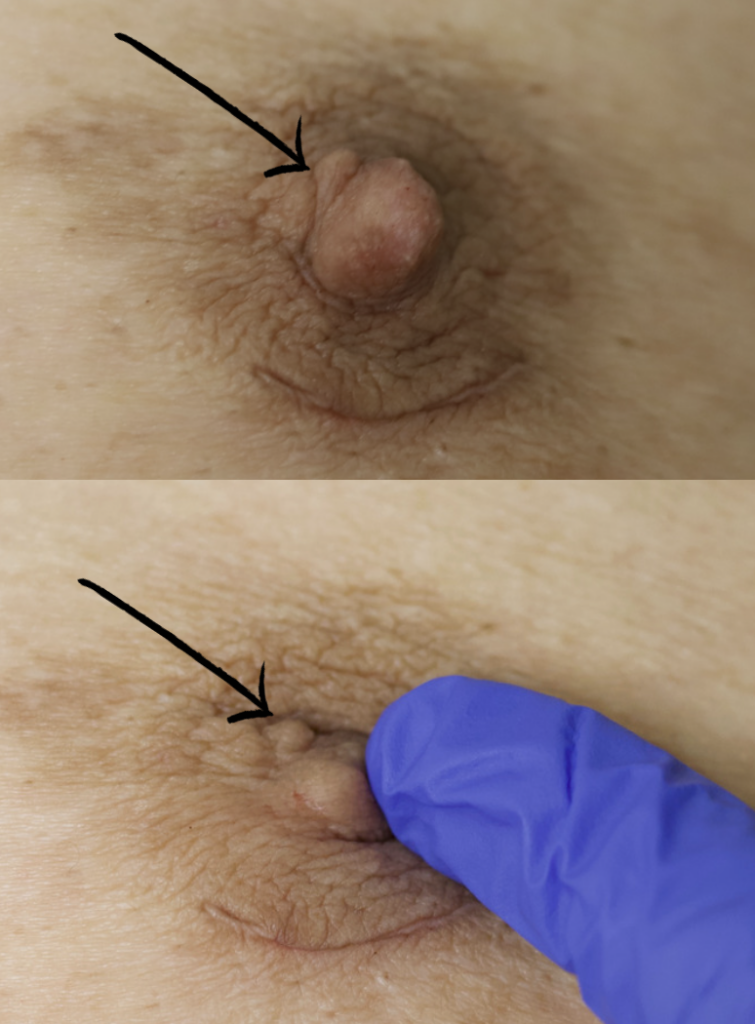
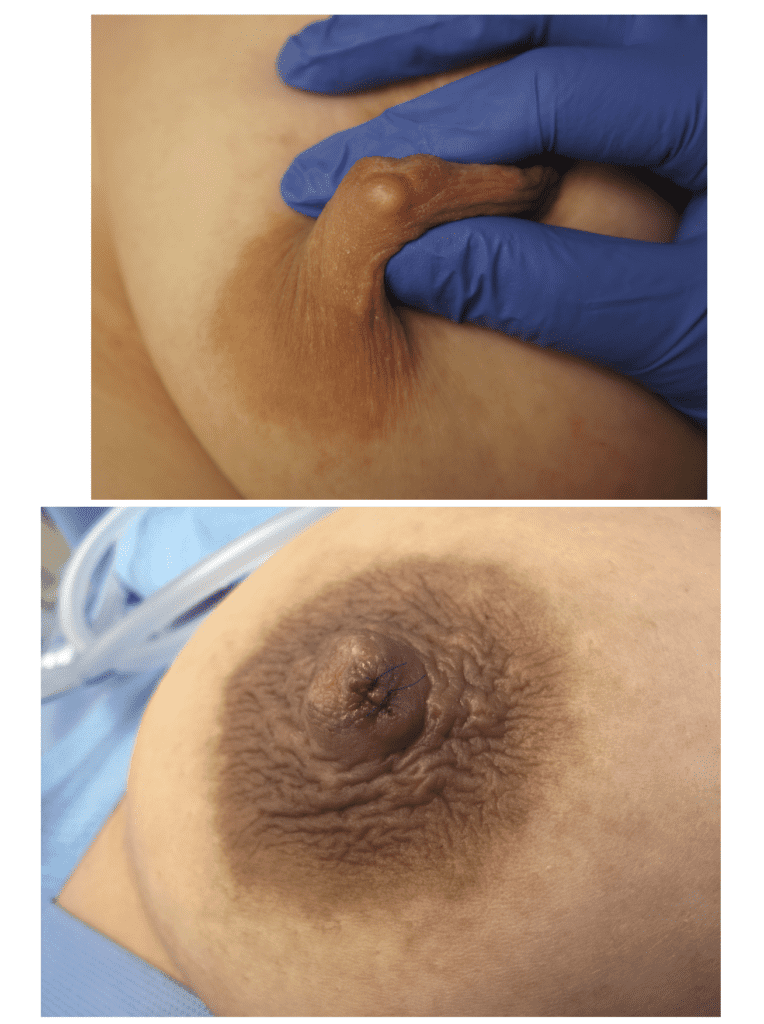
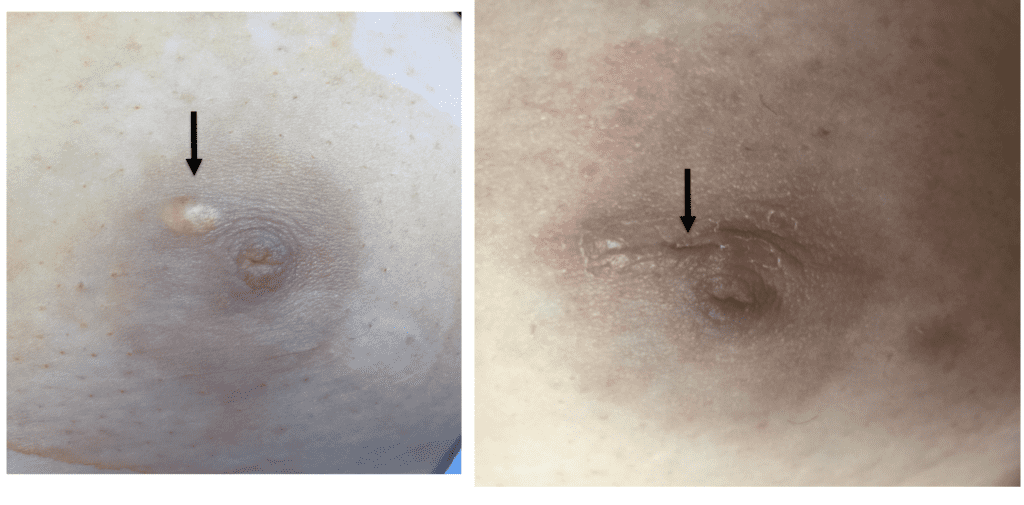
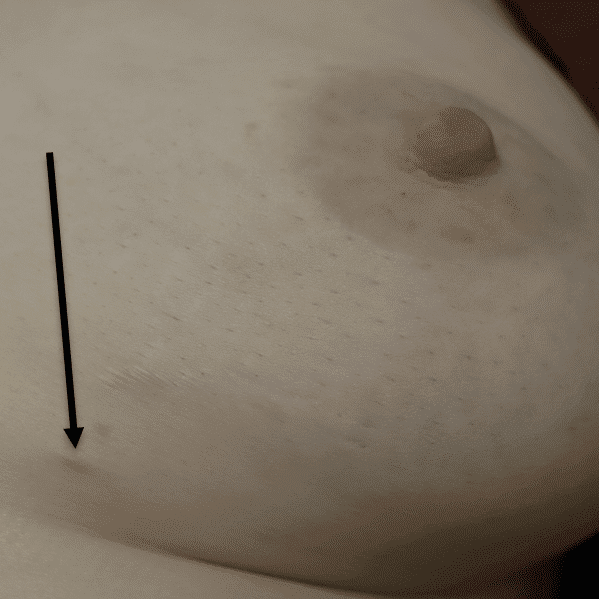
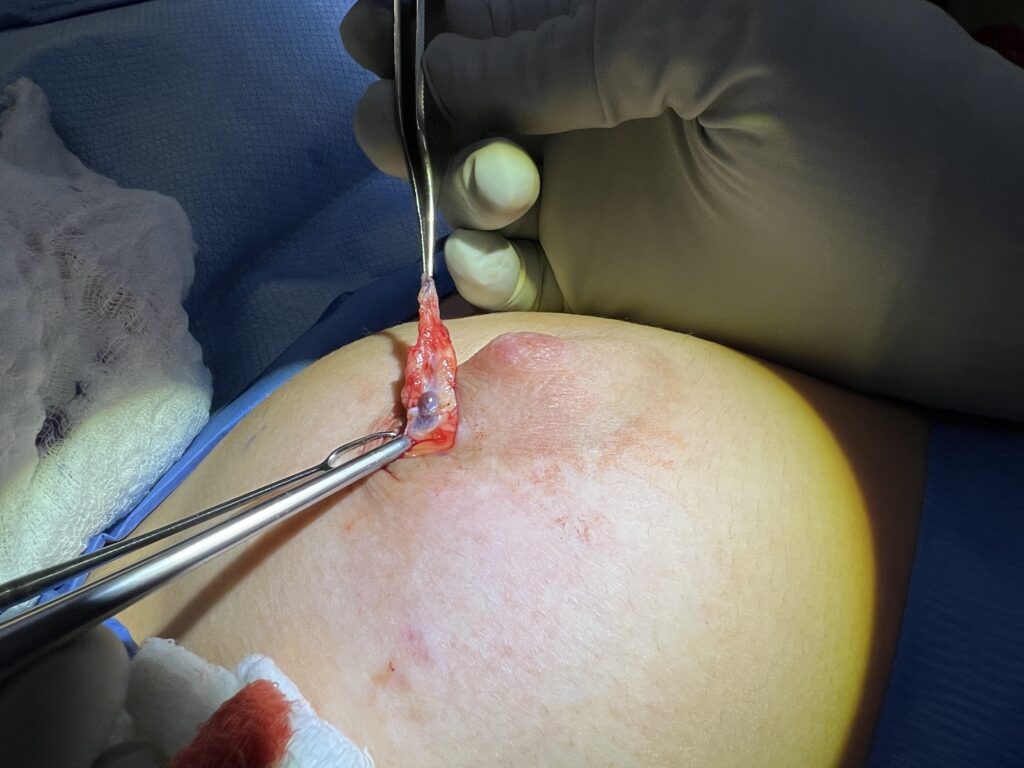
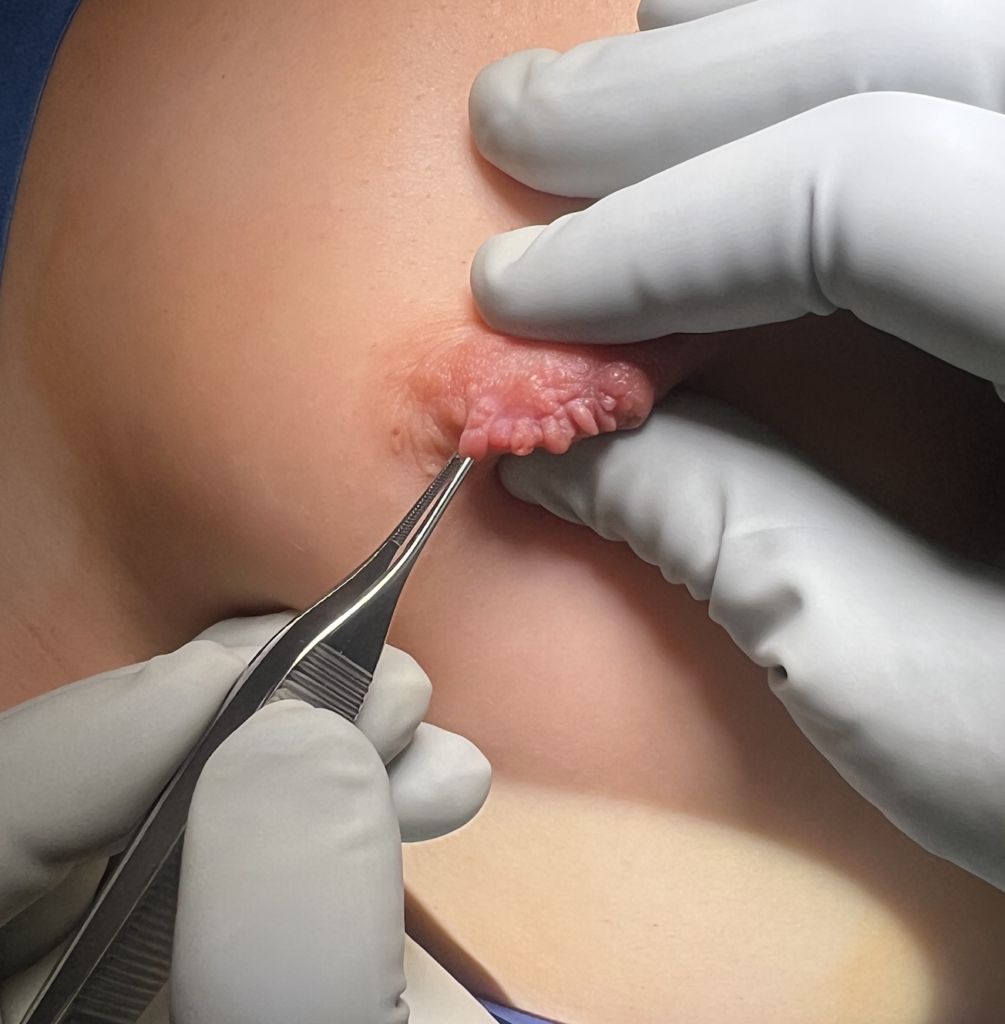
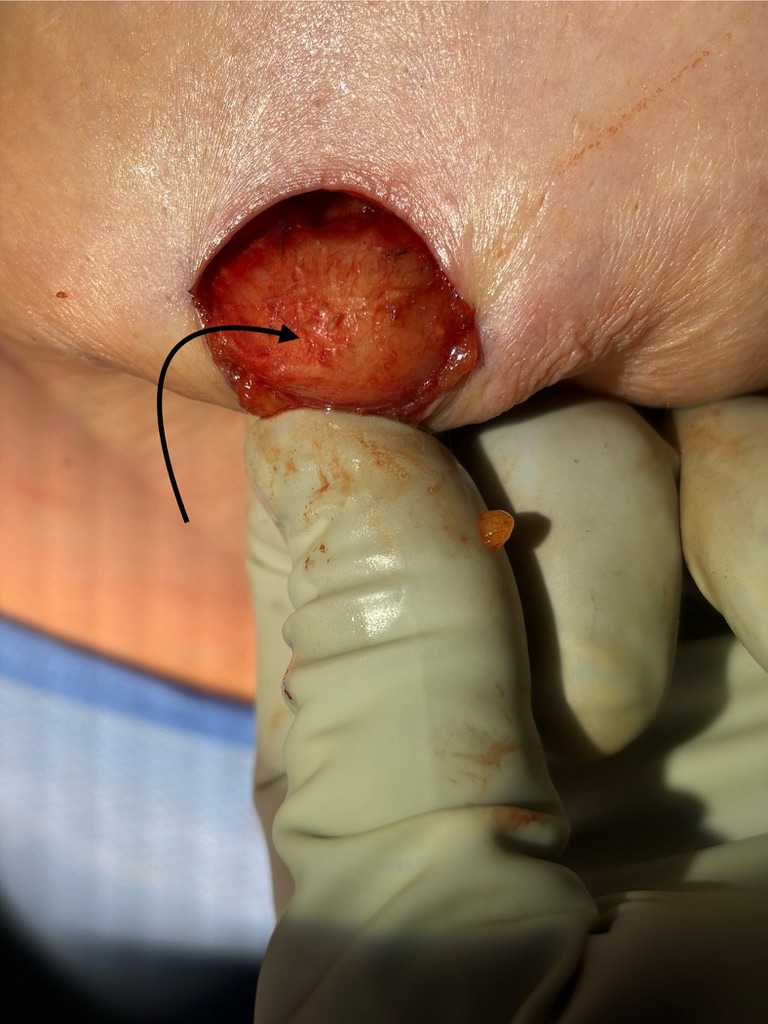 This is one of the reasons why you don’t want to attempt to squeeze or extract a bleb or “plug”: Even within the nipple (the largest convergence of ducts in the breast), the ducts are extraordinarily small and delicate (the arrow is pointing out the biggest ones visible with naked eye when I am in the OR inverting a nipple from the outside). If you try to squeeze these, all it will do is damage ductal tissue, cause bleeding, and cause a lot of pain and ultimately scarring.
This is one of the reasons why you don’t want to attempt to squeeze or extract a bleb or “plug”: Even within the nipple (the largest convergence of ducts in the breast), the ducts are extraordinarily small and delicate (the arrow is pointing out the biggest ones visible with naked eye when I am in the OR inverting a nipple from the outside). If you try to squeeze these, all it will do is damage ductal tissue, cause bleeding, and cause a lot of pain and ultimately scarring.
Blebs are not related to surface trauma or infant latch. Infants may pull off the breast in the setting of oversupply, and patients assume this caused the bleb. Instead, it’s the oversupply that causes the ductal inflammation that causes the bleb. And the infant is simply pulling off the breast because of being choked by high flow in high supply. Other infants may pull at the breast due to distraction or frustration with lower flow. Though less common, blebs are possible with low supply in the setting of subacute mastitis.
Appropriate treatment includes utilization of 0.1% triamcinolone crème (over the counter products such as hydrocortisone are not potent enough to be effective) on the surface of the nipple to reduce inflammation. Sunflower lecithin by mouth reduces underlying ductal congestion and inflammation. Therapeutic ultrasound is also helpful. Underlying hyperlactation also must be treated.
It should be noted that blebs are different from the sucking blister that appears early in lactation and results from vigorous suckling, malposition, or high pump suction. This type of blister covers a larger area, appears more blister-like with a thin membrane and underlying fluid, and is not associated with underlying associated conditions as described above.
Bloody Milk
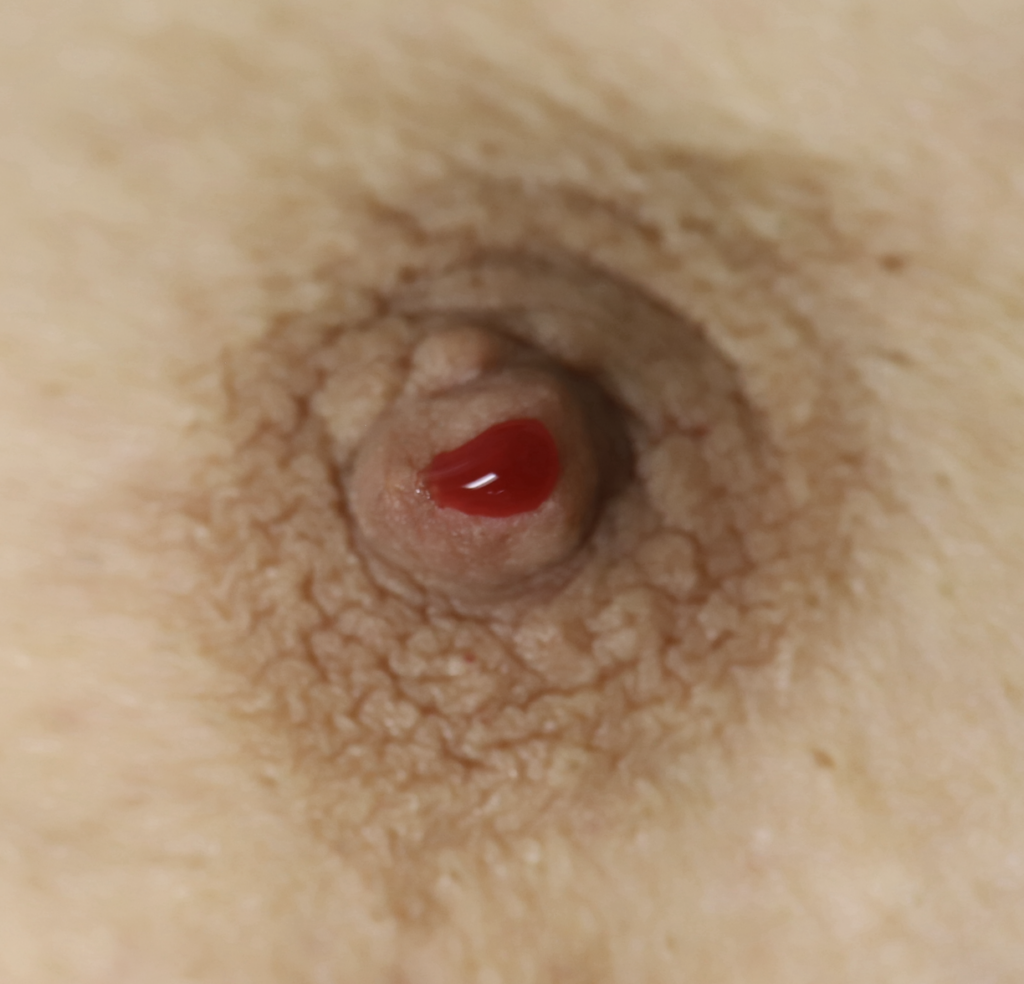
Bloody nipple discharge may occur in up to 20 percent of women in the pregnant and early postpartum period. It is related to breast growth, increased blood flow, and preparation of the breast to make milk. It generally occurs in both breasts and from several nipple orifices, and will worsen with nipple stimulation. If you have any concern, you should seek evaluation by your healthcare provider. More concerning discharge is from one breast and one nipple orifice.
Mothers with hyperlactation, exclusively pumping, doing lots of massage or compressions of the breast, or those taking blood thinning medications may also experience transient bloody milk. These cases should be evaluated carefully with history and exam, and also may warrant imaging.



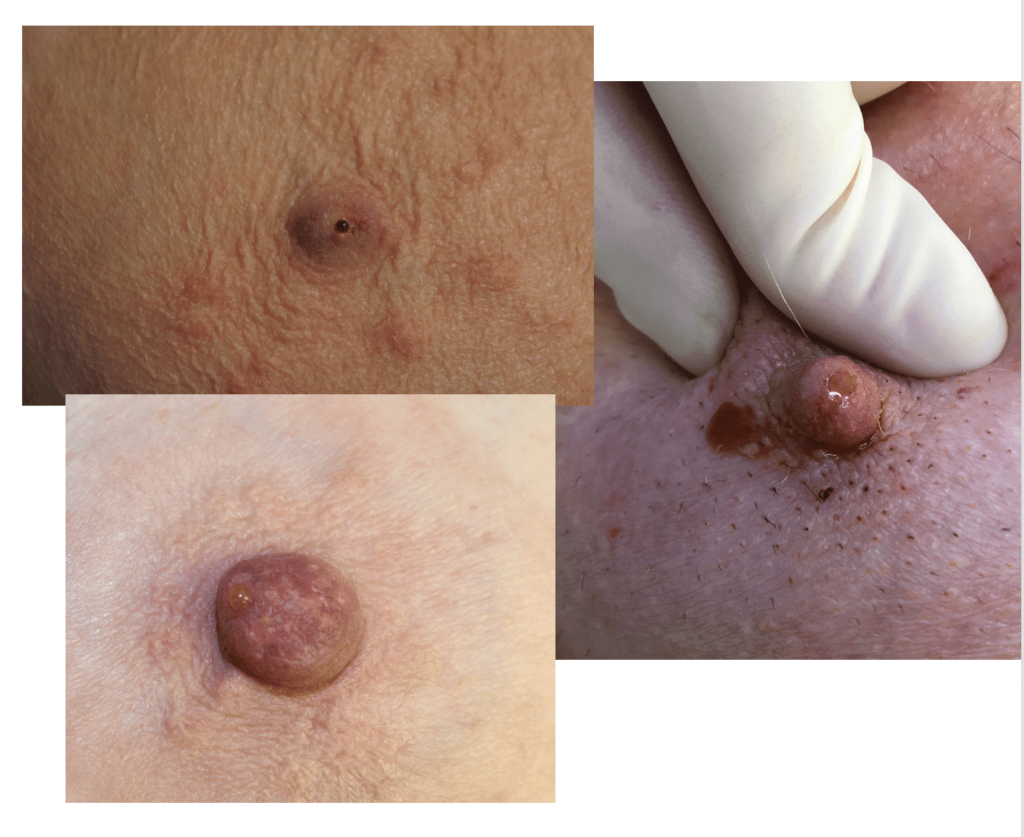
Cysts
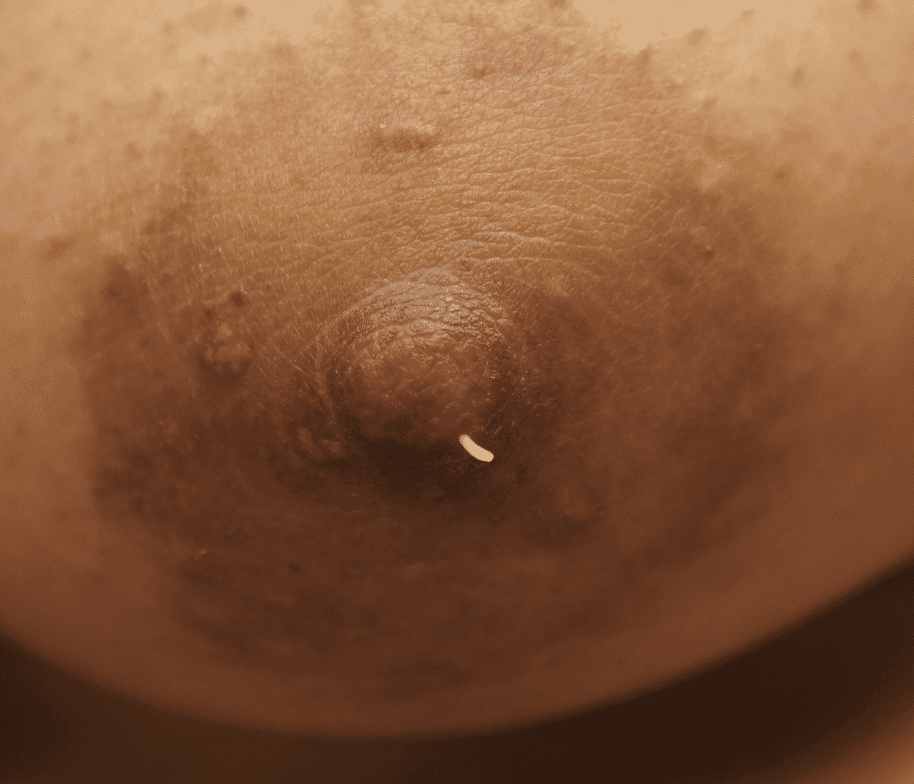
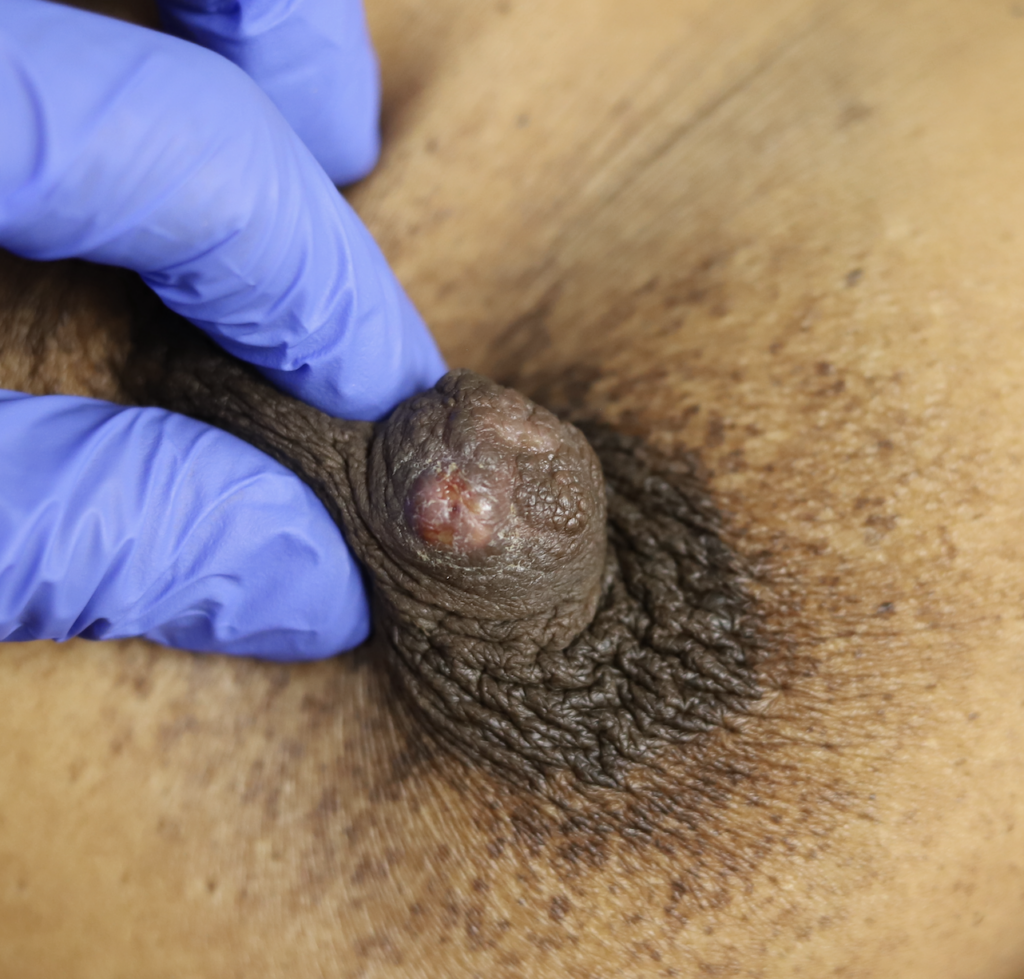
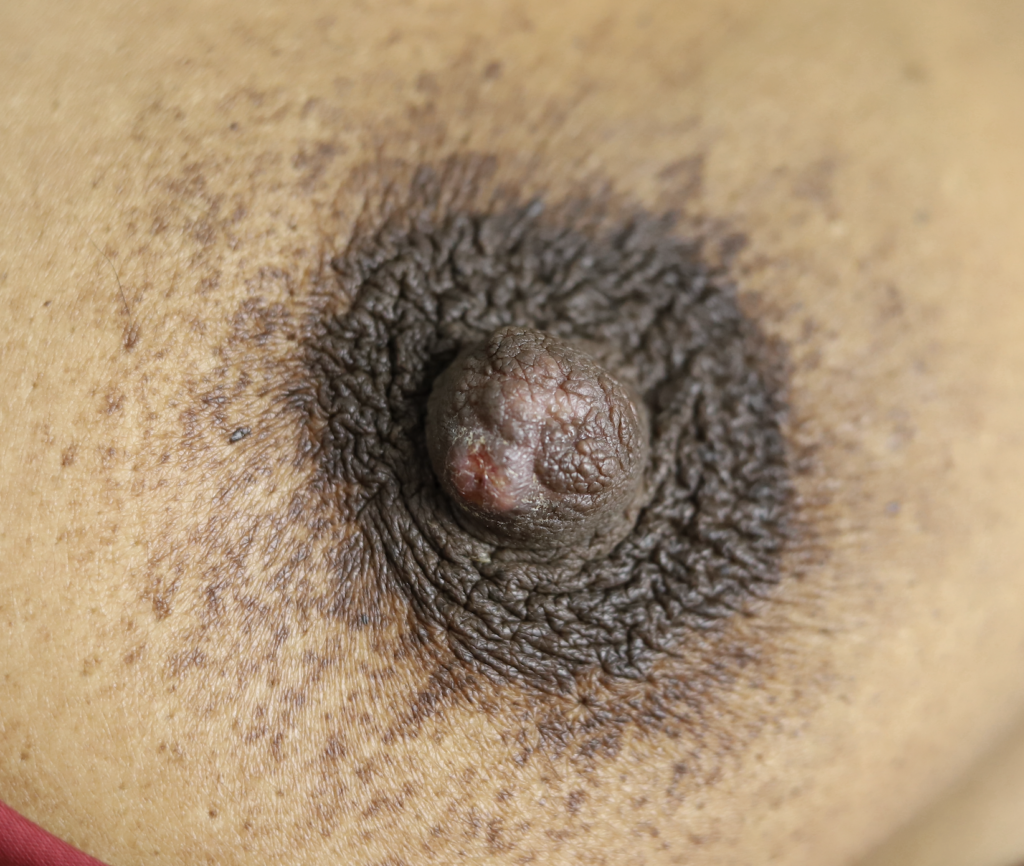
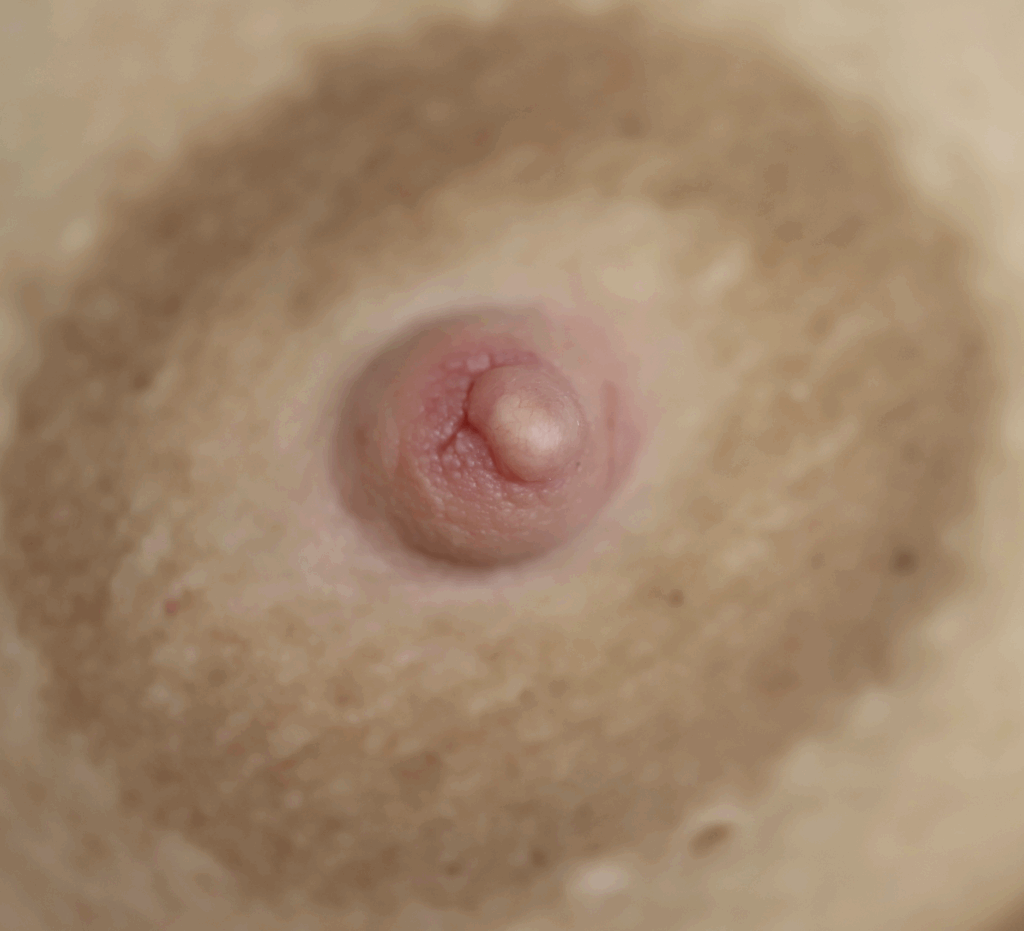
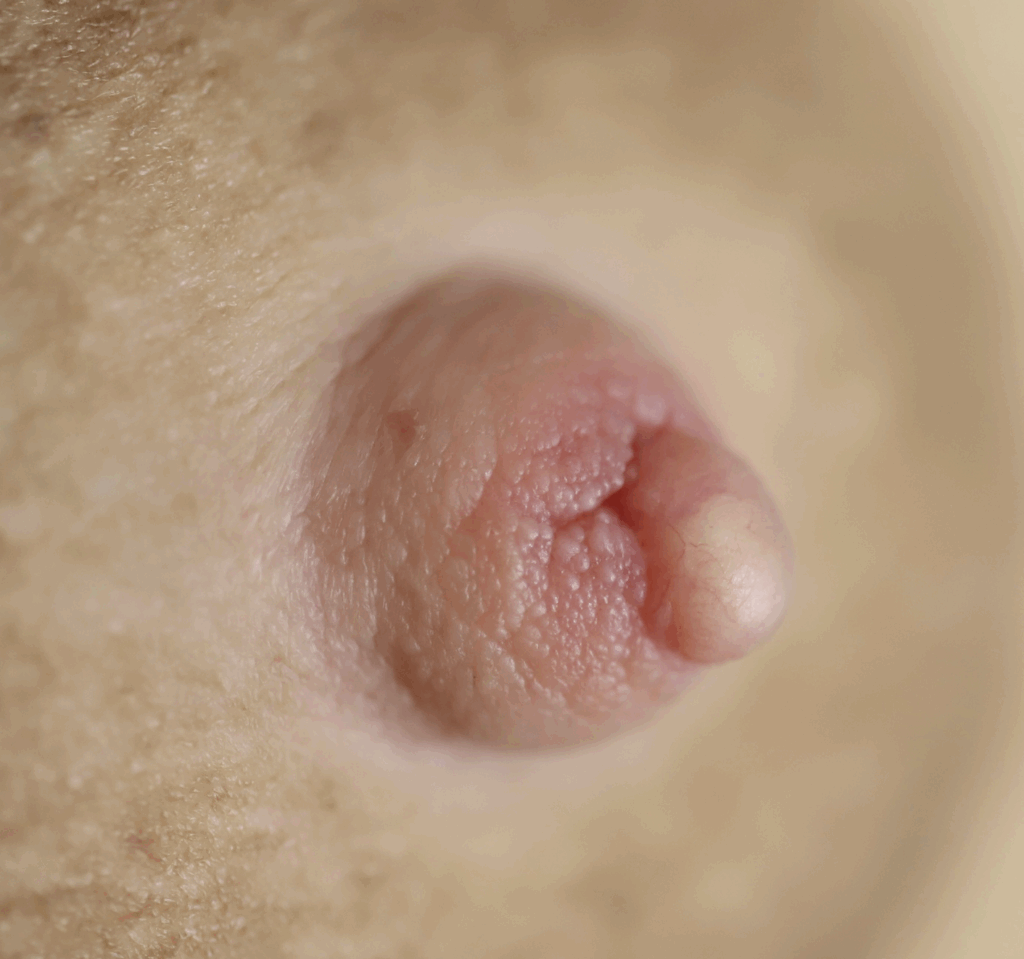
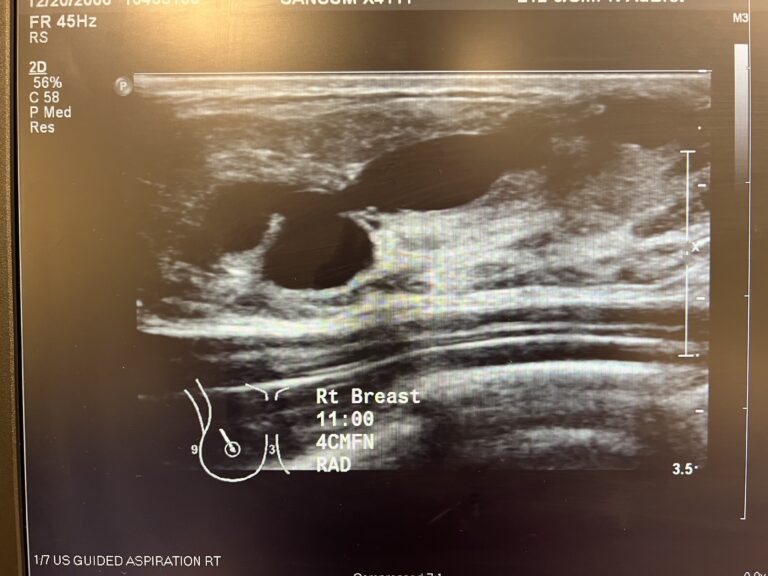
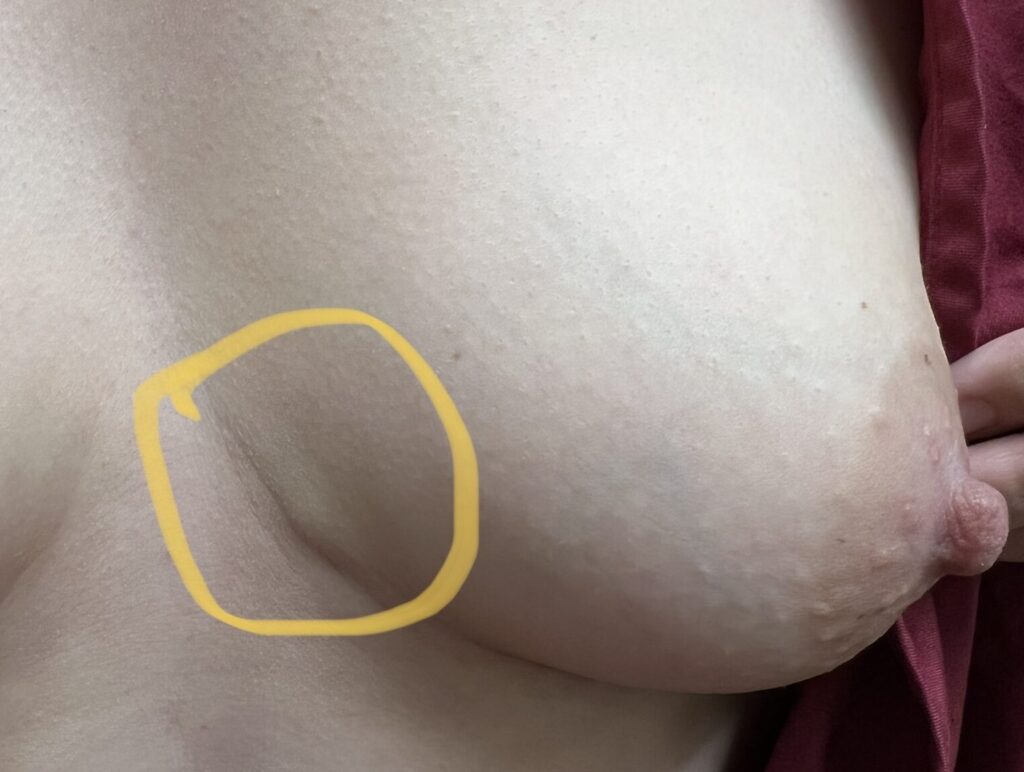
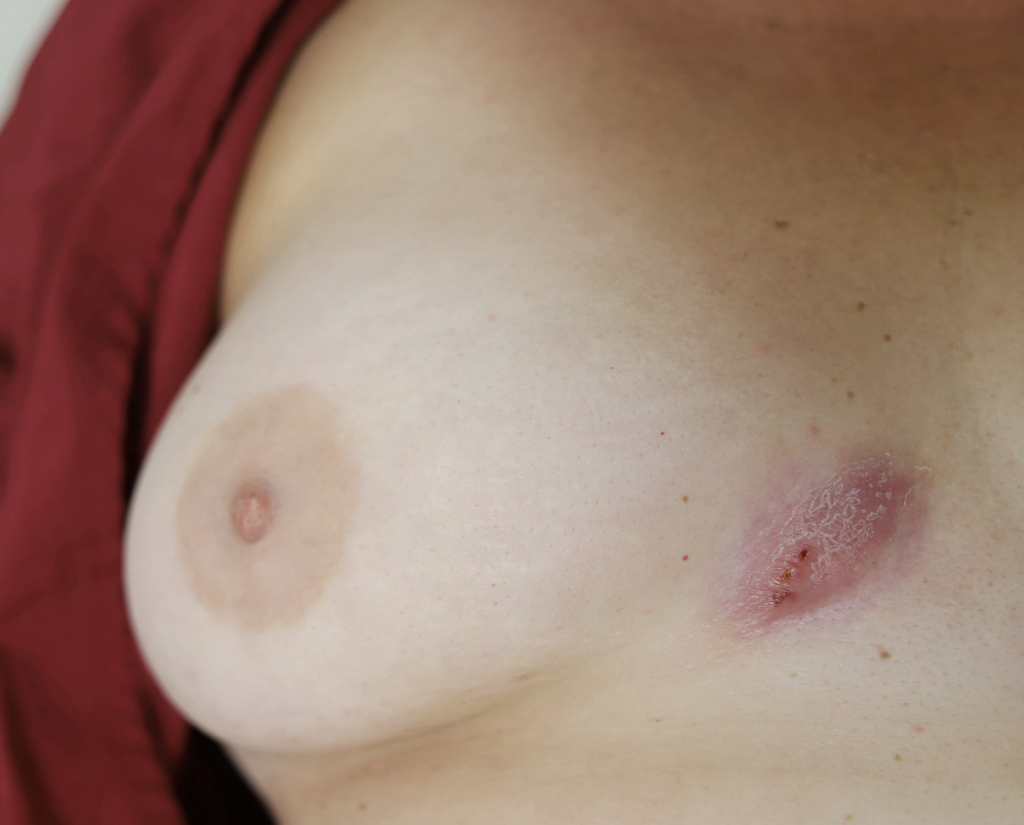
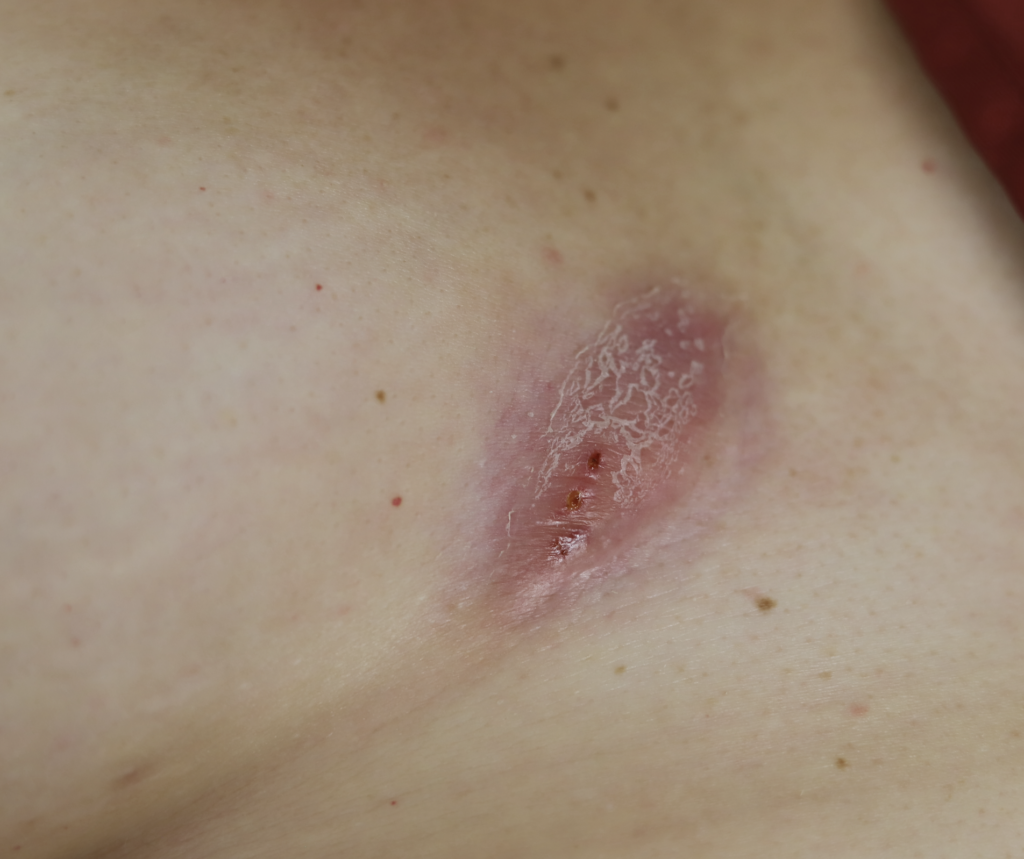
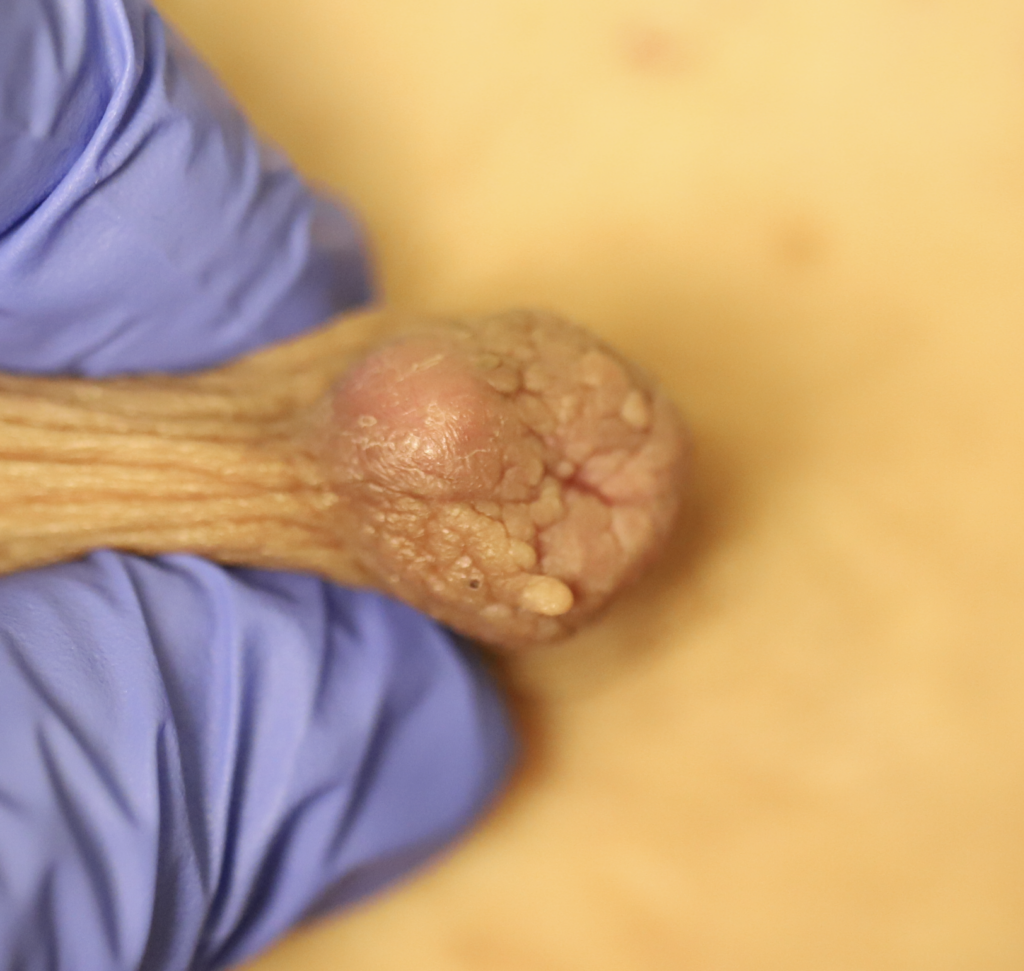
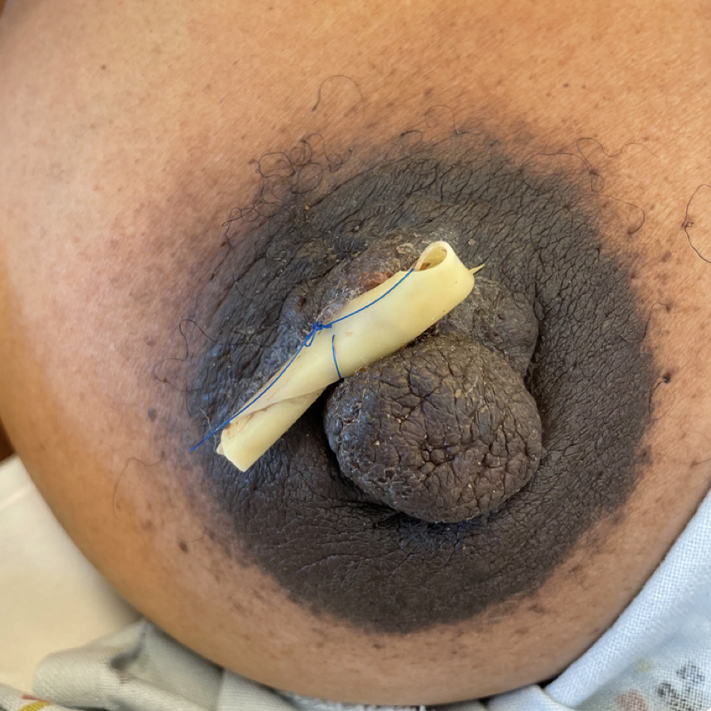
Sebaceous cysts and epidermal inclusion cysts (EICs) present most commonly on the nipple or areola. Nipple areolar dermal cysts can be repeatedly traumatized by a nursing infant and may become painful. If this occurs, warm compresses and/or antibiotics may be indicated. If diagnosed prenatally, surgical excision under local anesthesia may prevent future trauma, pain, and infection while breastfeeding. Given cysts are dermal (skin) lesions, excision should not affect underlying ductal tissue or nipple orifices, though attention should be given to careful placement of incision, closure, and suture type. Non-absorbable suture produces less tissue reaction and scarring and would be an ideal choice in this circumstance.

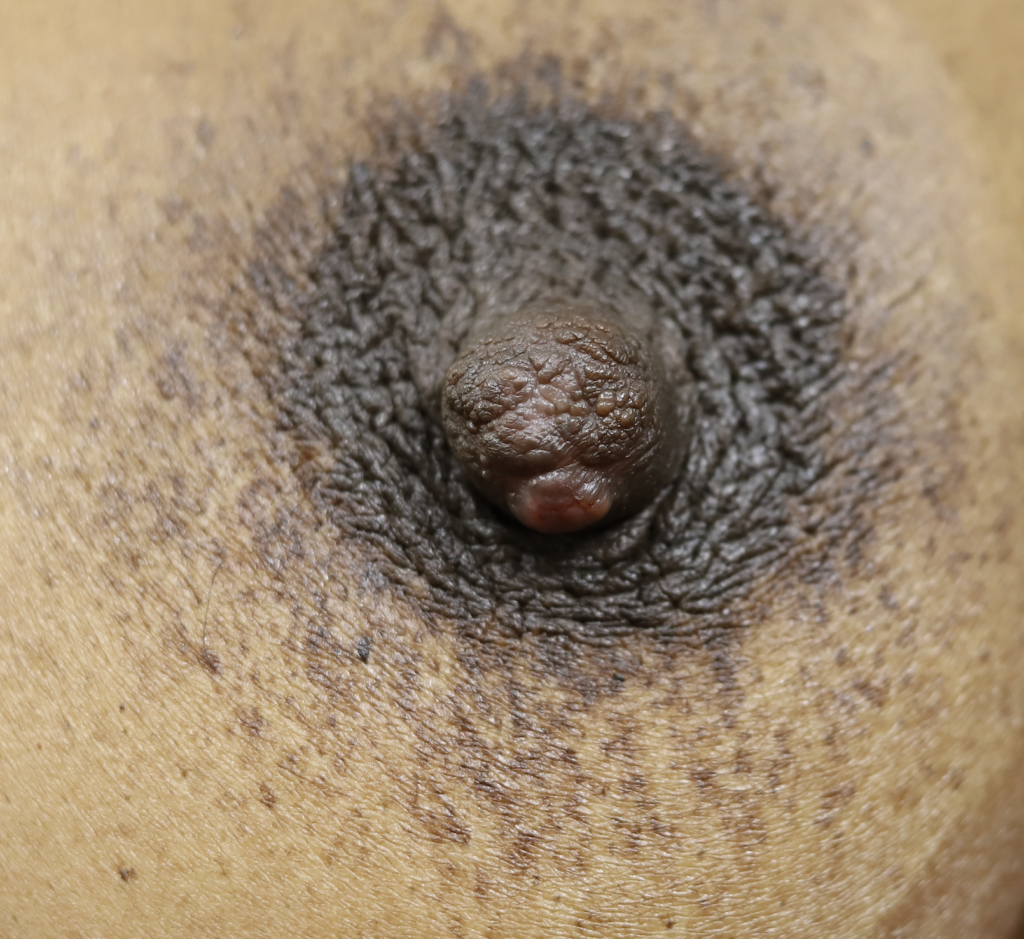
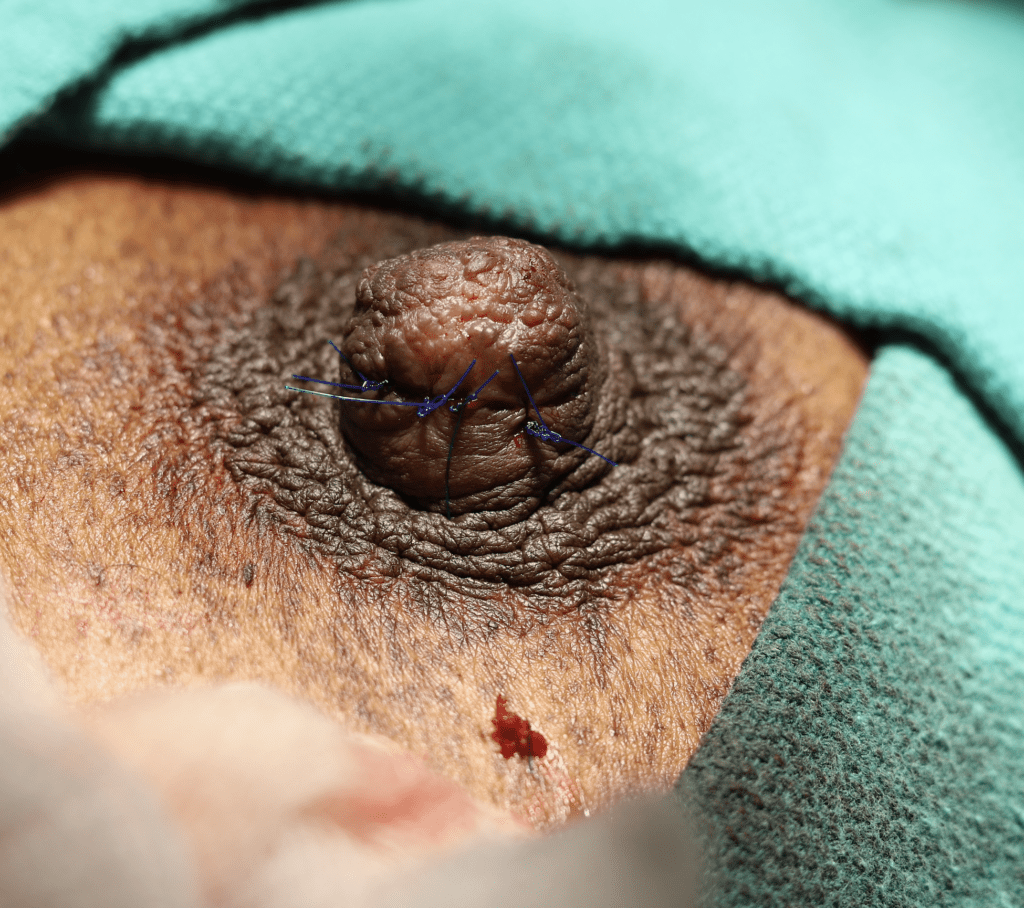
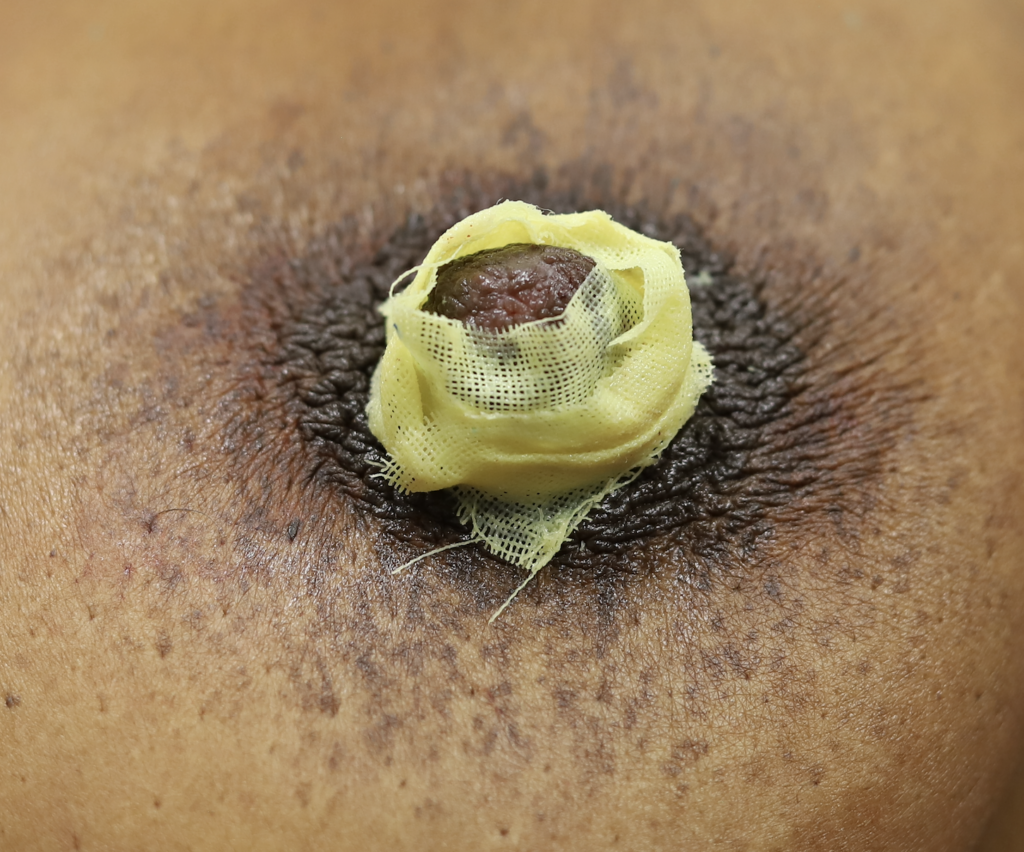
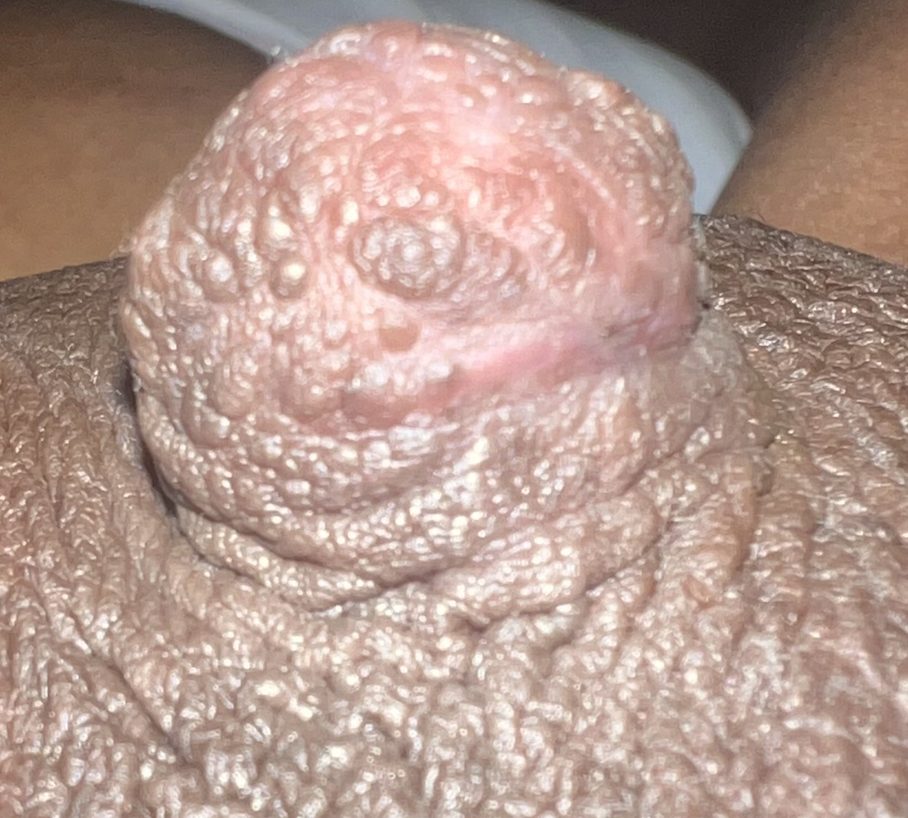
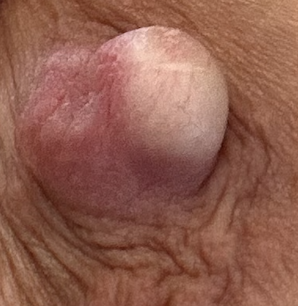
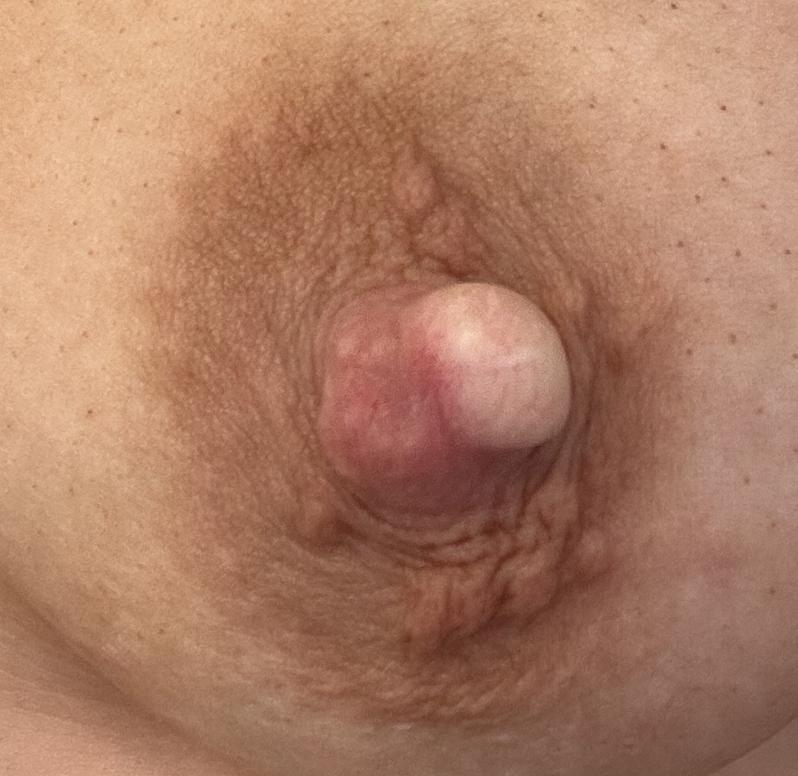
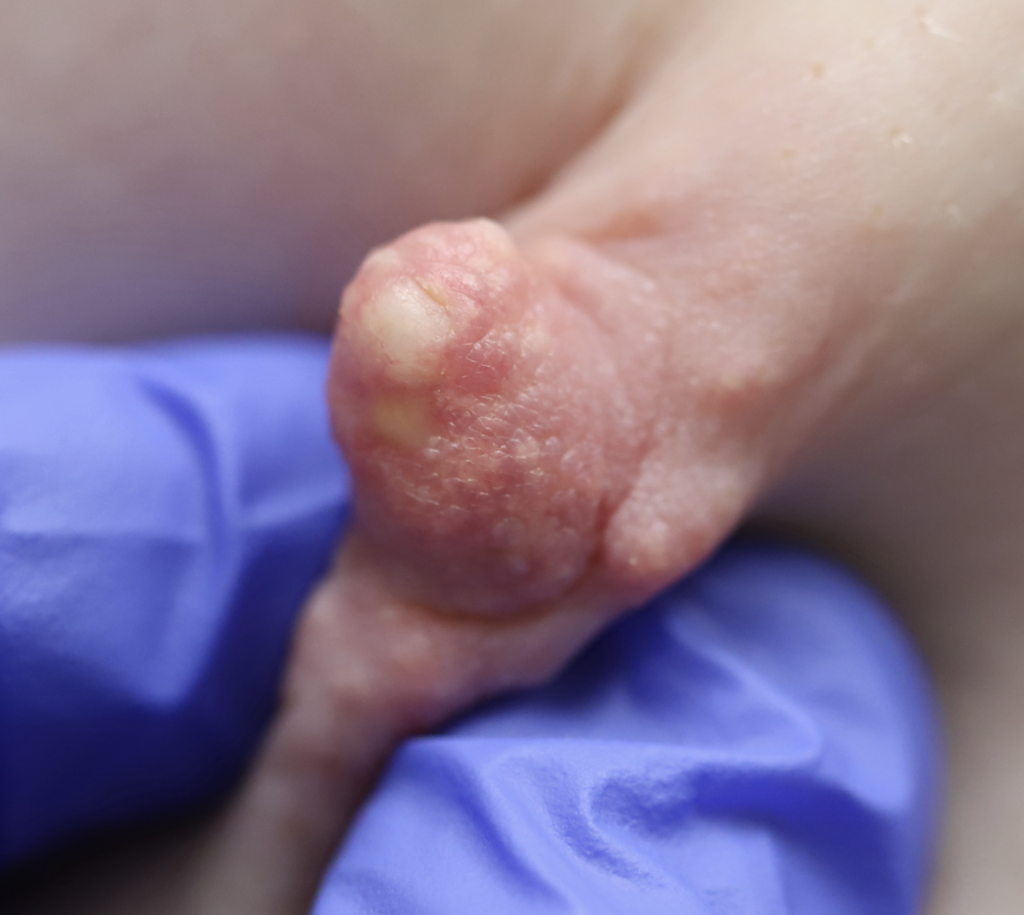
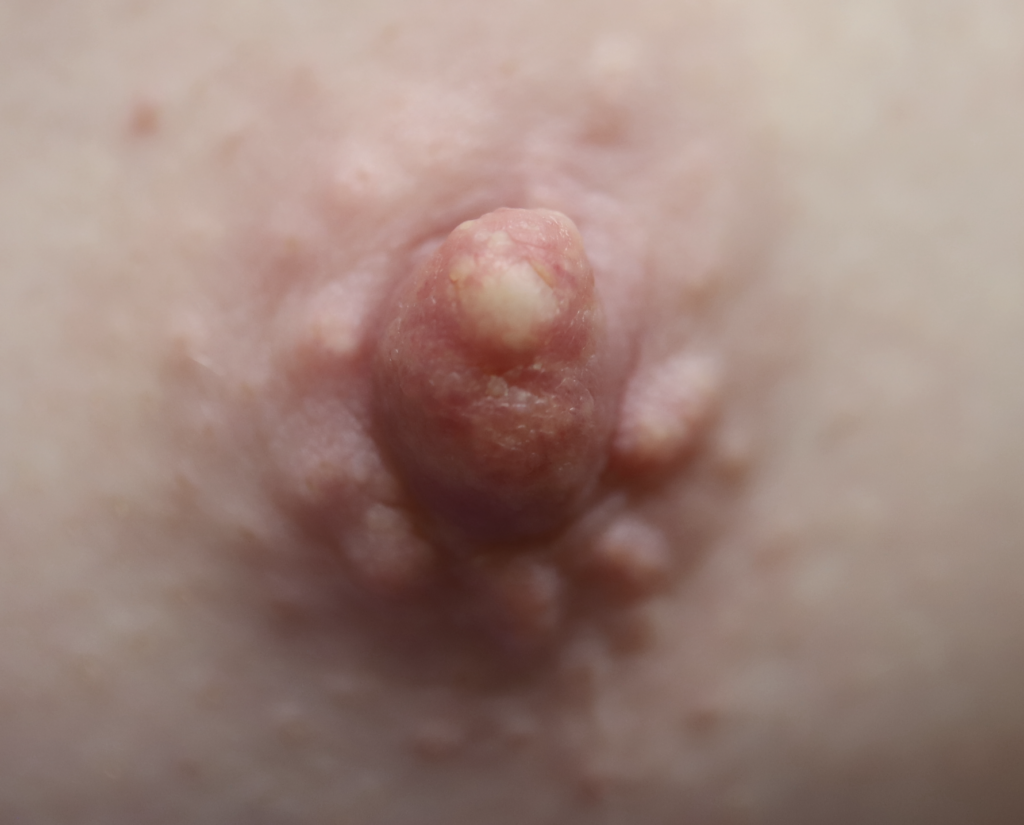
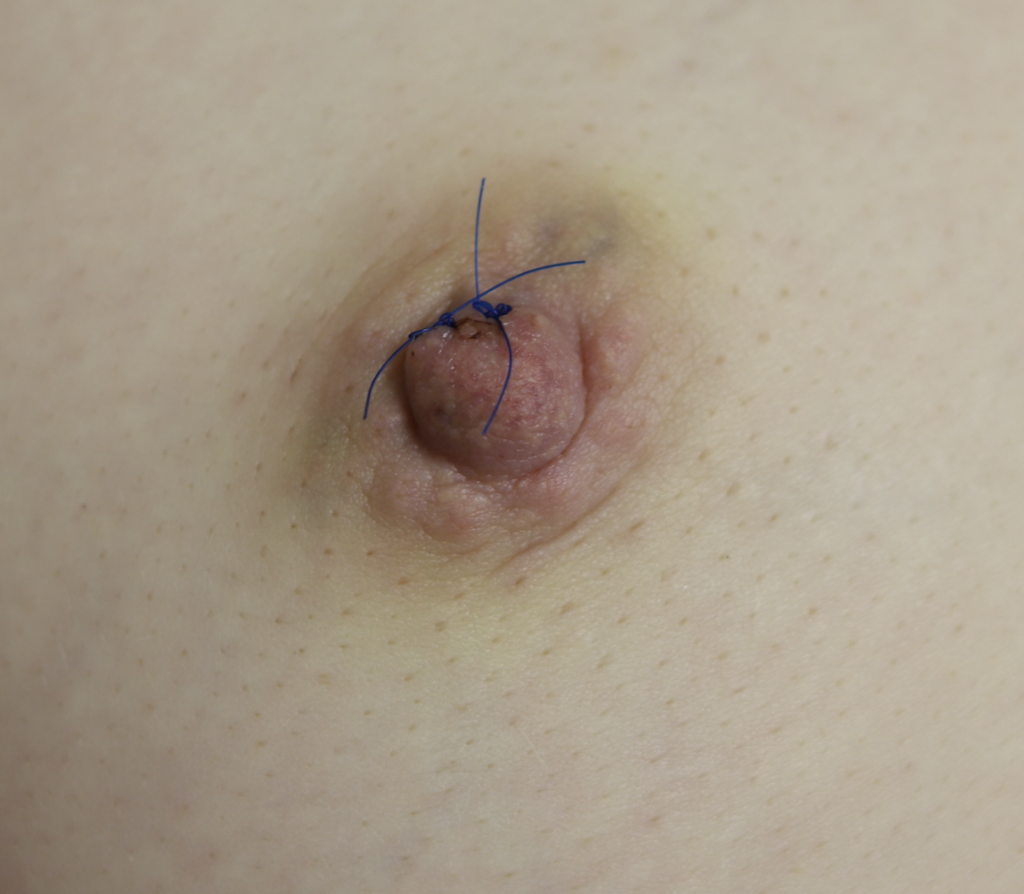
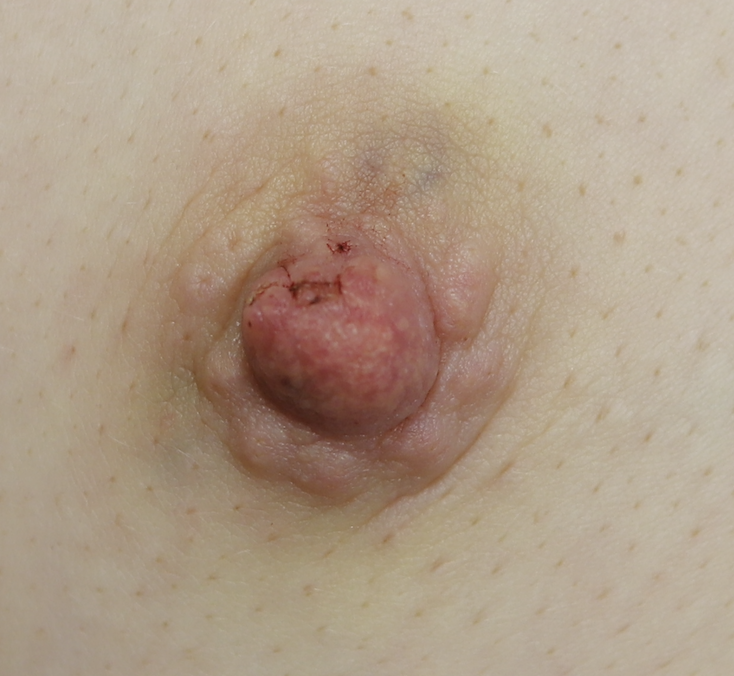
Video of this procedure below:



Dermatitis (Eczema)
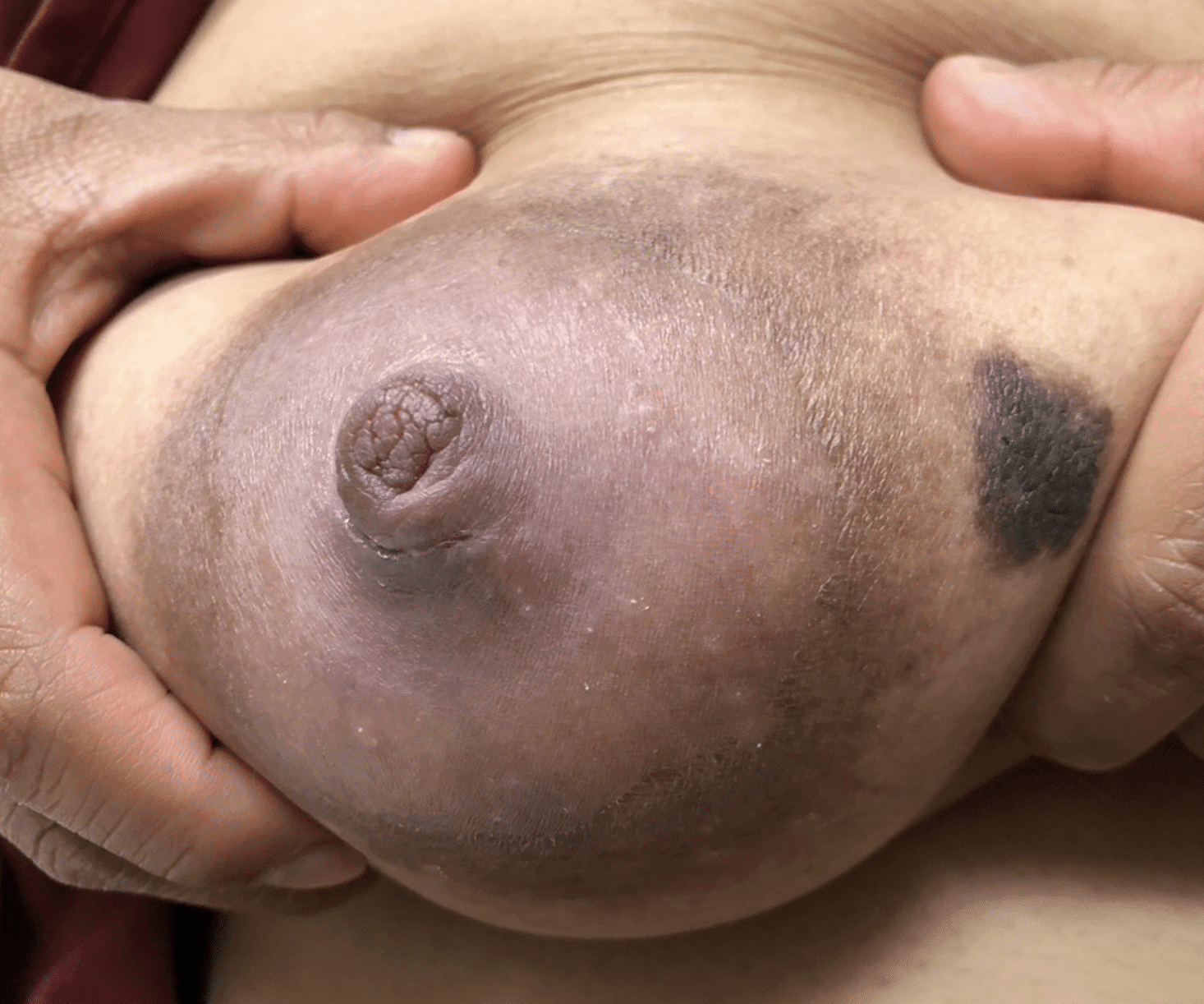
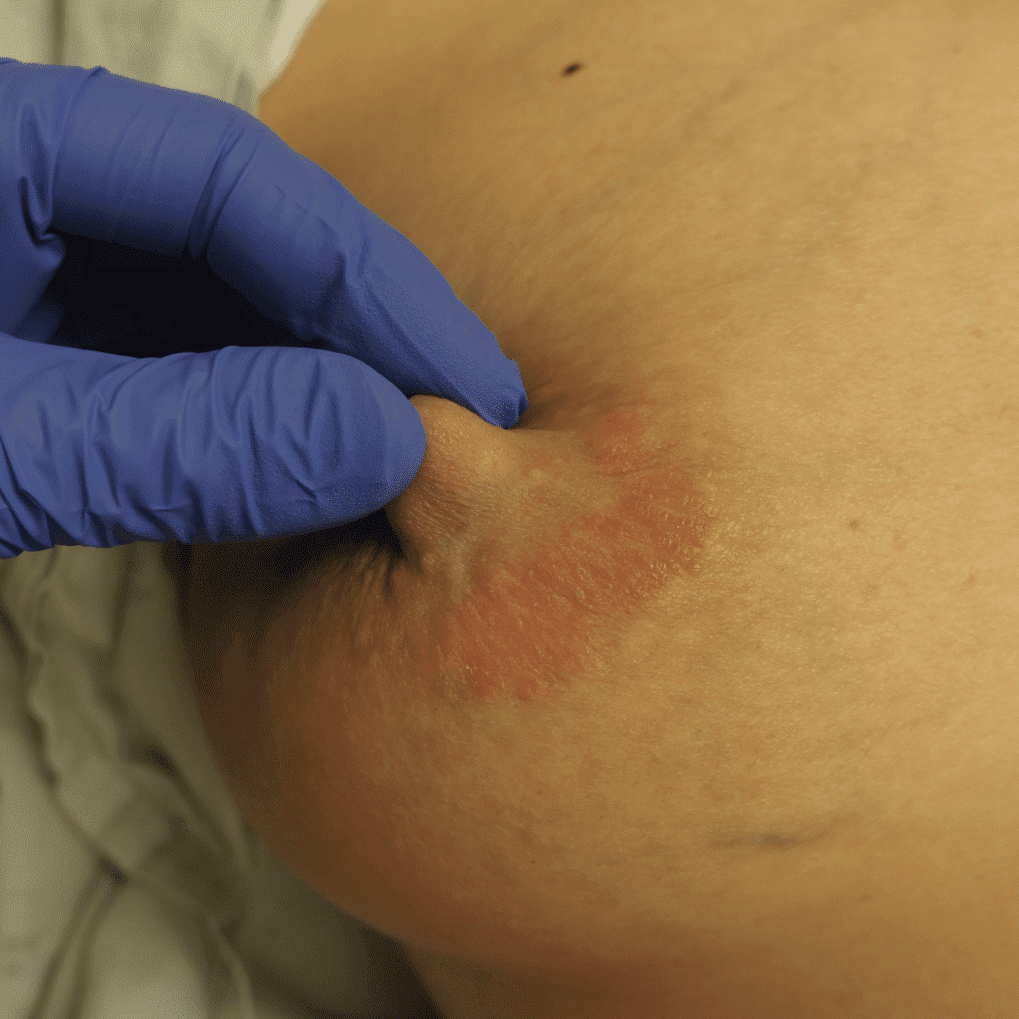
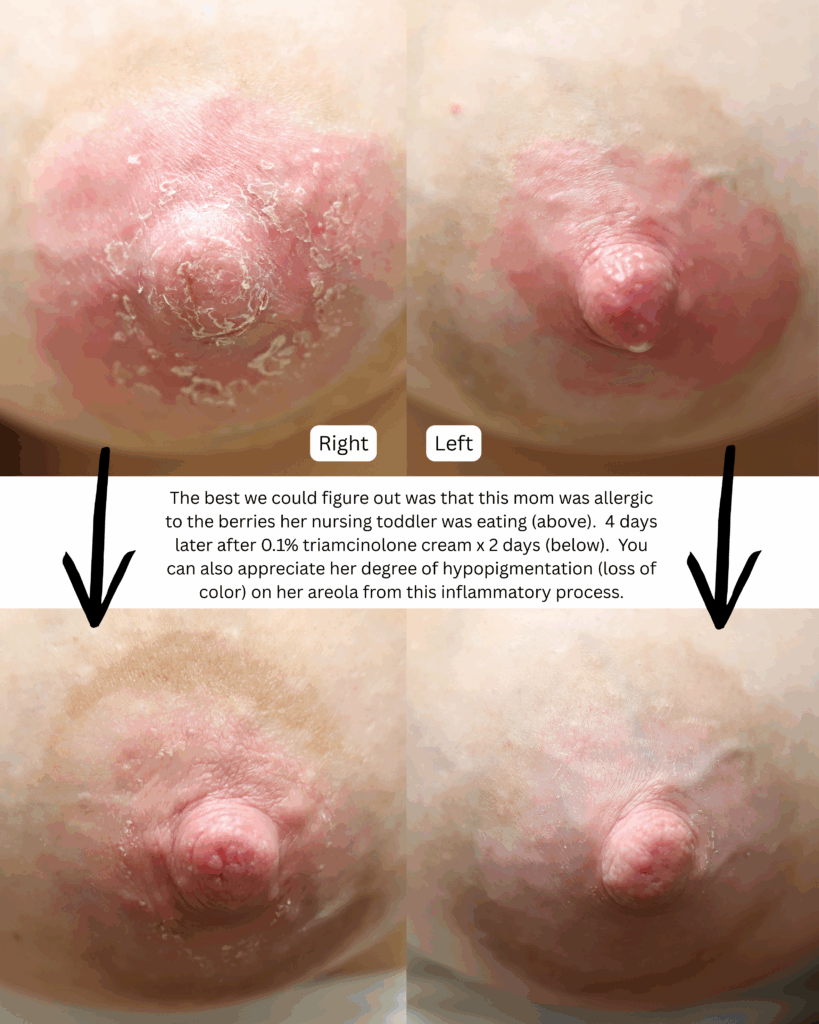
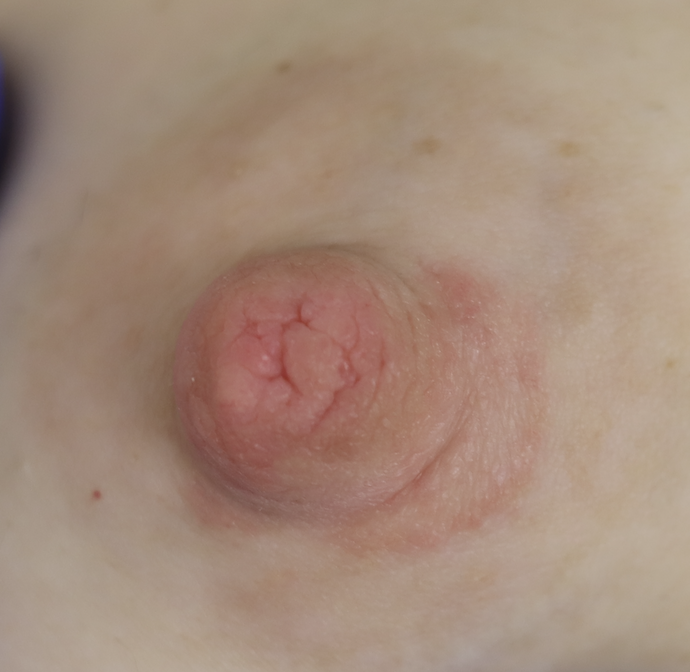
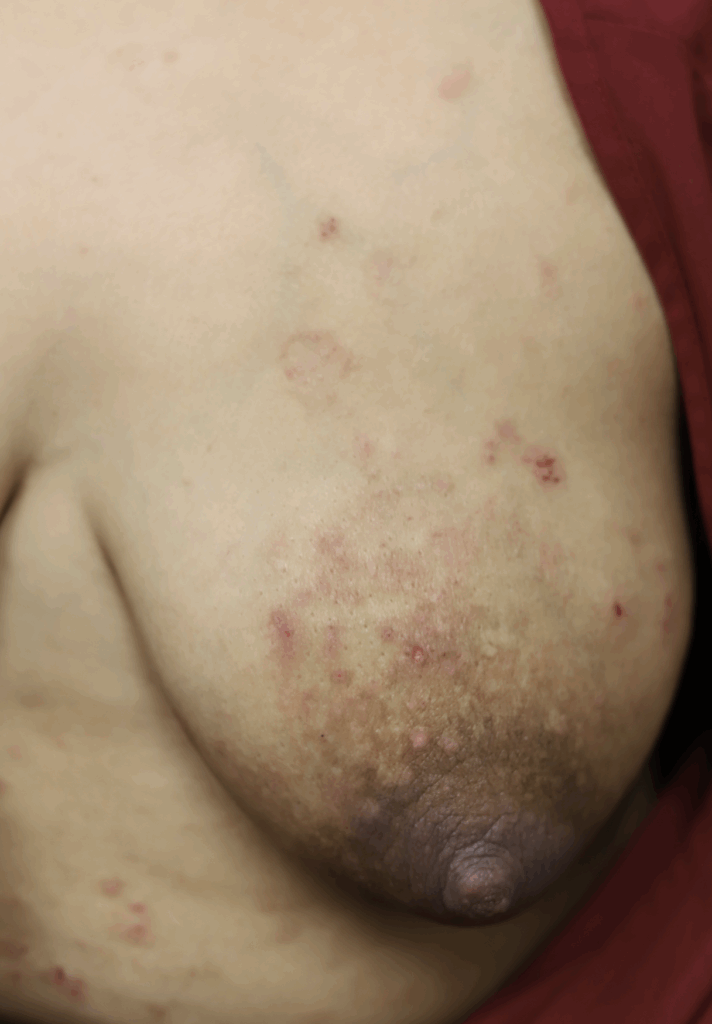
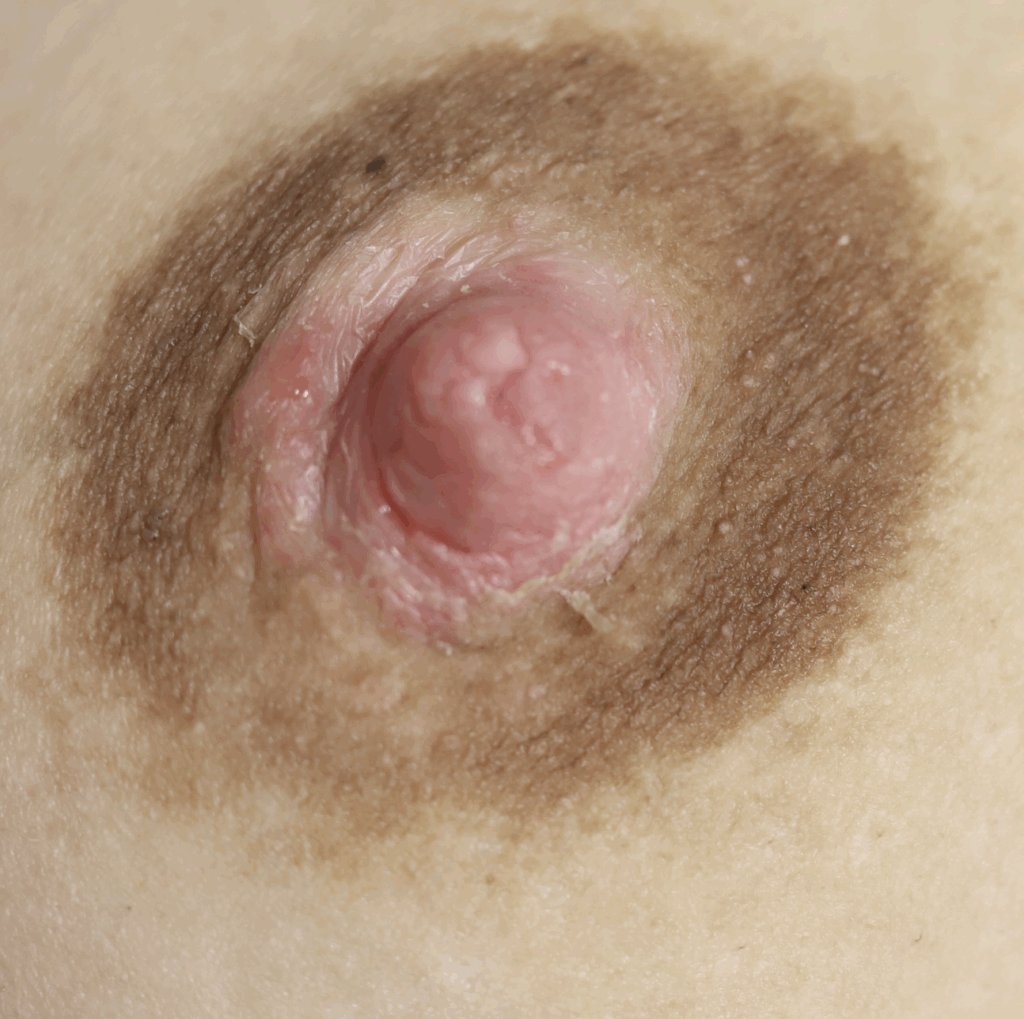
Dermatitis (or eczema) of the nipples, areolae, and breasts, presents as a red, burning, painful flaking rash. Often, patients are misdiagnosed with a “yeast infection” when in fact the etiology of their symptoms is dermatitis. One breast may be affected and not the other, without good explanation. Dermatitis can result from countless potential allergens, but the most common scenarios in breastfeeding are these:
- Topical anti-fungal and antibacterial agents such as those contained in APNO, petroleum, lanolin, coconut, and emollients contained in creams, lotions, or ointments.
- Pump parts, nursing bras, nursing pads, new detergents or soaps, and nipple shields
- Substances that children are ingesting or touching, including antibiotics and complementary foods
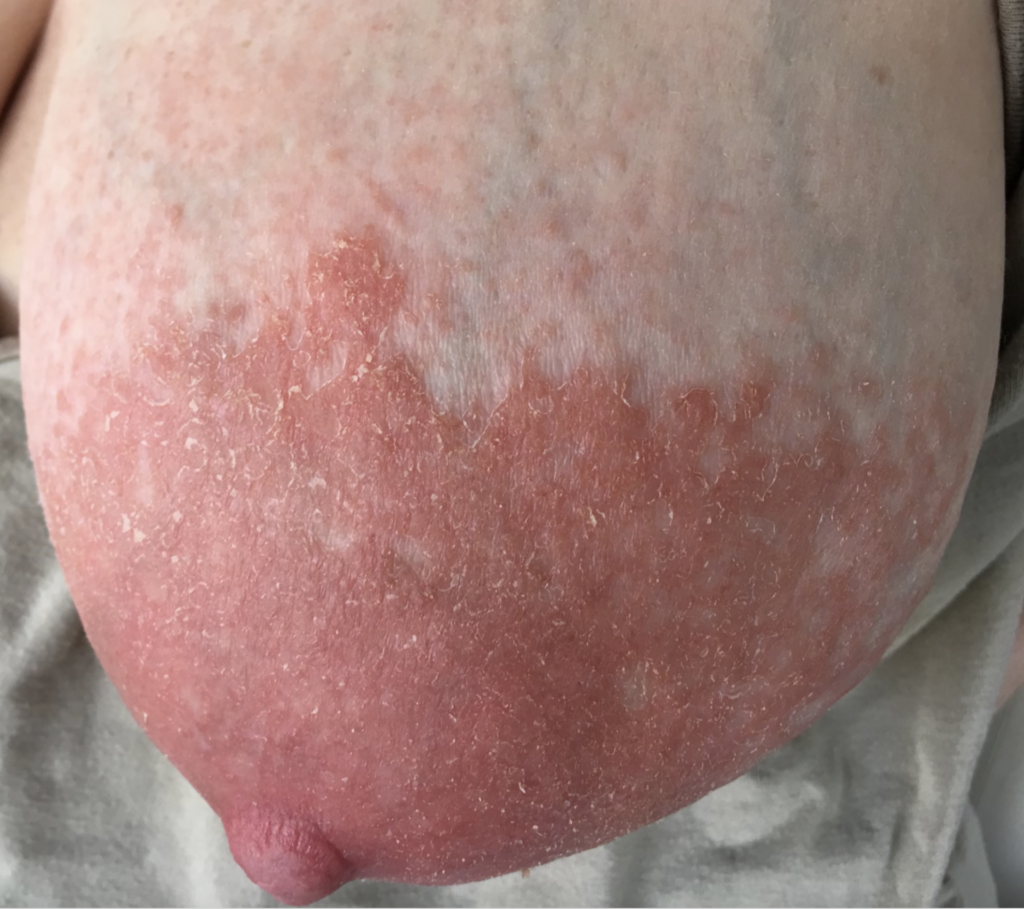
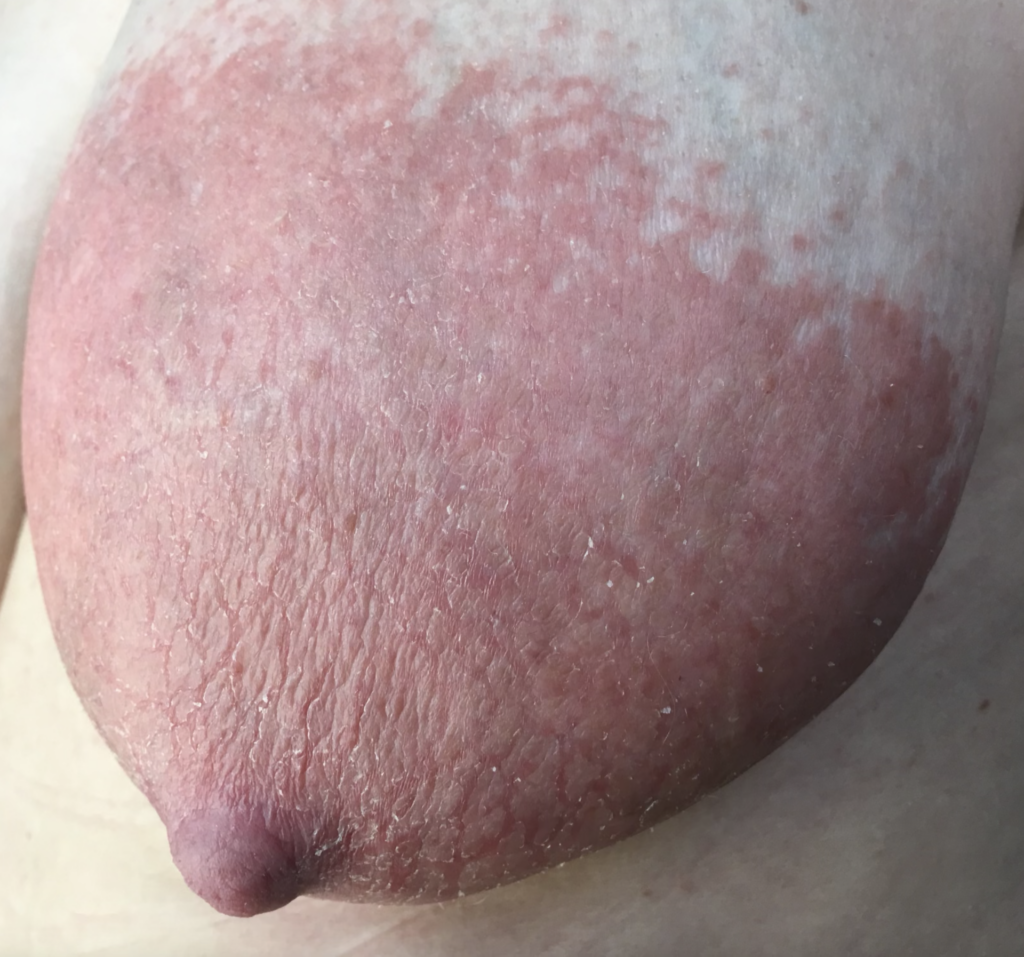
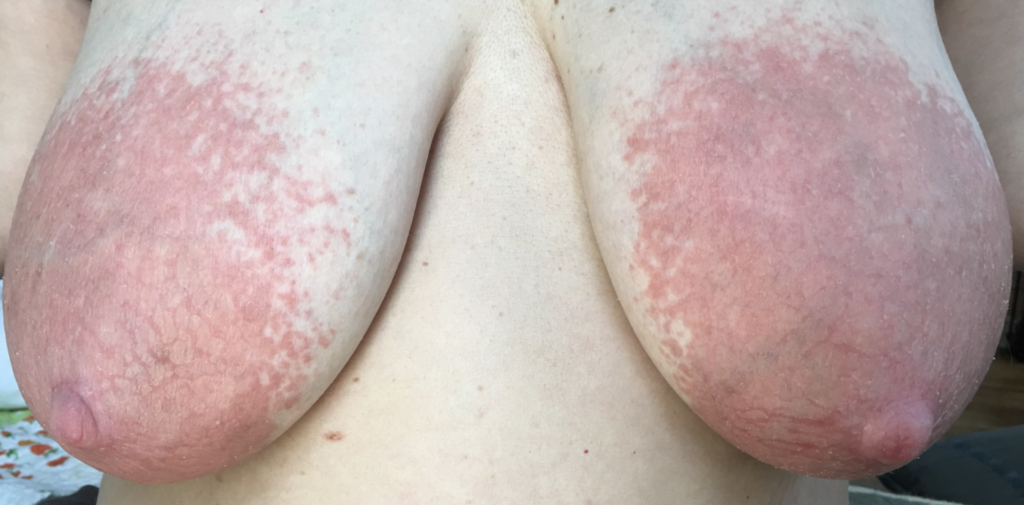
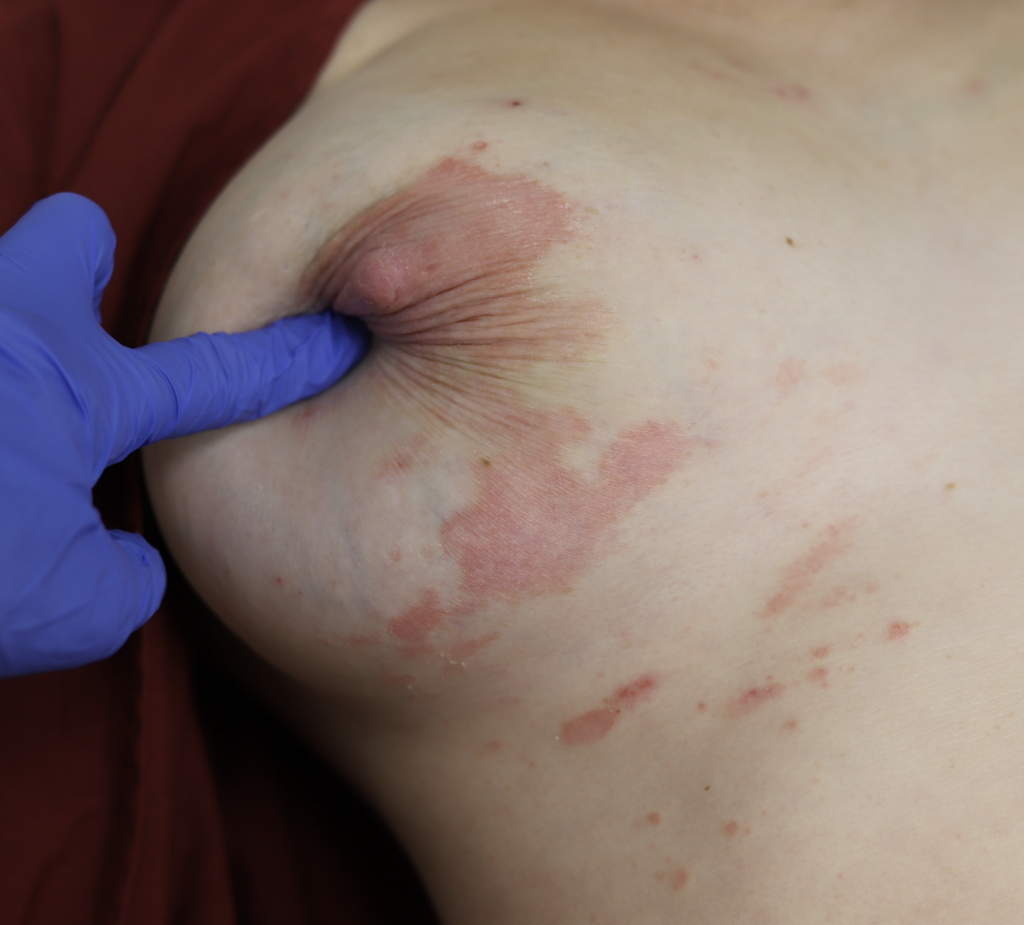
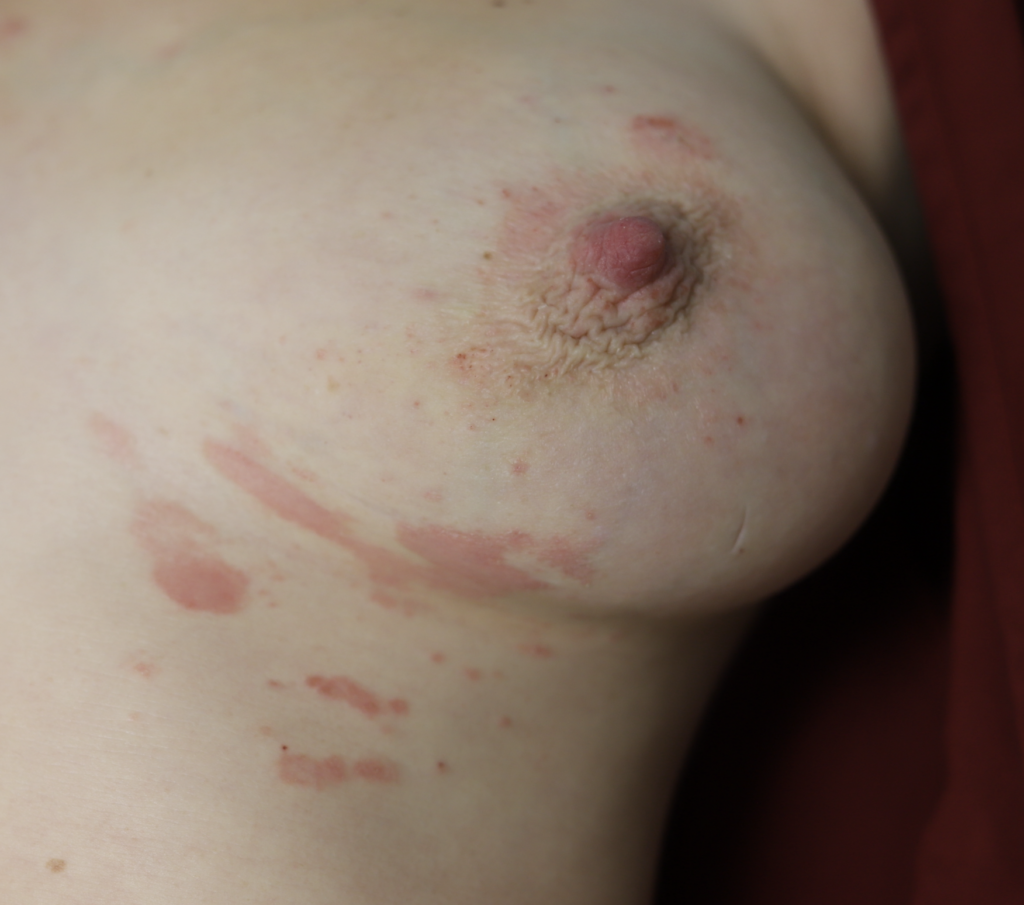
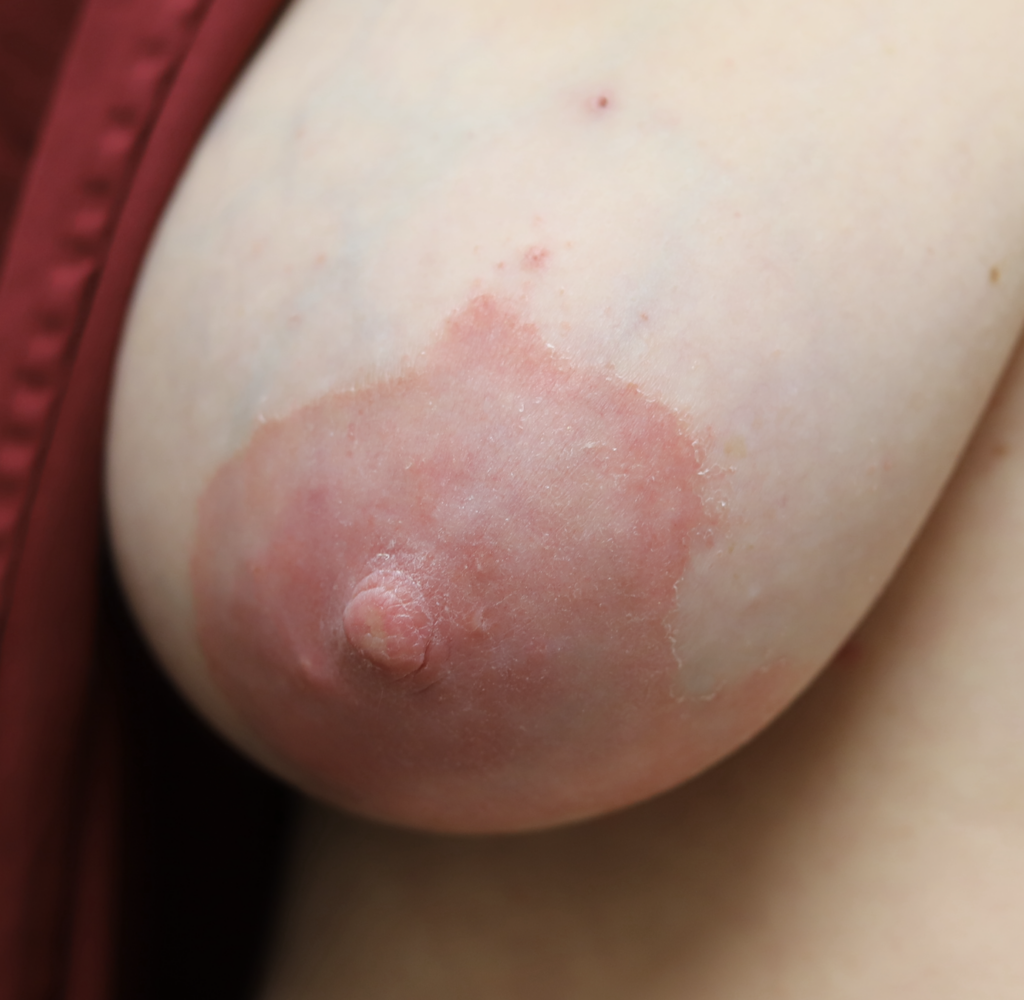
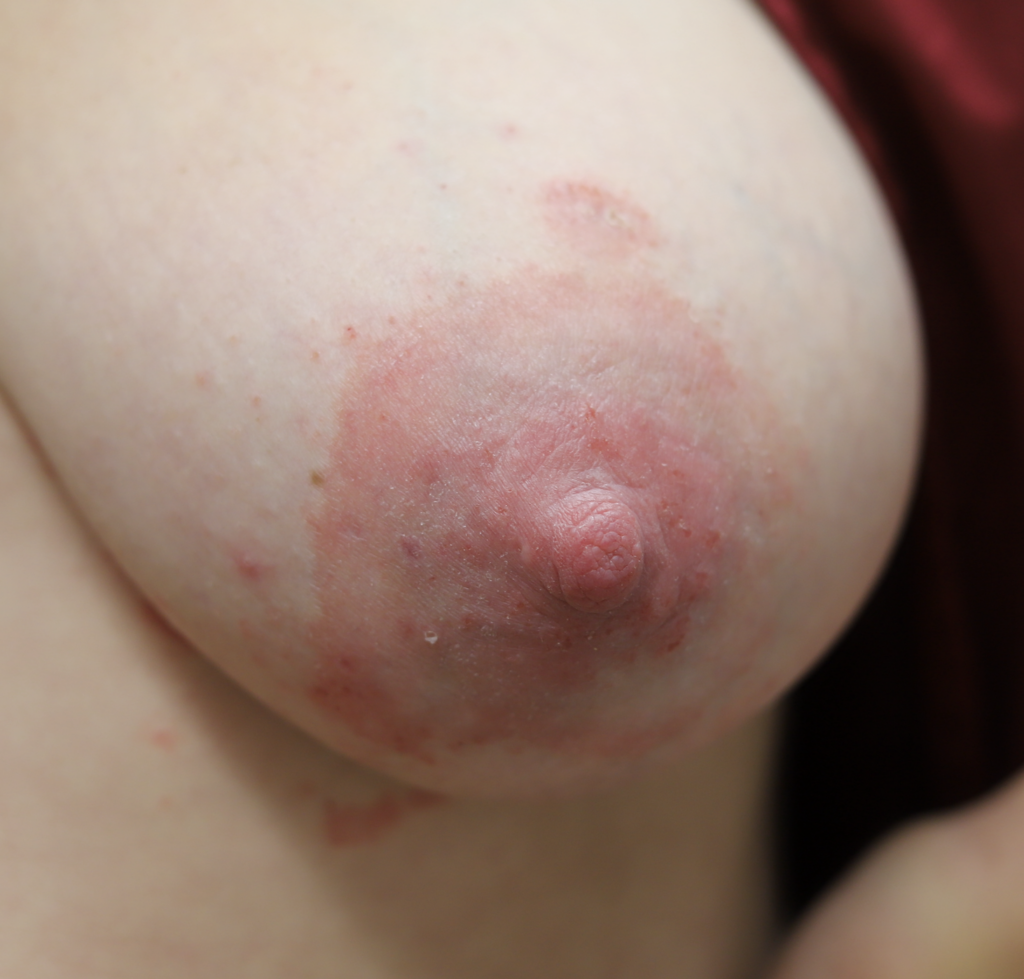
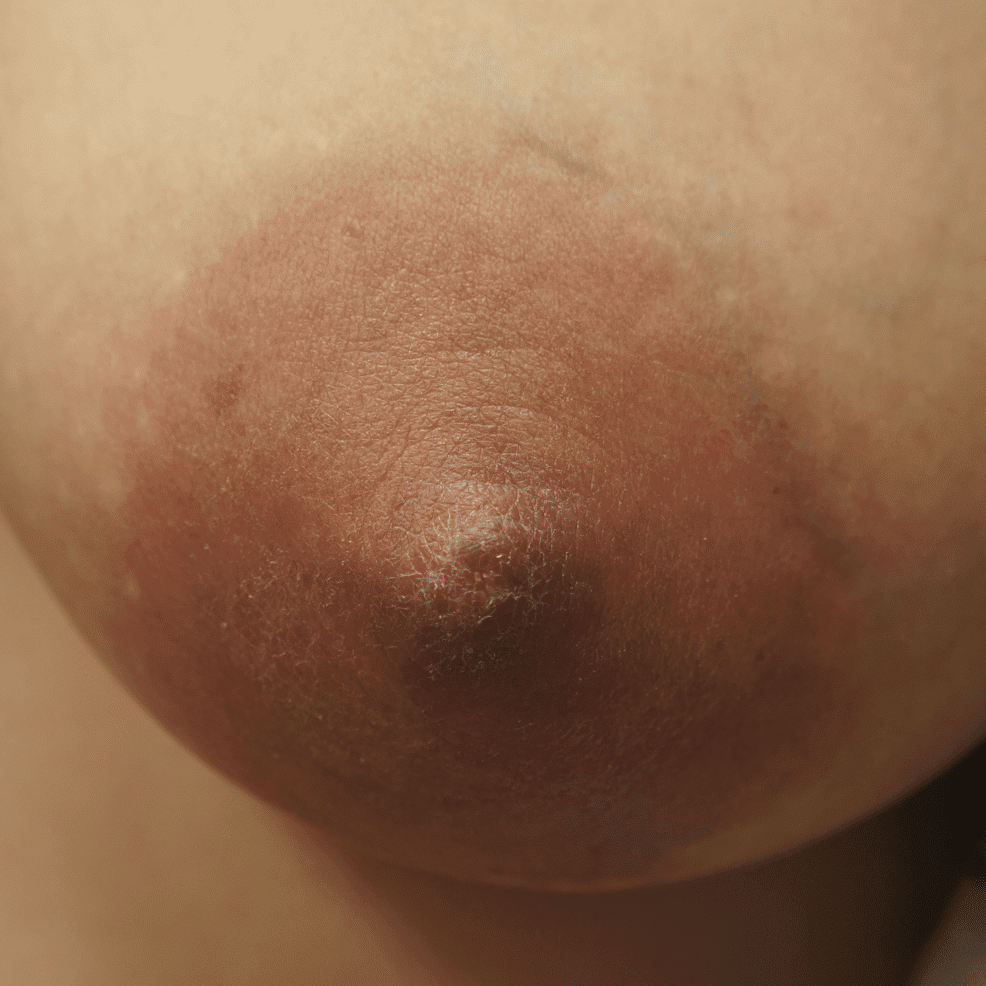
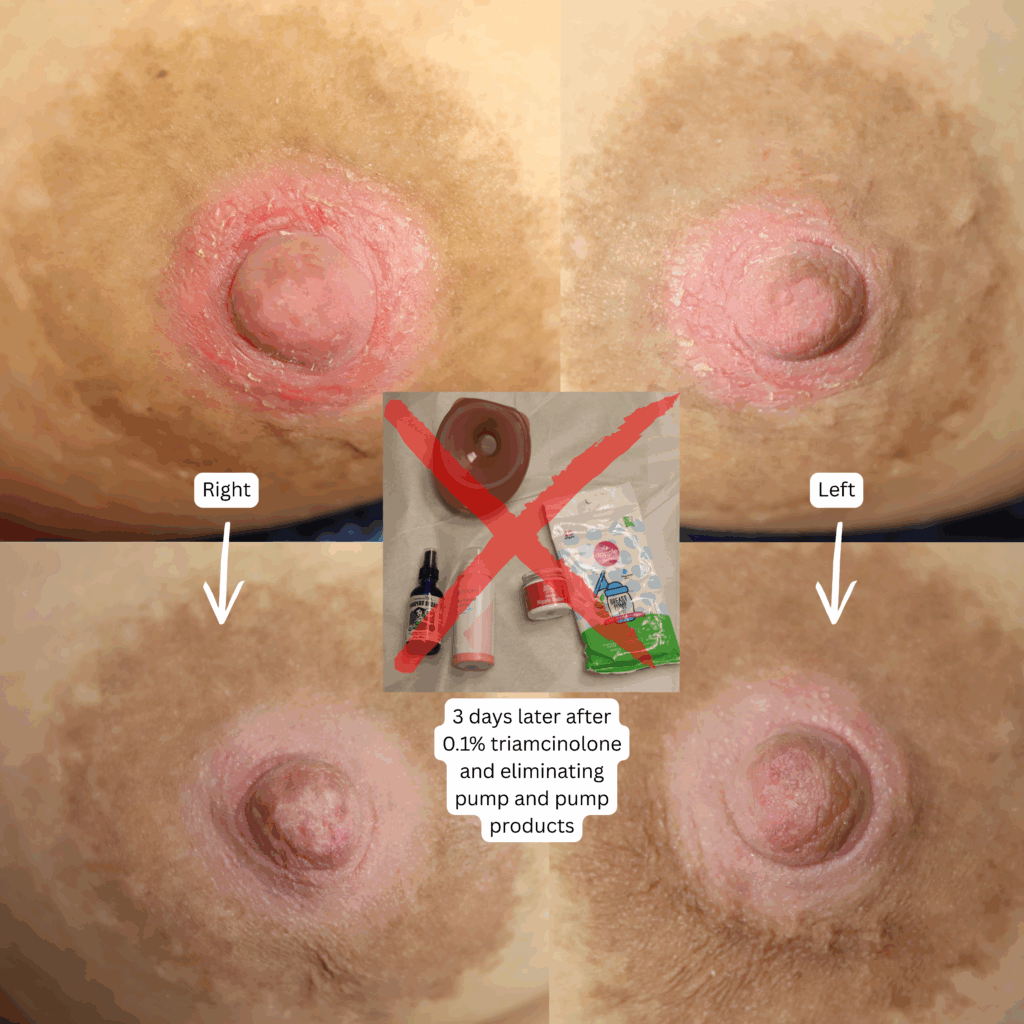
One week later, complete resolution after just a few days of steroid cream:
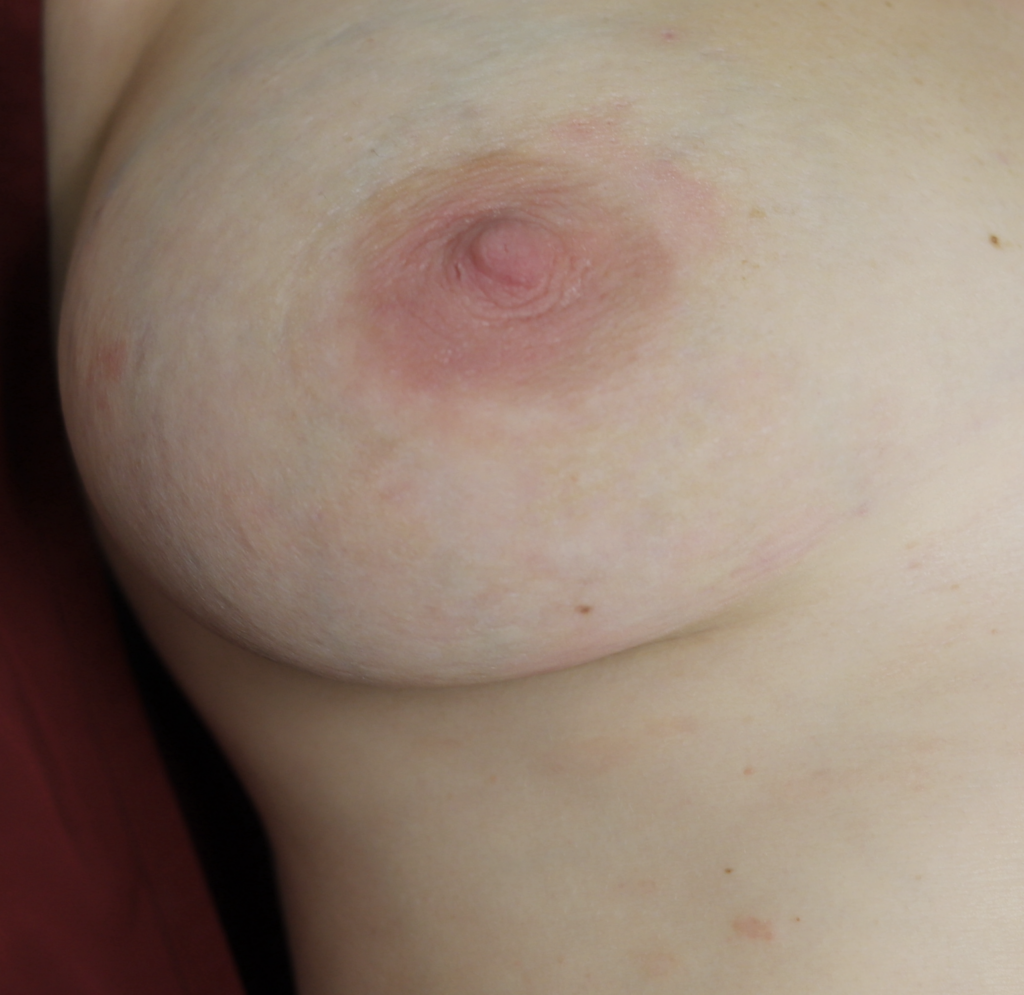









Treatment involves the following:
- All potential allergens should be explored and eliminated
- A short course of prescription steroid (e.g. 0.1% triamcinolone) will clear a persistent case in a few days.
- Oral antihistamine medication or steroids used in cases of severe allergy may not affect milk production in most women, patients should watch for changes in output, particularly those with lower baseline milk production. However, the vast majority of the time, these oral agents are not necessary.

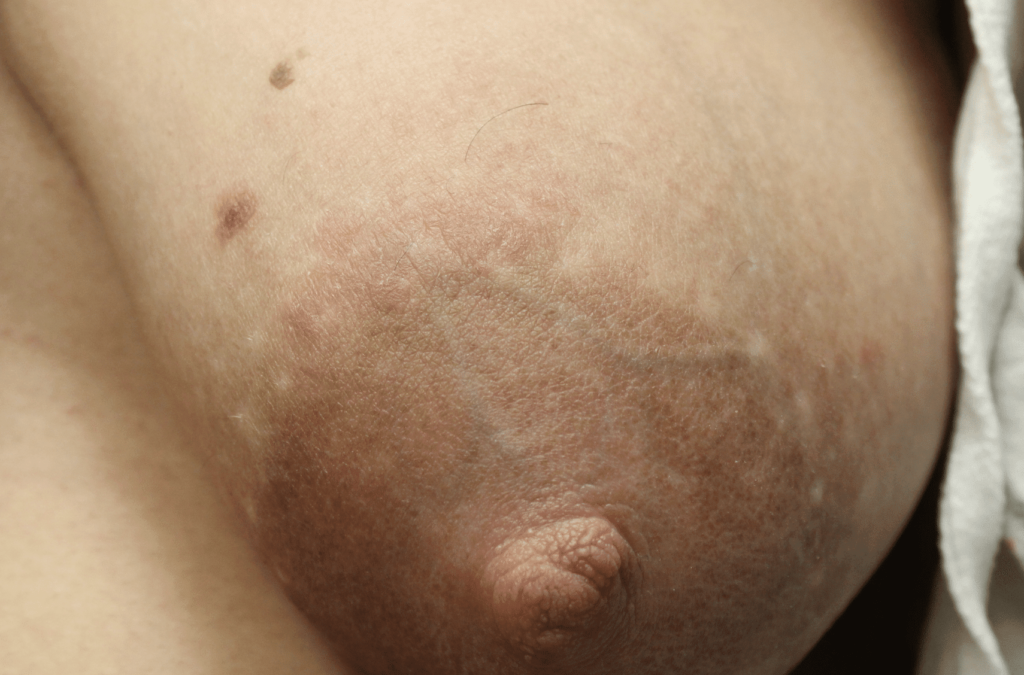

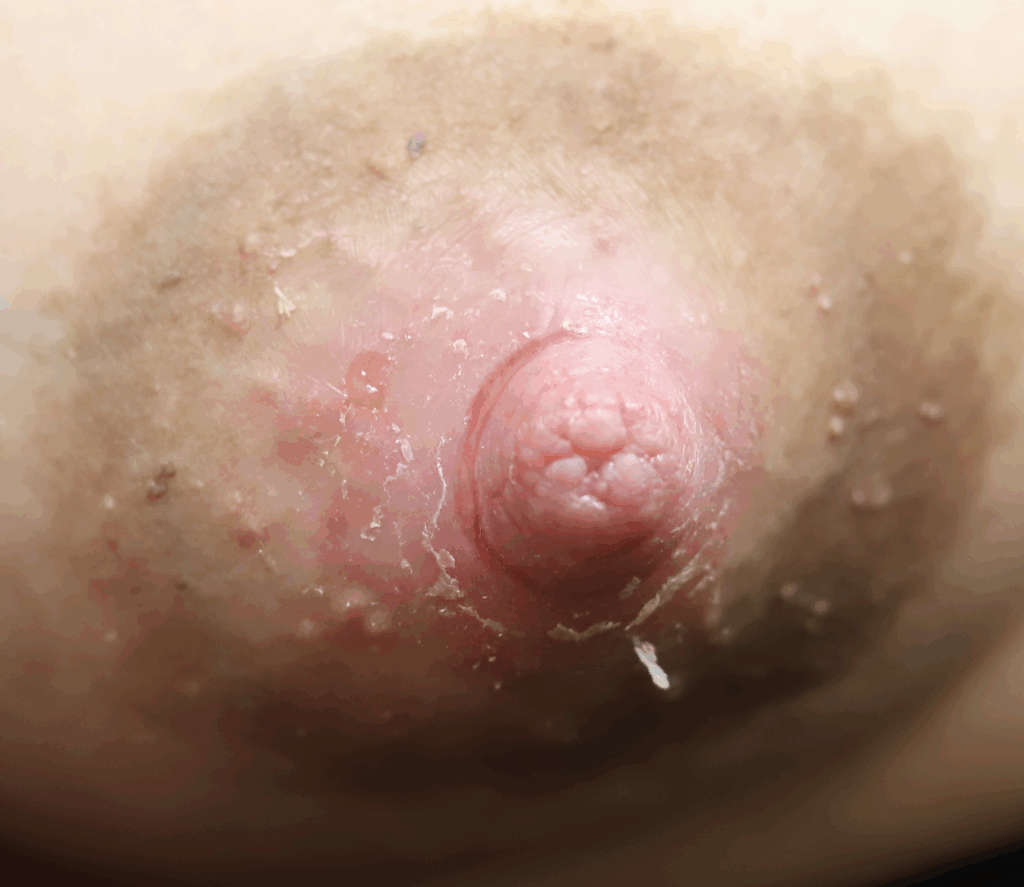
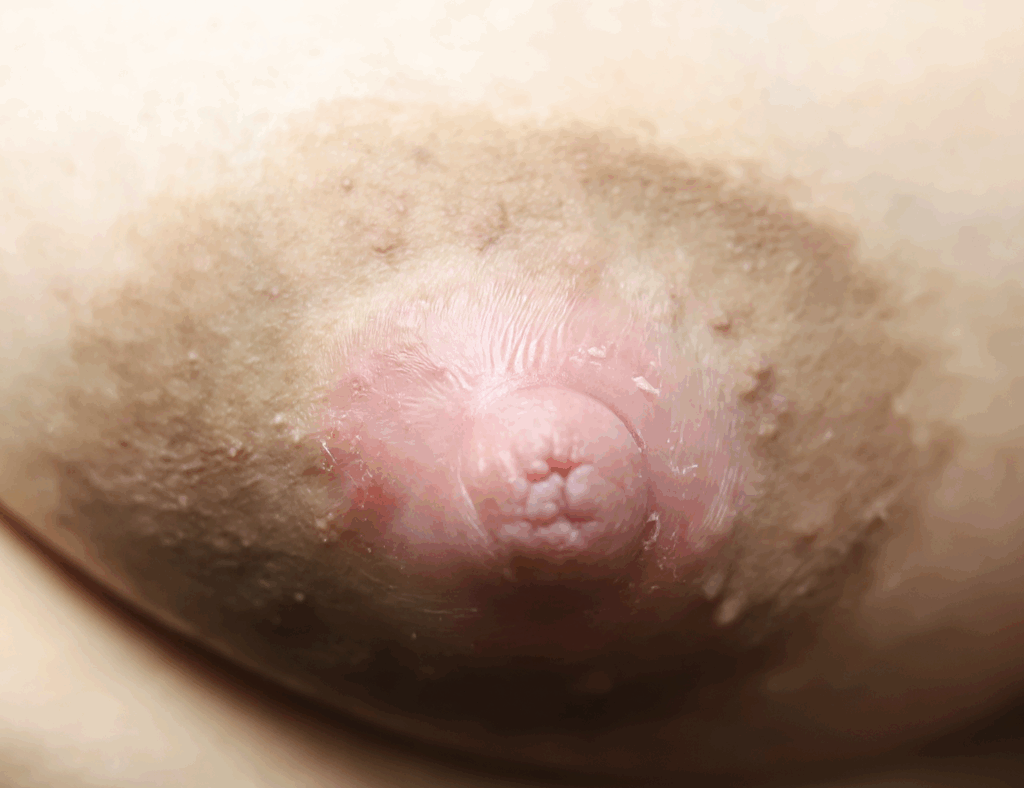
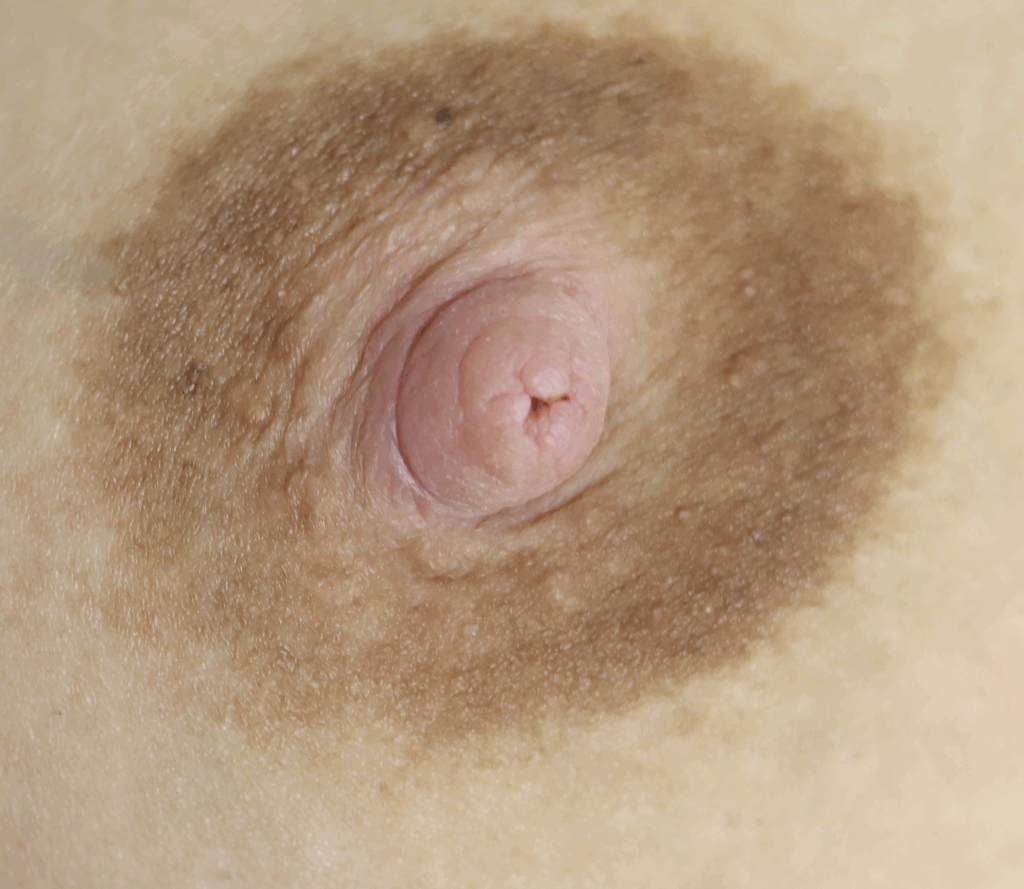
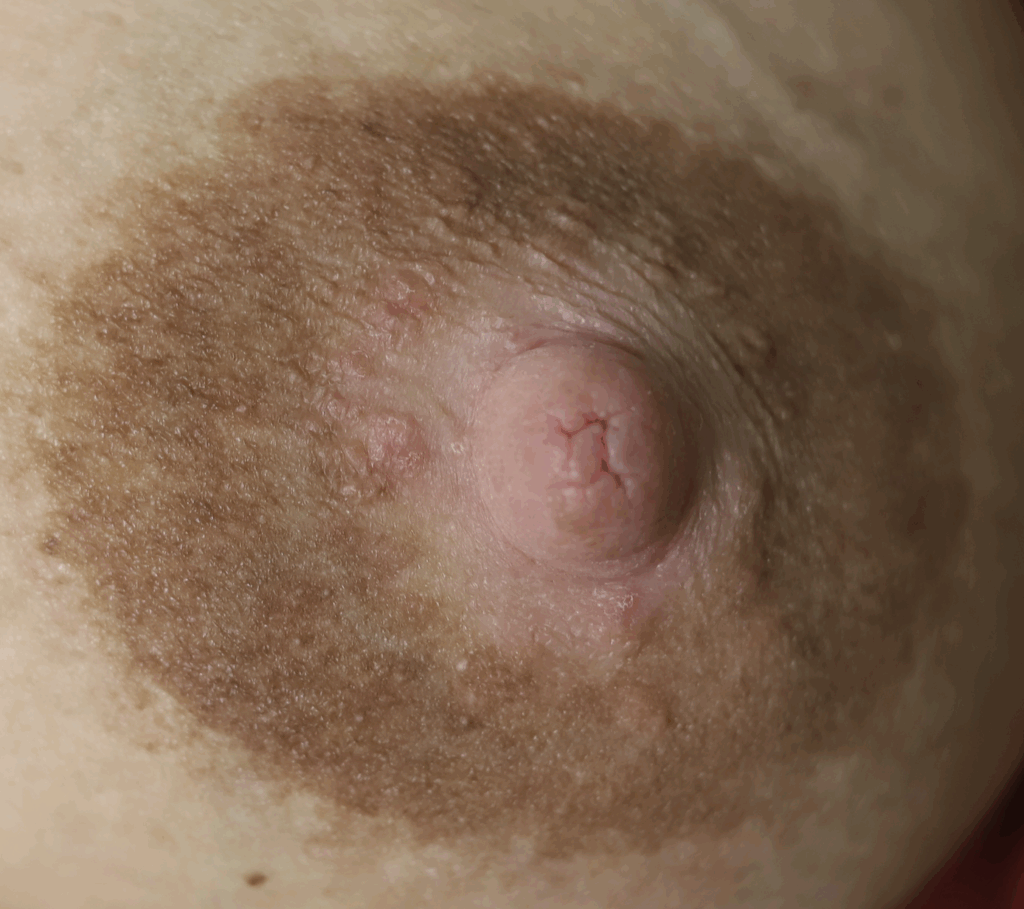
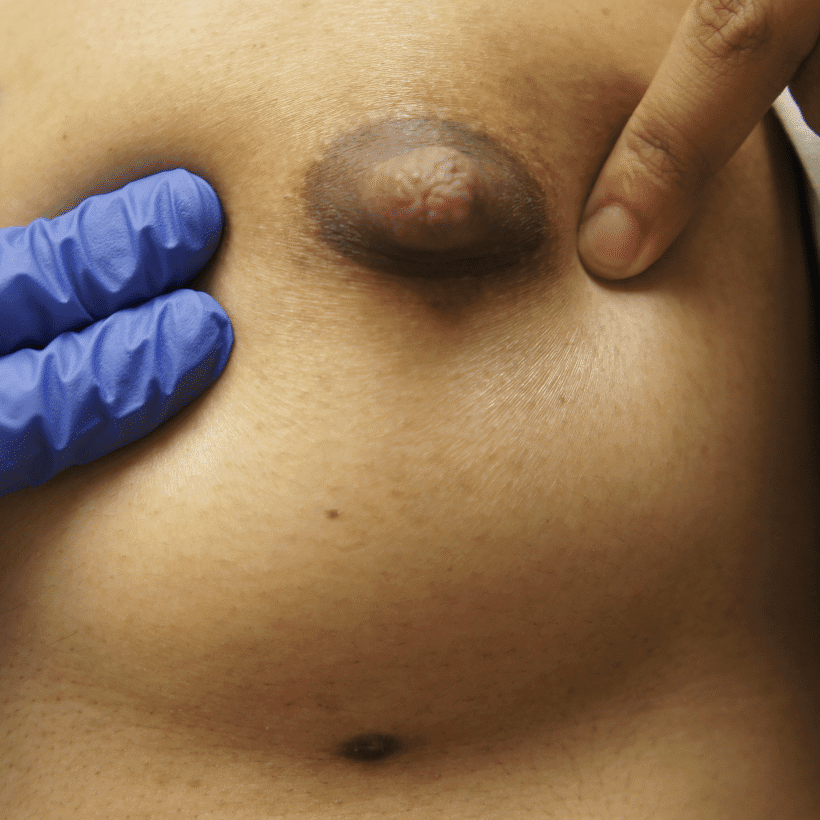
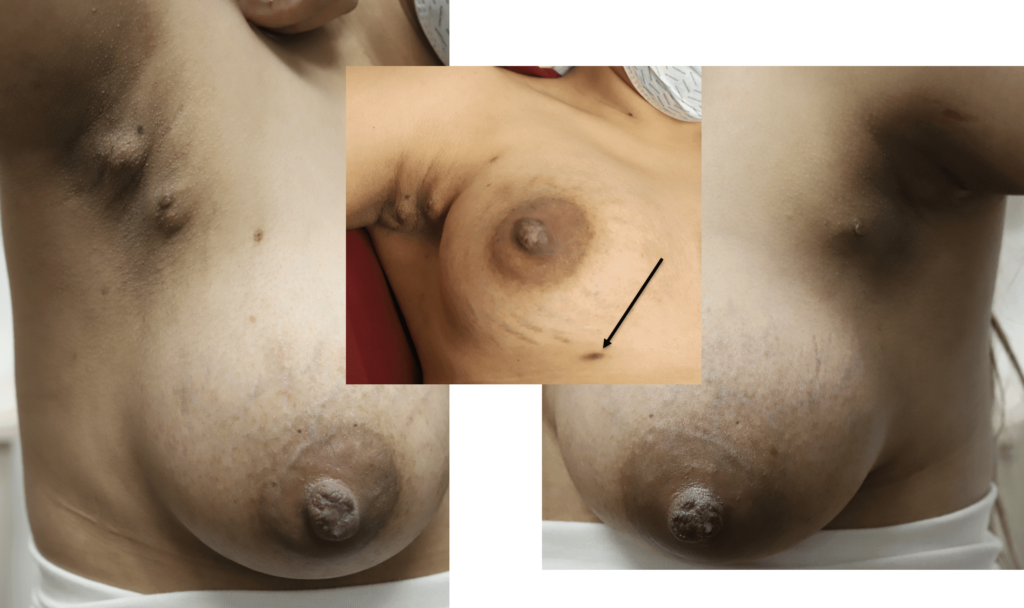
Extra Nipples
Supernumerary, or “accessory nipples” are common and may become engorged or produce milk. They will regress within a week if they are not continually stimulated or expressed.


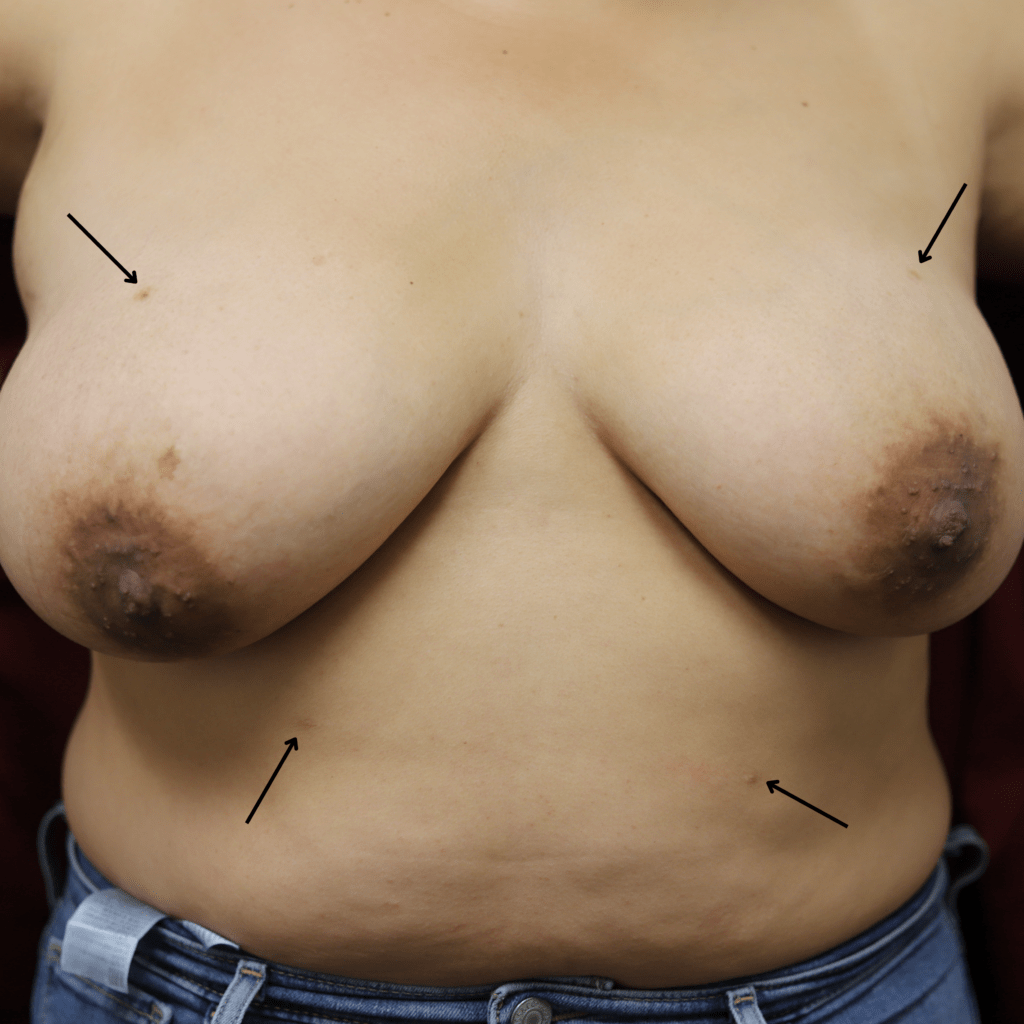
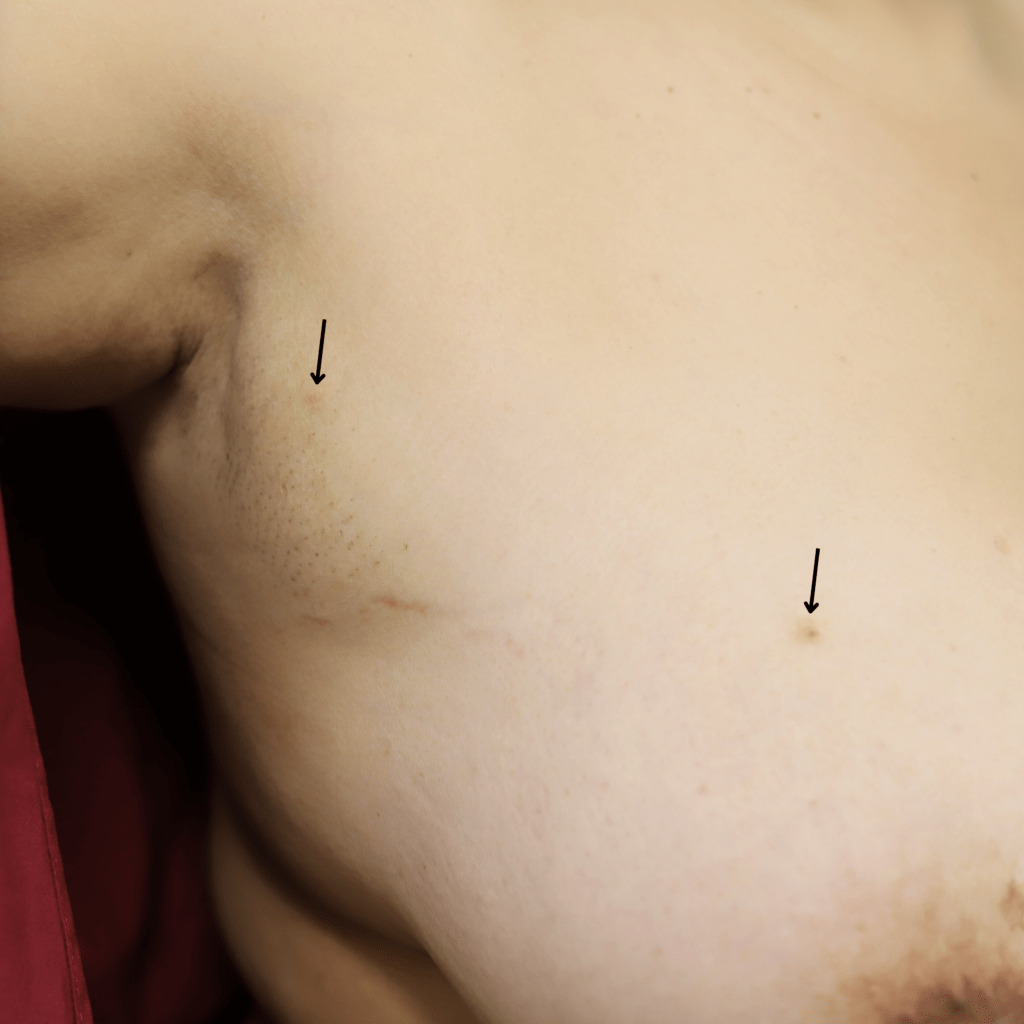









Fungal Infections
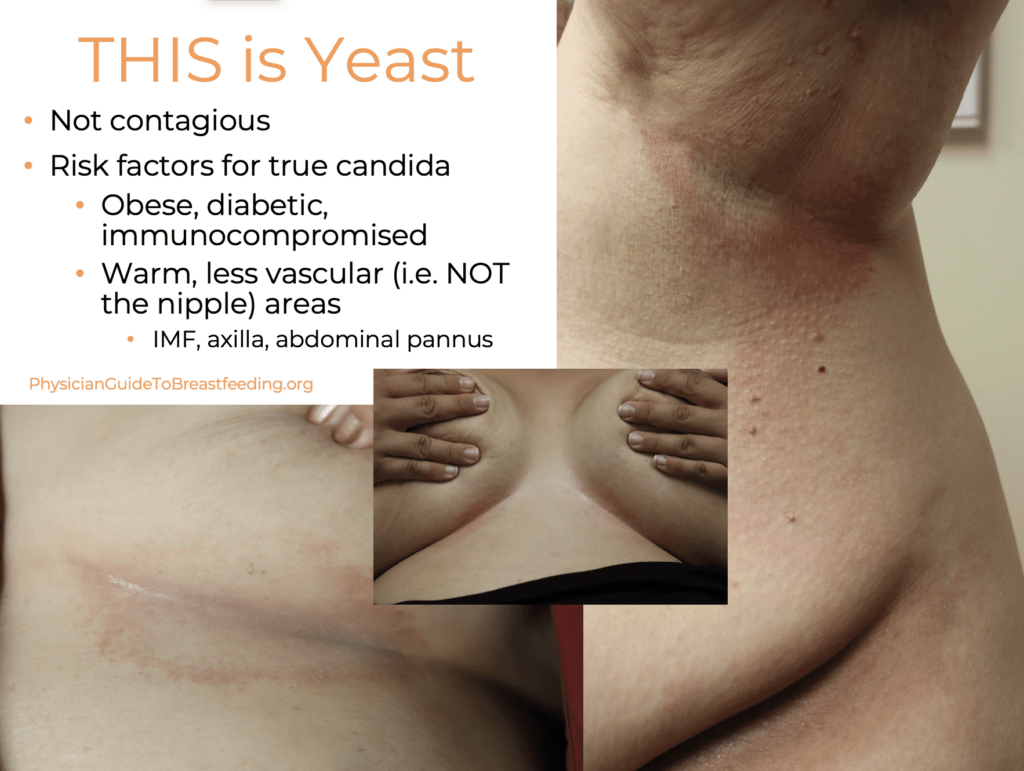
The most common superficial fungal infection of the skin of the lactating breast is Candida intertrigo, which presents as an itchy, beefy red rash located in the inframammary fold (the skin underneath the breast that can get sweaty and chaffed during hot weather) or under the arm (axilla).
Candida is not contagious just as vaginal yeast infections are not contagious. Therefore, if an infant is diagnosed with thrush (which is also unlikely in the absence of formula feeding, prematurity, repeated antibiotics, and other risk factors for significant immunosuppression), the mother’s breast and nipple does not require treatment. In fact, anti-fungals on the nipple of the breast are highly irritating and may produce a contact dermatitis.
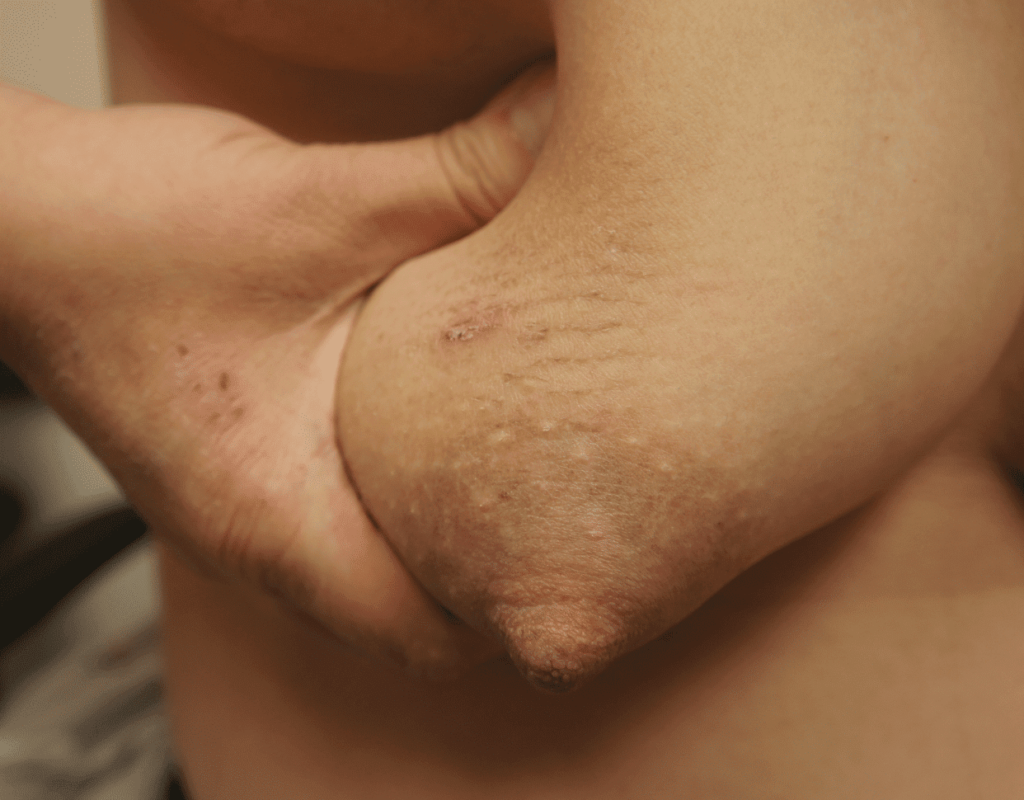
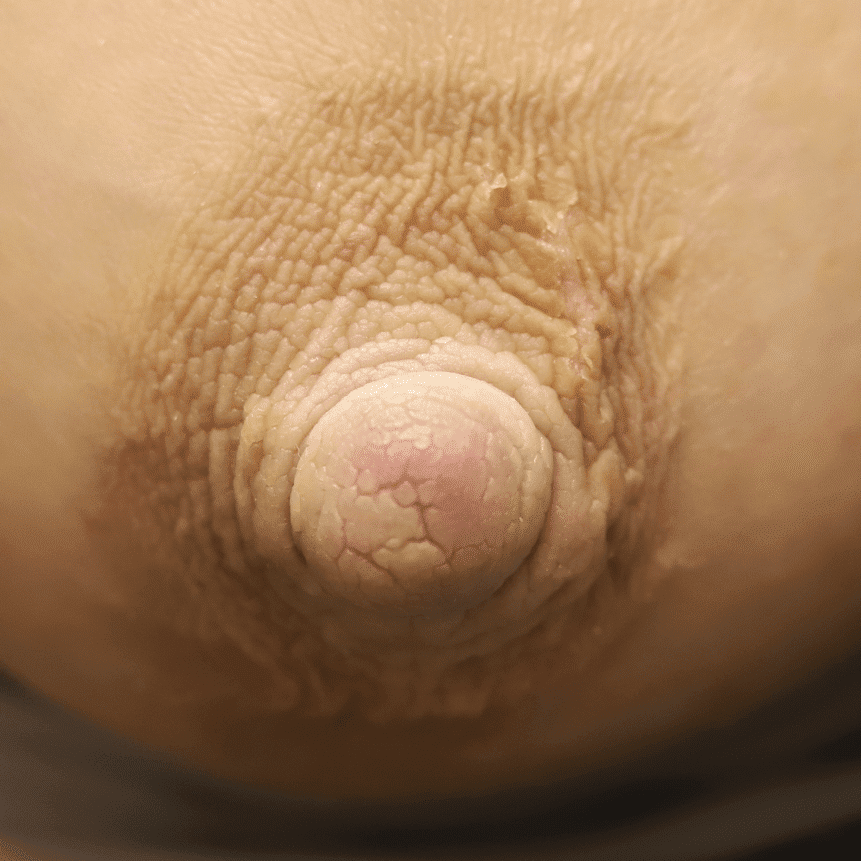
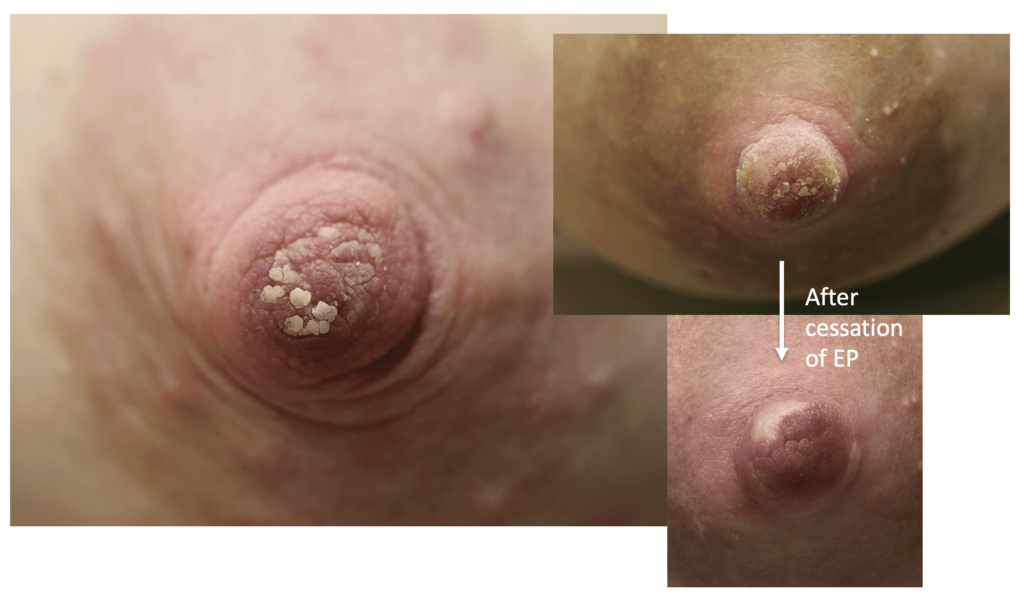
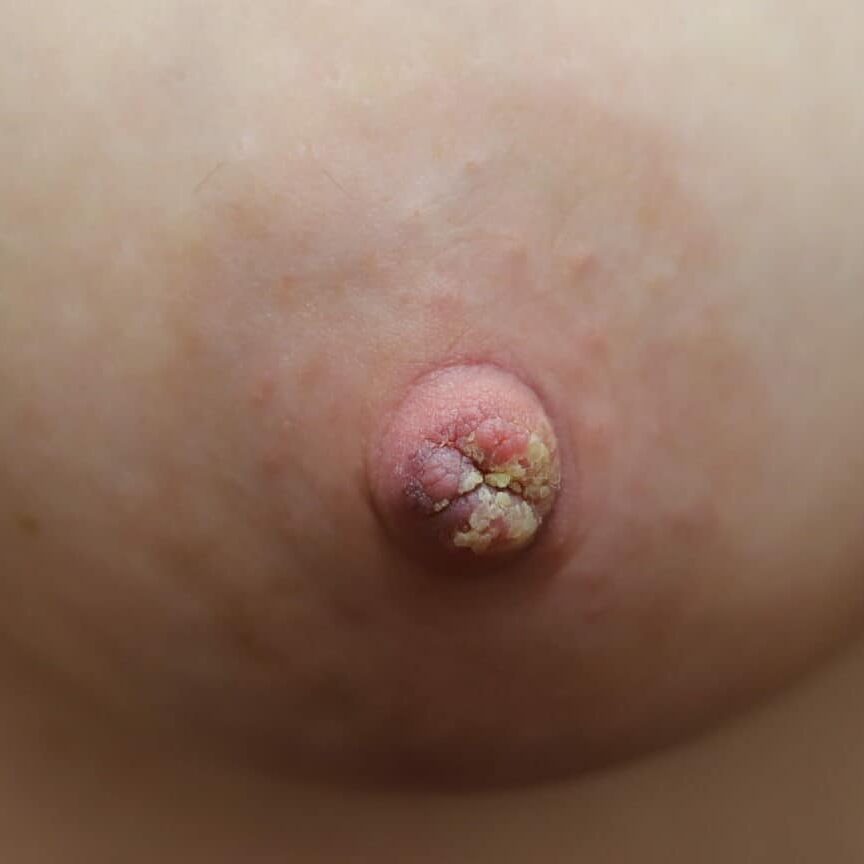
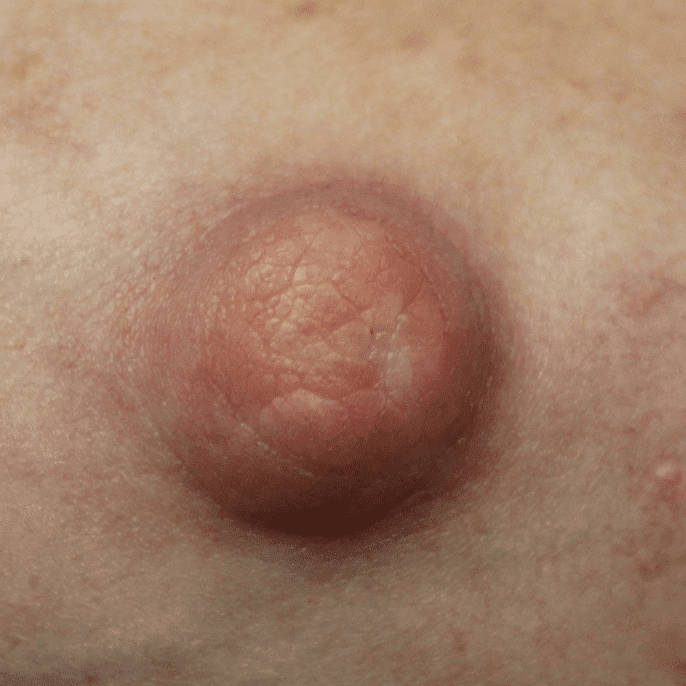
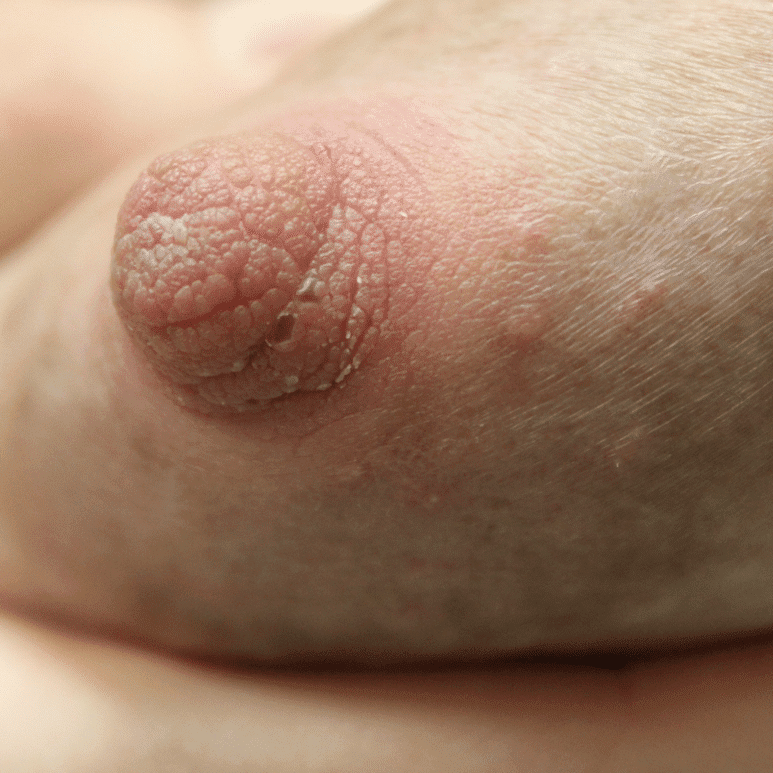
Hyperkeratosis ("Warty Nipple")
Hyperkeratosis is a thickening of the stratum corneum, the outer layer of skin, and is usually associated with an abnormal quality of keratin. Breastfeeding is possible with hyperkeratosis.
To reduce the thickening prior to breastfeeding, pregnant women should utilize a keratolytic moisturizer (containing urea or lactic acid) or calcitrene (a synthetic derivative of vitamin D). Crryotherapy, and topical steroids represent alternate treatment strategies. Laser therapy is definitive, and should be considered in more severe cases as repeated latching or pumping can cause frequent skin shedding and hypersensitivity on underlying raw tissue.
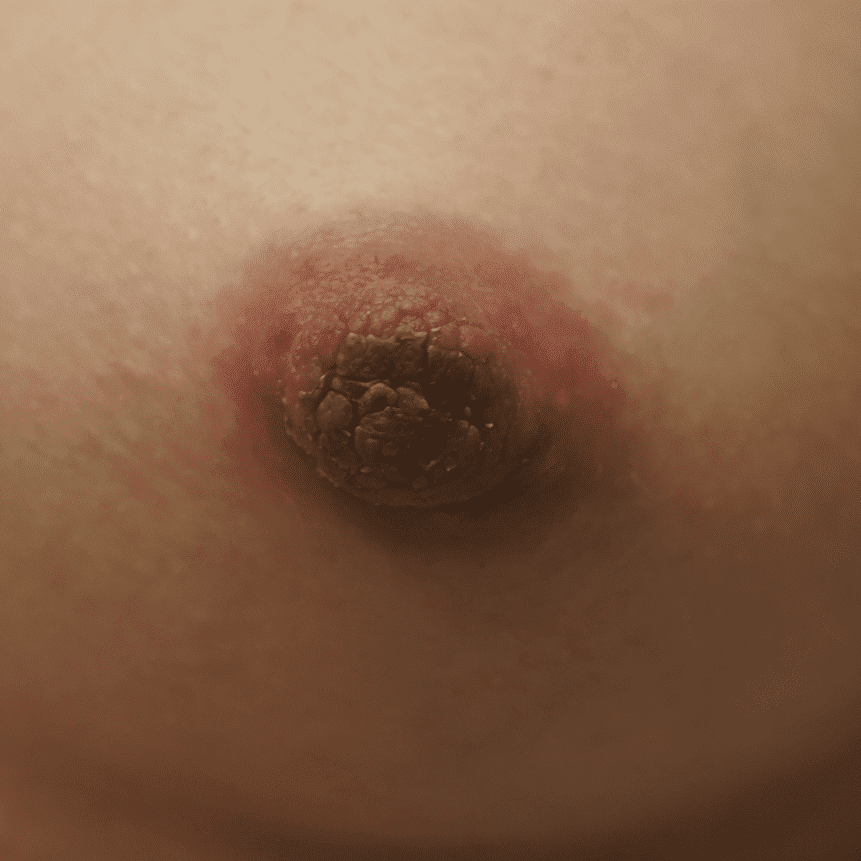





Lactiferous Sinuses
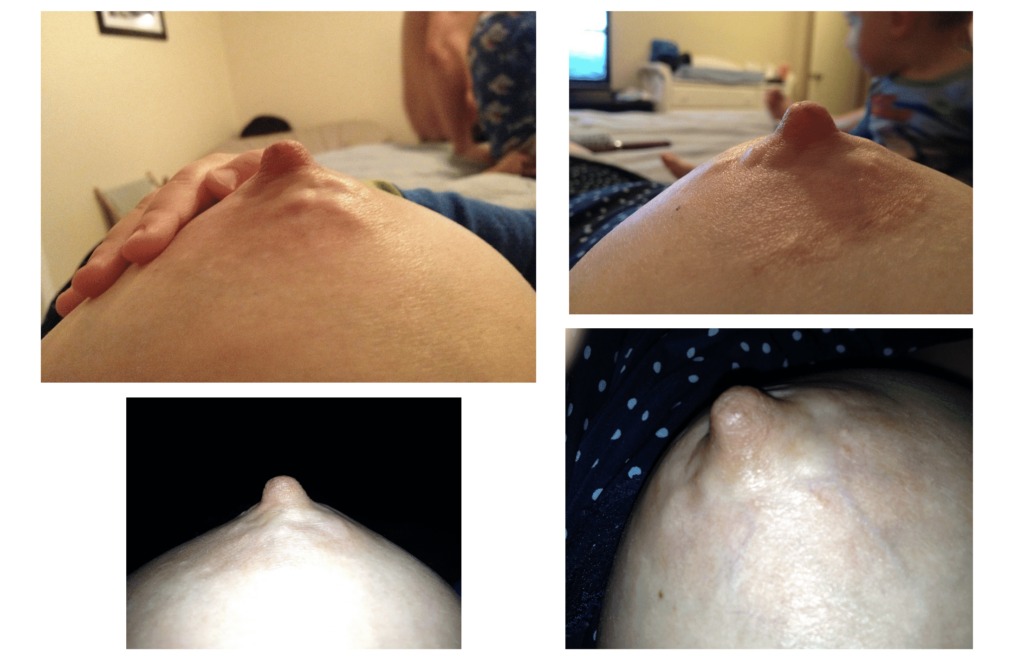

There is no subcutaneous fat behind the areola, so it is common to see dilation of ductal tissue and for patients to even worry they have a mass in this region. If a patient feels a persistent mass in this area, she should undergo physical exam and imaging evaluation.
Leiomyoma
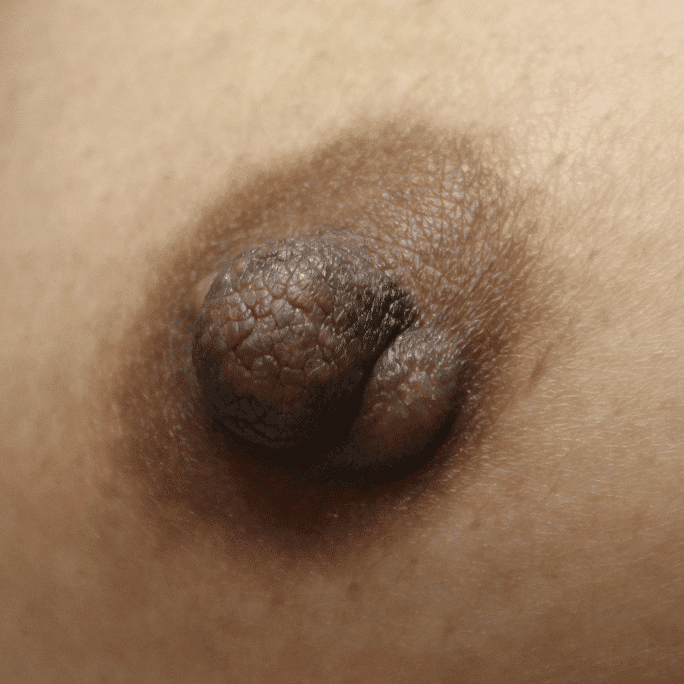
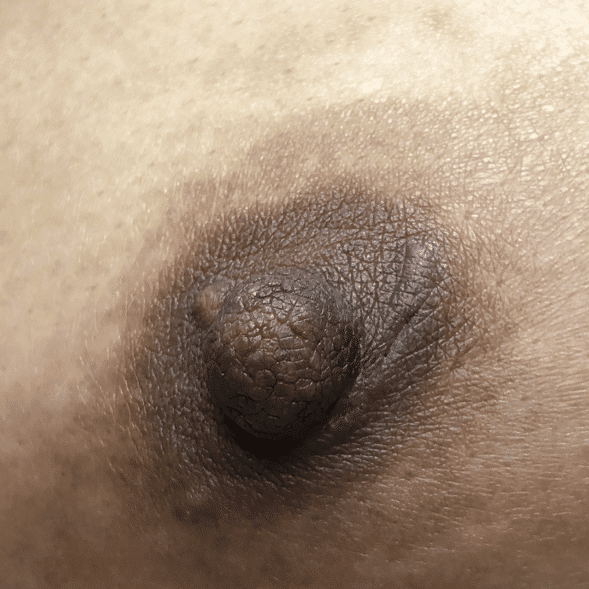
Leiomyoma, a benign tumor comprised of smooth muscle cells, rarely occurs on the breast. When leiomyoma does occur, it most often occurs on the areola, due to the presence of smooth muscle fibers. Like other lesions on the nipple areolar complex, larger leiomyomas may interfere with latch, and treatment is excision. They rarely recur.


Milk after Weaning
Continued milky discharge (galactorrhea) after weaning is normal if the breast continues to receive any kind of stimulation from squeezing or sexual activity. Even without stimulation, milk production can take several months to fully stop, based on overall duration of breastfeeding and level of milk production. If you do notice new onset significant milk production from both breasts without stimulation after complete weaning for at least several months, this should be investigated with a medical professional. Your prolactin level and thyroid can be tested. If prolactin is elevated in combination with new headaches or vision changes, this could indicate the presence of an uncommon pituitary tumor. Some psychiatric medications also can cause milky discharge.
Montgomery Glands
Montgomery glands are sebaceous (oil producing) glands on the surface of the areola, and are naturally enlarged in pregnancy and lactation. Like other sebaceous glands, they can become blocked and develop pain and a pimple-like appearance. If this occurs, use gentle soap and water, warm compresses to promote opening of the skin for drainage, and an acne cream like salicylic acid or benzyl peroxide that you should wipe off before breastfeeding.
Lubrication of pump flanges with coconut oil is a frequent reason why patients are more commonly developing Montgomery gland blockages. A pump should be comfortable without lubrication, and lubrication often allows women to turn the suction higher than what was intended. If lubrication must be used, it should be wiped off after pumping to decrease the risk of Montgomery Gland obstruction.
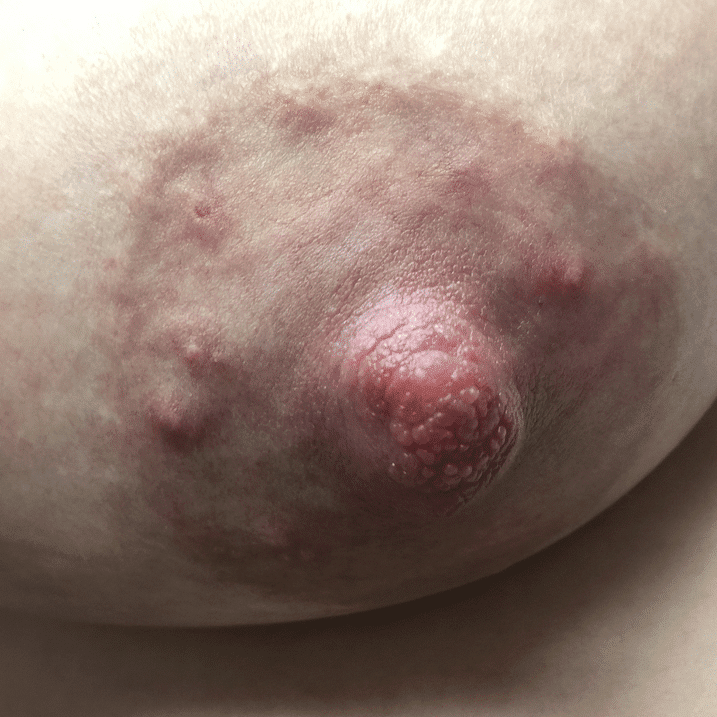
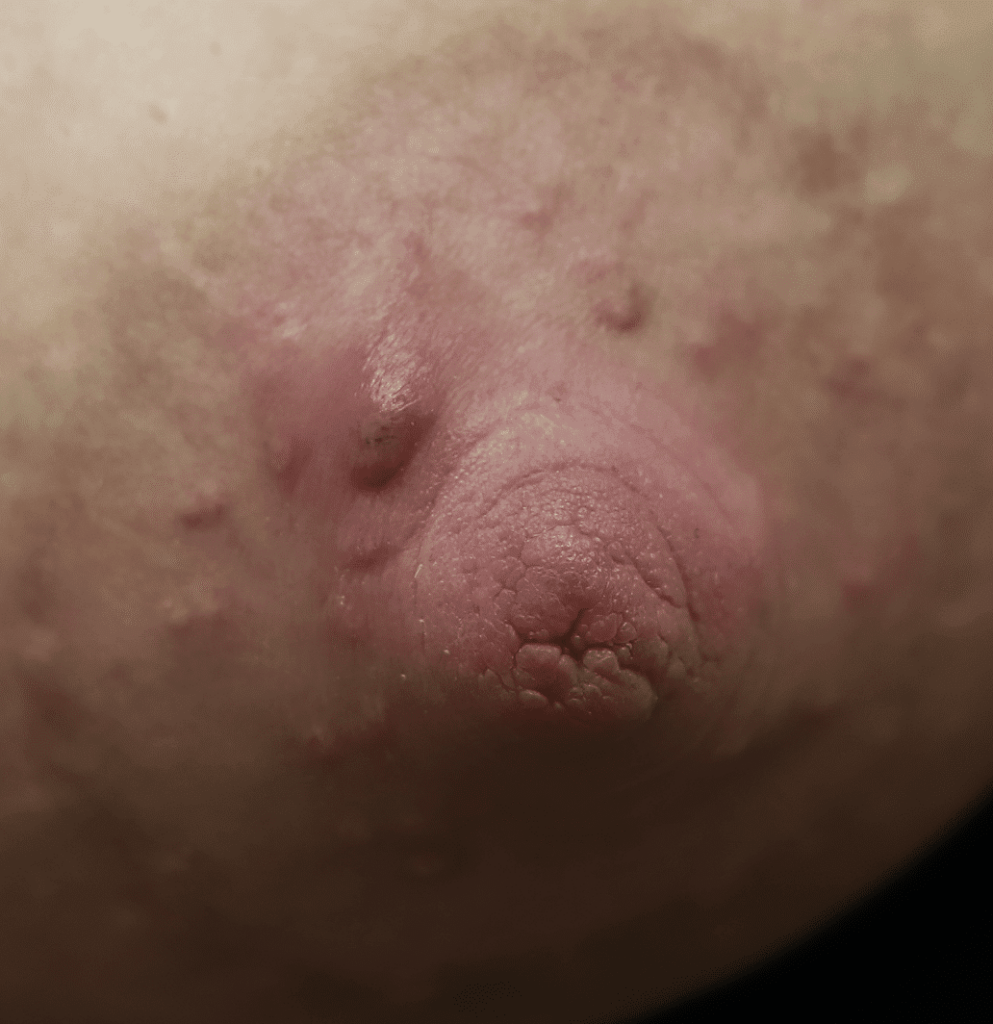
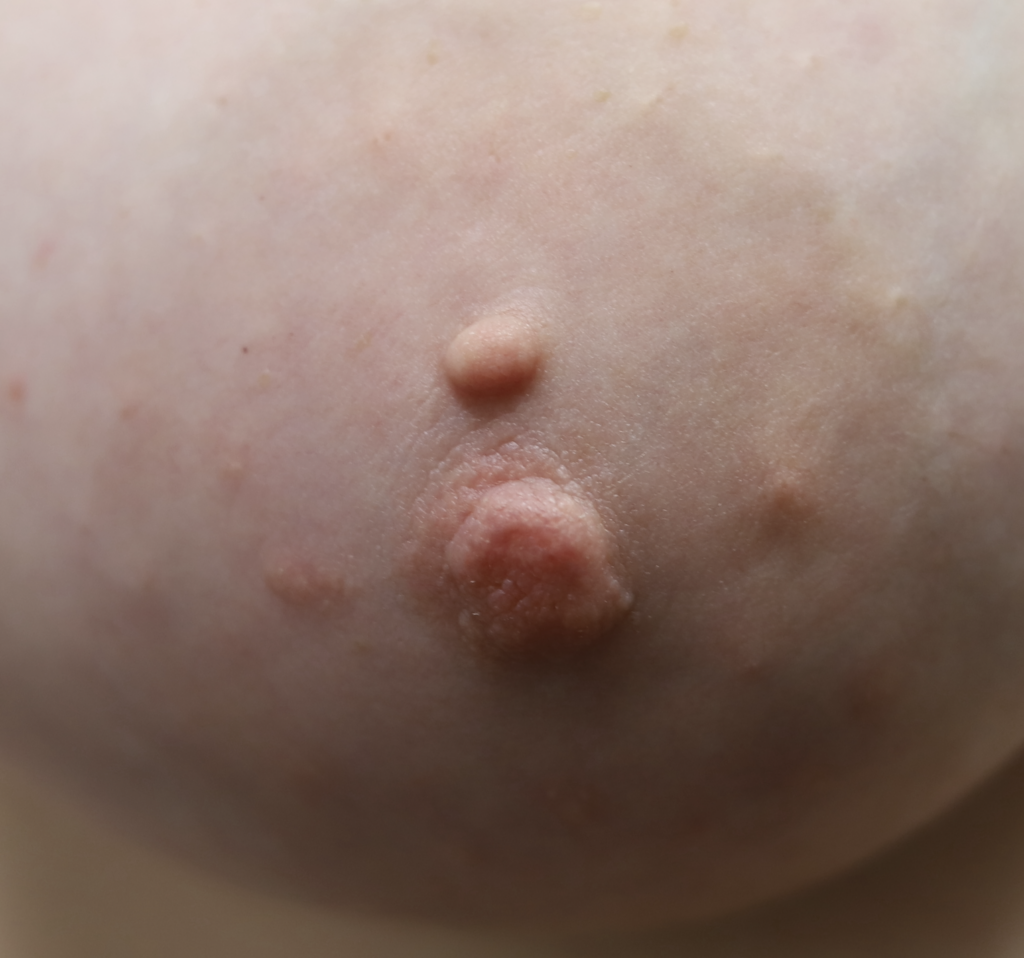
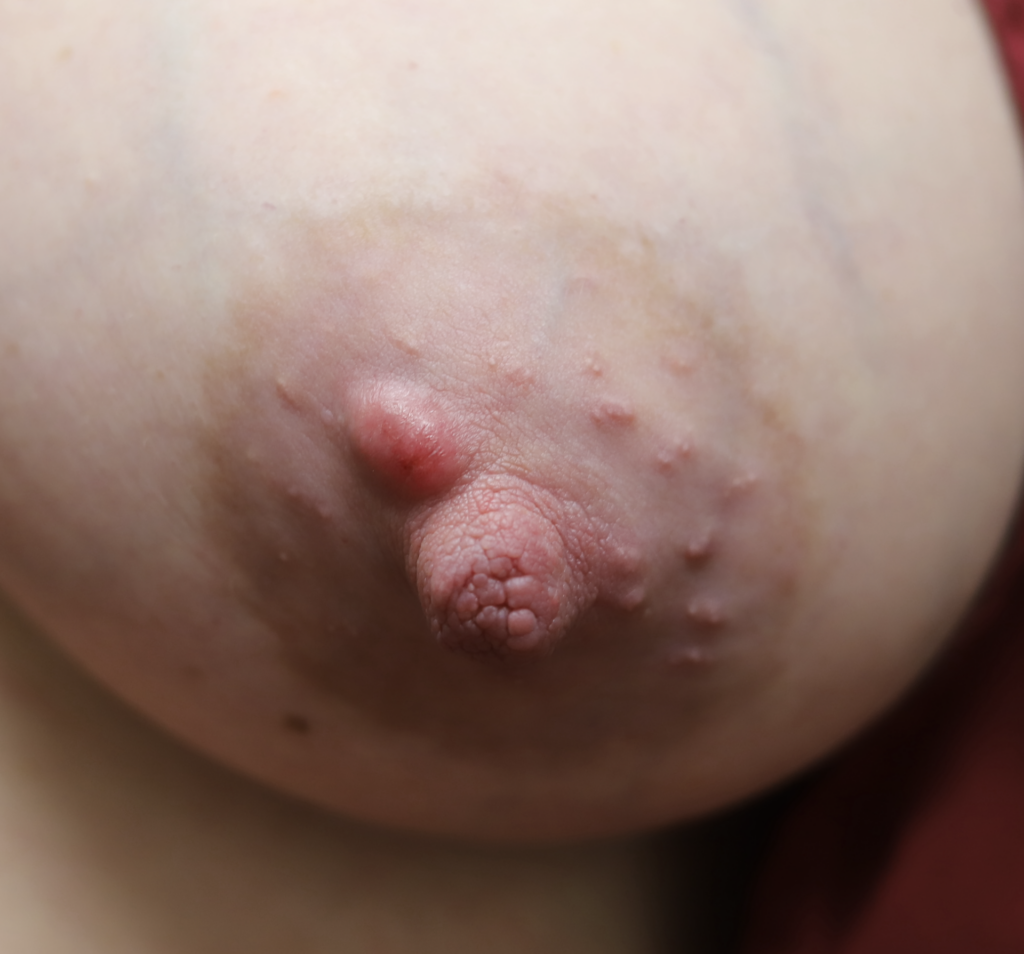

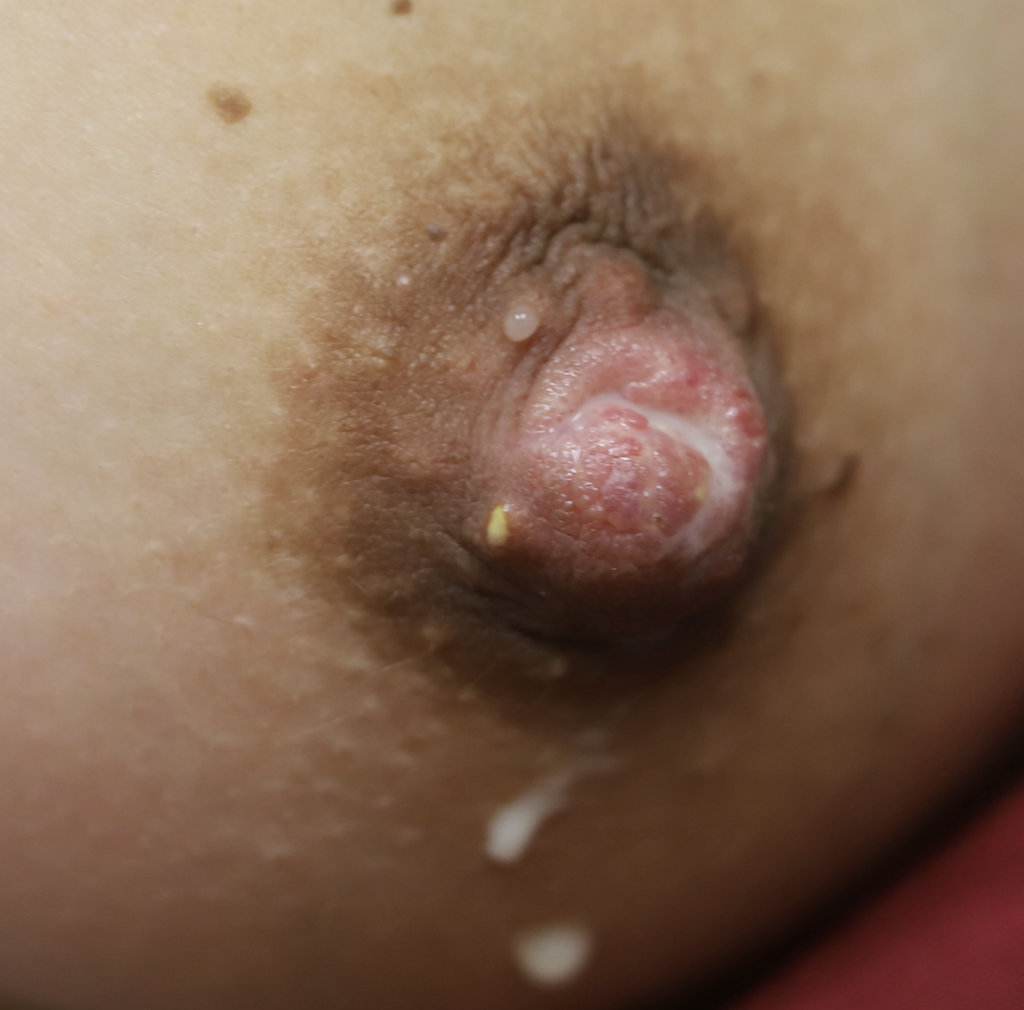
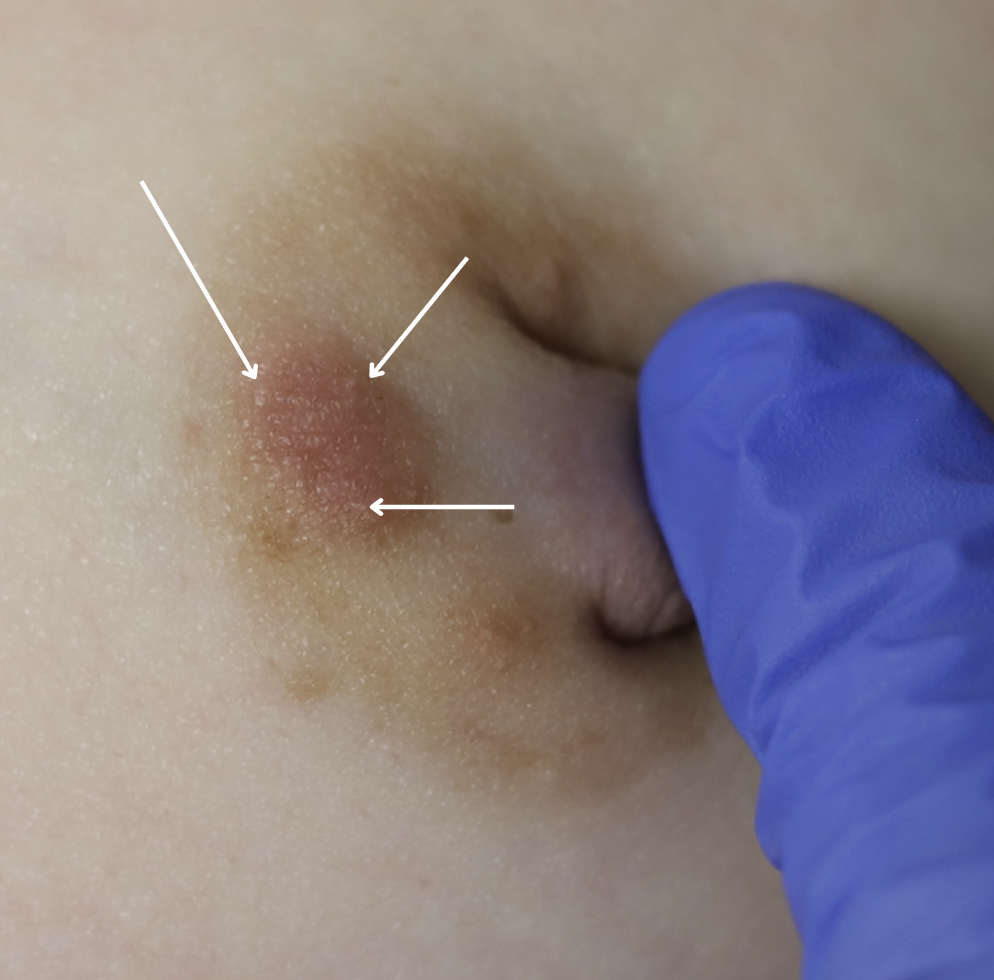
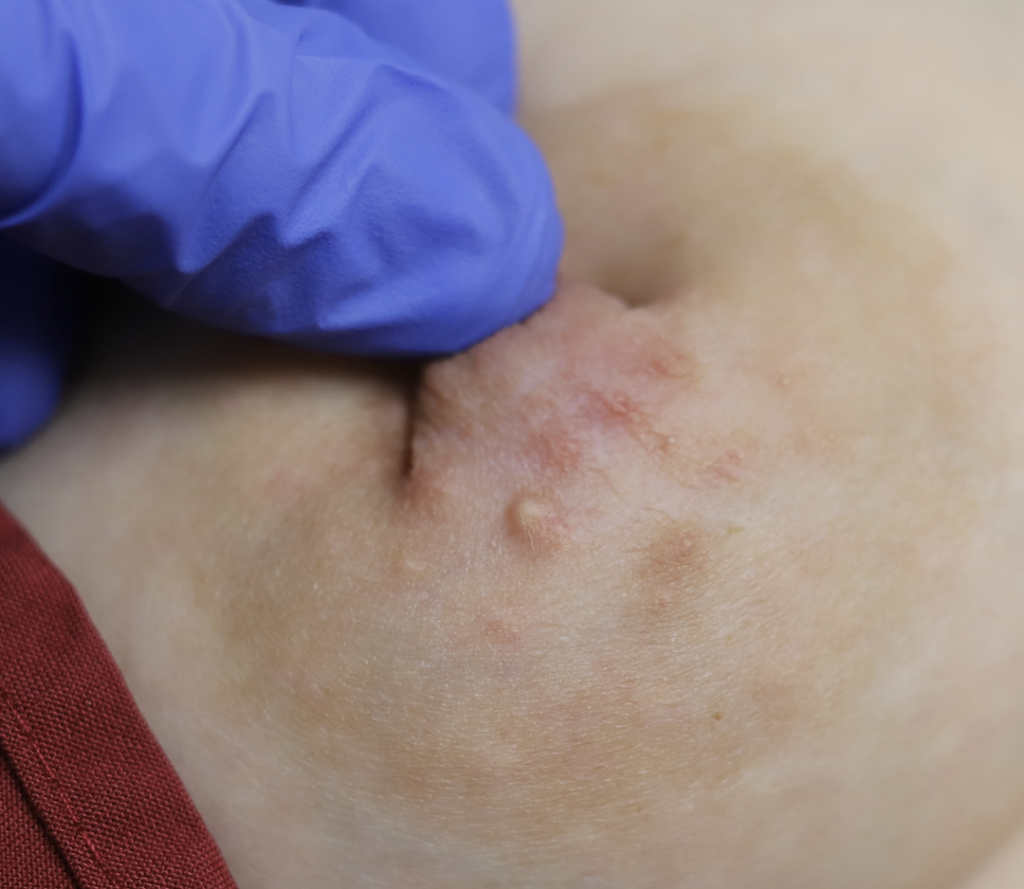
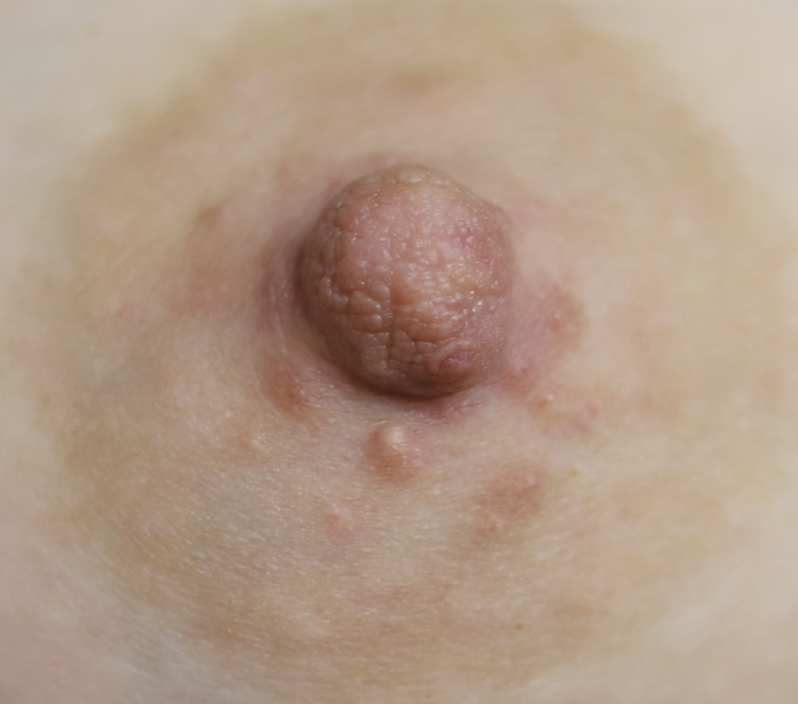
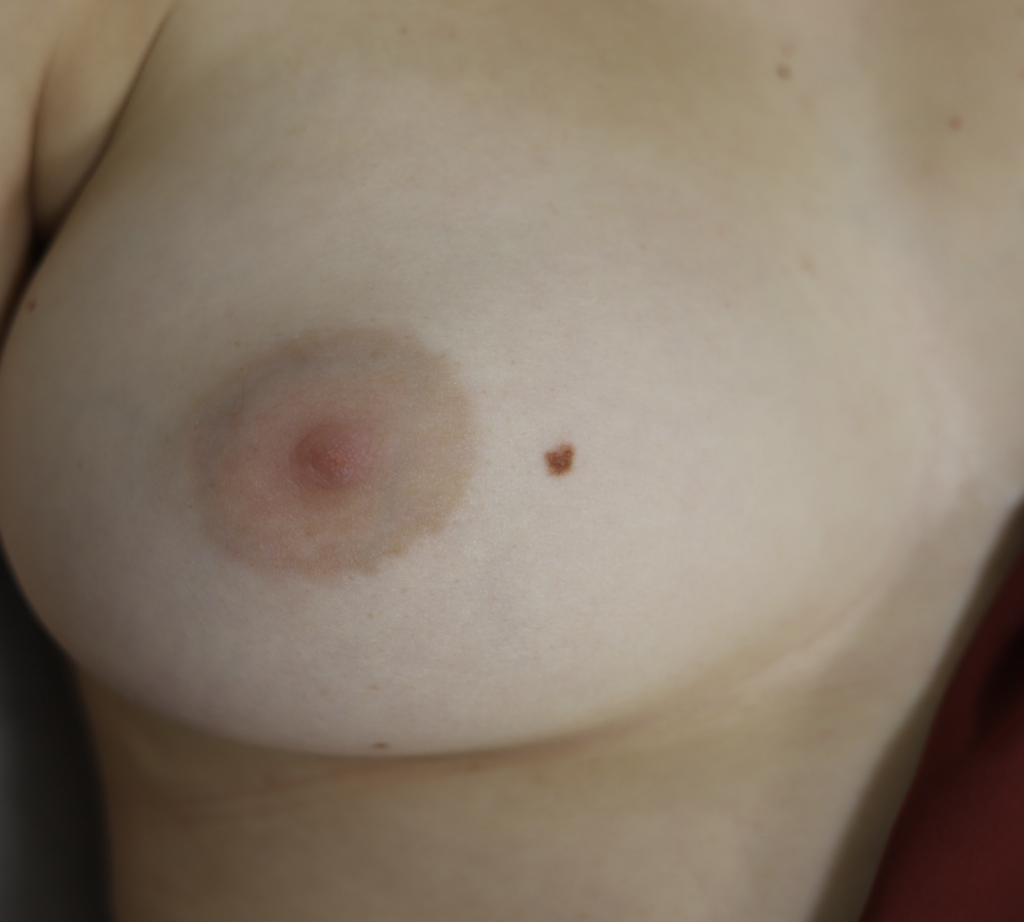
Nevi (Moles) and Seborrheic Keratoses
Lentigo and seborrheic keratosis commonly occur around the nipple areolar complex and breast and do not present difficulty with breastfeeding. Any concerning or changing lesions should be referred for dermatologic evaluation.
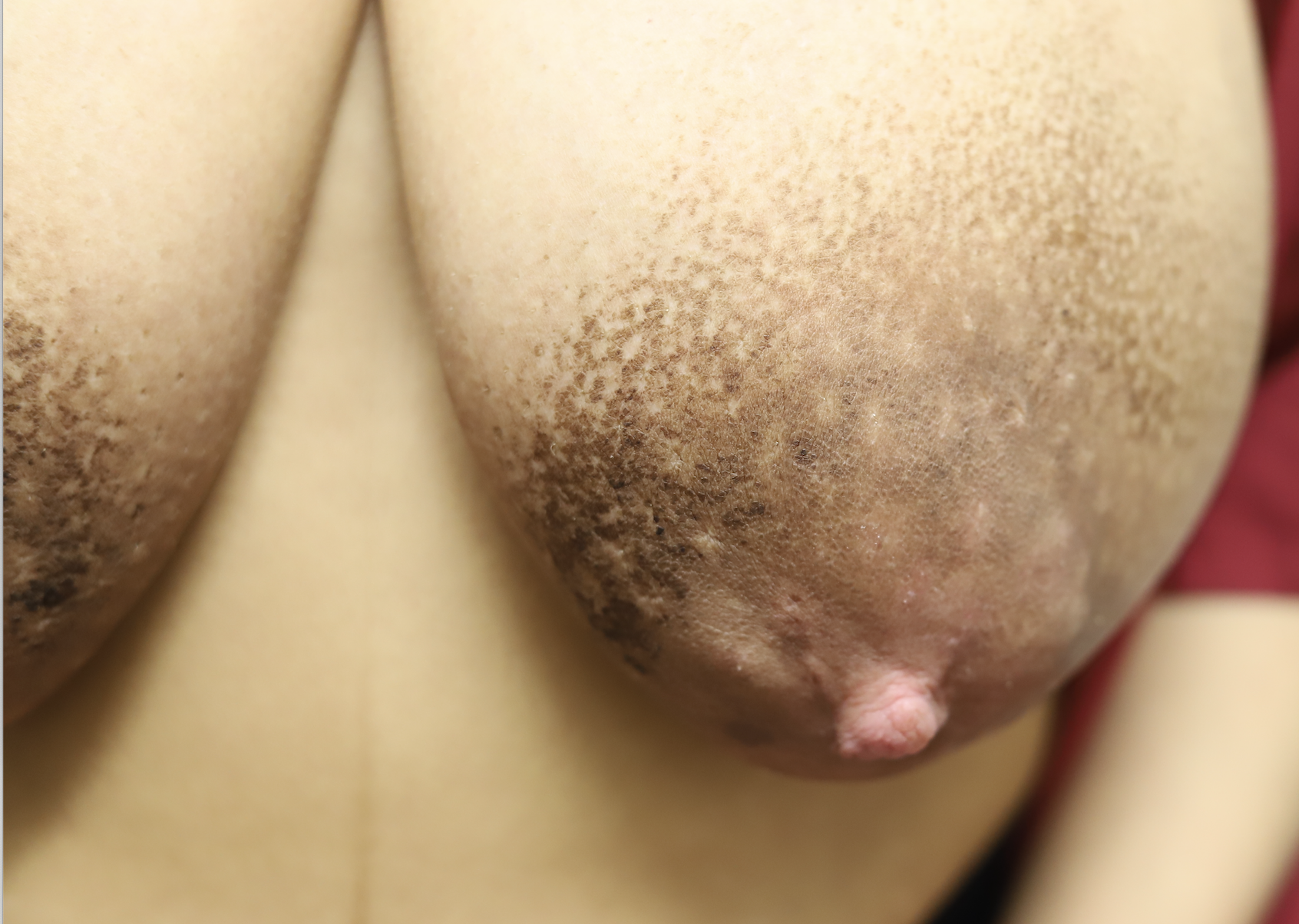 Seborrheic keratosis that developed on both breasts during pregnancy.
Seborrheic keratosis that developed on both breasts during pregnancy.
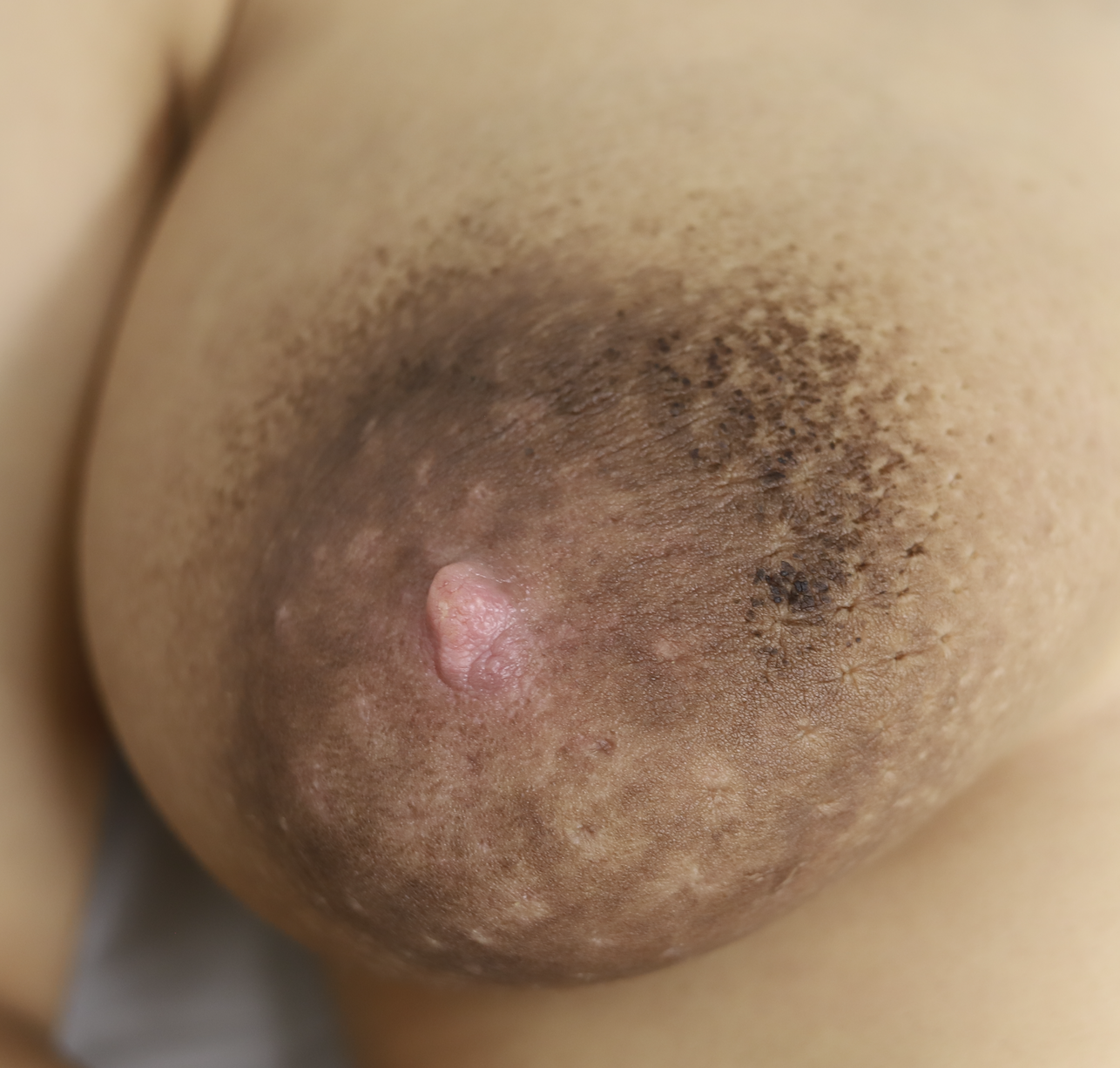 Right areola seborrheic keratosis
Right areola seborrheic keratosis
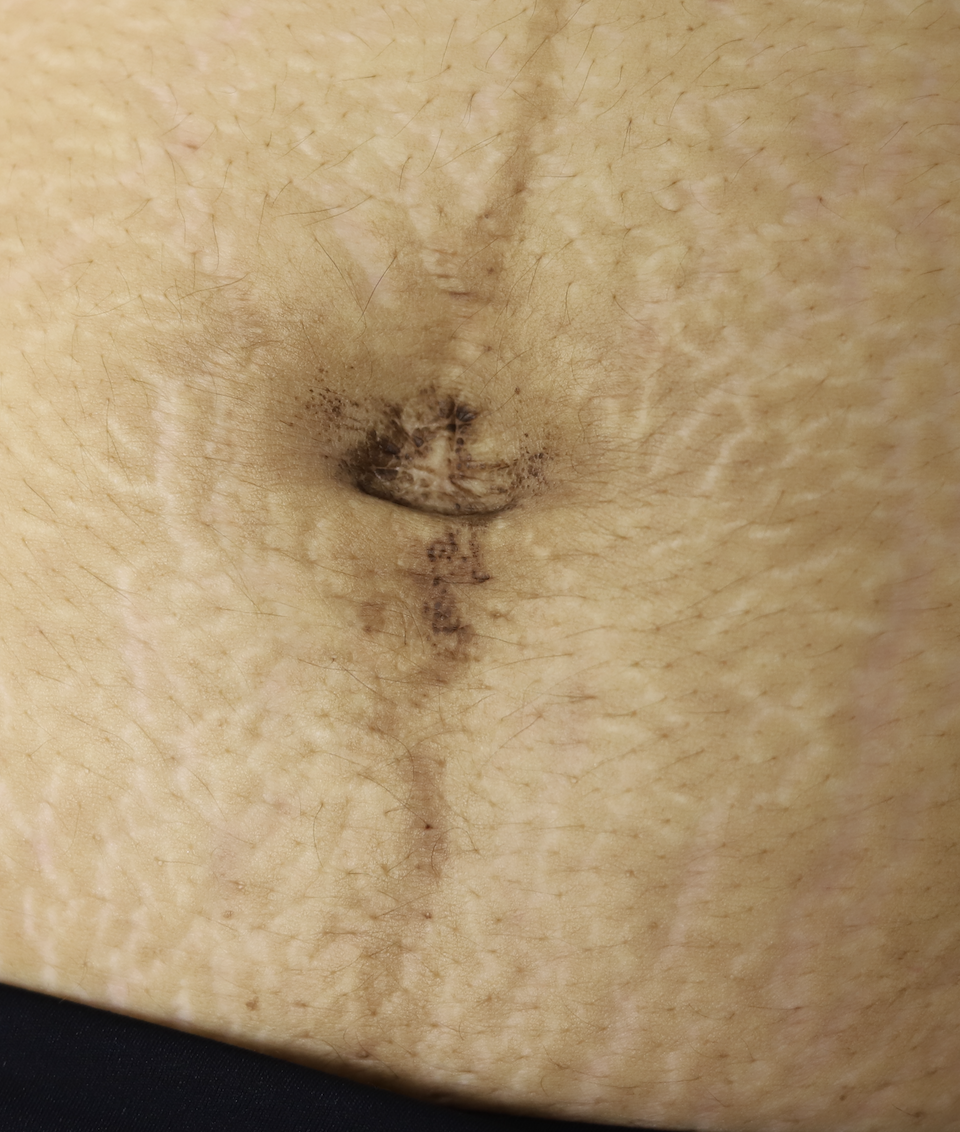 She also developed SK in her umbilicus.
She also developed SK in her umbilicus. Pinpoint seborrheic keratosis on face of nipple and just medial to base.
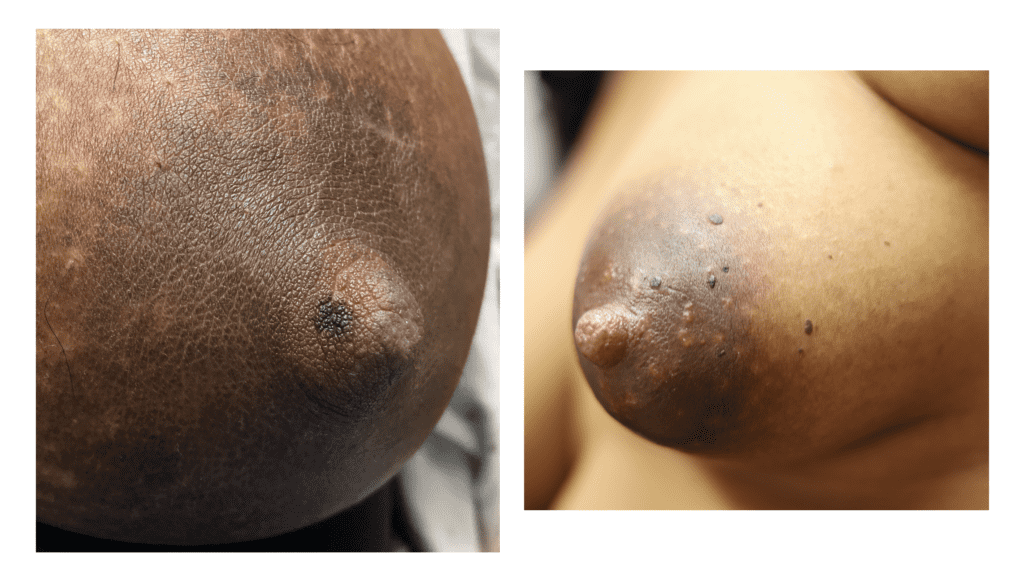
Pinpoint seborrheic keratosis on face of nipple and just medial to base.
 Seborrheic keratosis on areola during pregnancy.
Seborrheic keratosis on areola during pregnancy.
 Seborrheic keratosis at areola edge, 1:00 position and two smaller ones just below it on areola.
Seborrheic keratosis at areola edge, 1:00 position and two smaller ones just below it on areola.
 Seborrheic keratosis at 10:00, 12:00, 1:00, and 2:00 at junction of depigmentation area of areola and intact areola. Normal Montgomery Glands at 3:00 closer to the nipple in depigmentated area.
Seborrheic keratosis at 10:00, 12:00, 1:00, and 2:00 at junction of depigmentation area of areola and intact areola. Normal Montgomery Glands at 3:00 closer to the nipple in depigmentated area.
 Seborrheic keratosis on neck developing during pregnancy.
Seborrheic keratosis on neck developing during pregnancy.
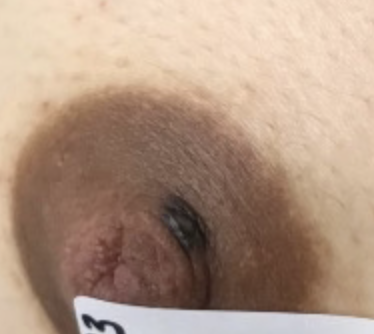
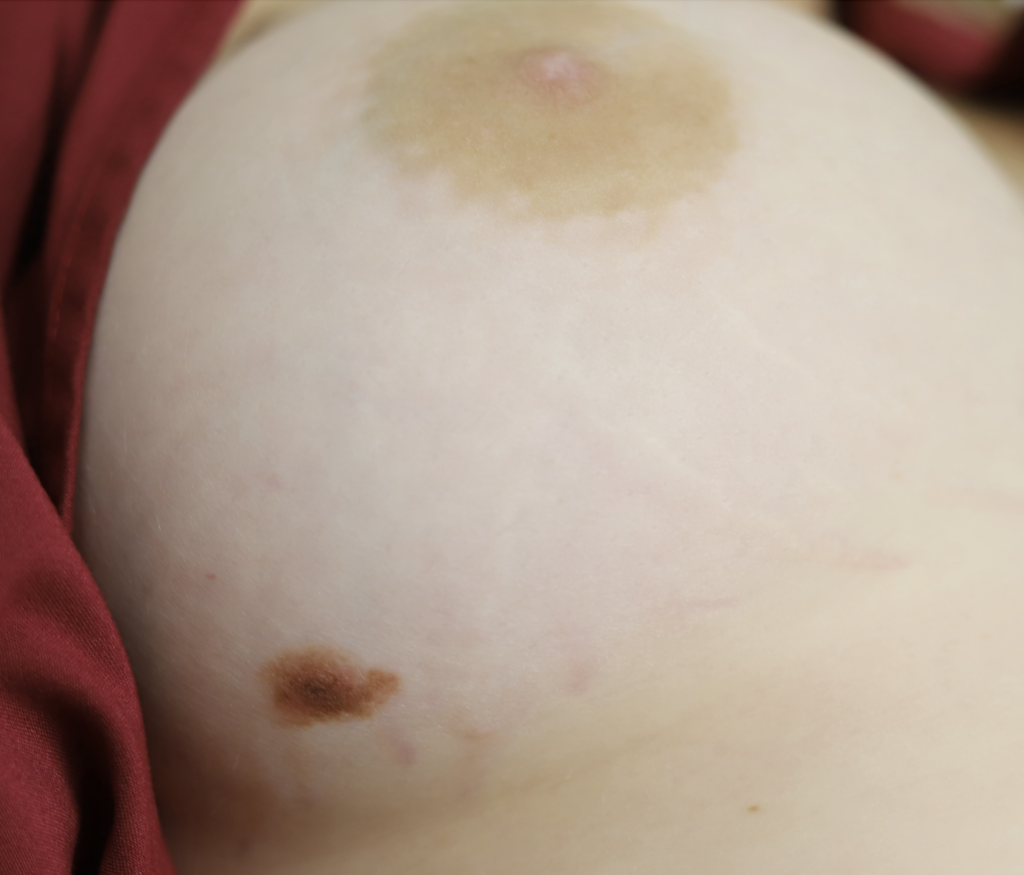
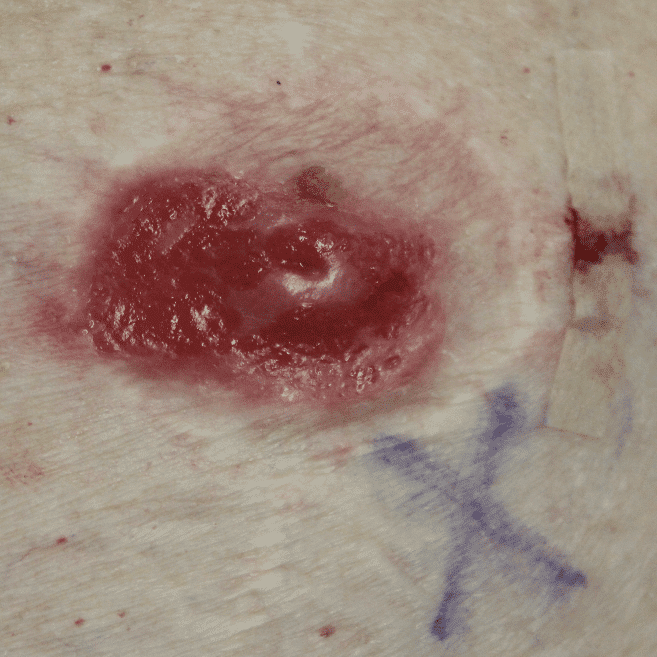
Above: atypical mole that became more raised, irregular, and changed pigmentation during pregnancy and postpartum. A dermatologist performed a shave biopsy for diagnosis of whether it was atypical or melanoma. The third photo is after excision during lactation. Because of the size of the incision and potential for it to open up and breakdown, we had mom downregulate this breast and upregulate her other breast. She exclusively breastfed from the other breast until this completely healed. She then resumed feeding and increased production from there.
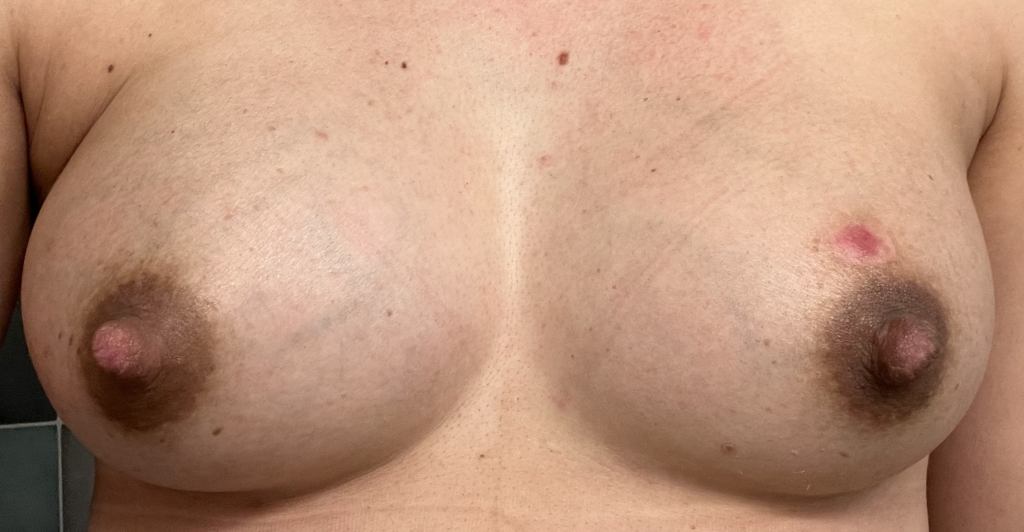
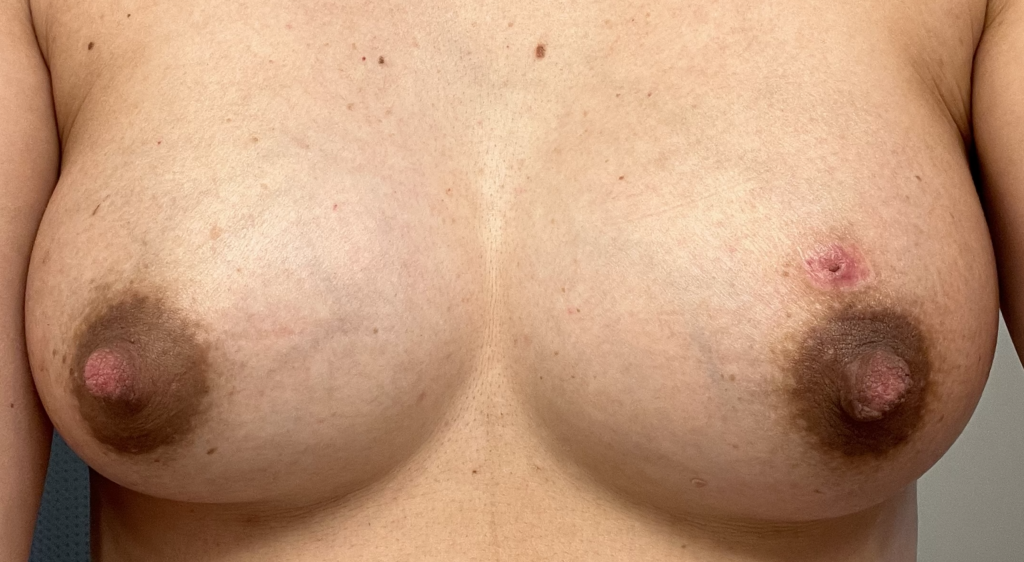
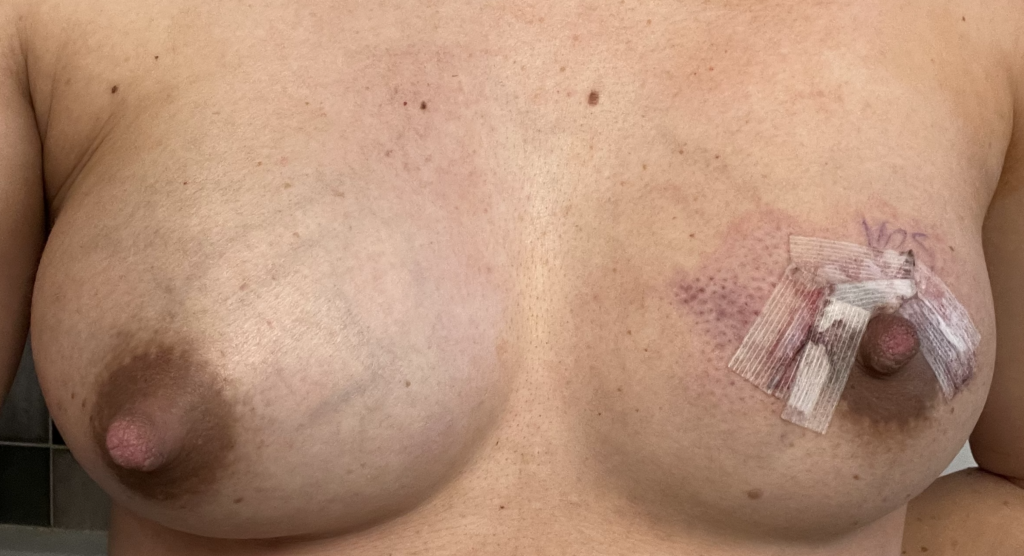
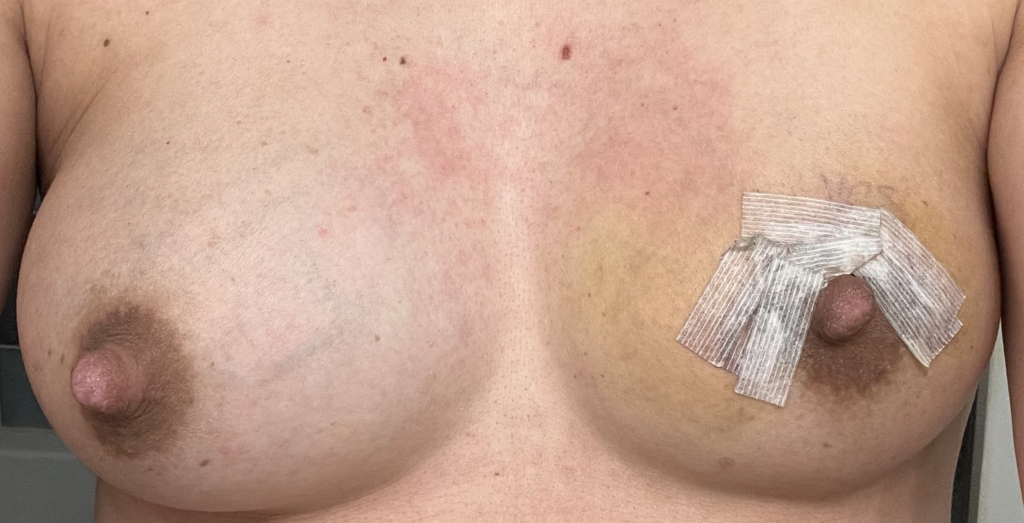
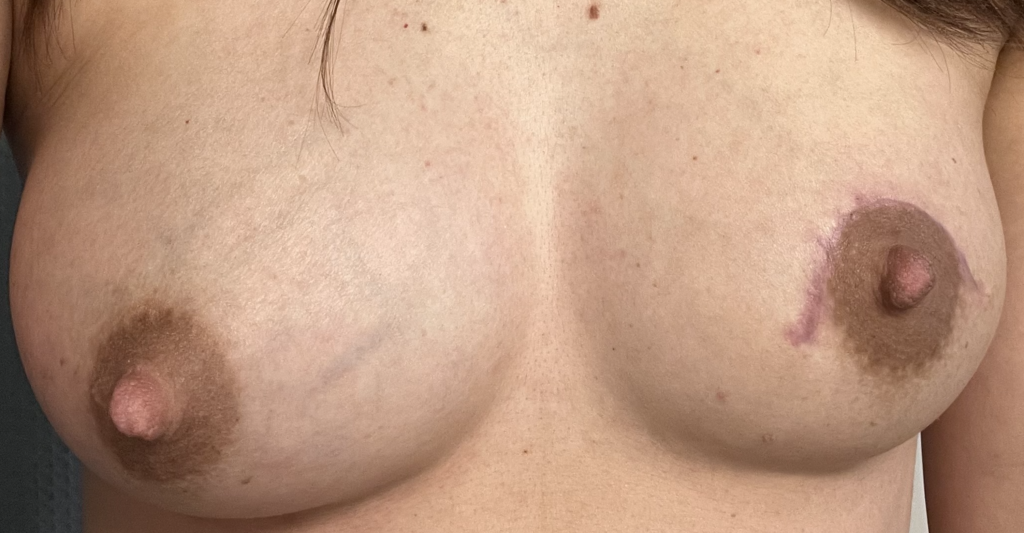
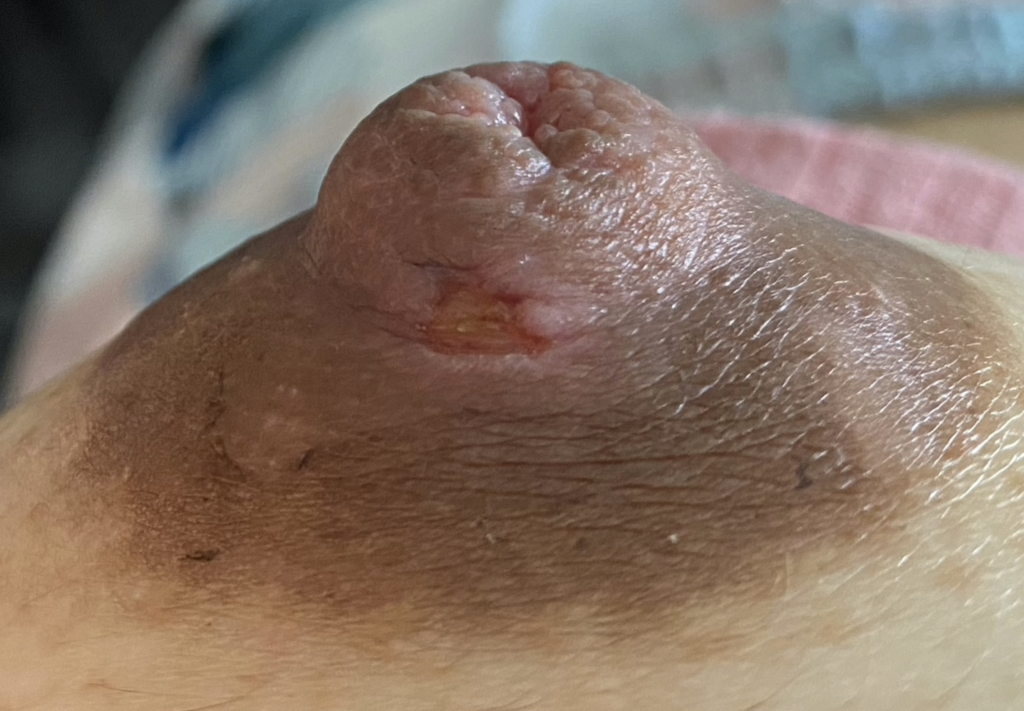
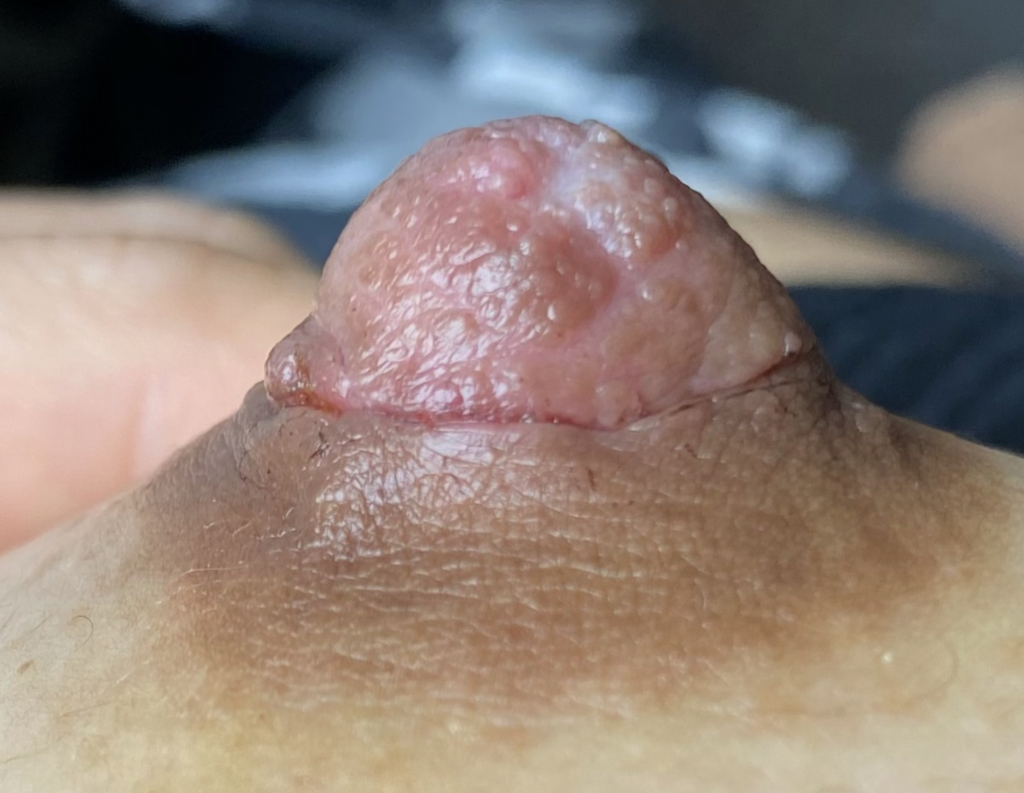
Left breast melanoma (top photo showing patient healing after shave biopsy by dermatologist, then last three showing her post-operative course after formal surgical resection by surgical oncologist. She was able to continue feeding exclusive breastmilk from the right breast during this time, and you can see how much her breasts changed sized to accommodate.
Nipple Crust
Many women who exclusively pump without breastfeeding may develop a white crust on their nipples. This may be dried milk, or may be related to biofilm production. Researchers have documented the variation in milk microbiome that occurs with exclusive pumping, and it is possible this crust is related to that phenomenon. While further research is necessary in this area, vigorous cleaning and/or attempts to remove this crust should be avoided as these interventions can produce nipple trauma and scarring.
Pain
Causes of pain during breastfeeding can range widely, and moms and babies should be evaluated together, with a differential diagnosis (potential causes) formulated based on their history, exam, and time postpartum.
Some moms have initial struggles “learning to breastfeed” in the early postpartum period with engorgement and simply needing to adjust position to enable a comfortable latch. Other pain can result from situations that require medical management such as treatment of hyperlactation (“oversupply”), blebs, and dermatitis.
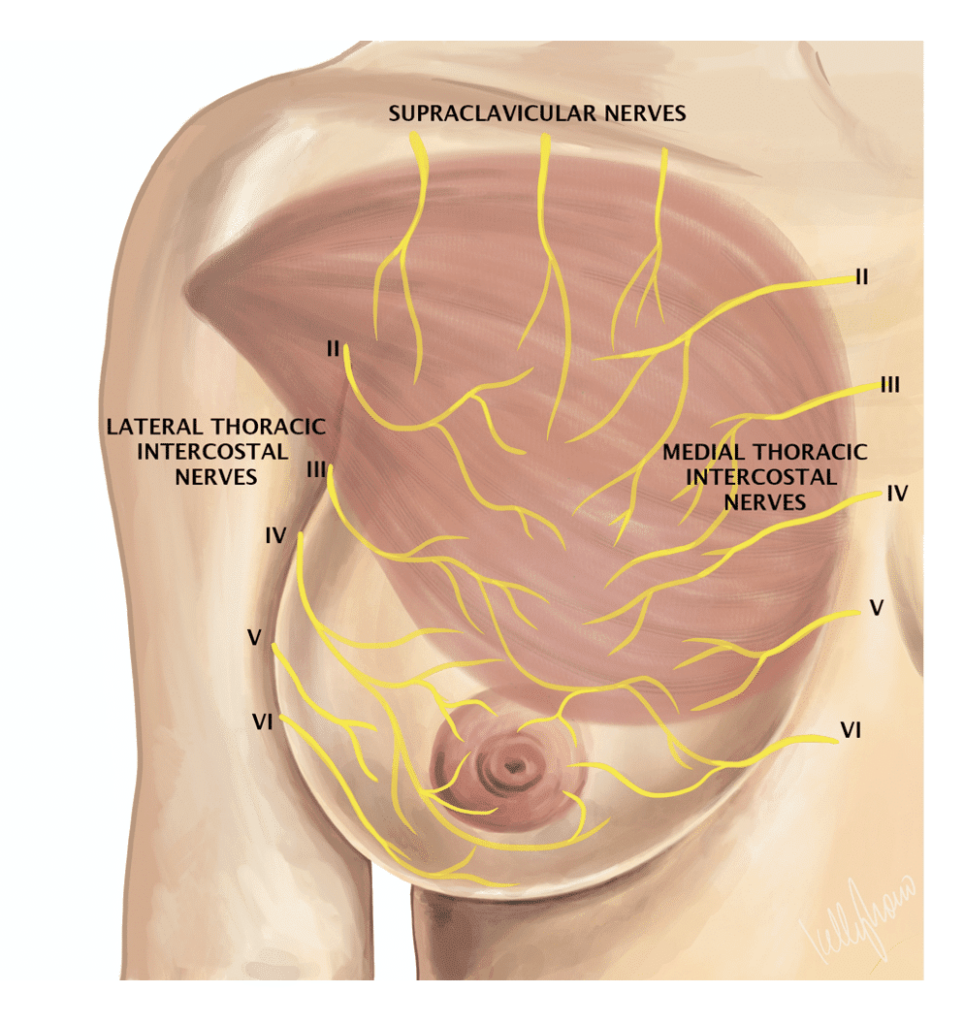
Because of the complex innervation of the nipple, deeper breast pain may present as nipple pain or vice versa. If a mom resumes menstruation, she may notice increased breast and/or nipple sensitivity prior to her cycle. Pregnancy may also produce increased sensitivity. In general, the most common causes of breast pain are outlined in the box below:
- Nipple Conditions
- Trauma/wounds (e.g. pump, infant latching to engorged breast)
- Vasospasm (changes in blood flow that impact the nipple and breast)
- Dermatitis (allergy causing)
- Nipple bleb
- Neuropathic pain that responds well to the SSRI class of drugs
- Breast Conditions
- Engorgement
- Hyperlactation
- Mastitis
- Neuropathic pain that responds well to the SSRI class of drugs
- Hormonal fluctuations with menstruation or pregnancy
Wound Care
Surgeons learn wound care from day one of residency. Treatment and resolution can be quite complicated at times when wounds/injuries become chronic. However, the goal is to treat early and appropriately to avoid this. Basics of surgical wound care are listed here:

Trauma most commonly results from early postpartum engorgement, feeding too long from a breast that is producing too little milk, infants clamping to stop heavy flow from oversupply, and improperly fitting flanges or pump on high suction. Other causes include soaps, oils, ointments, lubricants that can cause dermatitis and subsequent skin breakdown.
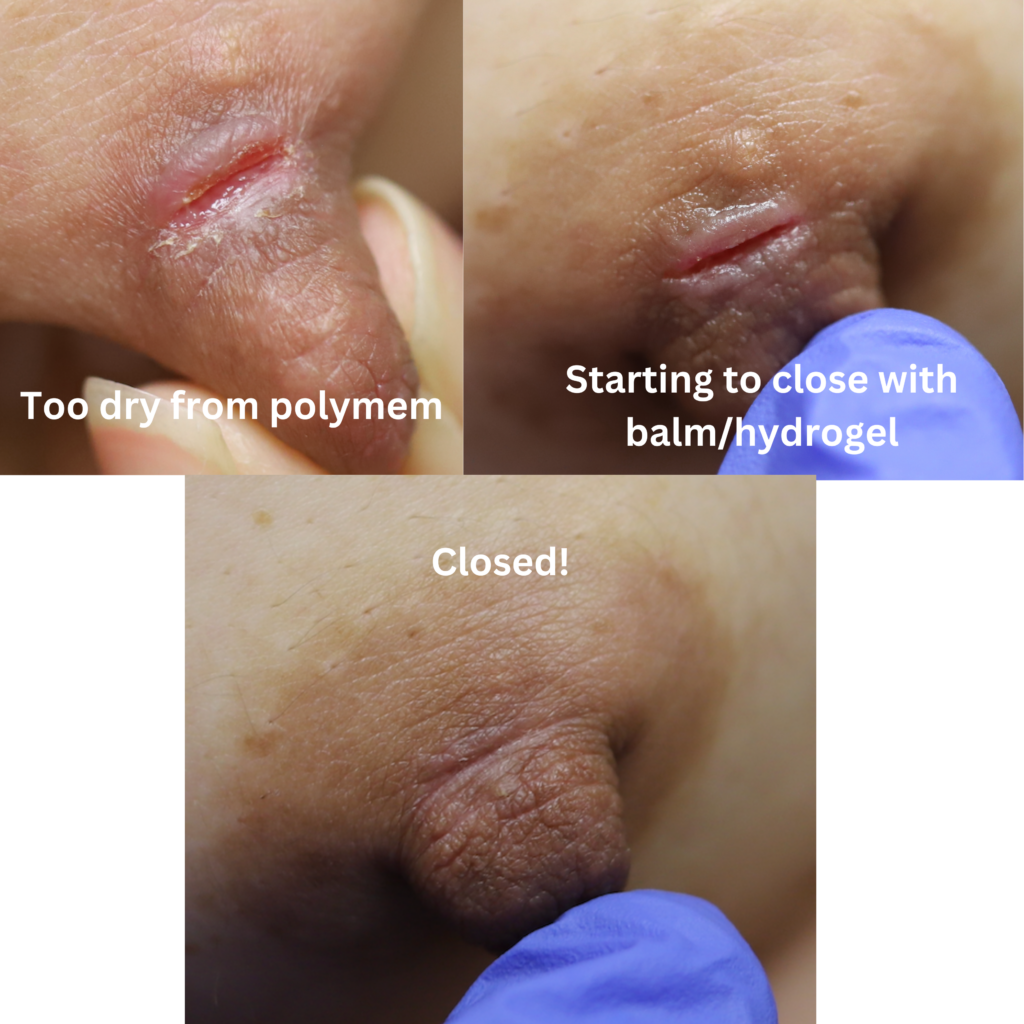
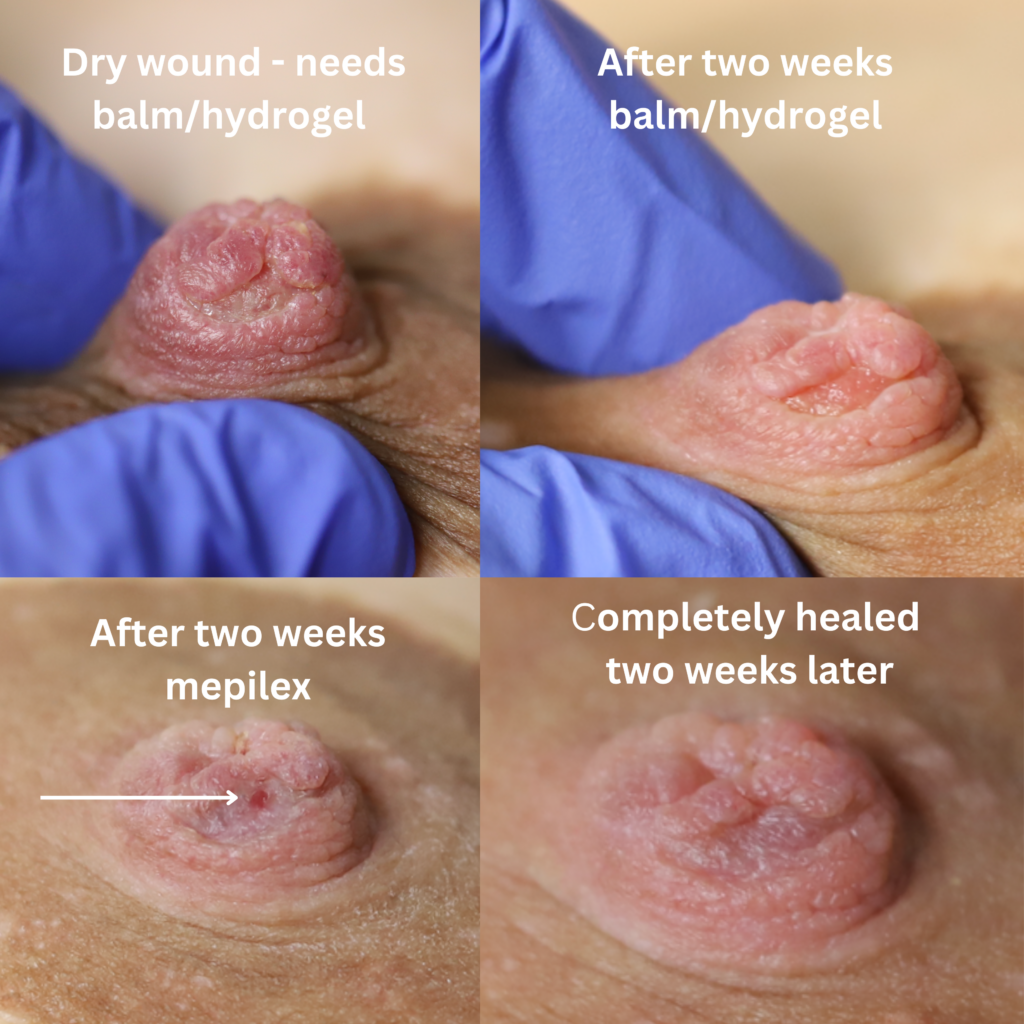
Nipple wounds should be lubricated and covered to heal effectively, just like burns or other open wounds on the body. An organic balm coupled with a hydrogel “soothie” pad to “close” the wound can be utilized. Moms should keep nipples covered both day and night to enable uninterrupted wound healing.
Excessive cleansing, whether prenatally or postpartum, can remove natural oils and predispose skin to breakdown. Care for the nipple like any other surface on your skin.
It should be noted that the product insert for hydrogels marketed to the lactation community recommends hydrogels be used without any additional ointment. However, surgical literature recommends the use of hydrogels as a wound dressing specifically for the reason that it “can easily be combined with various substances that facilitate wound healing and/or have anti-inflammatory properties.” If a patient has a deep wound or one in an area that the hydrogel won’t contact (e.g. a deep fissure), balm can work synergistically with the hydrogel to provide a moist environment.
If you are recommended to strictly follow the lactation product insert, then it would be preferential to use hydrogel alone rather than nipple balm alone. Hydrogel has important wound healing technology that facilitates more rapid resolution.
Normal human wound healing time is 8-10 days after traumatic insult if it’s a simple, superficial (not deep) wound. Some moms will question how nipple trauma can heal when an infant continues to stimulate the nipple frequently. The lactating breast and nipple areolar complex are highly vascular and therefore heal well, even in the setting of continued breastfeeding. In fact, continued breastfeeding promotes healing from the enzymatic action of the infant’s saliva as well as healthy bacterial exchange.
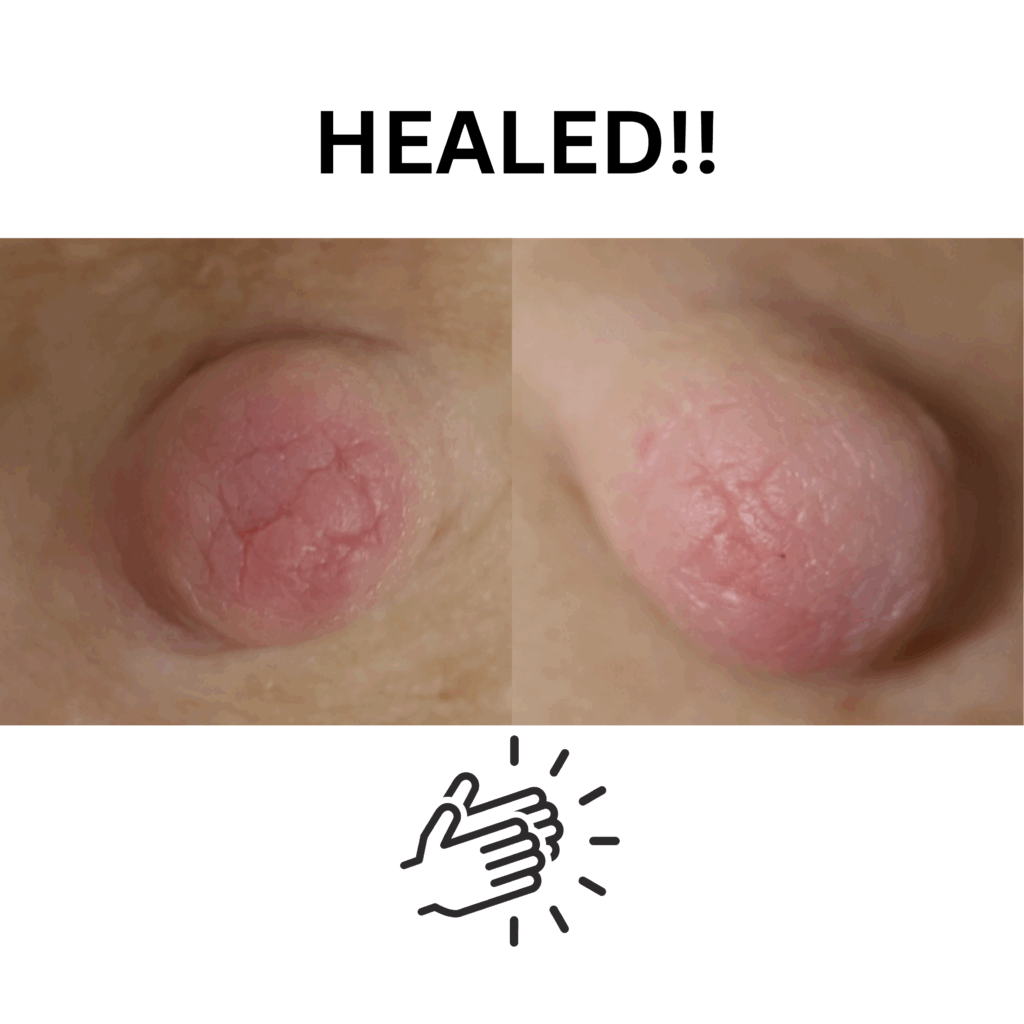
Below shows an example of healthy wound healing with continued breastfeeding. This did take longer to heal due to the depth of the tissue loss.
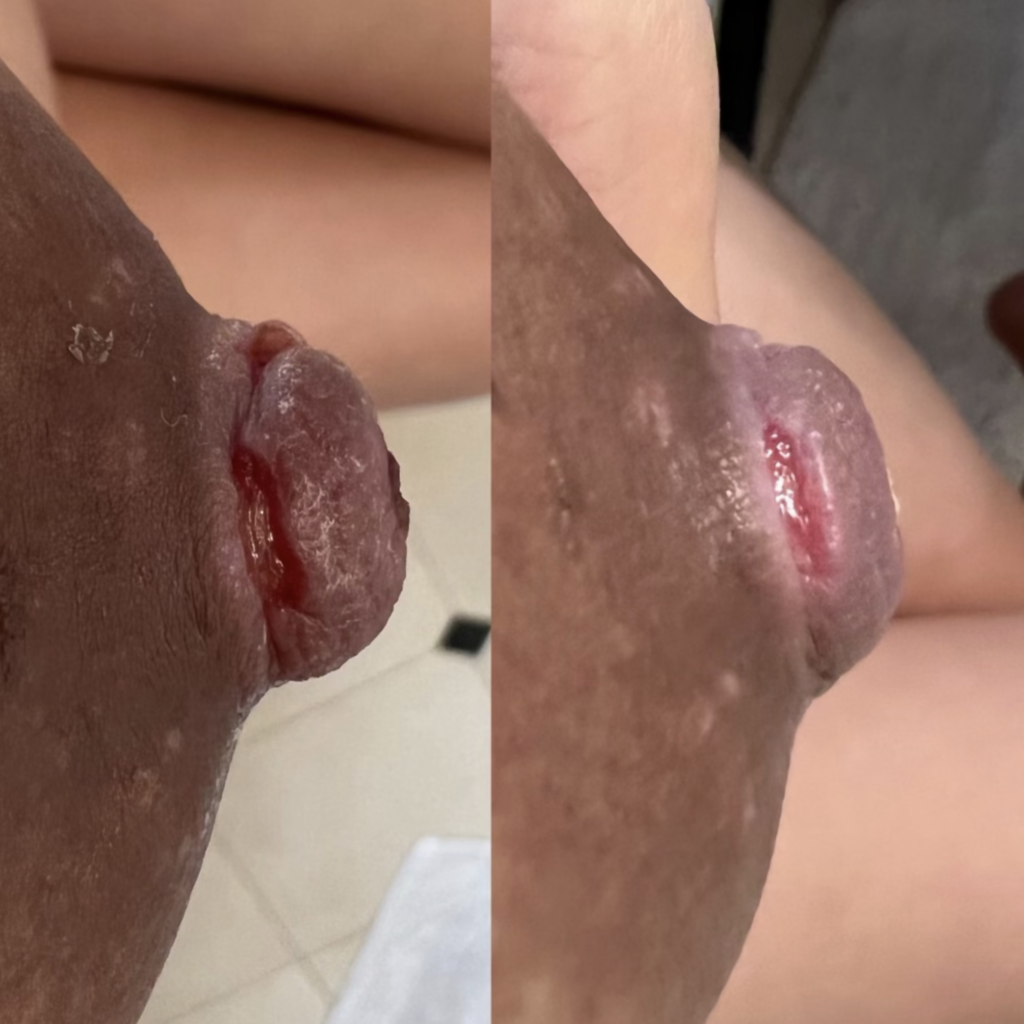
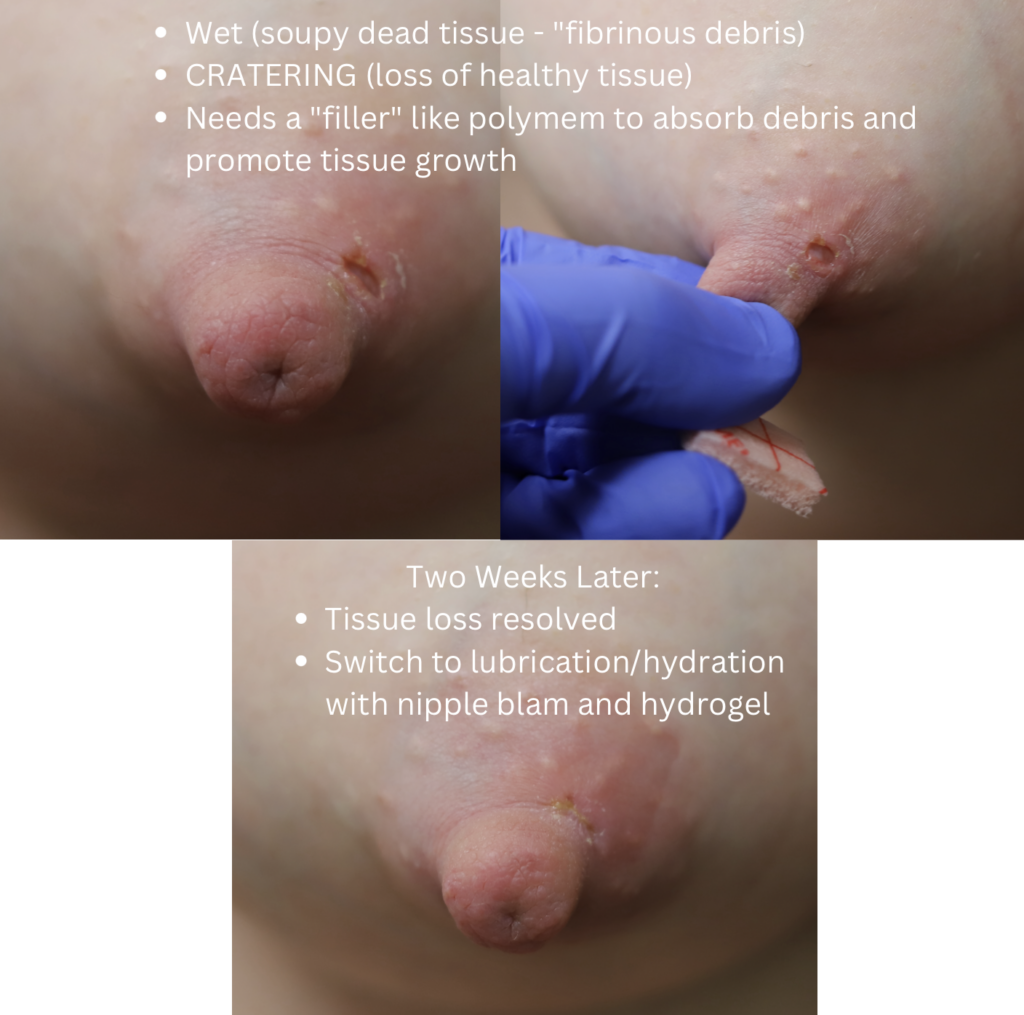
Significant trauma may result in deeper fissuring with the development of fluid seepage. Many women and healthcare providers incorrectly believe this fluid to be “infected.” This seepage is NOT infection. It is something called “fibrinous debris.” Surgeons commonly deal with these types of wounds in different parts of the body.
Wounds with significant seepage may benefit from polyurethane matrix pads (e.g. Nursicare) to provide both closed wound healing and absorptive capacity. Unlike hydrogel pads, polyurethane pads or mepilex should not be used with balm as the absorptive surface should contact the skin directly.
Some wounds respond well to medical-grade honey (Medi-Honey), which is irradiated and therefore does not pose risk of botulism to infants who may ingest small amounts.
Open wounds should not be closed with suture or surgical glue. Instead, these wounds should heal following principles of closure by secondary intention. Additionally, surgical glue may pose harm to the breastfeeding infant.





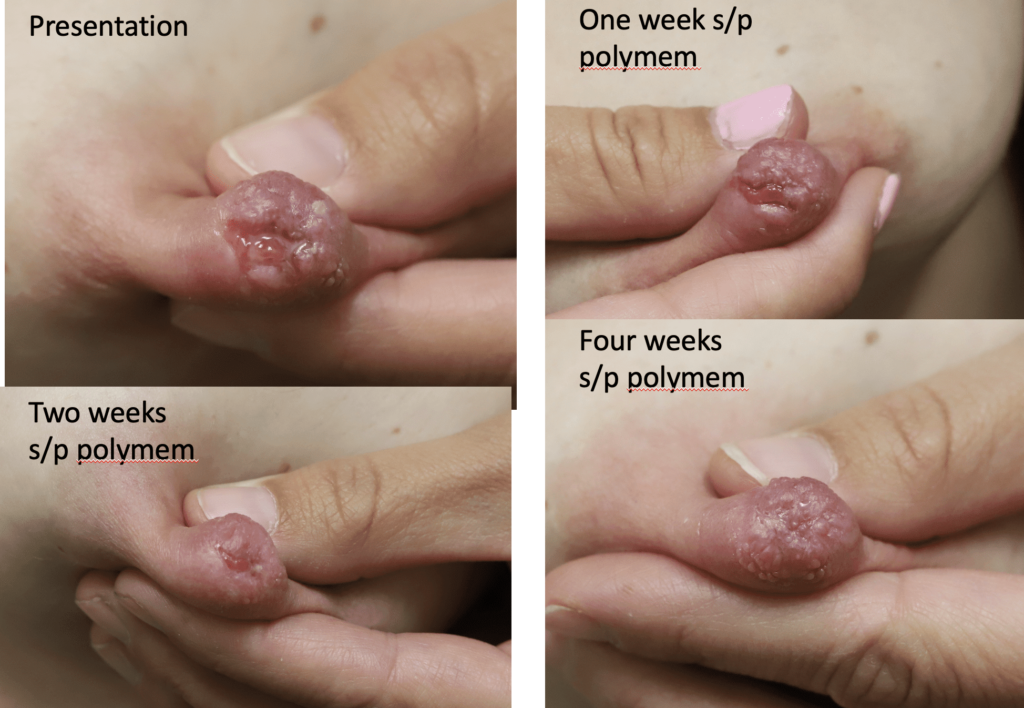
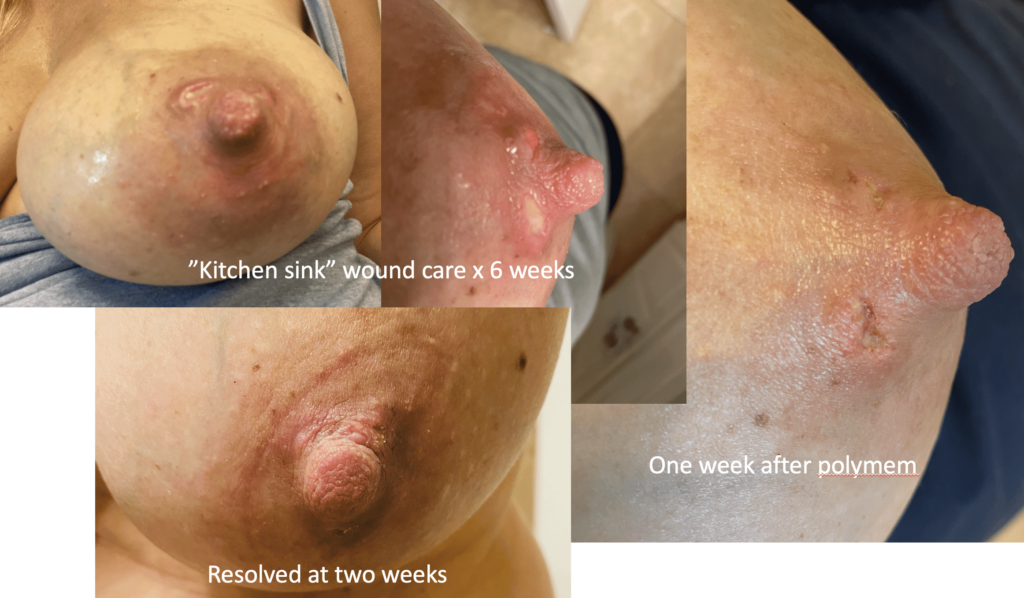

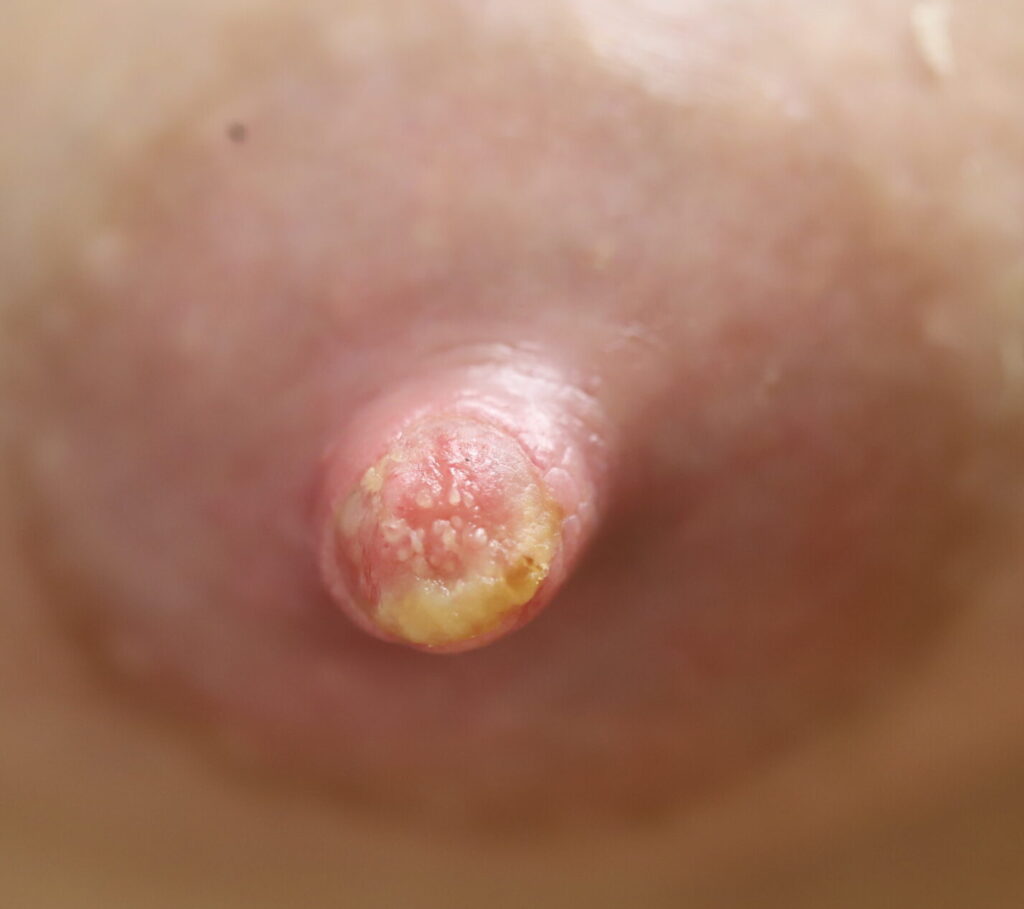
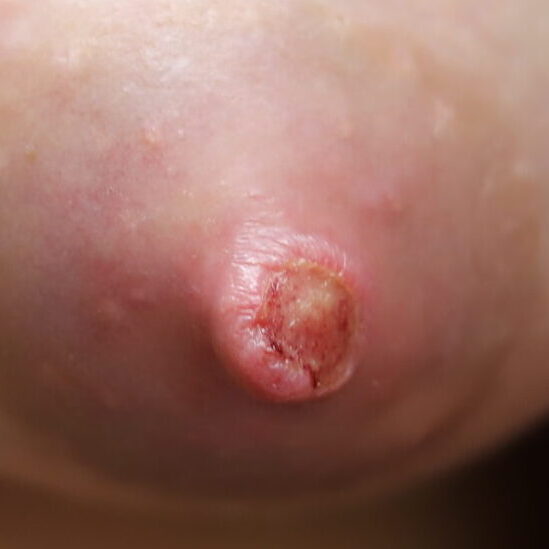
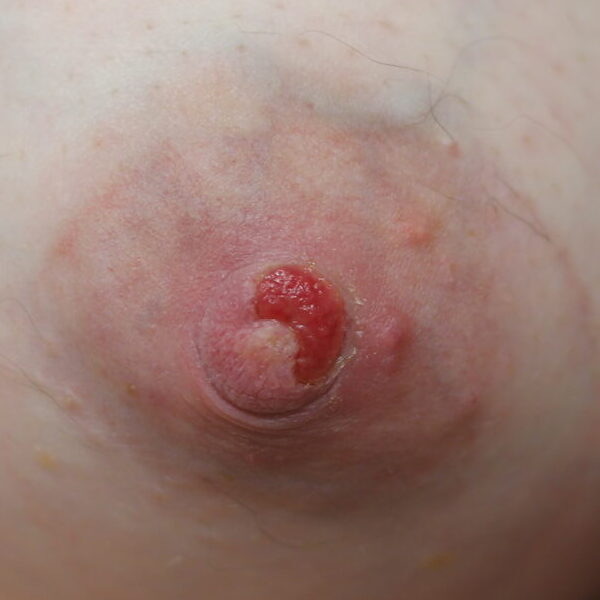
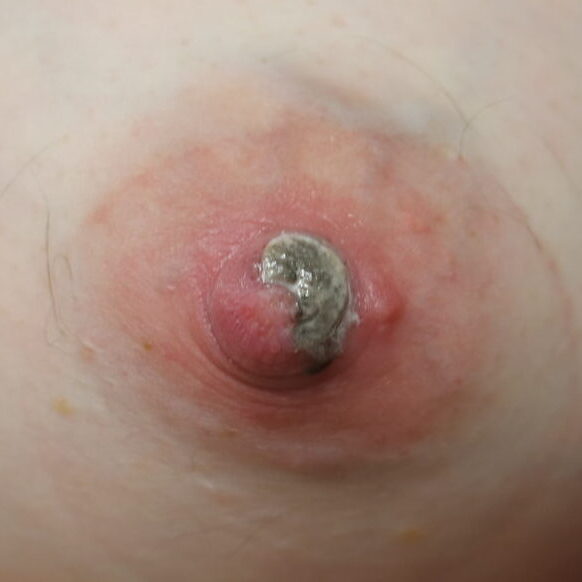

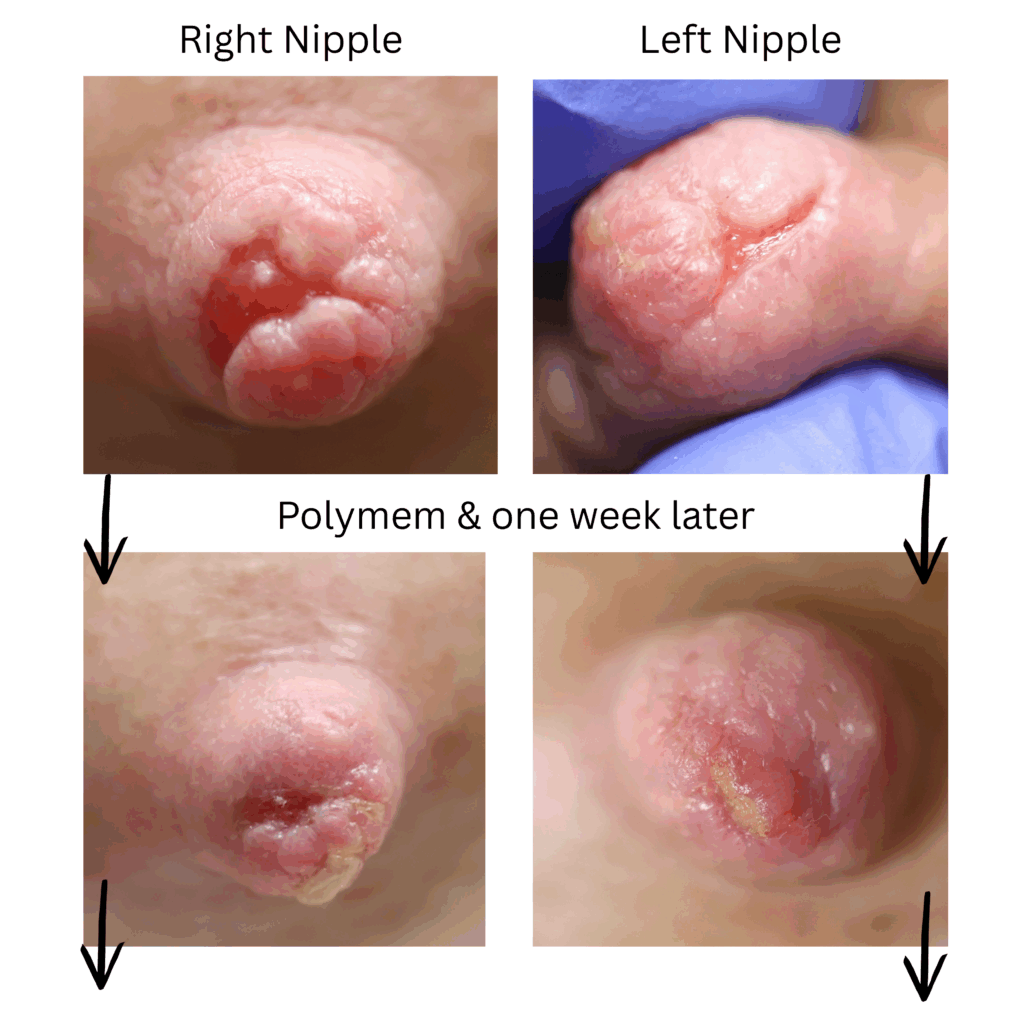
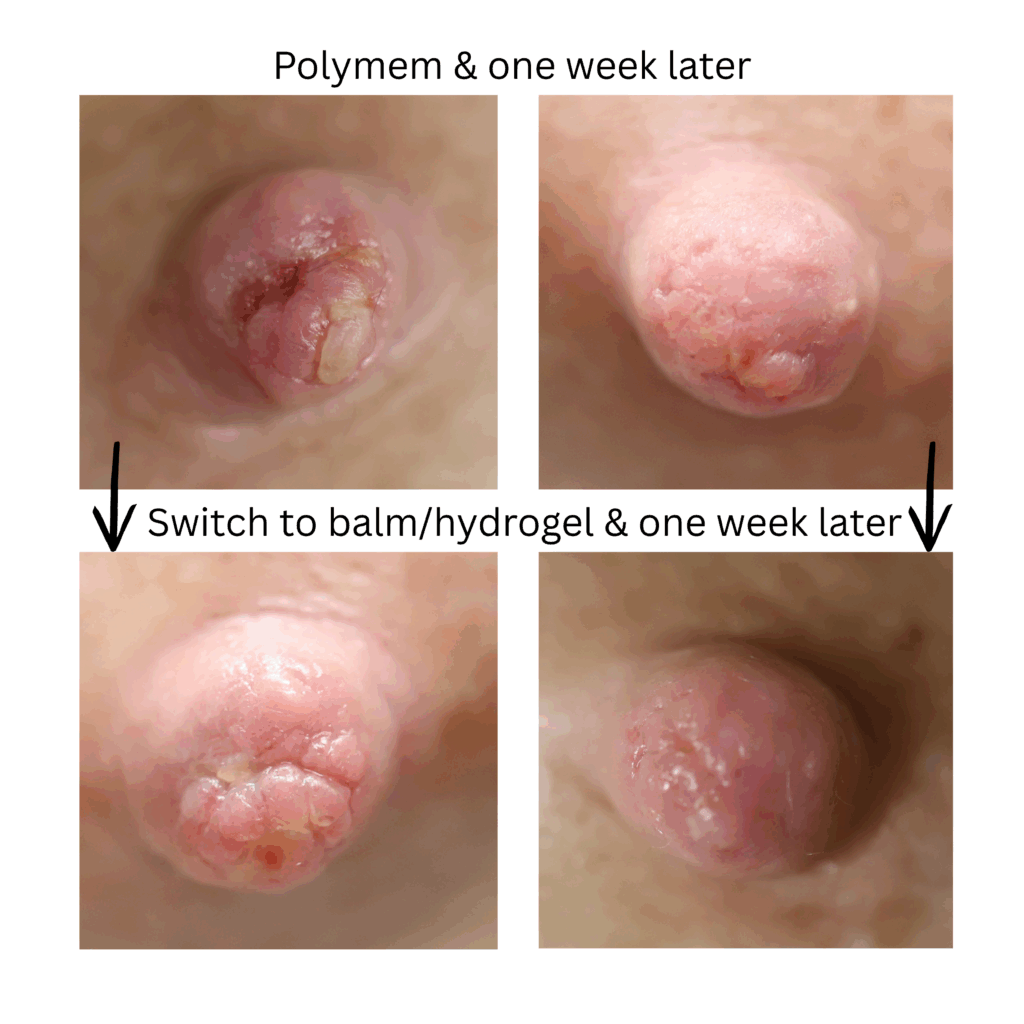
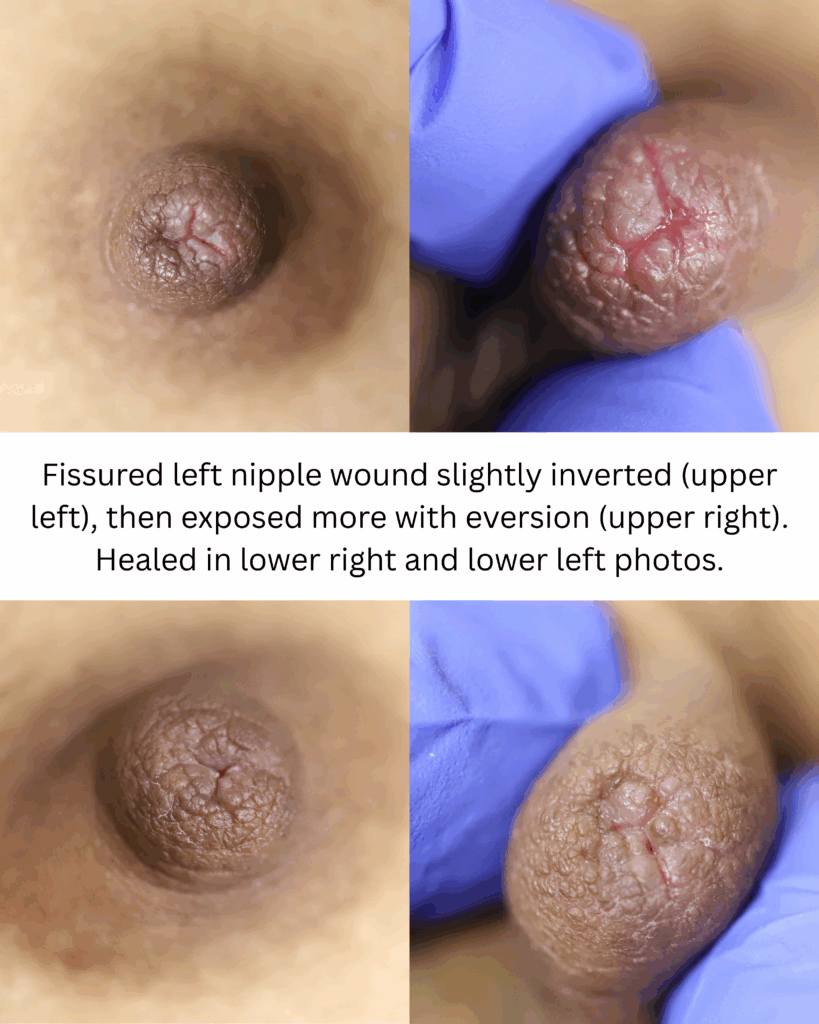
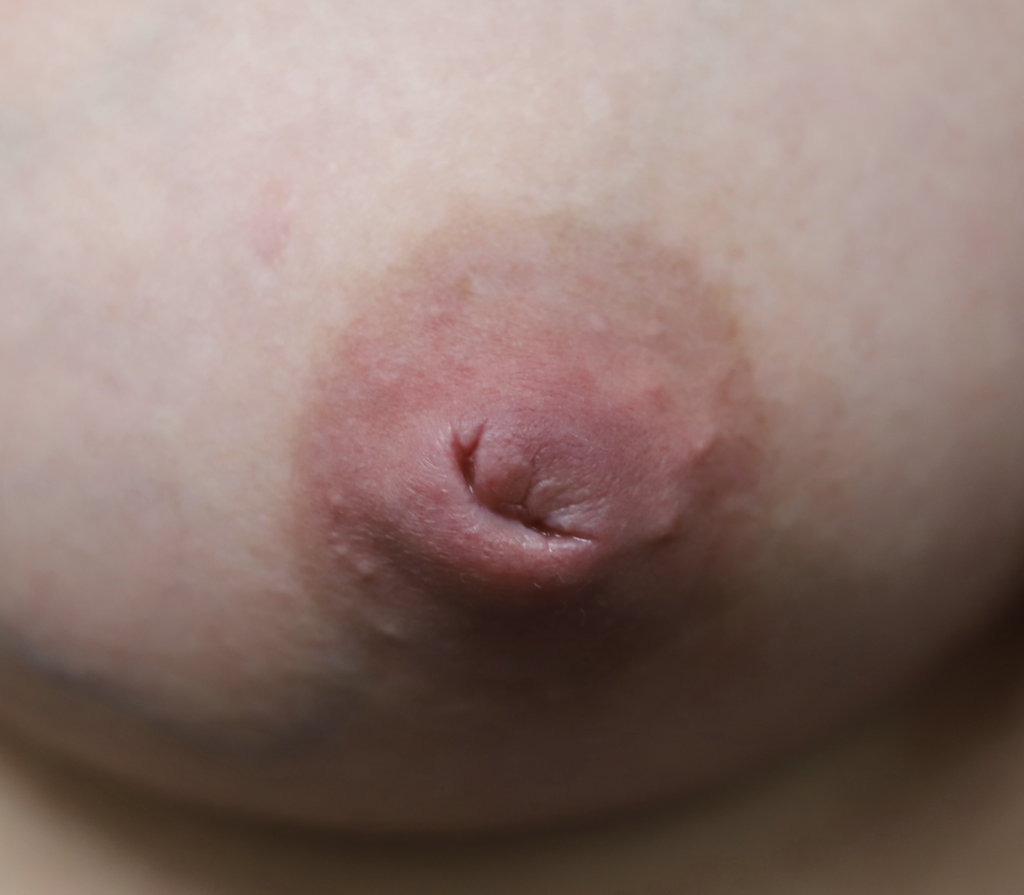
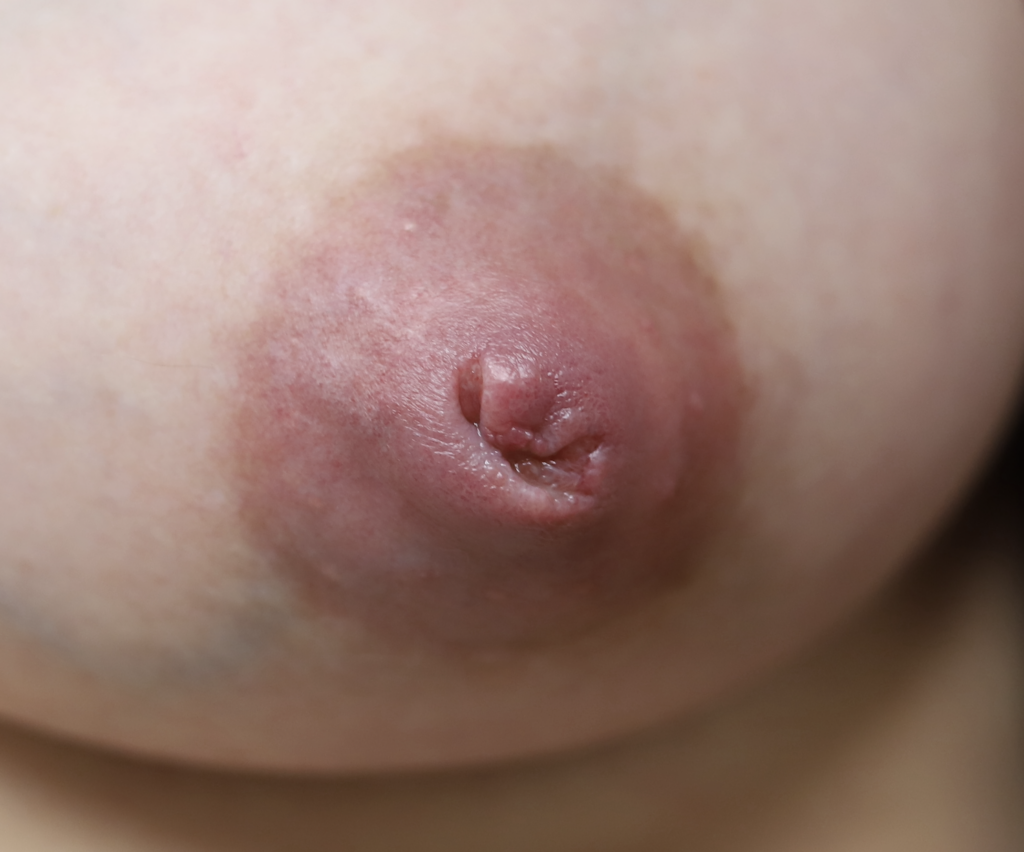
The six images below show how hard it can be to heal a chronic wound in a patient with nipple inversions, because it is hard to get the polymem or hydrogel to approximate the tissue that needs help. We also tried medihoney, regular balm, and a fancy new wound care product that we use in the OR that is extremely expensive but the rep gave me as a sample. That unfortunately also didn’t work. 🙁
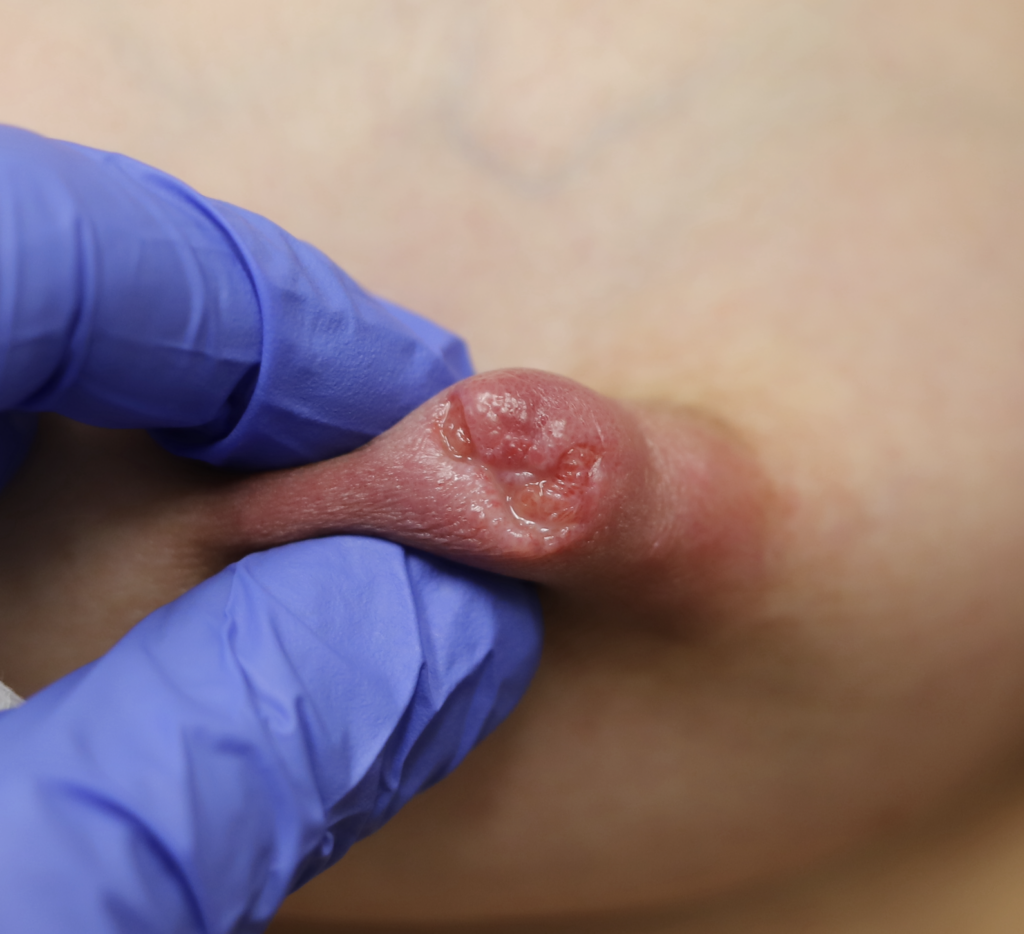
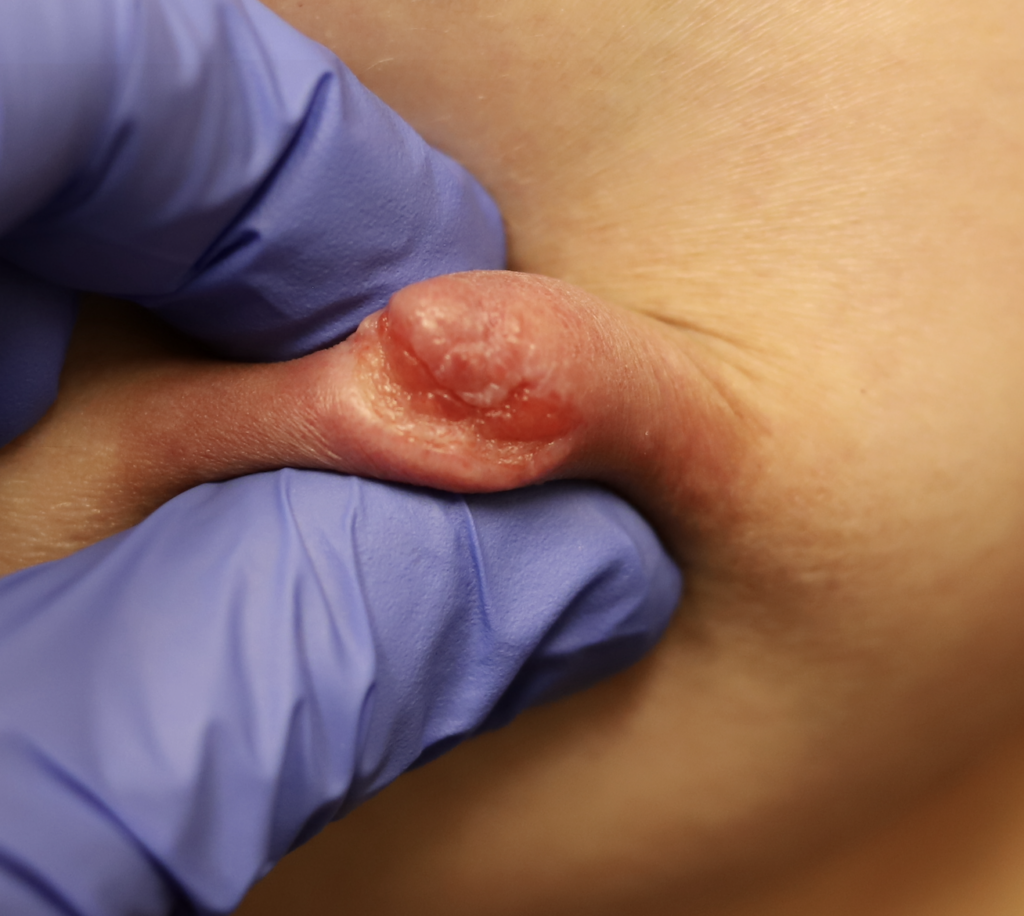
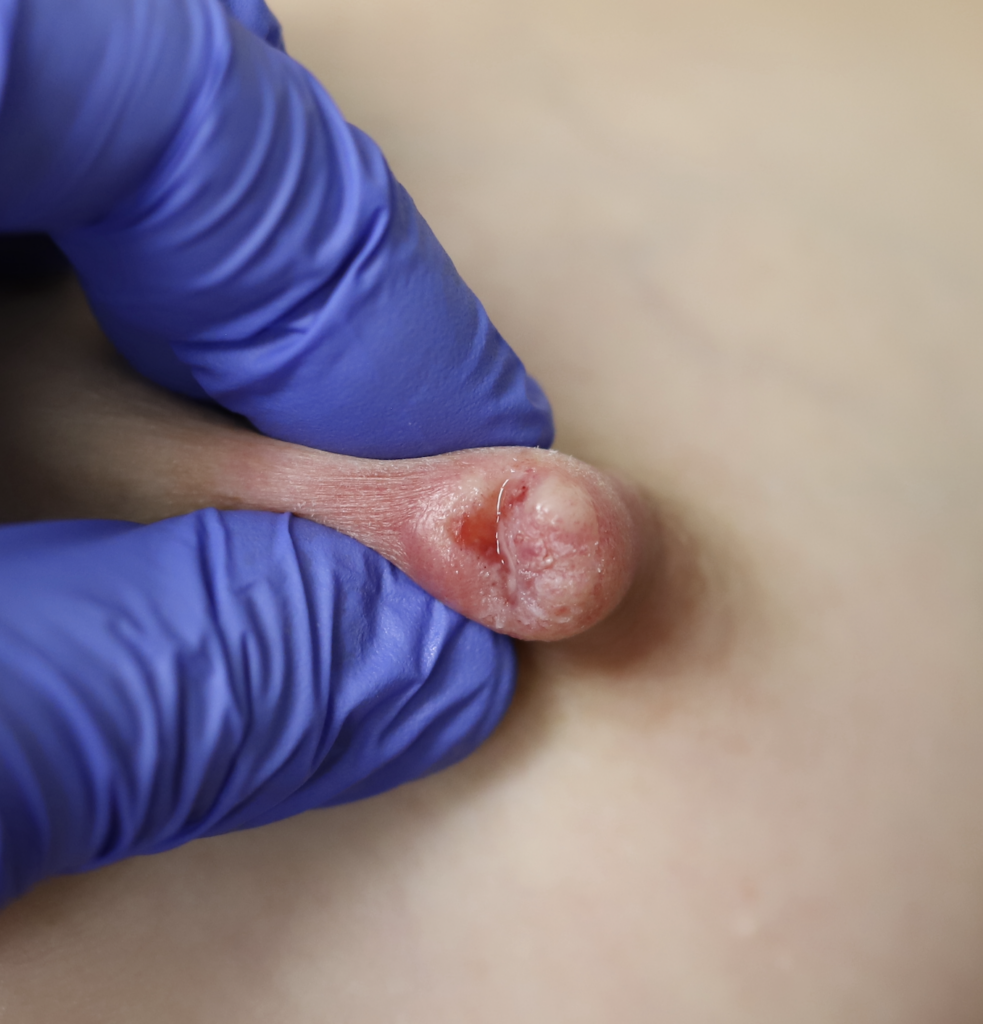
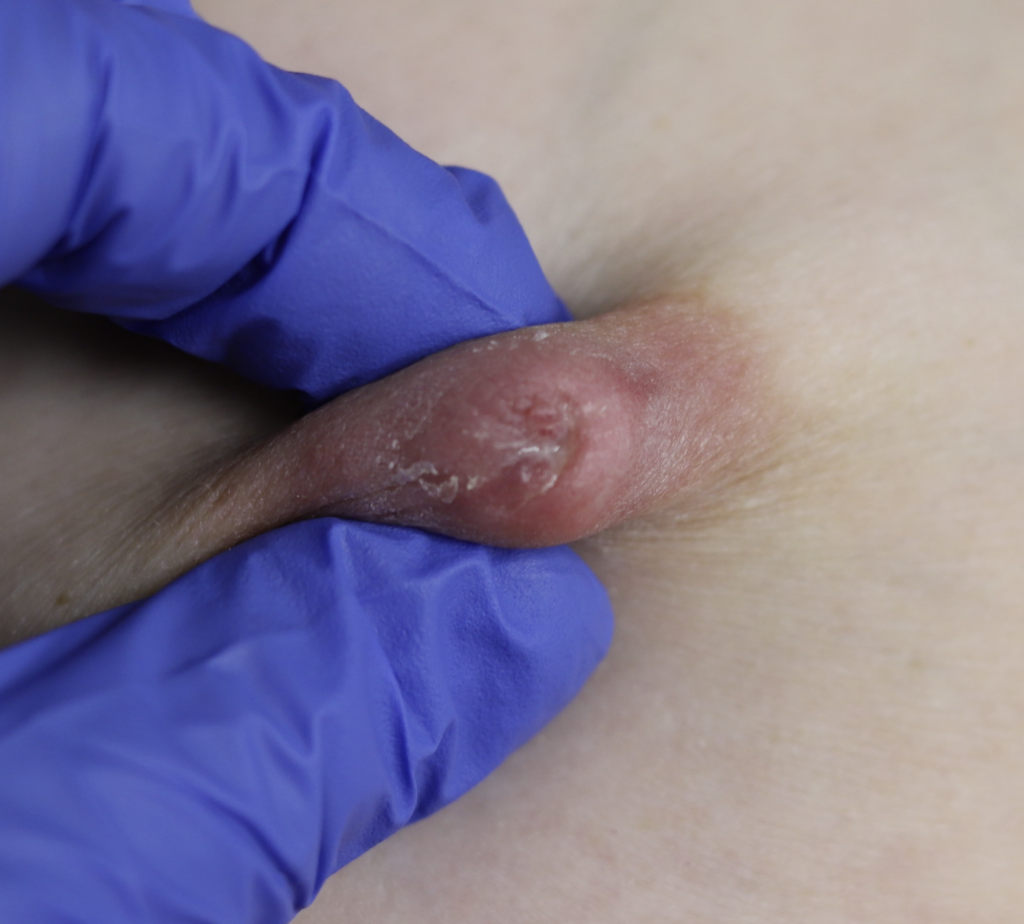
This patient also had hyperlactation and was constantly flooded with breastmilk (high water content – hard for healing) in her inversion. The top two photos show the appearance of the inverted nipple (top left) and partially everted (top right). Middle left is the cratered wound early on, and middle right is the wound trying to heal itself but demonstrating hypertrophic granulation tissue (look how the beefy red is fatter/beefier and more elevated compared to the middle left).
We did use silver nitrate and started to close the wound (bottom left) and it finally healed itself (bottom right).
Now for some additional guidelines about things to avoid!
- Do not use drying agents such as antiseptics and alcohol.
- Gentian violet can produce significant tissue ulceration and should never be used on a nipple.
- Some women may lubricate dry skin with nursing balms. They should be aware of potentially allergenic ingredients such as lanolin, petroleum, and coconut.
- Balms containing multiple ingredients may result in dermatitis from allergens.
- Antifungals creams worsen pain and vasospasm, and can cause dermatitis and ulcerate skin. They are not indicated for use on nipples.
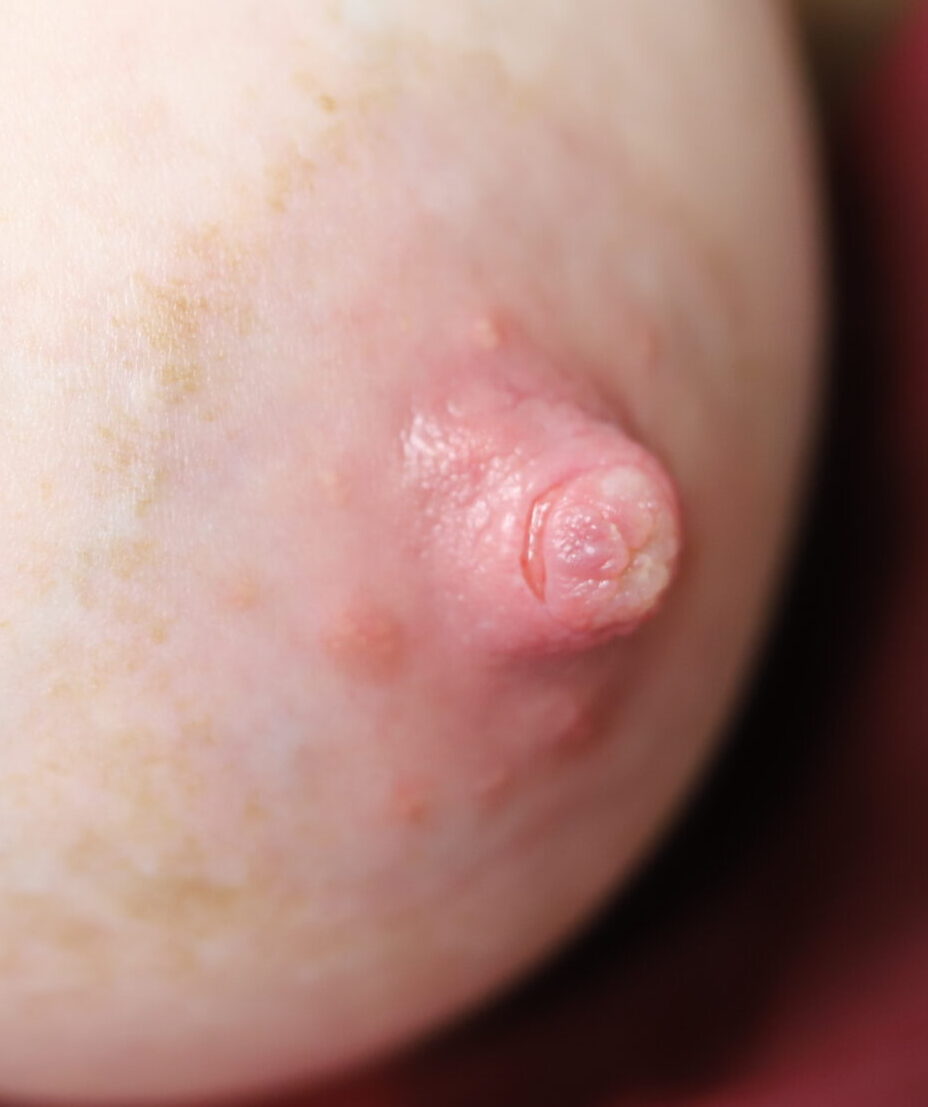 Nipple fissuring that began after a mom used nystatin continuously on her nipple.
Nipple fissuring that began after a mom used nystatin continuously on her nipple.
- APNO (All Purpose Nipple Ointment) is an expensive compounded product that should be avoided. It contains an antifungal, antibacterial (which is similar to antifungals in that it is not indicated for use on a nipple and can cause dermatitis), and a steroid. The steroid is the component that provides relief from pain. If a steroid is indicated, it should be prescribed separately (e.g. 0.1% triamcinolone). Most dermatitis and pain do not respond to over-the-counter non-prescription strength steroids. 4th Trimester Physician Michelle Haggerty has a great blog post on the dangers of APNO as well.
- Breast shells designed to “keep the nipple dry” or “protect the nipple from the bra” worsen swelling in the nipple, cause areola compression, and subsequently worsen pain
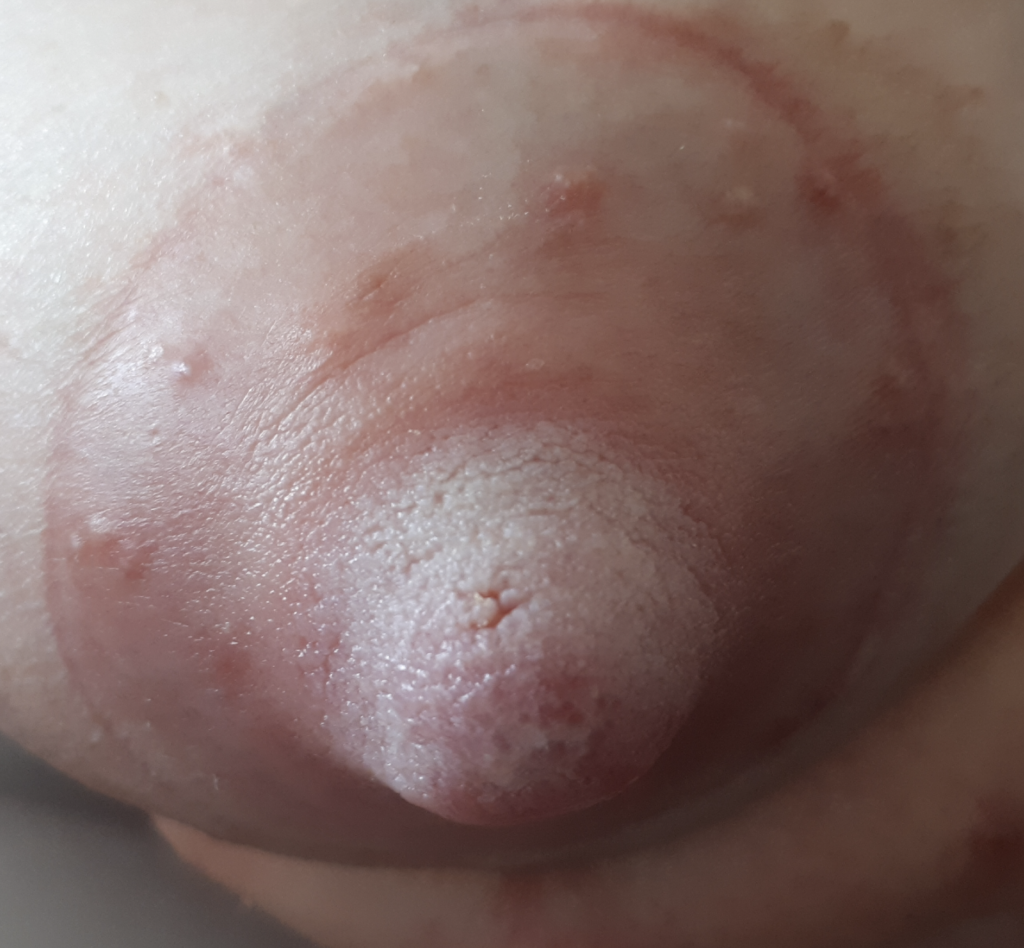


- Using a hair dryer on nipples causes drying and increases risk of skin breakdown.
- Epsom salt soaks are used to promote opening and drainage of skin, such as with abscesses in the buttock region. Epsom salt soaks will similarly break down nipple skin and should not be utilized for the purposes of nipple care.
- Wet tea bags and warm compresses similarly increase the risk of skin breakdown.
- Pumping to “rest” the nipple in settings of pain and/or trauma/wound brings with it a new set of complications: Pumping is rigid and mechanical with fixed suction (i.e. not “physiologic” like a baby’s mouth with constant variation in position and pressure), it does not allow a baby to use its saliva to help heal wounds, patients can develop new problems with suction blisters, blebs, and reduced blood flow to the nipple, and it may stimulate over or underproduction of milk. A baby may not want to return to the breast. It is much better to treat the nipple pain with topical (e.g. steroid cream) and/or oral pain medication than to introduce a pump.
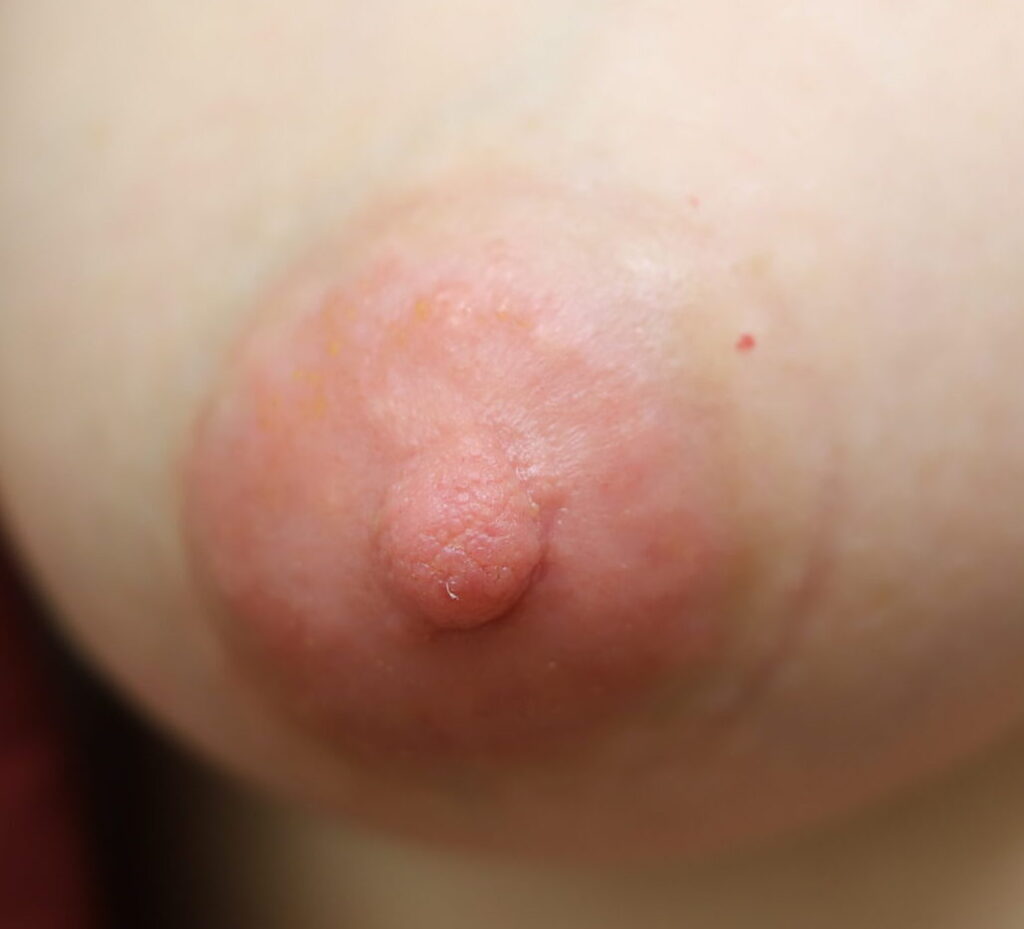
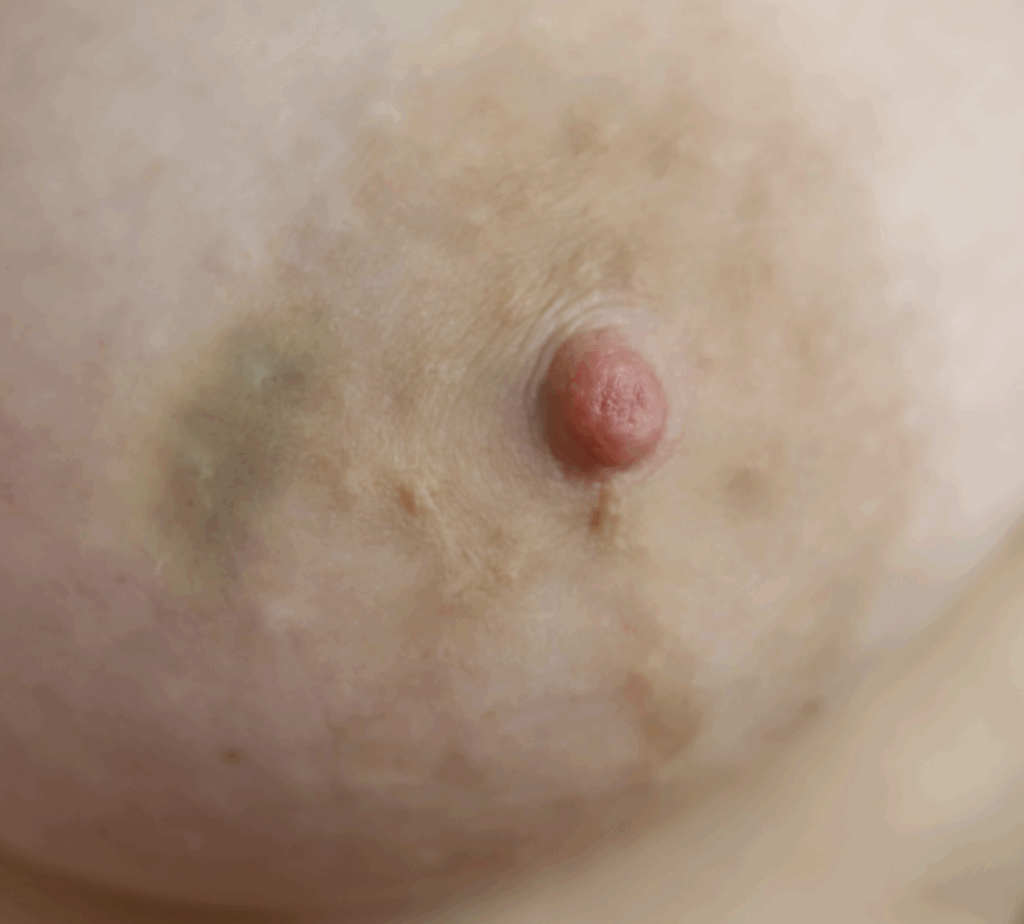
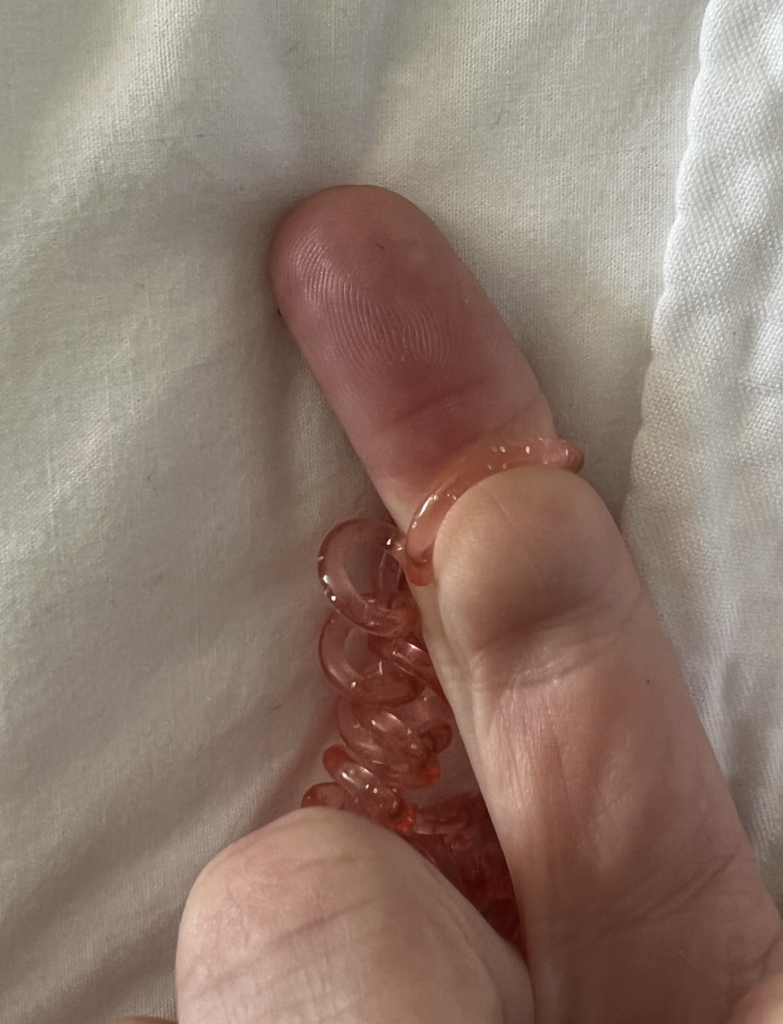
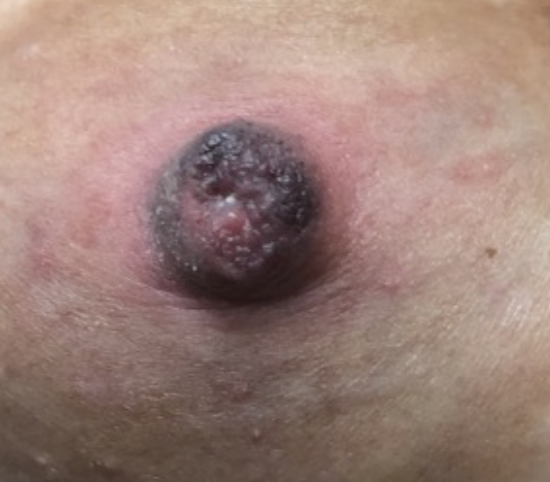
A pump, unlike an infant, has the unique ability to strangulate (literally like putting a rubber band around your finger and tightening it — then adding suction pressure on top) your nipple. I use this example when talking to patients about what happens when you use too small of a flange, too high of suction, or pump for too long a duration of time: Your nipple, just like a fingertip, is going to turn varying shades of red, purple, and white when it doesn’t have enough blood flow. If it hurts, STOP!
If absolutely necessary, hand expression may represent the most efficacious solution to resting painful nipples.

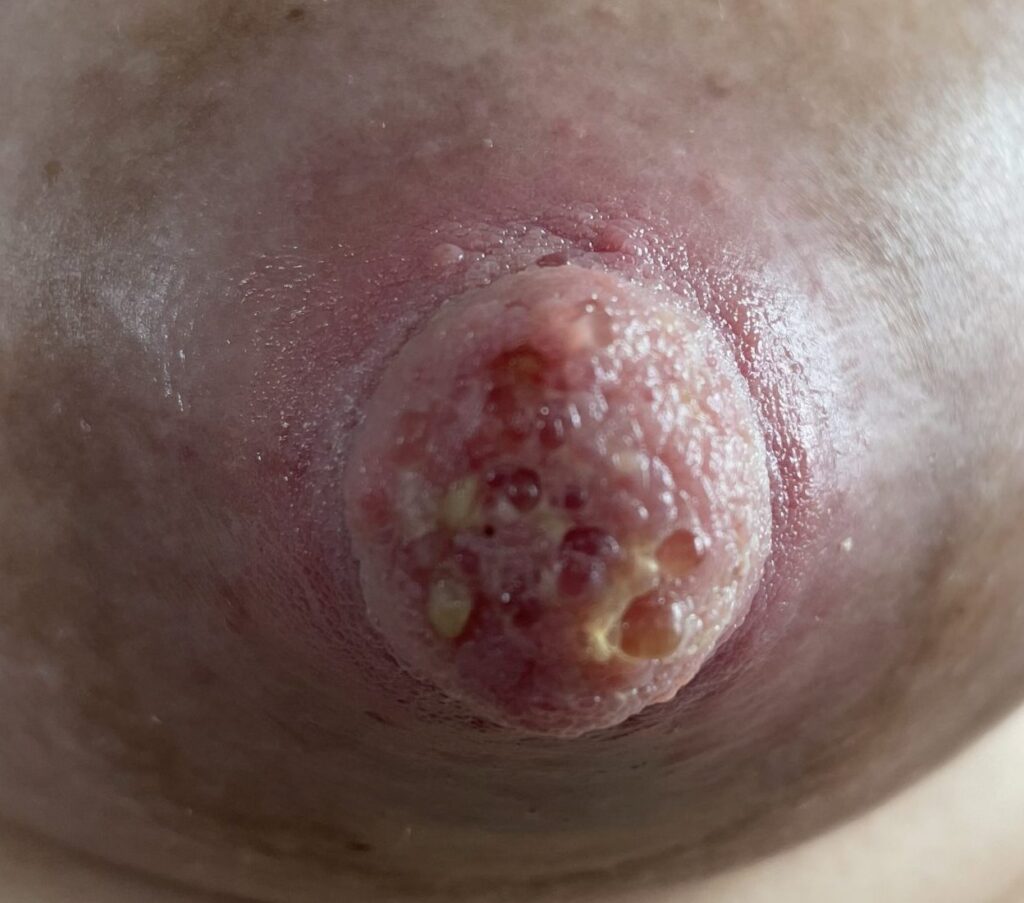
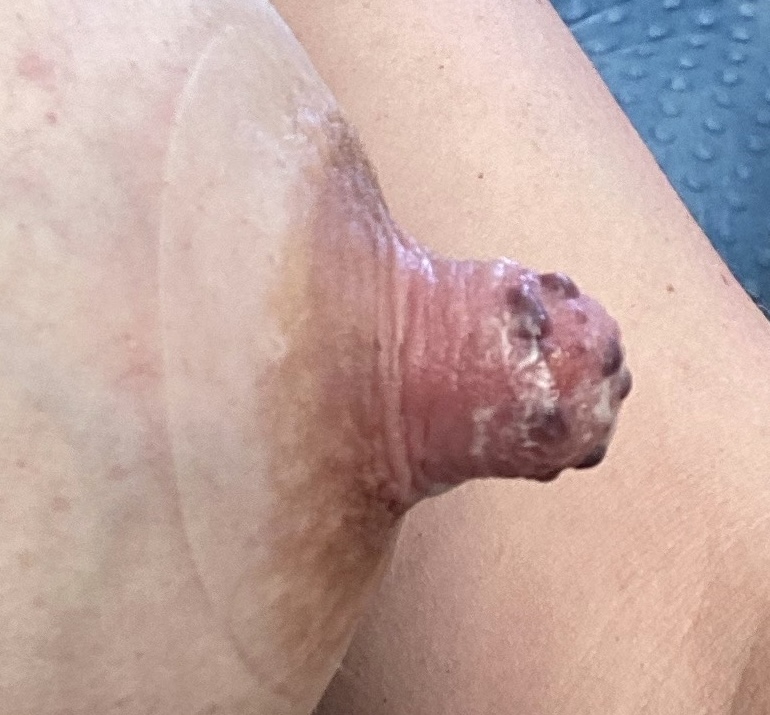

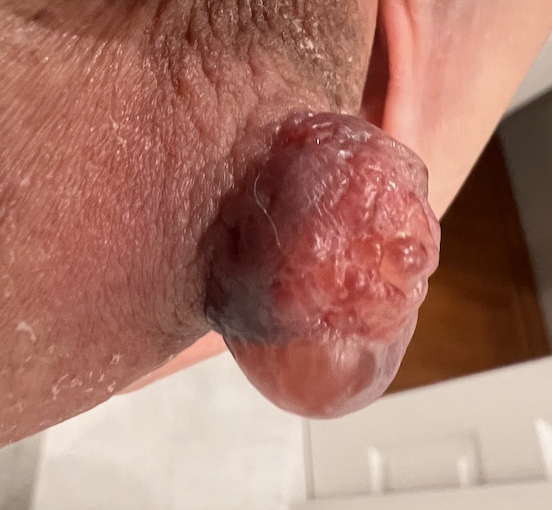


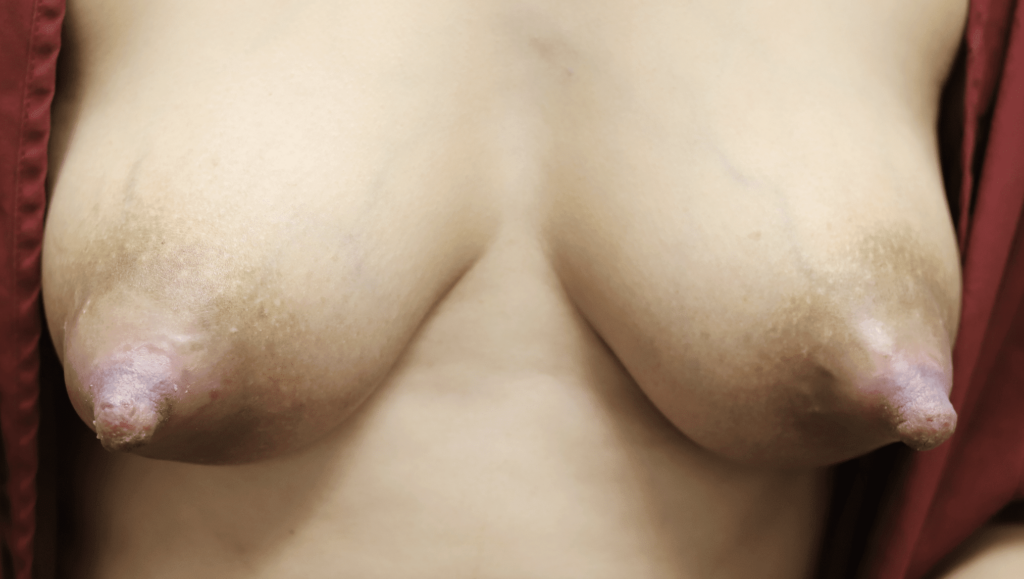






Just say “NO” to nipple shields. Patients with pain also may be recommended to use nipple shields. Nipple shields are associated with multiple complications, including mastitis, plugging, and significant reductions in milk production and transfer. Many mothers have difficulty weaning infants off the nipple shield once it has been used regularly.
Given these known complications, the breastfeeding dyad should undergo a thorough evaluation prior to introduction of a nipple shield.
Often, nipple shields are introduced when a small infant struggles to latch to a larger, pendulous breast and causes pain. This may instead simply require adjustment of a position that is more amenable to feeding with large breasts, such as the laidback or side lying position.
Infants also may refuse to latch when the flow of milk is very high; adjusting position and treating hyperlactation can address this issue without introducing nipple shields. In other situations, very large nipples as shown in this image to the right preclude any sort of latch due to size and this is a situation in which mom should express breastmilk via a pump.
Persistent pain may be neuropathic (nerve level – no overt physical injury).
The SSRI class of drugs can provide significant relief of pain as serotonin receptors are expressed in many parts of the body, including the breast and intestinal tract.
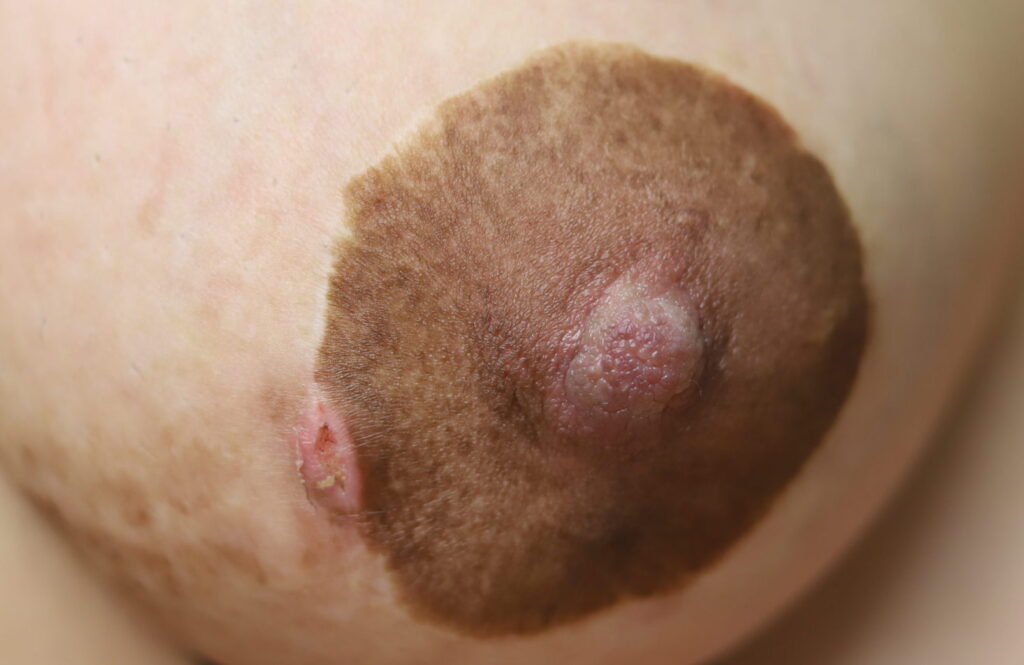
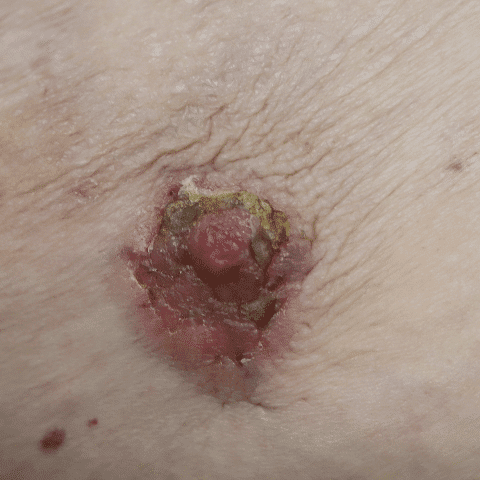
Paget's Disease
Paget’s disease presents most commonly in older postmenopausal women and comprises 0.5-5% of all breast cancer. While it is important to refer any woman with a concerning finding to a breast surgeon for evaluation, this disease is extremely uncommon in younger lactating women. “Pagetoid” changes must start with the nipple and spread outward toward the areola over the course of many years. In contrast, dermatitis (allergy or eczema), occurs very frequently in breastfeeding women and starts on the areola or breast skin. Dermatitis rarely involves the nipple.
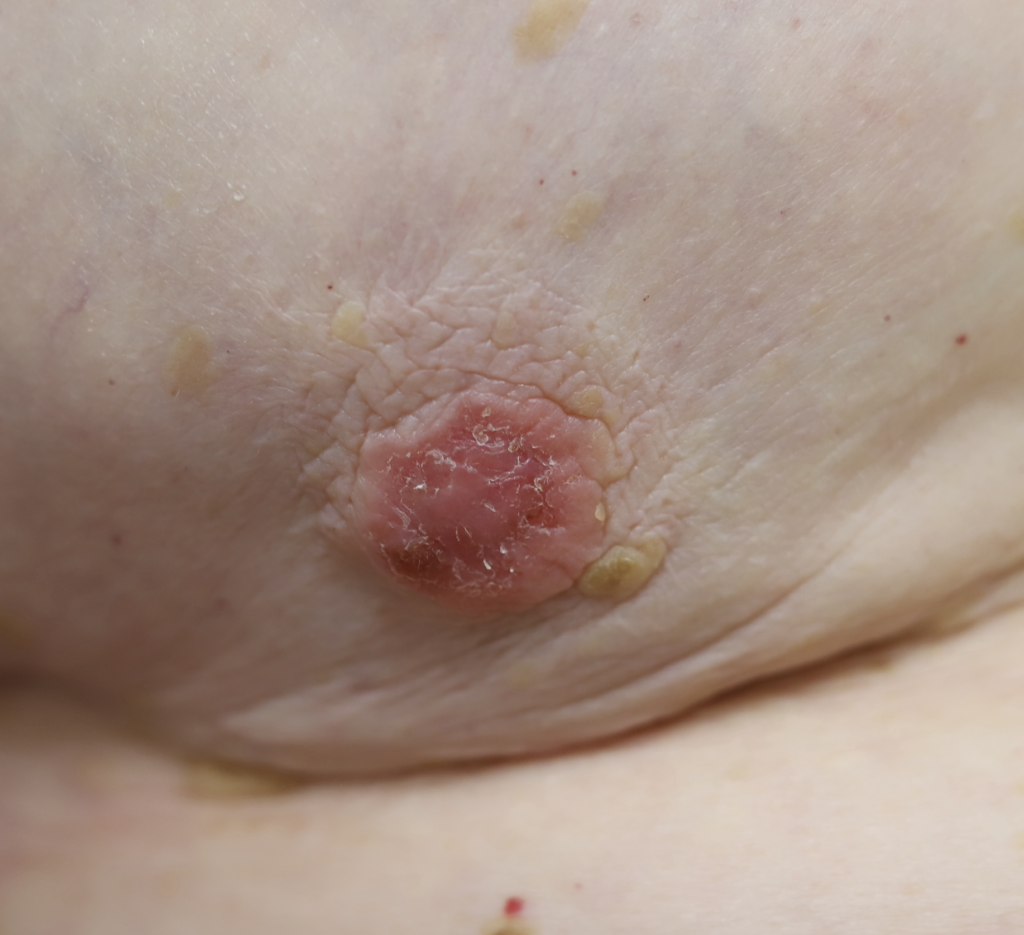
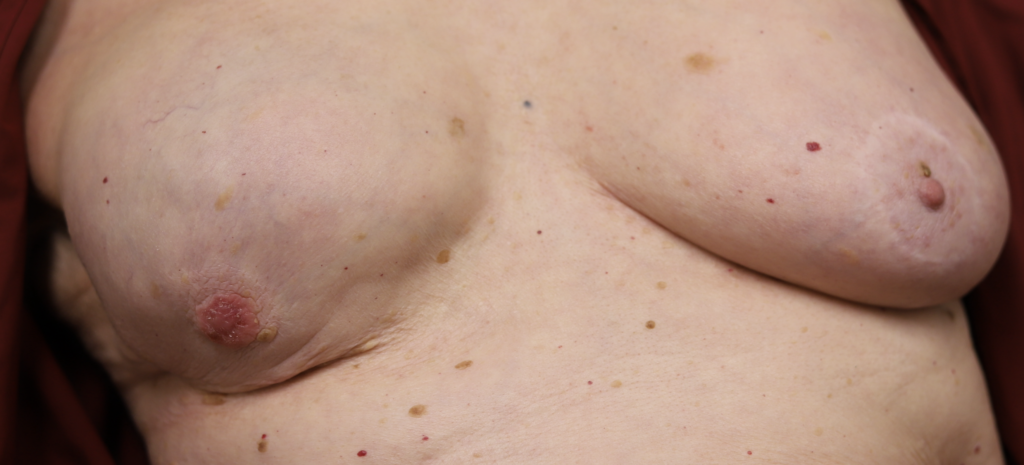

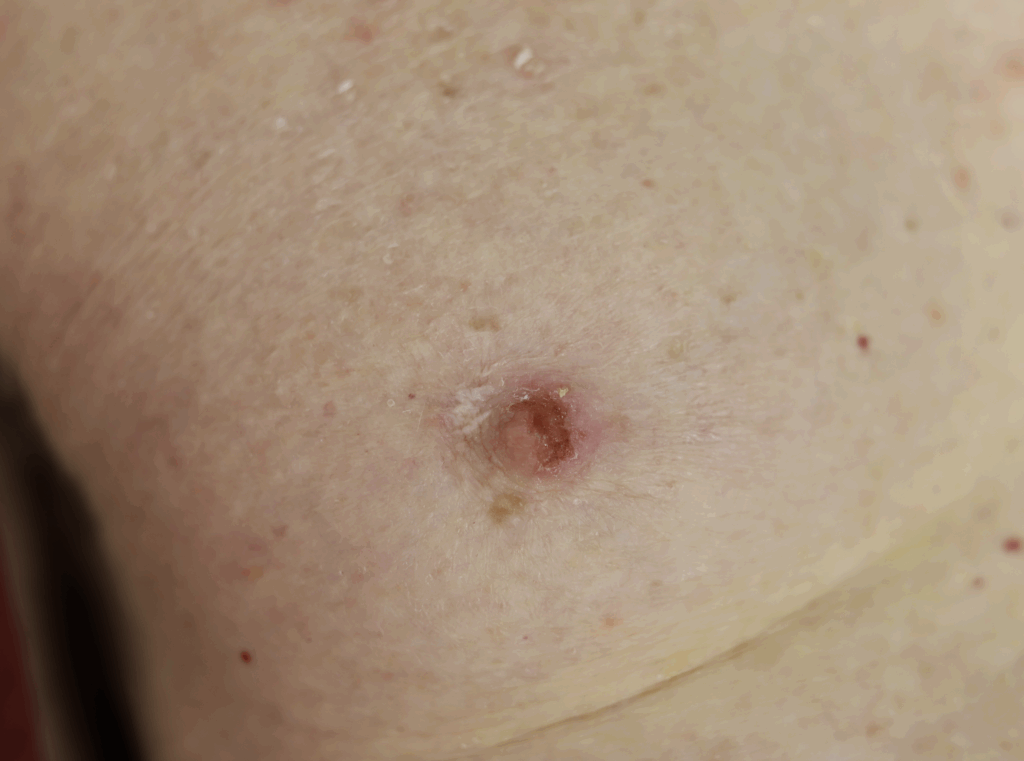
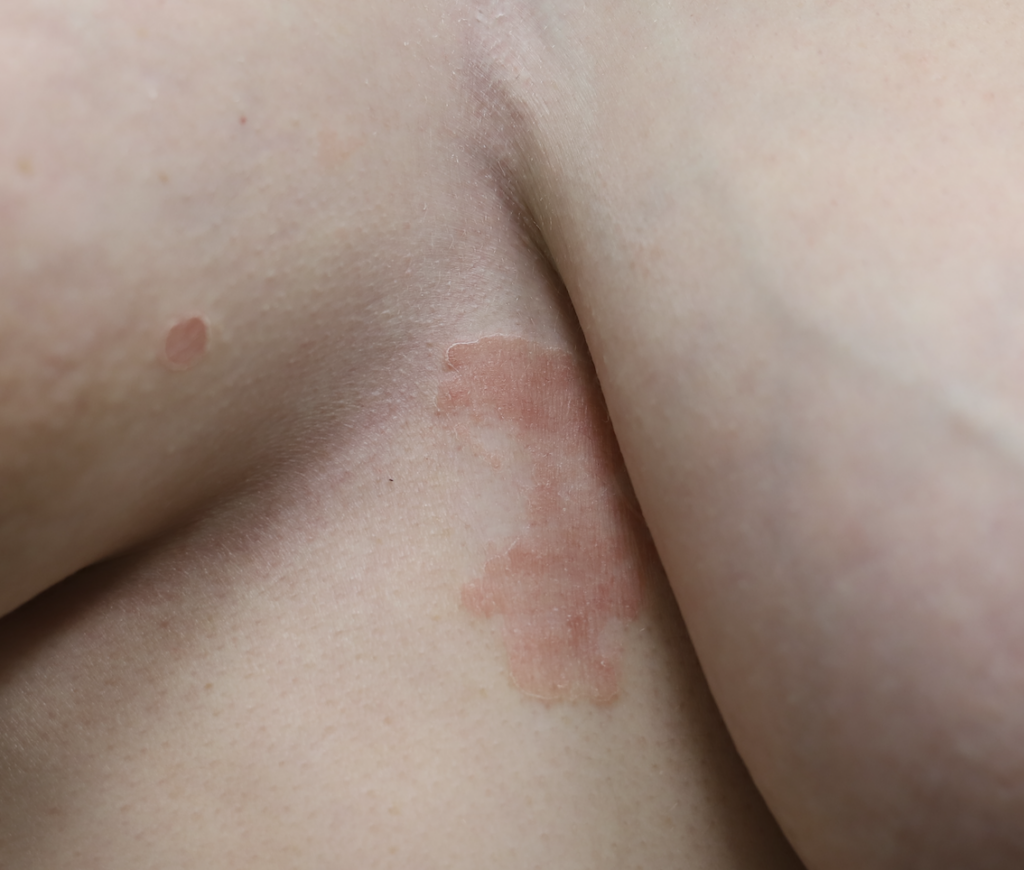
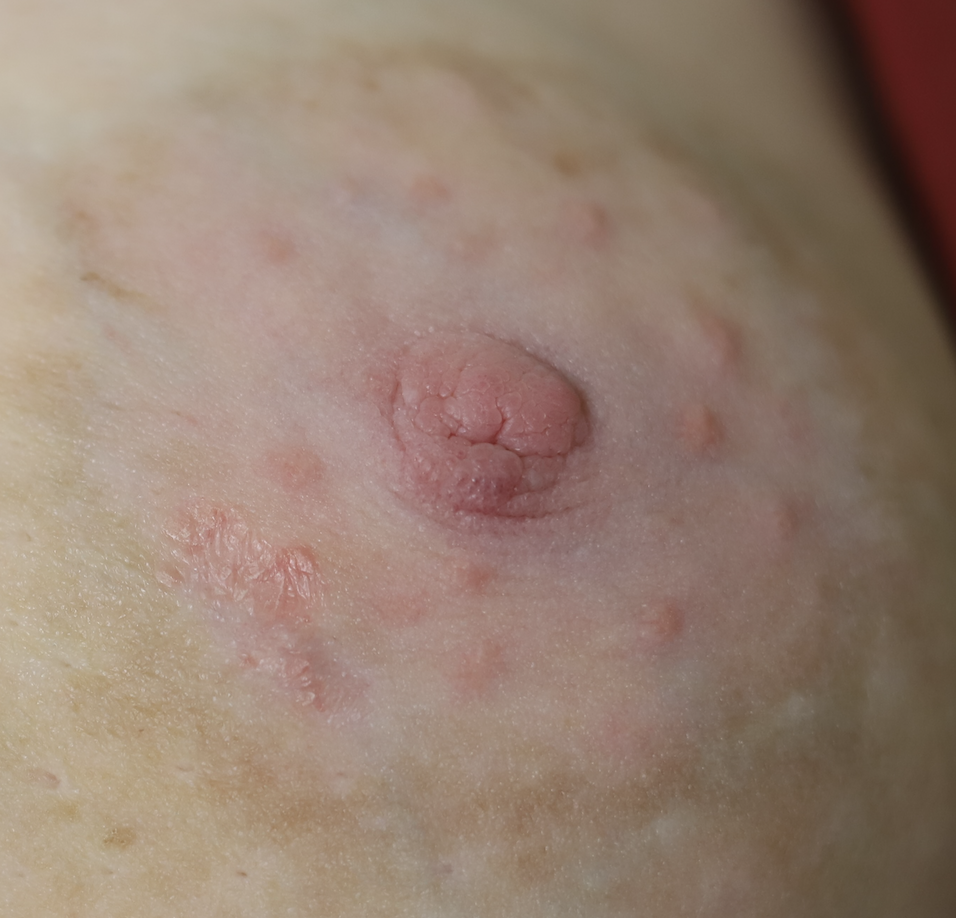
Psoriasis
Lactation may provoke a psoriatic flare in women with a history of this autoimmune condition, possibly due to skin irritation or microtrauma from breastfeeding. It is extremely uncommon for psoriasis to occur only on the nipple areolar complex, and most commonly occurs on breast skin or the inframammary fold tissue underneath the breasts. Treatment options include topical steroids, ultraviolet phototherapy, immunomodulators, and biologic agents; however, methotrexate is not recommended in lactation.
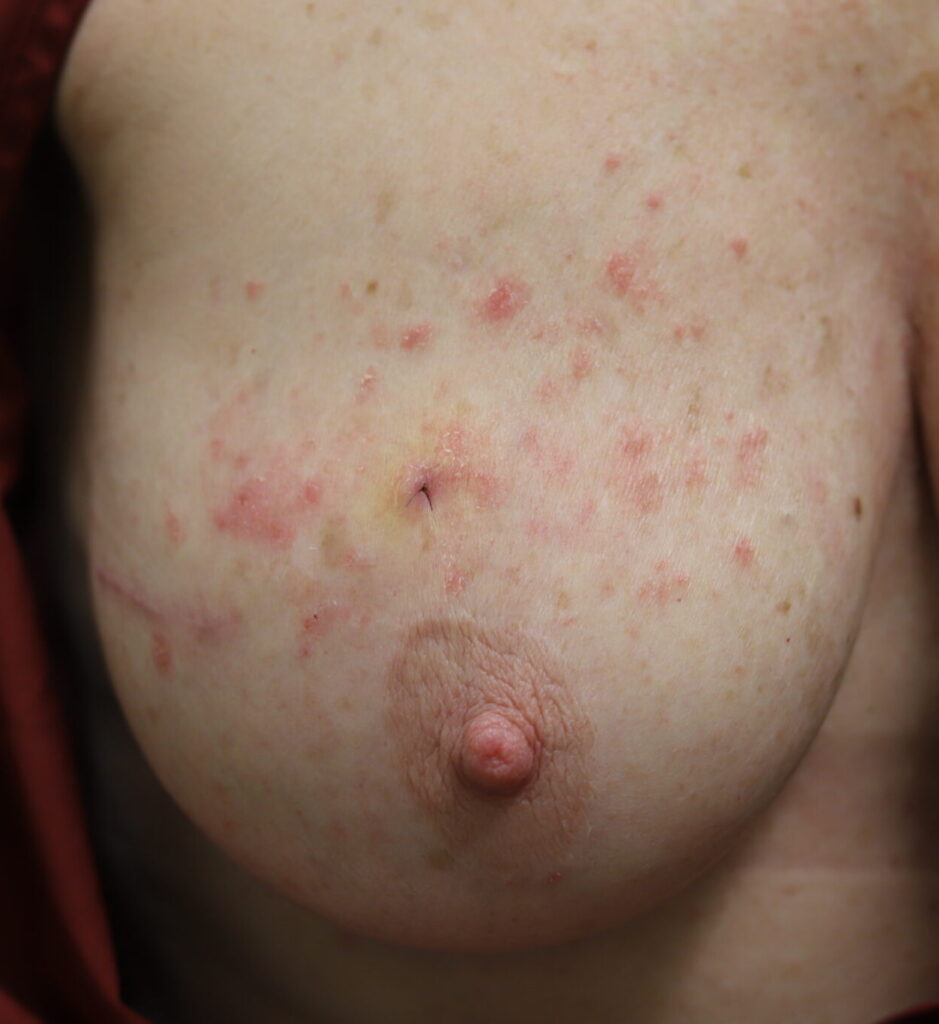
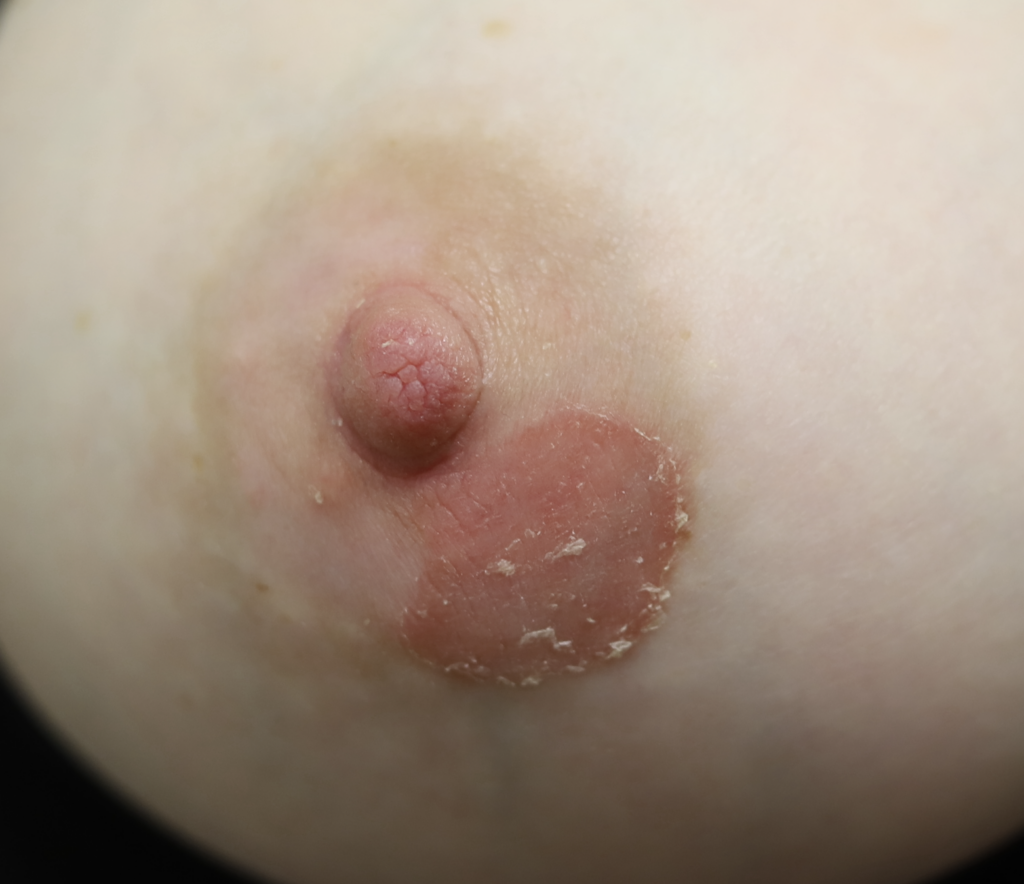
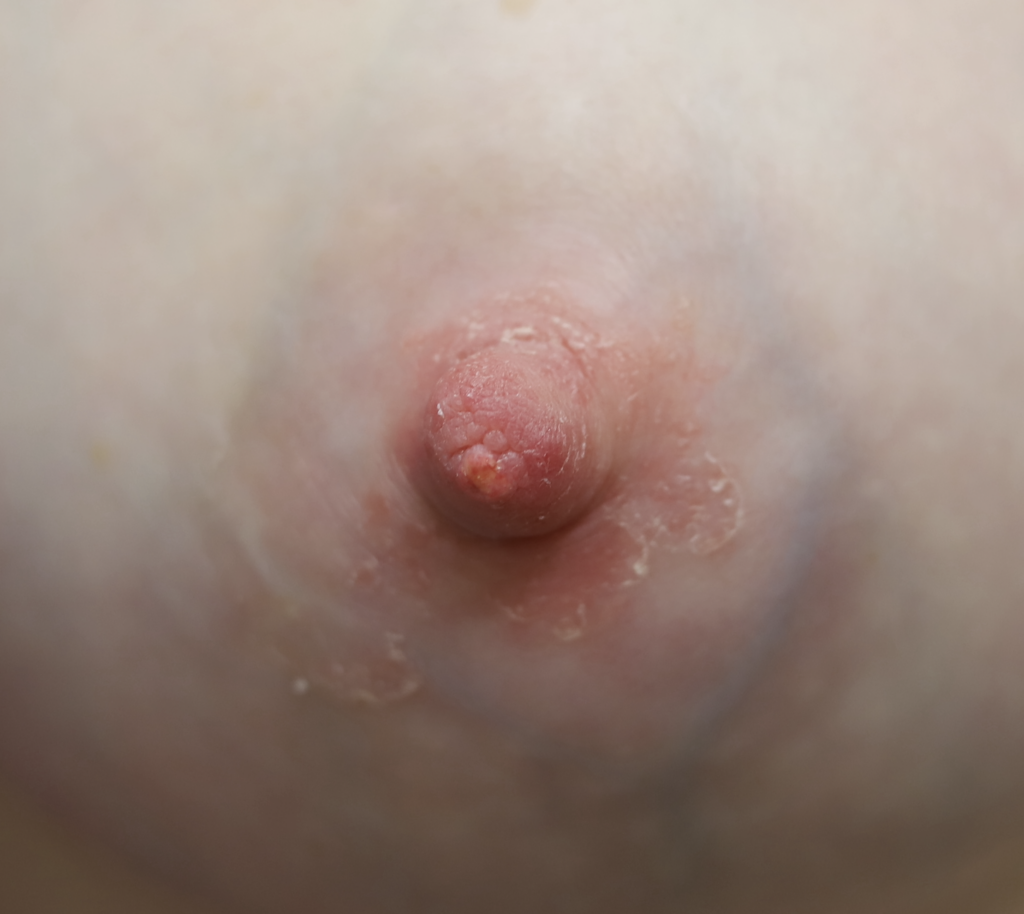
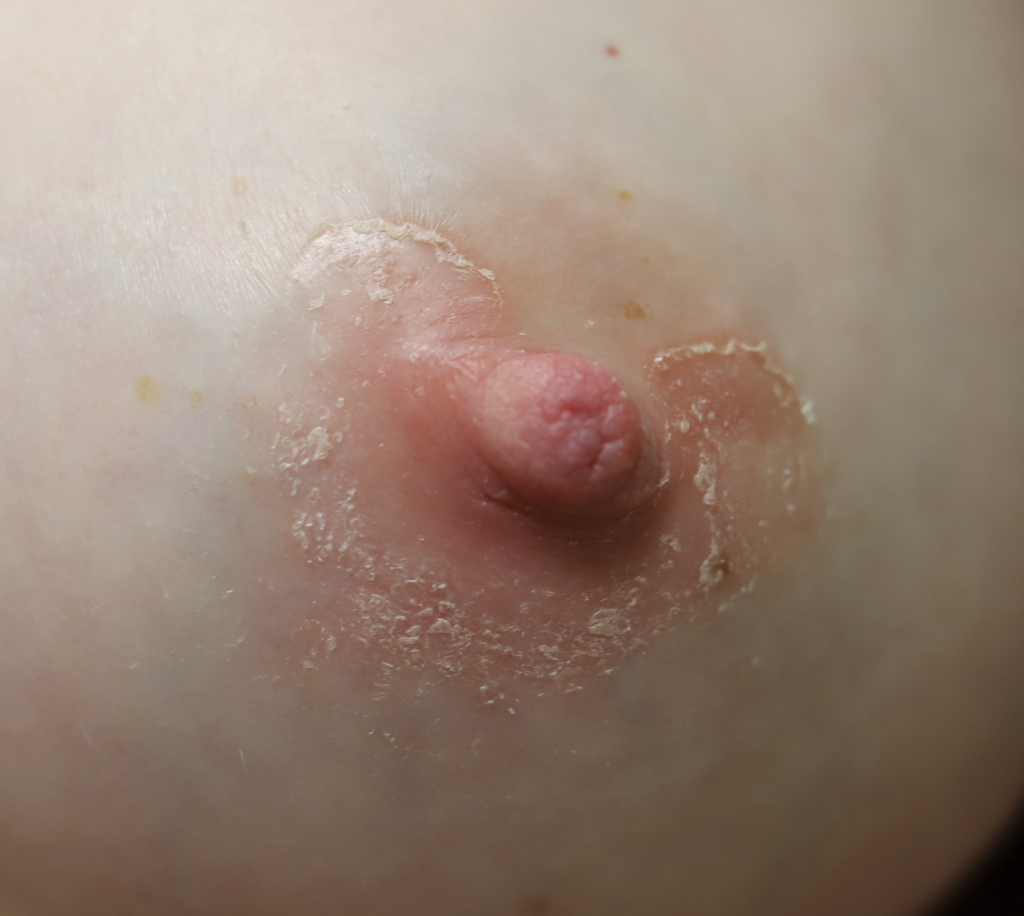










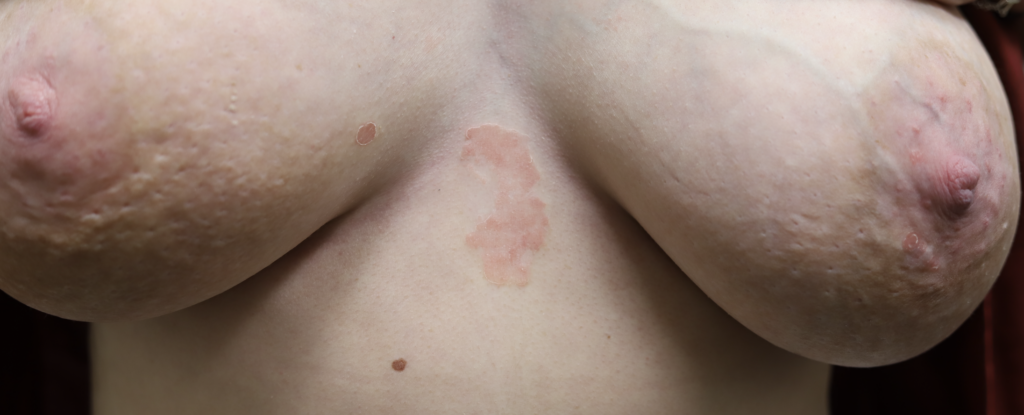
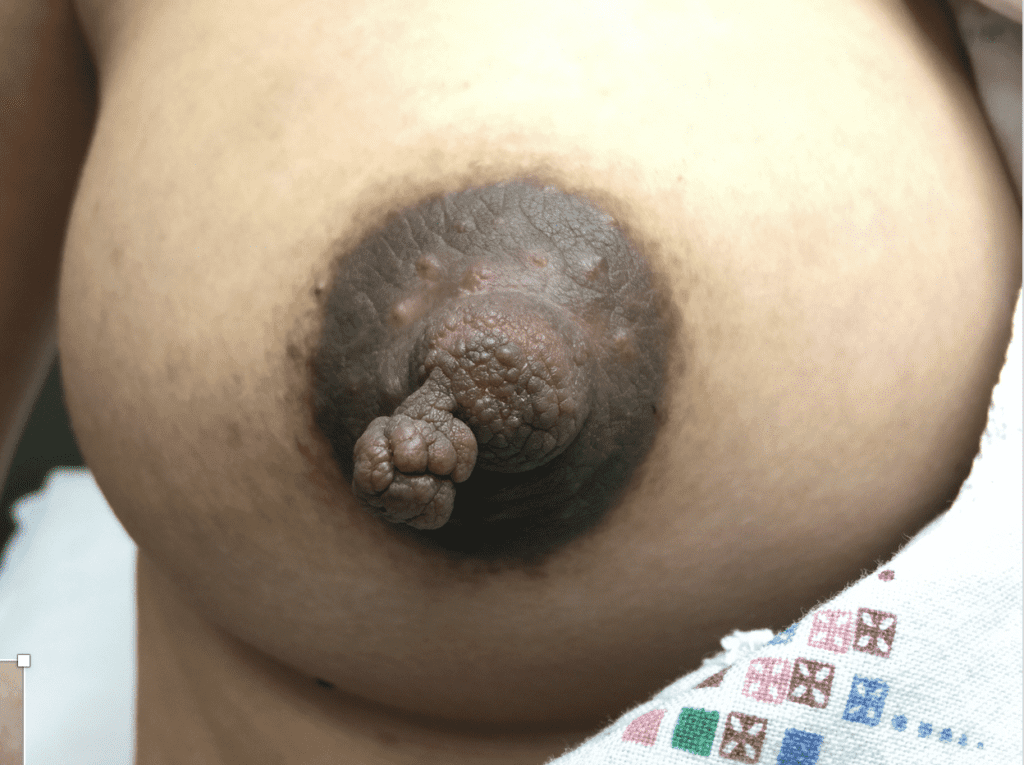
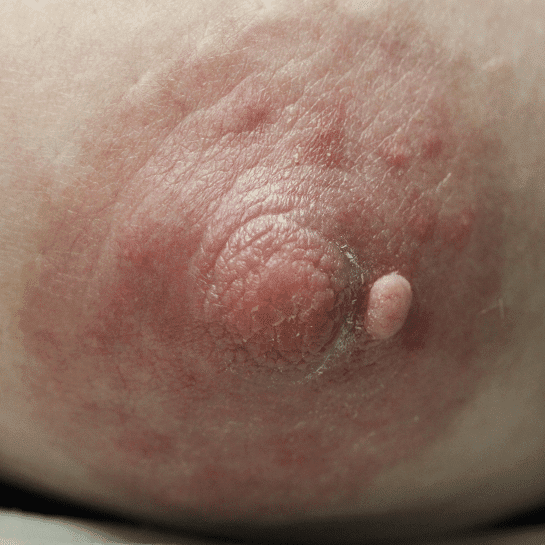
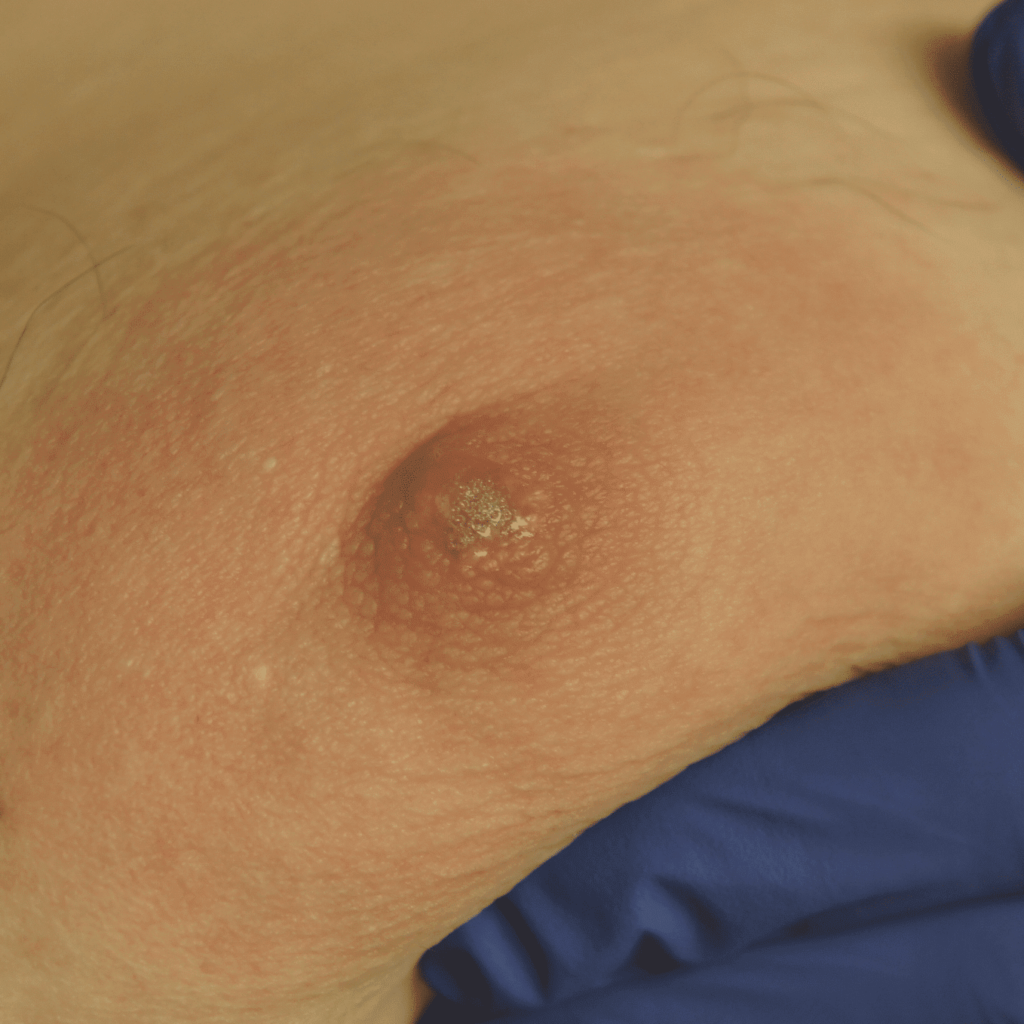
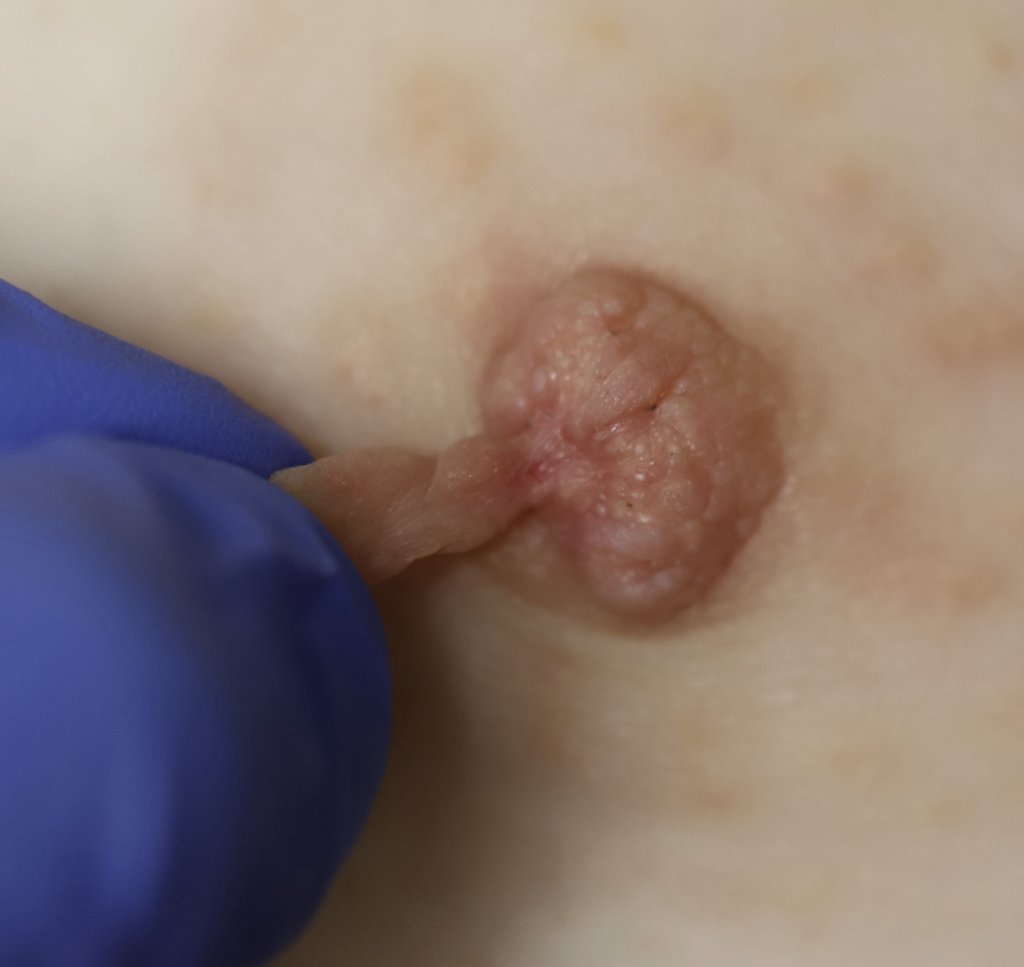
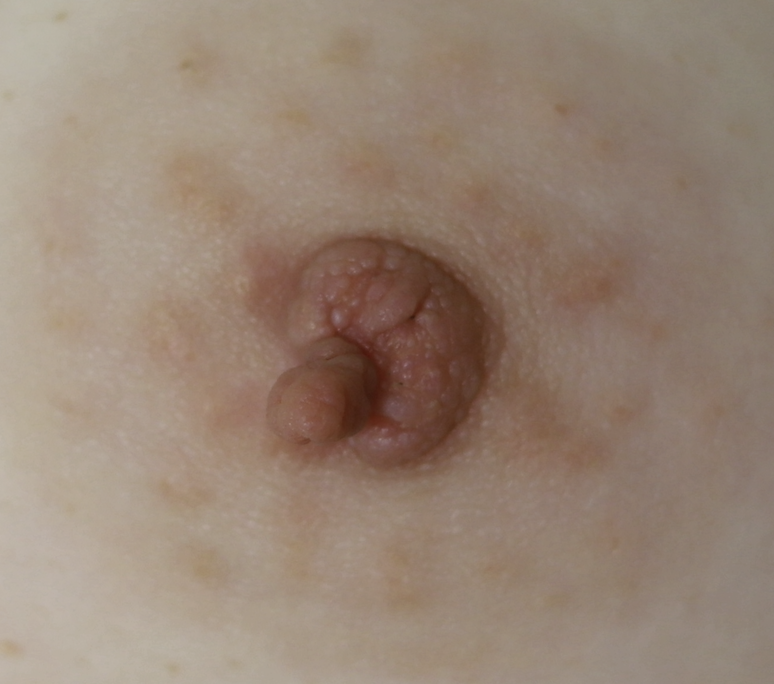
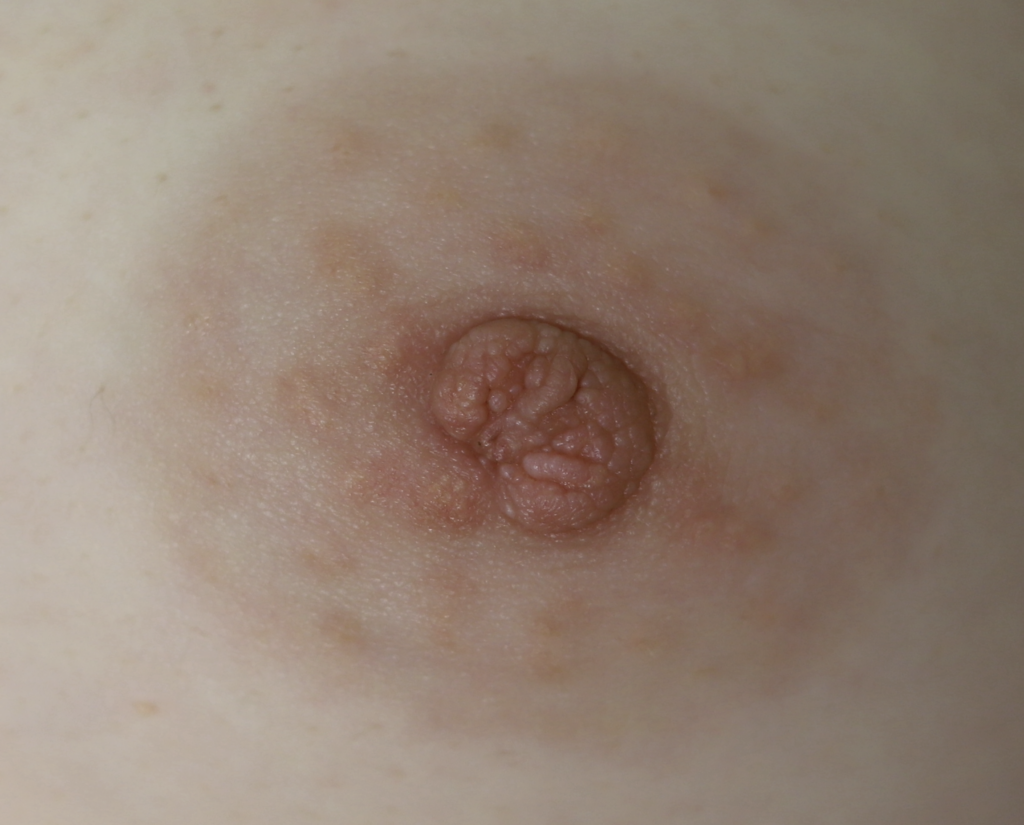
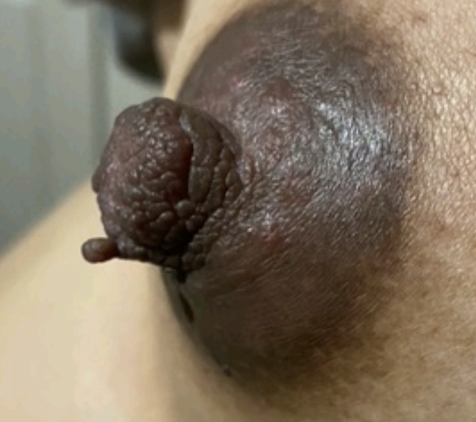
Skin Tags
Skin tags (squamous papillomas) occurring on the nipple areolar complex may enlarge with pregnancy and present an issue with postpartum latch. If concerning, they can be excised under local anesthesia during pregnancy. A non-absorbable suture should be used to reduce tissue reaction and scarring, and a surgical glue may be utilized for smaller lesions that do not necessitate formal closure with suture.





Vasospasm
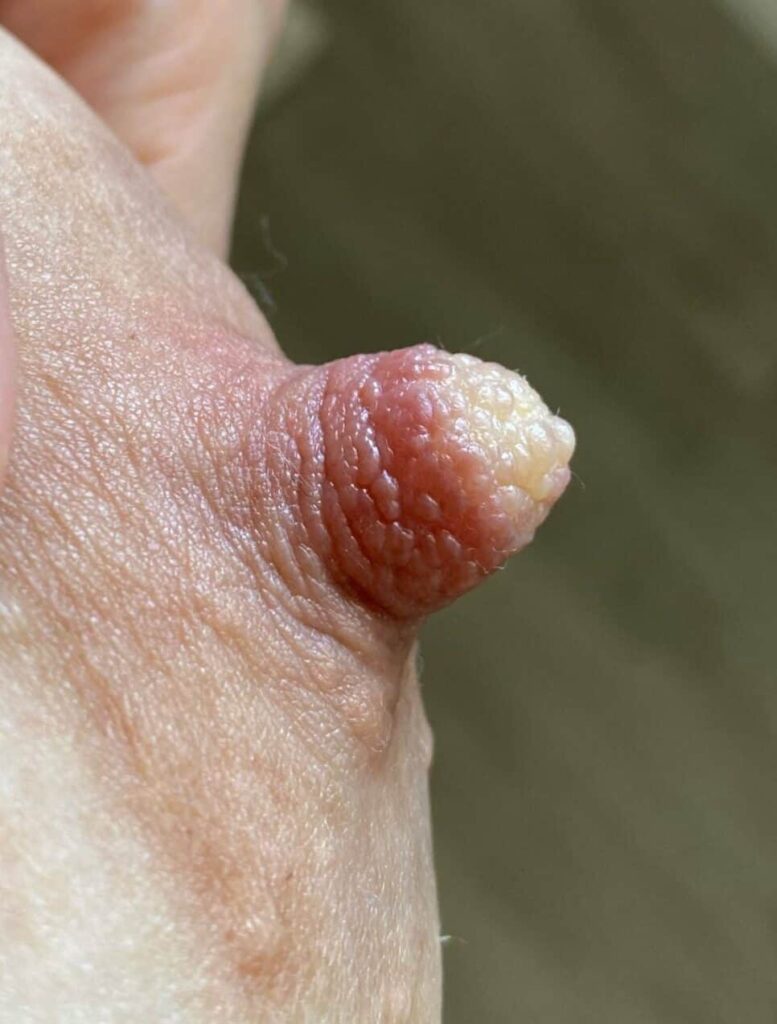
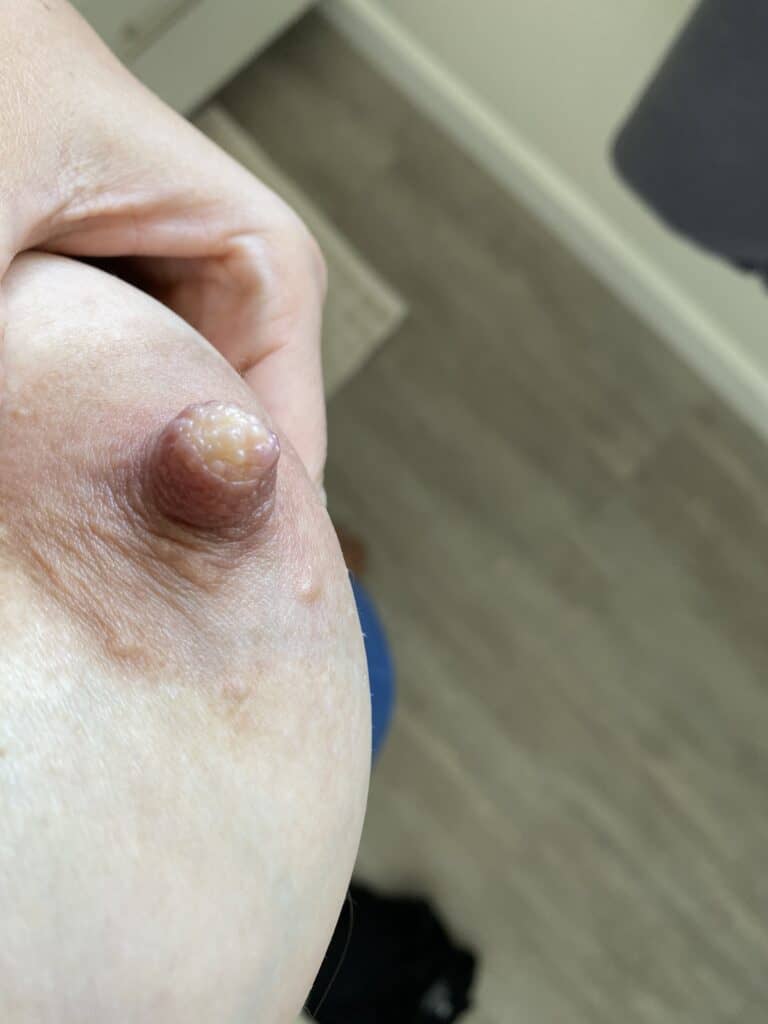
Vasospasm is a painful condition related to changes in blood flow that presents with hardening of the nipple and color changes on a spectrum from white to blue to red. Due to the complex innervation of the breast, pain can focus in the nipple or radiate deep into the breast, and may last for over thirty minutes. Pain often is worst after the baby unlatches or the mother finishes pumping. It also may present when the mother moves from a warm environment to cooler environment, such as leaving the shower or pool, going from indoors to outdoors in the winter, or transitioning from warm weather to air conditioning. It also may have no known trigger.
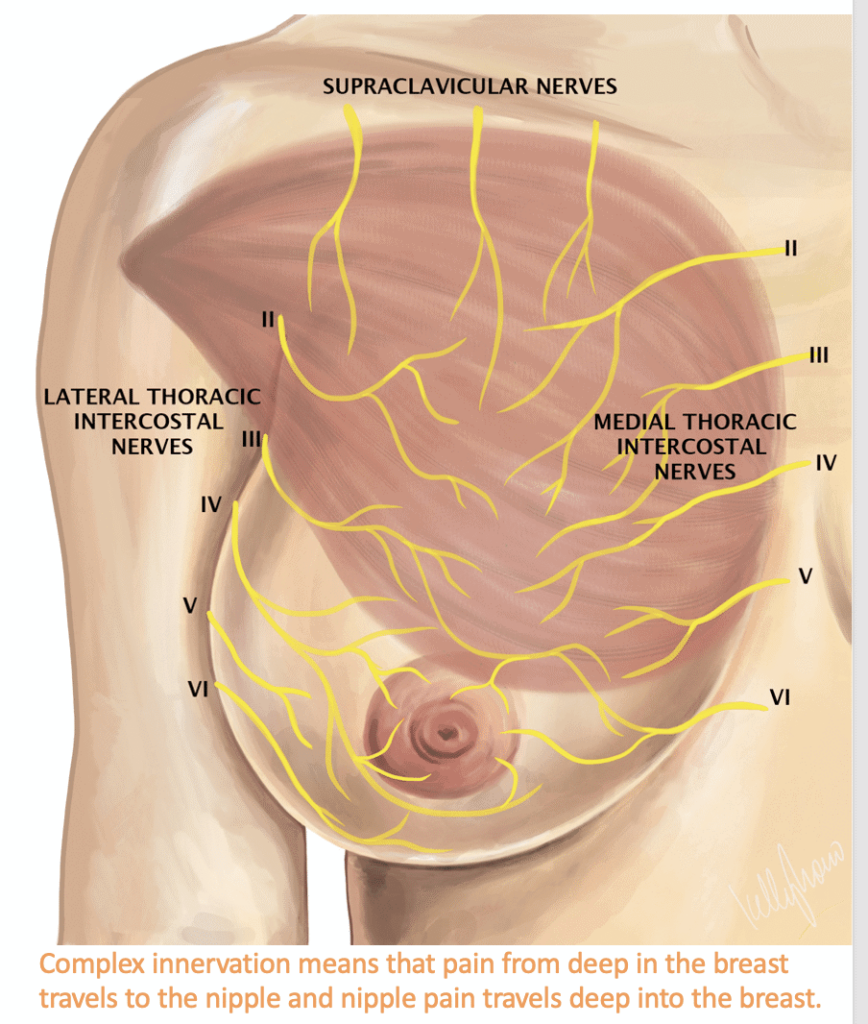
Vasospasm may be more common in those with a history of Raynaud’s phenomenon of the fingers. Secondary vasospasm may occur following trauma to the nipples. Persistent vasospasm can result in a cycle that potentiates trauma, due to vasoconstriction and inability to heal in the setting of chronic alterations in blood flow. Mammary blood vessels are exquisitely sensitive to epinephrine and norepinephrine. Serotonin and PGF20C as vasoconstrictive agents also play a role.
Treatment of vasospasm involves the following:
- Resolve any underlying persistent trauma. Women with larger breasts and/or history of breast augmentation benefit from laid back or side lying nursing positions to reduce trauma from superficial latch.
- Keep nipples at all times (wear a bra at night) with pads made of wool, ThinsulateTM, Flectalon®, or fleece.
- For additional warmth, use heating pads or reusable heated products such as microwaveable rice packs or hand warmers on top of the pads; these products should not be applied directly to the skin due to risk of burns.
- While the calcium channel blocker agents such as nifedipine traditionally have been recommended for intractable vasospasm, the SSRI class of drugs such as sertraline demonstrate remarkable resolution of pain in most patients without the side effects of headache, fatigue, and low blood pressure that the calcium channel blocker class of drug risks. The effectiveness of the SSRI class of drugs is likely due to the activity of serotonin in the breast.
Viral Infections
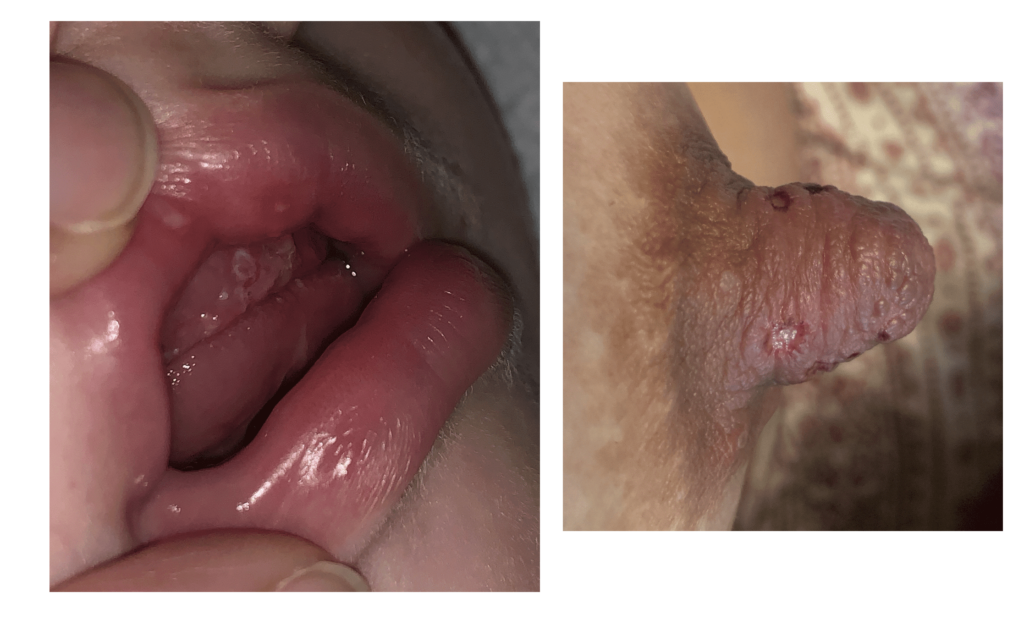
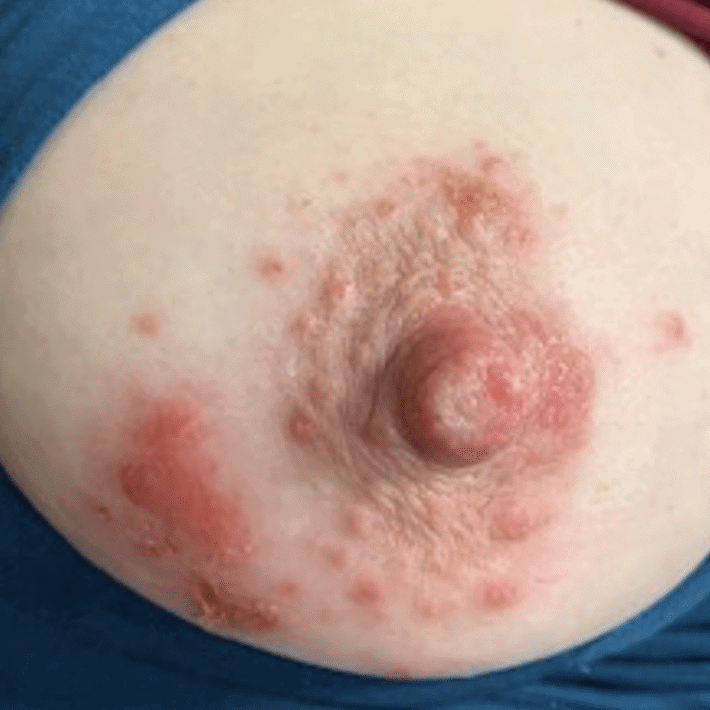
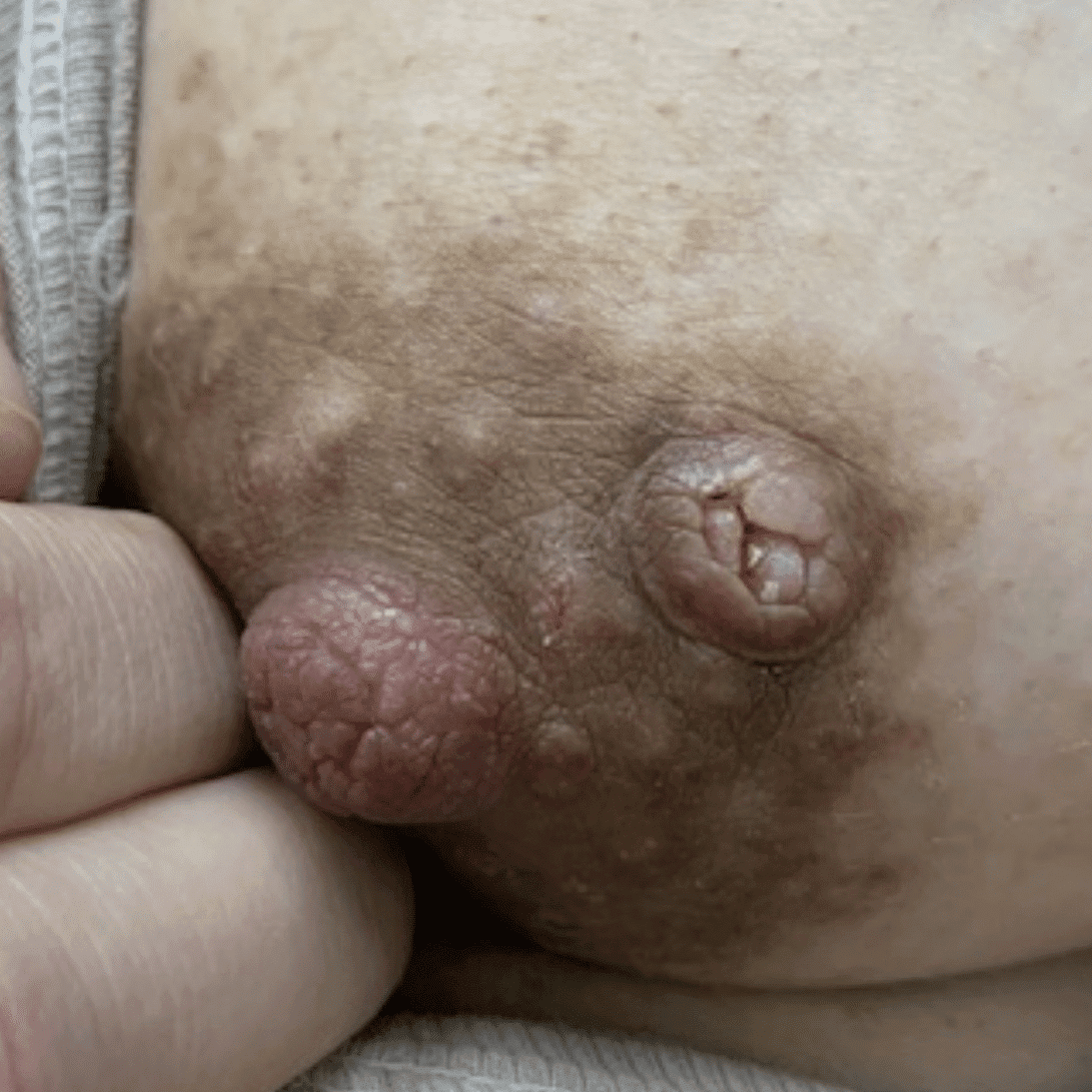
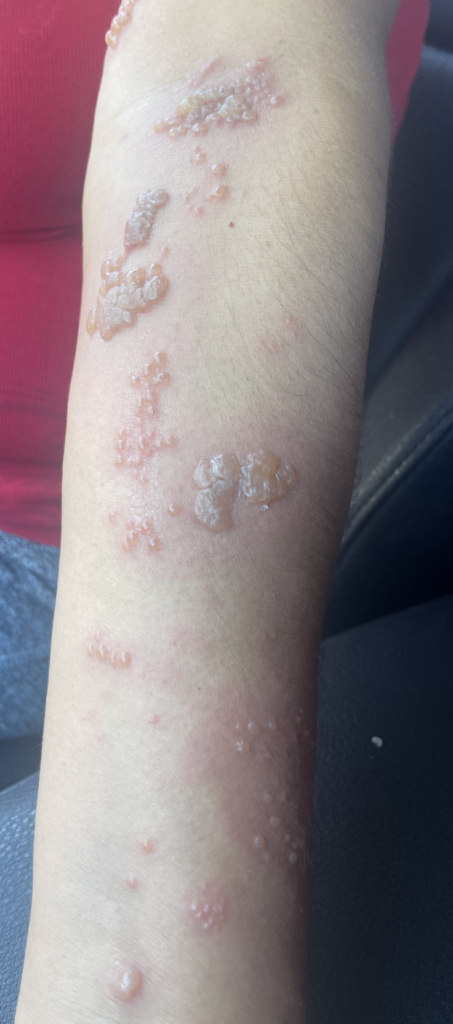
The lactating breast and nipple areolar complex are highly vascular and therefore heal well and are unlikely to develop bacterial infection. However, viral infections with herpes and warts from HPV are more common.
Herpes simplex virus (HSV) infection (“cold sores”) of the nipple areolar complex presents as a cluster of tender vesicles. The virus can pass between mom and baby, and can be dangerous to neonates with immature immune systems under three months of age. If a neonate under the age of three months presents with suspected neonatal herpes, the infant should undergo blood and spinal fluid testing for HSV to confirm diagnosis, and begin immediate treatment with acyclovir. Diagnosis in the mom can be confirmed using a skin swab culture or blood testing.
Moms with a herpes outbreak undergo treatment with a five to seven day course of acyclovir, which is safe in lactation. If a mom experiences a herpes outbreak on one breast, she can continue to express and discard the milk to maintain milk production. However, she should keep this breast covered until lesions scab over, and the infant should nurse only from the unaffected breast. There is no recommendation for routine suppression in breastfeeding mothers with a history of HSV-1 to prevent transmission to infants.
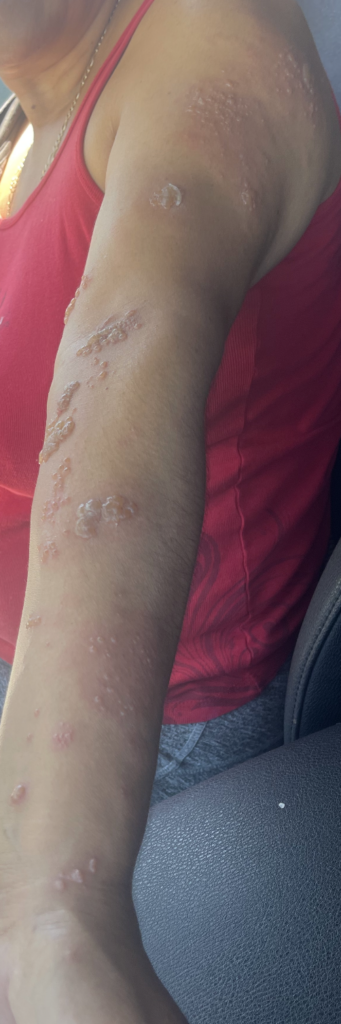
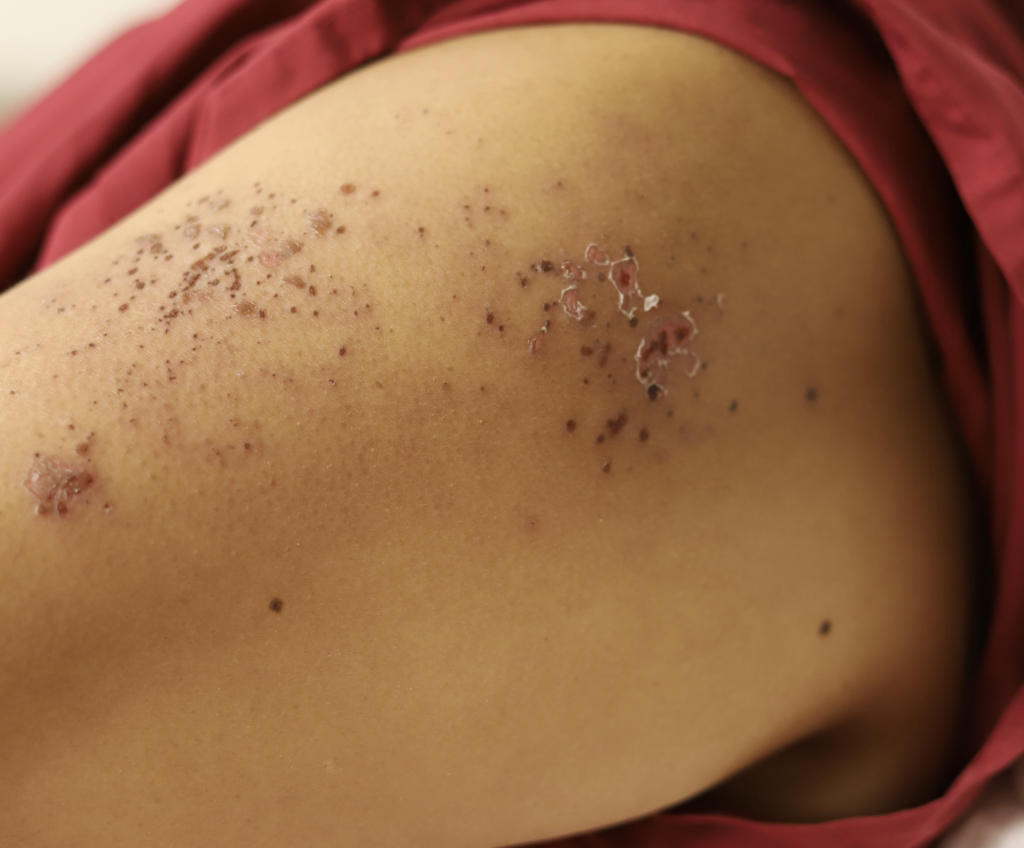
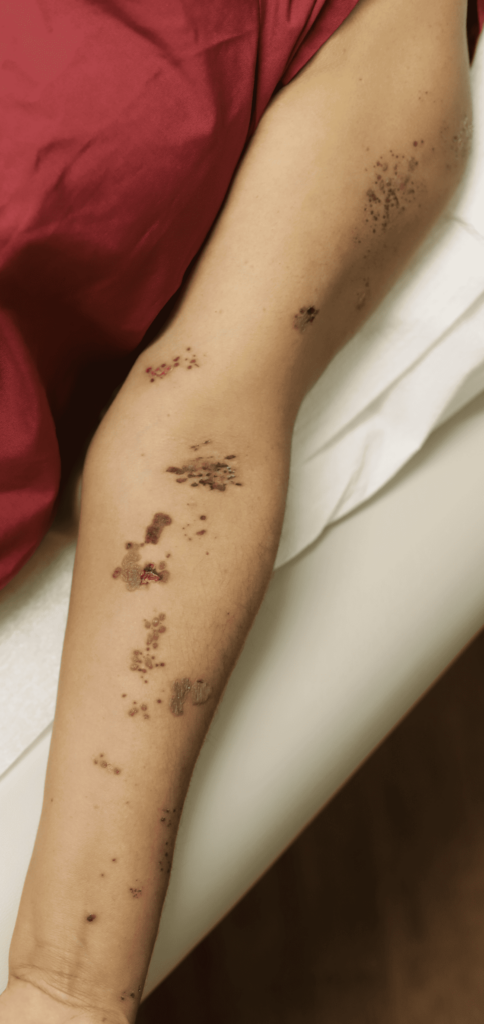
The varicella zoster virus remains dormant in nerve tissue of individuals with a history of chickenpox. Reactivation of the virus results in herpes zoster, a contagious rash in a specific “dermatomal” distribution. Until lesions are crusted over, women with vesicles on the nipple areolar complex should avoid breastfeeding from the affected breast. During that time, milk should be expressed to maintain production, but is not safe to feed to the infant.
Viral warts (verruca vulgaris) are benign (non-cancerous) tumors that arise from infection of the skin or mucosal cells (e.g. mouth, vagina) from infection with the HPV virus. They may clear spontaneously, or may need excision if large and on the areola. Other therapies include salicylic acid, cryotherapy, and laser treatment.