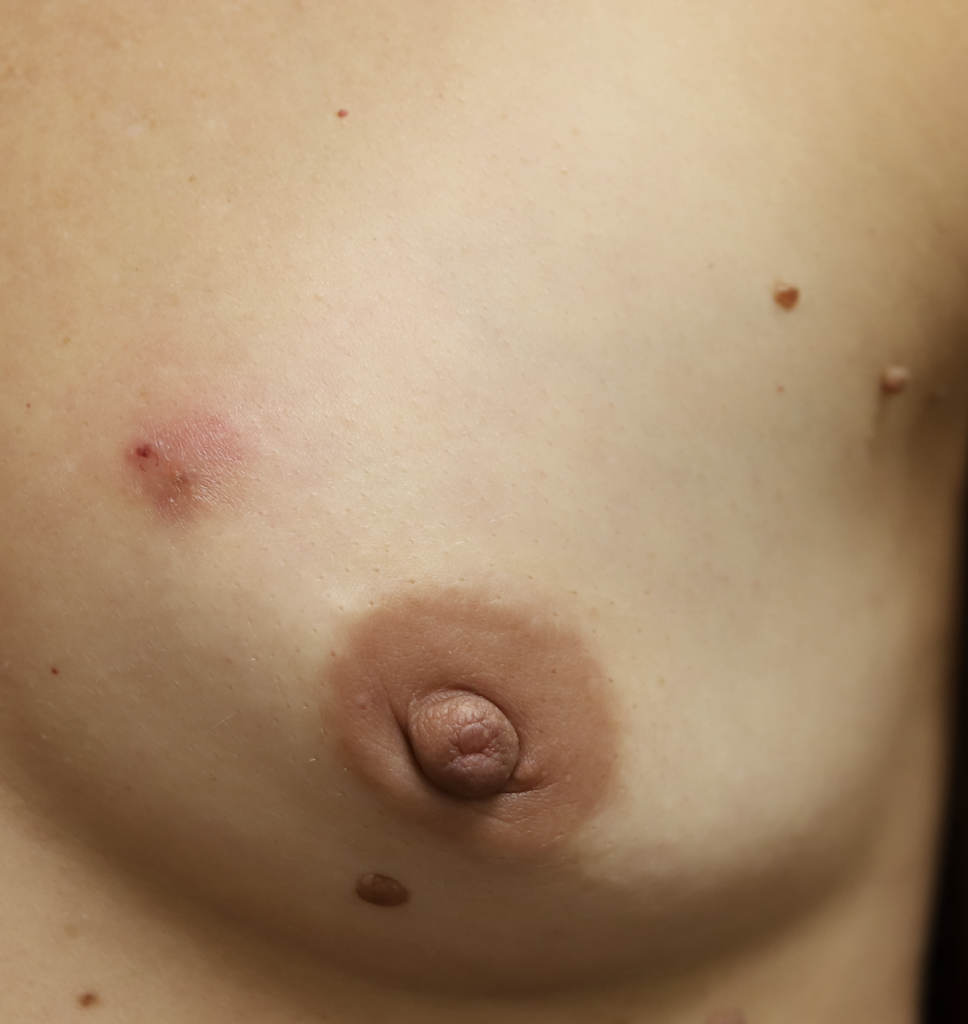
Breast Masses and Conditions
Gigantomastia
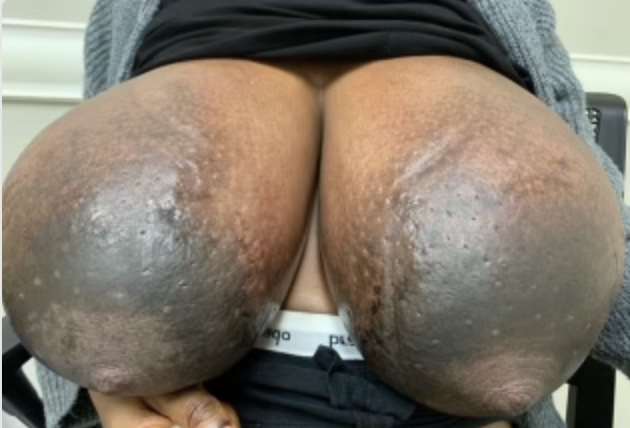
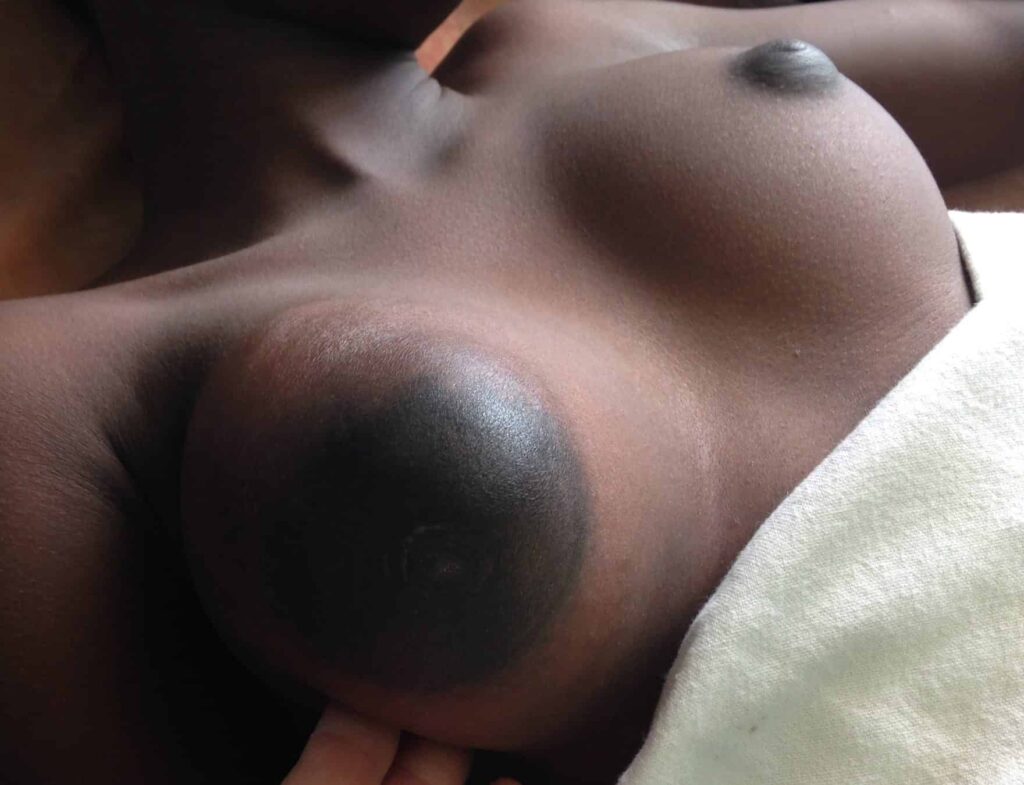
Gestational gigantomastia likely represents a spectrum of excessive breast growth during pregnancy. It may include women who grow multiple cup sizes, or those for whom the breast growth is so significant it can cause mobility impairments. Hormonal factors may play a role in gigantomastia, but true cause remains unknown. It also remains unclear whether the growth represents true glandular development or simply fluid retention in the breast as occurs in other parts of the body during pregnancy. Women gigantomastia that is not significant enough to cause skin breakdown but do experience growth do not necessarily produce large volumes of milk.
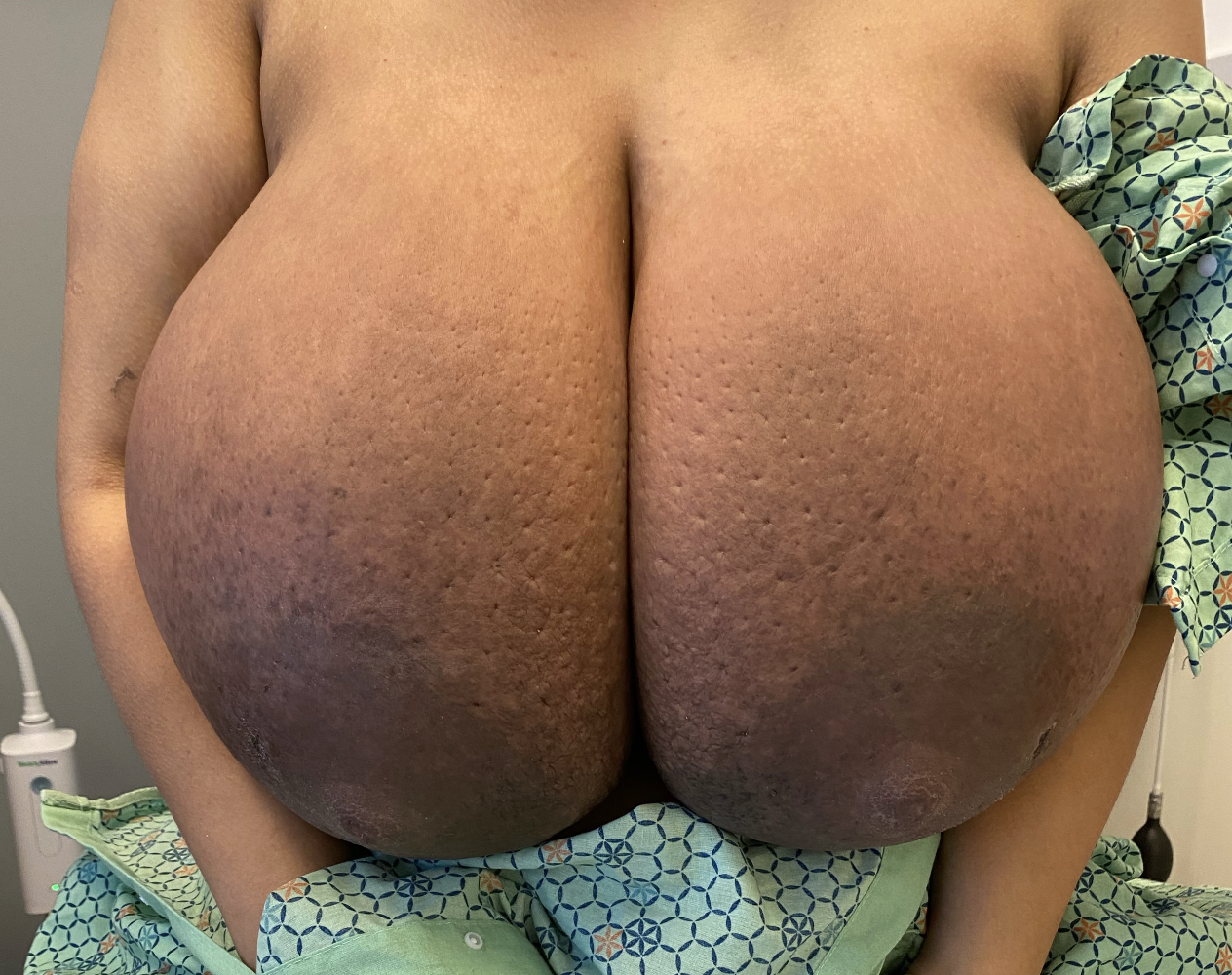 Photo: Clara Farley
Photo: Clara Farley
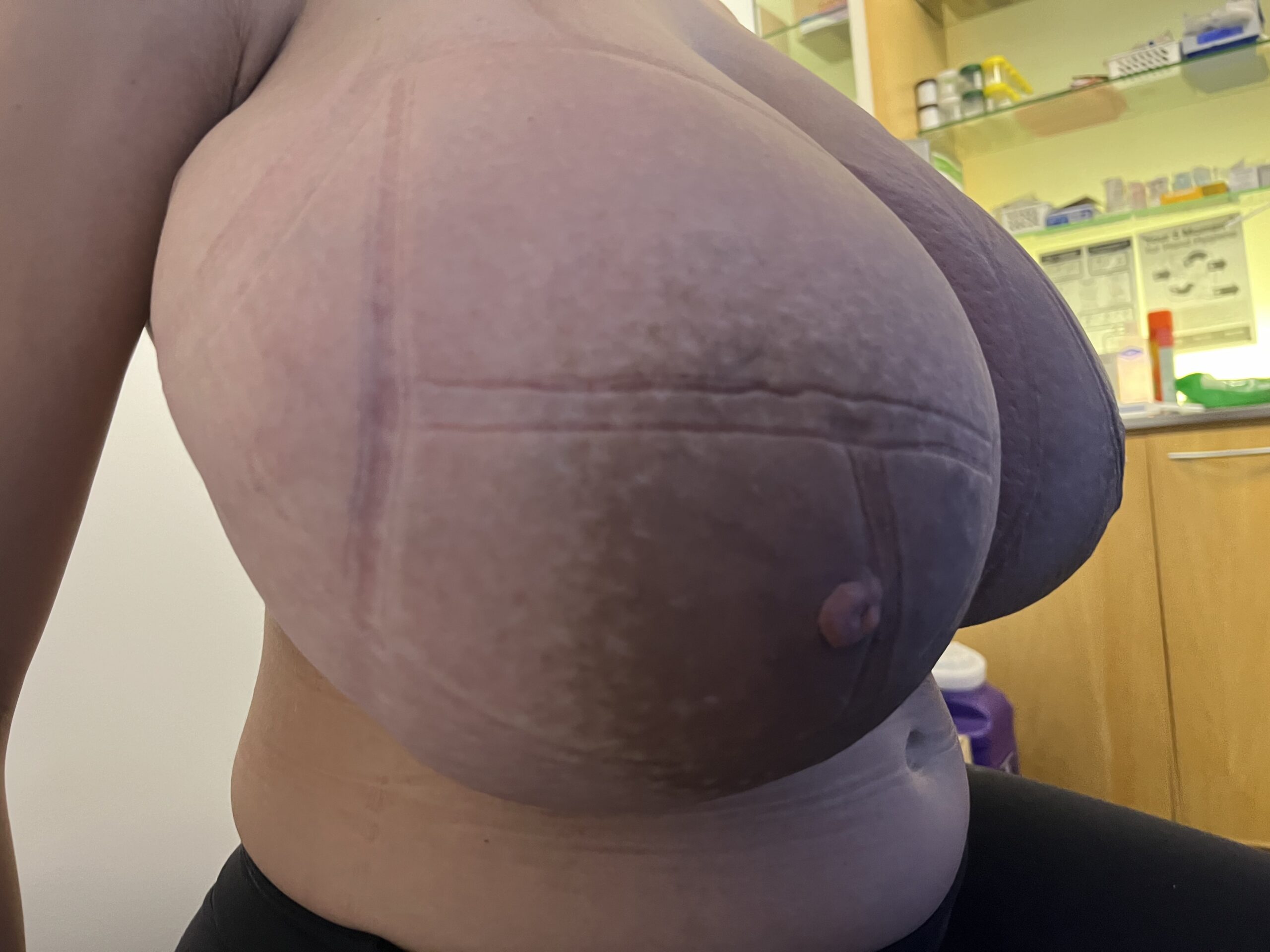 Photo: Clara Farley
Photo: Clara Farley
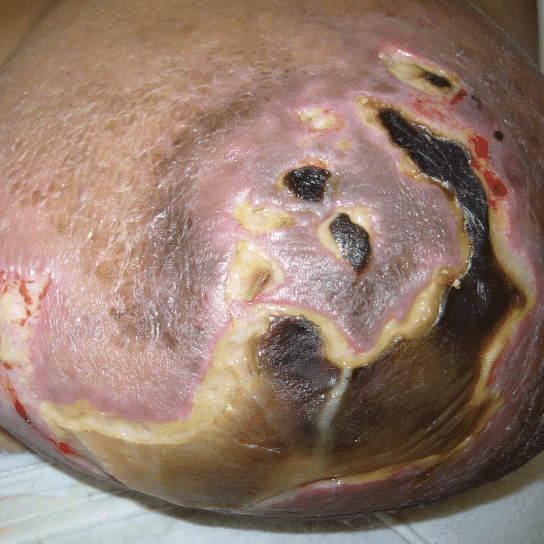
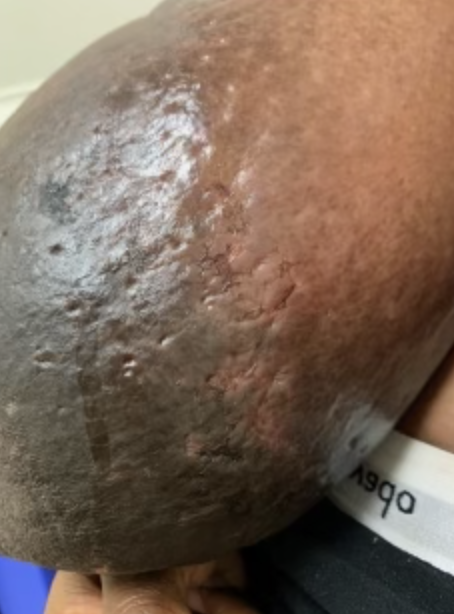
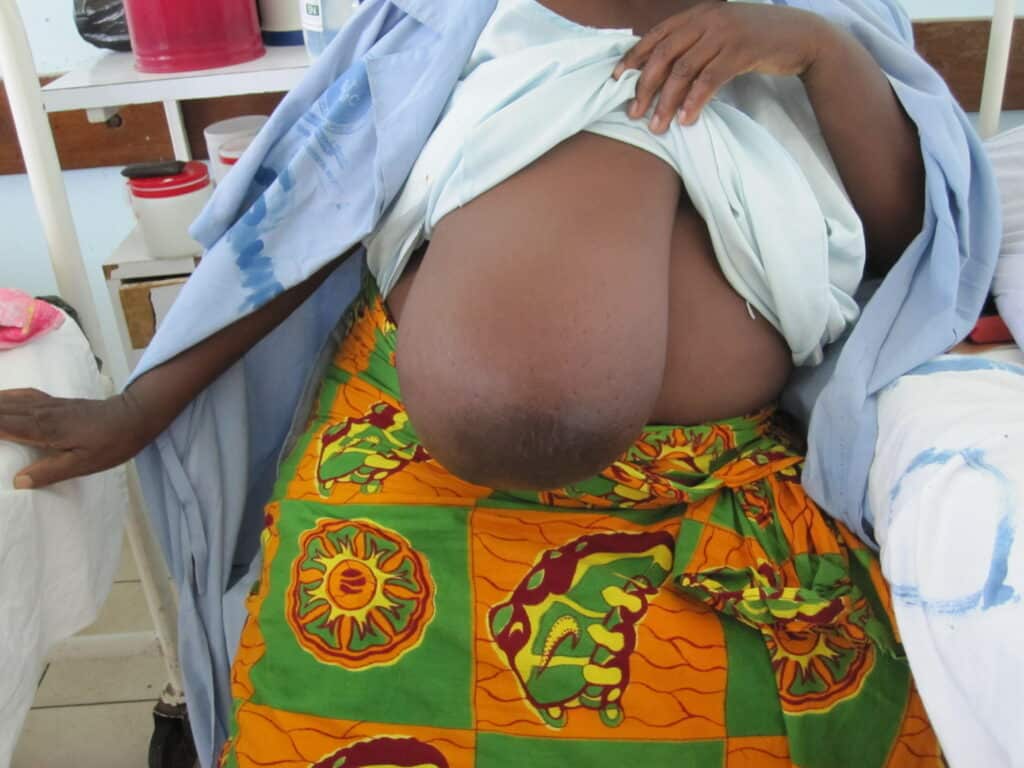
During pregnancy, it is treated by bromocriptine (an anti-prolactin agent) alternating with metformin (modulates insulin). Postpartum, patients should be given bromocriptine or cabergoline (anti-prolactin agent) before lactogenesis II (secretory activation, or “milk coming in”) to reduce the risk of skin necrosis (ulceration and death of skin). Donor milk or formula supplementation should be planned. Patients can later undergo elective breast reduction. The patient above is pictured below at end of pregnancy after being treated with lymphatic drainage and bromocriptine during pregnancy:

Improvement in lymphedema with lymphatic drainage and supportive bra/garment, just before delivery. Photo: Clara Farley, MD

Engorgement, Lymphedema, and Pain
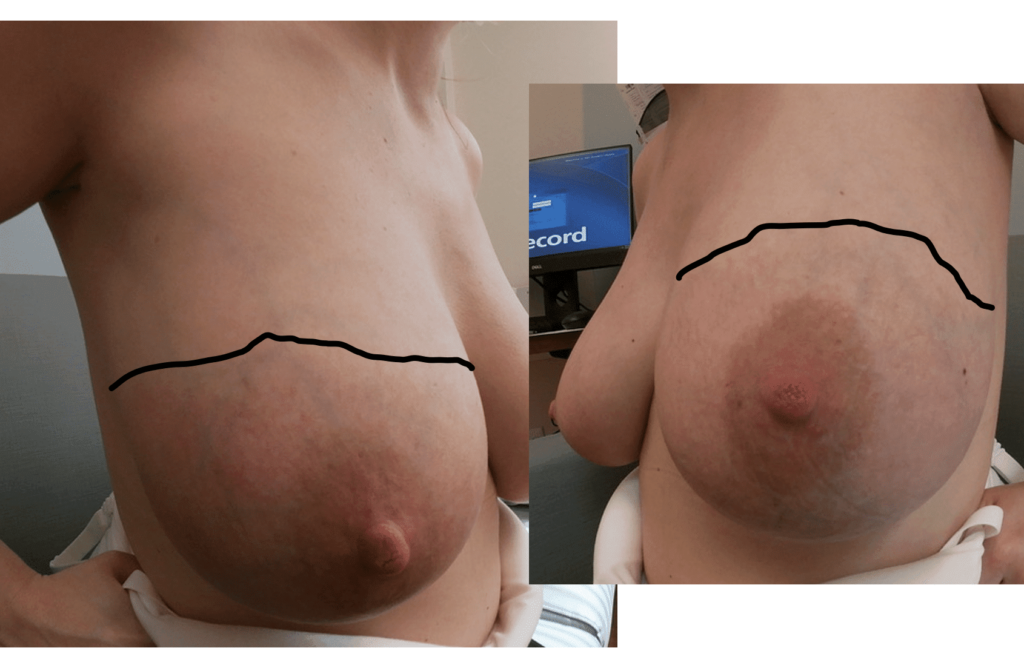
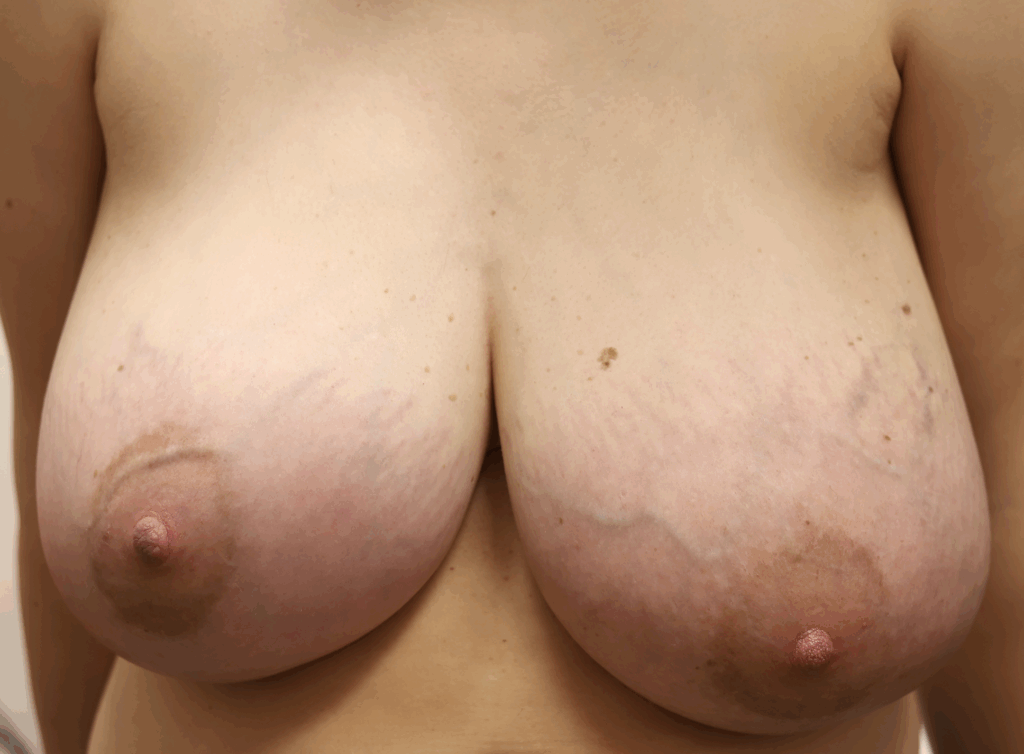
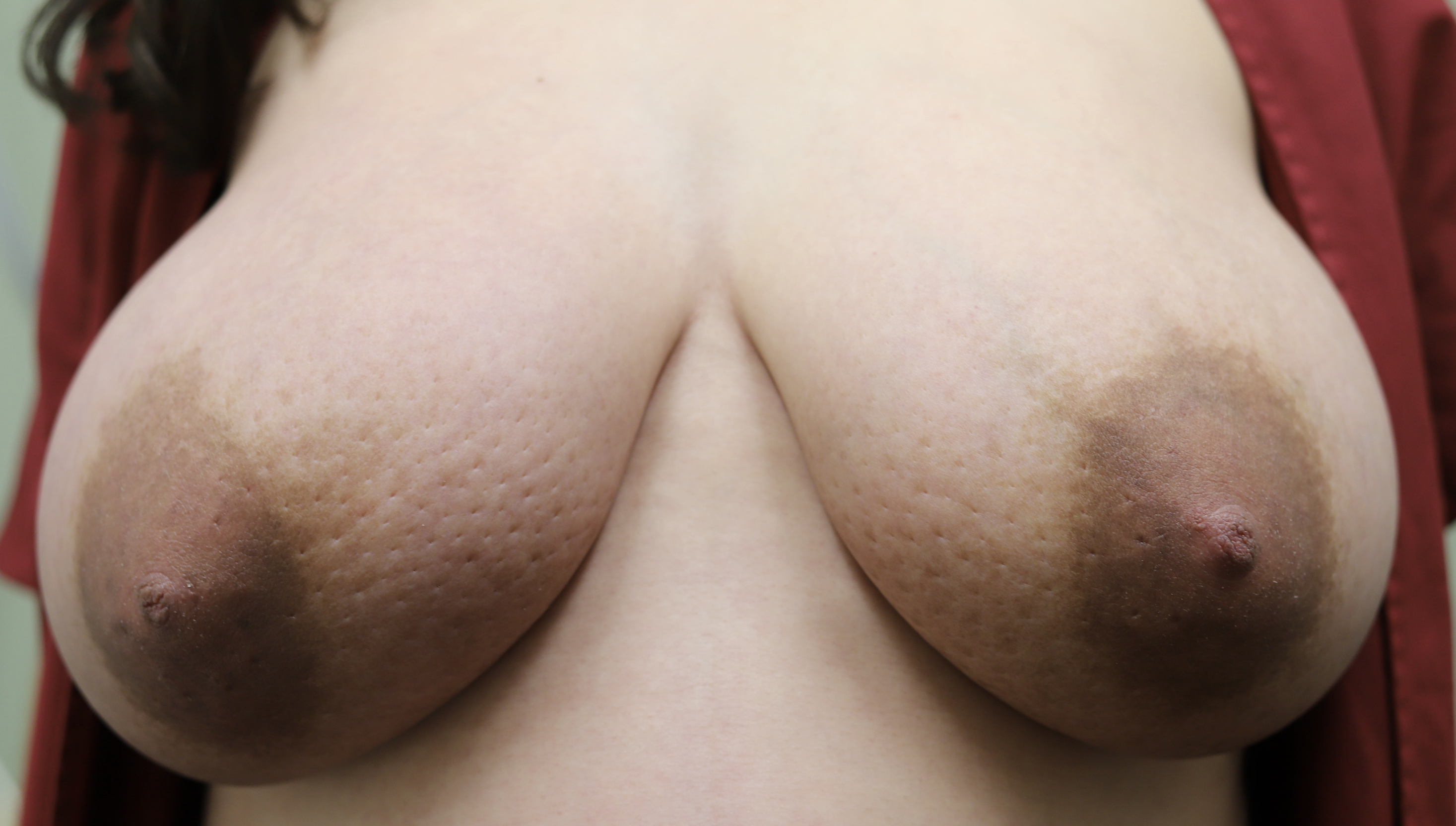
As discussed in the Pregnancy and Birth section, women may experience breast lymphedema (swollen breast) and pain, particularly during periods of early breast growth in the first trimester and in the last trimester nearing childbirth. This is more common than true gigantomastia. This discomfort is related to increase in the gland, blood vessels, and surrounding fluid. Swelling and even pitting usually is most evident in the lower part of the breast, and can be pink or mildly reddish in color. These cases also. can gain significant relief from lymphatic massage and supportive bras. Any asymmetry in presentation warrants referral to a breast surgeon to evaluate for breast masses and/or inflammatory breast cancer.




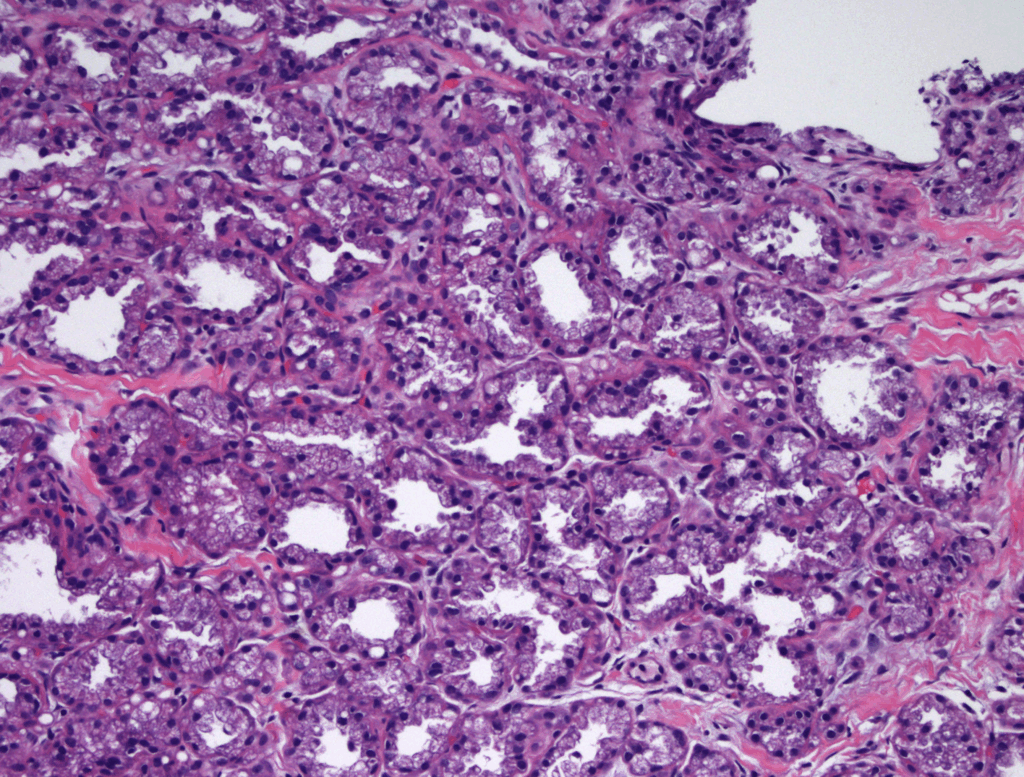
Lactating Adenoma
Lactating adenomas are benign (non-cancerous) masses comprised of dense glandular tissue and most commonly occur in the upper outer part of the breast. They can present during pregnancy or lactation and likely are related to hormonal stimulation. They may become large; however, they reduce in size as a woman progresses further in the postpartum period and eventually disappear when lactation is complete. They can appear similar to fibroadenoma on breast imaging, as smooth, oval lesions. Diagnosis can be confirmed with a core needle biopsy, but they do not require surgical excision.

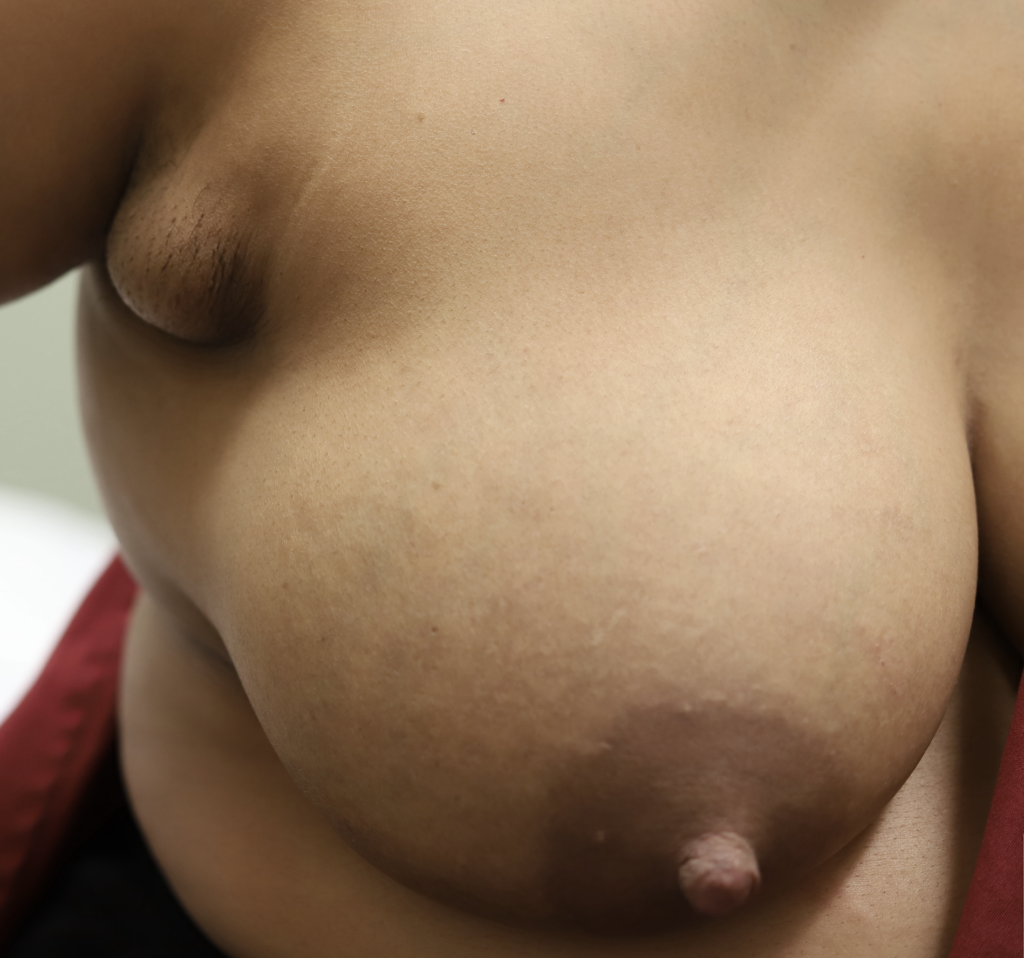
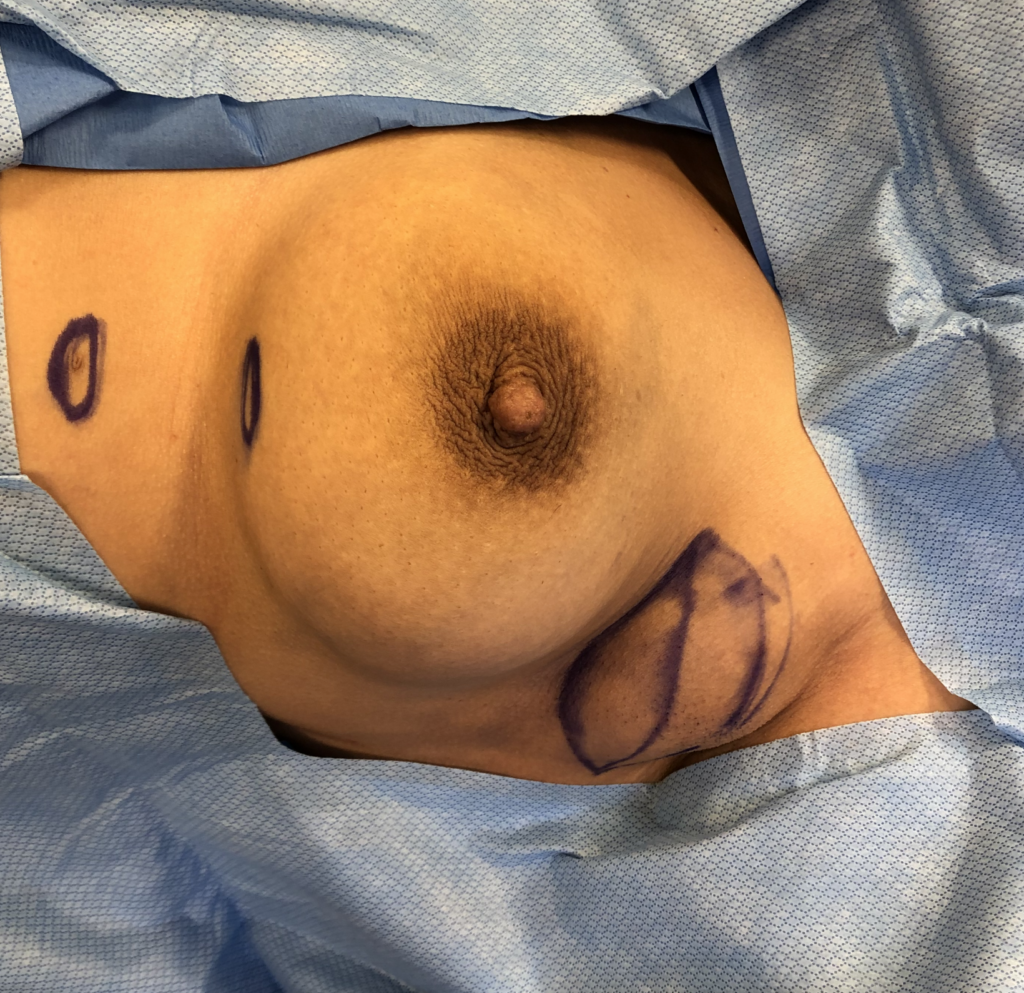
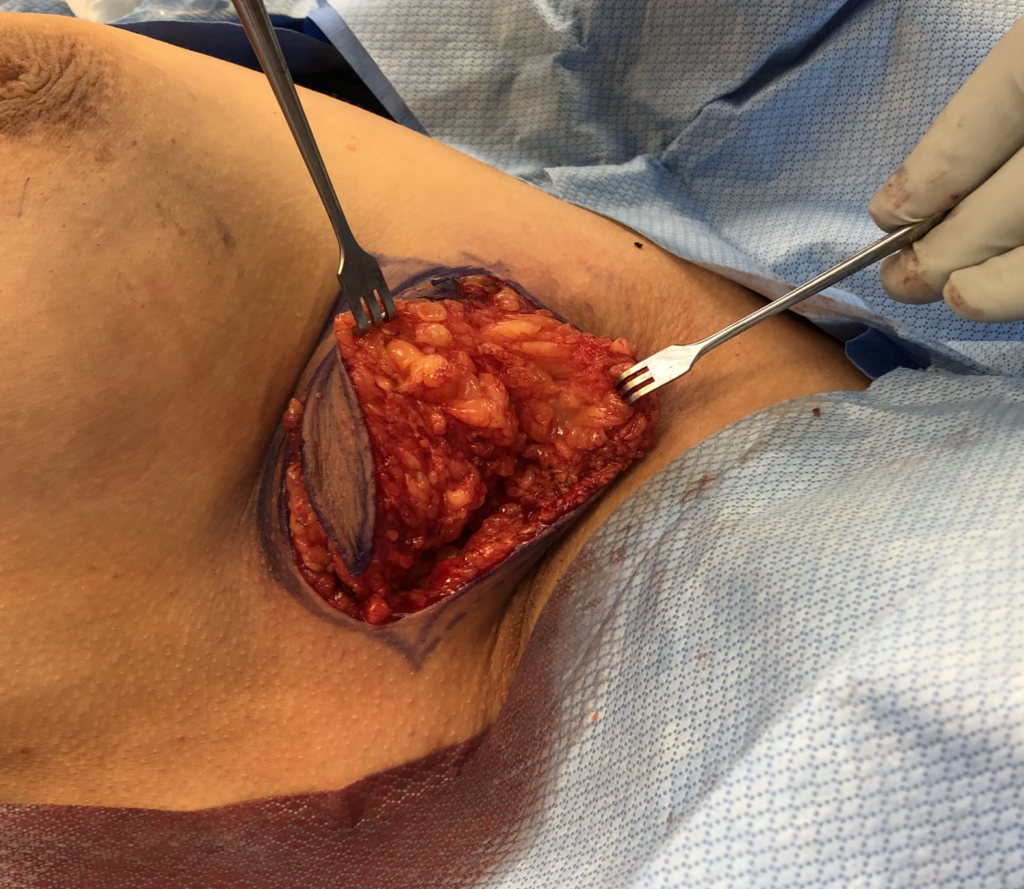
Axillary Tissue
Accessory breast tissue in the axilla (under the arm) is common. It often grows during pregnancy and lactation. If not stimulated, it will regress within one week. Do not massage the accessory tissue as this can cause trauma and swelling. Treat with Top images: Early inflammatory mastitis. Bottom images: Resolved with BAIT (Breast Rest, Advil, Ice, Tylenol) no massage, no overfeeding or pumping, and therapeutic ultrasound.. It can be excised between pregnancies if extremely bothersome, or after childbearing is complete.
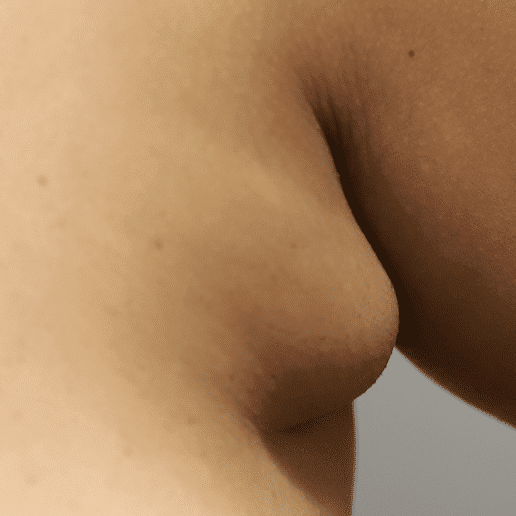

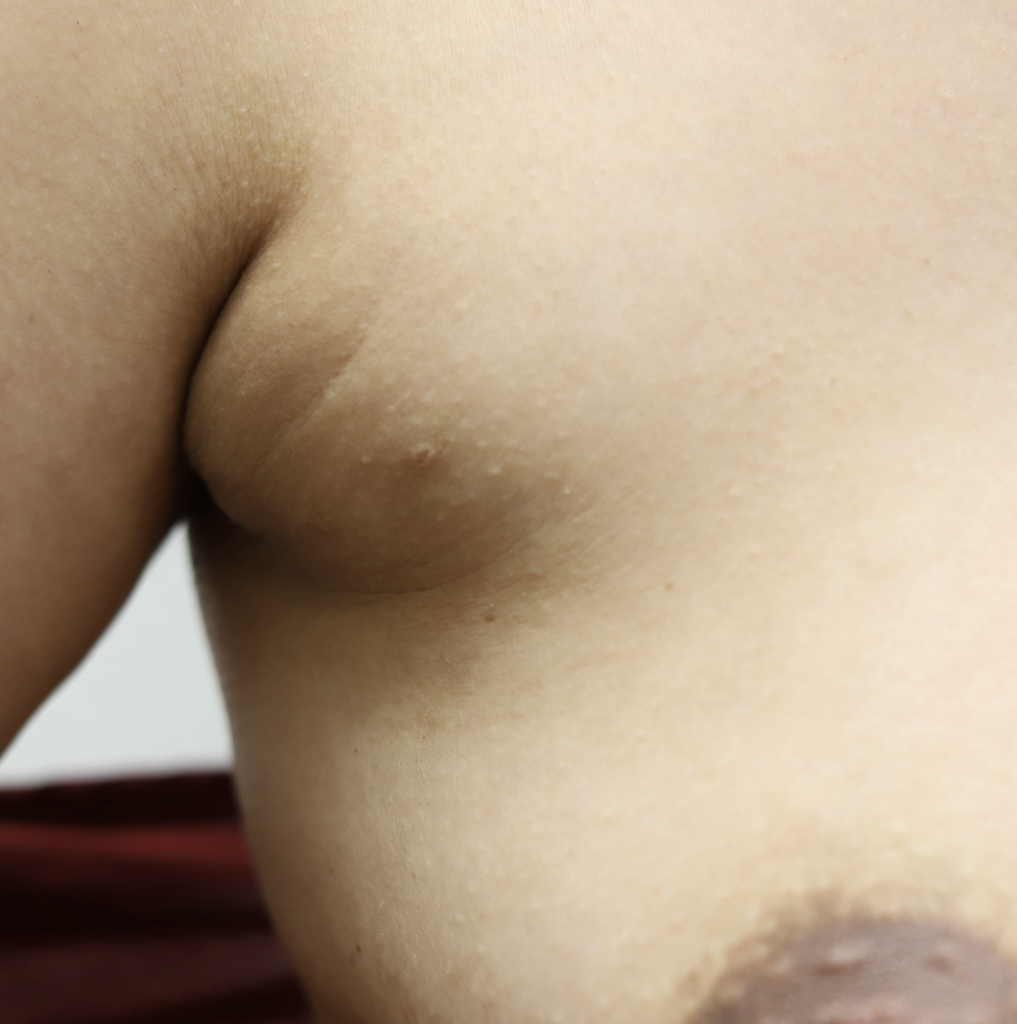
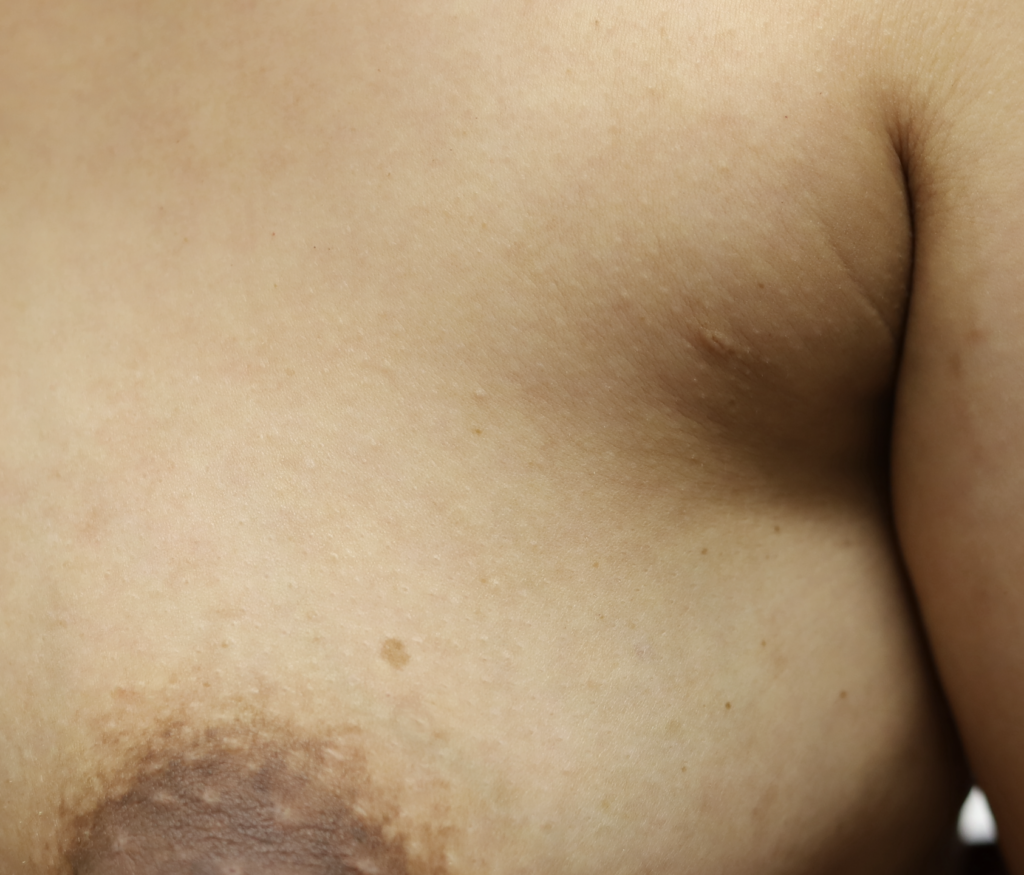
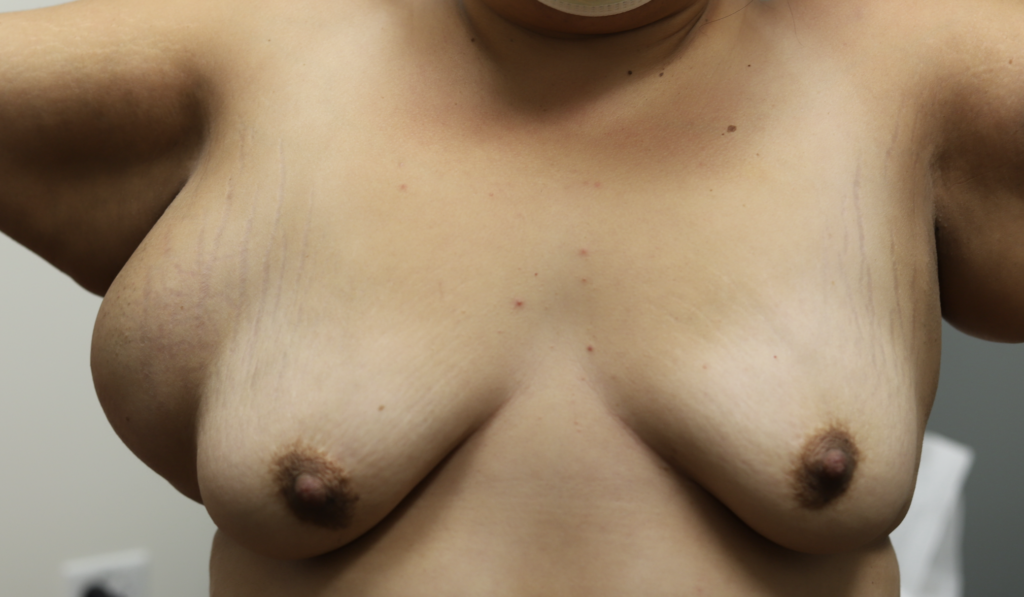
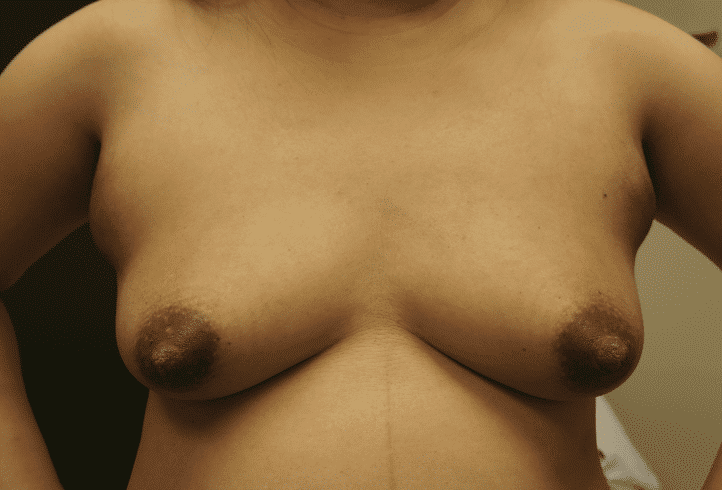
Lymph Nodes
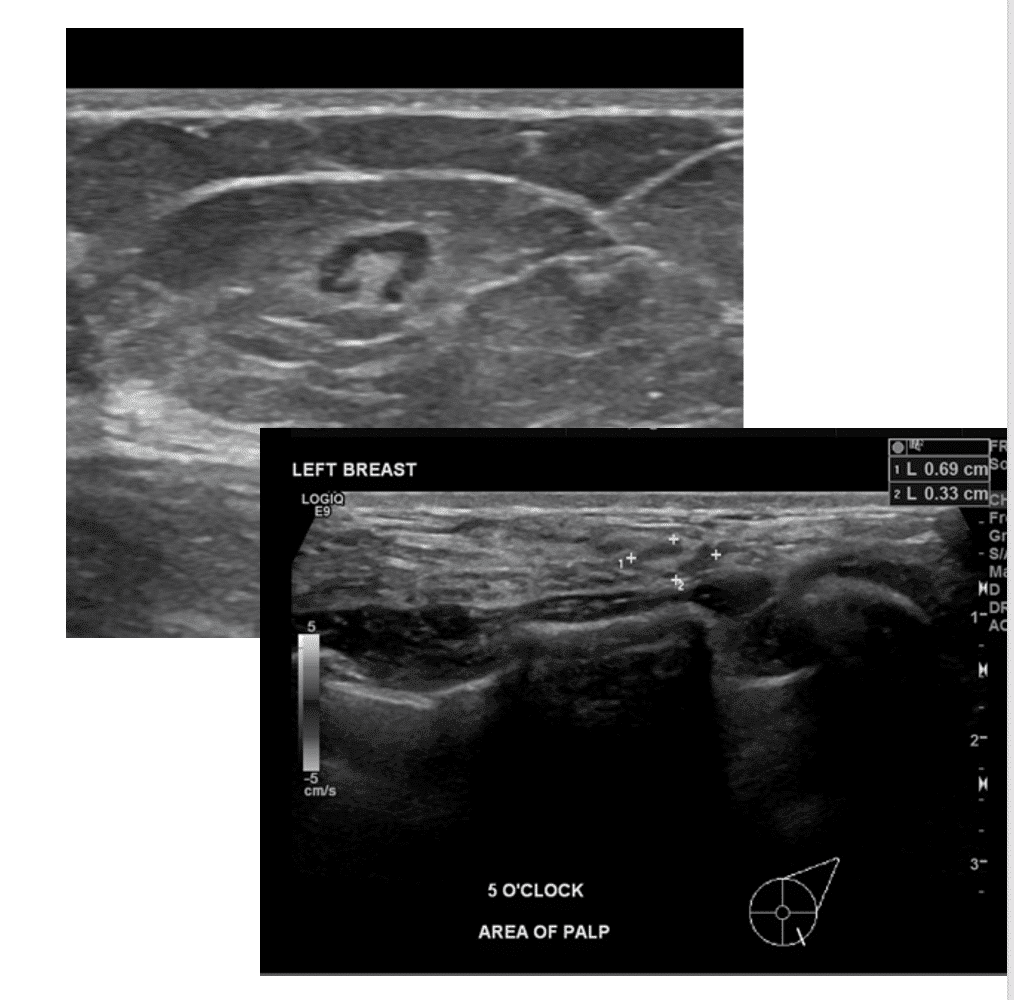
Prominent lymph nodes are common during lactation, both in lymph nodes under the arm (axilla) or within the breast (intramammary lymph nodes), which often are noticed by thinner individuals with smaller breasts. Ultrasound and/or mammogram can be obtained to confirm benign appearance.
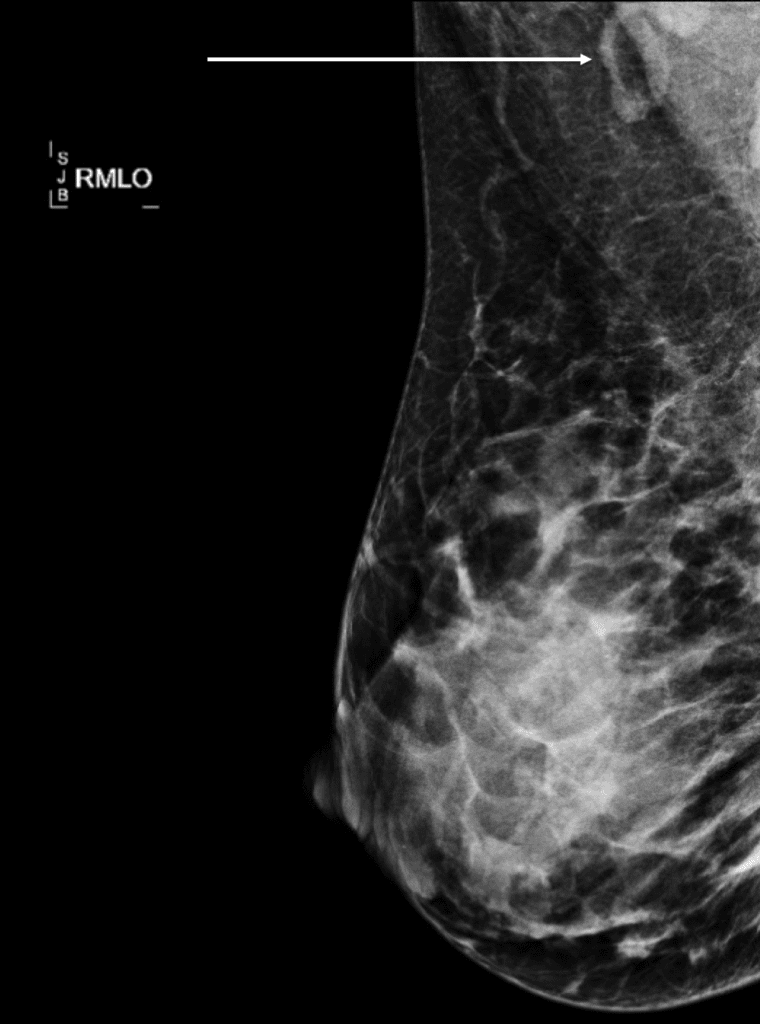
Fat Necrosis
Fat necrosis (literally, death of fat cells) is a common phenomenon and can occur after trauma or breast surgery. It can feel worrisome and look worrisome on imaging, but and sometimes needle biopsy is necessary to confirm the diagnosis
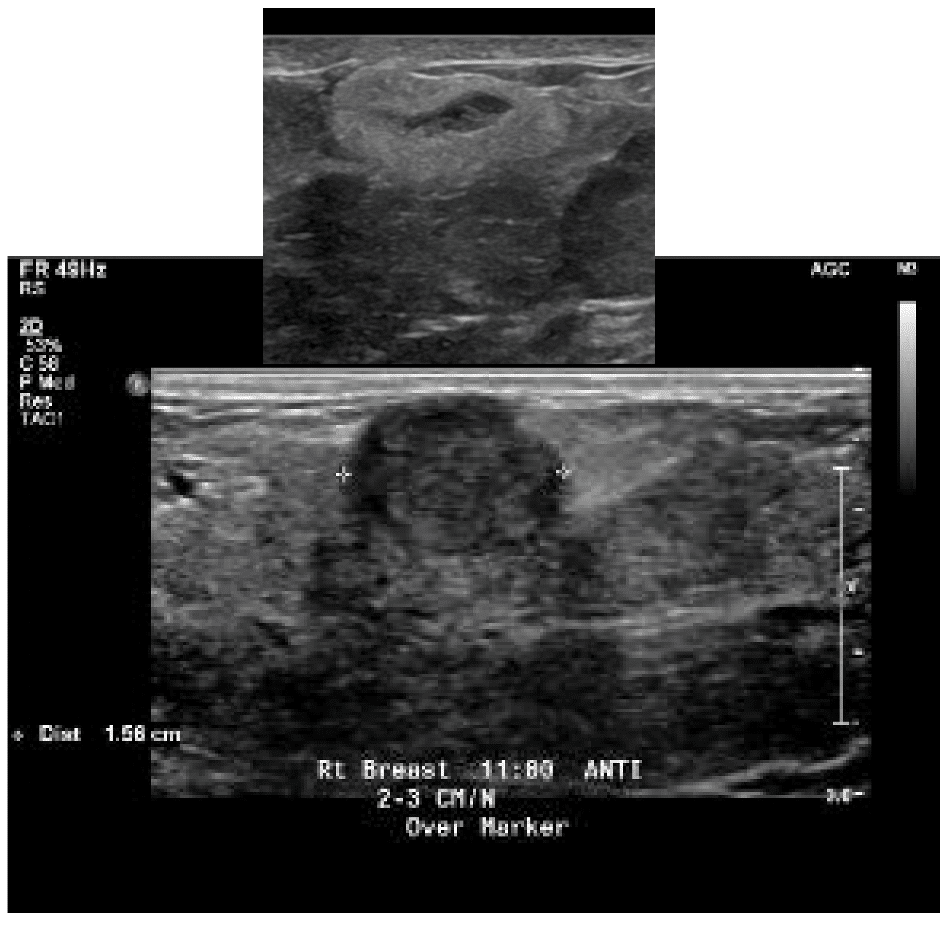
Idiopathic Granulomatous Mastitis (IGM or GM)
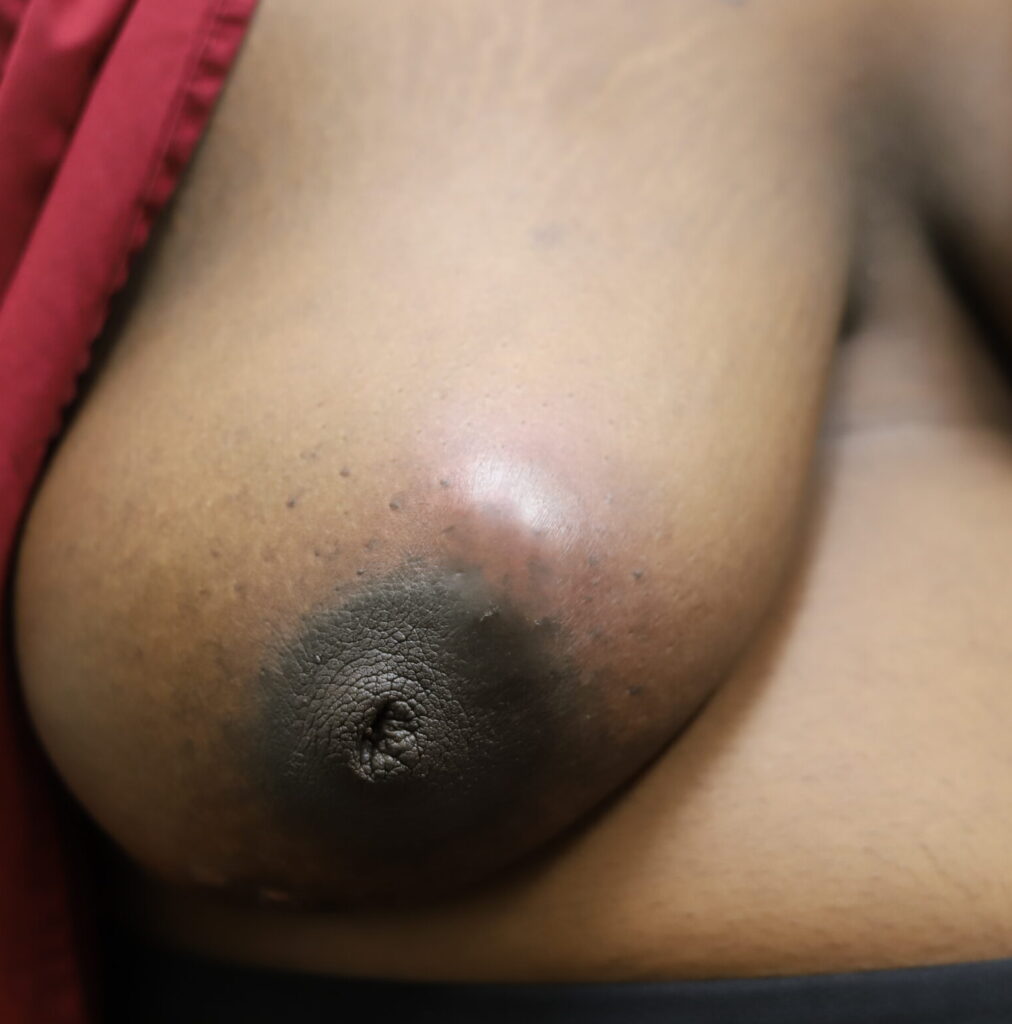
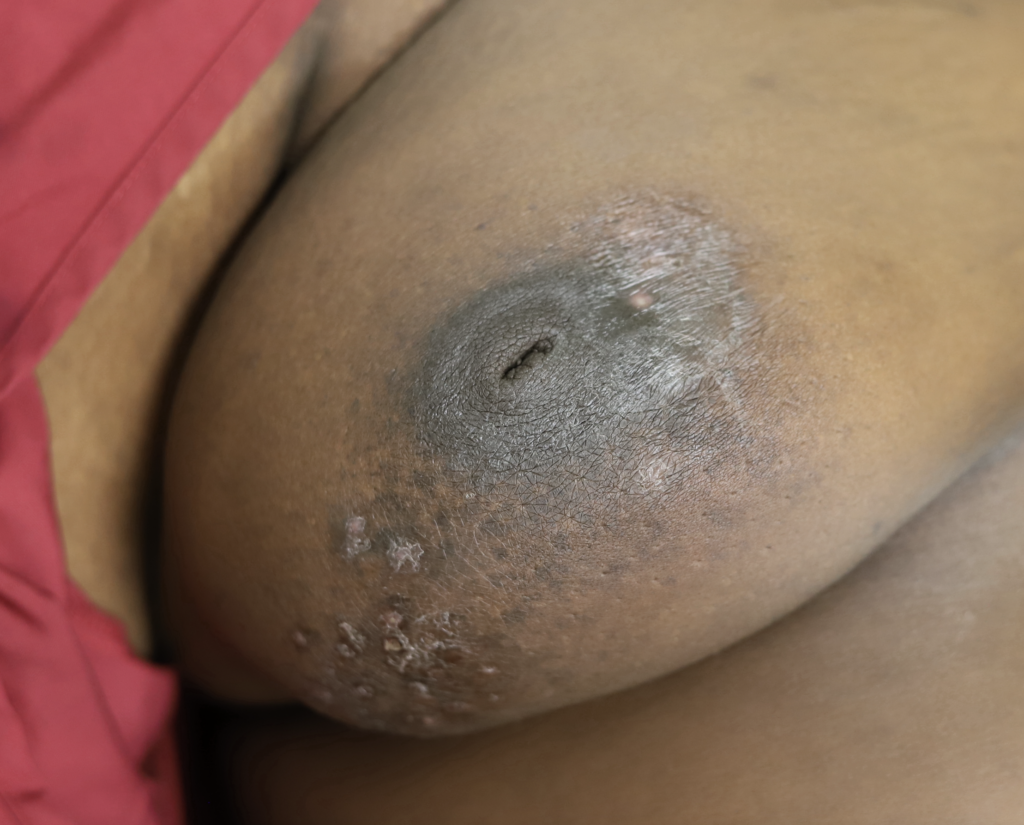
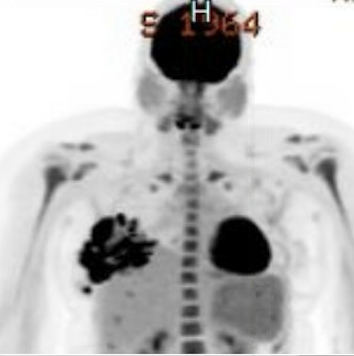
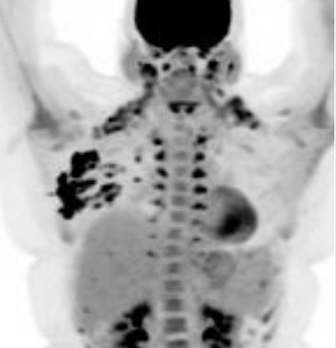
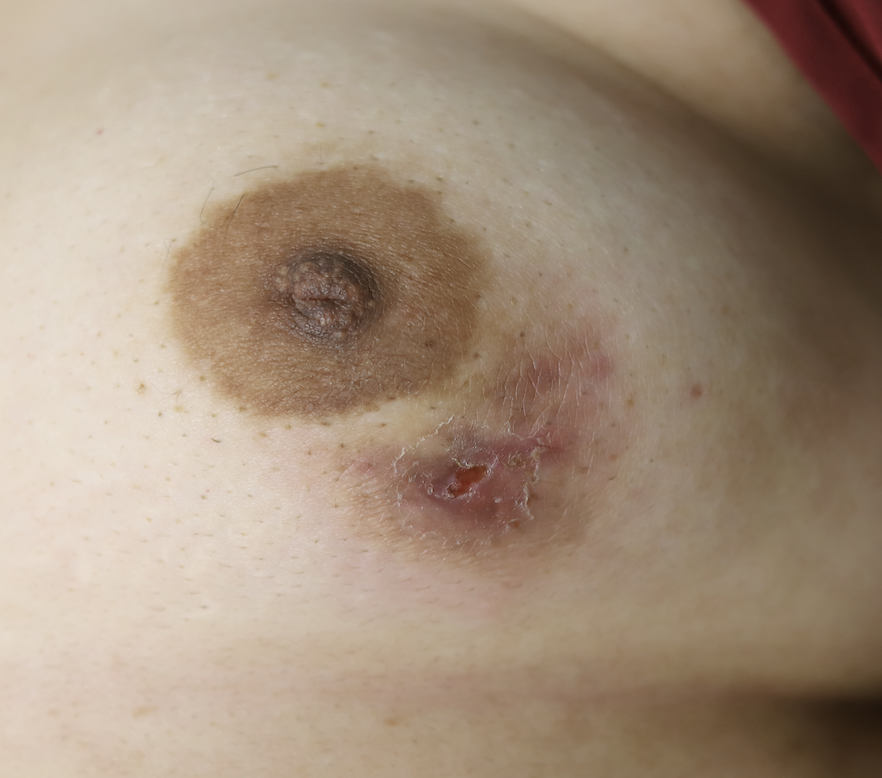
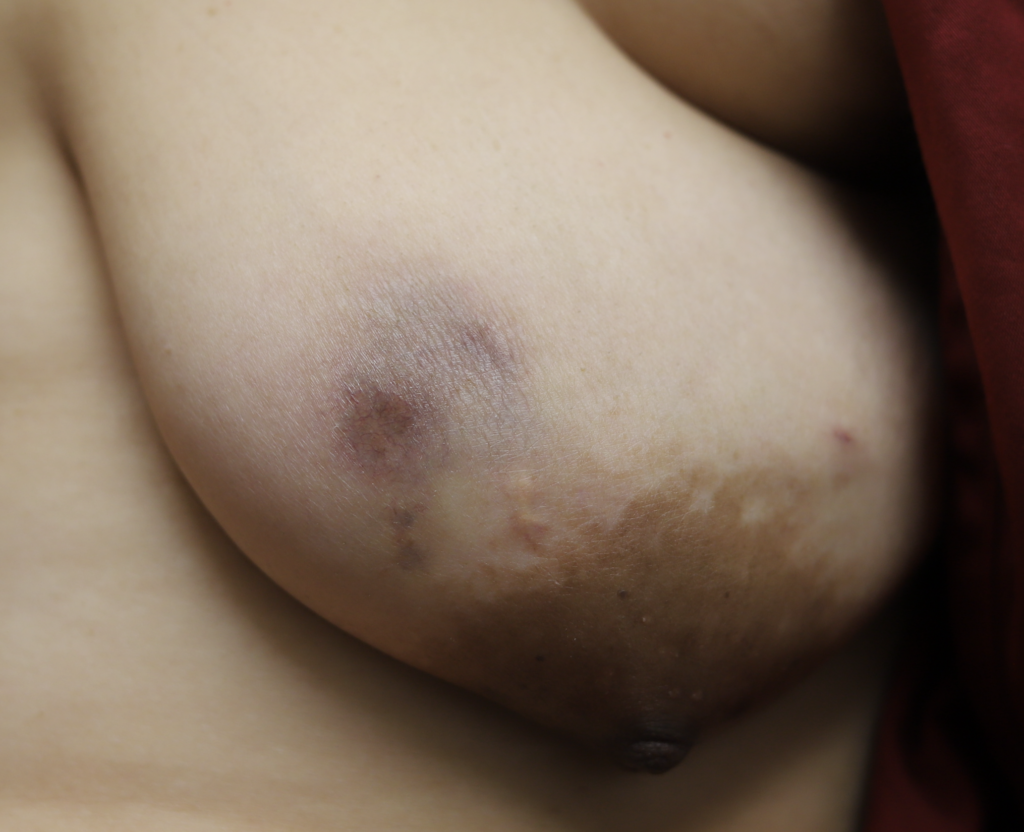
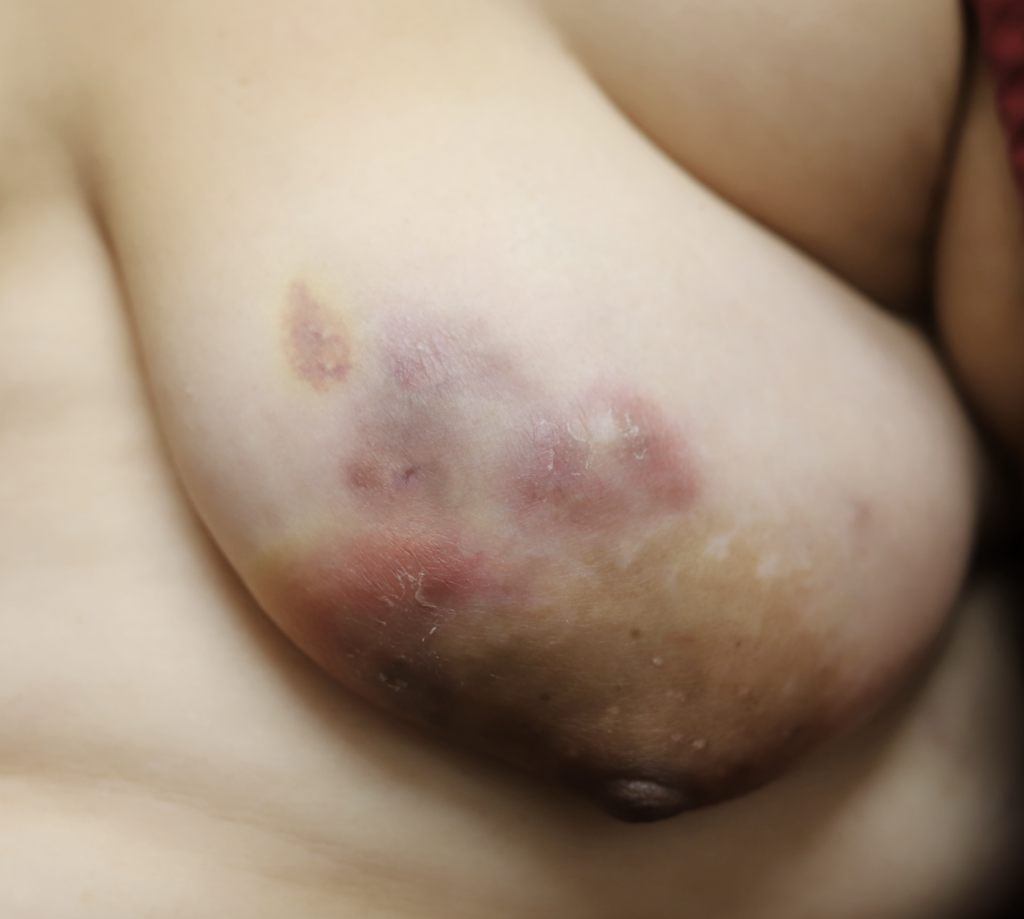
Idiopathic granulomatous mastitis (IGM) is an inflammatory disorder affecting the breast of young women in their childbearing years, and can overlap with lactation and pregnancy. It can result in development of painful inflammatory masses, fluid collections, and fistula formation. While breastfeeding from the affected breast in the setting of IGM is safe, many mothers report significant pain and difficulty with latch or milk production.
The definitive treatment for IGM is immunosuppression with the oral medications methotrexate (not safe with lactation or pregnancy) or azathioprine (safe with pregnancy and lactation). This case report describes continued breastfeeding and resolution of IGM with azathioprine therapy.
A really amazing addition to IGM treatment has been low dose naltrexone (LDN). One of my patients resolved her flaring IGM after a functional medicine doctor started her on LDN for general wellness. I had another patient who was refractory to both methotrexate and azathioprine (i.e. thought to be the curative treatment) who received LDN from a different functional medicine doctor and also resolved her disease.
I then researched the pretty extensive literature on low dose naltrexone use in Crohn’s Disease (an inflammatory bowel disease that shares a lot of similarities with IGM). Naltrexone is a medication that is traditionally used for recovery from drug and alcohol abuse.
However, it was inadvertently discovered when tapering patients off of naltrexone in their sobriety that the very lowest doses of naltrexone exhibited a significant anti-inflammatory effect on the body. This includes being anti-inflammatory on a neuronal level, stabilizing epithelial barriers, reducing endoplasmic reticulum stress, reducing cytokine production, and having various impacts on T cells.
The results in Crohn’s Disease have been extremely promising. In one study, 75% of patient had resolved their symptoms and 25% had experienced a significant improvement. I have a lot of the studies linked here on the resources/medical publications section of my website.

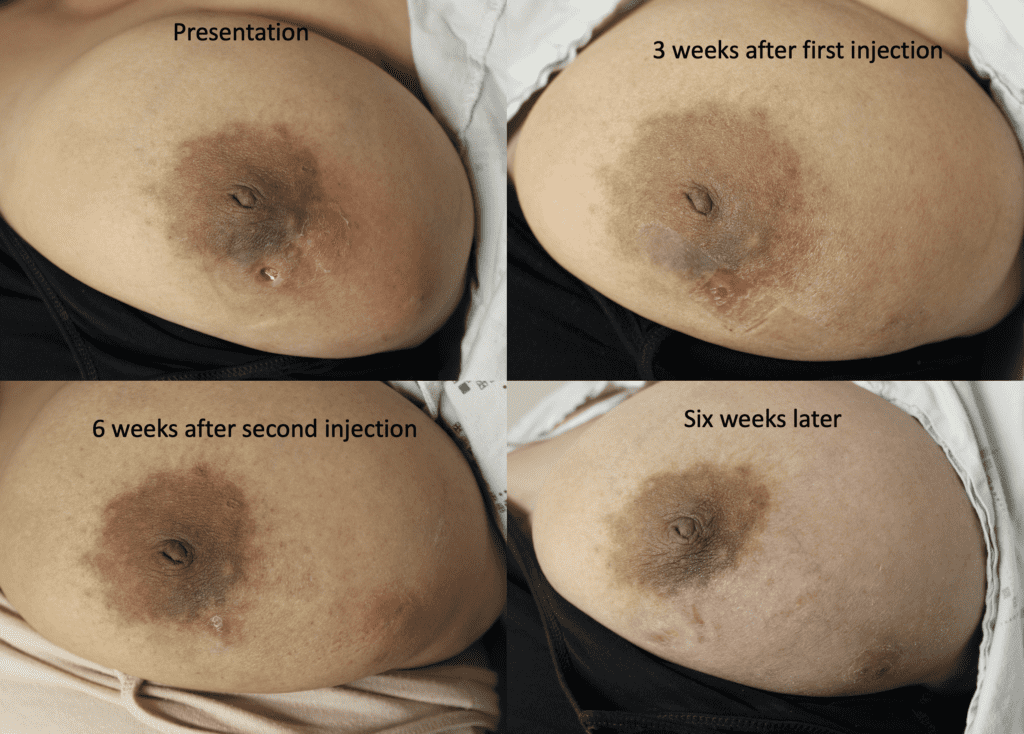
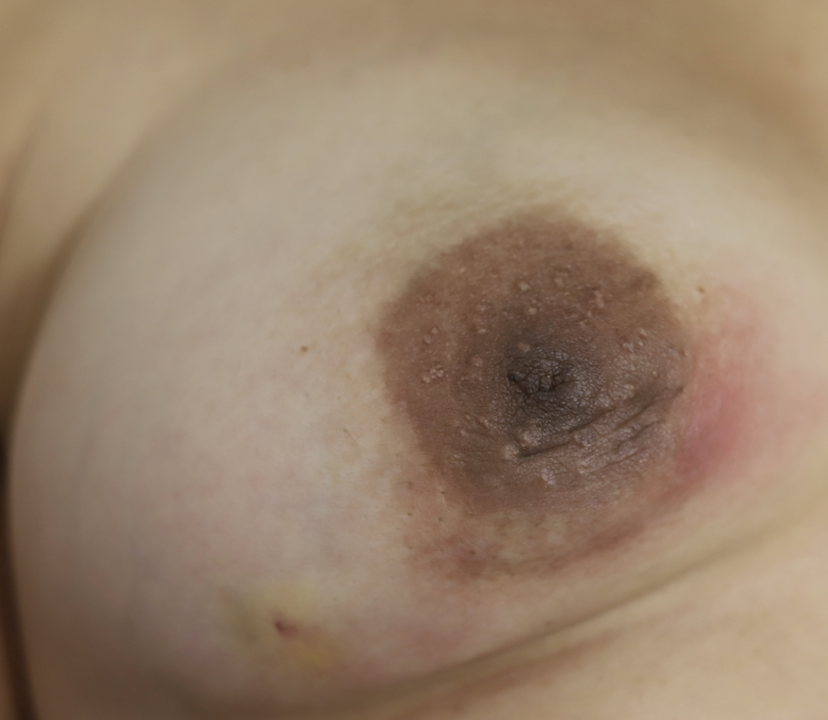
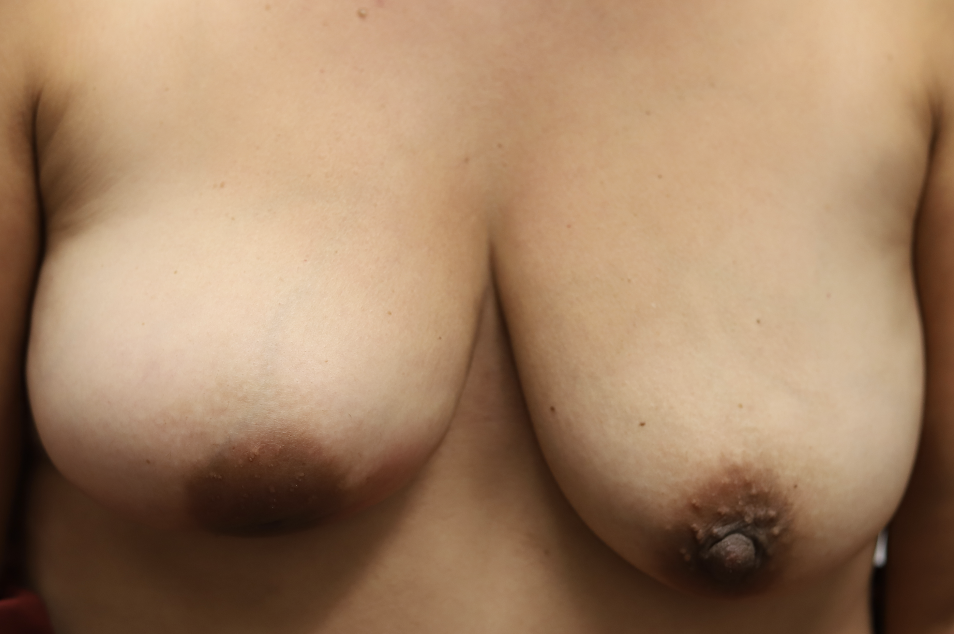
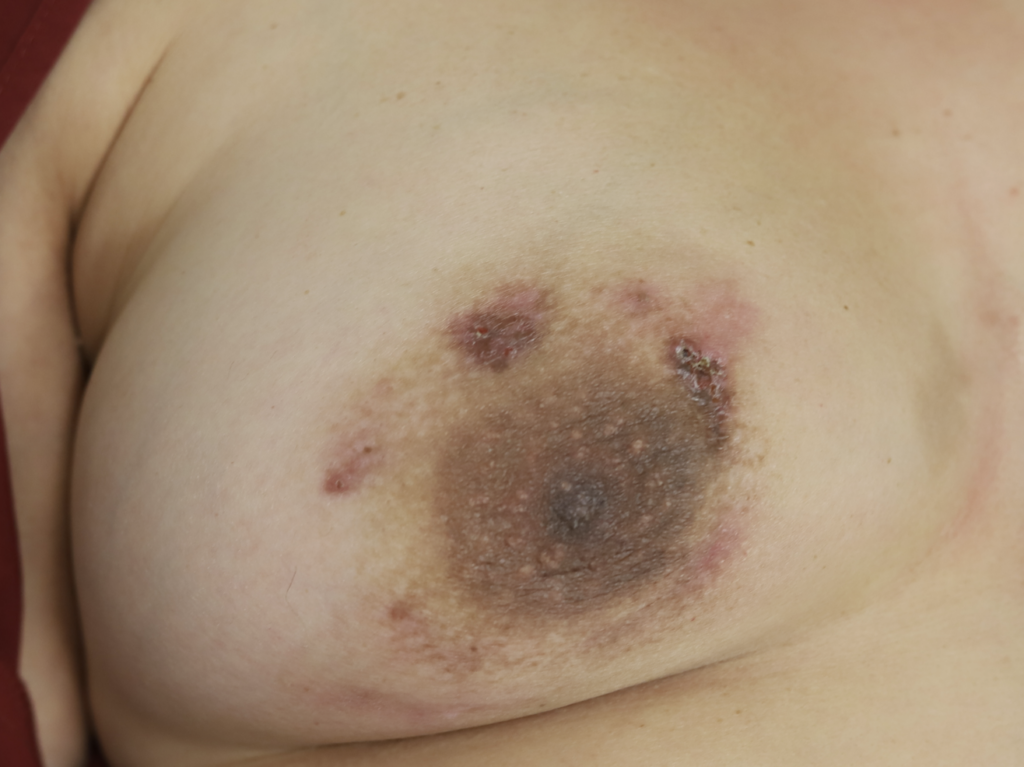
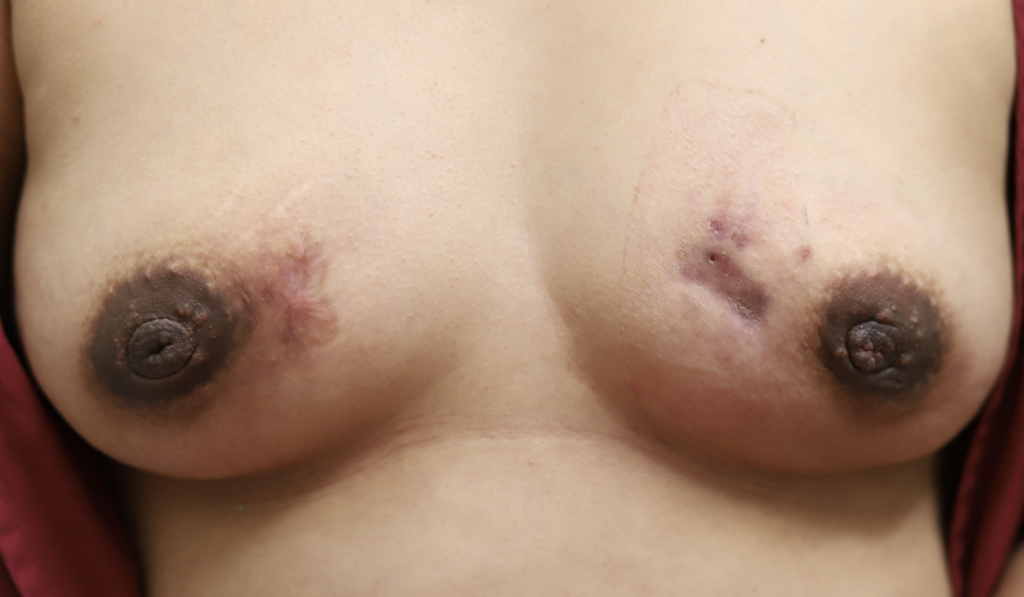
I have had similarly impressive results in my IGM patient population. I first prescribed LDN in the summer of 2024, and the patient resolved completely by the fall. Many others have resolved within just a month or two. All have experienced improvement within a month. Only one of my patients has remained symptomatic, but her disease is far better and far less painful than before (consistent with the Crohn’s Disease literature). Some of these patients are pictured below – keep scrolling :).
As this is a completely new approach to treating IGM, there is no set “regimen” for dosing. Given that I had never prescribed it before, I started initially in my patients with 1.5 mg for one month, increased to 3.0 mg the next month if not totally resolved, and then 4.5 mg the next month if not totally resolved. The Crohn’s Disease clinical trial in Europe (linked on the resources/medical publications section of my website) is studying patients on 52 weeks of 4.5 mg before considering tapering.
Given that patients are tolerating this medication without any side effects other than possibly some more vivid dreams than usual, I may start prescribing 4.5 mg at the outset — depending on the severity of disease (since I have had patients with more mild disease resolve at 1.5 mg). The only downside of this medication is that it isn’t covered by insurance (it’s about $50-60 cash per month) and it has to be obtained at a compounding pharmacy (i.e. not your regular CVS, Walgreens, etc). This is because the medication has to be “compounded” (the 50 mg tablet is broken down into the very small doses and put into a capsule). Most communities (even small ones like where I live) have them Example of a prescription from one of our local compounding pharmacies. Because the cost of 1.5 mg is the same as 3.0 mg and I anticipated increasing this patient’s dose from 1.5 to 3.0 mg, I prescribed it twice daily so we could titrate. However, once on a stable dose, I prescribe it once a day at bedtime.
Example of a prescription from one of our local compounding pharmacies. Because the cost of 1.5 mg is the same as 3.0 mg and I anticipated increasing this patient’s dose from 1.5 to 3.0 mg, I prescribed it twice daily so we could titrate. However, once on a stable dose, I prescribe it once a day at bedtime.
A few other breast surgeons have now tried LDN, all with improvement in their patients as well. If you’re a surgeon reading this website and you start using this medication, please reach out as it would be great to get the largest patient cohort possible to publish this in the medical literature eventually.
Another option for treating a flare of IGM is a steroid injection into the affected breast. This video that I presented at the American Society of Breast Surgeons in Boston spring 2023 illustrates this procedure:
Without access to formal ultrasound, a simpler approach is illustrated in the below video:
PharmD Phil Anderson, who runs LactMed at the NIH, initially suggested that the infant would receive a large oral dose of steroid if they breastfed after injection. However, the dose of steroid is still lower than what would be used to treat infants for certain conditions. A more recent case report demonstrated no steroid in breastmilk and our subsequent report of a higher dose of steroid confirmed negligible transfer.
Oral steroids will reduce milk in both breasts rather than just the breast where the steroid is injected. However, if a mother has very high milk production in general, she may not notice a difference. Steroids also can cause significant insomnia and anxiety in patients taking them, so this should be considered in postpartum patients who are already at risk for mood and anxiety conditions. Below is an image and video of a mom taking oral steroids and breastfeeding from her breast with IGM.
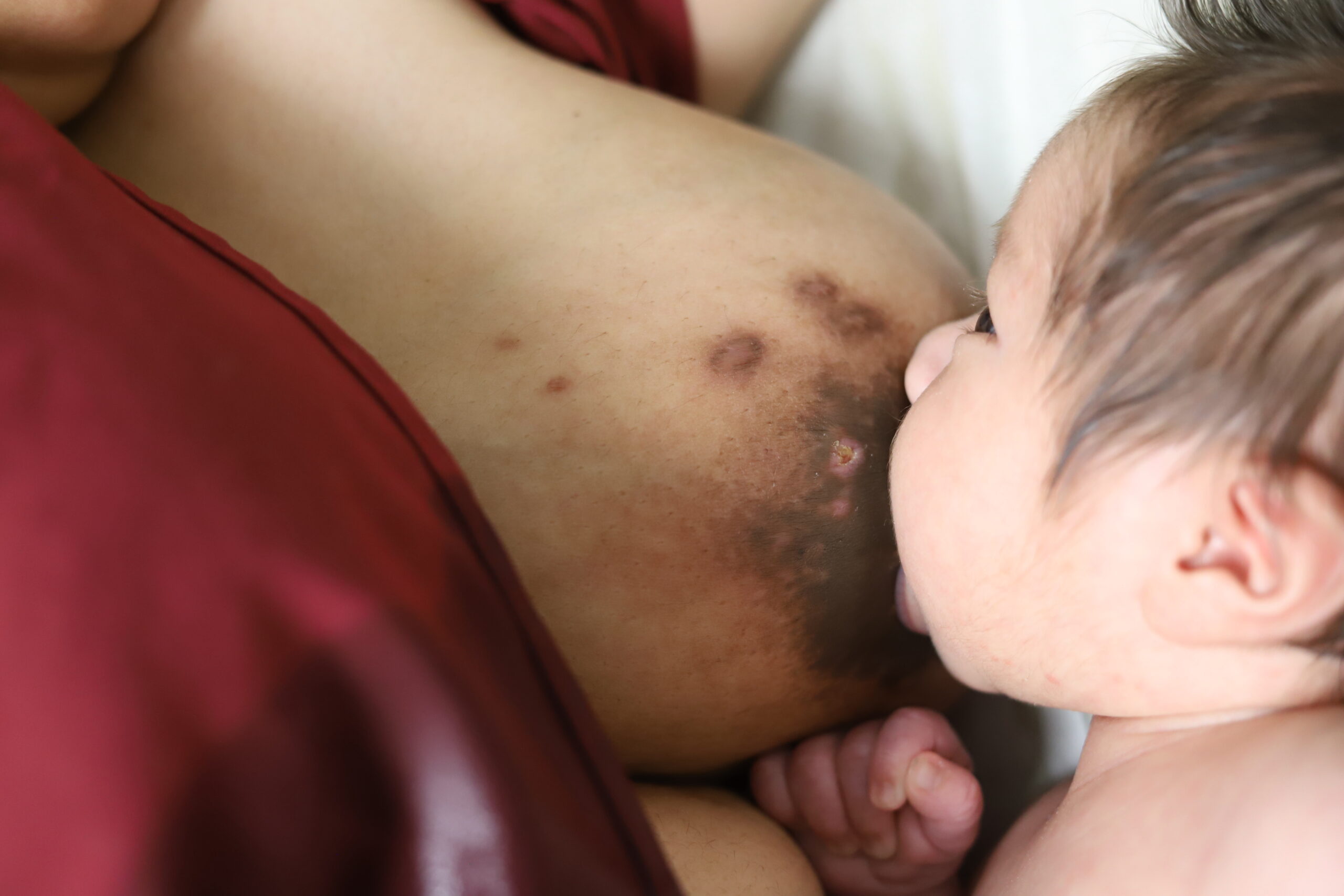
Mothers also may elect no treatment during lactation; fluid collections, fistula formation, and other symptomatology can be managed on an as-needed basis.
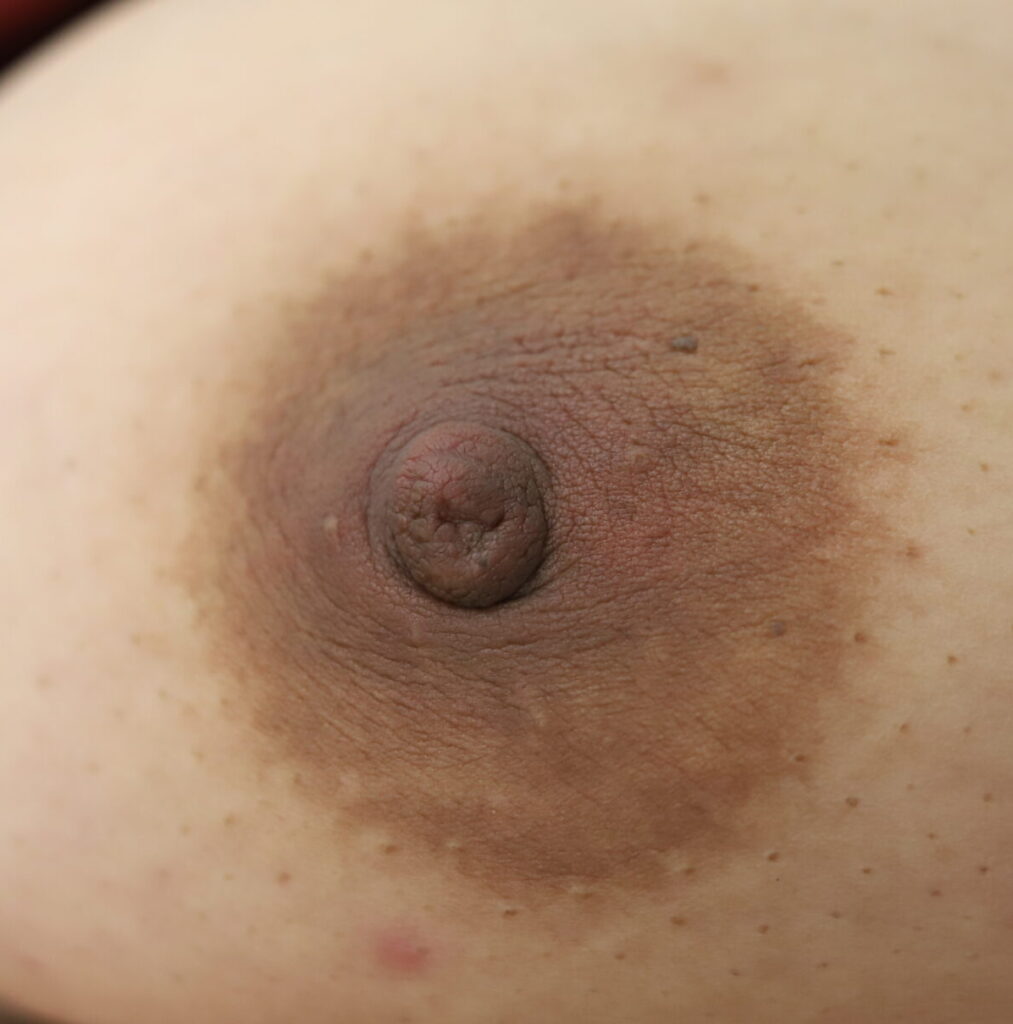
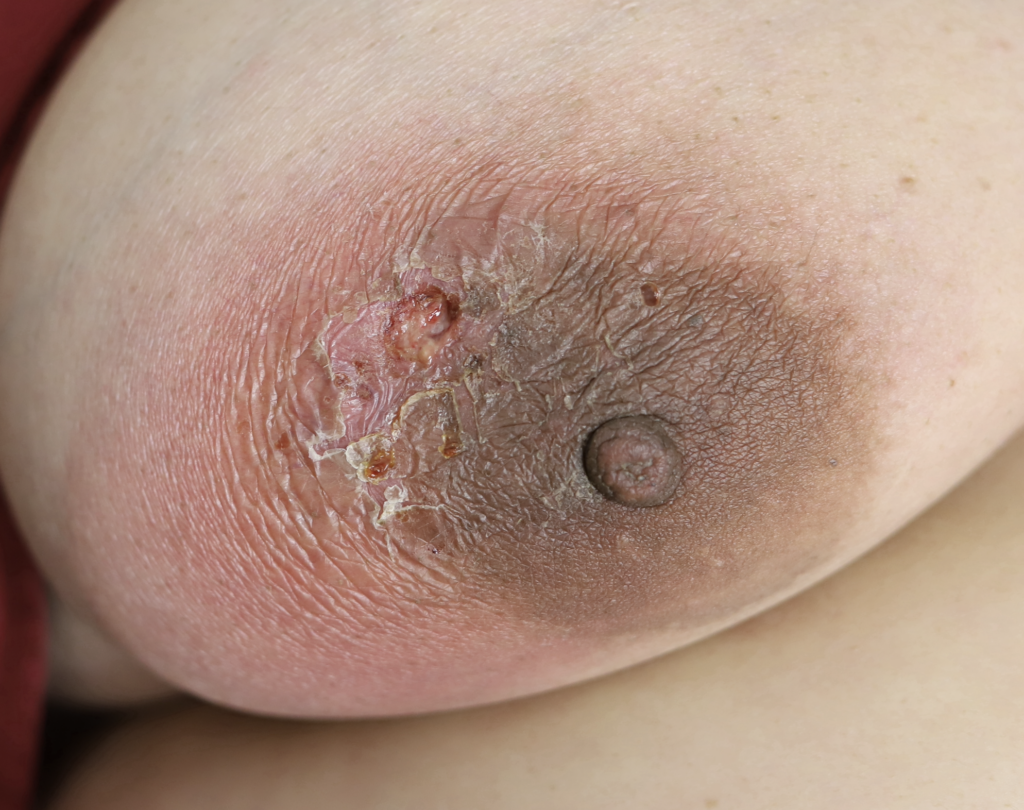
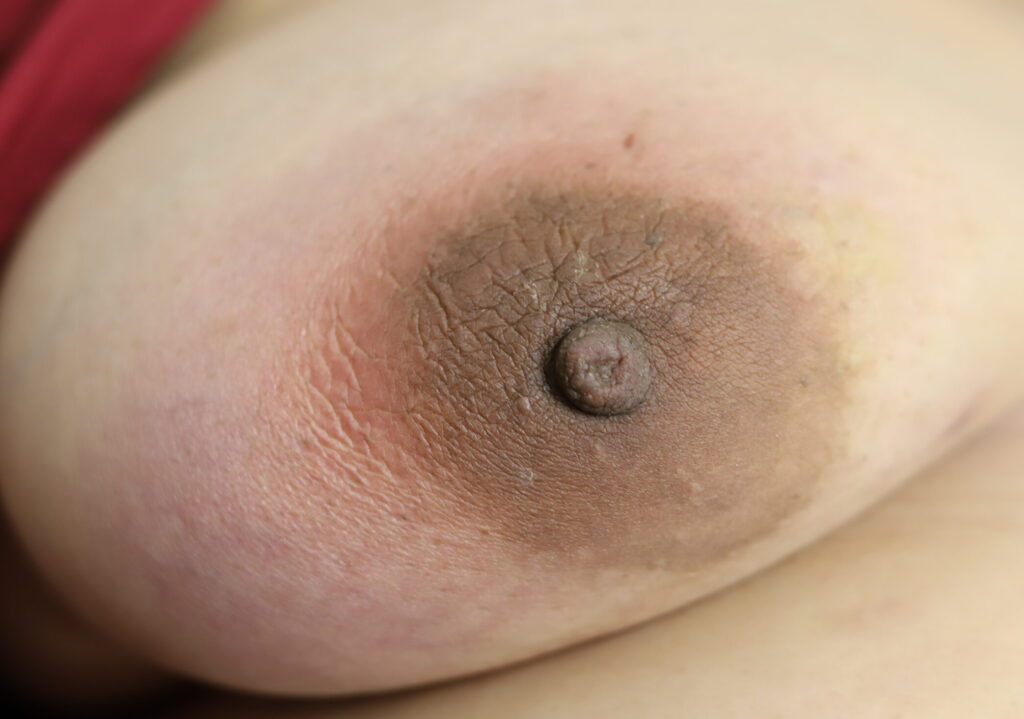

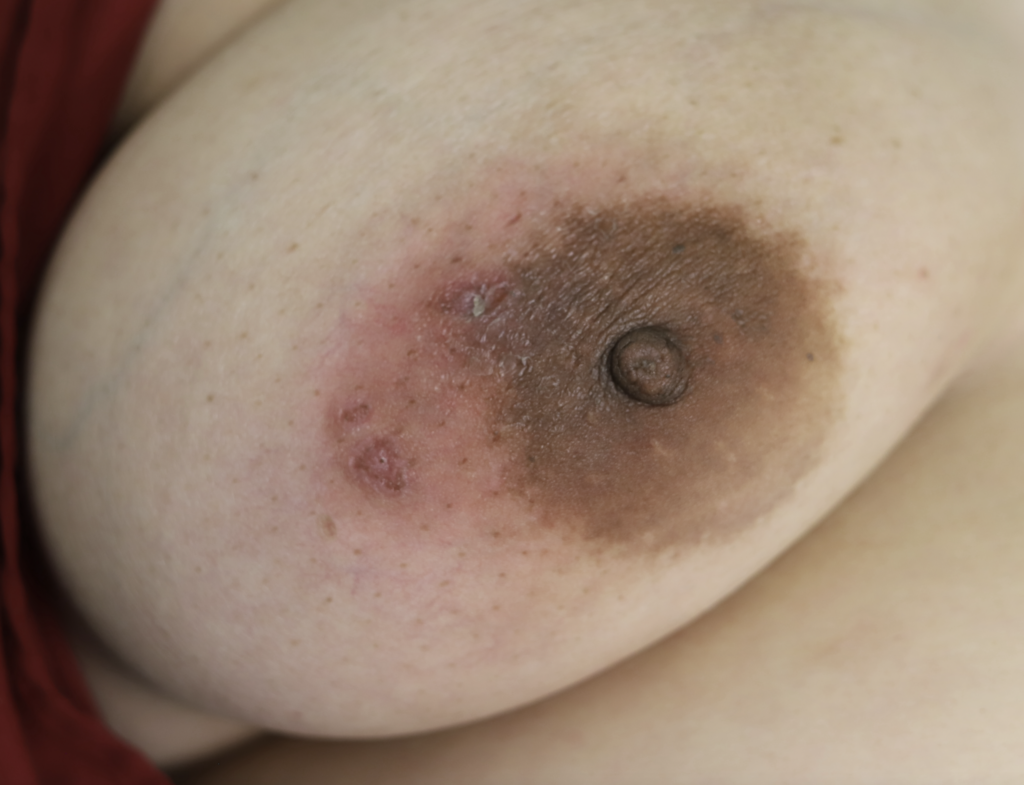
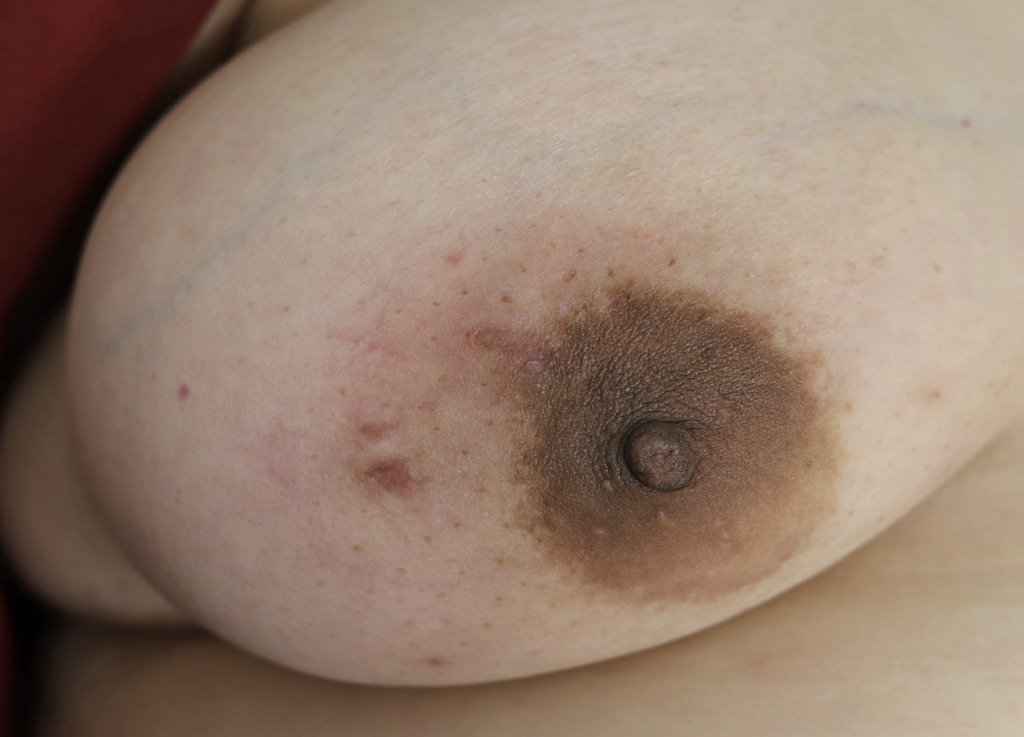



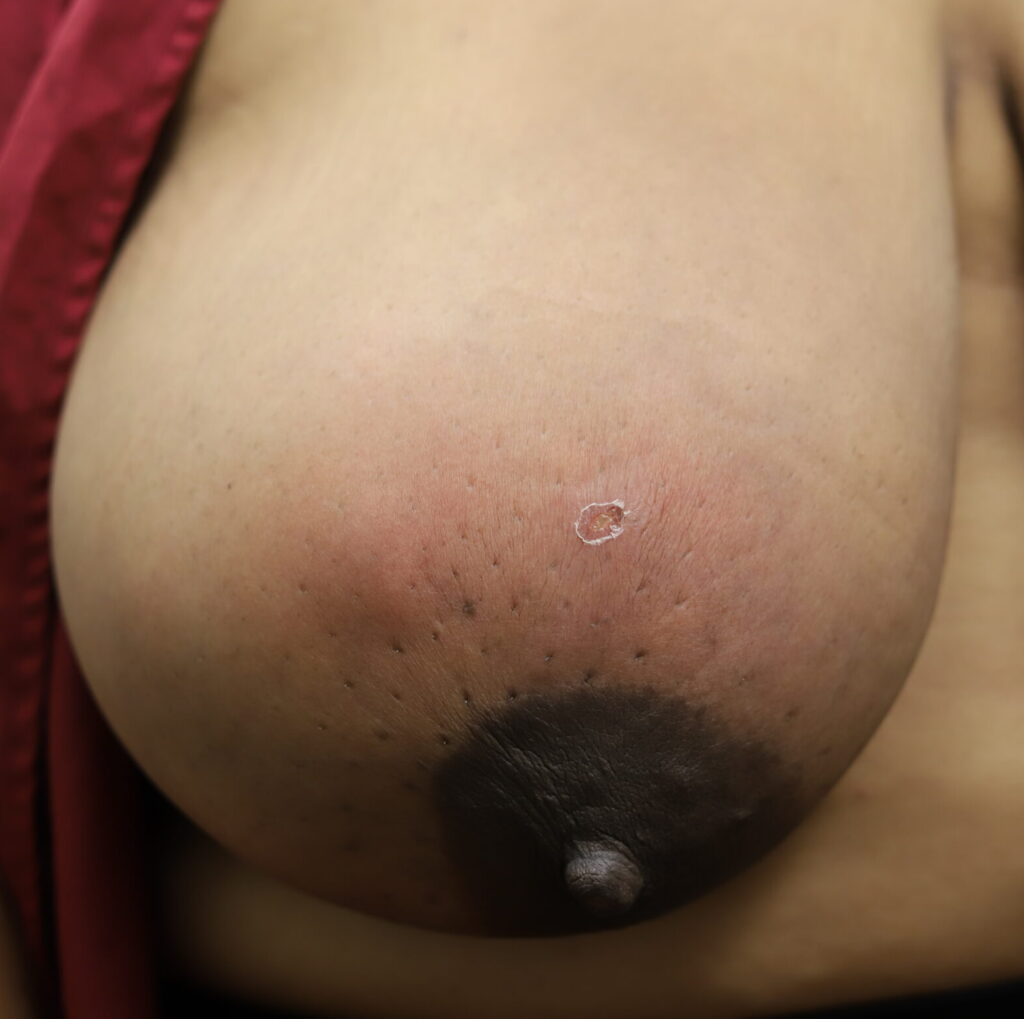
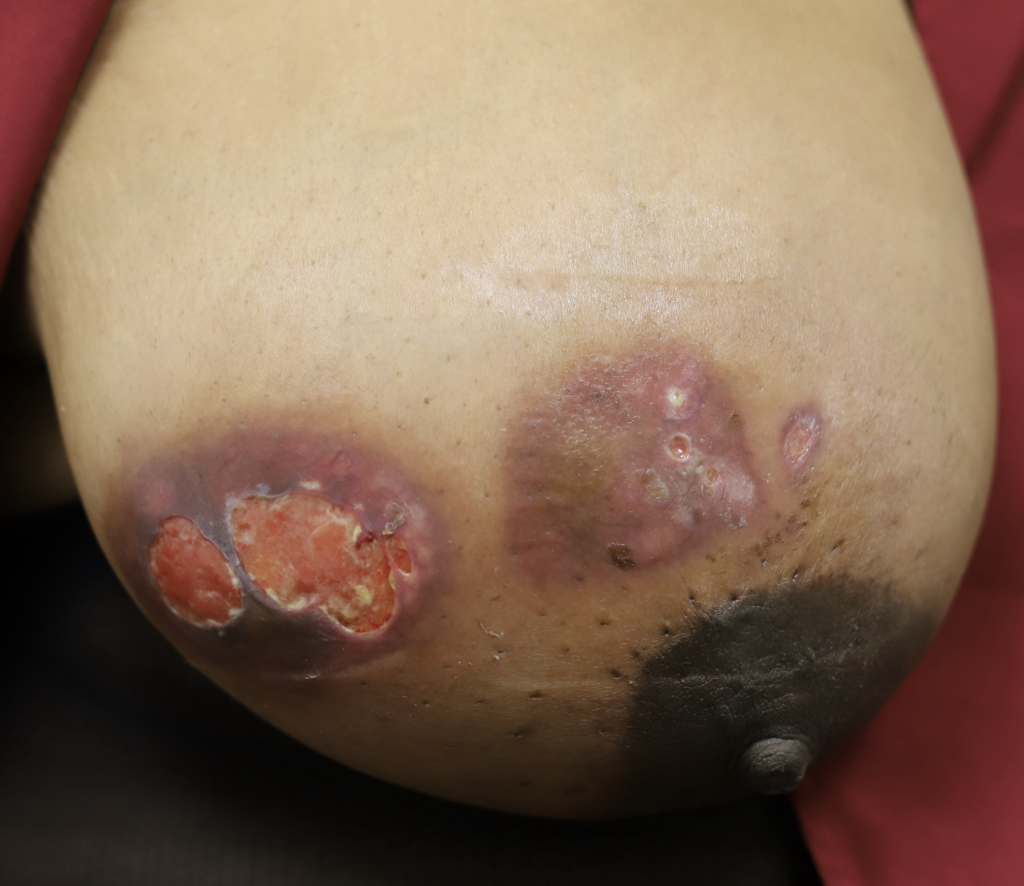
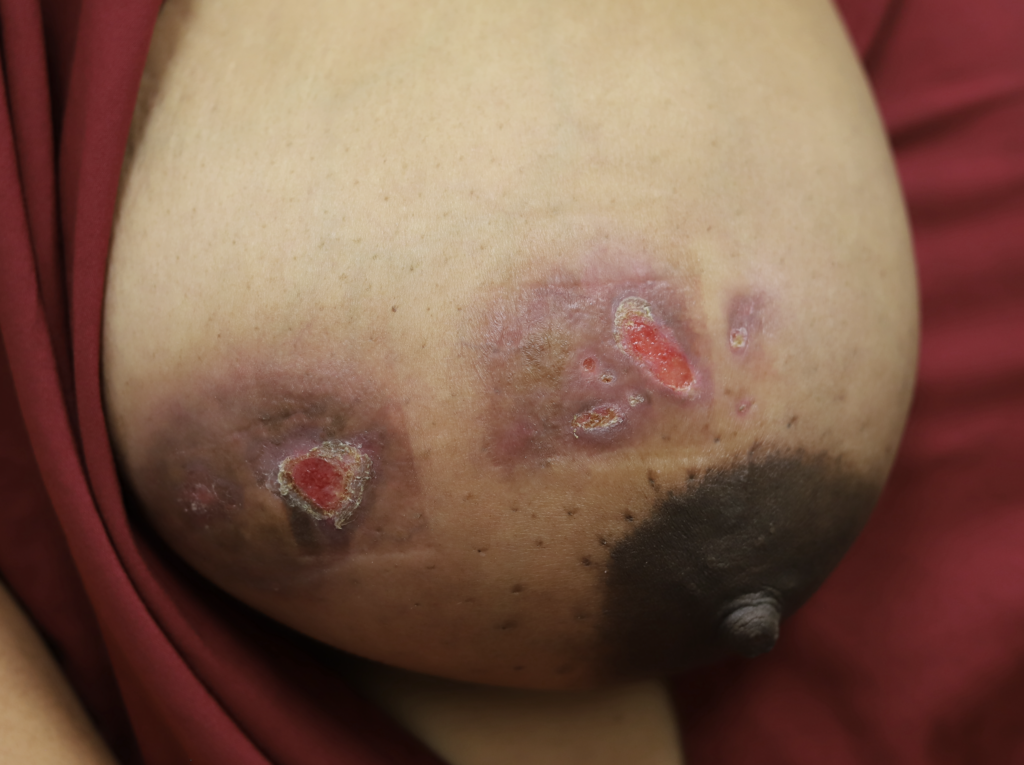
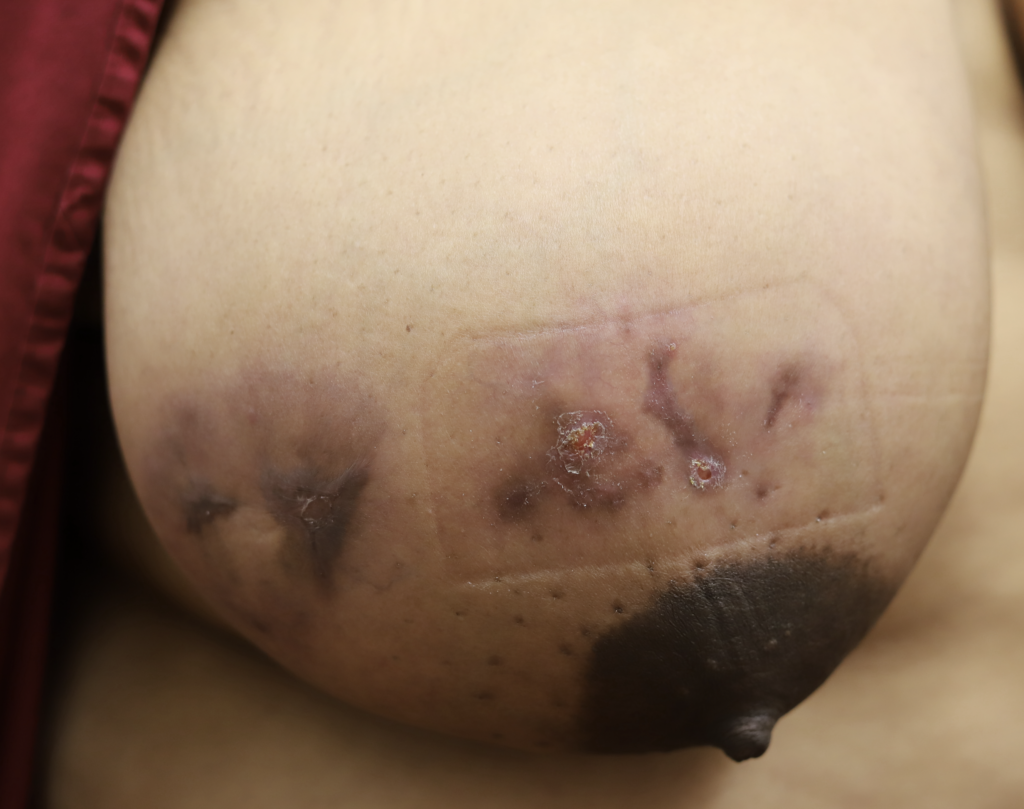
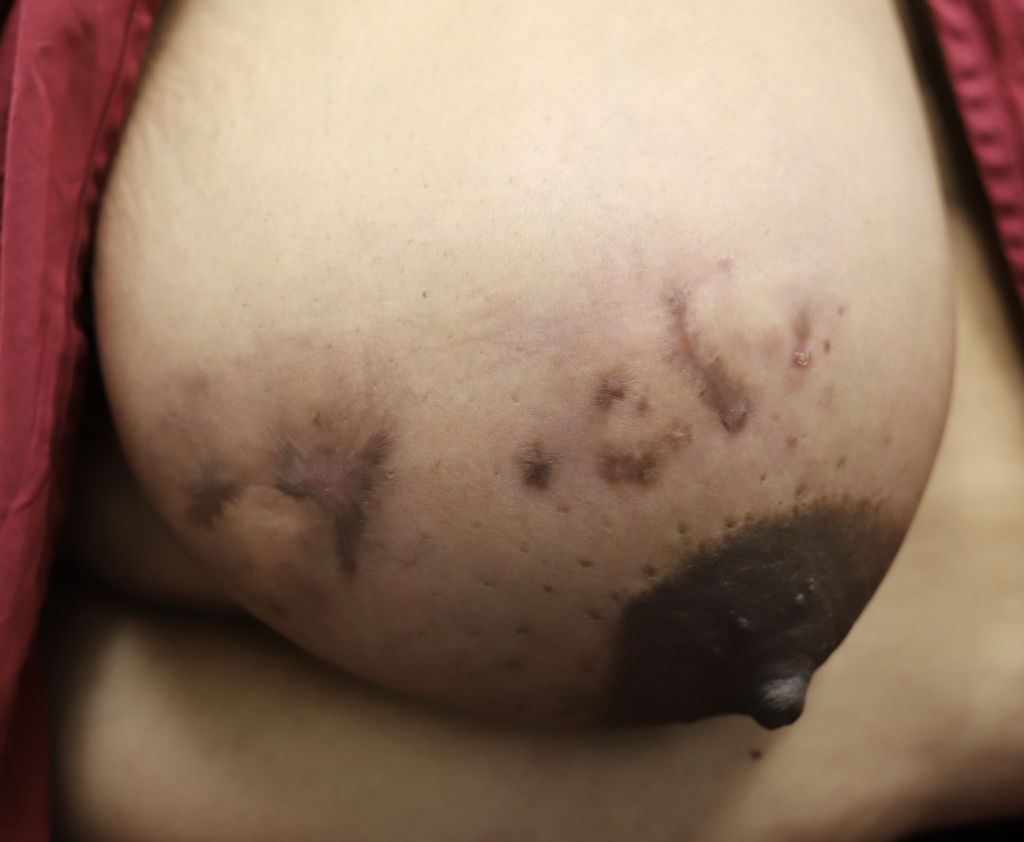
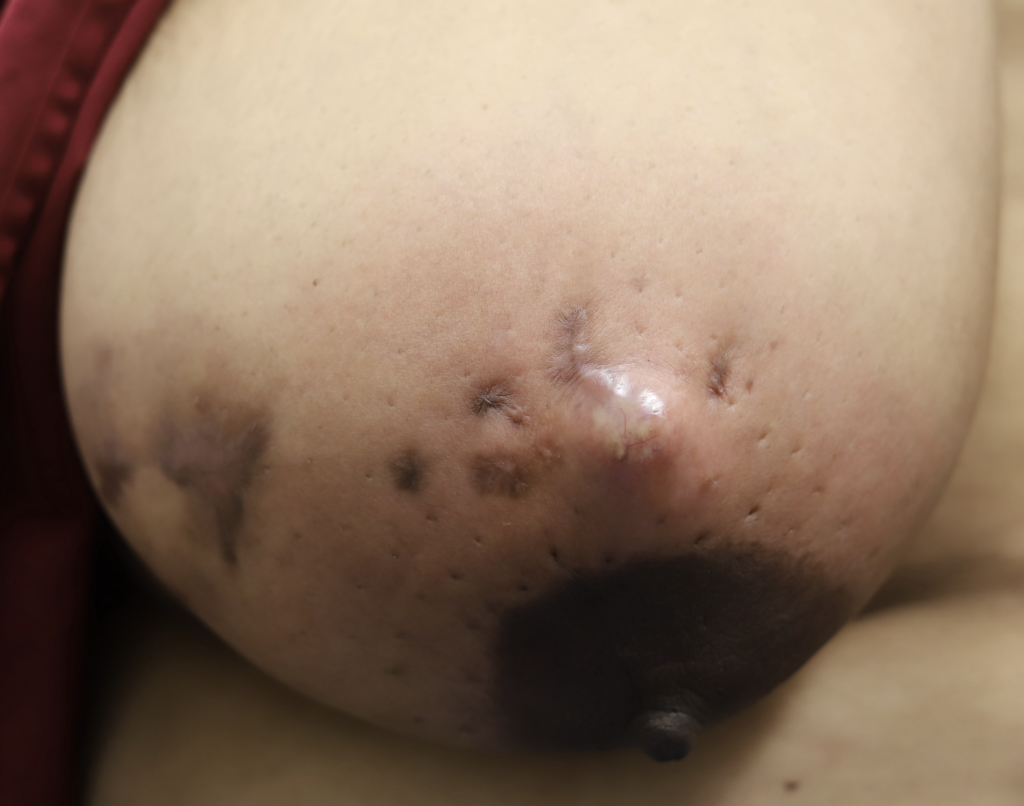
Drainage of recurrent fluid collection and injection of steroid:
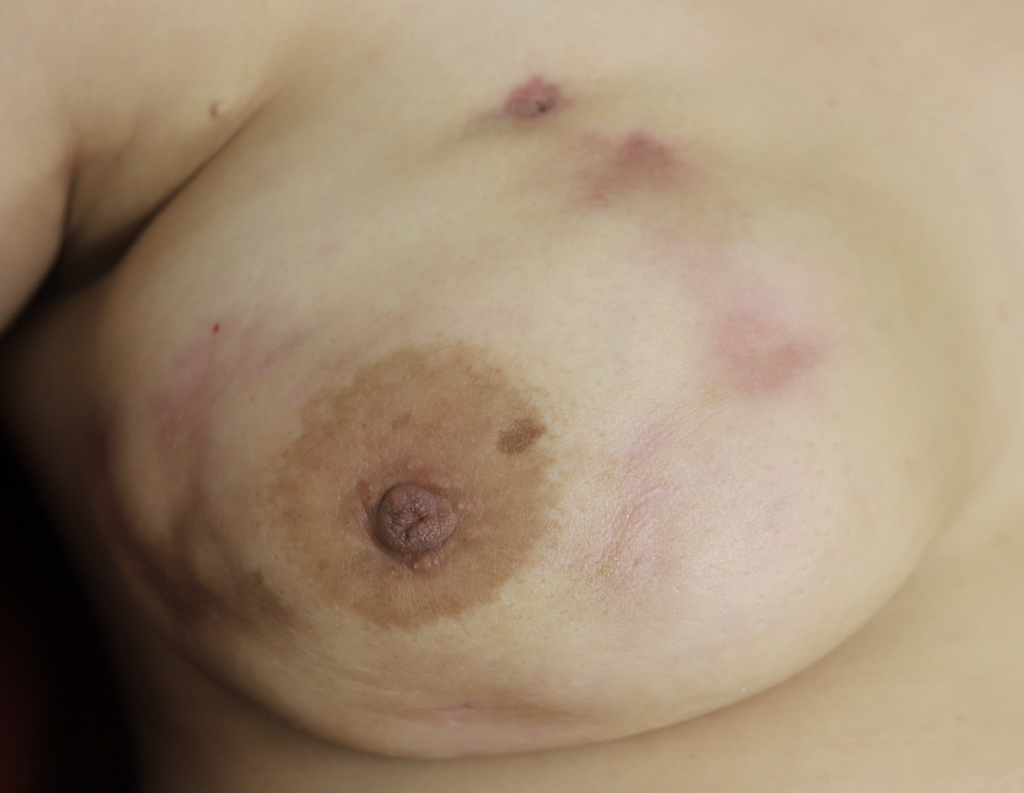
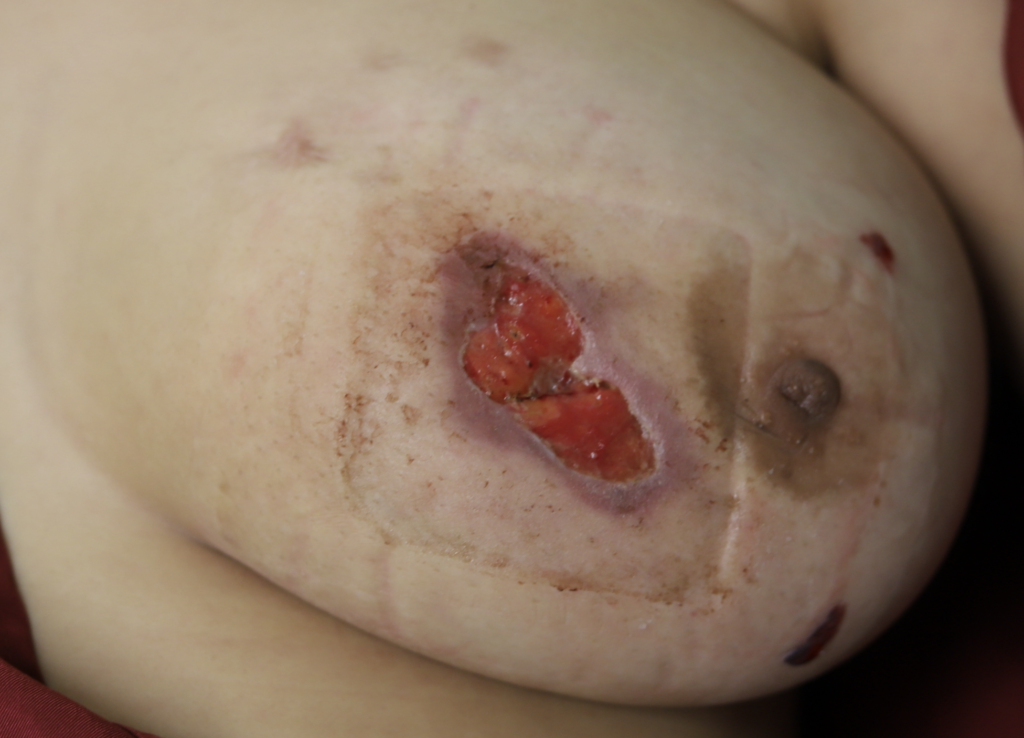
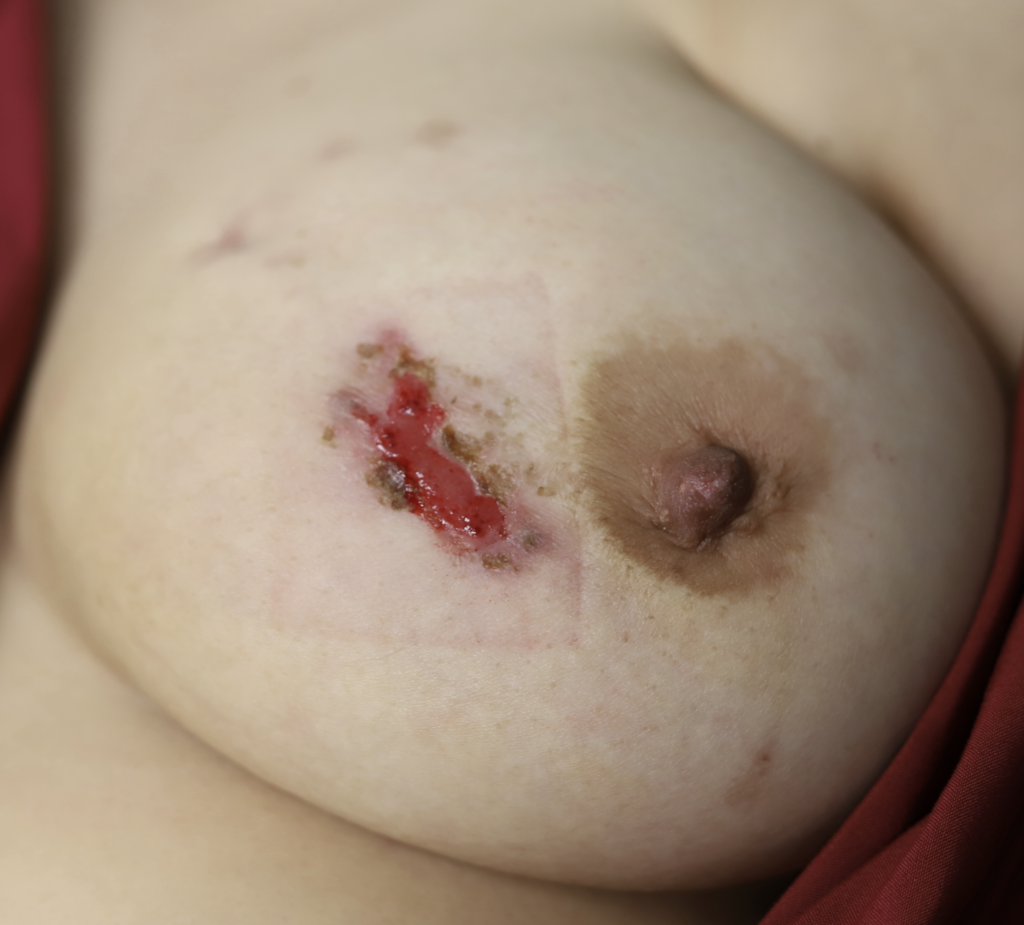
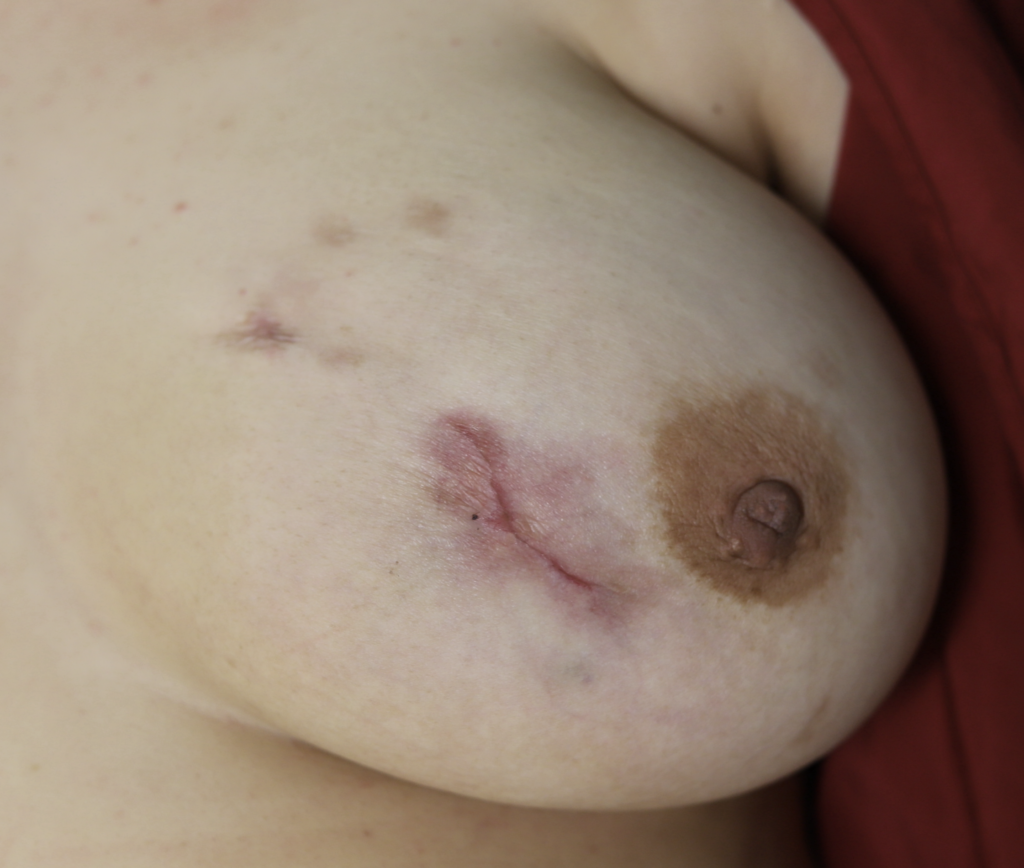
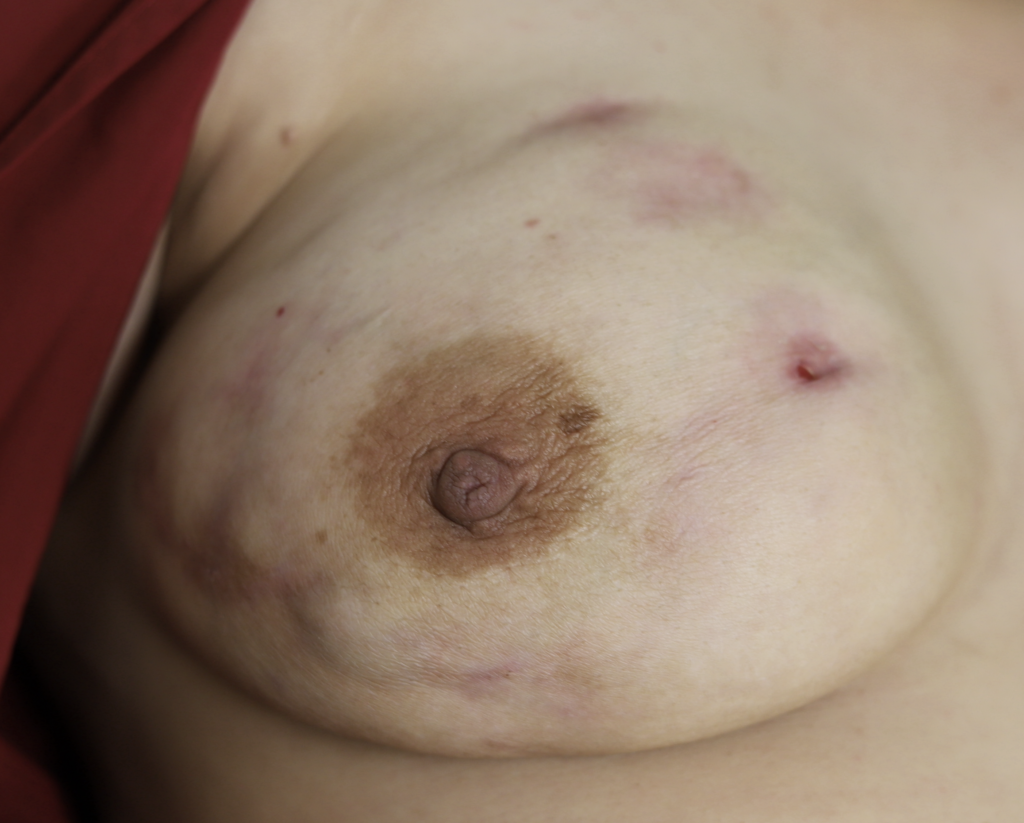
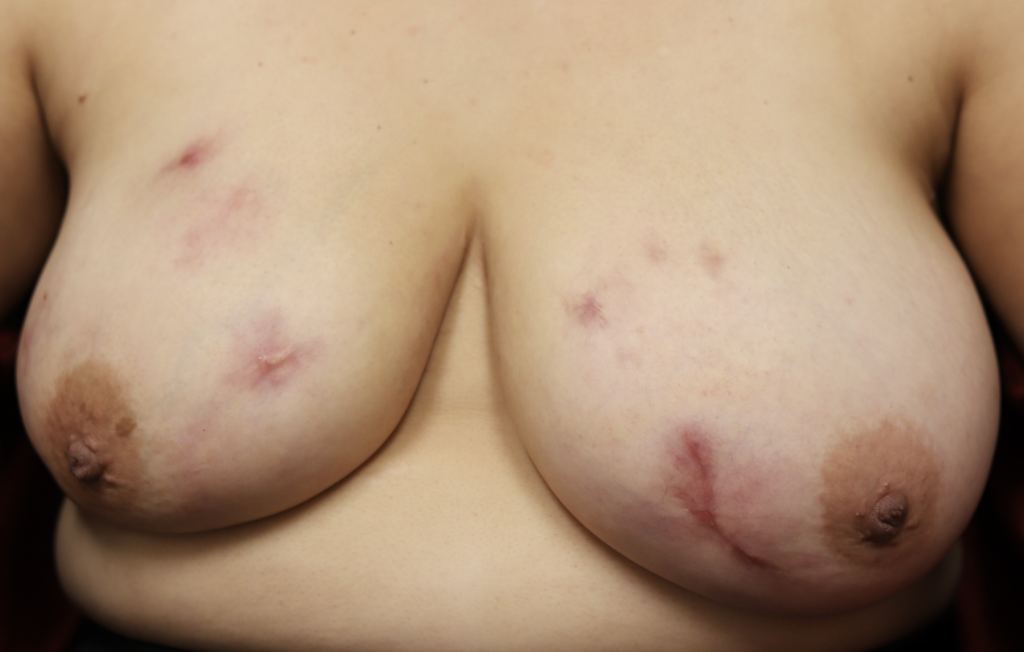
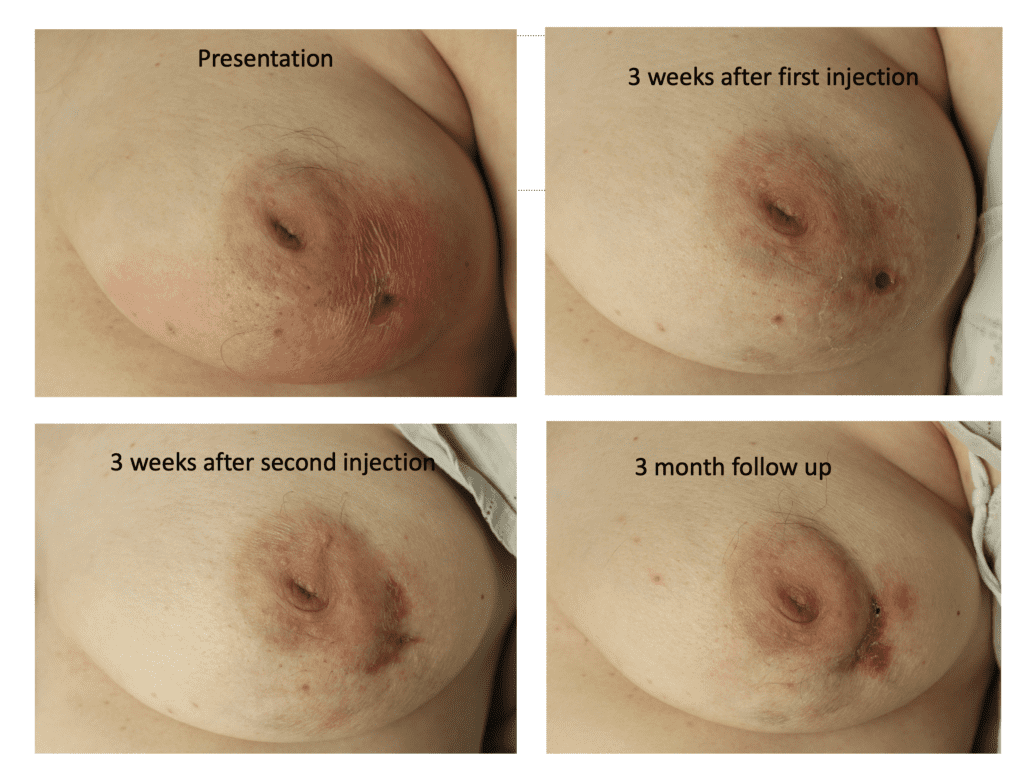

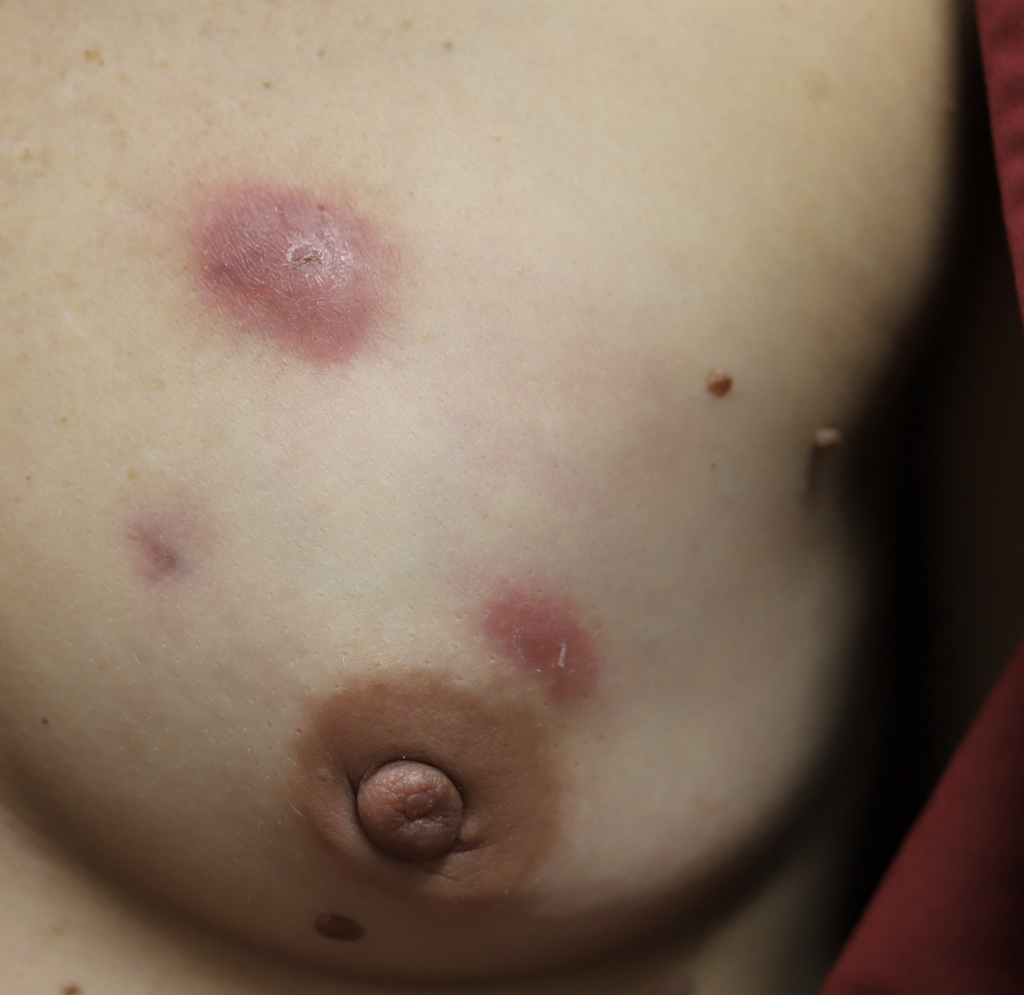
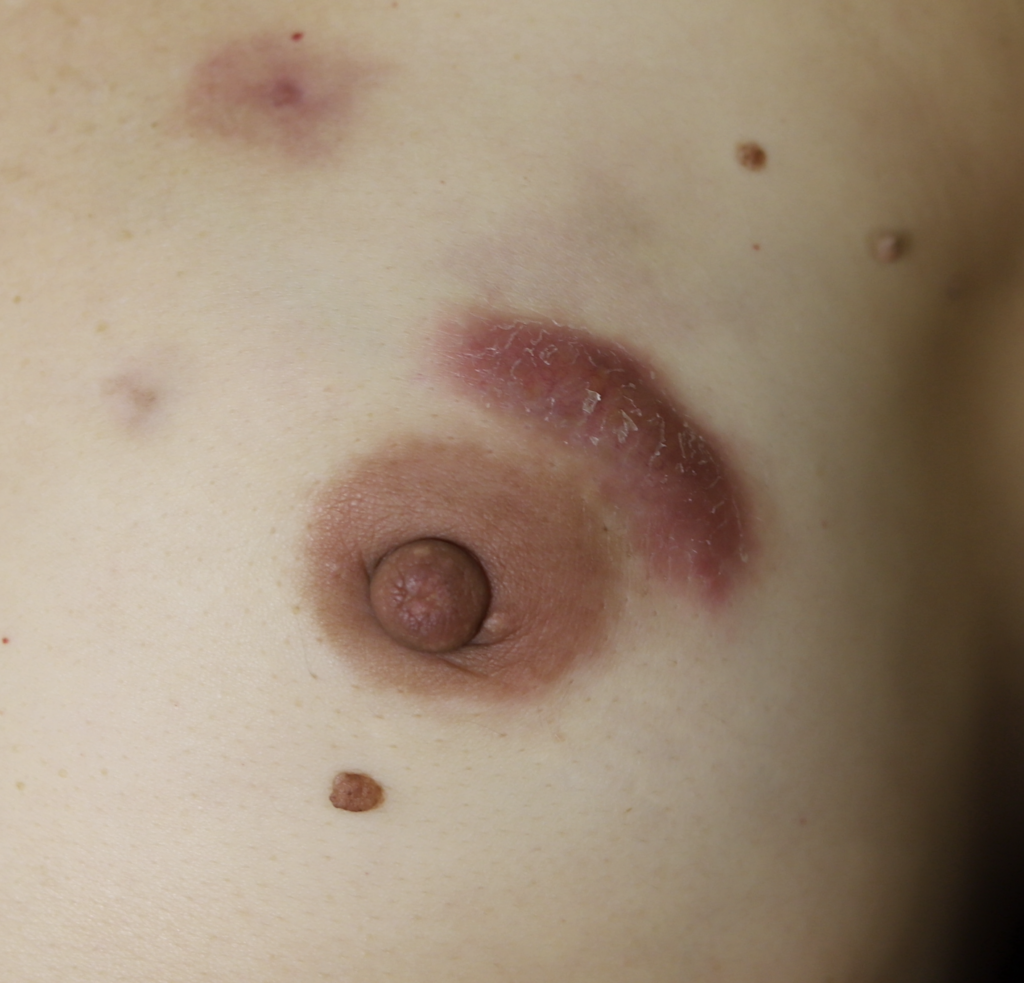

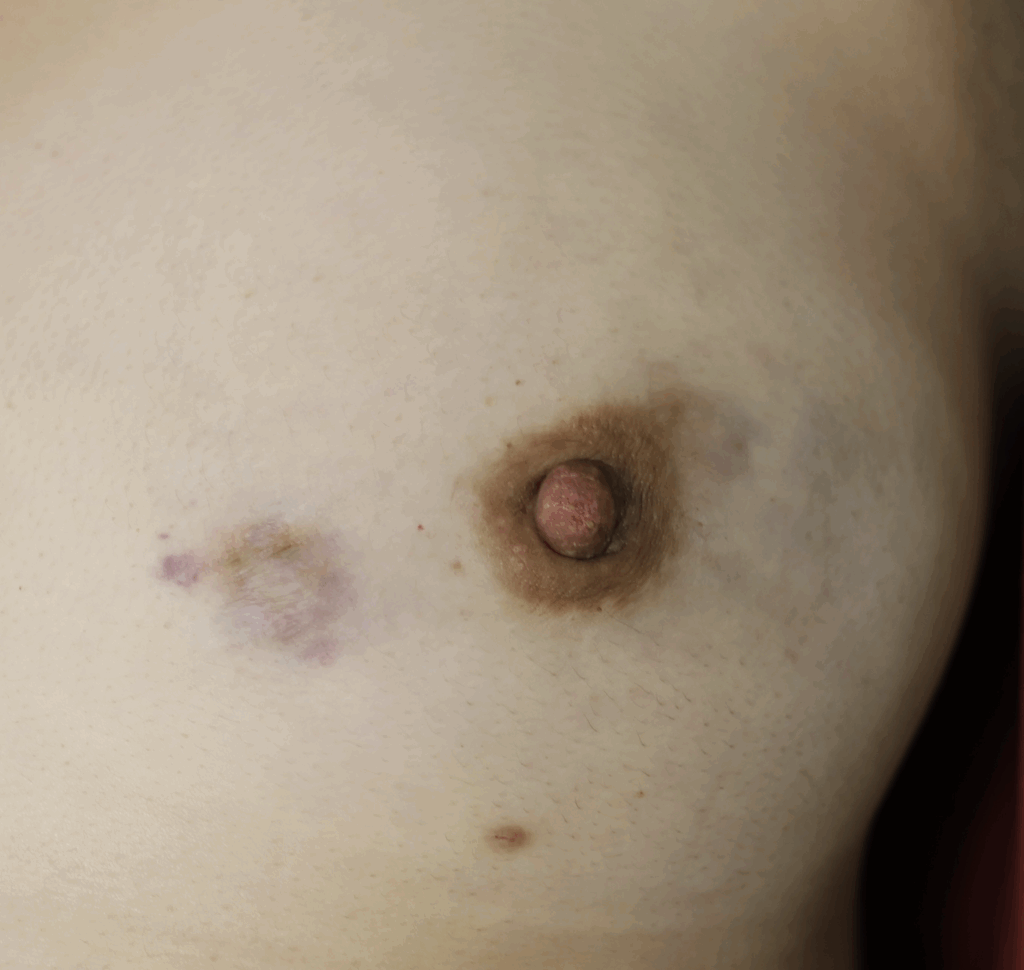
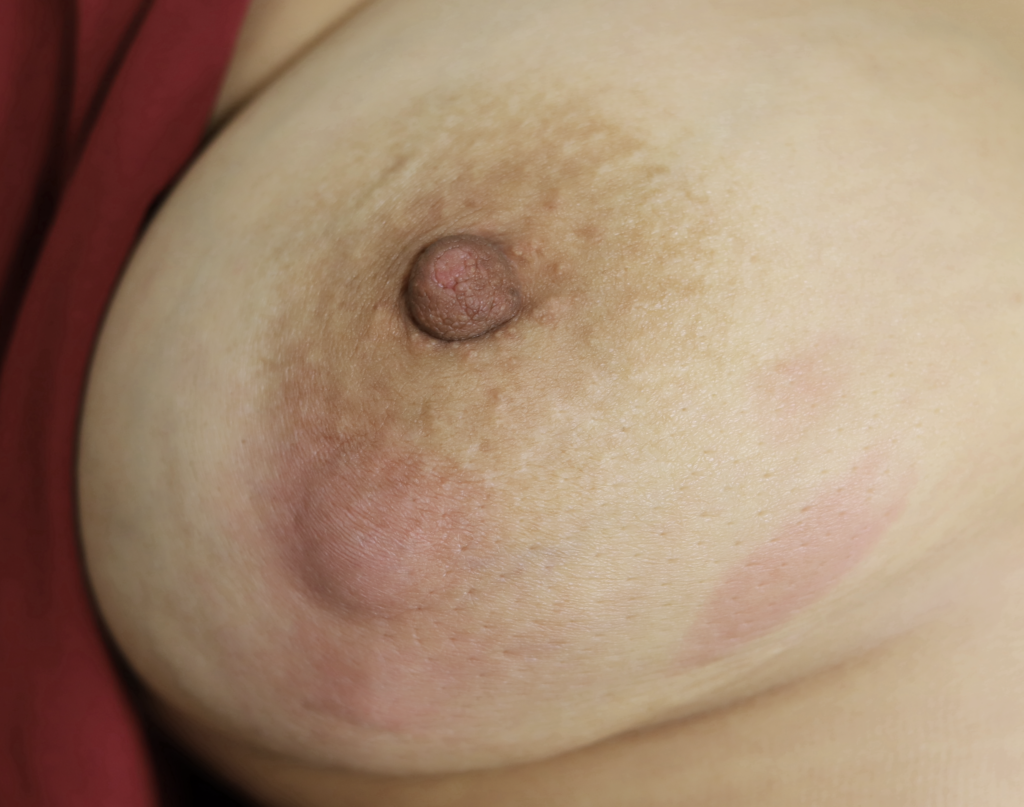
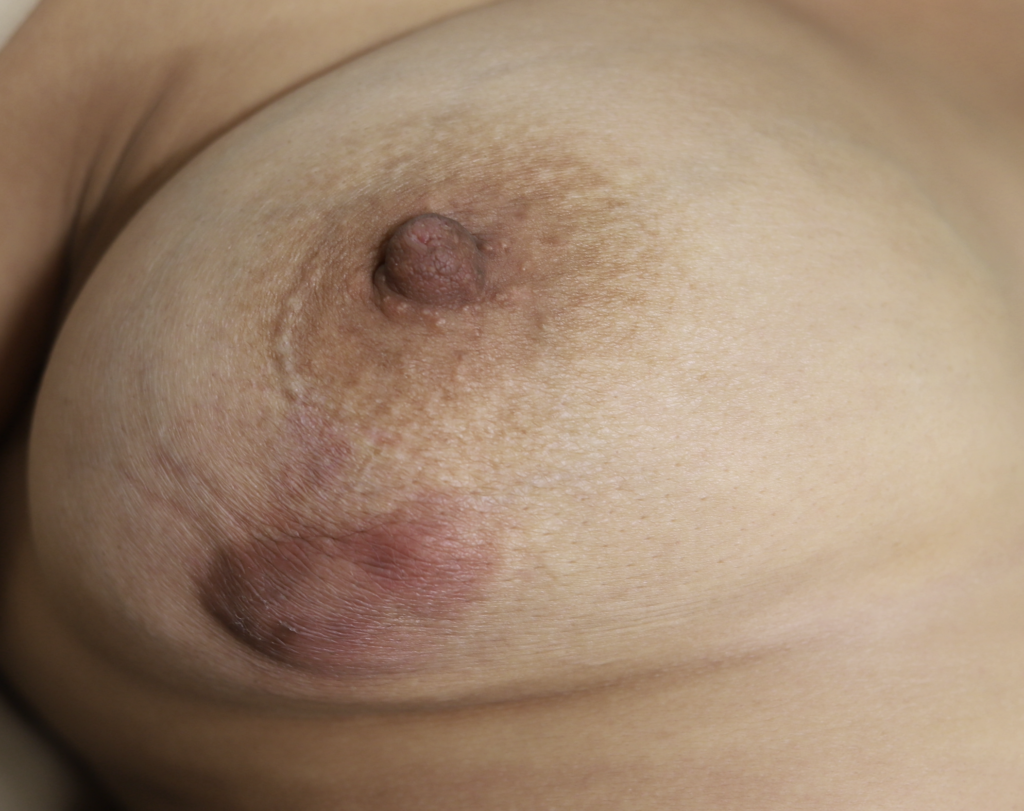
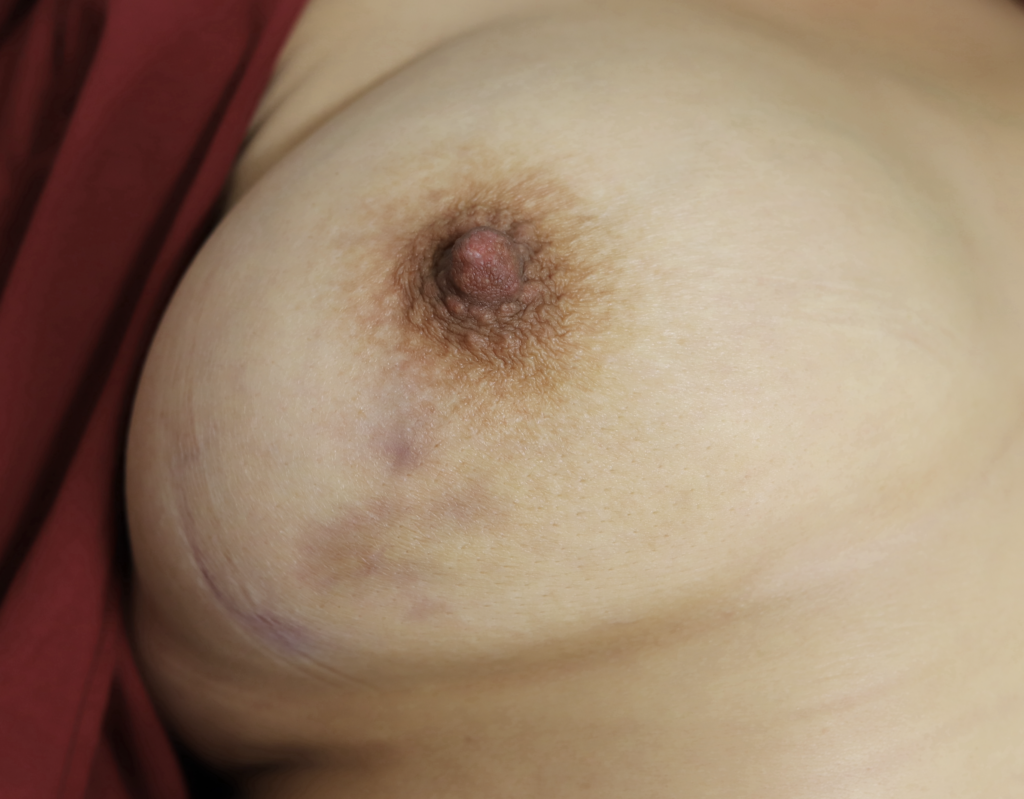













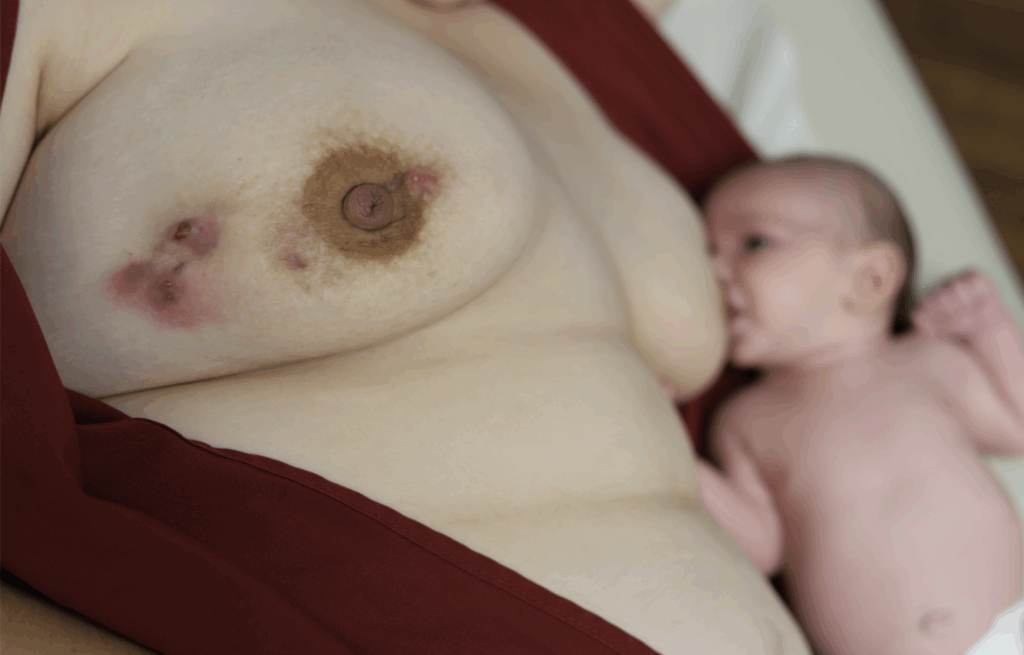
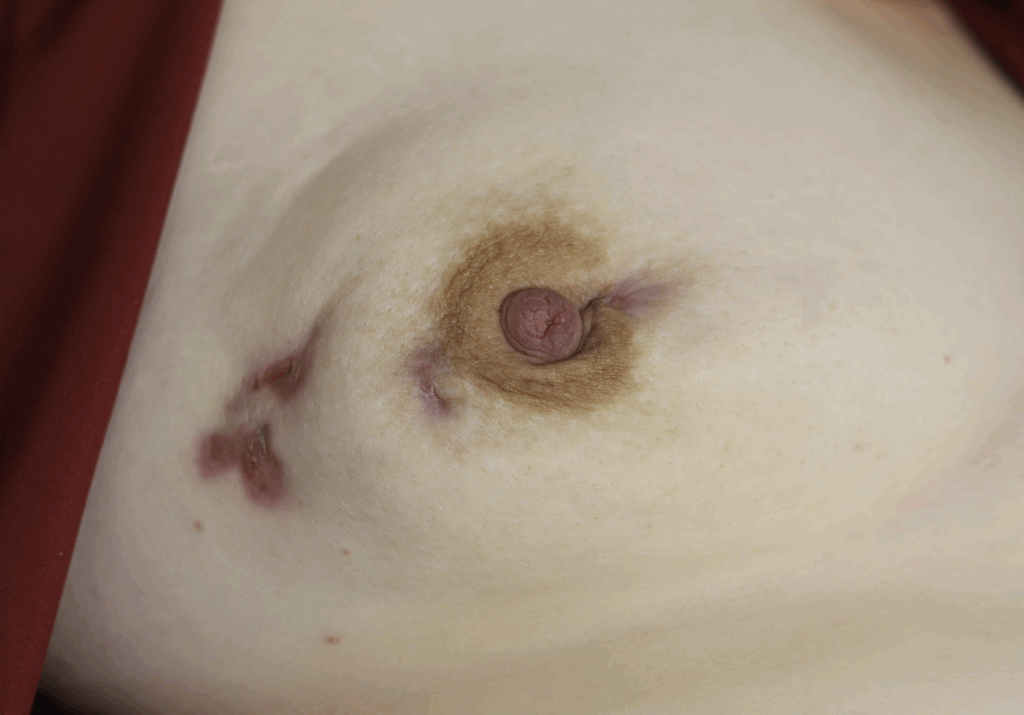
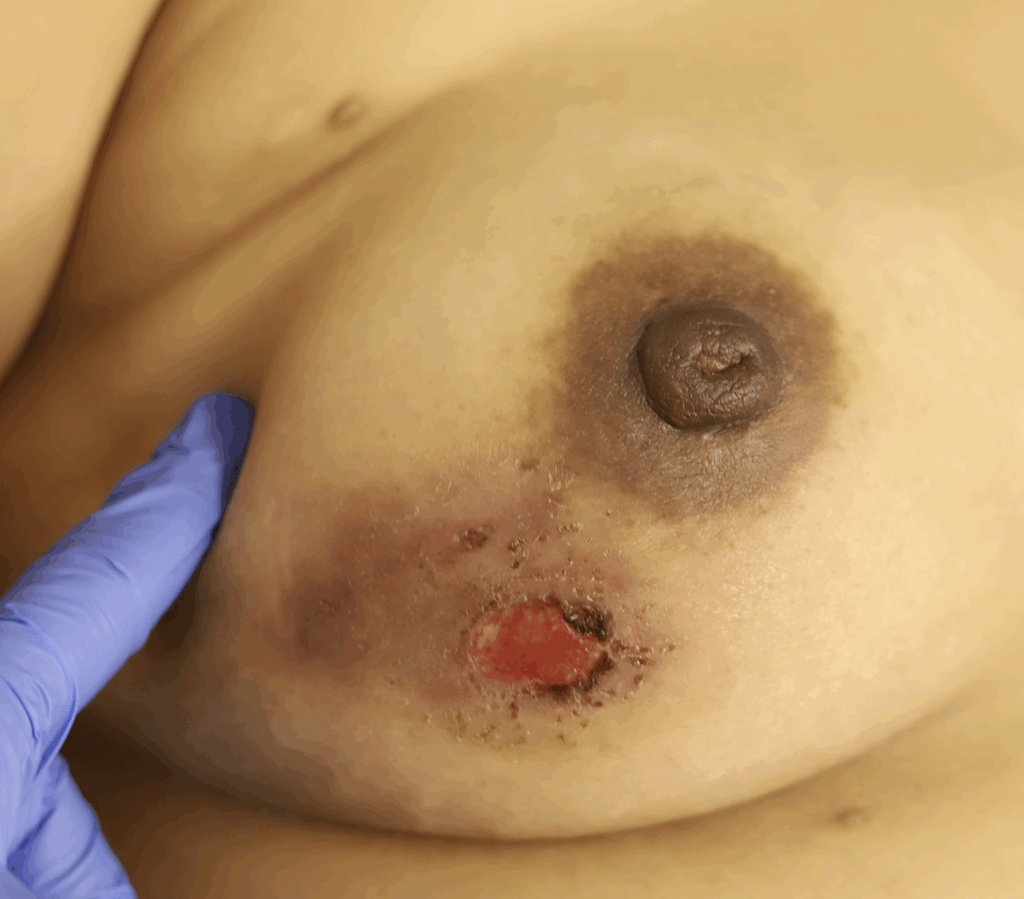
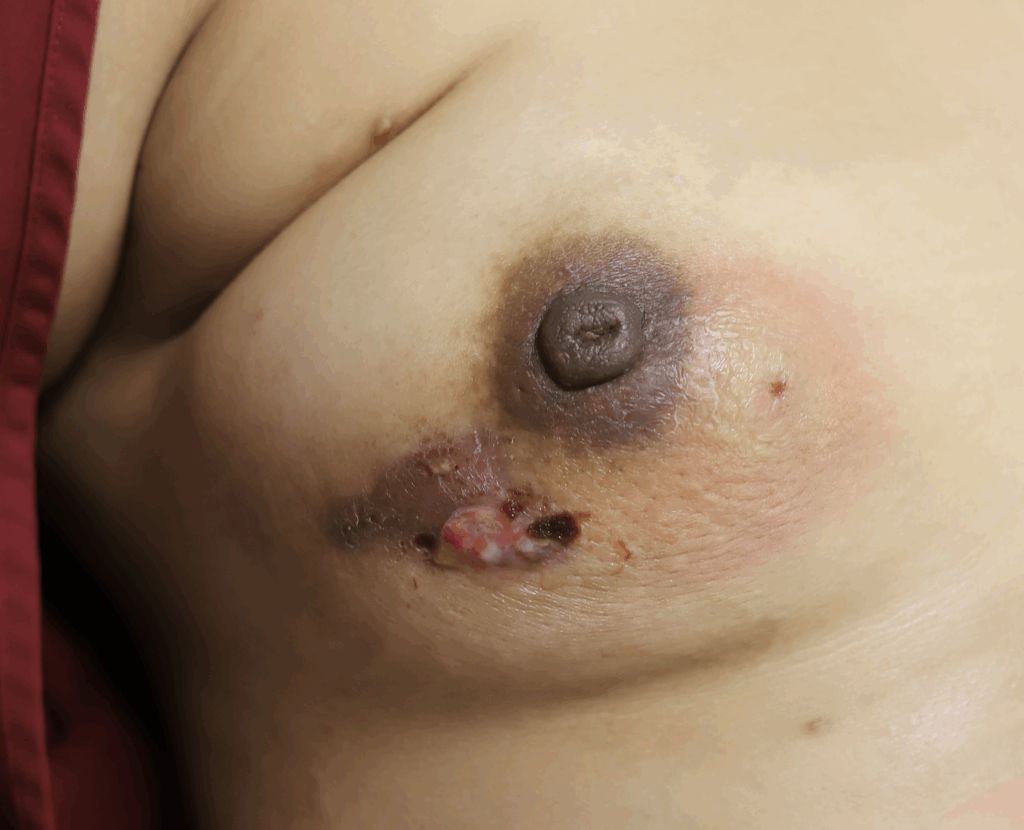
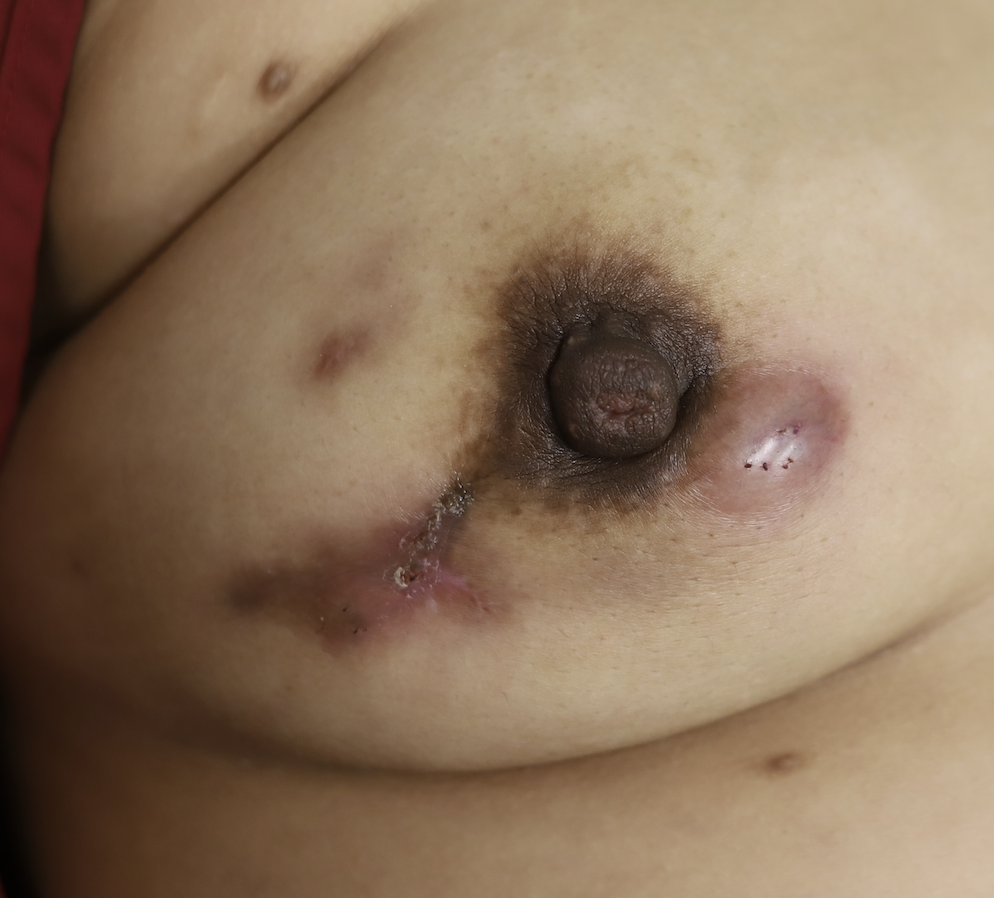
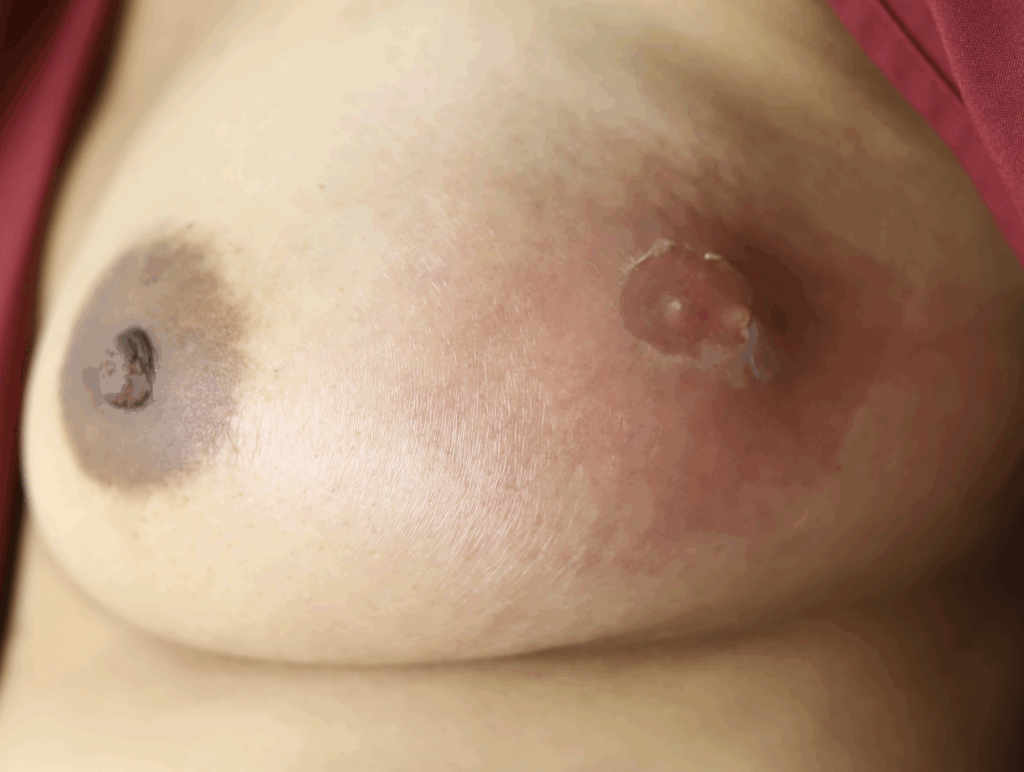
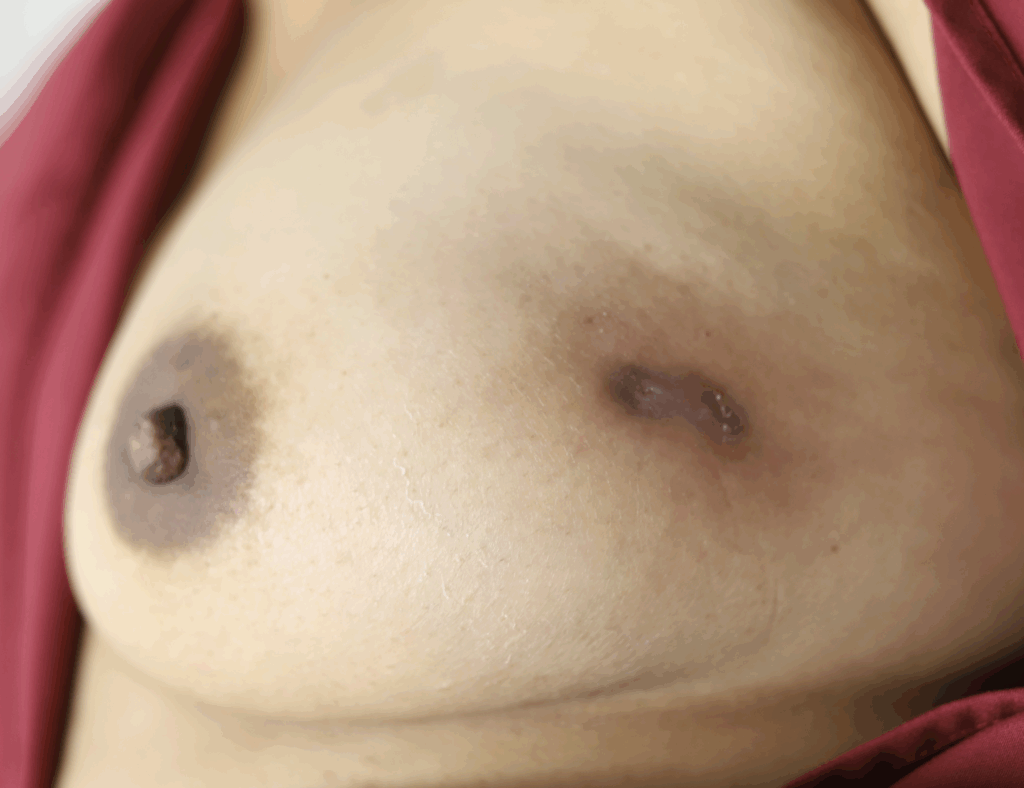
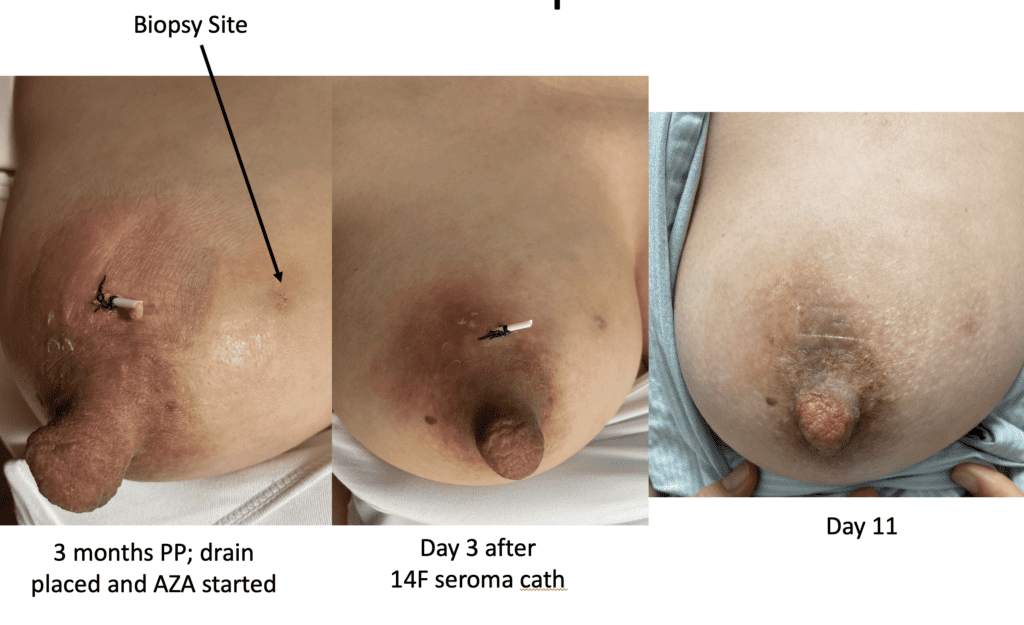
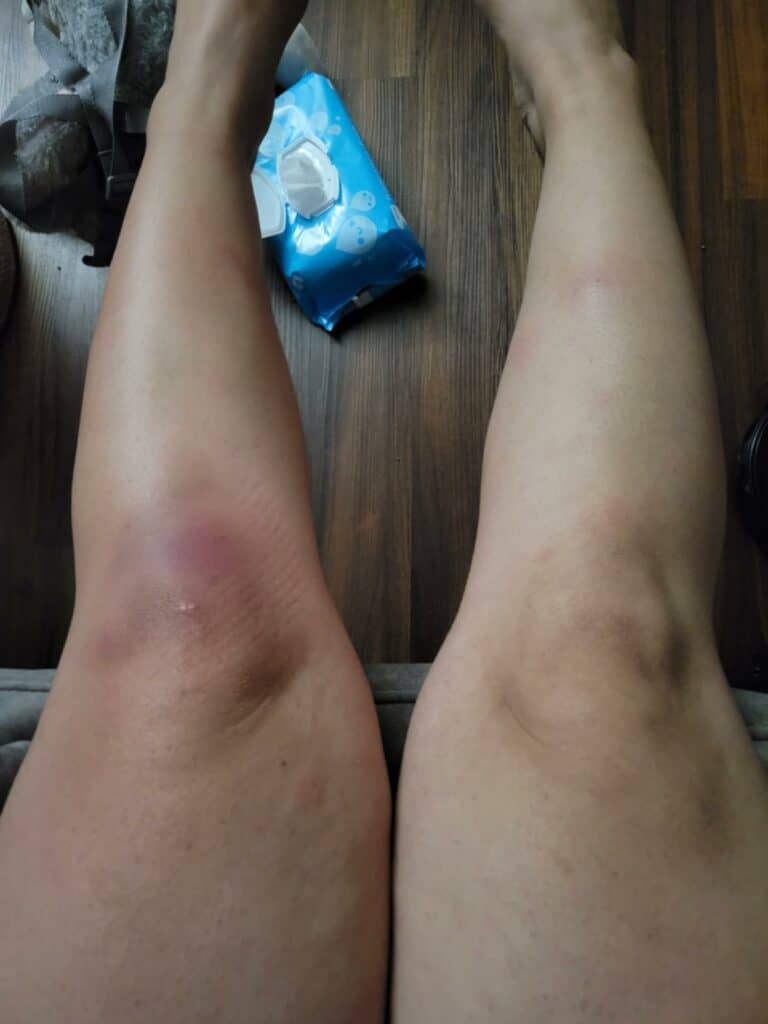
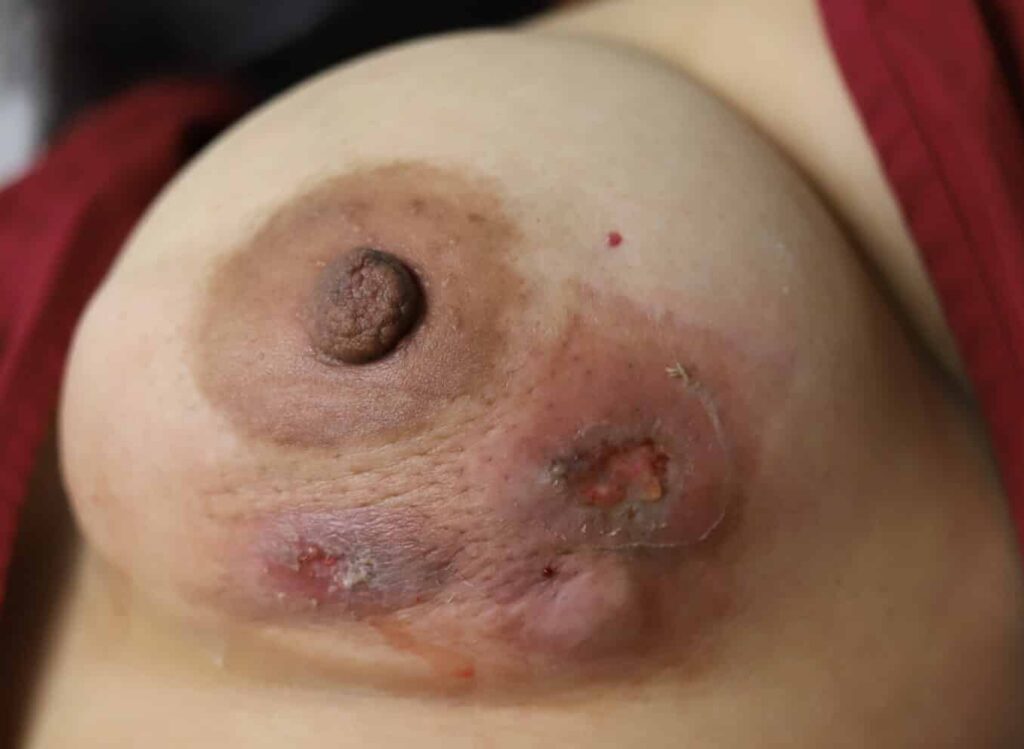
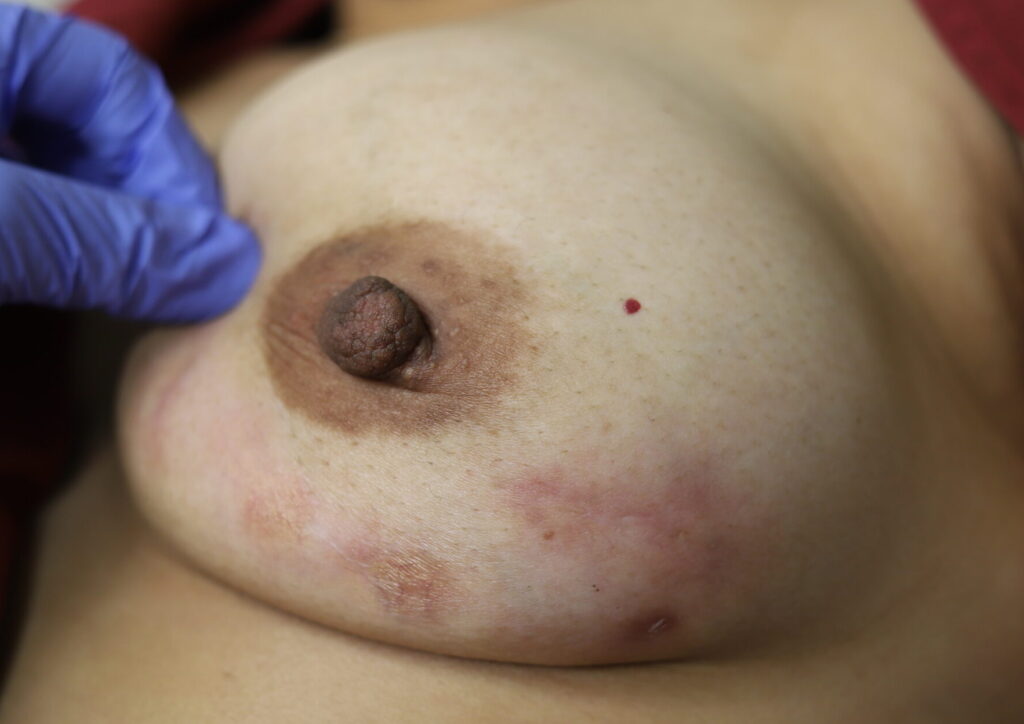
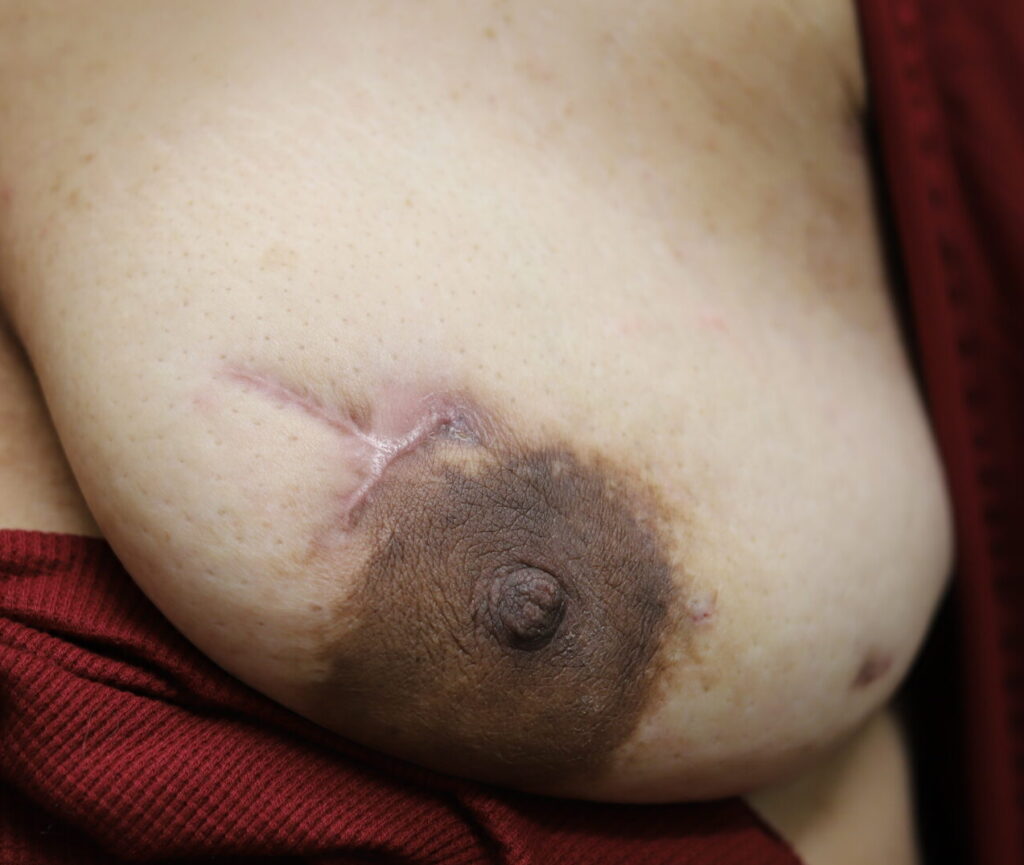
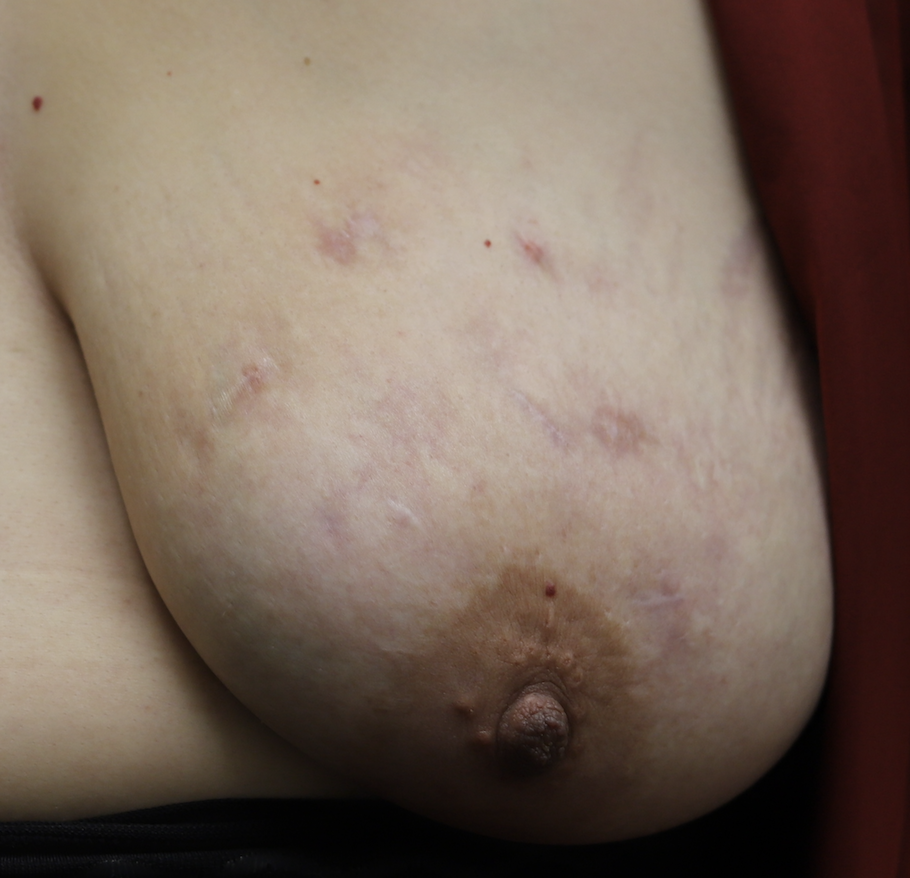

While some cases of IGM may resolve from a simple mass, many go on to form fluid collections (above and below) that may drain on their own. These are mistakingly called “abscesses.” They are in fact just fluid collections of dead inflammatory cells. Patients need either local treatment with needle drainage of the fluid (NOT large incisions with packing tape, which make inflammation worse) and steroid injection, or oral steroids/anti-inflammatories/immune suppressants.
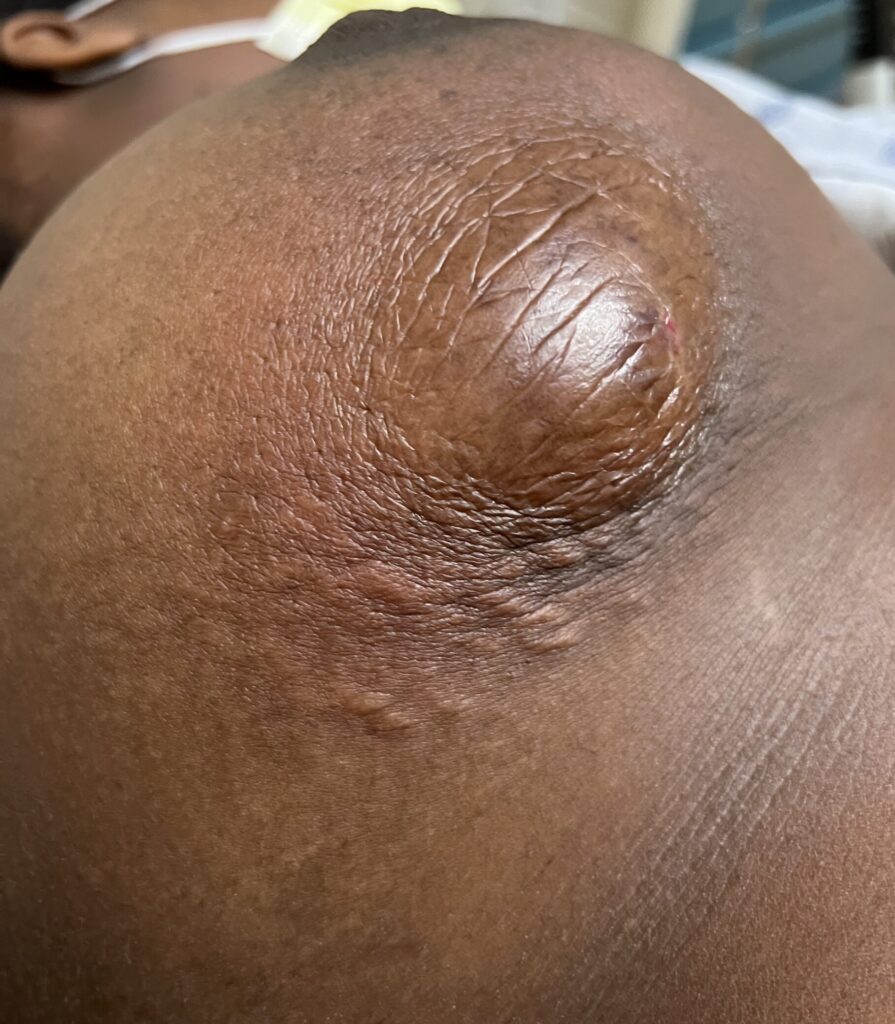
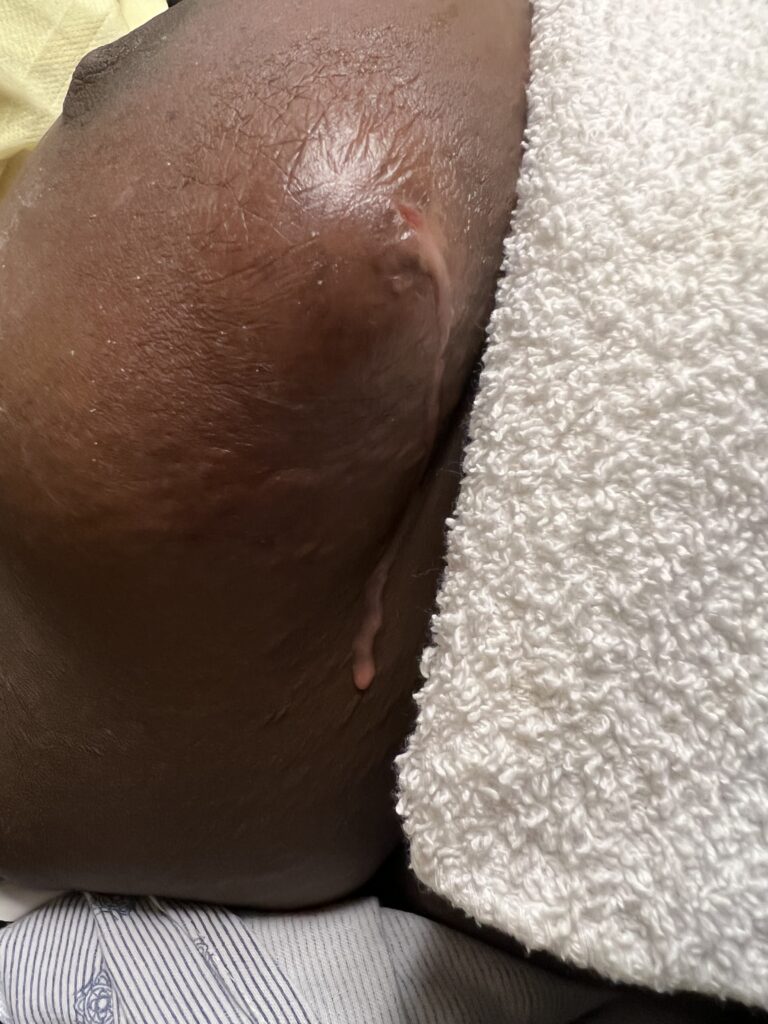
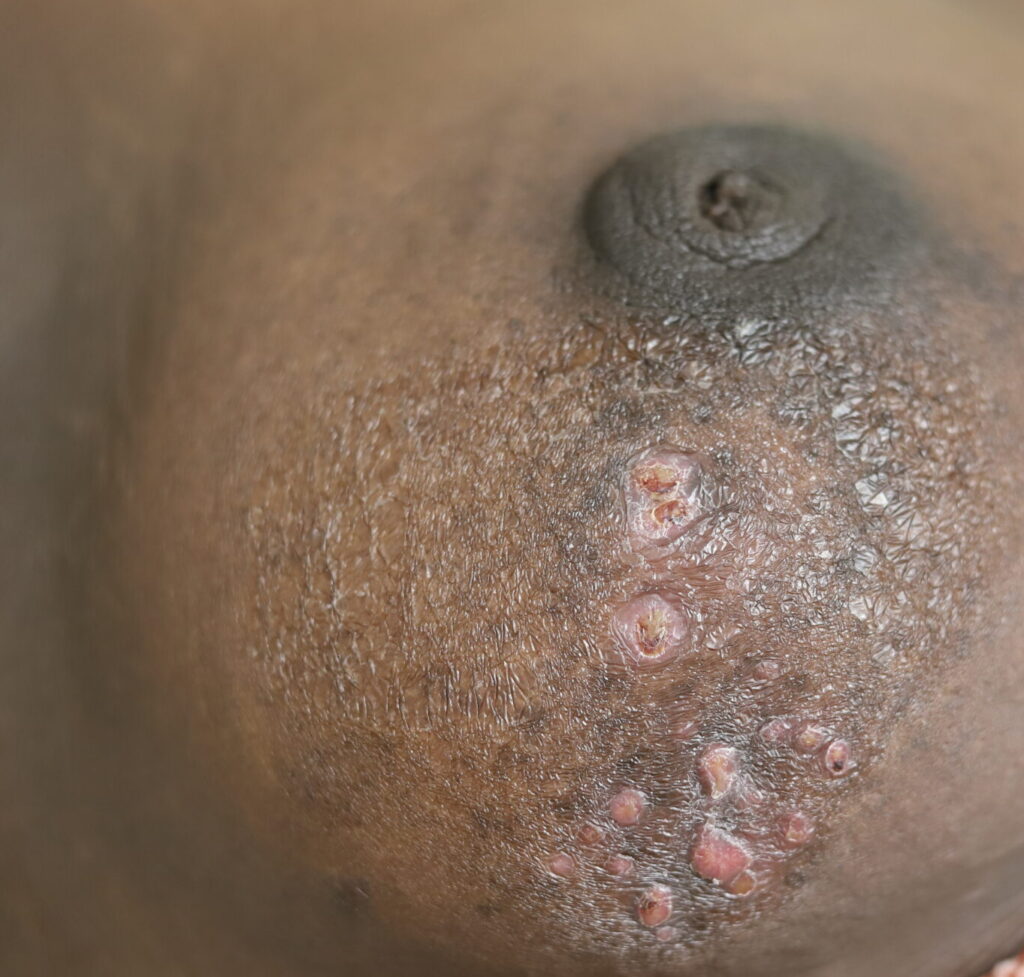









Fibroadenoma
Fibroadenomas are the most common benign (non-cancerous) growth of the breast. Fibroadenomas grow during pregnancy and lactation, and can significantly change appearance on ultrasound. Therefore, biopsy to confirm diagnosis prior to pregnancy is very important. If the lesion is not able to be confirmed fibroadenoma and is designated a non-specific fibroepithelial lesion, the patient should undergo excision to determine whether the lesion is a fibroadenoma or a phyllodes tumor (which can grow more rapidly and may not always be benign).
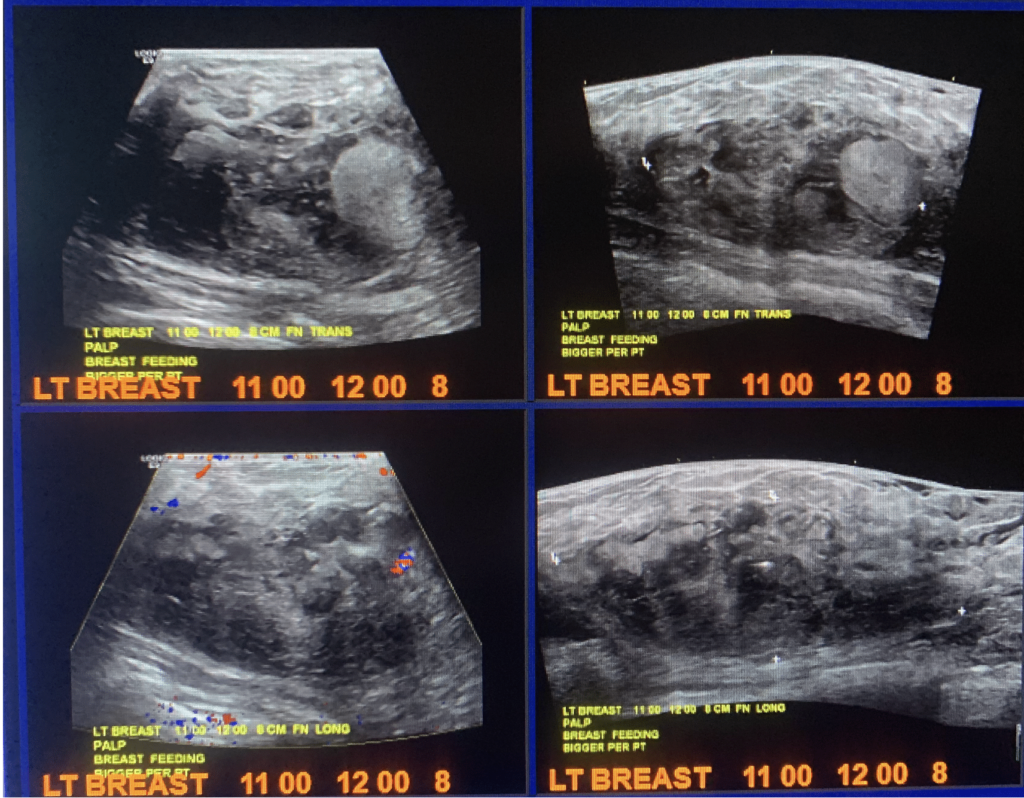
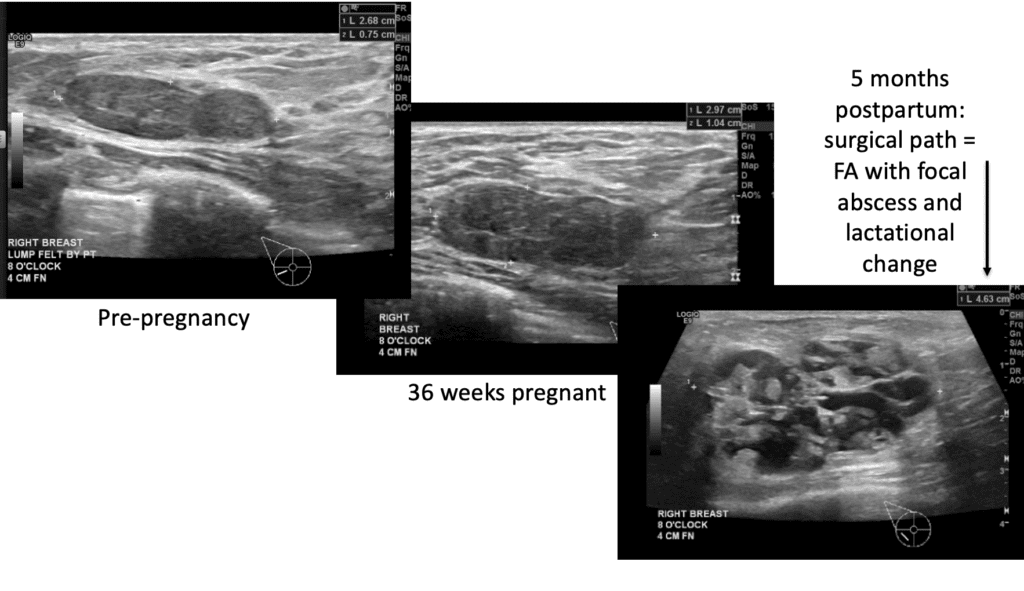
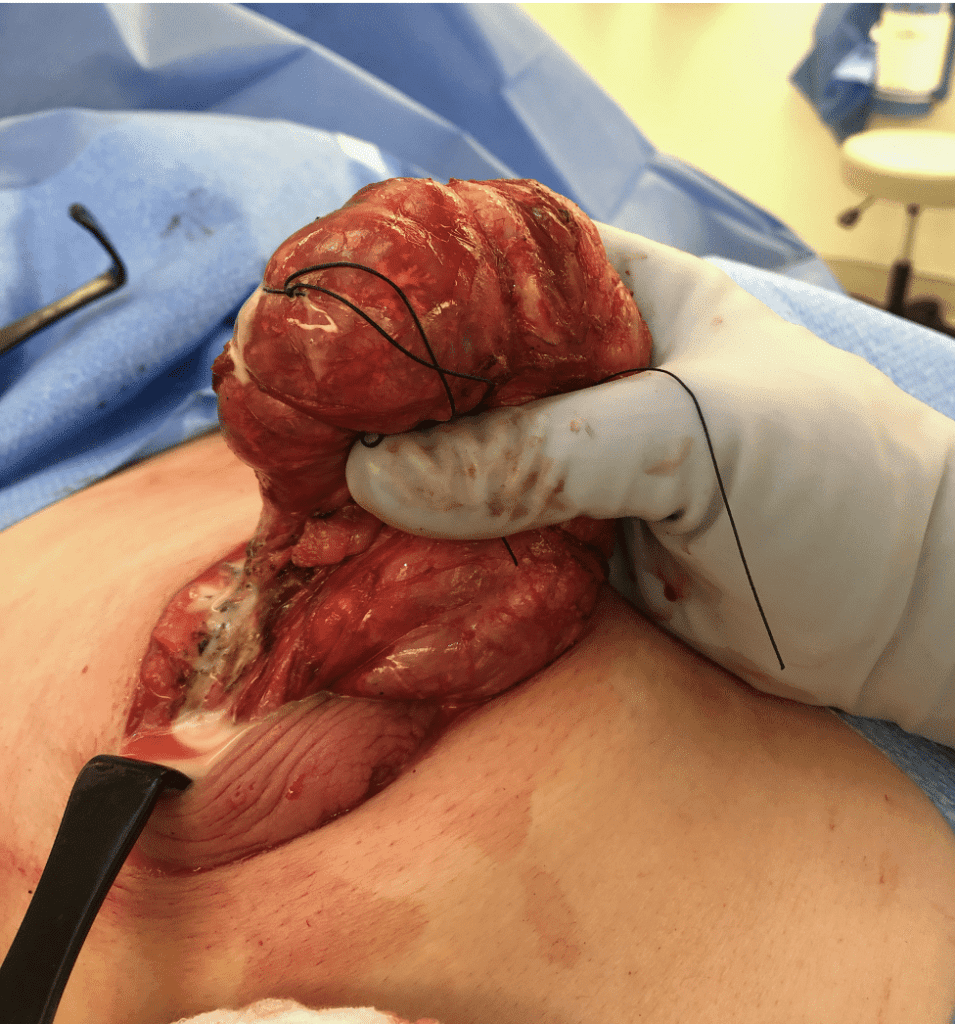
The video below demonstrates removal of a phyllodes lesion during lactation. There are several things to learn from this video:
- Breast imaging, breast biopsy, and breast surgery are safe during pregnancy and lactation. In fact, it would have been more ideal to remove this mass during pregnancy (before it grew and to rule out anything worrisome like a malignant phyllodes tumor). It also is far easier to operate without complication on a pregnant, rather than lactating, breast.
- In retrospect, this patient would have benefitted from a drain post-operatively rather than repeated aspirations.
- Breastmilk is under autocrine (local – i.e. the breasts function independently) control after two weeks postpartum (the first two weeks are endocrine, or central control). This means you can upregulate and downregulate the breasts independently.
- It is very important to treat hyperlactation (overproduction of breastmilk) in general, as well is when it is present when a patient requires surgery.
Hamartoma
Hamartoma is another benign (non-cancerous) mass in the breast that is not common but can present in the breastfeeding population. Like fibroadenomas, hamartomas can grow during pregnancy and lactation.
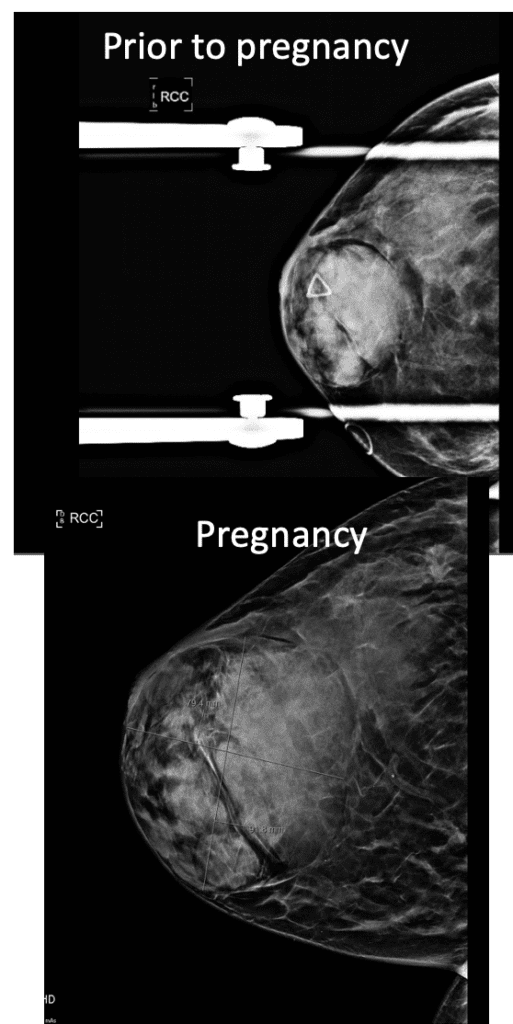

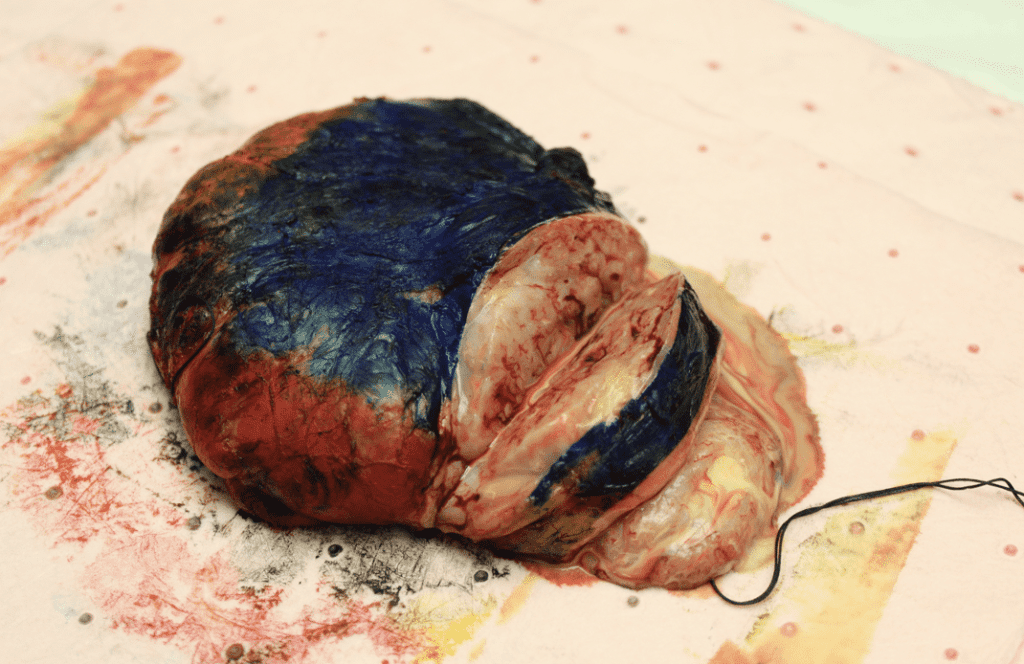

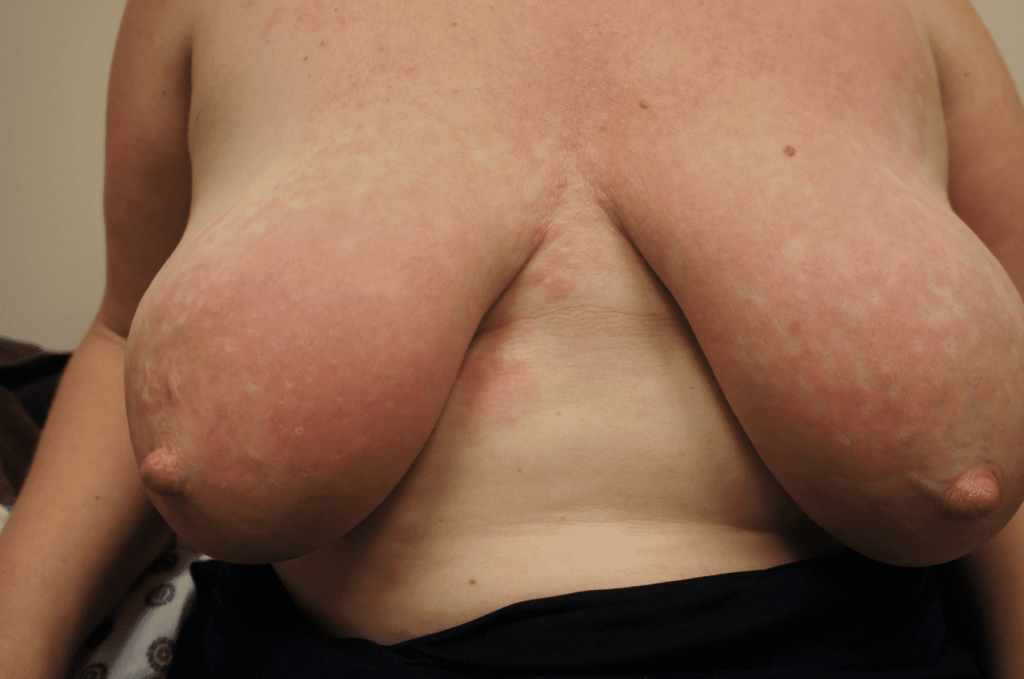
Dermatitis (Eczema)
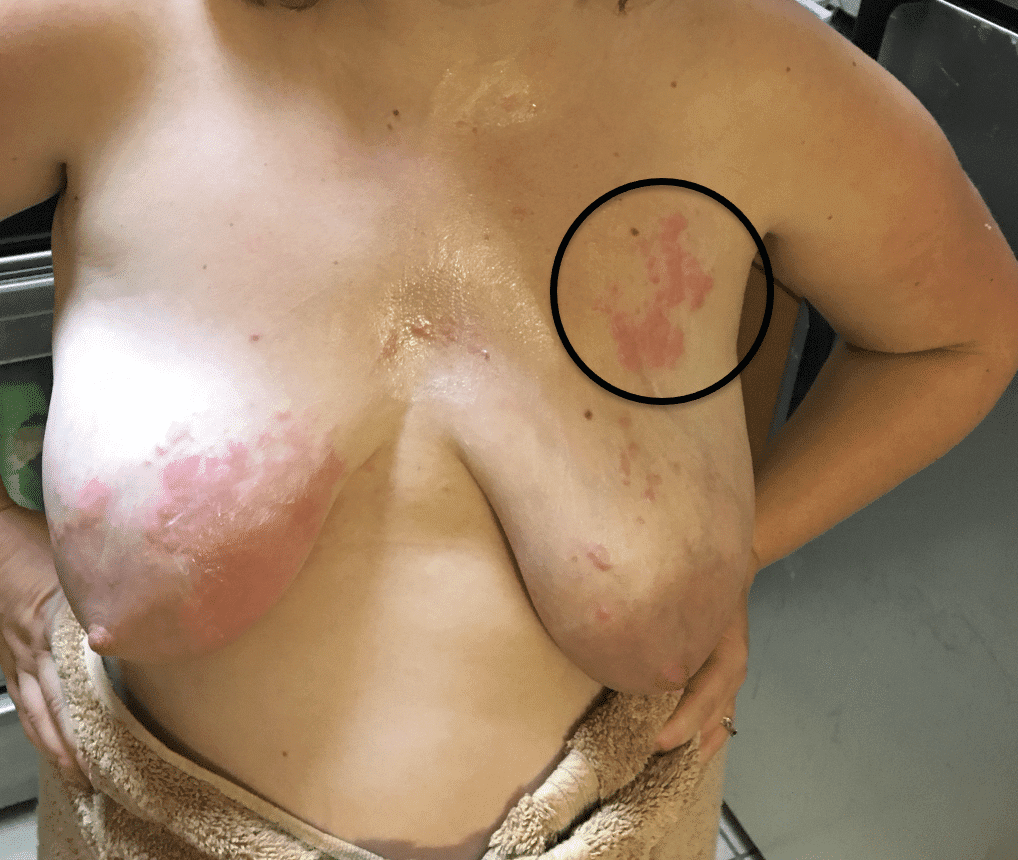
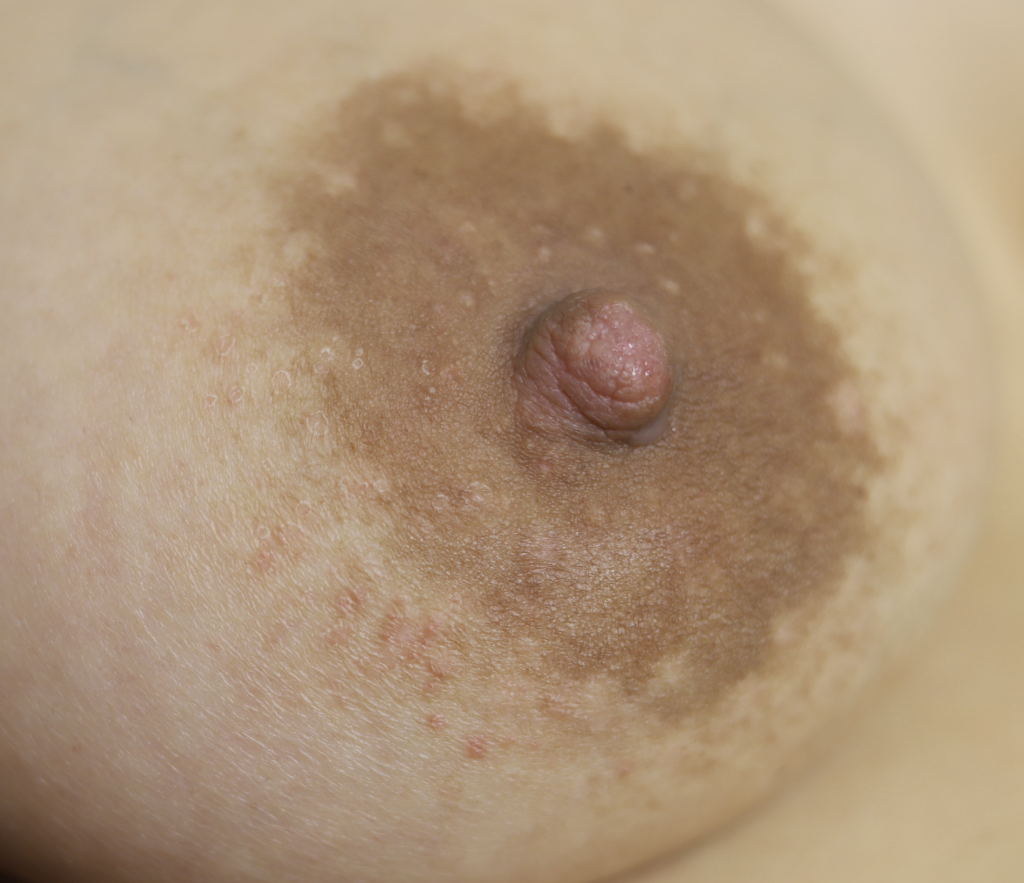
Breast dermatitis may occur in the setting of lactation and may be related to underlying predisposition to eczema and/or reaction to new allergens a mother is exposed to through breastfeeding products and/or her infant. Breast dermatitis management follows the principles of NAC dermatitis management as outlined in the Nipple Complications section. Patients should remove allergens and use a prescription steroid crème such as 0.1% triamcinolone for a short period of time to resolve symptoms.



Mondor's Disease
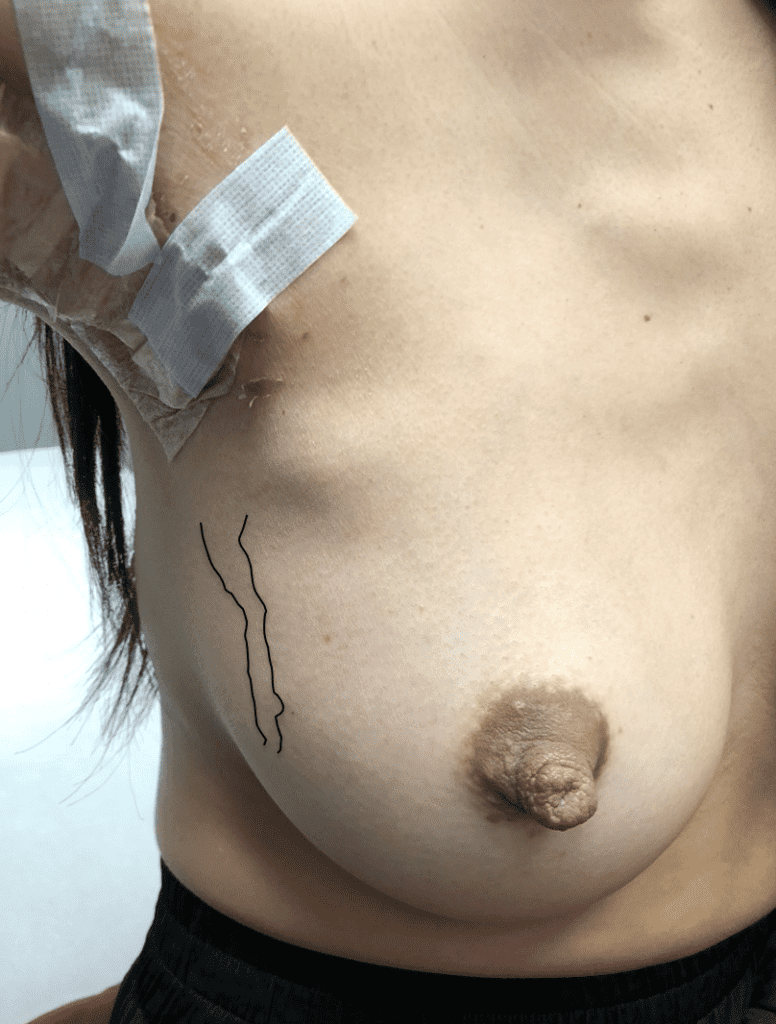
Superficial thrombophlebitis (inflammation of veins) of the chest wall veins is termed Mondor’s disease. The affected vessel, most often along the side of the breast closest to the arm, assumes the appearance of a tender, red “cord”. This condition self-resolves in several weeks and may be treated symptomatically with anti-inflammatory medication, moist heat, ice, and therapeutic ultrasound.